Abstract
Background:
Hip fractures have significant effects on the geriatric population and the health care system. Prior studies have demonstrated both the safety of intravenous (IV) acetaminophen and its efficacy in decreasing perioperative narcotic consumption. The purpose of this study is to evaluate the effect of scheduled IV acetaminophen for perioperative pain control on length of hospital stay, pain level, narcotic use, rate of missed physical therapy (PT) sessions, adverse effects, and discharge disposition in geriatric patients with hip fractures.
Methods:
A retrospective review was performed of all patients 65 years and older admitted to a level I trauma center, who received operative treatment for a hip fracture over a 2-year period. Demographic data, in-hospital variables, and outcome measures were analyzed. Three hundred thirty-six consecutive fractures in 332 patients met inclusion criteria. These patients were divided into 2 cohorts. Group 1 (169 fractures) consisted of patients treated before the initiation of a standardized IV acetaminophen perioperative pain control protocol, and group 2 (167 fractures) consisted of those treated after the protocol was initiated.
Results:
Group 2 had a statistically significant shorter mean length of hospital stay (4.4 vs 3.8 days), lower mean pain score (4.2 vs 2.8), lower mean narcotic usage (41.3 vs 28.3 mg), lower rate of PT sessions missed (21.8% vs 10.4%), and higher likelihood of discharge home (7% vs 19%; P ≤ .001). Use of IV acetaminophen was also consistently and independently predictive of the same variables (P < .01).
Conclusion:
The utilization of scheduled IV acetaminophen as part of a standardized pain management protocol for geriatric hip fractures resulted in shortened length of hospital stay, decreased pain levels and narcotic use, fewer missed PT sessions, and higher rate of discharge to home.
Level of Evidence:
Therapeutic level III.
Introduction
Hip fractures remain a major cause of morbidity and mortality among the aging population of the United States. According to the Center for Disease Control, there are 586 000 admissions annually for fractures in people aged 65 or older. Of these fractures, nearly half, 273 000, were hip fractures, defined as either femoral neck or intertrochanteric fractures, excluding pathologic fractures. In addition, of the 324 000 admissions for hip fracture in all age-groups, an overwhelming 84% were in people aged 65 and older. 1 The average length of hospital stay for this population was over 6 days. 1,2 Greater than half of patients with a hip fracture show a measurable decline in functional status after their injury, often necessitating secondary care facility admission. 2 –4 The risk of mortality in an elderly individual 3 months after hip fracture is greater than 4 times that of one without, and the risk of death at 1 year is twice that of a comparable uninjured person, 3,5,6 and studies have demonstrated that decreased preoperative function is predictive of increased postoperative morbidity and mortality, emphasizing the importance of improved postoperative cognition and exercise for maximizing functional outcome after a hip fracture. 7,8 Estimates of total cost to the health care system for hip fractures, including both hospital and posthospital care, are up to US$30 billion annually in the United States. 2,4,9 –11 Despite increased emphasis on bone health, given the rapidly increasing elderly populace, the associated costs of hip fracture care are only expected to continue to rise. 4,9 –11
Postoperative pain control remains difficult in the aging population, and opioid analgesia dominates current pain management strategies. Pharmacokinetics and pharmacodynamics are more complex in elderly persons who experience higher peak effect and longer duration of action of opioids due largely to decreased renal and hepatic clearance as well as a change in body composition including an increase in adipose tissue, decrease in lean body mass, and decrease in total body water. This puts them at increased risk of respiratory depression, constipation, delirium, pulmonary complications, and oversedation. 2,12 –17 Despite pain-induced complications such as delirium, many physicians are reluctant to prescribe opioid analgesics to elderly patients for fear of potential resultant opioid-induced adverse effects. 12,13 Postoperative pain has been associated not only with delirium but also with prolonged bed rest following surgery. These disruptions in physical therapy (PT) and postoperative ambulation lead to a relative increase in risk of thromboembolism and functional impairment, which in turn may result in significantly longer hospital lengths of stay, long-term functional impairment, and other costs. 12 Not surprisingly, improved functional outcomes, both short term and long term, are associated with superior patient performance in inpatient PT sessions. 8,17 –19 Any obstacles to PT participation by either opioid-induced side effects or undertreated pain will have a deleterious effect on functional recovery. Many opioid-related adverse drug events occurring in hospitals led The Joint Commission to publish a Sentinel Event Alert with opioid use guidelines. 20 Evidence-based guidelines do exist for prescribing opioids in acute and postoperative pain, but numerous studies show that these guidelines are rarely followed and pain control remains a difficult issue, especially in geriatric patients. 12,21,22 Although caution is warranted in opioid analgesia use, compromising adequate pain control for fear of adverse effects is not recommended. These fears have facilitated the desire for nonopioid analgesics to be utilized as often as possible.
Traditional nonsteroidal anti-inflammatories (NSAIDs) and COX-2 inhibitors have been shown to be efficacious in postoperative pain control but also have their own limitations, primarily the risk associated with their use in patients with impaired renal and/or cardiovascular function. 23 –25 An alternative to narcotics and NSAIDs is acetaminophen. Acetaminophen has a well-established analgesia profile and a more reliable bioavailability when administered intravenously versus orally or rectally 26,27 and does not have a significant effect on kidney function in the postoperative period. 24 The safety and efficacy of its use in patients aged 65 years and older have been shown to be comparable to that in younger patients without a need for dosing adjustments. 25 Intravenous (IV) acetaminophen has repeatedly been shown to be a safe and efficacious analgesic in major orthopedic surgery. 26,28 –31 Although other studies have successfully demonstrated that the use of acetaminophen can reduce opioid use in the perioperative time period, 24,32,33 no published studies have evaluated its effect on patient outcomes.
In June 2012, the hip fracture committee at our institution adopted the use of scheduled IV acetaminophen in patients with hip fractures as the standard of care. The aim of this study was to determine whether the implementation of scheduled perioperative IV acetaminophen during hip fracture treatment for those aged 65 and older influenced the following: (1) length of hospital stay, (2) pain level, (3) narcotic use, (4) rate of missed PT sessions, (5) adverse effects, (6) gastrointestinal disturbance, and (7) discharge disposition.
Patients and Methods
After Institutional Review Board approval was obtained for a retrospective comparative cohort study, a search utilizing Current Procedural Terminology (CPT) 34 codes 27235, 27236, 27244, and 27245 was performed. All patients aged 65 years and older admitted to the orthopedic service at a Level 1 trauma center who received operative treatment by 1 of the 6 fellowship-trained orthopedic surgeons over a 2-year period, from June 1, 2011, through May 31, 2013, were identified. The patients were divided into 2 cohorts. Group 1 consisted of patients treated for 1 year before the initiation of a standardized IV acetaminophen pain control protocol on June 1, 2012, and group 2 consisted of those treated for 1 year after the protocol was initiated. All other aspects of the geriatric hip fracture protocol remained consistent throughout this 2-year period.
The CPT code search returned 433 consecutive fractures in 425 patients. Ninety-seven fractures were excluded for the following reasons: admission to a nonorthopedic service (55), subtrochanteric (13), pathologic (8), periprosthetic (8), simultaneous orthopedic injuries requiring operative intervention (8 fractures in 7 patients, including simultaneous bilateral hip fractures in 1 patient), and perioperative death (5). This resulted in 332 patients with 336 intertrochanteric or femoral neck fractures (169 in group 1 and 167 in group 2), classified as Arbeitsgemeinschaft für Osteosynthesefragen/Orthopaedic Trauma Association (AO/OTA) 31-A or 31-B. 35 Radiographs were verified by the investigators. Bilateral hip fractures were included in 4 patients with nonsimultaneous injuries that occurred at a mean of 11 months (range 5-19) apart. The patients had a mean age of 82.6 years (range 65-101).
Group 1 received oral acetaminophen as well as a combination of oral and IV narcotics, all of which were ordered on an as-needed basis for pain control. Although the specifics varied from patient to patient, orders for oral acetaminophen were 1000 mg every 8 hours, oral narcotics typically consisted of tramadol 50 mg every 6 hours and/or oxycodone 5 to 10 mg every 4 hours, and IV morphine was ordered as 2 to 4 mg every 2 hours. The standardized pain management protocol at our institution for group 2 consisted of IV acetaminophen administered to patients with a hip fracture in 1000-mg increments every 8 hours for a minimum of 24 hours from the time of admission or until they were taken to surgery if that time period exceeded 24 hours. Throughout that time they were given IV narcotics for breakthrough pain as needed, ordered at the same frequency as group 1. Patients were transitioned to as-needed oral acetaminophen and traditional narcotics after the initial time period ended. Patients also continued receiving IV acetaminophen if they were unable to tolerate oral medications and/or traditional narcotics.
We performed a retrospective chart review and collected data for patient demographics (eg, age, body mass index [BMI], and sex), in-hospital variables (eg, diagnosis, surgical treatment, time to the operating room, and doses of acetaminophen received), and outcome measures (eg, length of stay, total narcotic usage, pain score, PT sessions missed, discharge location, and adverse effects). The primary outcome variable for our study was length of stay (days from admission to discharge). Pain score was documented using 10-point visual analog scale (VAS) with word descriptors. Mean pain score was calculated from 4 points in time: the first entry at admission, 6 hours postoperatively, 24 hours postoperatively, and the last entry before discharge. Narcotic use was calculated by converting all doses of oral and IV opioid narcotics to cumulative milligrams of morphine-equivalent using equianalgesic tables. 36 The percentage of missed PT sessions was calculated as the ratio of PT sessions missed to the total number of PT attempts. Gastrointestinal disturbance was determined using the number of as-needed bowel motility and antiemetic agents used. Discharge to a secondary care facility was defined as a skilled nursing facility, subacute rehabilitation, or acute rehabilitation, versus discharge to independent living at home.
A power analysis based on length of stay as the primary outcome variable indicated that with α = .05 and β = .20, a statistically significant difference would be detected with a sample size of 284 patients (142/cohort). Descriptive statistics were completed to provide the mean, standard deviation, range, percentages, and distribution of variables. Quantitative data, including length of stay, narcotic use, acetaminophen use, bowel motility use, antiemetic use, pain score, and hours to surgery, were analyzed using the unpaired t test, while nominal data, including missed PT sessions and discharge location, were analyzed using the chi-square test. Quantitative data are reported as mean ± standard deviation, while nominal data are reported as percentages. Separate multivariate regression analyses were performed using length of stay, pain score, total narcotic usage, and PT sessions missed as dependent variables, while age, IV acetaminophen use, sex, BMI, time to the operating room, diagnosis, pain score, and narcotic use were used as independent variables. A logistic regression analysis was also performed using discharge location as the dependent variable and the same independent variables. Multivariate regression data are reported as the β coefficient, while logistic regression results are shown as odds ratios and 95% confidence intervals. Significance for all analyses was assessed at P < .05. Analyses were performed using SPSS v21.0 (IBM, Armonk, New York).
Results
Baseline Data: Demographic and In-Hospital Data by Treatment Group.

Abbreviations: IV, intravenous; OR, operating room.
aReported as mean ± standard deviation (range).
bReported as number (percentage).
*p indicates statistical significance ≤0.05.
Outcome Variables by Treatment Group.
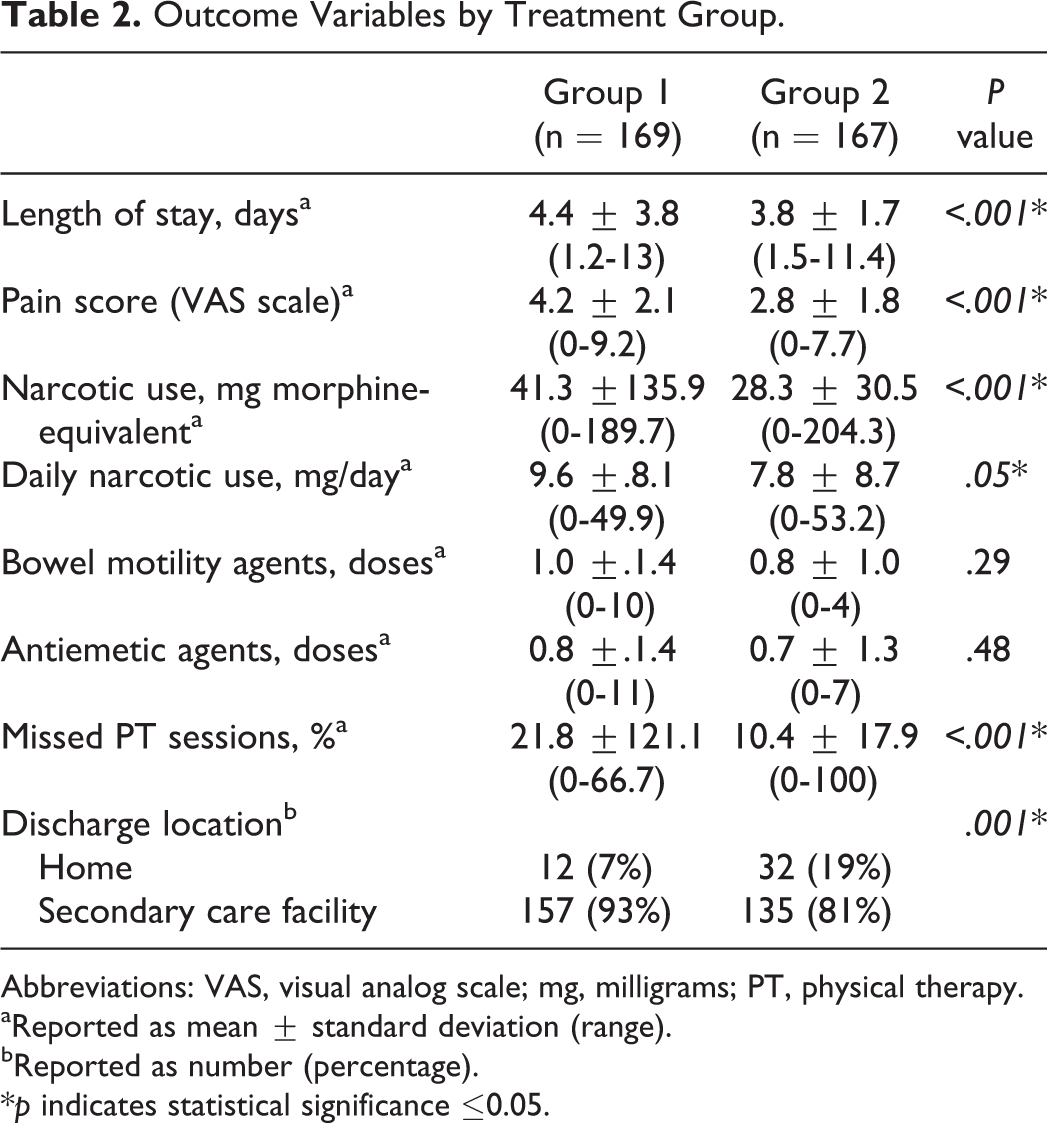
Abbreviations: VAS, visual analog scale; mg, milligrams; PT, physical therapy.
aReported as mean ± standard deviation (range).
bReported as number (percentage).
*p indicates statistical significance ≤0.05.
A-D. Regression Analyses.a

Abbreviations: IV, intravenous; BMI, body mass index; OR, operating room; PT, physical therapy.
aMultivariate regression analyses for length of stay (A), pain score (B), total narcotic use (C), and missed PT sessions (D), with β coefficients for all variables that demonstrated statistical significance for one or more regressions.
*p indicates statistical significance ≤0.05.
Regression Analysis: Odds of Discharge to Secondary Care Facility.a

Abbreviations: CI, confidence interval; IV, intravenous; BMI, body mass index; OR, operating room; mg, milligrams; N/A, not available.
aLogistic regression analysis with odds ratios and confidence intervals listed for those variables demonstrating statistical significance as predictive of likelihood of discharge to a secondary care facility as opposed to home.
*p indicates statistical significance ≤0.05.
Discussion
Hip fractures are a common problem in the elderly population of the United States, having substantial impact, including patients’ functional decline and economic burden to the health care system. A vast majority of hip fractures are treated operatively, and opioid-based pain control remains a mainstay in treatment of perioperative pain. However, opioid-based regimens are associated with a number of adverse side effects that may complicate a patient’s perioperative care.
An institutional geriatric hip fracture program was well established by the time of our data collection. Recent studies have shown the effectiveness of geriatric hip fracture programs in improving patient outcomes. 37,38 Our institution’s hip fracture committee further standardized hip fracture care by adopting a scheduled IV acetaminophen protocol for perioperative pain management. Our data demonstrated no statistical significance in total acetaminophen use between the 2 groups, but we did note a difference between the 2 routes of administration for the groups. As group 2 used a higher ratio of IV to oral acetaminophen, the improvements in our determined outcome measures with IV acetaminophen use supports the IV route of administration as more beneficial in improving outcomes. Studies have shown that IV acetaminophen not only reaches a higher peak plasma concentration than oral acetaminophen but also that IV acetaminophen reaches that point earlier. 26,27 It has also been shown that gastric emptying and gastrointestinal absorption is slowed in the elderly individuals, patients in a normal postoperative state, and those who have received opioid narcotics, 39,40 resulting in potentially slower absorption of oral acetaminophen. These serve as potential explanations for the increased efficacy of the IV route of acetaminophen observed in our study.
Other studies have demonstrated the importance of early surgery on fewer in-hospital complications, improved functional outcome, increased return to independent living, and decreased mortality. 37,41 –46 In this study, there was no statically significant difference in length of time from admission to the operating room between the 2 groups. Our data reinforced the findings of increased rate of home discharge with early surgery, but in addition we found that IV acetaminophen use was independently predictive of improved outcomes and a higher likelihood of home discharge when controlling for time from admission to the operating room in our analysis.
Intravenous acetaminophen usage was also predictive of decreased VAS pain scores as well as decreased narcotic usage, both of which are factors universally known to be common causes of delirium. 5,12,14,17,47,48 As such, in addition to the intrinsic value of decreasing patients’ perioperative pain, IV acetaminophen has the potential to be a useful medication in indirectly reducing delirium in the elderly population by reducing the likelihood of delirium resulting from both inadequately controlled pain and opioid narcotic use.
Chin et al demonstrated that a standardized regimen of scheduled analgesics improves participation in PT following hip fracture surgery, 49 and recent studies have shown that early functional outcome is predictive of improved 1-year mortality. 16,50 Our results also demonstrated improved postoperative participation in PT and that IV acetaminophen use was the only variable to demonstrate statistical significance in doing so.
This study has a number of strengths. We utilized a historical control (group 1) and found no difference between the 2 groups for any confounding variables. In addition, the large cohort sizes provided statistical power to determine significance for many variables. Furthermore, the geriatric hip fracture and the IV acetaminophen institutional protocols were consistently followed. However, our study is not without its limitations, many of which are inherent to its retrospective nature. The ability to measure and compare outcome variables was limited by the data consistently available within the electronic medical record. Mortality rate, readmission, pre- and postfracture objective functional capacity scores, and prehospital residence were not included. Additional narcotic-induced adverse effects, including pulmonary complications, respiratory depression, and oversedation, were not consistently available. Also, during the time of this study, there were no protocols in place that required consistent, objective documentation of episodes of delirium or causes for missed PT sessions. Furthermore, although the geriatric hip fracture program was well established before the initiation of this study, it is possible that immeasurable variables, such as education of physical therapists and nursing staff to the program’s goals and efficiency of care management personnel in the discharge process, improved throughout the period of our data collection, thus having a confounding effect. Prospective, randomized trials are therefore needed to delineate such effects, while including all desired outcome measures, including standardized functional outcome scores, hospital readmission rates, and mortality rates. The cost of IV acetaminophen will vary by institution, but in our study it was more expensive than oral acetaminophen and all individual IV and oral opioid medications. Whether this cost is offset or even overcome by decreased length of hospital stay and/or decreased use of all other pain medications remains to be seen. As such, in addition to comparative effectiveness research, it is essential for future research to include a cost analysis.
Conclusion
In the geriatric hip fracture population, pain control is an important aspect of patient care, yet narcotic use is complicated by a number of factors. The utilization of scheduled perioperative IV acetaminophen as part of a standardized protocol for geriatric hip fractures is efficacious for shortening hospital length of stay, controlling pain and decreasing narcotic use, improving participation in PT, and increasing home discharge rate. Other areas of orthopedics have demonstrated the benefit of IV acetaminophen, and this study supports its use in the geriatric hip fracture population.
Footnotes
Authors’ Note
This study has previously been presented in part at the Annual Meeting of the Michigan Orthopaedic Society (Mackinac Island, Michigan, June 2014), and Orthopaedic Trauma Association Annual Meeting (Tampa, Florida, October 2014), American Academy of Orthopaedic Surgeons (Las Vegas, Nevada, March 2015), and Mid-America Orthopaedic Association (Hilton Head, South Carolina, April 2015).
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
There was no outside funding received for this study.
