Abstract
Background.
Some studies have begun to show benefits of brief in-person mind–body skills training. We evaluated the effects of 1-hour online elective mind–body skills training for health professionals on mindfulness, resilience, and empathy.
Methods.
Between May and November, 2014, we described enrollees for the most popular 1-hour modules in a new online mind–body skills training program; compared enrollees’ baseline stress and burnout to normative samples; and assessed acute changes in mindfulness, resilience, and empathy.
Results.
The 513 enrollees included dietitians, nurses, physicians, social workers, clinical trainees, and health researchers; about 1/4 were trainees. The most popular modules were the following: Introduction to Stress, Resilience, and the Relaxation Response (n = 261); Autogenic Training (n = 250); Guided Imagery and Hypnosis for Pain, Insomnia, and Changing Habits (n = 112); Introduction to Mindfulness (n = 112); and Mindfulness in Daily Life (n = 102). Initially, most enrollees met threshold criteria for burnout and reported moderate to high stress levels. Completing 1-hour modules was associated with significant acute improvements in stress (P < .001), mindfulness (P < .001), empathy (P = .01), and resilience (P < .01).
Conclusion.
Online mind–body skills training reaches diverse, stressed health professionals and is associated with acute improvements in stress, mindfulness, empathy, and resilience. Additional research is warranted to compare the long-term cost-effectiveness of different doses of online and in-person mind–body skills training for health professionals.
Background
Many health professionals suffer from burnout, which adversely affects the quality of care and threatens professionalism. 1 –8 Burnout includes emotional exhaustion, cynicism (or depersonalization), and decreased sense of personal accomplishment. 9 Also called compassion fatigue, burnout can adversely affect empathic communication, relationships, and care. Because chronic, toxic stress and burnout have adverse personal and professional consequences, 6,10 institutions have prioritized programs to help reduce and manage stress. 11 –15
In recent years, mind–body skills training (MBST) such as mindfulness-based stress reduction has become a popular strategy to improve health professionals’ mindfulness, decrease burnout, and improve patient care. 16 –21 Mindfulness has been defined as paying attention in a particular way—on purpose, to the present moment, nonjudgmentally. 19,22 In a previous study, we found that mindfulness was correlated with resilience, 23 and other studies have confirmed that over time mindfulness training enhances health professionals’ resilience. 24,25 Most mindfulness-based stress reduction training for health professionals requires in-person group meetings of 2.5 hours per week for 8 weeks, and sometimes includes ongoing “booster” sessions monthly, 18 though some programs offer abbreviated, intensive group training. 21 Unlike the pharmaceutical model for acute symptom management in which a single analgesic dose is used to treat a headache, mindfulness-based stress reduction tends to operate on the healthy lifestyle model that benefits accrue, as with optimal diet and exercise, with repeated practice over time. However, there are gaps in understanding the effects of timing, onset, duration, delivery method and dosage of different types of MBST. Some studies suggest that even very short-term in-person training and practice can have potent effects on pain, cognition, stress, and empathy. 26 –31
Although health professionals are known for self-discipline and ability to delay gratification, as work demands and stress increase, professionals may be unwilling to commit to time-consuming elective training without the prospect of some immediate benefit. In a national survey of nurses, convenience was rated as the most important factor influencing a choice of stress management training.
32
Although online training offers a convenient way for busy health professionals to learn and practice mind–body skills, little is known about whether it is indeed attractive, who enrolls, and what the short-term impact of such training might be. If attractive, feasible, and impactful, online MBST might represent a reasonable alternative to more costly, less convenient in-person training. However, the lack of a supportive group learning environment might limit the attractiveness and effectiveness of online training. Therefore, this project addresses 3 specific questions: Will health professionals and trainees enroll in free elective online MBST and complete at least 1 hour of training? How do online MBST enrollees’ scores on standard measures of stress, resilience, and burnout compare with previous studies? Are there any acute changes associated with completing a 1-hour online module in enrollees’ stress, mindfulness, resilience, or empathy?
Methods
Design
This was a prospective cohort study using data collected as part of an ongoing online elective educational program in MBST at a large Midwestern academic health center between May 1 and November 30, 2014.
Participants
From May 1 to July 31, 2014, participants were eligible if they were over 18 years old, spoke and read English, had access to the Internet, and agreed to participate in a survey as part of a larger study evaluating a novel online curriculum in MBST. Recruitment occurred by e-mail and focused on entering graduate trainees in the health professions. Approximately 450 individuals received a direct email inviting them to take the course. We did not count e-mail “bounces.” The first 200 participants who completed the premodule questionnaires were eligible to receive $10 in recognition of their time completing the surveys. On August 1, 2014 registration was opened throughout the academic health center, and announcements about the new Continuing Medical Education–approved course were made on university Web sites and e-newsletters. The program was offered for free, was voluntary, was not associated with course credit, and was not required for students or academic health center employees. No deadlines were imposed on completing modules. Nor were there any financial incentives for completing modules.
Registration Data
During registration, participants were asked for their profession. Because they were not relevant for teaching purposes, data on gender, age, race, and ethnicity were not requested. Profession was categorized 2 ways: (a) trainee (students, residents, and fellows) versus practicing professional and (b) health professionals were categorized as dietitians/nutritionists, nurses (clinical nurse specialists, advanced practice nurses, and other nurses), physicians, social workers (including licensed professional counselors as well as social workers), health researchers, and others (including psychologists, dentists, lab technicians, physical and occupational therapists, and others).
Curriculum: Mind–Body Skills Training for Resilience, Effectiveness, and Mindfulness
The new MBST curriculum (http://mind-bodyhealth.osu.edu) was described to potential participants as a way to help health professionals become more personally resilient and to be more effective in helping patients manage stress. The training included up to 12 one-hour modules, 3 for each of 4 types of mind–body skills: (a) focused attention meditation (relaxation response), (b) mindfulness, (c) guided imagery and hypnosis (including autogenic training), and (d) positive affect–generating meditation (such as gratitude and loving-kindness). Although 2 modules included the word “introduction” in the title: “Introduction to Stress, Resilience, and the Relaxation Response” (one of the focused attention meditation modules) and “Introduction to Mindfulness” (one of the mindfulness modules), participants were allowed to complete the modules in any order, any number, and any combination.
Self-Reflection
Each module began with a case. This was followed by 1 to 3 self-reflection exercises, some of which were repeated at the end of the module. Self-reflection questions were included to engage learners and help them reflect on qualities that might be affected by mind–body training. The Introduction to Stress, Resilience, and Relaxation Response module included 3 items on a visual analog scale (VAS) for relaxation, stress, and resilience. It also included the Maslach Burnout Inventory at the beginning to help the learners understand the potential relevance of the curriculum to their personal well-being 9 ; because of its length, the Maslach Burnout Inventory was not repeated. In the other modules, most self-reflection opportunities were short, standard instruments to assess stress (10-item Perceived Stress Scale), 33,34 mindfulness (10-item Cognitive and Affective Mindfulness Scale–Revised in 1 module, 35 Mindful Attention Awareness Scale in another module), 36 resilience (Smith’s 6-item Brief Resilience Scale), 37,38 or empathy (empathic concern subscale of the Interpersonal Reactivity Index), and perspective taking (another subscale of the Interpersonal Reactivity Index). 39,40 For each standardized instrument, scores were automatically calculated within the Web-based program and stored on the project’s servers. The modules that provided the same questions for self-reflection at the beginning and ending of the module (before and after the other module content) provided a unique opportunity to evaluate the immediate impact of the training contained in that module. Participants were told that changes were not necessarily expected with a single practice session, but that by developing the habit of self-reflection in conjunction with mind–body practice, they might observe changes over time, as they would if they engaged in regular weightlifting.
In addition to the self-reflection questionnaires, to engage learners in active learning, most modules included open-ended questions throughout (eg, “Which practice do you think would be most appealing to your patients and why?” “Which practice would you like to try first?” “What barriers do you anticipate in using this skill and how might you address them?”); responses to these questions were not saved or scored.
Additional Module Content
The central features of each module were links to free, downloadable MP3 recordings of guided mind–body practices to support experiential learning. Audio recordings were paired with printed directions for the guided practices as well as links to publically available YouTube videos of mind–body practices to support experiential learning for both auditory and visual learners. The length of the mind–body practice recordings varied from 5 minutes (Introduction to Stress, Resilience, and the Relaxation Response) to 20 minutes (the longest option in the Introduction to Mindfulness: Body Scan Meditation).
Modules also included extensive clinically relevant didactic information with hyperlinks to research available on the US National Library of Medicine’s PubMed site and other public access Internet sites. There were also summary tables describing the physiologic and clinical effects of mind–body practices. In addition, modules offered links to other academic Web sites with additional data and/or free recordings of mind–body practices; tips for teaching mind–body skills to patients; and resources such as books, articles, and Web sites.
Data Management and Analysis
Although 12 modules were available, to ensure an adequate sample size, we analyzed data from the 5 modules that had at least 100 enrollees within the study period. Data were extracted from the project servers and downloaded into a Microsoft Excel spreadsheet for analysis. After cleaning and sorting, the data were de-identified for analysis using simple descriptive statistics and paired t tests.
The project was approved by the Ohio State University Office of Research Institutional Review Board as part of a larger evaluation of the impact of professional training in integrative health and wellness.
Results
Among the 1031 MBST registrants between May 1 and November 30, 2014, a total of 513 completed one or more modules and 42 registrants completed all 12 modules by November 30. The modules that had 100 or more completers by November 30 included Introduction to Stress, Resilience, and the Relaxation Response (n = 261), Autogenic Training (one of the guided imagery and hypnosis modules, n = 250), Guided Imagery/Hypnosis for Pain, Insomnia, and Changing Habits (n = 112), Introduction to Mindfulness (n = 112), and Mindfulness in Daily Life (n = 102) (Table 1).
Registrants for the Most Popular Modules.

For these 5 modules, the percentage of enrollees who were trainees ranged from 16% (Autogenic Training) to 28% (Guided Imagery/Hypnosis for Pain, Insomnia and Changing Habits). A variety of health professionals enrolled in each of the modules, including dietitians, nurses, physicians, social workers, and health researchers. Although participants could take any number of module(s) in any order, more than two-thirds of those who enrolled in Guided Imagery or Mindfulness modules had also completed the Introduction to Stress, Resilience, and the Relaxation Response module.
On the initial self-reflection exercises, enrollees reported high levels of stress and burnout and moderate levels of resilience. For example, at the beginning of the Introduction to Stress, Resilience, and the Relaxation Response module, the mean score on the 10-item Perceived Stress Scale was 18.4 ± 4.9, compared with Harris poll average scores of 12 to 15 in American adults. 41 For the same module, Maslach Burnout Inventory scores were above threshold for burnout for 56% on the Emotional Exhaustion subscale and for 33% on the Depersonalization subscale. 9,42 The average item score on Smith’s Brief Resilience Scale was 3.43 ± 0.6, which is slightly lower than the samples in which Smith reported normative data (3.53-3.98). 37
The visual analog scales in the Introduction to Stress, Resilience, and the Relaxation Response module improved significantly for stress (P = .02), but not for relaxation or resilience (Table 2).
Self-Reflection Scores at the Beginning and End of Each Module.
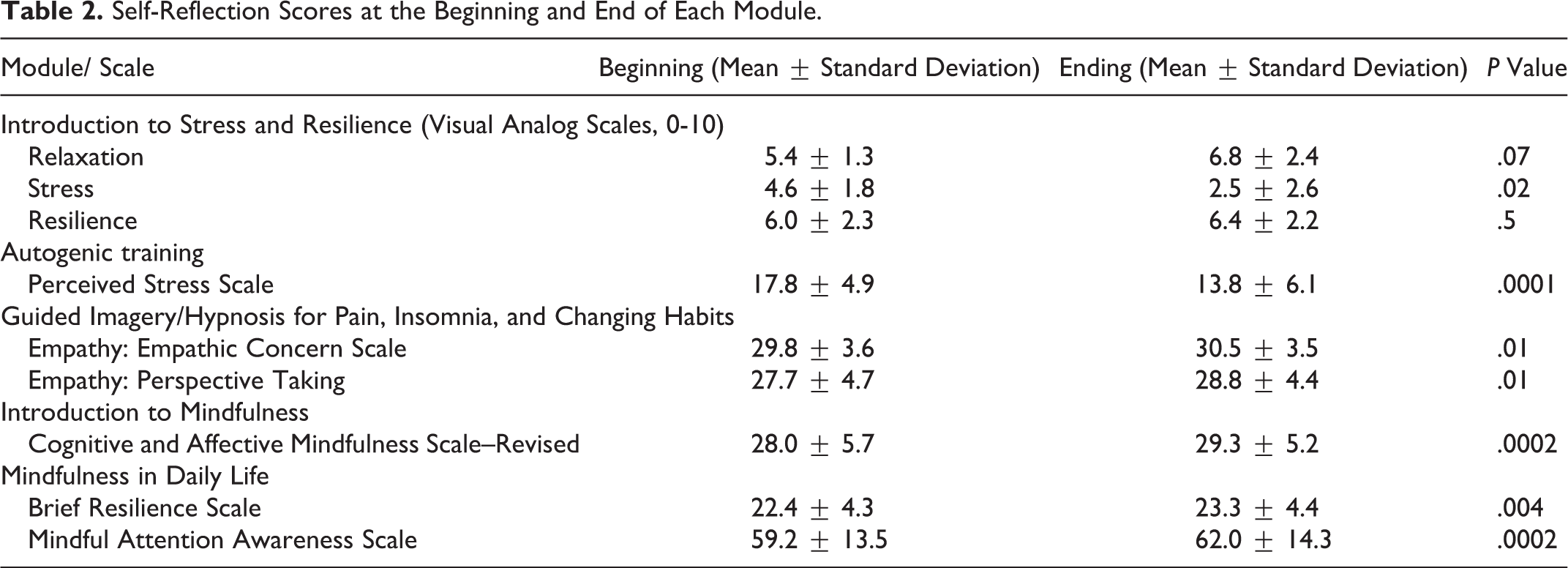
Scores improved significantly from the beginning to the end of other modules (Table 2). For example, for the Autogenic Training module, scores for perceived stress fell from 17.8 at the beginning of the module to 13.8 at the end after engaging in 15 minutes of audio-guided practice (P = .0001). Mindfulness scores improved significantly for both the Introduction to Mindfulness module and for the Mindfulness in Daily Life module (P = .0002 for both). Empathy improved significantly on both the Empathic Concern Scale and the Perspective-Taking Scale (P = .01 for both) for participants who completed the Guided Imagery/Hypnosis for Pain, Insomnia, and Changing Habits module.
Comments on module evaluations regarding planned behavior changes as a result of participating fell into 2 major categories: (a) plans to personally practice mind–body skills (49%) and (b) teaching the skills to patients or others (44%); only a few (7%) did not report any planned behavior change as a result of completing a module.
Discussion
This study examining the acute effects of brief, online MBST for diverse health professionals had 4 major findings. First, MBST was popular; enrollment occurred among diverse health professionals and trainees. Second, participants initially reported high levels of stress and burnout, suggesting that the training was attractive to those who might benefit from it. Third, the most popular modules included not just mindfulness, but a variety of mind–body skills, including Relaxation Response and Guided Imagery/Hypnosis; the only group of MBST that did not attract at least 100 registrants within the first 7 months was positive affect–generating meditation practices. Finally, completing even brief, 1-hour modules online outside of a group setting was associated with significant acute improvements in stress, empathy, resilience, and mindfulness.
This is one of the few studies to include a variety of health professionals and trainees, including dietitians and researchers. 43 Most studies of mind–body training focus on a single group of professionals or trainees such as physicians or nurses. 17,18,24,44,45 Although the project successfully recruited more than 1000 diverse registrants, only slightly more than 50% completed any modules, and of these, most completed only 1 to 2 of the available 12 modules. This low completion rate is consistent with our previous experience with online, noncredit, nonrequired, no-deadline elective training. 46 The low completion rates raises questions about why participants choose to continue or stop training, what factors might improve completion rates, and how the impact might differ for different “doses” or combinations of the curriculum. Although “only” 513 participants completed 1 or more modules, this is still a substantially larger number than the number of participants who enroll in most in-person MBST training programs, which typically have sample sizes less than 100 participants, and suggests that online training offers large numbers of diverse, busy, stressed health professionals a chance to at least “dip their toes in the water” of mind–body practices. Future studies could explore whether registering for online MBST increases later enrollment in more in-depth, in-person MBST or increases patient counseling or referred to MBST.
As in other studies of individual types of health professionals, the diverse participants in this project reported high levels of stress and burnout. More than 50% met criteria for burnout, which is similar to the rates of 40% to 60% reported in individual groups of health professionals. 8,12,47 –50 Participation by highly stressed health professionals means that the online MBST training is not simply “preaching to the choir” of professionals who already have high levels of mindfulness, empathy, and resilience 51,52 but is instead reaching its target audience of those whose skills could be improved with training. Because other strategies, such as duty hour restriction, have not proven universally effective in preventing burnout, 53 additional strategies are needed to help build resilience and manage stress to maintain empathy and mindfulness, and thereby improve the quality of care provided by diverse professionals. As health care undergoes rapid change, there is likely to be an increased need for accessible, affordable, attractive, nonstigmatizing MBST as part of a group of strategies to protect and promote clinicians’ health and caring skills.
The MBST offered in this project included multiple types of skills—mindfulness, relaxation response (focused attention meditation), guided imagery/hypnosis, and positive affect–generating meditation (eg, gratitude and loving-kindness–focused meditation). This differs from most previous types of MBST, which tend to focus on 1 type of mind–body skill, and offers unique insights into the types of mind–body topics that appeal to health professionals. Given their introductory titles, we were not surprised that the Introduction to Stress, Resilience, and Relaxation Response training and Introduction to Mindfulness modules were 2 of the most popular modules. However, we were surprised that Autogenic Training was the second most popular module. This raises the questions of why health professionals find certain topics more attractive than others and whether certain kinds of training are best suited to certain kinds of professionals. Was Autogenic Training popular because it was a less familiar, more novel topic, or was there some other reason for its popularity? Additional research is needed to better understand the reasons for selecting a topic like Autogenic Training while avoiding another topic such as loving-kindness meditation, particularly if educators are interested in fostering empathy, compassion, and loving-kindness among health professionals. Perhaps health professionals are more interested in developing skills they can use with patients than in practices they can use for their own well-being, or perhaps they already feel that they are compassionate and empathetic, and need to develop different skills to maximize their effectiveness. The questions for future research raised here point to the strengths and opportunities inherent in offering multiple “flavors” of mind–body skills.
The brief training offered online in this study resulted in significant acute changes in stress, mindfulness, empathy, and resilience. This is consistent with other studies of abbreviated in-person MBST. 21,26,30,31 Together, these studies suggest additional study questions about the optimal dosage combination of MBST. What dosage is best for whom? Furthermore, how is a program’s impact affected by previous training in yoga or a participant’s ongoing prayer experience? How long do effects last? How can training programs support ongoing practice? How much impact can be attributed to the group support offered by in-person training, and how does this affect ongoing practice or willingness to seek out booster training? How do initial stress and burnout levels affect the number of modules completed and the likelihood of ongoing practice? What is the long-term uptake, impact, and cost-effectiveness of different types, formats (online vs in-person) and dosages (number of hours) of MBST for specific types of health professionals? These questions are important and will require additional prospective, controlled trials.
Although this study offers several unique and important observations, it also has several limitations. It was conducted at one academic institution in the Midwest, and needs to be replicated in community settings elsewhere. It has a large sample size, but the sample is quite diverse, and an even larger sample is necessary to determine differences between professions and between trainees and practitioners. As a cohort study of an ongoing educational elective, this project did not randomize participants and there was no control group, so there may be self-selection bias, limiting generalizability. Because it was an elective, we cannot generalize the results to mandated or required programs. As an online project, it included standardized self-report measures, but future studies would benefit from use of objective measures of improvement in actual communication and care.
Despite these limitations, results of this study suggest that online training in mind–body skills is attractive to diverse health professionals struggling with high levels of stress and burnout, and that such training can acutely improve clinically relevant qualities such as empathy and mindfulness. Additional research is warranted to compare the cost-effectiveness of online with in-person MBST to improve mindfulness, empathy, occupational health, and the quality of care provided to patients.
Footnotes
Acknowledgments
We are grateful to the Deans of Medicine, Nursing, and Social Work; the residency directors for Pediatrics, Family Medicine, Hematology and Oncology; and the PhD program in Dietetics for informing their students and faculty about the online mind–body skills training course.
Author Contributions
KJK conceived of the project and drafted the manuscript. MK was the webmaster for the project, scored the standardized instruments, and reviewed and edited the manuscript.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This project was funded in part by an internal Ohio State University College of Medicine Alumni gift of $1000.
Ethical Approval
This project was approved by the Ohio State University Office of Research Institutional Review Board: 2013B0611.
