Abstract

Introduction:
Spina bifida (SB) frequently results in neurogenic lower urinary tract dysfunction (NLUTD) with stress urinary incontinence (SUI) despite clean intermittent catheterization (CIC). 1,2 Only a small proportion of patients can void spontaneously. 1 While the artificial urinary sphincter (AUS) is the standard for post-prostatectomy incontinence, 3 its use in NLUTD is limited by high revision rates, the potential need for CIC, and the risk of erosion or malfunction. 4 –6 Puboprostatic sling (PPS) procedures using autologous fascia have demonstrated efficacy in neurogenic patients while maintaining CIC ability, though only open techniques have been described. 7 We present the first robotic-assisted autologous fascia lata PPS in a patient with SB and neurogenic SUI.
Materials and Methods:
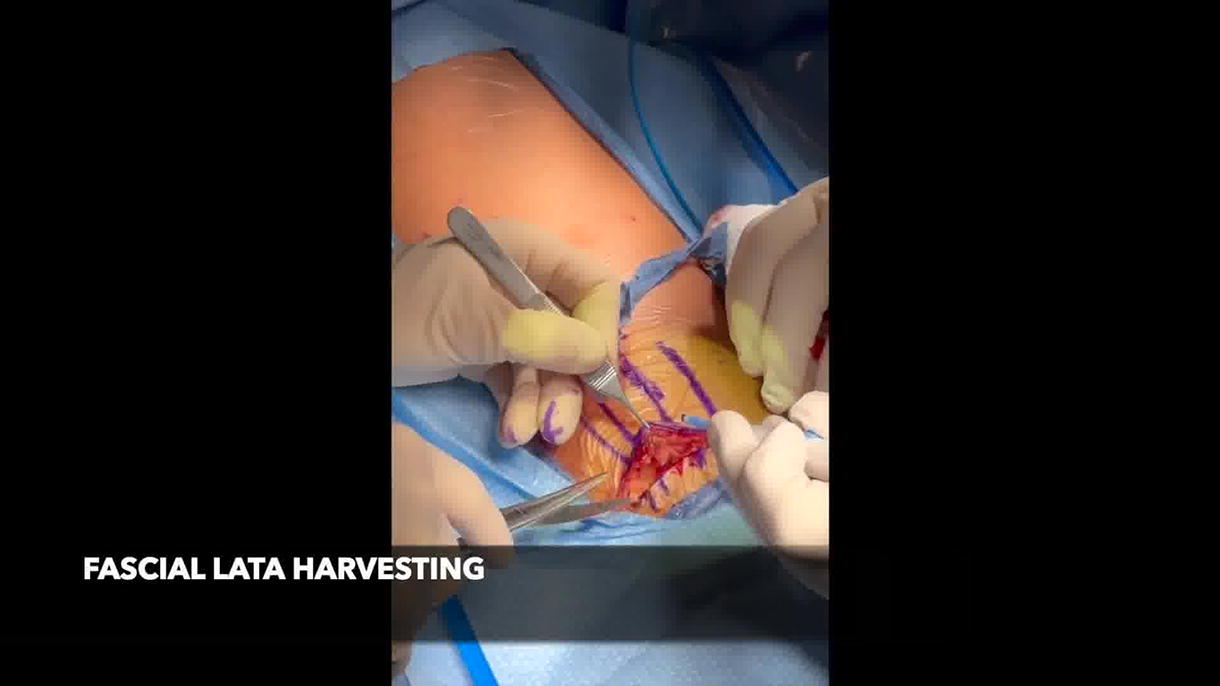
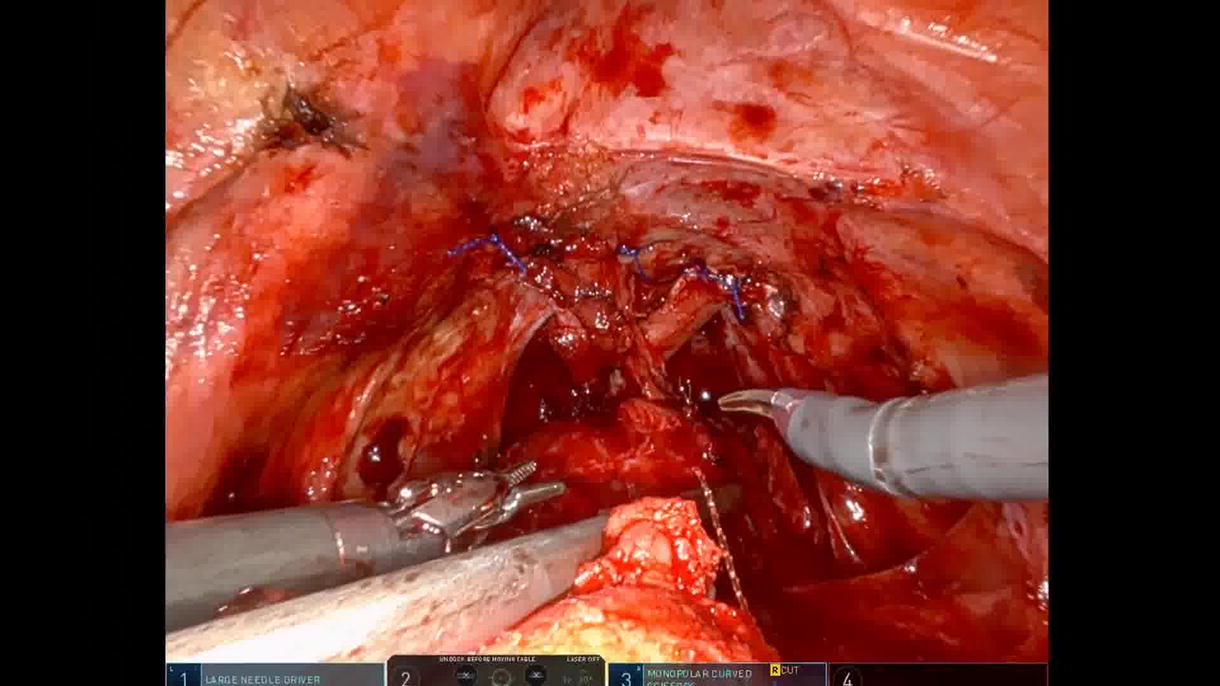
A 22-year-old man with closed SB, performing CIC every 3 hours, reported stress-predominant leakage. Urodynamics demonstrated safe storage pressures, bladder capacity of 598 mL, and abdominal leak-point pressure of 125 cm H2O; fluoroscopy confirmed bladder-neck incompetence. After counseling on AUS versus sling, robotic autologous fascia lata PPS was performed. A 10–12 cm fascia lata graft was harvested via a short lateral-thigh incision and prepared on the back table. The patient was then placed in dorsal lithotomy with steep Trendelenburg. Access was obtained at Palmer’s point using a 12-mm AirSeal trocar and three additional robotic ports. The space of Retzius was developed to expose the intrapelvic urethra. The sling was passed beneath the urethra distal to the prostate, arms crossed, and sutured to Cooper’s ligaments with 2-0 polypropylene sutures. A flexible 17 Fr cystoscope with 300 mL bladder fill confirmed urethral patency and elevation. Hemostasis and layered closure were achieved, and a 16 Fr Foley catheter was placed for drainage.
Results:
The procedure was completed robotically without conversion. Estimated blood loss was 50 mL, and hospital stay was 1 day. No intra- or postoperative complications occurred. The Foley catheter was removed on postoperative day 5; the patient resumed CIC every 4–5 hours without resistance. At the 3-month follow-up, he remained continent between catheterizations.
Conclusions:
Robotic autologous fascia lata PPS is feasible and safe for male SUI in NLUTD, achieving continence while preserving CIC and maintaining low storage pressures. Robotic assistance allows precise sling placement, optimal visualization, and secure fixation with minimal morbidity. Larger, multicenter studies with long-term follow-up are required to confirm durability and reproducibility.
Disclosure Statement:
The authors declare no conflicts of interest or financial relationships. Author(s) have received and archived patient consent for video recording/publication in advance of video recording of the procedure. No funding was received for this work.
Runtime of video: 8 mins.
Keywords
Get full access to this article
View all access options for this article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
