Abstract
Background
Fragility hip fractures are a common and often devastating event, and a shared care approach between orthopaedics and geriatrics can improve patient, health service and quality of care outcomes. The aim of this cross-sectional survey, administered to all hospitals caring for patients with acute hip fracture, in New South Wales (NSW), Australia, was to establish current models of care (e.g. shared care or other), and barriers and facilitators of best care.
Methods
A combination of quantitative and free-text data was collected. In total, 30/36 (83%) hospitals responded, with representation from all 15 state local health districts.
Results
Overall, 21/30 had a formal orthopedic surgery/geriatric medicine shared care model; orthopaedic surgery admission with routine (ortho)geriatrician input was commonest (13/21). Multiple barriers to optimal hip fracture care were identified along the various stages of the national guideline-recommended care pathway. Common barriers reported included staffing deficits (for pain assessment, fascia iliaca block administration) and gaps in service structure (lack of specialist services for refracture prevention). Multidisciplinary meetings were in place to enable best care and to promote team communication, but were impeded by absence of relevant team members (8/16). Free-text themes of enablers of good practice included clear escalation and hand-over processes, multidisciplinary communication strategies, and guideline-aligned clinical pathways.
Conclusion
Moving forward, addressing common barriers such as staffing and knowledge deficits, and harnessing enablers of good practice such as multidisciplinary communication and support, combined with effective implementation strategies, are likely to optimize care for patients with hip fracture.
Introduction
Hip fracture is a common and often devastating event, and the most costly fall-related injury in older people. In Australia and New Zealand, 16,395 patients were included in the 2022 Australian and New Zealand Hip Fracture 1 ; rates in the US, Canada and Europe are likewise high, with upwards of 300,000 hip fractures in the Unites States each year. 2 Two thirds of patients presenting with hip fracture are female; median age in Australia is 84 years. 3 Comorbidity, cognitive impairment, frailty and dependency are common in these patients.1,3-6 Patients sustaining a hip fracture are at high risk of poor outcomes, including in-hospital adverse events such as delirium.,3-7 and long-term decline in mobility and function compared to pre-fracture status,8-10 which may require residential care placement.1,3,6,10 Hip fractures can dramatically reduce older patients’ life expectancy,1,3,10 and the risk of death is increased 3-4-fold within one year of hip fracture, compared to the general population. 11
Despite a plethora of guidelines internationally highlighting the principles of high quality hip fracture care, and the endorsement of the importance of an orthogeriatric approach to care for such patients,6,8,12-15 registries and audit data continuously indicate that care is neither standardised nor optimized.1,16,17 An orthogeriatric approach to the care of patients with hip fracture is recommended, and evidence suggests that this can reduce surgical delays, hospital length of stay and mortality.8,12,14,16,18-20
As in other jurisdictions, the importance of hip fracture care is increasingly recognized in Australia. This survey was developed as part of a larger body of work leading to the generation of an evidence-based Orthogeriatric Clinical Practice Guide, 21 aligning with state priorities as highlighted by the New South Wales (NSW) Agency for Clinical Innovation’s priority of Leading Better Value Care for people with Hip Fracture (LBVC Hip Fracture). 22 This program aims to reduce unwarranted clinical variation, improve patient assessment, management and experience, and ensure effective and efficient care.
In this context, the purpose of the current survey was to establish what models of orthogeriatric/hip fracture care are used in hospitals across NSW, Australia, and barriers and facilitators of best care for patients with hip fracture. We sought to explore the existing provision of care to patients with hip fracture, models of care, and barriers and facilitators of best care, in a state-wide survey of hospitals providing acute care to patients with hip fracture in NSW, Australia’s most populous state.
Methods
This state-wide cross-sectional survey of hospitals caring for patients with acute hip fractures was developed as part of a larger body of work leading to the generation of an evidence based Orthogeriatric Clinical Practice Guide. 21 New South Wales is Australia’s most populous state, with a population of just over 8 million, 23 stretching along the eastern cost between Victoria and Queensland, and South Australia, and encompassing Australian Capital Territory in its south-east; NSW hospitals offer surgery to almost 6000 patients with hip fracture each year.1,22
The survey was developed de novo by a collaborative multidisciplinary expert group, comprising clinicians and other healthcare personnel, supported by the Executive team at the Agency for Clinical Innovation, NSW. Questions were informed by the Australian and New Zealand Hip Fracture Registry (ANZHFR) audit data 1 and the national Hip Fracture Care Standard in existence at the time (2016 version), which has since been revised, 12 and refined by expert consensus. Through assessment of ANZHFR data and stakeholder consultation with multidisciplinary clinicians and healthcare managers, potential areas for improvement in hip fracture care were identified and explored in the survey. The survey was piloted with senior hip fracture clinical care coordinators (similar to target population) prior to finalization, in an iterative process until developers and pilot testers were satisfied with final version. Questions, numbering 77 in total, related to aspects of recommended hip fracture care, the models of care provided (e.g. shared care or other, and type of shared care if yes), whether and how length of stay is addressed, and barriers to and facilitators of recommended best practice. The final version is available as an Appendix (Supplemental Material).
In order to determine case load for individual responding hospitals, annual hip fracture numbers were drawn from existing ANZHFR data. Hospitals were also segregated according to case volume (site number of fractures per year < [‘lower volume’] or ≥ [‘higher volume’] group mean).
Inclusion criteria included all key hip fracture care contacts as identified by the Agency for Clinical Innovation register for Leading Better Value Care leads at all clinical sites which care for patients with acute hip fractures in NSW (N = 36), across all (15) of NSW’s local health districts (LHDs), which formed our purposive sample. There were no additional sample size calculations. Each site was permitted to respond to the survey once, and cross-disciplinary input from local stakeholders was encouraged in the completion of survey questions. The survey was made available in electronic and/or paper form, for completion as per respondent preference. The survey was disseminated December 2022-March 2023, with reminder emails to encourage uptake. No formal marketing or advertising were conducted prior to survey launch. Data were held on secure servers and only research personnel had access.
Data are de-identified for purposes of the current study. A shared care model was defined as joint patient responsibility between Orthopaedics and Geriatric medicine for all older hip fracture patients from admission. Free text responses from the questionnaire were exported verbatim into Excel®. A conceptual content analysis approach was utilised to code these. This involved manual coding of explicit terms (by 2 authors), sorting the free text into themes, adapting these themes as needed as additional data were coded, until final themes emerged.
The study is reported in line with the Checklist for Reporting of Survey Studies. 24
Statistical Analyses
Descriptive statistics are presented. Simple comparisons of distribution were performed comparing metropolitan and regional/remote hospitals, and higher vs lower hip fracture volume hospitals. Missing data for any individual questions were not imputed, and were thus not included in analysis. All items were equally weighted, and propensity scoring was not conducted.
Informed Consent
Participants provided online consent via the secure survey platform, but were not required to submit hard copy signatures.
Results
Participating Hospitals and Their Models of Care
Thirty hospitals (12 metropolitan and 18 regional/remote) out of 36 eligible responded to the survey (83.3% response rate), with representation from all 15 of our state’s Local Health Districts, although not all respondents completed all sections of the survey; response rate to individual questions varied from 28-30/30 respondents (93-100%; Figure 1). The six hospitals which did not respond comprised a mix of regional/rural (N = 4) and metropolitan (N = 2) hospitals, with a mean number of annual hip fractures of 150 (data for 5 hospitals, ANZHFR, 2023
1
). Mean number of annual hip fracture patients for the responding hospitals, determined as per the ANZHFR data (not survey data), was 149.8 (SD 92.2), with similar numbers seen for metropolitan (mean 156 per annum) and regional/remote hospitals (mean 145). Proportions identifying barriers to best practice hip fracture care recommendations (n = 30 hospitals). *N = 28 for these specific questions; **medical cover = geriatric medicine/medical/physician/GP.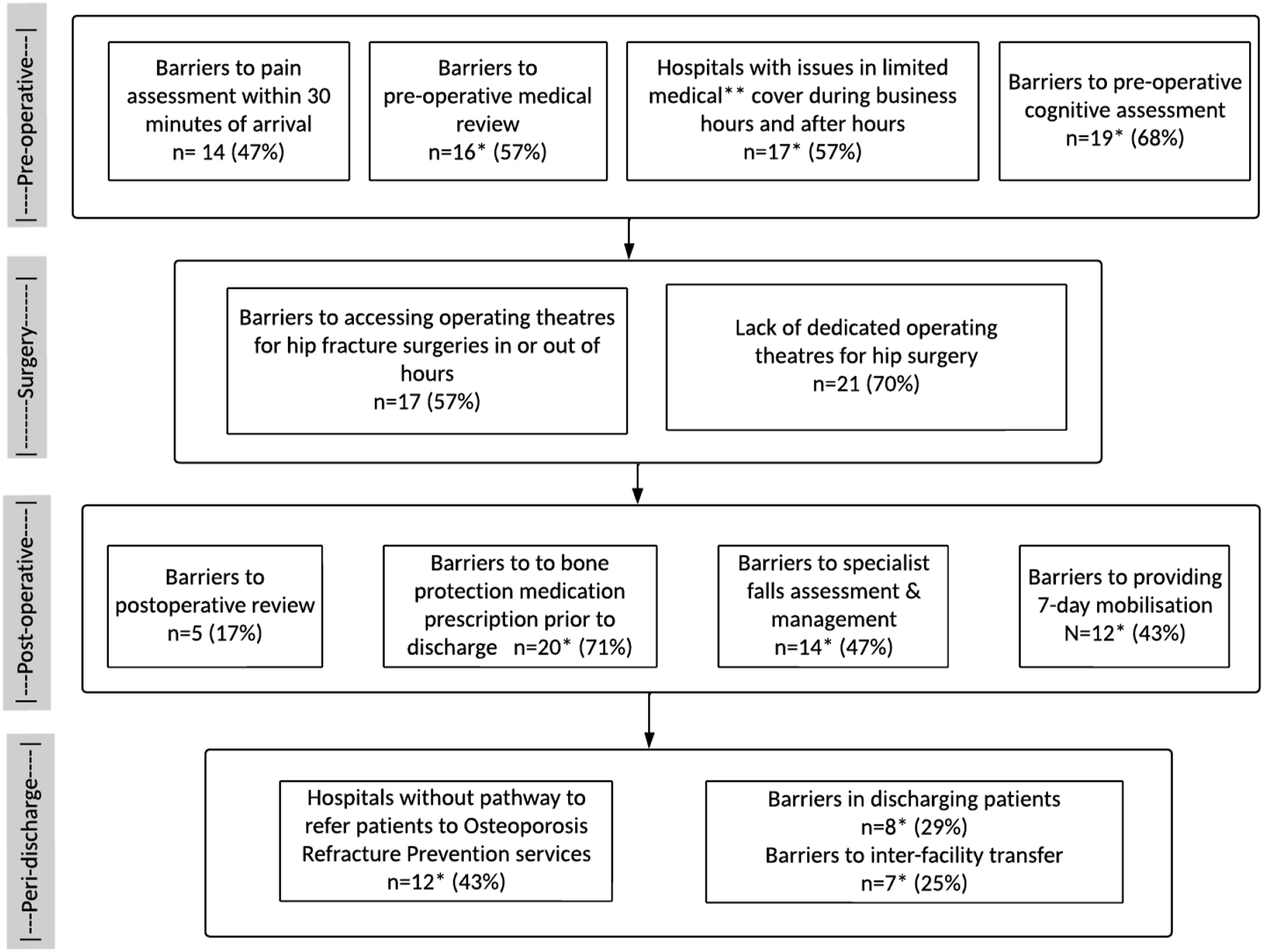
Nine hospitals (32%) reported the absence of a shared care model (for hip fracture patients, with patients cared for by the orthopaedic surgical team alone (Figure 1). Those with a shared care model (N = 21) in place were still largely orthopedic-surgeon led with routine (ortho-)geriatrician review (13/21)- noting that review availability was usually within weekday business hours (rather than after hours). Remaining models included other (ortho-) geriatrician involvement (i.e. not routine review; n = 4), shared-admission orthogeriatric model (n = 3), and geriatrician-led (n = 1). Hospitals using shared care models were fairly evenly distributed between metropolitan hospitals (N = 11) and regional and remote hospitals (N = 10), but proportions showed geographic variation, with 8 of the hospitals which did not have a shared care model being located in regional/remote regions.
Looking at other aspects of how care was provided, in terms of pre-operative optimization, 15 hospitals reported this happened at the ‘receiving site’, an additional 3 hospitals reporting this happened at a combination of transferring and receiving sites, and 3 hospitals reporting not applicable (no/few transfers); the remainder reported optimization happened at the transferring end.
Barriers Reducing Alignment with Best Practice Guidelines
Figure 1 illustrates the various points at which barriers to optimal assessment and management of hip fracture patients were encountered, along various stages of the guideline-recommended care pathway. Barriers were commonly reported at almost all stages of the patient journey: 17 (61%) of hospitals reported barriers to administering a fascia iliaca block, 19 (68%) faced barriers to pre-operative cognitive assessment, and 12 (43%) reported barriers to 7-day mobilisation of patients.
Not all respondents detailed the nature of the barriers. But, staffing issues were commonly cited barriers to optimal care, mentioned by 7/8 hospitals reporting barriers to suboptimal pain assessment and 4/4 hospitals reporting barriers to fascio-iliaca block (FIB) administration, with other knowledge and literature deficiencies (3/4) also contributing to suboptimal FIB use.
Not having a dedicated operating theatre for hip fracture surgeries was raised as a barrier by 78% of the respondents.
Lack of knowledge was the main barrier in almost two thirds (63%) of the 19 hospitals reported issues with pre-operative cognitive assessment and in 6/8 hospitals reported barriers in routine post-operative delirium assessment. Less common reasons for lack of compliance with the clinical guidelines were: absence of protocols (range 6% to 26%), staff non-compliance with completion of assessments (16%), lack of knowledge of the literature, and need for training on the procedures. Shortage of specialist staff for formal falls assessment and lack of time were the commonly mentioned barriers in 7/14 hospitals identified this issue citing staffing (52%) and service structure (16%) as the main barriers.
Reasons mooted for barriers to post-operative medical review were overstretched medical trainees during business hours and lack of availability of relevant specialists after hours, on weekends and public holidays. Only one hospital reported not having regular mechanism for communicating with multidisciplinary teams, and 28% reported not incorporating nutrition as part of their hip fracture model of care. However, 16/28 (57%) uncovered multiple challenges of these multidisciplinary meetings, dominated by lack of representation from all needed parties (50%, 8/16), in particular senior medical/orthopedic, rehabilitation or pharmacy staff, followed by lack of structure and time.
In terms of refracture prevention, the 20 hospitals reported barriers to bone protection medication prescription prior to discharge, citing reasons such as role delineation perceptions (the perceived responsibility of the community general practitioner for initiating same) (55%), clinical uncertainty (concerns about low vitamin D delaying initiation of antiresporptive therapy) (45%), clinician judgment (surgeons’ preference to delay) (25%), workload (heavy workload of junior doctors) (20%), and lack of knowledge or awareness of these medications (15%). Fourteen hospitals (14/29, 47%) reported barriers to specialist falls assessment and management, most commonly due to staffing deficits (8/14) and service structure deficits (6/14). Just under half (47%) of responding hospitals reported not having a pathway for referring hip fracture patients to Osteoporosis Refracture Prevention services (Figure 1), with reasons given including lack of specialist services in the area (7/14), with some respondents noting the need for several hours of travel to the nearest available service, or telehealth options which are not accessible to all patients/consumers.
At the end of hospitalization, staff from eight hospitals reported that insufficient resources for placement in residential aged care, different criteria for private or public rehabilitation service entitlements, cognitive impairment and medically unwell patients precluded appropriate or timely discharge. There were five hospitals where patients or caregivers were not routinely provided with an individualized care plan, as recommended in then-current national guidelines (updated 2023). 12 Reasons cited included staff workload, lack of awareness and lack of ownership of the responsibility for patient education.
Barriers Based on Metropolitan vs Regional/Remote and Case Load
On simple comparison of proportions, only the reported presence of barriers to falls assessment differed between metropolitan and regional/remote hospitals (22% metropolitan vs 77%, P = 0.04 Fisher’s exact test).
When hospital were segregated by higher vs lower case volume, more ‘higher volume’ hospitals (≥149.8 cases per year) had an osteoporosis refracture prevention path than lower volume hospitals (80% vs 36%, P = 0.047 Fisher’s exact test). No other proportional differences were observed in terms of reporting barriers to various steps in the patient journey.
Enablers of Adherence to Evidence-Based Guidelines
Many hospitals (67%) had a care pathway which spanned arrival in the emergency department right through to the post-acute care ward; 13% had a pathway only for the emergency department, 7% (2/30) only for the acute ward, and 1/30 (3%) only following transfer from the tertiary hospital; 4 hospitals (13%) had no formal care pathway. All 30 responding hospitals reported the existence of a clear escalation and handover process between clinical areas, with a third (10/30) reporting this in the way of multidisciplinary meetings. Others took the form of either nursing handovers, nurse leaders (nurse unit manager or clinical nurse consultant) taking responsibility, and/or allied health staff (physiotherapists/occupational therapists) or junior doctors liaising with geriatricians. Only one hospital reported no designated clinician for this task.
Survey respondents highlighted enablers of regular multidisciplinary communication, consisting of daily whiteboard meetings (24/28, 86%), ward rounds (10, 36%) and weekly case conferences (9, 32%). It was reported that six hospitals were making efforts to reduce prolonged length of stay, through interventions such as prompt identification and management of acute medical issues, advocacy for early access to onsite rehabilitation, introduction of clinical pathway(s) to promote adherence to guidelines, a dedicated operating room, and incentives to reduce bed blocks.
Strategies were also proposed to facilitate 7-day/week mobilization including 7-day/week physiotherapy coverage (43%), nursing staff mobilising patients (29%), use of allied health assistants (21%) and less often resorting to physiotherapy students (7%). Potential solutions to overcome the barriers to pre-discharge bone protection medication prescription included use of a protocol for junior doctors, hospital initiation with handover to community doctors via the discharge summary, and addition of the medications to the State formulary or District subsidy to ensure medication availability within the facility.
Overall, 16/28 (57%) hospitals reported making a focused effort to address (long) length of stay, with 13/16 reporting effective (1/13 ‘very effective, remainder ‘somewhat effective’), one reporting ineffective, and two others ‘too soon to tell’. Initiatives ranged from implementation of standardized care pathways, to ensuring dedicated theatre time, to smoothing transfer processes to rehabilitation beds, with two centers noting the importance of multidisciplinary decision making in trying to address length of stay.
Discussion
In a real-world survey of hospitals across Australia’s most populous state, barriers were commonly reported at multiple phases of the patient journey after hip fracture. Major stumbling blocks to guidelines-adherent care included workforce limitations and service structure obstacles. These included assessments, prescribing, drug administration and referral activities, and were noted to be restricted by the shortage of specialist staff and service structure barriers, while limited access to operating theatres posed significant impediments to timely surgical intervention.
The identification of multiple, multi-level barriers is perhaps not surprising to clinicians and managers, who deal with barriers to best care in everyday practice. Despite the existence of national recommendations for hip fracture care embraced by key healthcare organisations here,8,12 as elsewhere, ongoing disparities in care provided are evident. 1 In Australia and New Zealand, bi-national registry data suggest that here in Australia and New Zealand, one third of patients with hip fracture do not have their cognition assessed pre-operatively, and opportunities to mobilise or receive post-acute care rehabilitation are variable. 1 Across the globe, deficits are noted, 16 including in other large national registries such as those in Ireland,6,17 and the United Kingdom (UK).25,26 Key markers of quality of care such as time to surgery, complication rates, hospital readmission rates and length of stay can vary considerably. At the same time, and somewhat reassuringly, initiatives to standardise and improve care continue to be described, with the establishment and revision of national evidence-based guidelines in multiple countries, and development of international collaborative networks 27 to opimise the care for patients with hip fracture. On simple proportional comparisons, regional/remote hospitals more often reported barriers to falls assessment, and lower-volume units less often had a formal osteoporosis refracture prevention pathway. It is interesting to note that, in this survey, reported prevalence of barriers to other steps along the care pathway were largely similar irrespective of geography or case load. However, in-depth exploration of other differences in how care is provided in specific regions or based on patient volumes was beyond the scope of this study, and would be of interest.
In addition to providing a contemporary picture of barriers and enablers of recommended care for patients with hip fracture, the findings from this survey informed the development of a pragmatic guide for clinicians and managers providing hip fracture care, with the roll-out of an orthogeriatric hip fracture care clinical practice guide. 21 The data from the current survey were used to determine enablers and barriers in hospitals across NSW managing hip fractures, as well as key issues and aspects of care which are being managed well. This allowed the development of informed guidance for the management, including cognitive impairment and delirium assessment, and discharge planning, for patients who have experienced hip fracture.
Previous reviews have called for more integrated orthogeriatric care models (Midleton, 2018), 28 acknowledging the intricacies of culture change management, governance, and financial incentives. Adequate resourcing is likely to be key. Even in units with formal shared care models, orthogeriatrician specialist input is often minimal at weekends or overnight. A Canadian database study revealed that overstretched resources were more often the culprit for non-adherence to the 2-day to surgery benchmark, rather than clinical (contra-)indication to surgery. 15 In the UK, performance incentives have been proposed as a potential solution to overcoming organizational and other factors driving practice variation and guideline deviation, 29 where implementation of the Best Practice Tariff (BPT) appears to have been associated with reduction in mortality. 30 In Ireland, a performance incentive has been in place since 2018, where compliance with all seven Irish hip fracture standards for any individual patient, plus two additional standards regarding data quality and governance, earns the treating hospital a small monetary reward. 6
Addressing care fragmentation, such as that found in our survey, is an important step in improving patient outcomes, and may be overcome by collaborative models of care which embrace a sharing of care between orthopaedic surgeons and geriatricians/physicians, as showcased by an orthogeriatric model of care.18,20,31
Implications for Practice and Research
Moving forward, clinicians and healthcare managers alike need to be aware of local barriers and strengths and use these to work towards improved care for patients with hip fracture. Studies such as our own give a snapshot of care and factors affecting this, and, in conjunction with evidence-based recommendations, can be used to better inform local policies and interventions to improve care. While it is important to acknowledge barriers, sometimes we just need to ‘get on with’ best care and figure out efficient ways of providing this. Future research should build on the solutions proposed by clinicians on the ground by implementing and evaluating locally relevant co-designed projects cognisant of local strengths and weaknesses. These will be complemented by further mixed methods investigation into the views and lived experiences of patients and carers, especially as these may evolve in the context of newer clinical practice models. Economic evaluations of the different models of care could also shed light on the most cost-effective approaches in low-resource settings in the developed world.
Limitations of This Study
Our survey was confined to a single -though the most populous- state in Australia and its findings cannot be generalized to other health systems. While the survey was developed with multi-stakeholder input, and was piloted prior use, it had not been previously validated. We used a purposive sample, and all hospitals providing care to patients with hip fracture were eligible for inclusion; no further sample size testing was done. The response rate was less than perfect, but is better than the standards of the survey-based studies in the medical literature, and we think is probably representative of clinical experience. Our 83% (30/36) response rate was also subject to some incomplete responses (response completeness rates: 93-100%). While cross-disciplinary collaborative input was encouraged when, individual perspectives might have missed some details of the surveyed care provision, and in seeking binary responss- although complemented by free text options- we may have missed some of the granularity of impediments to best care. We also acknowledge that shared care does not always represent an equal sharing of patient management, and orthogeriatric support is often confined to ‘working’ hours. While fairly inclusive, our survey has still not captured relevant aspects of care like advance care planning and cultural appropriateness of care, which deserve further research.
Nonetheless, the findings from this study add granularity to the big picture data captured in national registries and allowed identification of barriers and enablers of best practice. At a local level, options such as site-specific audits will facilitate targeted quality improvement initiatives relevant to that particular setting. Local data collection, review and governance, are needed to support individual units to achieve best practice and help translate recommendations into clinically and locally appropriate plans. Clever staff reconfiguration and educational endeavours to overcome knowledge deficits may help support some aspects of care, but given competing priorities in a clinical setting, local initiatives are likely to be maximised in the context of higher level resourcing and support. Furthermore, to be effective, change implementation is likely to require multifaceted intervention, for example incorporating aspects such as staff education, decision support systems, clinical audit and opinion leaders; existing evidence is less supportive of single-faceted interventions such as audit/feedback, computerized decision support and opinion leaders. 32 Identifying barriers and facilitators in many cases may be the first step in improving care for hip fracture patients, as was evident in a recent systematic review which identified key features of improvement programs which successfully improved time to surgery in patients with hip fracture. 33 Change implementation support programs and targeted education and coaching may prove a helpful resource local services on their quality improvement path. Platforms which support patient and caregivers to report on their experiences, such as the co-designed Health Outcomes and Patient Experience (HOPE) which is being implemented on a phased basis across NSW, will enhance our understanding of the lived experience for these patients. 34
Conclusions
In this survey of urban and regional/remote hospitals providing acute care to patients with hip fracture over a large geographic area in Australia, we identified multiple barriers- commonly related to staffing and/or lack of knowledge/education- and enablers, often related to multidisciplinary communication and collaboration, at multiple phases of the patient journey. Addressing and building on these factors are likely to need a combination of local measures and higher level support. Integration of guide-line-recommended assessment and care components requires resourcing and local identification of strengths and barriers but may be worth it if it translates into real benefits for older patients with hip fracture.
Supplemental Material
Supplemental Material - Current Care and Barriers to Optimal Care of People With Hip Fracture: A Survey of Hospitals in New South Wales, Australia
Supplemental Material for Current Care and Barriers to Optimal Care of People With Hip Fracture: A Survey of Hospitals in New South Wales, Australia by Danielle Ní Chróinín, Zsolt J. Balogh, Jennifer Smith, Glen Pang, Jessica Wragg and Magnolia Cardona in Geriatric Orthopaedic Surgery & Rehabilitation.
Footnotes
Acknowledgments
The authors would like to thank the hospitals/respondents who contributed to the survey, and the members of the overseeing ACI Orthogeriatric Model of Care working group.
Author Contributions
Conceptualization, DNíC, JS, JW, GP; methodology, DNíC, JS, JW, GP; investigation, DNíC, JS, JW, GP, ZJB; formal analysis, JW, DNíC, MC.; data curation, JW; writing—original draft preparation, DNíC, MC; writing—review and editing, DNíC, JS, JW, GP, MC, ZJB; project administration, JW. All authors have read and agreed to the published version of the manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Statement
Data Availability Statement
Data are potentially available upon reasonable request. The data herein comprise deidentified data held within a database at Liverpool Hospital, New South Wales, and could potentially be made available with ethics committee approval for distribution/use beyond the current study.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
