Abstract
Background.
Mind–body skills (MBS) training is popular, but in-person training can be inconvenient and costly. We assessed the impact of online MBS training on clinicians’ and trainees’ stress, mindfulness, and confidence in providing calm, compassionate care.
Methods.
This was a prospective cohort trial. Trainees entering medical school; graduate programs in nursing, social work, and dietetics; and residencies in family medicine and pediatrics at a large Midwestern academic health center were invited to complete online surveys before and 12 weeks after enrolling in online elective integrative health courses on MBS training or not. The elective offered no course credit and had no mandated deadlines for completion.
Results.
At baseline, the 60 who engaged in MBS training were similar to the 43 who did not in terms of profession, gender, perceived stress levels, mindfulness, resilience, and compassion. MBS participants engaged in a median of 3 of 12 available modules with a bimodal distribution peaking at 1 to 2 and 12 modules. Twelve weeks later, those who participated in MBS showed significantly greater improvements in measures of stress, mindfulness, and confidence in providing calm, compassionate care than those who did not.
Conclusions.
Online elective training offers a feasible strategy to improve mindfulness, stress, and confidence in providing calm, compassionate care. Additional studies are needed to determine the impact of required versus elective courses, the optimal dosage and content of training, and the costs and benefits of online versus in-person training.
Mindfulness and resilience have gained increasing attention as possible protective factors against clinician burnout, a major risk factor for poor clinician health and poor quality of patient care. 1,2 Mind–body skills (MBS) training (eg, mindfulness-based stress reduction [MBSR]) has become a popular strategy to improve health professionals’ mindfulness, decrease stress and burnout, and improve patient care. 3 –15 Mindfulness has been defined as paying attention in a particular way—on purpose, to the present moment, nonjudgmentally. 6,16 In physicians, mindfulness is correlated with resilience, self-compassion, and confidence in providing calm, compassionate care and negatively associated with burnout and stress. 17 Similarly in nurses and other health professionals, mindfulness training enhances resilience over time. 18,19
Although evaluations of most professional training focus on knowledge, attitudes such as compassion for self and others are also linked to important outcomes. In one study, we found that self-compassion was positively associated with clinician resilience and mindfulness. 17 In another study, mindfulness and self-compassion were both significantly inversely associated with burnout, which makes them promising targets for training programs aimed at decreasing burnout and improving quality of care. 20
Earlier research suggested that an 8-week in-person elective significantly improved trainees’ confidence in providing calm, compassionate care 21,22 ; however, that research did not include a comparison group, and trainees’ confidence may have improved over time regardless of the specific content of their studies. Similarly, many studies of mindfulness training use a waiting list control group, but waiting lists themselves may contribute to frustration and stress, making the study intervention appear better than it might compared with a non–waiting list control group. 23
In-person MBS training may not be feasible to deliver to large interprofessional groups of trainees, leading to interest in convenient, less costly online training. Typical in-person MBSR courses involve weekly 2.5-hour sessions plus a day-long retreat with a highly trained instructor. Briefer in-person training (90 minutes to a weekend in length) can offer benefits in stress, resilience, mindfulness, and quality of life. 24 Delivering MBS training online is convenient, and studies in patients suggest that it may offer comparable benefits to in-person training. 25 –30 However, few studies have evaluated the feasibility or impact of online MBS training for diverse health professionals. One study evaluating the acute impact of a single hour of online MBS training found significant improvements in stress, mindfulness, resilience, and empathy, 31 but the duration of the impact of brief online MBS training is unknown.
As health educators, our long-term goal is to determine the most cost-effective strategy to improve clinicians’ mindfulness and compassion to enhance their health and the quality of care they provide. To evaluate the specific effects of this training, we offered trainees their choice of either no training or a similar online elective course on another popular topic in integrative health care, herbs and dietary supplements (HDS). All training was free, optional, and not required for course credit. Our primary question for this study was to assess the 12-week impact of an online elective in MBS (compared with no online MBS training) on clinicians’ mindfulness, empathy, compassion, and confidence in providing calm, compassionate care.
Methods
To answer these questions, we conducted a cohort trial between May 1 and October 31, 2014, at a large Midwestern university that offers degree programs in several health professions.
Subjects
Participants were eligible if they agreed to participate in a study evaluating new online curricula in integrative medicine. Recruitment occurred by email. Our goal was to recruit 200 diverse participants within the 3 months prior to the start of the 2014 fall semester.
The administrative offices of the Deans of the Colleges of Medicine, Social Work, and Nursing, the Director of the PhD Program in Human Nutrition and Dietetics; as well as the Program Directors for Pediatrics, Family Medicine, Hematology-Oncology, and Palliative Care at the Ohio State University sent emails to incoming graduate students, residents, and fellows in May and June of 2014 inviting them to participate in the project with a link to the pretraining survey. The last page of the survey included a link to register for a free online course on herbs and dietary supplements (HDS) or mind–body skills (MBS) training for resilience, effectiveness, and mindfulness. Survey participants were not required to enroll in either course.
Approximately 450 individuals received a direct email inviting them to participate; we did not count email “bounces” or returns, though there were a substantial number since many trainees were moving from other institutions to begin new programs. Some faculty and staff also asked to participate so they could review the curricula.
The online curricula were created and reviewed by an interprofessional group of clinicians, researchers, educators, and trainees in the health professions. The HDS program contained 14 one-hour modules of continuing medical education–approved material. Each module focused on one topic (eg, safety, cardiology, mental health, women’s health, pediatrics, etc) and included learning objectives, cases, and evidence-based information with hyperlinks to primary source material, self-assessment questions, and additional resources. The HDS curricula had been tested in large randomized controlled trials and showed significant immediate and long-term effects on knowledge, confidence in talking about HDS with patients, and improvements in communication about HDS. 32,33 However, it had no known impact on mindfulness, resilience, or compassion.
The MBS curriculum contained 12 one-hour modules of continuing medical education–approved material organized in 4 general topics: (1) focused attention meditation (relaxation response); (2) mindfulness meditation; (3) positive affect meditation (positive or sacred word, gratitude, and loving-kindness/compassion meditation); and (4) guided imagery/hypnosis (autogenic training; guided imagery to prepare for surgery, procedures, or childbirth; and guided imagery for sleep and changing habits). Module organization was similar as for HDS, and also included links to free online MP3 recordings of practices to encourage personal practice of MBS. It also included tips on introducing these skills to patients.
Both courses were free, voluntary, and elective. There were no deadlines for completing either course. Because one of the purposes of the MBS course was to help decrease perceived stress, participants were invited to complete the modules of greatest interest and relevance to them without any pressure to complete a certain number by any particular deadline. Participants were assured that we were most interested in their feedback to improve the courses for future participants. Participants were not required to complete any modules in order to be eligible for gifts for completing the baseline ($10) or follow-up ($15) surveys.
Demographic Measures
Demographic items used to describe the survey sample included age, gender, and profession. Participants were asked which (if any) of 10 common health conditions (such as headaches, high blood pressure, allergies, and “other”) they had experienced in the last year. Perceived stress levels were assessed using Cohen’s 10-item Perceived Stress Scale 34 to assess whether students with higher stress levels preferentially enrolled in training in MBS.
Mind–Body Training and Practice
One question asked about training in mind–body practices (“In which of the following have you had formal training in the past 3 years?”). Ten practices (including “other”) were listed; answers were scored as the number of practices (0 to 10) in which the participant had received formal training in the past 3 years. Another question asked about frequency of mind–body practice; answers included 0 (never), 1 (once or twice a month), 2 (2-3 times monthly), 3 (weekly), 4 (3-5 times weekly), and 5 (6-7 times weekly).
Mindfulness was assessed using the 10-item Cognitive and Affective Mindfulness Scale–Revised (CAMS-R), 35 which has a 5-point summative rating scale (1 = rarely or never at all, 5 = almost always), and one reverse-coded item, with a typical total mean score of 31 ± 5.
Self-compassion is distinct from self-esteem, self-pity, and self-indulgence in that it focuses on kindness toward self as a human being, not better or worse than other humans, mindfulness, and a sense of common humanity. We included self-compassion because in our pilot studies, it was significantly associated with mindfulness and confidence in providing calm, compassionate care to others and inversely associated with burnout. 17,20 Self-compassion was assessed using the 12-item Neff’s self-compassion scale, which has 6 reverse-scored items rated on a 0 = never to 5 = always scale and a total mean score among undergraduate students of 36 ± 7 and an item mean score of 3.0. 36
Confidence in providing calm, compassionate care was assessed using the 10-item Calm, Compassionate Care Scale. 37 This scale has possible scores ranging from 0 to 100, with mean scores of 62 and Cronbach’s α of .87. In our pilot study, scores on this scale were inversely related to perceived stress, and positively related to mindfulness and self-compassion. 17 Due to a clerical error in preparing the posttraining questionnaire, only 7 of the 10 items were included in the posttraining questionnaire. To promote a fair comparison, only these 7 items were scored on the pre- and posttraining questionnaires, giving an expected mean score of about 40.
Resilience was assessed using Smith’s 6-item Brief Resilience Scale, 38 which has 3 reverse-scored items and a typical item mean score of 3.5.
Empathy was measured with the 7-item Empathic Concern Scale (ECS) and the 7-item Perspective-Taking (PT) scale, which are both part of the Interpersonal Reactivity Index. 39 –46 Both scales use a 5-point summative rating scale where 0 = does not describe me well and 4 = describes me well; both the ECS and PT scales have normative median scores of 24. We chose these measures rather than the Jefferson Scale of Physician Empathy because our participants included diverse health professionals, not just physicians. 41
Compassion was measured using the 5-item Santa Clara Brief Compassion Scale, which uses a 7-point summative rating scale (1 = not at all true of me and 7 = very true of me), and has a typical mean score of 30, with a range from 9 to 35. 47
Links to follow-up online questionnaires were emailed to participants approximately 12 weeks after they returned their pretraining surveys. Participants were asked to complete the posttraining survey regardless of whether they had registered for any course and regardless of how many modules they had completed to assist in program evaluation. Up to 4 reminders were sent to nonrespondents.
Module engagement was tracked by the online web management system. To provide a conservative estimate of the impact of the MBS modules, we combined those who started a module and those who completed a module evaluation. This combination includes all those who engaged with a module, but it may underestimate course impact if those who started a module failed to use all of its components.
Surveys were completed online using Survey Monkey. Data were de-identified and cleaned by a research assistant blind to the study question, exported into a spreadsheet, and exported into Statistical Analysis System (SAS 9.2) for scoring. Univariate analysis was employed to evaluate the distribution of each variable including demographic variables and questionnaire scores. Two-tailed t tests were used to compare continuous variables such as age, and analysis of variance was used to compare distributions of nominal variables such as profession. The nonnormally distributed variables, such as frequency of mind–body practice, were compared using Wilcoxon rank sum test.
This study was approved by the OSU Office of Research Institutional Review Board (2013B0611).
Results
Participant Demographics
The recruitment strategy succeeded in recruiting to the baseline survey 218 individuals with an average age of 28 years; 76% of whom were trainees. Most (73%) were female, and all targeted professions were represented (dietetics = 26; medicine = 77; nursing = 29; social work = 51; plus other professions such as dentistry, occupational and physical therapy, public health, and psychology = 45).
Of the 218 pretraining survey respondents, 38 provided insufficient identifying information to send a follow-up email, leaving 180 eligible to receive the posttraining survey (Figure 1). Overall, 103/180 (57%) eligible participants completed the posttraining survey. At baseline, the posttraining survey completers were similar to noncompleters in terms of age, gender, profession, number of health problems, perceived stress, prior training in mind–body practices, their frequency of mind–body practice, mindfulness, resilience, and self-compassion. At baseline, those who did not subsequently complete the posttraining survey had significantly lower scores than those who did on perspective-taking, compassion, and confidence in providing calm, compassionate care (P < .05 for each).

Participant Flow.
Among the 103 participants who completed both pre- and posttraining surveys, 60 engaged in MBS and 43 did not; only 7 registered for and completed any HDS modules. Among those who did not engage in MBS, there were no significant differences among those who enrolled in HDS or neither, so their data are combined as “Not MBS.” Those who enrolled in MBS were slightly older than those who did not (29 vs 26 years old; P = .04). However, there were no other significant differences between groups. They were similar in terms of age, stress, and prior training in and frequency of practicing mind–body skills. Fewer than half of both groups had previous training in MBS, and of those who reported some training, the most common type of MBS training was yoga. Both groups reported similar baseline levels of mindfulness, self-compassion, and confidence in providing calm, compassionate care, as well as resilience, empathy, and compassion for others (Table 1).
Baseline Characteristics of Health Professionals and Trainees Who Did Not Engage in Mind–Body Skills Training.

Abbreviations: MBS, mind–body skills; CAMS-R, Cognitive and Affective Mindfulness Scale–Revised; BRS, Brief Resilience Scale; IRI, Interpersonal Reactivity Index; SCBCS, Santa Clara Brief Compassion Scale.
*P < 0.05 for differences at baselevel.
Module Engagement Rates
Among those who enrolled in MBS, participants engaged with a median of 3 modules with a bimodal distribution. The first peak was at 1 to 2 modules, and the second peak was at 12 modules. The 2 most popular modules were (1) Introduction to Stress, Resilience, and the Relaxation Response and (2) Autogenic Training (a form of guided imagery). There was a similar bimodal pattern for those who enrolled in HDS.
Changes Over 12 Weeks (Table 2)
Over 12 weeks as graduate school and residency began, perceived stress levels increased 2.5 points (a 17% increase) among those not engaged in MBS, but fell nearly a point (a 5% decrease) among those engaged in MBS (P = .006 for difference). Over the same period, there was also a drop in both mindfulness and confidence in providing calm, compassionate care among those not engaged in MBS, whereas both scores increased in those enrolled in MBS (P = .008 and P = .03, respectively, for differences). Self-compassion also increased significantly more among those engaged in MBS than those who were not (P = .008). There were no significant differences between MBS and others over 12 weeks in terms of reported changes in resilience, empathy, or compassion.
Changes in Scores From Pretraining to Posttraining Among Health Professionals and Trainees Who Did or Did Not Engage in the Mind–Body Skills Training Course.
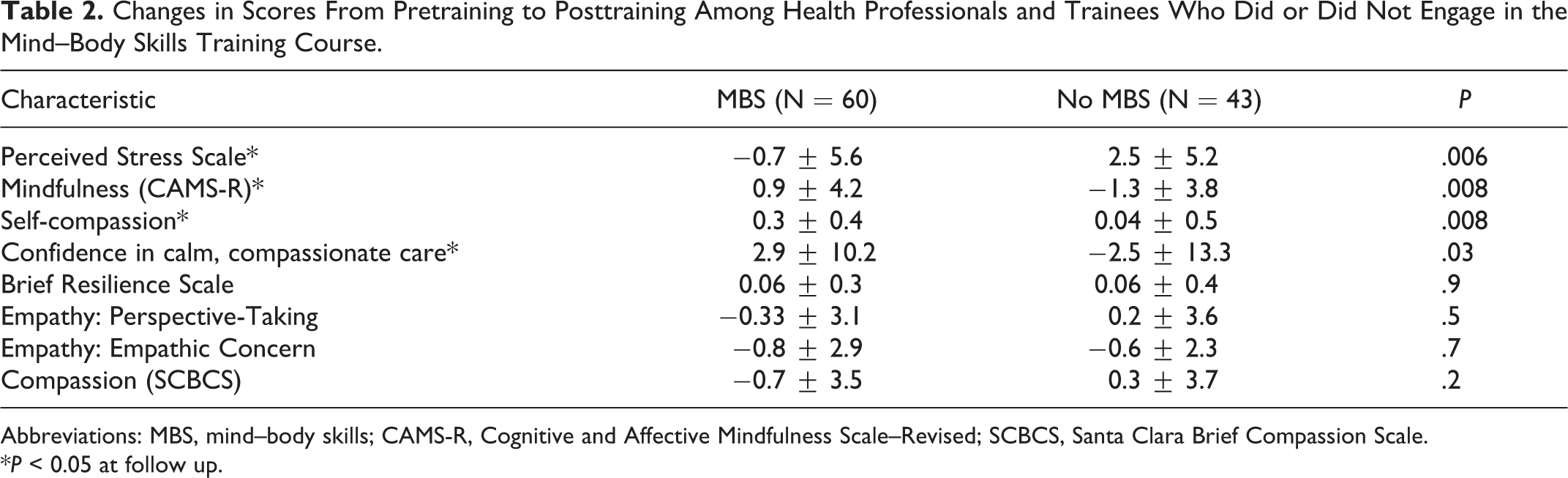
Abbreviations: MBS, mind–body skills; CAMS-R, Cognitive and Affective Mindfulness Scale–Revised; SCBCS, Santa Clara Brief Compassion Scale.
*P < 0.05 at follow up.
Discussion
To our knowledge, this is the first study evaluating the impact of an online elective program for clinicians in MBS training, and one of the few studies incorporating a concurrent comparison rather than a wait-list control group. The online MBS elective attracted participants from diverse health professions including dietetics, medicine, nursing, and social work despite the absence of course credit, deadlines, or other incentives for participation. Although those enrolled in MBS engaged with a median of only 3 modules, there were significant improvements over 12 weeks in stress, mindfulness, self-compassion, and confidence in providing calm, compassionate care during a stressful period at the beginning of graduate school/residency training when others reported more stress and declines in mindfulness and confidence in providing calm, compassionate care.
At baseline, participants in this study appear similar to those in other studies of trainees in the health professions. Our participants reported similar levels of mindfulness, self-compassion, and resilience as those reported in other studies. 35,38,48,49 There were also many similarities at baseline between those engaged in MBS and those who did not, suggesting that this project was not “preaching to the choir.” 50 On the other hand, those who eventually failed to complete the outcome survey had lower baseline scores for perspective taking, compassion, and confidence in providing calm, compassionate care, suggesting that additional work may be necessary to recruit and retain trainees who could benefit from training, and minimize the risk of ceiling effects in studies of MBS interventions. Other studies of dental, medical, nursing, pharmacy, social work, and mental health students have reported perceived stress levels ranging from 14.5 to 16.5 on Cohen’s Perceived Stress Scale, comparable to our participants’ levels of 14 to 15. 51 –54 Although the stress levels in those who enrolled in this study were no higher than in other studies of trainees in the health professions, these levels are higher than those of the general population, 55 and academic health center leaders may wish to take extra measures to guard against further increases in trainees’ stress to reduce the risk of burnout. Our data suggest that online training in MBS offers a promising strategy to mitigate this stress.
The benefits associated with this relatively small dose of MBS training (median engagement with 3, 1-hour modules) were similar to effects observed in other MBS intervention studies, most of which relied on lengthier in-person training. 15 For example, as in most studies of MBS interventions, our brief online training was associated with a significant improvement in stress. 8,27,56 –59 Similarly, as with in-person MBS intervention, our online intervention was also associated with a significant increase in mindfulness. 5,60,61 Our participants also showed a significant increase in self-compassion, similar to that reported in a study providing an 11-week medical student elective on Embodied Health. 52 As in a small study of clinicians engaged in a hybrid of online and in-person training, participants in our study showed a significant improvement in confidence in providing calm, compassionate care. 62
On the other hand, unlike some other studies of in-person MBS training, we did not detect a significant impact on empathy using 2 subscales of the Interpersonal Reactivity Index (Perspective Taking and Empathic Concern). 5,52,60,63 This may be because different studies used different instruments to assess empathy or because of actual differences in programmatic impact. Most of those engaged in our MBS curriculum completed either the Introductory module or the module on Autogenic training (a form of self-hypnosis), rather than modules focusing on loving-kindness or compassion meditation or modules requiring self-reflection on empathy. We also did not observe significant improvements in measures of resilience or compassion for others with our online curriculum; both have had variable, but often disappointing responses to MBS interventions in other research as well. 8,58,59,62 It is easy to speculate that the limited dose provided some benefits, but that higher doses, supplementation with in-person discussion groups, a focus on other topics, or additional interventions may be necessary to reap the benefits of higher resilience and compassion for others in the stressful and challenging environments in which modern health care is taught and practiced. Alternatively, other measures may be needed to more sensitively detect meaningful improvements in critical clinical qualities like resilience and compassion for others. Additional studies are needed to determine the optimal dose, format, and content of MBS training and optimal outcome measures in different kinds of health professionals.
We did not determine the depth of participant engagement with the MBS training, such as length of time spent on modules, use of the guided recordings, or application of the skills outside of the module itself. Our sample size and uneven distribution of module engagement prevented a dose–response analysis to evaluate the impact of engaging with more modules on the study outcomes. It will be informative and important for future studies to measure the depth of engagement to better understand this crucial element of the effectiveness of online MBS training.
Furthermore, although the sample size for this study was larger than many other studies of MBS training, it was too small to make meaningful comparisons among the multiple types of health professionals and trainees who enrolled in this project. Future studies will require larger sample sizes to make comparisons between trainees at different stages of training (first year medical students vs senior residents); between trainees and practicing clinicians; and between different types of professionals (eg, dietitians vs social workers vs nurses or physicians) to determine which modules work best for different kinds of health professionals. We noted that those who enrolled in MBS were slightly older than those who did not, and future studies will need to address the question of whether younger trainees benefit from the same MBS as older trainees or practitioners.
The study had additional limitations. It was a cohort study conducted at one academic health center and recruited a high proportion of female trainees. Results might not generalize to randomized trials conducted at nonacademic community settings with more experienced and/or male clinicians. The participants may have been primed by the pretraining questions to choose the mind–body training and a majority did so; setting expectations differently might have changed enrollment patterns. Although two thirds of participants chose the MBS training, most completed less than one third of the 12 modules. Whether forcing trainees to take all 12 modules by making this curriculum required rather than elective will have the same impact is unknown. We also did not have a sufficient sample to determine the unique benefits of modules on different topics. Our questionnaires did not include a standard measure of burnout, and future studies should explicitly measure this outcome. Because of their similarities, we combined the HDS enrollees and those who registered for neither course, but there may have been subtle, unmeasured differences between them. Future studies may employ randomization and an intention-to-treat analysis. As with many other studies of educational interventions, the long-term objective impact on patient care remains speculative. Although the cost of delivering online training is likely to be lower than the cost of in-person training, we did not collect cost data, and the cost–benefit of in-person versus online training will need to be addressed in other studies.
Conclusion
This study suggests that interprofessional online MBS training is not only feasible, but that it may protect against increases in stress and decreases in mindfulness and self-compassion in health professionals that are associated with burnout. Additional studies are warranted to determine the optimal dose of MBS training, the impact of making training required versus elective; the impact on burnout and objective measures of quality of care; and the cost–benefit of in-person versus online training.
Footnotes
Acknowledgments
We are grateful to Deans Thomas Gregoire (Social Work) and Cynthia Anderson (Nursing) for informing their students about the opportunity to participate in this study.
Author Contributions
KK developed the study questionnaire, prepared the institutional review board application, drafted and revised the manuscript, planned the data analysis, and coordinated the study team that recruited subjects. JL helped recruit subjects and revise the final manuscript. JM helped recruit subjects, interpret the data, and revise the final manuscript.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This project was supported by a gift from the OSU College of Medicine Alumni Association.
Ethical Approval
This study was approved by the OSU Office of Research Institutional Review Board (2013B0611).
