Abstract
Supported employment (SE) is an evidence-based program that has shown much promise in helping people with severe mental illnesses (SMIs) to gain and sustain competitive employment. However, there are significant variations in employment outcomes across SE programs in Canada that can be partly explained by SE service users’ experiences in their work environment. The work environment can exert a considerable influence on the interest in and ability to sustain the employment of a person with an SMI. This study explores the work experiences of individuals with SMIs who are involved in an SE program and who understand the challenges of and barriers to sustaining such employment. Semistructured, in-depth interviews were conducted with 15 individuals with SMIs, and the data were analyzed using a constructivist grounded theory approach. Challenges to the employment sustainability of an individual with SMI were found to arise primarily from three intersecting contexts: the SE program, the work environment, and the larger Canadian labor market. The findings suggest that SE programs will better promote employment sustainability if they adhere closely to individual placement and support model of SE. SE service providers (employment specialists) must be equipped with a wide range of knowledge and skills to meet the needs of individuals with SMIs if sustainable employment is to be achieved. It is recommended that there must be investment in training for employment specialists to assist SE service users to achieve sustainable employment outcomes.
Introduction
An accumulating body of research highlights the importance of employment in the recovery from severe mental illness (SMI). Employment not only provides income but also enhances mental well-being, facilitates community participation and social inclusion, and can be crucial in the development of a valued personal role in society and a social identity (Elraz, 2018; Krupa et al., 2009). There is evidence that many individuals with SMIs want to participate in some kind of remunerative employment (Kinn et al., 2014; McQuilken et al., 2003). In Canada, 70% to 90% of the individuals recovering from mental illness remain unemployed or underemployed; many are dependent on social assistance or on time limited allowances (Canadian Mental Health Association [CMHA], 2016). When an individual recovering from mental illness finds a place in the workforce, workplace conditions and experiences can trigger anxiety, interfering with his or her capacity to perform certain aspects of the work (Ebuenyi et al., 2019; Krupa et al., 2009; Woods et al., 2019). Employers’ apprehensions about hiring individuals who are recovering from mental illness and substance use disorders are often due to misguided fears about potential aggressive behaviors, absenteeism, a need for excessive supervision; employers’ worry that individuals who have experienced SMIs might find it difficult to follow instructions, and have a low ability (or desire) to socialize (Drebing et al., 2011; Krupa et al., 2009; Russinova et al., 2011).
In recent years, supported employment (SE) (service provisions wherein people with disabilities, including intellectual disabilities, mental health, and traumatic brain injury, among others, are assisted with obtaining and maintaining employment) has shown better success than traditional vocational programs in helping people with mental illness gain and sustain competitive employment (Drake & Bond, 2014; Drake et al., 2019). Traditional vocational programs essentially follow a “train-in-place” model and include prevocational training that places emphasis on extensive training and preparation prior to a return to competitive employment; this model may be appropriate for some individuals. However, traditional models place little urgency on commencing immediate competitive employment, thus delaying the positive effects of employment. The systematic meta-review by Modini et al. (2016) points out that such delay can add to a sense of exclusion from mainstream society in those who experience SMI. SE is an alternative approach based on a “place and train” model in which an individual is employed then supported with training to maintain this employment (Bond et al., 2016).
Individual placement and support (IPS) is a model of SE for people with serious mental illness. IPS programs are based on the philosophy that anyone is capable of gaining competitive employment, provided the right job and the appropriate support can be identified (Corbière et al., 2014, 2017). The IPS program has eight core principles: (a) eligibility is based on consumer choice (zero exclusion); (b) competitive employment is the goal; (c) work preferences are the focus; (d) the job search must be rapid; (e) SE and mental health treatment are integrated; (f) continuous and time-unlimited follow-along supports are provided; (g) benefits counseling is offered; and (h) systematic job development (a relationship with employers is cultivated to facilitate work integration) (Drake et al., 2012). The IPS model of SE has been applied successfully in many settings (Drake et al., 2019), and its effectiveness has been confirmed by more than two dozen trials conducted in numerous countries (Drake et al., 2016; Johnson-Kwochka et al., 2017; Killackey et al., 2019; Marshall et al., 2014). Employment specialists (ESs) play a key role in SE programs. They coordinate all steps in the vocational process and are expected to develop cooperative relationships with employers (Corbière et al., 2017; Glover & Frounfelker, 2011).
Despite the success of SE for people with SMIs, approximately one-third of SE participants either do not gain employment or they experience limited job tenure, and they fail to achieve long-term career goals. In part, this reflects the absence of quality standards for SE (Corbière et al., 2005; Bond et al., 2011, 2012). Other reasons for the limited job tenure of people with SMIs include insufficient training of (or a lack of competency in) the ESs (Corbière et al., 2017). In Canada, there is considerable heterogeneity in SE programs and the outcomes are variable. In Canada, IPS programs vary in their fidelity to the reference model, and tend to coexist with other SE modalities (Corbière et al., 2014). While organizational and contextual factors—institutional pressures, values, and ideologies—are responsible for the diversity in SE programs (Menear et al., 2011), the variation in employment outcomes across SE programs can be explained by the support provided by the SE program, the SE service user’s experience of the workplace environment and the work arrangements, and the current labor market conditions that can promote precarious employment (Carter et al., 2013; Dollard & Bakker, 2010; Inoue et al., 2010; Lippel et al., 2017). Precarious employment is a cumulative combination of atypical employment contracts, limited social benefits, poor statutory entitlements, job insecurity, short tenure, and low wages. Precarious employment includes exposure to stressful and hazardous work environments, increased workloads, repetitive work, high worker turnover, and jobs that offer little scope for career progression or benefits (Clumeck et al., 2009; Lewchuk et al., 2015).
Since the emergence of SE for people with SMIs, researchers and practitioners have invested significant efforts to improve the interpersonal work environment for people with SMIs through programs that increase the mental health literacy of employers and reduce discrimination toward these employees. There is now a growing number of educational resources, ranging from online webinars and modules to in-person training, that teach methods to increase psychological health and safety in the workplace (CMHA, 2016). The workplace arrangement, the organization of the work, and the content of work each has a significant influence on mental health and can empower or disable people with mental illness (Mik-Meyer, 2016). Accordingly, this study explores the work experiences of SE service users with a view to determining what interventions can promote their mental well-being and improve their job tenure.
Research Questions
The research questions are as follows: (a) What challenges do individuals with SMIs who are enrolled in an SE program face in the workplace? (2) How do these challenges pose a barrier to employment sustainability? (3) How do individuals with SMIs perceive the roles of employers, coworkers, and ESs in relation to the challenges that they face in sustaining employment?
This exploratory study is not aligned with any conceptual framework. However, we draw from the social model of disability and the social determinants of health theory to contextualize the experiences of SE service users with SMIs. The social model of disability adopts a “social barriers” view. This view proposes that it is societies and social systems that “disable” individuals who have SMIs but who want to work. The social model of disability separates the psychological variations (designated their “impairment”) by which a person with an SMI differs from most other persons from their “disability,” and considers their “disability” to be the “contextual factor that mediates the experience of impairment” (Foster, 2018, p. 191), including the social consequences of being labeled as disabled. Studies framed around the social model of disability have examined “how brutal workplace practices can be towards people with mental illness related impairments and how workplace practices and policies targeting these individuals can disable rather than assist or empower them” (Mik-Meyer, 2016, p. 986). Despite the success of programs like IPS, many people with SMIs do not have access to such programs because of several factors. Many communities do not have funding for programs like IPS. SE services require resources for training SE service providers, and such resources are scarce. Finally, there is a lack of political will on the part of decision makers to improve employment outcomes for people with mental illness.
Methods
This study employed a qualitative design informed by a constructivist grounded theory approach to explore, understand, and explain the work experiences of individuals with SMIs who were enrolled in an SE program. Constructivist grounded theory positions the researcher as a co-author in the (re)construction, interpretation, and representation of knowledge, experiences, and meanings, while retaining participants’ own words and stories in written representations (Charmaz, 2014; Mills et al., 2006). A constructivist grounded theory approach is relevant for this study because it enables the researchers to co-construct participants’ stories of workplace participation and workplace challenges based on their subjective experiences. Constructivist grounded theory considers the researchers’ interpretive frames and prior experiences associated with the phenomenon being studied (Charmaz, 2008, 2014; Mills et al., 2006). Constructivist grounded theory has been used in previous studies of workplace experiences that included individuals with SMIs (Gaffney et al., 2012; Krupa et al., 2009; Martin & Barnard, 2013), and has been an effective approach to examine the challenges and strategies directed at workplace integration, worker motivation, and staff retention.
Participant Recruitment and Data Collection
Participants in this study were SE service users of a mental health service provider in a Canadian city in the province of Alberta. In Alberta, the ratio of the number of people reporting mental illness/the number of SE program sites is higher than that ratio in other provinces (Mental Health Commission of Canada, 2016). In Alberta there are 11,452 persons per SE site, whereas in Nova Scotia, there are only 6,178 persons per SE site. Little research has been undertaken in Alberta to examine the experiences of SE service users with SMIs (Mental Health Commission of Canada, 2016).
The mental health service provider in Alberta has a Wellness Recovery program that offers SE for people with SMIs who want to return to work. The ESs in the program reported that they work closely with SE service users and liaise with their treatment providers as needed. ESs also collaborate with disability employment services in the community and refer SE service users to these disability employment services to get information on available jobs and services. Group programs are offered on a regular basis. These programs focus on areas like interview skills development, appropriate work behaviors, how to deal with workplace challenges, and how to seek support from supervisors. SE service users are also counseled regarding the benefits and limitations of disclosure to employers. ESs often accompany SE service users to job interviews and provide one-to-one support after the SE service user gains employment.
The purpose of this study was widely disseminated to SE service users by service providers at Wellness Recovery Services during 2013. Service providers at Wellness Recovery Services referred individuals interested in participating in the study to the first author. The sampling for this study was purposive, as only those who were enrolled in the SE program were interviewed. The sample size was determined by the principles of theoretical saturation and maximum variation (Coyne, 1997); that is, the sampling continued as long as new concepts continued to emerge. Fifteen SE service users participated in the study. Interviews were conducted during 2013 to 2015 by the author and a trained research assistant who had considerable experience with people experiencing mental illness. Data were collected using face-to-face, semistructured interviews of 1.5 to 2.0 hours. The interviews collected information about the kinds of jobs participants had held while enrolled in the program, their work experiences, the challenges they faced, their reasons for leaving their job, the kinds of employment support they received versus what they had expected, the best and worst workplaces, and the additional supports they needed to stay in the workforce. With the informed written consent of the participants, the interviews were audio-taped and transcribed verbatim for coding and analysis. Interviews commenced only after receiving ethics approval from the University of Calgary Ethics Board.
Data Analysis and Rigor
Data were analyzed using the constant comparative approach. It involved studying the data on a case-by-case basis, coding the data, analyzing the data across participants (in comparison), and collapsing the initial codes into “categories of meaning” that represented themes (Charmaz, 2008). An initial coding framework was established based on the transcripts of the first few interviews. The authors conducted independent coding of the interviews. The resulting codes were compared to ensure that intercoder reliability was achieved and maintained. Rigor of the study was established by the following strategies: maintaining an audit trail of the research process, using data saturation, using intercoder reliability, and peer debriefing. Several illustrative excerpts were used throughout the analysis to add strength and authenticity to the analysis.
Results
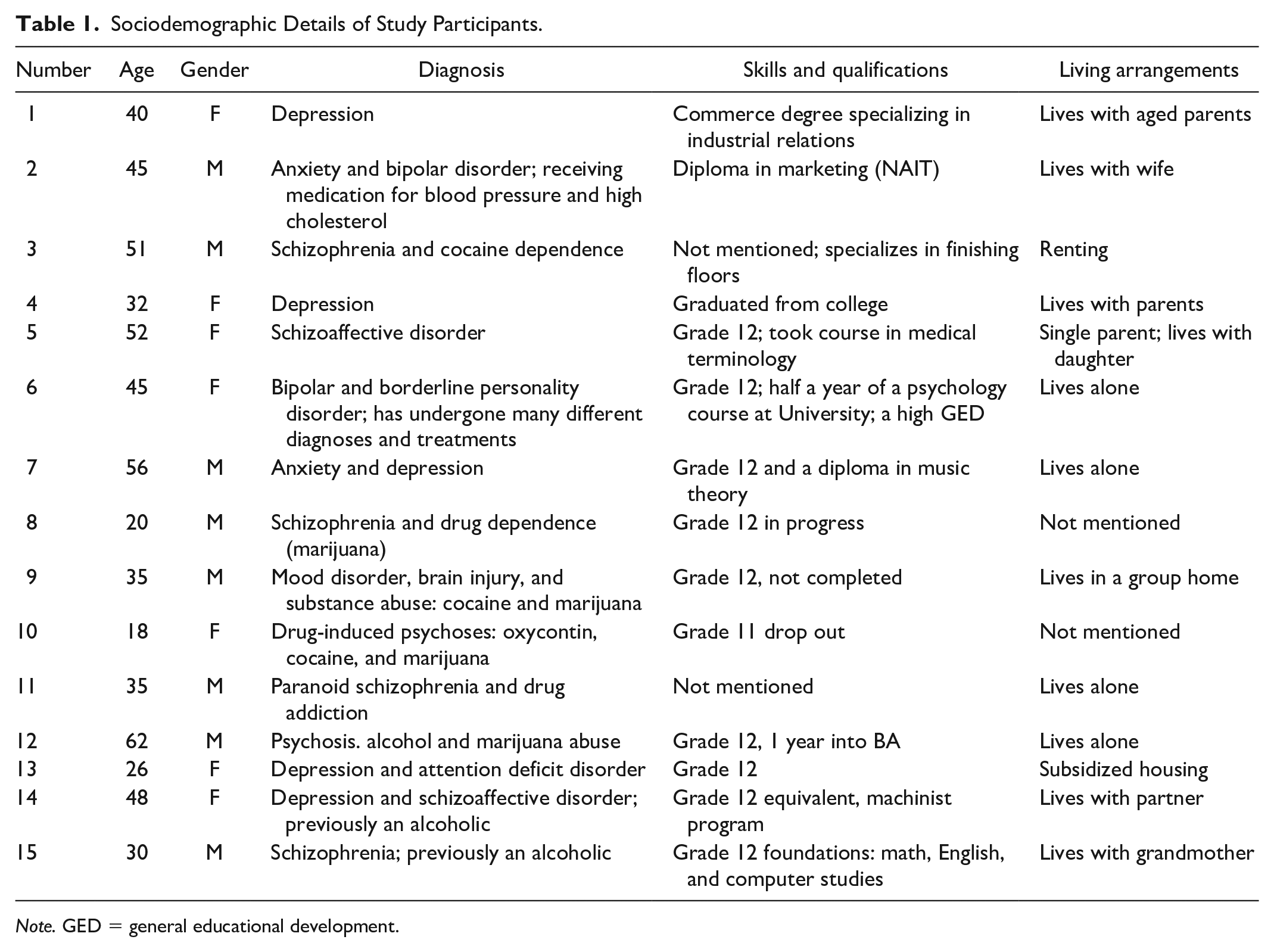
Sociodemographic Details of Study Participants
Sociodemographic details of the 15 study participants are presented in Table 1. Six participants had a co-occurring substance use disorder. At the time of the interviews, the participants had been enrolled in the SE program for periods ranging from 6 months to two and half years. Only seven participants were working at the time of the interview; they were all in part-time, casual employment. Participants’ jobs included security assistant, janitor, cashier, customer service assistant, food preparation assistant, landscaper, and factory hand. The other eight participants were in different phases of job seeking; for examples, working on resumes, undergoing interview skills training, and attending interviews. At least five participants had experienced job loss while they were in the SE program. All the participants had work experience before they entered the SE program, though the length and nature of their experiences varied. Some participants had not worked in many years while others had experienced periods of employment and periods of unemployment. All the participants in the study were Canadian born and had Caucasian or European ancestry. Each of the seven participants who were working at the time of the study interview had disclosed a mental health-related disability to their employer. In addition to mental illness and substance abuse, some participants experienced high blood pressure, poor eye conditions, irregular sleeping patterns, and lack of rest. The most frequently mentioned reasons for job loss reported by participants were illness related. Some participants had experienced an increase in symptoms that interfered with their capacity to fulfill their duties and either left their employment or their employment was terminated. Some participants mentioned their noncompliance with medication as a reason for a loss of employment. Despite these challenges and past experiences, all the participants were keen and motivated to gain and sustain employment.
Sociodemographic Details of Study Participants.
Data Analysis
In the following sections, we discuss six themes related to the work experiences of the participants.
Strategies to sustain employment
Participants identified several strategies that were used to sustain employment. They had learned these strategies through personal experiences and through the SE group programs. These strategies included demonstrating appropriate work behaviors, managing illness at work, seeking support from supervisors, and accessing support from family members, friends, and significant others. Many participants mentioned the importance of developing and demonstrating a positive attitude toward work. One participant described a positive attitude as: Better attendance, more dedication to my job, show a little more interest in the people I work with, and that’s about it. Well, I mean not take days off because you’re tired, or days off because you’re uncomfortable, something like that. That really shows dedication to your job and some interest in the people you’re working with, some interest in the product or the service that your company or department sells or does business with; show an interest, show an interest and dedication toward your job.
Participants mentioned factors like understanding the employer’s/supervisor’s expectations, keeping occupied, and “always asking for more tasks to keep busy” as important strategies for sustaining employment. One participant highlighted the importance of appearance and had spent money on buying herself good clothes and having an attractive haircut after getting a job. Many participants had made positive efforts to get to know their coworkers and to work collegially with them. One participant, who was currently working and who had experienced negative experiences with coworkers in previous jobs, shared what he had learned: I heard one time 80% of your job is your effectiveness with people you’ve got to work with and that you’re actual doing the job counts only for 20% of your effort. Trying to deal with employers and supervisors and colleagues can weigh very heavily on you sometimes—you’ve got to go with the flow, even if you feel something’s wrong or being done wrong, or something’s been said that you take exception to, you can’t, you can’t fly off the handle and you’ve got to roll with the punch a lot I find.
In the context of establishing a good rapport with job supervisors, some participants highlighted the importance of disclosure. They felt that disclosure of their mental health–related disability to the supervisor in advance could be beneficial, as it would be easier to negotiate work duties and hours and reduce the stress of “hiding” their illnesses. In addition, participants felt that the disclosure of a mental health–related disability could minimize the risk of slips in their work behaviors being viewed as performance issues. One participant, who had negotiated a reasonable accommodation with his supervisor, said: I think it’s good to have a rapport with your supervisor and be able to discuss openly your situation with that person, and lots of times a person is more productive in the workplace instead of working, say, 4 days a week, and not being productive because they’re stressed, they may be a lot more productive and get more work actually done in 3 days because they’re not under stress, and if you mutually agree upon with the supervisor to only work 3 days instead of 4 days. You may get more done.
Participants who were currently working said that managing their illness at work by taking prescribed medications was crucial for maintaining employment. Medication helped to control the disease symptoms and that gave them confidence. A participant who used self-talk as a strategy said, I’ll take some Xanax and then when I get to work, I get things done and you know time goes by. I say to myself ‘fight or flight’ . . . I say that a lot, to myself, when I’m feeling down.
Another participant whose work involved dealing with difficult/angry customers shared his experience: Customers would ask me if I’m okay and I would tell them no, give me a minute or two, or I’ll just walk away and say I’ll be right back and walk away and just try to calm down, but a lot of time the customers are yelling at me and it’s like, okay, it’s like, I couldn’t do anything so as soon as the customer left I would take a break.
Other helpful strategies mentioned by participants included following a healthy lifestyle by giving up alcohol, taking good rest, and being aware of one’s limitations. In the following excerpt, one participant summarized the importance of knowing one’s own limitations: As a person with mental illness I need to understand my mental illness, I need to know what my capabilities are, I need to know what my limitations are in the job I’m in; I need to know that if I feel that 4 days a week is just too stressful for me that I should only take 2 or 3, not try to do the 4 day a week sort of thing because that affects, that affects my mental health if I’m under stress. So, in order to balance my mental health and my work, I have to know how much I can handle and what I think my limits and limitations are.
Several participants reported that the support they received from close family members and friends helped them to stay in employment. They shared that having this support made them feel that people cared about them and had positive expectations of them. This provided the motivation to stay healthy and be successful at work. One participant noted: Support such as positive, positive people in your life, whether that be family, or friends, positive people who like I have this little kind of team behind me that I know all want me to succeed and it’s comforting and it makes me feel that even if it doesn’t work out then we tried to do it.
Participants held to different standards: Experiences with employers
Participants recounted both positive and negative workplace experiences. All the participants emphasized that positive employer/supervisor attitudes toward people with mental illness are critical for maintaining the employment of such individuals. Participants expressed that employers who hire workers with mental illness must have some understanding of the needs of these workers and the kinds of challenges they face in the workplace. Such employers must be empathic, willing to communicate, and able to provide relevant and timely support. One participant appreciated that her supervisor did not treat her like a “second-class citizen” or see her as a “person with mental problems.” Participants felt proud when their employer showed trust and confidence in them and entrusted them with responsibility.
It’s very, it’s very receptive, we’re treated with respect which on other jobs you just don’t get respect, that’s a big part of it. I mean you’re not treated like you’re a second class citizen or there’s something wrong with you or you can’t achieve this or you can’t do this or you can’t do that because you’re mentally ill, or we don’t want to give you responsibility because maybe something’s going to happen and you can’t handle responsibility. It’s not like that in my present job.
Another participant appreciated her supervisor’s patience with her while she was learning the job. The supervisor was not angry or rude when she made mistakes, and taught her the right ways to do the job. A few participants expressed how elated and motivated they felt when their employers were friendly, when they provided regular feedback on the work performance, when they accepted them with their limitations and treated them as an integral part of the work team.
However, participants also recounted negative experiences, many related to unfair dismissals and terminations. One participant shared her feelings of frustration and powerlessness when she was terminated by her supervisor just because she had a mental illness (which she had disclosed when she was hired), although her illness had in no way affected her work performance. In another case, a participant was dismissed by her immediate supervisor, even though she had disclosed her illness to the manager. She explained: She never told me until I approached her, and she said, “well, it’s because we think this job’s too stressful for you.” And I know for sure she knew that I had a mental illness because I had discussed it with the manager, and he said that he would tell the supervisor what the conditions of the employment were.
In another case, the participant had noticed that she was always assigned harder jobs than her coworkers, and when she did not perform well, she was “fired for poor performance.” Other reasons that prompted participants to quit their jobs included: unreasonable demands from supervisors, long working hours, a physical injury sustained at work, a toxic interpersonal work environment, a contract not being renewed, the closing of a factory or supermarket, the job being a seasonal position. Some participants believed that they were not hired into permanent positions because their employers perceived that they did not have the skill set or the capacity to do the job.
Participants recounted many experiences in which their employers/supervisors were rude or sarcastic, did not communicate well, and held them to standards different from other employees because of the illness. Examples of participants’ negative experiences with employers/supervisors are described below.
Employer was rude and sarcastic: We didn’t talk much unless we had to, he had a very snide attitude, it was hard to take, sarcastic at times and as I said before you have to roll with the punches sometimes and, it was really bad sometimes when you’re there and you’re struggling with something and they’ve got something to say about it, it’s none of their business, or they can’t appreciate the difficulty that you’re having—I’ve had that happen and you know there’s not much you can do about it. Employees with mental illness were assigned jobs that were mundane and that lacked creativity: They don’t give you feedback, they don’t give you the challenging jobs, they restrict your job to the easy stuff and the stuff they think you can handle. I think easy stuff is more stuff that is sort of routine and then more mundane and more routine, like folding clothes or stocking shelves or, you know, running a printing press—was pretty mundane—just keeping it functioning. I think that challenging jobs would be like anything that involved creativity or any personal judgment—things of that nature. Supervisor did not want to communicate directly with employee with mental illness: Well, at X (a large grocery store) I had a boss who, I admit, she bugged me when she would go to somebody else and that person would come to me if she had a problem. I think it was a supervisor that she went to. Well, I always thought, it’s like if you have a problem with me come to say it to my face, not go and get somebody else’s boss. Supervisor “yelled” at employee with mental illness: Well, a lot of the time it’s the people. I used to work at a warehouse, I hated that job, it was the worst job I ever had, it was because of my supervisor, getting yelled at all day long, you know, stop for two seconds and then he’d come along and yell at me and so, yeah, I think that’s another place, too, where the depression started to, to come on a little bit, just because it was the same thing every day, day in, day out.
One participant mentioned that her employer never offered her a full-time position because this would mean giving her access to benefits, like a pension. Another participant shared that she was never promoted or given a raise in salary despite working in the organization for many years. These participants felt exploited and taken advantage of because of their illnesses. One participant noted: “I really worked hard but I never got credit from the boss for all the labor, he never even gave me a hint of a raise and he just abused all the labor that I was putting in there.” Participants also observed that some supervisors did not care about workers with special needs and were only interested in getting the work done so “they don’t get any flak from the higher authority.” Such negative attitudes and behaviors from employers/supervisors was an impediment to learning, and created additional stress for the participant quoted below: The pressure from supervisors is probably my biggest, biggest handicap I have in getting work done. Lack of patience from supervisors, to understand that it takes time to learn certain things, certain skills. Even if you’ve done school you should know the pieces, but in school they don’t teach you how to be a master machinist in 9 months, it takes years and years, you know.
Not feeling included: Experiences with coworkers
Participants also had expectations from their coworkers. They wanted to feel accepted by coworkers and to be treated with respect and trust. Participants who had worked (or were working) in settings like fast food restaurants, appreciated the way their coworkers interacted with them and made them feel included and accepted. As a result, they experienced a high level of integration with the workplace and with the work team. Other workplaces were not as inclusive and accepting. Participants felt socially excluded and isolated when coworkers had “their own circle, would gather for a meal, smoke, and spend time chatting with one another.” Some participants experienced feelings of isolation even after several weeks at the workplace, and often worked alone and spent their breaks alone. One participant remembered that when he was new in the job, his working partner was too busy to answer his questions. Some coworkers showed impatience with the inexperienced worker and sometimes even joked at his or her expense. A participant who worked in a supermarket said that it was hard to communicate with his coworkers because they were immigrants and had limited English language skills. Some participants had experienced coworkers becoming uncomfortable, uptight, and discriminating when they found out that their coworker had a mental illness, as illustrated in the following excerpts: It’s like, it’s hard to say, it’s kind of unspoken, it’s like they’re uptight around you or something, you know, they don’t approach you openly and they all talk to the other staff behind your back. I never really faced that until this year, and it was like people look at me funny and don’t want anything to do with me, so I was kind of like left on my own to do stuff. It’s like, it’s hard to describe, it’s like, oh you’re one of those that hurt people like the stories that you hear on the news, if they are depressed they’ll go out and kill people and then kill themselves, kind of . . .
Positive and negative workplaces and the “good fit job.”
Positive workplaces
Participants described positive work-settings as places where the work environment encourages creativity, interaction, independence, provides good accommodations to workers with mental illness, and where it is enjoyable to work. One participant who worked in a care center said that although her job is demanding and involved a lot of paperwork, she enjoys the intensity and enjoys taking care of people. Another participant enjoyed the busy morning shift in a bakery. For some participants the ability to finish tasks independently and be part of a team was important. For example, a participant who works in a retail store explained that in her workplace, employees were required to work together or to work independently, depending on the task at hand. Another participant expressed that he likes his job because the workplace is close to his home, he can walk to the workplace, which is a regular exercise for him.
Negative workplaces
Participants agreed that negative workplaces are those in which there is high staff turnover, the job is repetitive, there is no job security, and there is a lack of training for new employees. The supermarket was an example of a negative workplace because of the high staff turnover that made it difficult for participants to develop and maintain stable long-term relationships and feel a sense of belonging. Other examples of negative workplaces included workplaces where participants had received no job-related training, where their supervisor was never available to show them how to do the job, and where their job duties were not clearly outlined. In such workplaces, participants described feeling confused and frustrated because their supervisor wanted them to do lots of different things and gave confusing instructions on how to perform the tasks. Another example of a negative workplace was given by a participant who was supposed to have a job evaluation after certain time, but she never got it (lack of feedback).
The “good fit job.”
In the context of discussing their expectations from employers and coworkers and positive and negative workplaces, many participants alluded to the importance of finding the right kind of work and work-setting, which one participant referred to as the “good fit job.” Perceptions of “good fit jobs” varied among participants. For some participants finding a good fit job meant knowing before being hired the expectations and challenges that might be encountered.
Just that person with mental health issues might need to know everything before they start, that would be good, if you know somebody has a mental health issue it might make it less stressful if they know exactly what’s expected of them, they know how to do the job.
To some participants, a good fit job meant liking what they did and “not getting stuck in a job.” For others a good fit job meant a job in which they are active and not sitting for long periods of time. Some participants wanted jobs that allowed a lot of interaction with other people at work, while others preferred work that involved minimal interaction with others. One participant said she had been “a people person,” but after being diagnosed with mental illness, she does not like to work with many people. Another participant admitted that she has low tolerance for some people, particularly “difficult customers who have lots of questions and issues.” A few participants expressed that not having too much contact with coworkers had its benefits because they would not have to deal with the stress involved in the event of getting hurt. In this context, one participant shared that feelings of isolation were easier to cope with than stressful relationships. For these participants a good fit job meant being able to work independently with minimum contact with coworkers or customers. Other aspects of the good fit job included skilled jobs with multiple tasks, jobs that called for attention to detail, limited repetitive work, working with peers rather than younger people, jobs involving limited digital technology, and jobs that did not require much physical labor, like lifting, and did not involve long working hours. Some participants said that working during some seasons, for example during the Christmas season, was stressful and overwhelming, as it involved much heavier work, long working hours, and dealing with a lot of different customers.
Dealing with feelings and emotions
Due to poor work experience, many participants experienced feelings of self-doubt about their competence after being hired. Some participants felt inadequate when they compared themselves with coworkers who were more educated and skilled. One participant added: Another part is performance anxiety, you wonder if you’re good enough at what you’re doing. Am I really, really good? That, messes with your self-esteem and motivation, and a lot of things; so, there’s a lot of factors that come into play there: you’re struggling, you have a job to do—that’s minor; the feelings that you have to deal with is the heart burn.
Several participants had to grapple with maintaining motivation. These participants experienced loss of motivation when their supervisors failed to acknowledge their work and instead goaded them to work harder/faster, as illustrated in the following excerpt: He wasn’t motivating me to go to work, he was just using, sapping out my energy. After all those tasks that I had to do I just couldn’t make it in that day. I had to come up with another excuse, and why should I have to give him any excuse anyway? It’s not that I didn’t want to work for the guy, but he was trying to embroil me under a situation that was just sapping me of my energy and forced me to go to work, and that’s why we came to a confrontation.
Other participants experienced loss of motivation when they were faced with the stigma of the illness, had to deal with abusive coworkers, or heard negative comments about their physical appearance. Participants all agreed that having a person they could trust—a family member, a friend, a service provider—to talk with about their feelings, could help them cope with stressful work environments.
Participants’ expectations of ESs
Most participants valued the job skills training and coaching they had received from their ESs, including the workshops/group sessions, and the first aid training. They welcomed the seminars that explained how to discuss their disability with the employer in a professional manner during the interview, and how to manage stress in the workplace. Many participants appreciated the efforts of their ESs (accessible by phone) who helped to allay self-doubts and provided guidance if they asked for it. For many participants, the SE program had provided an opportunity to make friends with people who experienced similar problems. Yet, many participants felt that the SE program was not individually tailored to meet their specific needs. Some participants did not like having to work with several ESs. For example: I didn’t want to go from one person to another. I dealt with one person today, next week I would deal with somebody different, so I’d have to start all over again. It’s like if I dealt with this lady for resumes and I had an appointment to go over interview skills, I’d have to start from square one with the new lady. Not necessarily doing up my resume, but just going over my job experiences, how I felt, what I was looking for, that stuff.
Participants who had lost their jobs because of an illness relapse felt that there must be more collaboration among the different SE service providers, especially treatment providers and ESs. According to one participant: I wasn’t scared, it was just frustration, and I was also thinking, it’s like, can’t you guys (ES and mental health treatment provider) get together and talk? It’s like, I even said I saw such and such person, like, couldn’t you talk to them before you saw me?
Three participants expressed that they would have sustained their jobs if their employer had contacted the ES when it was noticed that their work performance was declining. They also did not recall any instance in which their ES had contacted their employer/supervisor and tried to prevent job loss. Thus, it was the participant’s responsibility to recognize when his or her work performance was declining and to seek support from the employer or the ES. This can be difficult to accomplish for many SE service users with SMI, who are in the early stages of becoming ill and are already under considerable stress.
Other intersecting challenges
Participants noted that despite their employment, they were unable to make ends meet because of the expenses of maintaining a car, paying rent, and having to invest in clothes and shoes. To minimize transportation costs and in some cases due to an inability to drive because of medical conditions, many participants wanted jobs that were situated a short distance from where they lived. Some participants wanted to take on more hours of work but feared that doing so would affect their benefits and their eligibility for income support that they received from the government, a situation called the “welfare trap.” One participant explained: No, I don’t want to (take on more hours). It’s hard to be in the situation where I’m going to lose my benefits, because I’m doing so well, but I have bills to pay, you know, I have a condominium to pay for.
Losing the pension could involve going through the cumbersome procedures of reapplying and appeals, and many participants were aware of these.
Discussion
This study adds to a growing body of knowledge about the work experiences of SE service users who have SMIs and who participate in SE programs to gain and sustain employment. The findings of this study highlight the challenges to employment sustainability that many participants faced. Figure 1 provides a visual representation of facilitators of and challenges to employment sustainability that are experienced by the participants in this study. In keeping with the social model of disability, the challenges to employment sustainability for people with SMIs can arise from several intersecting contextual factors. Based on the findings of this study, we discuss three of these intersecting factors—the SE program, the work environments for people with SMIs, and the Canadian labor market.

Challenges to and facilitators of employment sustainability for supported employment service users with mental illnesses.
The first contextual factor is the SE program that participants with SMI were enrolled in. Although the SE program helped many participants to gain employment, our interviews with participants with SMIs who have participated in the SE program raise the possibility that the SE program did not meet the standard—that is, the IPS model—for the placement and support of individuals in work situations using evidence-based SE (Drake et al., 2016) for a number of reasons: (a) the close collaboration and teamwork between the SE service providers and the mental health treatment team, which is a core feature of IPS (Drake & Bond, 2014; Drake et al., 2019) was not evident from our interviews with participants; (b) although the SE program provided participants with resources for gaining employment, our interviews with participants suggest that the program lacked an individually tailored approach, in which the focus of the ES is on helping the SE service user find the best job fit; (c) unlike the IPS model, in which there is a strong emphasis on cultivating relationships with employers to facilitate work integration and to provide continuous and time-unlimited follow-along supports (Drake et al., 2019), this SE program placed more emphasis on assisting participants to gain employment than on cultivating relationships with employers. Follow-along support was limited to individual counseling (provided by ESs) on job-related concerns. For some participants, job loss and the suffering associated with job loss, were the ultimate results of this limited SE effort.
A second contextual factor that posed challenges to employment sustainability for an individual with an SMI was the work environment, specifically, the employer’s level of commitment and the employer’s capacity to accommodate the needs and expectations of a worker who had a disclosed disability. Table 2 provides a list of the expectations that participants in this study had when they joined a workplace. The findings highlight that despite the disclosure of a disability, many participants experienced discrimination from their employers/supervisors, were held to standards different from other workers in terms of the jobs that were assigned to them, and were not considered for benefits, promotion, or permanency. These findings are supported by previous studies (Houtenville & Kalargyrou, 2015; Ju et al., 2013). The findings here suggest that employers/supervisors were either uninformed about participants’ specific needs, or did not know how to address and accommodate these needs. Research has shown that employers who have ongoing contacts with SE service providers are more willing and more able to meet the expectations and needs of SE service users with mental illnesses (Corbière et al., 2014; Glover & Frounfelker, 2011; Shankar et al., 2014).
Participants’ Expectations of Employers/Supervisors and Coworkers and Participants’ Perspectives on Positive and Negative Workplaces.

MI = mental illness.
The third contextual factor that could impact employment sustainability is the Canadian labor market, which has been experiencing a rapid increase in precarious employment in recent years (Lewchuk et al., 2015). Many of the characteristics of precarious employment—stressful work environments, repetitive work, poor job security, high worker turnover, and jobs that offer little scope for career progression or benefits—are reflected in the work experiences of the participants of this study. The results of the study suggest that many of the work experiences of participants are related to the fact that they have a mental health disability. However, lack of job security and not being considered for a permanent position could be due to uncertainties in the current labor market. An increasing number of workers are working on short-term contracts and lack supplementary benefits or pension plans (Kalleberg, 2011; Lippel et al., 2017). The methods employed in this study do not permit us to infer that participants’ experiences are related to a mental illness diagnosis. Participants’ perceptions of employers and experiences in the workplace are described in Table 2.
Based on the findings of this study, in the following section, we discuss some useful employment sustainability interventions and propose ways to improve employment sustainability for SE service users with SMIs.
Employment as a Mental Health Outcome: Investing in Evidence-Based SE and Capacity Building for SE Service Providers
The findings of this study argue for increased investment by health care systems in SE programs that closely follow the standardized SE IPS model. SE programs that do not have high fidelity with the standardized IPS model often achieve narrowly set employment outcome targets based on the number of SE service users with SMIs who gain employment. But SE service users in such programs might not sustain employment because supports—like individualized on-the-job support, and close collaboration between treatment and SE services are inadequate or unavailable. The findings of our study indicate that SE service users may drop out of employment, lose motivation, and blame themselves for their loss of employment. Each of these actions can have a negative impact on the mental health and well-being of the SE service user (Moscone et al., 2016). Such outcomes feed societal discourses that propose that people with SMIs are poor candidates for employment. On the contrary, SE programs that follow the IPS model can encourage health care decision makers and program managers to recognize that a “return to employment” is an important mental health outcome for people with SMIs, and accordingly allocate resources. Previous studies have shown that evidence-based SE programs contribute to reduced hospitalizations and produce a high social return on investment (Hoffmann et al., 2014).
An increased investment in SE services calls for resources that can build the capacity of the ESs and mental illness treatment providers who play key roles in the success of SE programs. ESs who have the knowledge and skills (Corbière et al., 2017; Glover & Frounfelker, 2011) to assess both short- and long-term work-related needs of SE service users can be recruited to proactively network and build relationships with employers at different levels. Whitley et al. (2009) presented eight self-identified characteristics of successful employment practitioners: initiative, outreach, persistence, hardiness, empathy, passion, professionalism, and team orientation. ESs must receive training to deal with complex issues and crises that might arise, like “job in jeopardy.” They must work closely with treatment providers and reach out to family members and other stake holders to minimize the risk of a relapse in an individual with SMI.
The findings of this study suggest that ESs must be aware of the current labor market and the risks, challenges, and limitations associated with various jobs and work-settings. ESs must be proactive in assisting SE service users to negotiate with employers about job expectations and duties. SE service users need to receive on-the-job training and mentorship, training in safety aspects of the job, and information regarding their rights and responsibilities. Since the risk of job loss/termination can be high in current work environments, regular contact with employers and follow-on support is vital and must be ongoing. In view of the wide range of skills required by ESs, some scholars recommend splitting their role into two roles, with some ESs focusing on the securing of employment and others focusing on employment retention, as these functions require different skill sets (Taskila et al., 2014). However, this would not be consistent with the IPS model generating discontinuity in SE services. Another approach might be to raise the pay level of ESs in recognition of the rare combination of skills needed to excel at this kind of work.
Supporting employers/supervisors
Research shows that employers who have good mental health literacy, who have had previous experience with people with SMIs, or who have personal experience of mental illness are more willing to hire people with mental illness than those who lack this literacy or experience (Ju et al., 2013; Shankar et al., 2014). However, their decision to hire and support these workers will be influenced by the resources they have at hand and are able to access, their time pressures and productivity demands, and the quality of support they received in previous experiences (Shankar et al., 2014). A growing number of online and in-person educational resources designed to increase the mental health literacy of employers are now available; however, there is little information on the extent to which these resources are being used by employers and supervisors. Even if employers have mental health literacy, they often have apprehensions about how to support employees with SMIs while balancing the pressures and demands of their businesses. The support of an employee with an SMI calls for sensitivity and skills. The employer of an individual with an SMI must know how to communicate with the employee, must recognize the signs of declining performance, must deal appropriately with behavior and performance issues, and must provide timely feedback and reasonable work accommodations when needed. The ES must be available to the employer/supervisor to build their capacity to develop these skills, and to help them when problems arise.
Conclusion
This study examined the work experiences of a sample of SE service users with SMIs who were enrolled in an SE program in a Canadian city in the province of Alberta. This study has limitations, but the findings are significant. The findings cannot be generalized because they are based on the experiences of SE service users in one program in Canada. The interviews provided rich information on the work experiences of participants and their expectations from work supervisors and environments. This can help SE providers and other mental health service providers understand the “real” challenges and barriers in the workplace as well the services gaps and knowledge deficits in mental health and vocational services. The findings suggest that supporting SE programs to achieve high fidelity to the IPS model would improve employment sustainability. There must be investment in training for ESs to assist SE service users to achieve sustainable employment outcomes. This training must equip ESs with knowledge about the current labor market, the kind of jobs available, and the risks and limitations of these jobs. Such knowledge will enable them to build alliances with diverse employers. Future research must examine the experiences and expectations of ESs, program managers, and employers to improve the employment sustainability for SE service users with SMIs who participate in SE programs.
Footnotes
Acknowledgements
The authors wish to thank all those who gave their valuable time to participate in this study.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study received part funding from Alberta Mental Health and Addiction Services.
Ethical Approval
This study received ethics approval from the University of Calgary Ethics Approval Board (approval id. REB 3174).
