Abstract
On March 11, 2020, the World Health Organization recognized the SARS-CoV-2 infection as a pandemic. The pandemic itself in addition to its containment measures affects individuals’ lifestyles and welfare including their sexual behaviors. Thus, we hypothesized that sexually transmitted infection (STI) incidence may be changed and so we evaluate urethritis incidence as the most common STI in men and some other related factors. Two cross-sectional surveys during the first 6 months of 2019 and 2020 were undertaken and data were collected from 11 urology offices located in different parts of the capital city. In total, 34,611 male participants were included in our study, and 191 (.55%) patients’ clinical diagnoses were urethritis. The urethritis incidence significantly decreased from 149 of 17,950 (.83%) to 42 of 16,661 (.25%) individuals in the same period of the years 2019 and 2020, respectively (p-value < .001). There was a higher percentage of single (p-value = .049) and older (p-value < .001) urethritis patients in the first 6 months of the year 2020 compared with 2019. Our survey provided urethritis incidence, demographics, symptoms, and treatment characterization. As our results show, the proportion of urethritis patients in all populations admitted to urologist offices had dramatically decreased during the COVID-19 pandemic compared with prior. The indirect effects of the pandemic and its containment measures on people’s sexual health should be noticed and an appropriate reaction and policy-making are recommended to manage issues properly in different aspects of sexual health.
Key Messages
Based on the data from 11 urology offices, urethritis incidence has significantly decreased during the COVID-19 pandemic.
The mean age of urethritis patients has significantly increased in the COVID-19 pandemic period.
Indirect effects of the COVID-19 pandemic on people’s sexual health should be noticed and an appropriate reaction is recommended on time.
Introduction
At the end of 2019, a new type of Coronaviruses was reported in Wuhan, Hubei, China, which is named severe acute respiratory syndrome coronavirus 2 or SARS-CoV-2 because of its main effect on the host‘s respiratory system (Fuchs et al., 2020; Yuksel & Ozgor, 2020).
SARS-CoV-2 could spread too quickly in the whole world and it was considered a pandemic on March 11, 2020, by the World Health Organization (Cito et al., 2021; Steffen et al., 2020). As a result, many countries rapidly reacted by containments like population quarantining in Italy or prohibiting public places to be opened in Poland (Cito et al., 2021; Fuchs et al., 2020). People’s lifestyles and welfare got affected by the pandemic itself besides the consequences of measures to contain it (Caruso et al., 2020; Panzeri et al., 2020). Therefore, changes in anxiety and depression levels, sleep and eating habits, and somatic symptomatology appeared (Panzeri et al., 2020).
SARS-CoV-2 was scarcely isolated from semen and there was no documentation of sexual transmission (Mahanty et al., 2021). Close contact that occurred during the act can lead to couples being infected (Naik, 2020). In addition to the previous point, cohabitations happened due to prevention measures and as expected accordingly sexual behaviors also changed (Caruso et al., 2020). Recently, some evidence shows alterations in sexually transmitted infection (STI) incidence in the United States and Taiwan (Crane et al., 2021; Lee et al., 2021). Former literature illustrated that STI incidence rates were remarkably different among countries. For instance, a French study mentioned that urethritis incidence in males during a decade was stable, while various research in the United States and Europe demonstrated an increasing trend for this disease (Rossignol et al., 2019).
Urethritis is the most common STI in men, which means infected urethra (Territo & Ashurst, 2021). Men with urethritis are mostly asymptomatic (Territo & Ashurst, 2021) though symptoms may include urethral discharge, irritation, or dysuria (Perkins & Decker, 2016). Sexual intercourse without protection, multiple sexual partners, and being youth or homosexual are some factors that may put you in some more dangerous situations (Reyniers et al., 2021; Young et al., 2021).
Infectious urethritis can be classified based on the offending agent as gonococcal or non-gonococcal (NGU) urethritis (Territo & Ashurst, 2021) usually due to Chlamydia trachomatis, which is critical for the patient’s treatment (Young et al., 2021).
Material and Methods
We conducted two retrospective cross-sectional surveys during the first 6 months of 2019 and 2020 to identify mainly the effect of the COVID-19 pandemic on urethritis incidence and changes in different variables that occurred in these two periods. Although studies were undertaken in 11 referral urology offices located in various parts of the capital city, the study participants were referred from the whole country and not just limited to the specific cities. Each office had at least a private room in which patients’ histories and examinations were carefully investigated by an expert urologist.
Male patients admitted to the clinics were asked about urethritis symptoms like any meatal secretions or urethral irritation or urinary tract infection manifestations in a private situation to acquire the most accurate data. In addition to urethritis characterization, a detailed medical history specifically on the patient’s lifestyle consisting of marital status (single or married), condom routine usage (yes or no), the usual number of partners (single or multi-partner), and being heterosexual or not was obtained. Moreover, the urologist reported each patient’s prescribed treatment regimen (ceftriaxone/doxycycline or streptomycin/doxycycline), and if any antibiotic resistance was identified, they were asked to mention it in the patients’ document.
Due to the complexity of confounding factors, participants who had characteristics including missing/unreliable data, a history of pelvic surgery/radiation, any psychiatric or neurologic disorder, or any malignancies were excluded from the study.
In addition, during these visits, patients were asked about using their data for research and publication purposes while their identification information was not disclosed and all the study’s participants willingly gave related verbal informed consent to their physicians.
Finally, SPSS Version 20 (SPSS, Chicago, IL, USA) was employed for statistical analysis. The number of participants and other variable values were collected. For continuous variables assessment, mean and standard deviation, and for the evaluation of categorical variables, the frequencies (number and percent) were considered. Chi-square test, Fisher exact test, and independent t-test were employed for the data analysis and the statistically significant difference was defined at p-values less than .05.
Results
Overall, a total of 34,611 participants were screened and 191 (.55%) were clinically diagnosed with urethritis. The analysis provided two clusters: Group 1 first 6 months of the year 2019 (n = 17,950 and 149 urethritis, .83%) and Group 2 first 6 months of the year 2020 (n = 16,661 and 42 urethritis, .25%).
The mean age of the study population was 25.9 years before and 31.2 years during the COVID-19 pandemic. The sociodemographic characteristics of the study participants are summarized in Table 1.
Demographic Characteristics and Sexual Status of Urethritis Patients Admitted to Urologists in the First 6 Months of the Years 2019 and 2020.
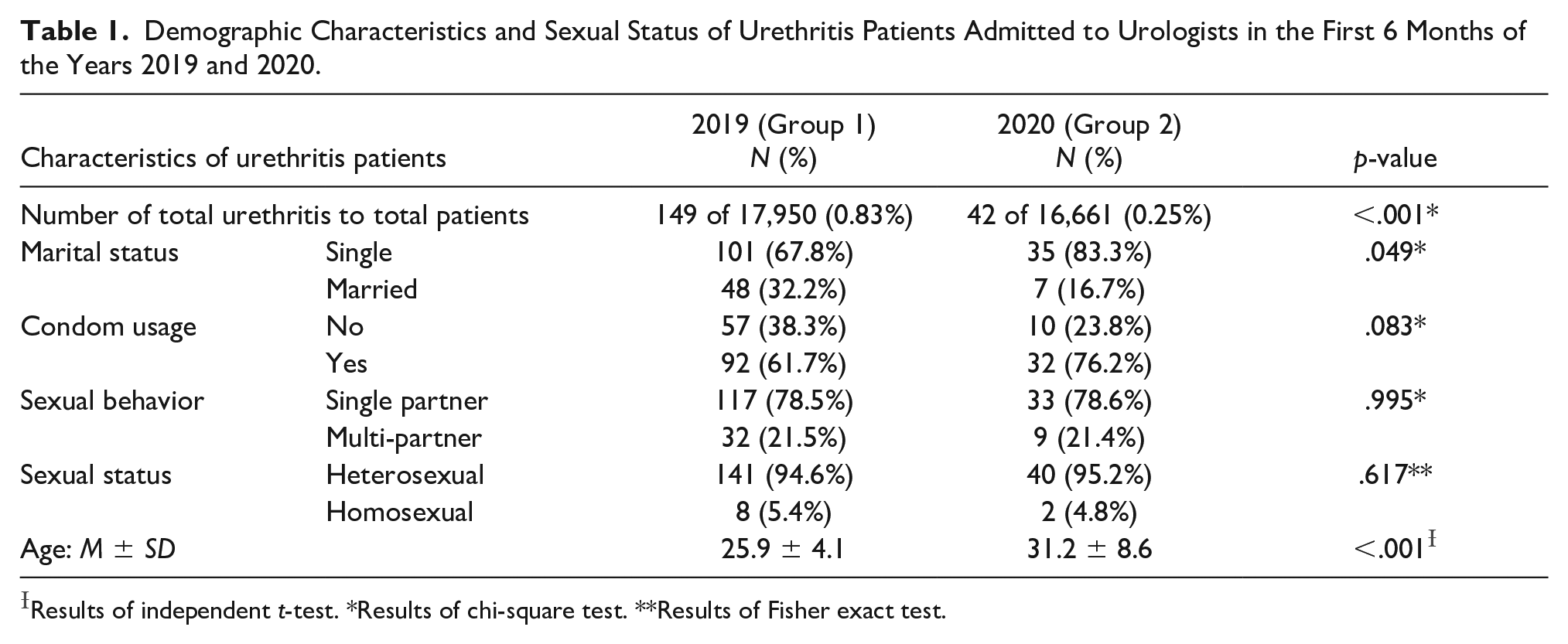
Results of independent t-test. *Results of chi-square test. **Results of Fisher exact test.
About two-thirds (n = 101, 67.8%) of patients with urethritis in 2019 mentioned marital status as single versus 35 (83.3%) individuals in Group 2. Moreover, on average 57 patients (38.3%) of Group 1 reported condomless sexual intercourse compared with 10 patients (23.8%) during the first 6 months of the pandemic. As regards sexual status, 141 (94.6%) men of Group 1 and 40 (95.2%) men of Group 2 described being heterosexual (Figure 1).

The Urethritis Patients Admitted to Urologists in the First 6 Months of the Years 2019 and 2020.
The results of Table 1 show that the proportion of urethritis patients in all populations admitted to urologists’ offices in the first 6 months of the year 2019 (149 of 17,950 patients, .83%) was 3.32 times higher in comparison with the same period of 2020 (42 of 16,661 patients, .25%), p-value<.001 in chi-square test. The percentage of single patients (p-value = .049, results of chi-square test) and mean age of patients (p-value < .001, results of independent t-test) were significantly higher in 2020 compared with 2019. The percentages of patients with high-risk behaviors, including not using a condom, having multi-partners, and homosexuality were similar in the two studied periods (p-values > .05, the first two and the third are calculated by applying chi-square and Fisher exact tests, respectively).
Our survey provided urethritis symptoms characterization in the study population, including urethral discharge, irritation, and dysuria prevalence among urethritis patients (Table 2). Half (80 [53.7%] and 22 [52.4%] individuals in the first 6 months of the year 2019 and 2020, respectively) of the patients with urethritis perceived dysuria symptoms, about 90% (131 and 40 participants in Groups 1 and 2, respectively) urethral discharge, and over eighty percent (127 and 35 participants in Groups 1 and 2, respectively) urethral irritation, without statistically significant difference between Groups 1 and 2 (p-values and employed tests are mentioned in Table 2).
Symptoms in Urethritis Patients.

Results of independent t-test. *Results of chi-square test. **Results of Fisher exact test.
We also assessed the prescribed treatments for the study population which is shown in Table 3. Doxycycline was prescribed for all urethritis patients in combination with ceftriaxone or streptomycin. About three-quarters (111 [74.5%] and 32 [76.2%] individuals in 2019 and 2020, respectively) of patients in both groups were managed by ceftriaxone/doxycycline, whereas the others got streptomycin/doxycycline for their complaint, without statistically significant difference between Groups 1 and 2 (p-value = .823, result of chi-square test). Although the rate of resistance to antibiotics was higher in 2019, this difference in Fisher’s exact test was not statistically significant (p-value = .143).
Status Treatment in Urethritis Patients regarding antibiotic resistance.

Results of chi-square test. **Results of Fisher exact test.
Discussion
Our study evaluates the impact of the COVID-19 pandemic and inherent restrictions on the urethritis rate and its related factors. The results show two exciting findings: first, the proportion of patients with urethritis to all population admitted to urologist offices during the pandemic had a large and significant fall in comparison with the same period in the previous year; and second, the age of the urethritis patient had been increased significantly.
Theoretically, these findings could be explained by some reasons. For example, a study in the United States among adolescent sexual minority males (ASMM) demonstrated that most participants were worried about COVID-19, so the majority reported being physically distanced from sexual partners, and besides they described increases in masturbating and viewing pornography (Li et al., 2020; Nelson et al., 2020). Another study declares an increasing trend in sex toy purchases and online pornography searches during the containment measures related to the COVID-19 pandemic (Li et al., 2020; Mahanty et al., 2021). Consequently, solo sex is assumed to be more common during the pandemic.
Besides, evidence in Italy shows that the majority of couples in quarantine reported less sexual intercourse per week; however, most of them did not report sexual desire reduction (Cito et al., 2021). So many confounding factors exist; during the pandemic, mood alterations and fear of COVID-19 effects on people’s lives can change the sexual health of participants. Furthermore, couples were forced to prolonged cohabitation, and also some had to spend much more time with children due to school cancelation, which resulted in repopulating the home by their presence and lack of privacy as a consequence (Cito et al., 2021; Panzeri et al., 2020). Although some studies declare decreasing trend in sexual desire and intercourse at the same time (Fuchs et al., 2020; Li et al., 2020), few findings in opposing ways show more frequent intercourse and growing sexual desire (Fuchs et al., 2020; Yuksel & Ozgor, 2020). Finally, however, our study demonstrated the number of partners has not significantly changed during these periods, Griffin et al. stated LGBTQ+ population in the United States chose fewer partners and lesser sexual activity during the pandemic compared with before (Griffin et al., 2022).
Our results align well with a finding in China about no changes in condom usage during this pandemic (Li et al., 2020), while other surveys showed condoms use to a lesser degree during the pandemic in China (Booton et al., 2020) and to a higher degree in Wales (Gillespie et al., 2021). Another harmonious study mentioned in Spain although the sexually transmitted infections (STI) incidence was diminished during the pandemic situation, people’s sexual behavior was not safe yet (Tarin-Vicente et al., 2022).
Assessing the changes in urethritis incidence was the main goal of our study. Previous studies report controversial findings. One indicated that during the COVID-19 pandemic streptococcal pharyngitis and acute otitis media incidence diminished, but gonorrhea became more frequent (McBride et al., 2020). A study in Taiwan declared their finding was consistent with the fact of increasing gonorrhea incidence too. It even explained their data may be underestimated since fear of COVID-19 transmission limits their access to hospitals (Lee et al., 2021). They explained their finding may be a consequence of the growing risk of unsafe sexual behaviors which occurred due to prolonged home residence (Lee et al., 2021).
Similar to our results and contrary to previous studies, in Switzerland and the United States, STIs including chlamydia and gonorrhea incidence have decreased due to the pandemic and its related containment measures (Crane et al., 2021; Steffen et al., 2020). This reduction is not necessarily interpreted as limited agent transmission and sometimes could be attributed to lesser visiting, testing, and reporting of STI cases like data identified by various outstanding undertaken investigations in South Africa, Belgium, Spain, and the United States. This phenomenon happening could be reasonable during the COVID-19 crisis, since the pandemic and its mitigation measures were able to interrupt sexual health accessibility (Bonett et al., 2021; Crane et al., 2021; De Baetselier et al., 2021; Dorrell et al., 2022; Maatouk et al., 2021; Martin-Ezquerra et al., 2021; Tao et al., 2021). Consistently, some evidence shows the reduction is mainly among urethritis patients with mild manifestations, and in a group of remarkable symptomatic participants, such a trend was not found (Berzkalns et al., 2021; Chow et al., 2021; Torres et al., 2021). Consequently, based on the mentioned theory, forward transmission prevention and controlling the STI epidemic are much affected by care services maintenance during disasters including the COVID-19 pandemic (Jenness et al., 2021; Yan et al., 2021).
We hypothesized that reduced urethritis incidences during the COVID-19 pandemic could be due to notably declined sex with non-steady partners in addition to having fewer opportunities for dating and sexing with anonymous. Although our findings described that more patients with urethritis report being single in 2020, probably single participants use a condom more often during the pandemic in comparison with patients having a regular partner (Gillespie et al., 2021).
Although Braunstein et al. reported STI patients’ characteristics mostly were similar in both pre and during-pandemic groups, we found out that the mean age of our patients during the first 6 months of the year 2020 was remarkably higher (Braunstein et al., 2021). Countless factors could be associated; to give an example a cross-sectional study demonstrated that the COVID-19 pandemic may have some adverse effects on the sexual behavior of couples below the age of 35 years old including declined sexual desire and less frequent intercourse (Shoar et al., 2020). A generation has a crucial impact on coping with stress (Fuchs et al., 2020). In addition, reports suggest that physical distancing and isolation of youths could put them in more risky situations by limiting their access to support services (Thomson-Glover et al., 2020).
This study is not without limitations. In addition to drawbacks related to the retrospective and cross-sectional study design, data are limited to the first semester of 2019 and 2020 and there is no information about a possible trend over time, even unrelated to pandemics. Also, urethritis laboratory testing is not available in our country, and as a result, urologists make diagnoses based on the patient’s clinical presentation which may limit the accuracy of our results.
Conclusions
Our study provides different aspects of urethritis in addition to its incidence changes in our country during the pandemic and prior. Its findings mainly demonstrated that the proportion of urethritis cases in all populations admitted to urologist offices had significantly diminished during the COVID-19 pandemic compared with the same period of 2020. Accordingly, the impact of COVID-19 on the urethritis trend is recommended to be investigated worldwide, and thus, various prompt measures should be undertaken based on the appropriate evidence. As well, the indirect effects of COVID-19 and its related actions on different aspects of sexual health state should be considered during pandemics carefully.
Footnotes
Acknowledgements
Special thanks to Sina hospital, Tehran University of Medical Sciences, Tehran, Iran.
Author Contributions
S.M.K.A. is the principal investigator who provides the data more than editing the manuscript, M.A.P. analyses the data, and A.R. wrote the manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval
Ethical approval was obtained from the Ethics Review Committee of Tehran University of Medical Sciences and the study approval number is IR.TUMS.SINA HOSPITAL.REC.1400.037.
Data Availability and Material
Information, data, and photos will be provided if requested.
