Abstract
Complementary and alternative medicine has been shown to be beneficial in reducing chemotherapy-induced nausea and vomiting. However, conclusive results are lacking in order to confirm its usefulness. The purpose of this study was to determine whether a standardized yoga intervention could reduce these adverse symptoms. This was a partially randomized and blinded controlled trial comparing a standardized yoga intervention with standard care. Eligible patients were adults diagnosed with stages I to III breast cancer receiving chemotherapy. Patients randomized to the experimental group participated in an 8-week yoga program. There was no significant difference between the experimental and control groups on chemotherapy-induced nausea and vomiting after 8 weeks. Results suggest the yoga program is not beneficial in managing these adverse symptoms. However, considering preliminary evidence suggesting yoga’s beneficial impact in cancer symptom management, methodological limitations should be explored and additional studies should be conducted.
Worldwide, breast cancer is the second most common cancer diagnosed excluding non-melanoma skin cancer. 1 In 2015, it was estimated that 25 500 Canadian women will receive a breast cancer diagnosis. 2 Chemotherapy is commonly offered to early stage, high recurrent risk, locally advanced, or recurrent breast cancer patients. 2 Despite improved oncological treatments and survival rates, this diagnosis is still associated with adverse symptoms linked to chemotherapy. 3,4 In fact, research reveals a plethora of psychological symptoms (emotional distress, impaired quality of life, anxiety, depression) and physical ailments (pain, fatigue, dry mouth, insomnia, nausea, vomiting) occurring at a prevalent rate. 5,6
Chemotherapy-induced nausea and vomiting remain 2 of the most distressing side effects experienced by cancer patients. 7,8 In fact, studies report the prevalence of these adverse symptoms ranges from 13% to 75%. 9 Consequently, they can lead to poorer chemotherapy adherence, diminished quality of life, increased depression and anxiety, and increased use of public health resources. 10 –12 Significant advances have been observed in symptom prevention and management by virtue of improved understanding of the pathophysiology of chemotherapy-induced nausea and vomiting. Janelsins et al 13 reported how following clinical practice guidelines for these symptoms outlined by several health agencies can improve chemotherapy-induced nausea and vomiting control by 20%. As such, research reports significant improvements in the treatment of acute chemotherapy-induced vomiting with antiemetic agents. 14 –16 However, despite improved efficacy of these agents, managing anticipatory and delayed chemotherapy-induced nausea and vomiting proves to be challenging for cancer patients and medical staff. 17,18
Prior studies have reported the variability with the incidence of these chemotherapy side effects to be multifactorial: emetogenicity of chemotherapy, treatment schedule, and dosage and patients’ characteristics (female gender, younger age, presence of anxiety, cancer-related fatigue, motion sickness, alcohol consumption, and history of nausea and vomiting). 19,20 Psychological factors such as anxiety can also contribute to the occurrence and maintenance of chemotherapy-induced nausea and vomiting. There is a general consensus in explaining anticipatory nausea and vomiting as a conditioned response to contextual factors (sounds, smells, and sight of the clinic), which become conditional stimuli paired with chemotherapy (unconditional stimulus), thus eliciting an unconditional response (nausea and vomiting). 21,22 Additionally, cognitive factors and emotional appraisal such as negative expectations, perceived lack of control, and fear of suffering have also been labelled as chemotherapy-induced nausea and vomiting contributing factors. 23 Altogether, additional interventions targeting these contributing factors are necessary due to their effect on these adverse symptoms.
An increasing number of women diagnosed with breast cancer seek complementary and alternative medicine to cope with their diagnosis. 24 Yoga practice has seen a significant increase for cancer survivors and patients undergoing treatment. 24 Yoga seems to yield positive outcomes in chemotherapy-induced nausea and vomiting management. A randomized controlled trial found both yoga and relaxation to be helpful in reducing these side effects among breast cancer patients. 25 A previous study, conducted by the same aforementioned authors, found yoga to significantly reduce anticipatory nausea and vomiting and posttreatment chemotherapy-induced nausea compared with a control group. Additionally, a significant positive correlation was found between chemotherapy-induced nausea and vomiting scores and anxiety, depression, and distressful symptoms. 26 Despite promising results, a systematic review and meta-analysis reported mitigated results of yoga interventions on chemotherapy-induced nausea and vomiting among breast cancer patients. 27 Most important, the selected studies lacked sufficient statistical power in order to detect not only statistical differences between both groups but also significant clinical changes. 27 In light of these findings and yoga’s increasing popularity among breast cancer patients, additional randomized controlled trials are necessary to further investigate the potential benefits of yoga interventions. A previous study conducted with the Bali yoga program for breast cancer patients receiving chemotherapy reported significant decrease in depressive symptoms and improvement in quality of life. 28 This program is based on the original method of Madan Bali. Dr Madan Bali’s method combines Hatha yoga postures, breathing, and visualization techniques in a unique way in order to promote the body’s ability to replenish itself in between frequent relaxation periods. Although this method can be characterized as Hatha yoga, the focus remains on the visualization techniques to increase one’s awareness about the psychological and physiological impact of the postures chosen. In the past few years, this method has been tailored to meet the needs of breast cancer patients. Among the distinctive features of this program, we found the psychoeducational content about the psychophysiological aspects related to cancer and the importance of the relaxation response during as well as between yoga poses. The validation of this program is underway.
The aim of this study is to determine the effects of a standardized yoga program on chemotherapy-induced nausea and vomiting among breast cancer patients. Primarily, we hypothesize that breast cancer patients enrolled in the 8-week Bali yoga program will show decreased chemotherapy-induced nausea and vomiting compared with patients on the waiting list. Our secondary objective will be to investigate how anxiety affects chemotherapy-induced nausea and vomiting.
Methods
Participants
Enrollment for the study occurred over a 2-year period from 2011 to 2013 in 3 hospitals in Montreal (Canada). Participants were recruited by nurses through direct contact during initial scheduled clinical visits prior to their first cycle of chemotherapy or just after their first cycle of chemotherapy. Eligibility was defined as follows: ability to understand French, be 18 years or older, have a breast cancer diagnosis (stages I-III), receive chemotherapy, consent from medical team, no regular practice of yoga, no current psychotherapy, no psychiatric diagnosis, and no heart failure. Eligibility was further confirmed by research assistants prior to study enrollment. Written informed consent was obtained from all participants. It was clearly stated that their approval or disapproval to participate in the study at any point in time would not interfere with their cancer treatments.
Procedure
Group assignment was determined by a computer-generated random table in cohorts of 10 with an allocation ratio of 1:1. The hospital staff enrolling participants were blinded to the allocation sequence. Blinding of participants and research assistants to group assignment was not possible due to the nature of the intervention. The treatment group received the Bali yoga program for 8 weeks along with standard care. Concurrently, the waitlist control group only received standard care for 8 weeks followed by the Bali yoga program for an additional 8 weeks.
The Bali yoga program for breast cancer patients consisted of 8 weekly group sessions of 90 minutes with 5 participants per group, led by one instructor. Participants were also given a DVD of the intervention with a 20- and 40-minute session format. The sessions were conducted in each hospital’s cancer department conference room. The 2 instructors available for the study were certified yoga teachers trained by Dr Bali and had extensive experience teaching yoga to cancer patients and survivors. Moreover, they each received an 8-week training that included a standardized manual delineating the program with detailed session guidelines, pilot groups, and discussion of the themes elaborated by 2 psychologists and Dr Bali.
This program combines Hatha yoga poses, frequent relaxation periods between poses, and breathing techniques as well as meditation and visualization. This combination aims to stimulate the body and mind to better mobilize them against illness. Each session was as follows: introduction of the theme (5 minutes); guided relaxation based on the theme (10 minutes); combination of gentle yoga poses and relaxation with breathing techniques (60 minutes); guided meditation with OM chant (7 minutes); final relaxation (8 minutes). The 8 psychoeducational themes were importance and benefits of relaxation; definition and causes of stress; power of a concentrated mind and positive imagery; immune system function; activation of the healing response; benefits of breathing; acceptance philosophy; and importance of daily yoga practice. During the session, the instructor discussed the physiological and psychological benefits of the gentle poses and emphasized the importance of being aware of one’s body sensations. Between each pose, a short relaxation/breathing/visualization sequence was carried out. The poses were added progressively as follows: 12 poses (session 1), 4 poses (session 2), 6 poses (session 3), 1 pose (session 4), and 1 pose (session 5). By the sixth session, 24 poses are practiced. Participants were instructed to practice at home daily with the 20-minute session format the first 4 weeks and the 40-minute session format the 4 remaining weeks.
All poses were seated, supine, or on all fours. Alternative poses adapted to the participants’ condition were also proposed. They were supplied with a yoga mat, a blanket, and supportive blocks. Table 1 present the list of poses. Please contact the first author for additional information concerning the Bali yoga program.
Bali Yoga Program Poses.

Data collected included medical (cancer related, medical history) and demographic (age, marital status, education, occupation) information obtained by nurses and research assistants using medical records and study-specific forms. Medical data were collected during the initial assessment and throughout patients’ chemotherapy, while demographic data were collected during the initial assessment. Participants were on a variety of chemotherapy protocols and antiemetic medication (see Table 2).
Sample Characteristics.

Abbreviations: BYP-BC, Bali yoga program breast cancer; WL, waitlist; AC, cyclophosphamide-doxuribicin; CMF, cyclophosphamide-methotrexate-fluorouracil; FEC, fluorouracil (5FU), epirubicin, cyclophosphamide; AC-T/TAC, cyclophosphamide-doxuribicin and taxol/cyclophosphamide-doxuribicin and taxotère; 5hT3, 5-hydroxytryptamine; NK1, neurokinin 1.
aN = 74 for family status variable.
bN = 75 for education and employment variables.
cCenter 1 = Centre hospitalier de l’université de Montréal; Center 2 = Centre intégré de cancérologie de Laval; Center 3 = Centre intégré de cancérologie de la Montérégie.
*P < .05. **P < .1.
Outcome Measures
Chemotherapy-Induced Nausea and Vomiting
Chemotherapy-induced nausea and vomiting was assessed with the Morrow Assessment of Nausea and Emesis Scale. 29 It is a self-administered scale measuring the frequency (absence vs presence), intensity (1-6; very mild to intolerable), worst moment (1-7; worst during treatment to no time more severe than any other), and duration (in hours) of anticipatory and posttreatment chemotherapy-induced nausea and vomiting. Test-retest reliability has been reported to range from 0.72 to 0.96 with different chemotherapy protocols. It was administered after the first chemotherapy cycle, midway through and at the end of the study (eighth week). Participants had to complete a weekly diary in which the intensity of chemotherapy-induced nausea and vomiting was assessed on a 4-point scale (0-4; not at all to very severe).
Anxiety
Anxiety symptoms were assessed using the French version of Strait-Trait Anxiety Inventory–Y Format. 30 It is a 40-item self-administered questionnaire assessing state (20 items) and trait anxiety (20 items) on a 4-point Likert-type scale (1-4; not at all to very much so). Internal consistency has been reported to range from 0.83 to 0.92. For the purpose of this study, only the 20-item state anxiety subscale was administered. The scores can range between 20 and 80. Higher scores indicate greater anxiety. Data was collected at baseline and after 8 weeks. Participants had to complete a weekly diary in which mood (frustration subscale, anxiety subscale, depressive subscale) was assessed on a 4-point scale (0-4; not at all to very severe).
Last, participants enrolled in the yoga Bali yoga program had to record their daily practice with the DVD and their daily activities while the waitlist group recorded their daily activities.
Data Analysis
Participants’ clinical and sociodemographic characteristics and outcome measures were analyzed using univariate and correlation analyses and χ2 tests to determine between-group differences and potential covariates. An intent-to-treat analysis using ProcMixed Models was employed in which all randomized participants were included in the analysis with all their available data. Repeated-measure analyses were conducted to assess within-group changes over time (baseline–midway–8 weeks) and between-group differences (experimental vs control group) with regard to chemotherapy-induced nausea and vomiting measures. Additionally, Mann-Whitney analyses were carried out to assess the difference between both groups on weekly intensity of these symptoms. Last, Pearson and Spearman correlations were conducted between anxiety symptoms and chemotherapy-induced nausea and vomiting measures to assess potential relationships. Primary outcome data were analyzed with Statistical Analysis System (SAS, Version 9.4), 31 and the secondary outcome data and descriptive statistics were conducted using Statistical Package for Social Sciences (SPSS, Version 22). 32 The α level used to determine statistical significance was P < .05. For all analyses each effect size was reported using the r coefficient.
Results
Participants
A total of 130 participants were screened and 82 were enrolled and randomly assigned to each group (see Figure 1). Uneven group distributions can be explained by recruitment difficulties in balancing cohorts resulting in 16 participants being assigned rather than randomized to each group. However, no statistical differences were observed when these participants were excluded from analyses.

Participant flow chart.
Differences among both groups were found on the following variables: employment and antidepressant medication (see Table 2). As such, these variables were included as covariates in the final analysis model. Age and cancer stage were also added in the final model as they correlated with the outcome variables. No other statistically significant differences on sociodemographic, medical, or baseline symptoms scale variables were found between both groups. Sixty-four participants completed the study. Completers received more chemotherapy (4.3 ± 1.6) than noncompleters (2.4 ± 1.6). Also, noncompleters had significantly more osteoarthritis (52.6% vs 17.9%, P = .00), muscle pain (78.9% vs 46.0%, P = .01), and headaches (68.4% vs 42.9%, P = .05). It is noteworthy to mention the observed differences were present prior to the start of the study. Finally, class attendance for the Bali yoga program was 5.5 ± 2.7 sessions while participants practiced 1.7 ± 0.8 hours per week at home. No adverse effects were reported due to study intervention.
Post–Chemotherapy-Induced Nausea
No group main effect (F[1, 96] = 1.33, P = .25, r = 0.12), time main effect (F[2, 96] = 2.03, P = .14, r = 0.06), nor interaction effect (F[2, 96] = 0.16, P = .85, r = 0.06) were found to be statistically significant for the frequency of nausea. The percentage of participants experiencing nausea in the treatment group (BYP-BC) varied from 71.2% after their first cycle of chemotherapy to 60.4% after 8 weeks. Meanwhile, after their first cycle of chemotherapy, 62.1% of participants in the WL group complained of nausea and said symptom was still present for 47.4% of participants after the eighth week (see Table 3).
Frequency, Mean Scores, and Standard Deviations of Post–Chemotherapy-Induced Nausea and Vomitinga.
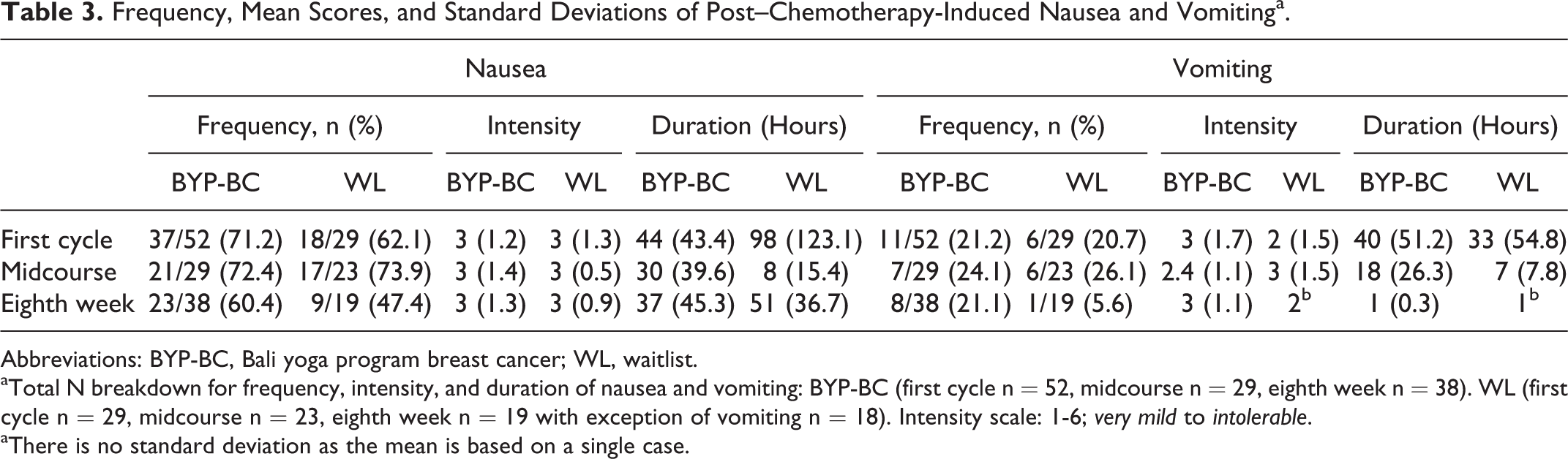
Abbreviations: BYP-BC, Bali yoga program breast cancer; WL, waitlist.
aTotal N breakdown for frequency, intensity, and duration of nausea and vomiting: BYP-BC (first cycle n = 52, midcourse n = 29, eighth week n = 38). WL (first cycle n = 29, midcourse n = 23, eighth week n = 19 with exception of vomiting n = 18). Intensity scale: 1-6; very mild to intolerable.
aThere is no standard deviation as the mean is based on a single case.
No group main effect (F[1, 64] = 1.33, P = .48, r = 0.09), time main effect (F[2, 64] = 0.99, P = .38, r = 0.17), nor interaction effect (F[2, 64] = 0.23, P = .80, r = 0.08) were found to be statistically significant for the intensity of nausea. The intensity of chemotherapy-induced nausea ranged from mild to moderate for participants in both groups (see Table 3).
No group main effect (F[1, 55] = 0.02, P = .89, r = 0.02), time main effect (F[2, 55] = 1.76, P = .18, r = 0.25), nor interaction effect (F[2, 55] = 1.72, P = . 19, r = 0.24) were found to be statistically significant for the duration of nausea. Duration of chemotherapy-induced nausea varied greatly ranging from 37.1 hours to 98.3 hours across both groups (see Table 3).
There was no statistical significant difference between groups concerning the worst moment of experiencing nausea across each time point (F[2, 86] = 0.53, P = .60, r = 0.11). After the first cycle of chemotherapy, most participants in the BYP-BC group reported nausea being worst 24 hours after treatment, while participants in the WL group did not seem to highlight a worst moment. After the midcourse cycle and the eighth week, there was no particular worst moment reported for participants in both groups.
Post–Chemotherapy-Induced Vomiting
No group main effect (F[1, 94] = 1.47, P = .23, r = 0.12), time main effect (F[2, 94] = 1.44, P = .24, r = 0.17), nor interaction effect (F[2, 94] = 0.80, P = .45, r = 0.13) were found to be statistically significant for the frequency of vomiting. The percentage of participants experiencing vomiting in the treatment group (BYP-BC) varied from 21.1% to 24.1% across cycles of treatment. However, the percentage of participants experiencing vomiting in the WL group was highest during the midcourse cycle (26.1%) and lowest at the eighth week (5.6%; see Table 3).
No group main effect (F[1, 64] = 1.23, P = .27, r = 0.14), time main effect (F[2, 64] = 2.11, P = .13, r = 0.25), nor interaction effect (F[2, 64] = 0.59, P = .56, r = 0.13) were found to be statistically significant for the intensity of vomiting. The intensity of chemotherapy-induced vomiting ranged from mild to moderate for participants in both groups (see Table 3).
No group main effect (F[1, 60] = 0.01, P = .78, r = 0.01), time main effect (F[2, 60] = 2.14, P = .13, r = 0.26), nor interaction effect (F[2, 60] = 0.53, P = .59, r = 0.13) were found to be statistically significant for the duration of vomiting. Duration of chemotherapy-induced vomiting varied greatly, ranging from 1 hour to 40 hours across both groups (see Table 3).
There was no statistical significant difference between both groups concerning the worst moment of experiencing vomiting across each time point (F[2, 85] = 0.93, P = .40, r = 0.15). After the first cycle of chemotherapy, most participants in the BYP-BC group reported vomiting being worst 4 to 8 hours after treatment while participants in the WL group rated it worst 4 to 8 hours and 12 to 24 hours after treatment. After the midcourse cycle and the eighth week, there was no particular worst moment reported for participants in both groups.
Anticipatory Nausea and Vomiting
The repeated-measures analysis was not carried out due to the frequency being too low to enable comparisons (see Table 4).
Prevalence and Mean Scores and Standard Deviations of Anticipatory Nausea and Vomitinga.

Abbreviations: BYP-BC, Bali yoga program breast cancer; WL, waitlist.
aAbsence of anticipatory vomiting for the BYP-BC group at the midcourse and eighth week time points.
bThere is no standard deviation as the mean is based on a single case.
cThere is no case to provide neither a mean nor a standard deviation.
Weekly Assessment of the Intensity of Chemotherapy-Induced Nausea and Vomiting
Mann-Whitney analyses revealed no statistical significance between groups on the intensity of chemotherapy-induced nausea for each time point across the 8 weeks (ranges from Z[−1.00], P = .31, to Z[−0.81], P = .42). No statistically significant differences were found between groups on the intensity of chemotherapy-induced vomiting for each time point across the 8 weeks (ranges from Z[−2.21], P = .84, to Z[0.00], P = .00).
Correlates Between Anxiety and Chemotherapy-Induced Nausea and Vomiting
First, the correlations were carried across the whole sample as there was no treatment effect. A cumulative score was computed to have an overall picture of chemotherapy-induced nausea and vomiting throughout the 8 weeks with the 3 assessment points of the MANE questionnaire. Hence, 6 scores were created: total frequency of post-chemotherapy nausea (TFPCN), total frequency of post-chemotherapy vomiting (TFPCV), mean intensity of post-chemotherapy nausea (MIPCN), mean intensity of post-chemotherapy vomiting (MIPCV), mean duration of post-chemotherapy nausea (MDPCN), and mean duration of post-chemotherapy vomiting (MDPCV).
Overall, no significant correlations were found between baseline anxious symptoms and overall frequency, intensity, or duration of post-chemotherapy nausea or vomiting (see Table 5). Spearman correlations revealed no statistical significance between weekly assessments of anxious symptoms and chemotherapy-induced nausea intensity (ρ = 0.07, P = .18) nor with chemotherapy-induced vomiting intensity (ρ = 0.03, P = .52).
Pearson Correlation Between Post-Chemotherapy Measures and Anxiety Baseline Score.

Abbreviations: TFPCN, total frequency of post-chemotherapy nausea; TFPCV, total frequency of post-chemotherapy vomiting; MIPCN, mean intensity of post-chemotherapy nausea; MIPCV, mean intensity of post-chemotherapy vomiting; MDPCN, mean duration of post-chemotherapy nausea; MDPCV, mean duration of post-chemotherapy vomiting.
aAvailable data for anxiety scores is based on 72 participants.
Despite the lack of correlation between anxious symptoms and chemotherapy-induced nausea and vomiting, a statistical significant time effect (F[1, 67] = 8.70, p < 0.00, r =0.34) and interaction effect (F[1, 67] = 4.99, P = .03, r = 0.26) was found for State-Trait Anxiety Inventory scores (see Table 6). While the decrease in anxious symptoms was not statistically significant in the WL group (t[67] = 0.48, P = .6, r = 0.06), a significant decrease in symptoms was found within the BYP-BC group (t[67] = 4.00, p < 0.00, r = 0.44). Last, there was a statistical trend found when comparing both groups postintervention (t[67] = 1.86, P = .07, r = 0.22).
STAI Mean Scores and Standard Deviations.

Abbreviation: STAI-Y, State-Trait Anxiety Inventory–Y Format.
Discussion
Chemotherapy-Induced Nausea and Vomiting
Our findings did not confirm our hypothesis and would suggest the Bali yoga program having no effect on chemotherapy-induced nausea and vomiting. Despite the lack of significant results, it remains worthwhile to explore possible reasons contributing to these findings.
First, it is possible the yoga intervention did not reduce these adverse symptoms as they were already well managed. Across the 3 time points assessed, participants in both groups rated post-chemotherapy intensity of nausea and vomiting as being mild to moderate. Overall, across both groups, approximately 80% of participants followed the antiemetic regimen and 80% rated them as being very helpful to helpful enough. Also, each participating hospital followed clinical practice guidelines for chemotherapy-induced nausea and vomiting management. Once more, managing these symptoms can be improved by 20% by following these guidelines. 15 Therefore, it is possible the sample in this study represents that category of patients.
Several studies have found exercise to improve quality of life and physical and emotional well-being of cancer patients during and after treatment. 33,34 It was observed that participants in both groups were physically active and had various coping strategies (shopping, walking, gardening, swimming, gym training, etc) and rated these activities as moderately to very helpful in coping with their illness and its side effects. It is possible the Bali yoga program did not provide an additional beneficial impact over these coping strategies.
Although no current psychotherapy was an eligibility criterion, once randomized, participants had access to psychological services if needed. There was no significant statistical difference between both groups on seeking psychological services. However, these sessions could have been beneficial in reducing chemotherapy-induced nausea and vomiting and psychological factors related to said symptoms in both groups. Altogether, the available resources, the participants’ self-care behaviors, and the effective management of these side effects could also explain the lack of correlations found between digestive toxicity and anxiety. However, we found a decrease of anxiety symptoms in the BYP-BC group but not in the control group. This is in accordance with many studies on yoga and anxiety symptoms during cancer. 24
It would have been purposeful to measure cognitions pertaining to chemotherapy-induced nausea and vomiting specifically and investigate locus of control. It would have provided relevant information pertaining to symptom experience. It could be speculated that despite having chemotherapy-induced nausea and vomiting, knowing what to expect and believing in one’s ability to manage them would prevent participants to rate these symptoms as debilitating, thus rating them at a lower intensity. It is also possible that a lack of significant results with the Bali yoga program could be due to the measurement methods selected. As previously mentioned, these symptoms are not only highly variable between patients but also within each patient. The MANE was primarily chosen due to its wide use 35 and also in attempt to replicate Raghavendra et al. 26 However, it is possible that retrospective self-report could have underestimated the intensity and duration of chemotherapy-induced nausea and vomiting. In fact, Carnrike et al 36 reported moderate concurrent validity of this questionnaire compared to asking directly each time, and Coolbrandt et al 37 reported discrepancies between immediate versus delayed self-reporting of side effects during chemotherapy. It would have been better to ask every day and every hour (acute vs delayed) and anticipatory versus post chemotherapy when there was a chemotherapy cycle scheduled. Ideally, it would be after every treatment.
Finally, the most cited study highlighting beneficial impact of yoga interventions in reducing chemotherapy induced nausea and vomiting is Raghavendra et al. 26 Several reasons can account for the current study’s lack of corroborating results. First, the way in which yoga was administered greatly differed. In his protocol, it was an individualized treatment starting 30 minutes before each treatment. Participants were asked to practice daily for 1 hour, 6 days per week, minimum 3 hours per week, and house visits were scheduled to monitor their home practice and discuss possible doubts, motivation, and education. Also, the authors highlighted the possibility of antiemetic regimen not following the international guidelines for delayed chemotherapy-induced nausea and vomiting. Additionally, he revealed the control group receiving less coping preparation and counselling support than the yoga intervention group that could account for the observed differences. In sum, all these differences can explain why our results did not corroborate his findings. Finally, it is possible no significant results were found due to the variability of adherence to yoga intervention and home practice (5.5 ± 2.7 sessions, 1.7 ± 0.8 hours per week for home practice). As seen in several studies, yoga interventions’ beneficial impact on chemotherapy-induced nausea and vomiting seemed to be found when these interventions were longer in duration and/or several times per week and adherence was highly rated. 38 Therefore, it is possible that improving class attendance and home practice could be a starting point to evaluate the potential benefits of the Bali yoga program for breast cancer patients in future studies.
Strengths and Limitations
First, the sample was of modest size, which resulted in a low statistical power for certain analyses, thus lowering the probability of having significant results especially with missing data. Furthermore, missing data due to noncompleters and methodological oversights contributed to an important loss of available cases to conduct analyses. Also, the research assistant and participants were not blinded to group assignment. The research design did not control for nonspecific ingredients of the yoga intervention other than the passage of time like therapeutic expectations. Also, the method of assessing chemotherapy-induced nausea and vomiting and possible confounding variables could have contributed to the lack of significant findings. Despite its limitations, this study has several strengths. The yoga intervention was based on a standardized manual with additional training ensuring feasibility and replication of the intervention. Also, several cofounding variables were included in the analyses procedures. Last, methodological limitations were explored and future studies goals were outlined.
Conclusion
Despite not being able to confirm our main hypothesis, this study will add to the growing body of research pertaining to yoga interventions and chemotherapy-induced nausea and vomiting. As it is becoming increasingly popular among breast cancer patients, a better understanding of their clinical significance in managing distressing symptoms is paramount. Moreover, our study can help future research in conducting improved randomized controlled trials with larger and homogenous sample sizes and improved chemotherapy-induced nausea and vomiting assessments. Ultimately, such studies are needed to determine to what extent yoga can be a beneficial, safe complementary adjunct in cancer support care.
Footnotes
Acknowledgments
The authors thank the patients in all 3 hospital centers in Montreal, Canada, for participating in the study. They also thank Maryse Carignan, Sylvie Coallier, and Sonia Joannette for their contribution with patient recruitment. The authors also thank both yoga instructors, Susan Frédérick and Chantal Vallée, for their time and dedication. The authors also acknowledge Jill Vandermeschen for her contribution in the preparation of this article.
Author Contributions
ASA conducted the data collection, primary data analyses, and wrote the majority of the final article as the thesis requirement for her Doctor of Psychology degree. GD is the thesis director who provided mentorship, conceptualized the study design and methodology, supervised the data analyses, and edited the final article. DL worked on the conceptualization of the Bali yoga program for breast cancer and contributed in the study design and methodology. MB contributed to the yoga intervention program based on his original method and edited the yoga intervention section in the article.
Declaration of Competing Interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article. MB is the founder of the original Bali method and contributed to conceptualization of the adapted program for breast cancer. DL and GD conceptualized the Bali yoga program for breast cancer based on MB’s original method. However, neither GD, DL, nor MB were involved in administering the yoga intervention or in data collection/analysis. GD’s involvement in data analysis was to supervise the first author’s data analysis methods and the work was also verified by an outside source (Jill Vandermeschen) who is a statistician from the university’s data analysis consultation department.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval
All study procedures were approved by the research and ethical committees of the following hospital centers in Montreal Canada: “Centre hospitalier de l’université de Montréal,” “Centre intégré de cancérologie de la Montérégie,” and “Centre intégré de cancérologie de Laval.” Patients did not receive any type of compensation for participation and there was no interference with their cancer treatments if they declined or opted out of the study.
