Abstract
Introduction
This article introduced the management of a case with severe left lower extremity pain and forced hip flexion after posterior lumbar interbody fusion and a final diagnosis of left psoas hematoma.
Materials and methods
Here we reported a case of a 65-year-old female received posterior lumbar interbody fusion (PLIF) for L4-L5 spondylolisthesis and L4 instability. On the postoperative day one, the hemoglobin level decreased from 108 g/L to 78 g/L. Meanwhile, the patient presented low back pain and inner thigh radiating pain (VAS pain scale = 8). The pain was so severe that it could be barely relieved by keeping left hip in flexion position. On the postoperative day 6, the pain was still severe even after taking mecobalamin, ankylosaurus, dehydrant agents and central pain relievers(VAS pain scale = 9). Computed Tomography indicated a left intramuscular hematoma image extending down to the left iliac fossa. Active hemorrhage of lumbar segmental arterial was detected by B-ultrasound. The patient then received vascular embolization under angiography on the postoperative day 7.
Results
The pain in the low back and inner thigh were significantly relieved after the procedure (VAS3-4). On the postoperative day nineteen, the left hip can be fully extended, but the patient was still not able to stand on left leg without a walking stick. On the postoperative day 27, she was able to walk independently.
Discussion
The main reason for the complication was the second conical dilation channel slipped and entered the lateral side of the vertebral body along the transverse process. After timely embolization, pain was significantly relieved and muscle strength was improved.
Conclusions
Angiographic embolization is an effective treatment for psoas hematoma after posterior lumbar interbody fusion.
Keywords
Posterior lumbar interbody fusion (PLIF) is one of the more common and effective surgical methods for the treatment of lumbar spondylolisthesis and lumbar spinal stenosis. It provides adequate removal of bony or non-osseous tissue that compressed nerves and strong internal fixation. Due to the dissection and disruption of local spinal anatomy, there can be short-term or long-term complications. Short-term complications include nerve injury, vascular injury, and infection of the surgical site. Long-term complications include degeneration of adjacent segments and loosening of internal fixation. Whether these complications are effectively managed will directly affect the patient’s recovery process and quality of life.
Vascular injury is a rare complication after PLIF, mainly including acute common iliac arteriovenous fistula and delayed abdominal aortic pseudoaneurysm. 1
Here we reported a case of a patient with severe left lower extremity pain and forced hip flexion after the PLIF operation and shared our experience with psoas hematoma complication management.
Materials and Methods
A 65-year-old woman with untreated low back pain felt that the pain was aggravated half-year ago. She also developed pain, weakness and numbness of both lower extremities, ranging from the lumbosacral region to the outer side of the thigh and the calf. Depending on CT imaging and physical examination, L4-L5 spondylolisthesis with lumbar 4 vertebral instability was diagnosed. Under general anesthesia, PLIF(L4-L5) were performed.
Postoperative Symptoms and Treatment


CT of the lumbar spine showed the left intramuscular hematoma (arrow) extending down to the left iliac fossa.
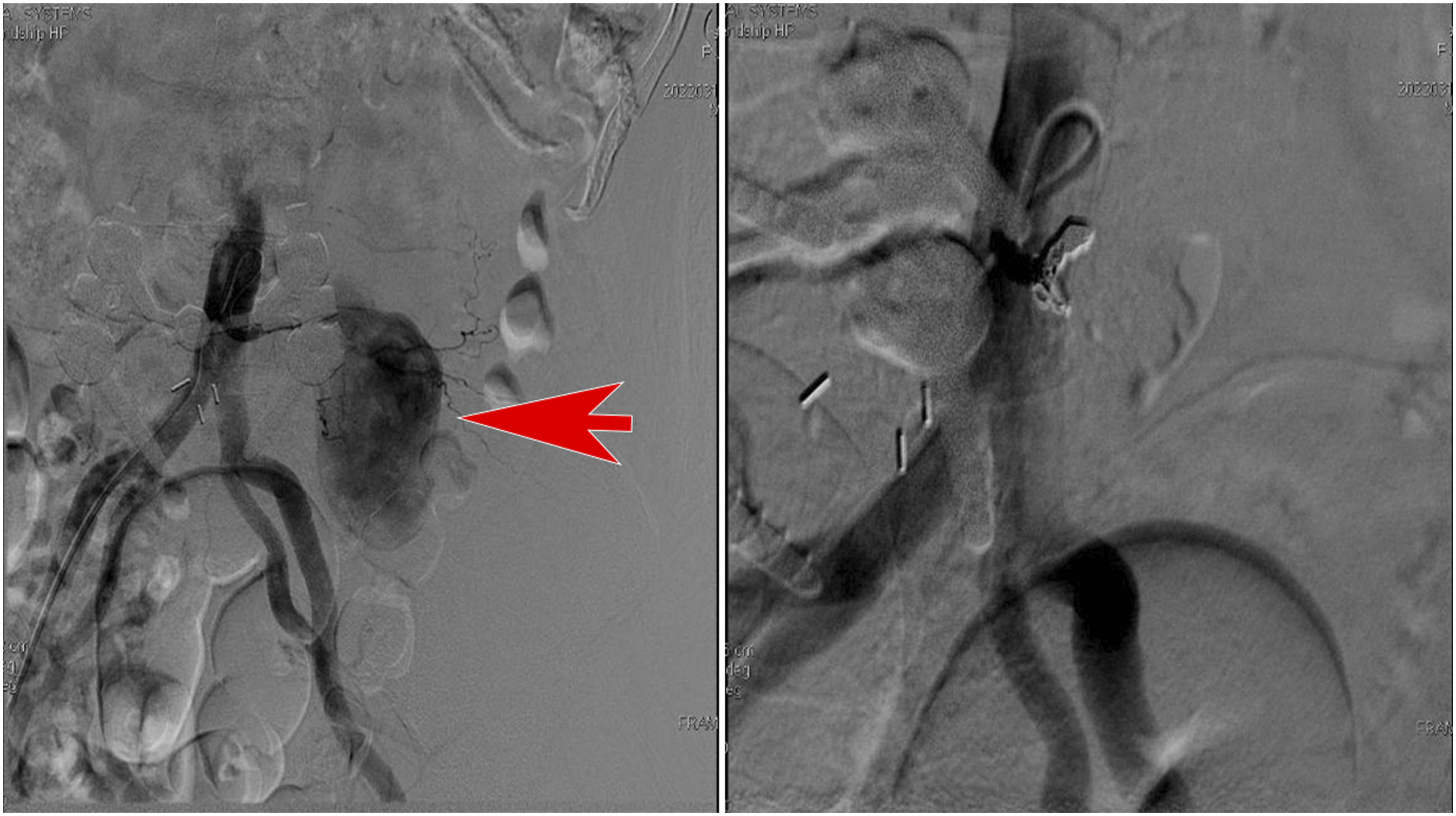
Lumbar segmental artery embolization was performed under angiography. Right: preoperation, Left: postoperation.

The left intramuscular hematoma was totally absorbed after 4 months after embolization.
Discussion
The main cause of psoas major hematoma is vascular injury during PLIF procedure. Vascular injuries are rare, with the incidence of .01% −1%, but potentially life-threatening complications in thoracic and lumbar spinal surgery of which the overall mortality rate ranges from 15% to 65%.2,3
The common sites of vascular injury caused by lumbar surgery including abdominal aorta, iliac artery and lumbar segmental artery. Risk factors of abdominal vascular injury were summarized by Liu et al 4 as (1) lumbar operation history which may lead to adhesion between retroperitoneal vessel and vertebral body (2) chronic disc disease which causes degeneration of the annulus fibrosus and anterior longitudinal ligament (3) improper use of pituitary rongeur (4) improper intraoperative position of patient (5) pressure to the abdomen in the prone position which shortens the distance between retroperitoneal vessel and vertebral body (6) proliferative spurs of anterior longitudinal ligament which may puncture major vessels (7) anterior longitudinal ligament defect (8) the abdominal radiotherapy history (9) hernia-towards-abdomen disc and (10) anatomical variations.
Abdominal aorta injury caused by lumbar surgery could be very dangerous. Sahinoglu M et al 5 reported one patient suffered injury of the left main iliac artery. The patient became hypotensive near the end of the operation. The incision was quickly closed and the patient was turned into supine position. Emergency abdominal ultrasound, computed tomography (CT), and CT angiography revealed an injury of the left main iliac artery, which was then repaired by endovascular stenting.
Ghazwan et al 6 presented a case of postoperative discoscopy immediately developed acute, sharp and burning pain in the left leg with diminished distal pulsation of dorsalis pedis, popliteal and femoral which was partially relieved on hip flexion. Urgent consultation with a vascular surgeon and a computed tomography angiography confirmed a vascular injury of the left iliac artery and vein near the bifurcation. After urgent retroperitoneal exploration of the left iliac vessels and primary repair with synthetic graft, the patient was successfully rescued. In this case, vessel injuries were caused by using the Tubular system and bionate instruments, which were longer than the usual kerrison used in open surgery.
Early and timely diagnosis of PLIF-related psoas hematoma is quite difficult. Lower extremity pain is not specific and in most cases was considered to be caused by edema of the nerve roots. Opposite to hematoma induced pain, nerve root edema induced pain can be significantly improved after a period of pain relief, nerve detumescence, and nerve nutrition therapy.
In this case, the pain was still obvious on the postoperative day six (VAS 8-9) after hereinbefore mentioned treatments. In addition, forced flexion of hip is a specific sign of stretched or inflammatory stimulation of the psoas. If the pain of the lower extremity does not relieve after operation, it is also necessary to consider whether it is related to the compression of the nerve root caused by the deviation of the internal fixation position by CT scan. In this case, the patient only lost about 260 mL (6.5 g/L) of blood during the operation and on postoperative day one, but the hemoglobin level decreased from 108 g/L to 78 g/L, indicating that the patient still has active bleeding. A cystic mass in the psoas major muscle was found with CT scan. At the same time, the screw in L4 and L5 are in right position (Figure 4). the cause of the patient’s lower extremity pain and passive flexion of the left hip was diagnosed as a psoas hematoma. The screws in L4 and L5 are in right position.
Tha similar case was a patient who suffered from hemorrhage abdominal pain and bloating after surgery. 7 This patient was initially suffering from neurostimulation in the right lower limb. As the psoas hematoma increased, the pain became persistent and more intense. Another patient had no major postoperative complications until the sixth day when the patient re-presented with acute leg pain and weakness. Following a multidisciplinary (MDT) discussion and an MRI showed a large haematoma at the right psoas muscle. 8 Therefore, it is very challenging to detect lower lumbar segmental arterial injury intraoperatively. If not detected early, it can cause massive bleeding, which can lead to serious consequences. Therefore, an early detection of postoperative bleeding caused by vascular injury is critical for providing timely and efficient treatment.
After reviewing the literature, the main mechanism of vascular injury caused by posterior thoracolumbar surgery are almost all sustained by impingement or avulsion of the artery leading to a delayed hemothorax.9-12
The main reason for our case is during the operation of the patient’s left side screw implantation, the second conical dilation channel slipped and entered the lateral side of the vertebral body along the transverse process. The abdominal aorta is located on the left side and may be injured during the operation. After observing the patient’s intraoperative monitoring, there was no significant change in blood pressure and heart rate. No sign of active bleeding was found in the operation area during the operation. However, judging from the postoperative symptoms, the segmental artery has been injured at this time. Due to the wound surface of the early lumbar segmental artery injury being wrapped by the psoas major, there was no obvious clinical symptoms during the operation. In addition, other scenarios injuring the artery could occur with lumbar surgery. A misplaced pedicle screw that deviates laterally through the lateral vertebral wall. A lateral transpsoas surgical approach used during lateral/oblique inter body fusion techniques.
Endovascular techniques, such as stent-graft placement, embolization, and thrombectomy, have proven to be useful in the re-establishment of blood flow.8,13
The patient’s pain symptoms in this case did not resolve after administration of analgesics and blood transfusions. Angiography showed active hemorrhage from a ruptured lumbar segmental artery. After immediate embolization, the patient’s pain symptoms were significantly relieved, and muscle strength was improved.
To sum up, severe lower extremity pain that couldn’t relieve by painkiller accompanied by passive flexion of the hip can help us make timely diagnosis of psoas hematoma after PLIF.
Conclusions
This treatment of angiographic embolization is one of the effective methods that can be used for reference.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed Consent
Informed written consent was obtained from the patient for publication of this report and any accompanying images. A copy of the written consent is available for review by the Editor of this journal.
Availability of Data and Materials
All the data supporting our findings are contained within the manuscript.
