Abstract
Objectives:
Intergenerational games offer a potential channel to impact parent–youth sexual health communication. The “Secret of Seven Stones” (SSS) is an 18-level online adventure game and parent website designed to engage parents and youth (11–14 years) in conversations about healthy dating relationships and sexual behavior and to provide sexual health skills training to youth. Study hypotheses were that SSS exposure would increase sexual health parent–child communication, increase youth intentions to delay sexual debut, and reduce youth exposure to situations that promote sexual activity.
Materials and Methods:
SSS was evaluated in the homes of parent–youth dyads randomly assigned to intervention (n = 40) and comparison (n = 45) conditions. Online surveys were used to collect baseline and three-month follow-up data on dyadic sexual health communication, determinants for communication and youth sexual behavior, and game usability ratings.
Results:
Dyads comprised parents (n = 83, 47% white, 93% female, 44.4 ± 5.8 years) and youth (n = 83, 42% white, 54% male, 12.9 ± 1.1 years, and 96% sexually inexperienced). Frequency of parent–youth sexual health communication and youth communication self-efficacy increased in those playing SSS compared with those in the comparison group (P < 0.01). Youth perceived parent–youth communication as more open and demonstrated significant improvement in condom and human immunodeficiency virus/sexually transmitted infection knowledge and perceptions of parents’ beliefs about sex (<0.001). Usability ratings were higher on ease, credibility, and helpfulness (all >78%) but lower on duration and appeal (<56%).
Conclusion:
This study demonstrated the utility of an in-home intergenerational sexual health education game to impact parent–youth communication by short-term follow-up. Further investigation of longer-term behavioral impact is indicated.
Keywords
Introduction
In the United States, adolescent sexual health remains a public health priority. Teen birth rates for youth 15–19 years of age approximate 13.6 births per 1000 females, 1 adolescents 15–24 years of age account for nearly half of new cases of sexually transmitted infections (STI) annually, and early sexual debut is associated with risky sexual behaviors that can compromise health outcomes.2,3 Sexual health programs can promote delayed sexual initiation for sexually inexperienced youth and risk reduction behaviors (e.g., condom use, contraceptive use, human immunodeficiency virus [HIV] and STI testing) for sexually experienced youth. Such programs target psychosocial antecedents to these behaviors and are benefited by contextualizing sexual health within a supportive social network (Fig. 1).4–8
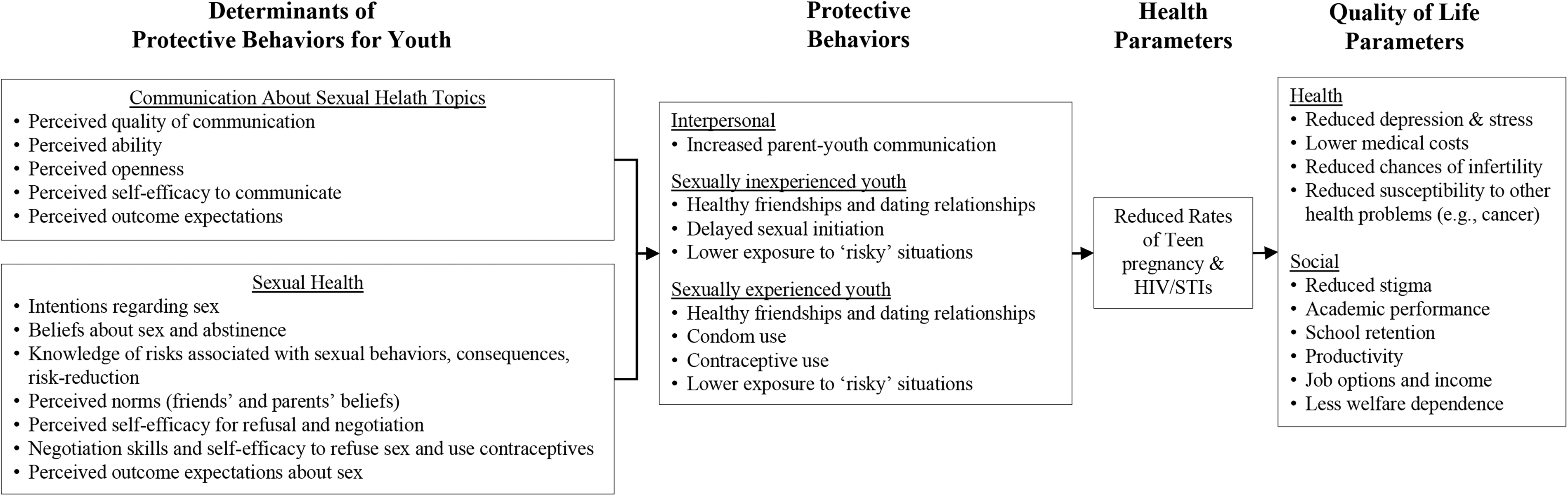
Within this social network, parents are critical in influencing youth risk behaviors.9,10 Empirically, health interventions involving caregivers demonstrate larger outcome effect sizes compared with those without caregivers. 11 Parental discussions can reduce risky sexual behaviors,12,13 delay sexual initiation, reduce teen pregnancy and STIs, and increase condom and contraceptive use. 14 Parents are not only open to discussing sexual health topics with their child 15 but also report barriers of limited knowledge, skills, or time, and feelings of embarrassment.16,17 Youth not only desire these discussions but also feel their parents need training on how to communicate about these topics. 18
School-based sexual health education programs can often improve youth sexual behaviors but provide only superficial parent involvement,19–23 while parent-focused and home-based in-person interventions focus on improved parent–child sexual health communication but often require intense parental training that limits reach and implementation.19,24 Youth-focused digital interventions can delay sexual initiation and reduce sexual risk behaviors, and such interventions are seen as appealing and relevant by parents and youth,25,26 yet parental involvement in these programs remains a challenge.13,19–22,27–31
Intergenerational serious gaming may have utility for improved parent involvement in sexual health education.25,32–34 An intergenerational game (IGG) for health provides a platform for adults and youth to learn and communicate with each other through collaborative engagement toward achieving a health-related objective. Intergenerational play can improve communication, learning, and emotional bonding between adults and youth, yet there is a dearth of research on the application of IGGs to enhance parent–youth communication and skills training for sexual health.35,36
The purpose of this pilot study was to explore the impact of an online sexual health IGG prototype, the “Secret of Seven Stones” (SSS), designed for in-home use by middle-school youth (11–14 years) and their parents. Respective hypotheses for youth and parents to assess primary and secondary outcomes were:
Youth
Compared with youth in the comparison condition, youth playing SSS will report significantly (1) increased communication frequency about sexual health with their parent; (2) increased intentions to delay sexual initiation (until high school graduation or marriage) and to use condoms if sexually active; (3) reduced exposure to risky situations; (4) improved attitudes, knowledge, and outcomes expectations regarding parental sexual health communication; (5) improved attitudes, knowledge, and perceived norms regarding delayed initiation of sexual behavior; and (6) improved quality of general parental communication.
Parent
Compared with parents in the comparison condition, parents accessing SSS will report significantly (1) increased communication frequency about sexual health with their youth; (2) improved perceptions of their youth’s intentions toward delayed sexual debut and condom use; (3) improved attitudes, knowledge, and outcomes expectations regarding youth sexual health communication; (4) improved attitudes and knowledge regarding their youth’s delayed initiation of sexual behavior; and (5) improved quality of general communication with their youth.
Materials and Methods
Study design and participants
The SSS was evaluated using a randomized, two-group pre- and post-test design in which parent–youth dyads (n = 85) were randomly assigned to intervention (n = 40) and comparison (n = 45) conditions. Inclusion criteria required participants to be English-speaking, that the youth be 11–14 years old, and that parents have mobile phones with short message service, and a home computer with consistent internet access. The study was conducted from Fall 2014 through Fall 2015 in a large, metropolitan area in southeast Texas that was geographically convenient to enable in-person data collection.
Recruitment and randomization
Interested parent–youth dyads (n = 109) contacted the research coordinator in response to community magazine and newspaper advertisements (32 dyads), school presentations (20 dyads), professional meetings (2 dyads), flyers posted in clinics and universities (13 dyads), or parental referral (42 dyads). Of these 109 dyads, 85 agreed to a home visit to obtain parental consent, youth assent, and baseline assessment, followed by simple random assignment of dyads into study conditions based on an a priori random number array. The remaining 24 dyads were ineligible, too busy, unable to commit for the duration, or unresponsive. Retention at 3-month follow-up was 97.6% (83 dyads-39 Intervention and 44 Comparison). Two dyads (one in each study condition) were lost to follow-up due to illness and disinterest, respectively. Incentives for each survey completed were $20 (youth) and $40 (parents). The study was approved by the UTHealth Houston institutional review board (HSC-SPH-12-0584) and the school district’s Office of Research and Accountability.
Intervention condition
The SSS prototype comprised (1) an adventure game, (2) text messages, and (3) a parent website. The description of SSS game mechanics and components has been published in detail elsewhere. 35
In the SSS adventure game, youth progress sequentially through 18 levels (each of 45–60 minutes duration) and win by rescuing 45 citizens in the town of Seven Stones from an evil “boss.” 35 In a single sequence of play the youth (1) visits a town location; (2) meets citizens who have an interpersonal challenge (e.g., protecting personal rules in the face of peer pressure); (3) visits the “Dojo” and completes educational activities (e.g., animations, mini games, role model videos, and simulations) to build relevant knowledge and skills; (4) completes a “challenge” quiz to earn “wisdom,” “skill,” and “support” battle cards (with higher quiz scores equating to higher value cards); and (5) engages in a card “battle” against the “boss” (Fig. 2). Winning the battle frees the citizen and enables continued game progress. A loss leads to remediation in the dojo to earn stronger cards and a repeat battle.

Example “Secret of Seven Stones” game components.
SSS is founded on social cognitive theory (SCT) and a life-skills self-regulation paradigm (Select, Detect, Protect) where youth select personal rules, detect challenges, and protect their rules.4–6,20–22 SCT methods include goal setting (e.g., youth sets personal rules and strategies), enactive mastery and verbal persuasion (e.g., interactive simulations), reinforcement (e.g., mastery of content enables higher value battle cards that enable battle wins and game progress), and modeling (e.g., parent/youth video testimonials describing communication success strategies).20–22,37,38 Educational topics comprise communication and negotiation, future goals and personal rules, healthy and unhealthy friendships and dating relationships, puberty and reproduction, consequences of sex, responsible internet use, dating violence prevention, and condom and contraceptive use. Embedded skills training activities (n = 179), each approximating 1–12 minutes, include mini-games, peer-modeling videos, fact sheets, virtual role-playing activities, and quizzes.20–22
Seven automatic text messages were sent to the parents that provides updates on their youth’s progress, cues to initiate a PEP talk (Partner-Engage-Plan) to discuss their youth’s behavioral goals and topics relevant to the educational topics covered by their youth (listed above), and linkage to the relevant activity on the parent website (discussed below). In each PEP talk, dyads partner together in a distraction-free environment, engage with each other to discuss SSS content, and plan strategies to maintain the conversation and protect the youth’s personal rules. After each PEP talk, parents retrieved a code that unlocked the next game level for their youth.
The SSS parent website was designed to increase parents’ involvement in the SSS game and build communication skills and self-efficacy to engage in each PEP talk. Parents could monitor their youth’s progress, adjust SSS content settings, preview game activities, access 15 3-minute peer role model videos describing positive real-world communication experiences, and refer to tip sheets describing strategies to engage youth.
SSS implementation occurred in the home on desktop computers. Trained study staff set up parent website accounts, installed SSS, gave an introductory orientation, and recommended a schedule for frequency and duration of play to enable SSS completion within a three-month testing period.
Comparison condition
Comparison condition dyads received “usual care,” defined as any dyadic or family communication, activities, or classes about sexual health that would occur in the context of regular family, school, and community life, irrespective of the study. They received baseline and follow-up surveys but no SSS exposure.
Data collection
Data were collected using computer-assisted self-interviews on study laptop computers in the home, and follow-up data were collected at 93 (±5.9) days post-baseline.
Primary outcome measures
The frequency of parent–youth conversations was assessed for eight sexual health topics in the past 3 months (Table 1). 39 Youth intentions to engage in oral or vaginal sex, remain abstinent until the end of high school or until marriage, and use a condom (if sexually active) and youth exposure to situations that could promote sexual activity were assessed with items having had extensive pretesting with middle school aged adolescents.20–22 Parents’ perceptions of their child’s intentions regarding sexual activity were also assessed.
Primary Outcome Measures
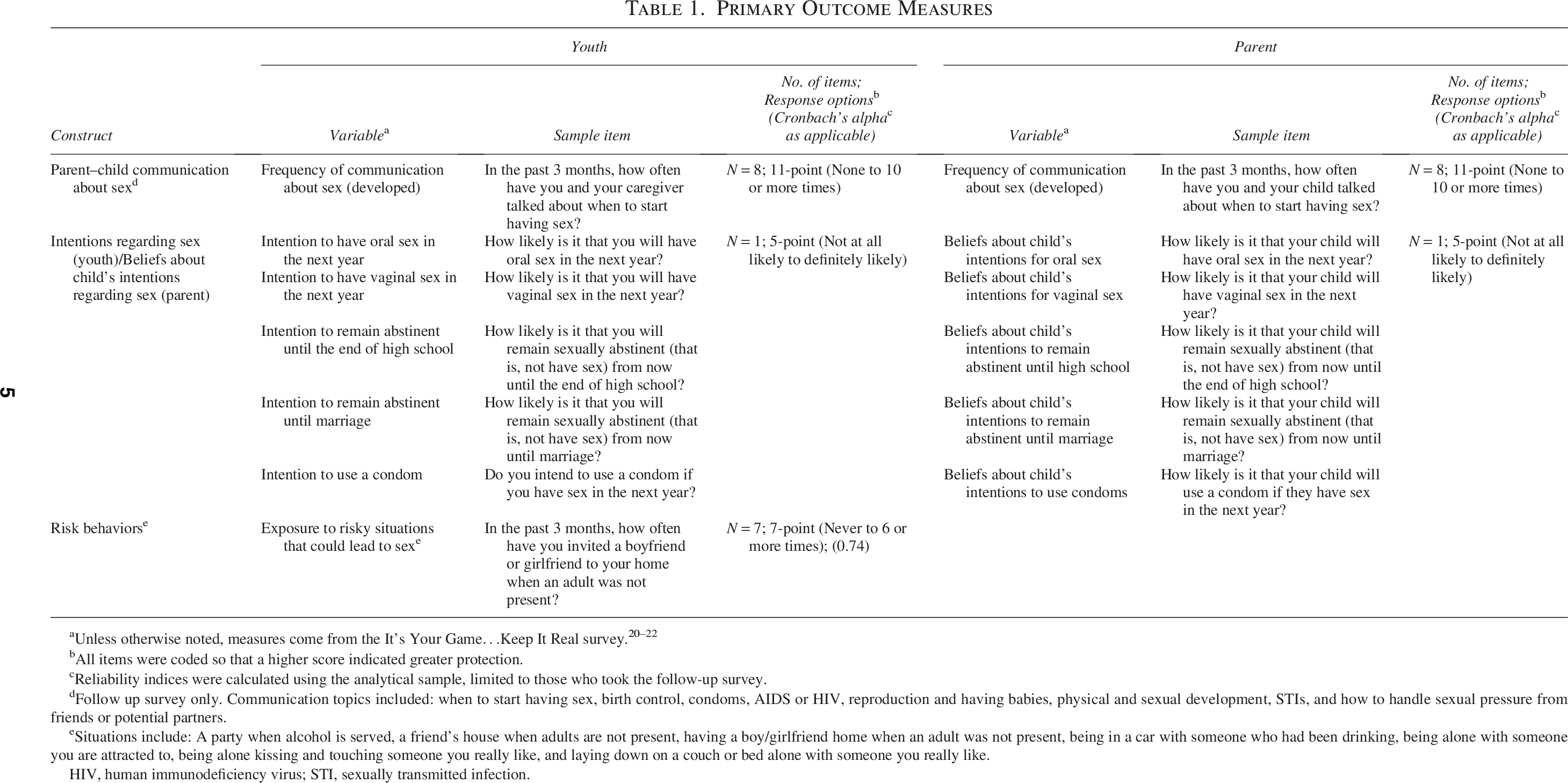
All items were coded so that a higher score indicated greater protection.
Reliability indices were calculated using the analytical sample, limited to those who took the follow-up survey.
Follow up survey only. Communication topics included: when to start having sex, birth control, condoms, AIDS or HIV, reproduction and having babies, physical and sexual development, STIs, and how to handle sexual pressure from friends or potential partners.
Situations include: A party when alcohol is served, a friend’s house when adults are not present, having a boy/girlfriend home when an adult was not present, being in a car with someone who had been drinking, being alone with someone you are attracted to, being alone kissing and touching someone you really like, and laying down on a couch or bed alone with someone you really like.
HIV, human immunodeficiency virus; STI, sexually transmitted infection.
Secondary outcome measures
Psychosocial determinants of parent–child communication comprised perceived quality of communication, 39 communication ability, 39 communication openness, 40 self-efficacy for parent–child communication, 41 and outcome expectations for communication (Table 2). 41 General parent–child communication was assessed on dimensions of openness and problems. 42
Secondary Outcome Measures for Youth and Parents 1
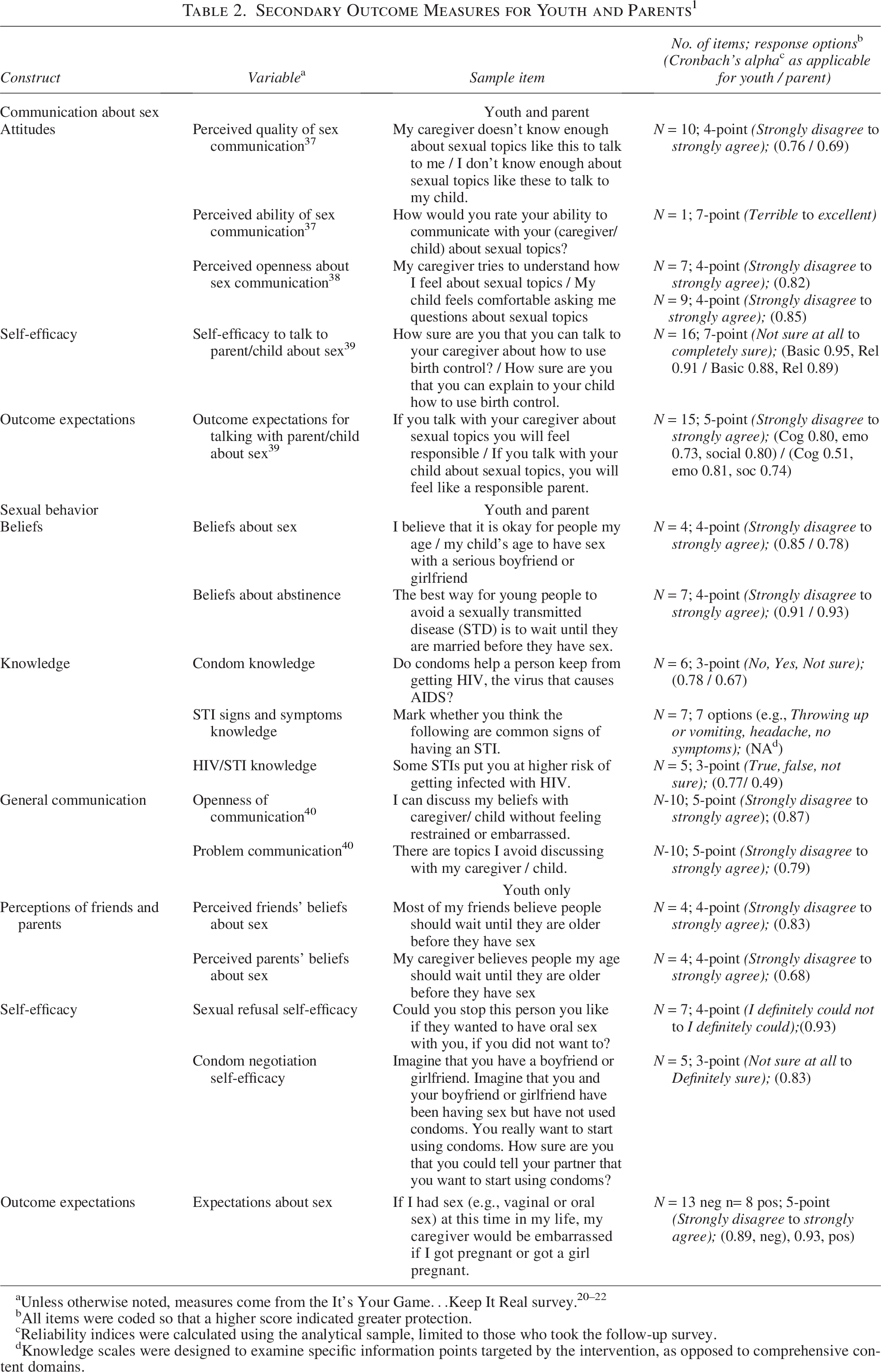
All items were coded so that a higher score indicated greater protection.
Reliability indices were calculated using the analytical sample, limited to those who took the follow-up survey.
Knowledge scales were designed to examine specific information points targeted by the intervention, as opposed to comprehensive content domains.
Psychosocial determinants of youth sexual initiation comprised youth attitudes about sex and abstinence, knowledge regarding HIV/STIs and condoms, perceived friends’ and parents’ beliefs about sex, self-efficacy to refuse sex, self-efficacy to use condoms, and expectations regarding sex (Table 2).20–22,39 Parents were also assessed on their beliefs about sex and abstinence, and knowledge regarding HIV/STIs, and condoms.
Usability
SSS was assessed on likeability, ease of use, duration, understandability, credibility, perceived impact, motivation to play, and appeal using youth and parent rating scales. 35
Demographic measures
Demographic measures included gender, age, grade, race/ethnicity, youth academic performance, parental education, household structure, household annual income, religiosity, and parenting style, adapted from other adolescent research.20–22 Items assessing youth sexual experience included ever having a boyfriend or girlfriend and ever engaging in oral and/or vaginal sex.20–22 Gaming experience included preferred platforms and frequency of play in the last 3 months. 43
Data analysis
Between-group differences in outcome variables from baseline to 3-month follow-up were evaluated using linear regression. Univariate regressions were run to assess between-group differences. Youth age at baseline, gender, ethnicity, and time between test administrations were entered into all models as covariates to adjust for any confounding variables. Missing values were left as missing and not imputed. All analyses were conducted using SAS 9.4.
Results
Sample characteristics
The analytic sample consisted of 83 parent–youth dyads. Youth were 12.9 (±1.1) years old, 54% male, 42.2% white, reported mainly A and B academic grades (75.9%), and most had never had a boyfriend or girlfriend (65%), vaginal (96.3) or oral sex (98.8%), nor any sexual health instruction in the last 3 months (65.9%) (Table 3). Parents were 44.4 (±5.8) years old, female (92.8%), of similar ethnicity to their youth, reported at least some college education (80.8%), were from two-parent households (73.5%), had over $50K income (72.3%), and were of Christian faith (86.1%). Youth reported that parents typically made decisions on their behalf (84.3%), often after asking their opinion (58.5%). Youth played games over 2 hours/week (69.6%), mostly on gaming consoles (35.8%) and phones (29.6%). Top-ranked genres were (in rank order): creative, fighting/shooter, adventure, casual, and simulation games. Parents played under 2 hours/week (87.4%), mostly on phones (56.3%). No significant demographic differences were observed across intervention and comparison groups. Top-ranked genres were (in rank order): casual, board, quiz, exercise, and educational games.
Sample Characteristics of the Final Analytic Sample (n = 83 Parent–Youth Dyads) a
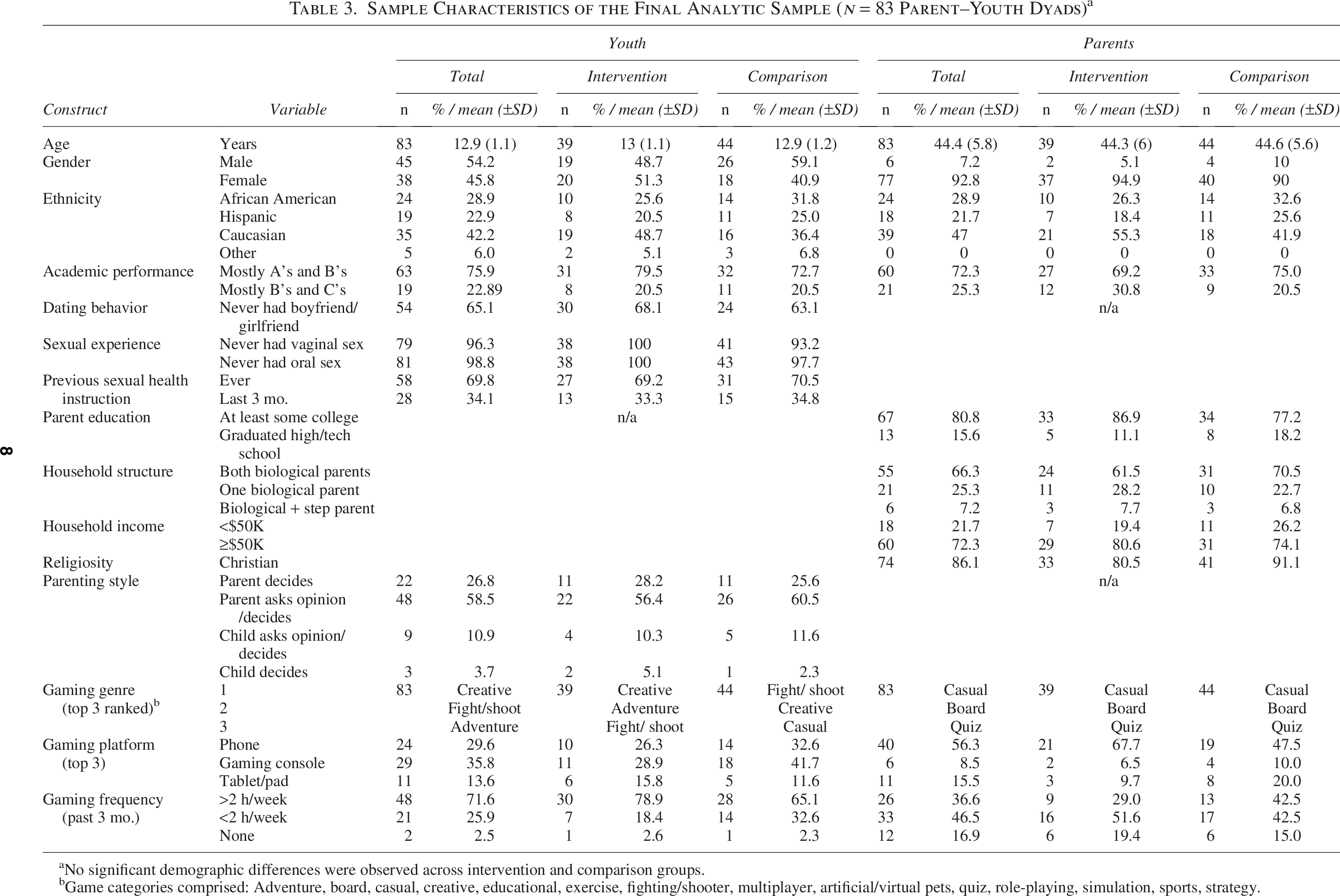
No significant demographic differences were observed across intervention and comparison groups.
Game categories comprised: Adventure, board, casual, creative, educational, exercise, fighting/shooter, multiplayer, artificial/virtual pets, quiz, role-playing, simulation, sports, strategy.
Primary outcomes
Parent–child frequency of communication about sex
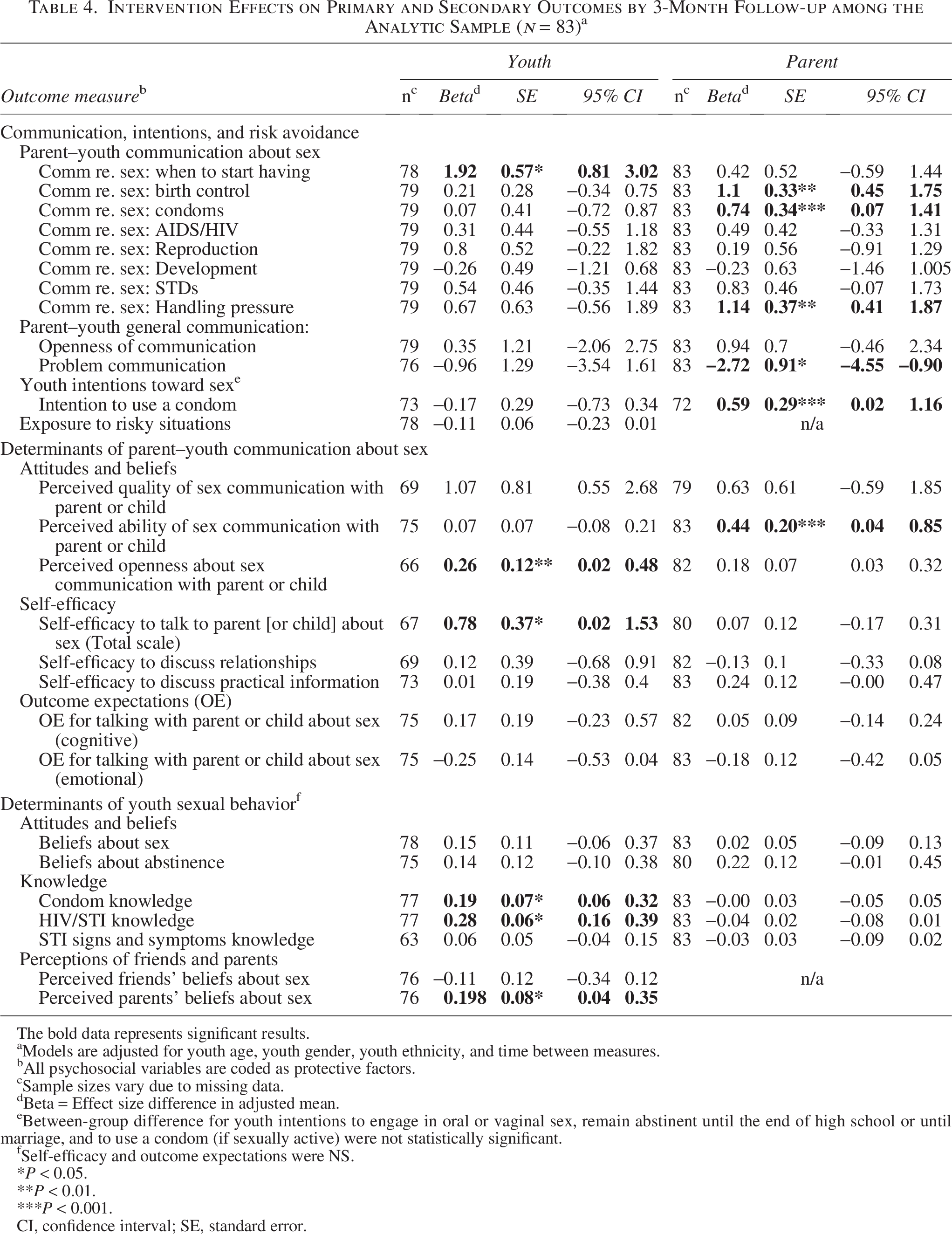
Youth exposed to SSS reported increased discussion regarding when sex should be initiated (P = 0.0012) (Table 4). Their parents reported increased discussion regarding birth control (P = 0.0014), condoms (P = 0.034), and handling peer pressure (P = 0.0028). Youth intentions and risk exposure did not change significantly. Parents reported an increase in their youth’s intentions to use a condom if they engaged in sex (P < 0.05), but that change in other youth’s intentions was not significant.
Intervention Effects on Primary and Secondary Outcomes by 3-Month Follow-up among the Analytic Sample (n = 83) a
The bold data represents significant results.
Models are adjusted for youth age, youth gender, youth ethnicity, and time between measures.
All psychosocial variables are coded as protective factors.
Sample sizes vary due to missing data.
Beta = Effect size difference in adjusted mean.
Between-group difference for youth intentions to engage in oral or vaginal sex, remain abstinent until the end of high school or until marriage, and to use a condom (if sexually active) were not statistically significant.
Self-efficacy and outcome expectations were NS.
P < 0.05.
P < 0.01.
P < 0.001.
CI, confidence interval; SE, standard error.
Secondary outcomes
Psychosocial determinants of parent–child communication
Youth exposed to SSS reported significantly more openness about sexual health communication with their parent (P = 0.031) and self-efficacy to talk to their parents about sex (P = 0.043) (Table 4). Parents reported greater ability to communicate with their youth about sex (P = 0.017) and significantly reduced problem communication (P = 0.003). Psychosocial determinants of youth sexual behavior: Youth exposed to SSS reported significantly greater knowledge about condoms (P = 0.005) and HIV/STIs (P ≤ 0.001) as well as more positive perceptions of their parents’ beliefs about sex (P = 0.013). Other determinants were not significant.
Intervention exposure
By 3-month follow-up, 24 dyads (60%) completed SSS, four dyads (10%) finished over 50% but did not complete SSS, and 12 dyads (30%) finished less than 50% of SSS. Delays in game play were attributed to competing school obligations and standardized testing, competing family activities, and program “bugs” (e.g., connectivity drops and program freezes).
Usability
Most parents in the intervention condition (70%) rated SSS favorably on all usability parameters except game duration. Most youth (70%) agreed that SSS was easy to use and would be impactful. Fewer youth (<70%) agreed that SSS was of appropriate duration, motivationally appealing, likable, and accurate. More youth liked the dojo activities (72%) and battles (67%), while fewer liked the PEP talks (50%). Most parents (66%) and youth (78%) required no help to play SSS.
Discussion
This study is among the first to report on an IGG for sexual health education.
Results suggest utility in facilitating parent–youth sexual health communication and enhancing psychosocial determinants (self-efficacy toward parental communication, knowledge, and perceived norms) that is commensurate with findings from previous computer-based and gaming interventions to promote sexual health that report small to moderate effects on sexual behavior, sexual health knowledge, and safer sex self-efficacy and intentions.13,28,36
Increased communication about sexual initiation and risk reduction (birth control, condoms, and handling pressure) and youths’ improved perceptions of communication openness and increased confidence to talk to their parent about sexual health topics is encouraging. Youth traditionally report discomfort in discussing sexual health or disclosing sensitive issues with their parents.25,44–46 IGG features, including a common educational experience, shared expectations for communication, and a game dynamic contingent on completion of PEP talks, may have contributed to these results.
Increasing youth confidence to discuss sexual health with their parents does little if parents themselves lack a similar confidence or are unprepared or untrained. The intergenerational dyadic approach offers advantages in this regard. Parents exposed to SSS reported greater ability to engage in communication and reported less problem communication, suggesting some mitigation of parents’ traditional feelings of discomfort and avoidance of these discussions.25,45–49 Parents’ increased perceptions that their youth would use a condom if they engaged in sex and youth’s enhanced knowledge about condoms and HIV/STIs were consistent with the increased parent–youth communication on this topic. Increased communication frequency did not prevent PEP talks from receiving the lowest likability rating from youth. These discussions were still not regarded as particularly “fun.”
The impact on psychosocial determinants of condom uses and increased positive perceptions of parents’ beliefs about sex were consistent with previous studies.11,20–22 Though not statistically significant, changes in the remaining determinants were in the predicted direction of protection for dyadic communication, delayed sexual initiation, and risk reduction. This suggests the potential for SSS to demonstrate greater effectiveness with increased analytic power.
Numerous national and professional guidelines advocate the implementation of sexual health education in schools and clinics.50–54 However, implementation of recommendations and sexual health education content and duration is inconsistent and often inadequate. 55 Parents remain a vital and consistent resource to facilitate life-skills training of their youth. 56 Policy- and decision-makers can support the inclusion of parents in this critical role by funding research into the development and dissemination of IGG best practice models in school, clinic, community, and home settings, and supporting evaluation of long-term outcomes of this strategy.
Results need to be interpreted in the context of study limitations. The randomized design, used to mitigate threats to internal validity, was not blinded by condition, so it was subject to possible compensatory bias. The short-term follow-up limited the ability to adequately assess behavioral changes such as risk avoidance or delayed sexual initiation. Using recall to assess communication frequency can introduce inconsistency because parents generally report higher frequencies,18,57 and report being more direct, less avoidant, and less controlling in conversations about sexuality than youth.44,58 SSS accommodates a passive, supportive gatekeeper role for parental players that represents one exemplar of an IGG, so findings are subject to mono-operational bias and may not generalize to all IGGs. 59 This study did not assess verbal and non-verbal communication mechanics and quality, including content, disclosure, depth, and flow. The degree to which discussions were superficial (e.g., simply handing over the unlock code) or “deep” (e.g., exchanging personal perspectives and experiences) remains open to further research.60–62 Despite positive usability ratings, many youths (30%) did not complete half of SSS, suggesting that it may be insufficiently motivating for all youths. This is important as exposure to core sexual health content needs to be sufficient to expect behavioral outcomes. 35 To more fully assess the fidelity of the parent website, tracking metrics are recommended. The study required greater statistical power to enable assessment of covariates (e.g., intervention intensity, duration, tailoring, and context), or moderating factors (e.g., preferred game genres or learning styles) that may have contributed to the findings and present a potential focus for future IGG research.
Conclusion
This study is among the first to rigorously evaluate an in-home IGG for sexual health education and demonstrated the utility of this strategy to positively affect parent–youth communication by short-term follow-up. The findings of this study are specific to the SSS but contribute to evidence for intergenerational gaming to increase parental involvement and enhance the reach and effectiveness of sexual health education. Further investigation of longer-term behavioral impact is indicated.
Authors’ Contributions
R.S.: Conceptualization, methodology, validation, investigation, resources, writing (original draft and review and editing), visualization, supervision, and funding acquisition. C.M.: Methodology, validation, and writing (review and editing). M.P.: Methodology, validation, and writing (review and editing). R.C.A.: Formal analysis and data curation. S.D.: Supervision and project administration. D.S.M.: Validation. S.T.E.: Methodology, validation and writing (review and editing). J.M.W.: Validation. E.B.: Formal analysis and data curation; L.A.: Investigation. P.C.: Investigation. H.-Y.S.: Investigation. A.S.: Investigation. J.M.: Conceptualization, methodology, resources, supervision, and funding acquisition.
Footnotes
Acknowledgment
This team would like to acknowledge the late Dr. Douglas Kirby for his enthusiasm for this work.
Author Disclosure Statement
The study was conducted under a National Institutes of Health R424 STTR (technology transfer) mechanism. This involves an inter-institutional agreement between the academic institution (UTHealth Houston) and the small business entity (Radiant Digital) and includes shared IP between these organizations if the intervention is marketed.
Funding Information
This work was supported by grant 1R42HD074324-01 from the National Institute of Child Health and Human Development, National Institutes of Health. This is a National Institutes of Health technology transfer grant with an inter-institutional agreement between the University of Texas Health Science Center at Houston (UTHealth Houston) and Radiant Digital.
Data Sharing Statement
The authors intend to make the study data available to other researchers subsequent to analysis by the research team. Analytic methods and study materials are available upon request to the corresponding author.
