Abstract
Background
High social risk, as quantified by the social determinants of health (SDH), may lead to disability. This association has not been well explored in remote settings. Using the three Villages Study cohort, we assessed the association between SDH and disability among stroke-free older adults living in a rural Ecuadorian community.
Methods
SDH were measured by the use of the Gijon Scale and disability by the Functional Activities Questionnaire. All participants had a brain MRI to assess subclinical biomarkers of cerebral small vessel disease. Multivariate models were fitted to assess the association between components of SDH and disability, after adjusting for covariates of interest.
Results
The mean age of 478 enrolled individuals was 70.1 ± 8 years (59% women). High social risk was observed in 220 (46%) individuals and disability in 222 (46%). There was an almost direct linear relationship between SDH and disability, after taking into account the effect of age. A generalized linear model, adjusted for all included covariates, showed an independent association between social risk and disability (P < .001). In addition, multivariate models showed that independent SDH components more strongly associated with disability were worse support networks and social relationships. In contrast, the single SDH component not associated with disability was the economic status.
Conclusions
This study showed a robust association between SDH and disability. Economic needs were surpassed by other components of SDH. This knowledge will help to develop strategies for the control of factors that may be in the path for disability among older adults living in rural settings.
Keywords
Introduction
According to the World Health Organization (WHO), “health is a state of complete physical, mental and social well-being and not merely the absence of disease or infirmity”. 1 In this view, the so-called “Social Determinants of Health (SDH)” are of fundamental importance for the healthy status and functional independence of individuals with or without chronic diseases. These determinants may also be in the path for the occurrence and progression of several morbid conditions. 2 Recent studies have suggested a link between SDH and cardiovascular diseases, including stroke.3-5 Accordingly, a high social risk not only increases the prevalence of cardiovascular risk factors and increases mortality after an event, but also increase disability among stroke survivors by means of several psychological, behavioral and biological mechanisms.6-8
The SDH include situations in which persons are born, grow, live, work and age, as well as the adequacy of medical care. 9 While these determinants have been associated with disability, the relationship between social risk and functional impairment is complex and probably bidirectional. As the social risk increases so too does functional impairment and the development of disability may lead to an increase in social risk. 10
While poverty and disparities in health care are contributors to higher social risk, SDH assessment varied across studies, and it has been difficult to standardize which determinants better assess the actual social risk in different settings. In any case, SDH vary according to the level of development of a given community and their assessment must be adapted consequently.11-14
The study of the association between SDH and disability in individuals living in diverse remote rural settings provides an optimal scenario to better understand their particular needs, the factors responsible for such association, and the application of region-specific interventions intended to reduce functional impairment among older adults living in underserved communities. Taking the opportunity of an already established clinical cohort of community-dwelling older adults living in 3 neighboring rural villages located in coastal Ecuador.15,16 the present study assessed the association between SDH and disability in stroke-free older adults living in these villages.
Methods and Materials
Results
Brain MRIs were performed in 590 (83%) out of 712 community-dwelling individuals aged ≥60 years identified during door-to-door surveys. Of the remaining 122 individuals, 53 refused the practice of MRI, 14 were bedridden and could not be transported to Guayaquil, 12 experienced claustrophobia during the exam, and one had an implanted pacemaker. In addition, 42 persons had died or emigrated between enrollment and the invitation for MRI. Of the 590 individuals with an MRI, 62 were excluded because of an overt stroke and 50 either declined further participation, emigrated or died between MRI and the interviews for assessment of SDH and disability, leaving 478 individuals enrolled in the present study.
There were several differences in demographics and cardiovascular risk factors across participants and those individuals that were not included in this study (Table 1). Such differences were mostly the result of the inclusion criteria, since patients with an overt stroke and those bedridden were excluded.
Differences in Demographics and Cardiovascular Factor Across Participants and Individuals Excluded for this Study.
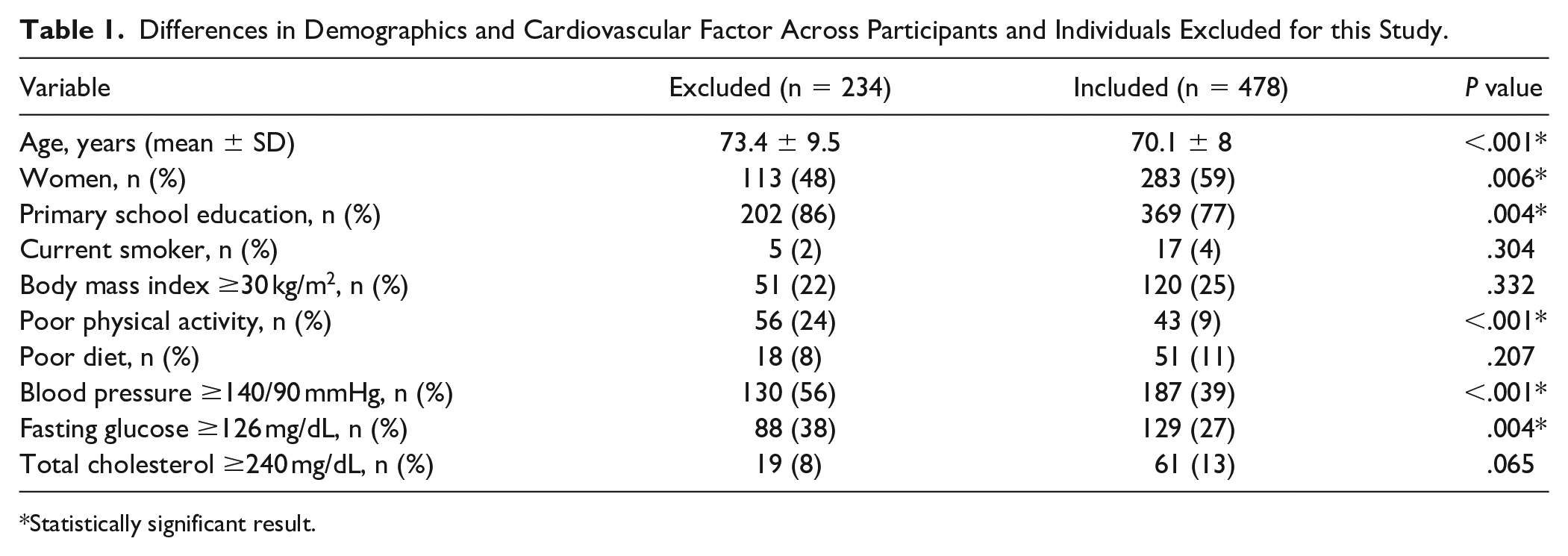
Statistically significant result.
The mean age of participants was 70.1 ± 8 years, 283 (59%) were women, and 369 (77%) had primary school education only. Seventeen subjects (4%) were current smokers, 120 (25%) had a body mass index ≥30 kg/m2, 43 (9%) had poor physical activity, 51 (11%) had a poor diet, 187 (39%) had blood pressure ≥140/90 mmHg, 129 (27%) had fasting glucose ≥126 mg/dL, and 61 (13%) had total cholesterol levels ≥240 mg/dL. One-hundred individuals (21%) were frail according to the EFS (≥7 points), 197 (41%) had a poor sleep quality according to the PSQI (≥5 points), and 60 (13%) had symptoms of depression according to the DASS-21 (≥5 points). Moderate-to-severe WMH were noticed in 116 individuals (24%), deep CMB in 29 (6%), silent lacunes in 32 (7%), and >10 enlarged BG-PVS in 126 (26%).
Measurements of SDH indicated social risk in 220 (46%) individuals. The mean ± SD score of the Gijon scale was 9.8 ± 2.8 points. Mean values for individual components of SDH were 1.7 ± 1.1 points for family situation, 3.5 ± 1.2 points for economic status, 1.7 ± 0.8 points for housing, 1.7 ± 1 points for social relationships and 1.1 ± 0.6 points for support networks. The mean FAQ score for the entire sample was 9.3 ± 6.7 points, with 222 (46%) having impaired functionality (disability). A locally weighted scatterplot smoothing (LOWESS) graph showed an almost direct linear relationship between SDH and disability, after taking into account the effect of age (Figure 1).

Locally weighted scatterplot smoothing (LOWESS) graph showed an almost direct linear relationship between social determinants of health and disability, after taking into account the effect of age.
Table 2 shows several differences in the investigated covariates across individuals with and without social risk and disability (univariate analysis). Individuals with social risk were older, more often female, and had more often primary school education, worse physical activity, poor diet, and high blood pressure than those without social risk. In addition, these individuals were more often frail, had worse sleep quality, more often moderate-to-severe WMH and >10 enlarged BG-PVS than those without social risk. On the other hand, disability was more frequent with increased age, in those with primary school education only, as well as in individuals with poor physical activity, high blood pressure, frail status, symptoms of depression, moderate-to-severe WMH, and silent lacunes.
Characteristics of Atahualpa, El Tambo and Prosperidad Residents Aged ≥60 Years Across Categories of Social Determinants of Health and Disability (Univariate Analyses).

Abbreviations: BG-PVS: basal ganglia-perivascular spaces; WMH: white matter hyperintensities.
Statistically significant result.
A fully-adjusted generalized linear model showed a significant (and independent) association between social risk and disability (β: 0.44; 95% C.I.: 0.26-0.62; P < .001). In this multivariate model, increasing age, poor diet, frail status, symptoms of depression, and the presence of moderate-to-severe WMH, silent lacunes, and >10 enlarged BG-PVS remained as significant covariates (Table 3). Age was the most influential variable in the above-mentioned association (t = 8.84). Other covariates with high influence included frail status, symptoms of depression, and the presence of moderate-to-severe WMH. To better understand the effect of age in the association between SDH and disability, we constructed a contour plot with Shepard interpolation. 29 The plot showed several clusters of individuals aged 80 years or older only at higher levels of disability but at different levels of SDH scores, suggesting no significant effect of age in the above-mentioned association (Figure 2).
Fully-Adjusted Generalized Linear Model Showing the Independent Association Between the Social Determinants of Health and Disability (as the Dependent Variable).

Abbreviations: BG-PVS: basal ganglia-perivascular spaces; WMH: white matter hyperintensities.
Statistically significant result.

Contour plot with Shepard interpolation showing several clusters of individuals aged 80 years or older only at higher levels of disability but at different levels of social determinants of health scores, suggesting no significant effect of age in this association.
In addition, generalized linear models were fitted to calculate the association between the 5 individual components of SDH and disability, after adjusting for the aforementioned covariates (Table 4). In these models, the components more strongly associated with disability were the presence of worse support networks (OR: 2.64; 95% C.I.: 1.77-3.50) and social relationships (OR: 1.79; 95% C.I.: 1.28-2.31). In contrast, the single component not associated with disability was the economic status (OR: –0.41; 95% C.I.: –0.83-0.01).
Univariate Analyses and Generalized Linear Models Showing Associations Between Individual Components of Social Determinants of Health and Disability, After Adjusting for all Covariates.

Statistically significant result.
Discussion
This study, conducted in a population-based cohort of community-dwelling stroke-free older adults living in 3 rural villages of coastal Ecuador, showed a robust and independent association between SDH (and most of their individual components) and disability. Interestingly, the single individual component of SDH not associated with disability was the economic status of individuals, which suggest that—at the rural level—economic needs that might lead to disability are largely surpassed by other components of SDH, in particular by social relationships and support networks. Similar findings have been reported from a developed country, where the association between a higher income and a healthy status was less important among rural women than in their urban counterparts. 14 Disparities across men and women regarding social risk are notable among people living in some rural areas of developed countries. 30 However, this seems not to be important in the rural population enrolled in the present study, where gender did not remain as a significant independent covariate in multivariate models assessing the association between SDH and disability.
The role of social relationships and support networks to reduce loneliness and its impact on impaired functionality among older adults has not been well studied in remote rural communities. The feeling of loneliness among older adults is currently a public health problem in the developed world, especially in large urban centers,31,32 and might also be affecting older adults living in some remote rural settings. 33 Loneliness often leads to depression, disturbed sleep and increased expression of cardiovascular risk factors, which, in turn, may facilitate the development of disability.34,35 However, the scenario is still less noticeable in other rural communities. As previously noticed, migration rate is low among individuals living in the current study population. This results in large families living in the same village and often in the same house or only a few blocks apart. In these settings, it is common for older adults to have more than 1 caregiver, which reduce the risk of burnout that results in functional impairment in the elder and an impaired quality of life of both the elder and the caregiver. 36
To our knowledge, there are no study systematically addressing the role of subclinical cSVD on the association between SDH and disability in rural settings, and this is a novel aspect of the present study, particularly because damage of the cerebral microvasculature has been associated with functional impairment in studies conducted in the developed world, 37 and this condition is prevalent in the study population. 38 The presence of moderate-to-severe WMH and >10 enlarged BG-PVS were significantly associated with SDH, and moderate-to-severe WMH and silent lacunes were significantly associated with disability in univariate analyses. In addition, almost all biomarkers of cSVD (with the exception of CMB) remained as independently significant covariates in the multivariate model. This suggests an important influence of subclinical brain damage of vascular origin in the association between SDH and disability. The presence of cSVD biomarkers should be considered as potential targets for prevention in apparently healthy individuals at risk.
The cross-sectional design precludes the evaluation of the direction of the relationship between SDH and disability is a limitation of this study. Another potentially limitation is that we did not explore poor cognitive performance, which may be associated with disability. However, assessment of cognitive frailty was included among the investigated covariates. While a frail status remained independently significant in the regression model assessing the association between SDH and disability, it was not important enough to make this association to vanish in the multivariate model. The above-mentioned shortcomings of the present study were compensated by the population-based design with unbiased enrollment of individuals and the systematic assessment of the main investigated variables by means of validated field instruments. Also, the routine practice of MRI allowed to assess the role of subclinical brain damage of vascular origin in the studied association. Assessment of SDH by the use of a field instrument that is appropriate for remote rural settings—the Gijon scale—is another strength of the present study, since the selection of a given scale must take into account the specific needs and characteristics of the study population.
Knowledge on the burden of social risk, disability and the association between them is indispensable for the development of cost-effective preventive policies for controlling modifiable factors that are in the path of functional impairment among older adults living in resource-poor communities. Further multicentric studies using similar protocols are needed to confirm these findings.
Footnotes
Authors’ contributions
OHD: study design, imaging readings, manuscript drafting; RMM: statistical analyses; BYR: data collection and analysis; VJD: imaging readings, significant intellectual contribution to manuscript content.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Study supported by Universidad Espíritu Santo – Ecuador. The sponsor had no role in the design of the study, nor in the collection, analysis, and interpretation of data.
Data availability statement
The data that support the findings of this study are available from the corresponding author upon reasonable request.
