Abstract
A 33-year-old female presented with finger pain, swelling, and erythema was diagnosed with cellulitis and treated with antibiotics. Persistent symptoms led to further evaluation including a point-of-care ultrasound revealing a cystic structure, concerning for abscess. Incision and drainage yielded a solid mass rather than fluid. Pathological examination revealed a schwannoma, a benign peripheral nerve sheath tumor. This case highlights the rare presentation of a schwannoma mimicking an infectious process and emphasizes the importance of considering peripheral nerve tumors in the differential diagnosis of soft tissue masses, especially when the clinical course is atypical. It also underscores the value of pathological examination in establishing a definitive diagnosis and preventing misdiagnosis, which can have implications for patient management.
Case Presentation
A 33-year-old female presented to clinic with 5 days of finger pain. She reported a tender mass with swelling and erythema at the base of her left third finger. She sought evaluation after she noticed that the redness started expanding over the dorsal surface of her hand (Figure 1). In addition, she noticed warmth in the area and subjective fevers. During her clinic visit she was afebrile with a blood pressure of 108/76 mmHg and a pulse rate of 99 bpm. A point-of-care ultrasound was performed and showed a cystic fluid-containing structure that measured 5 mm at the base of the left third finger. She was diagnosed with cellulitis and prescribed a 7-day course of Cefadroxil.
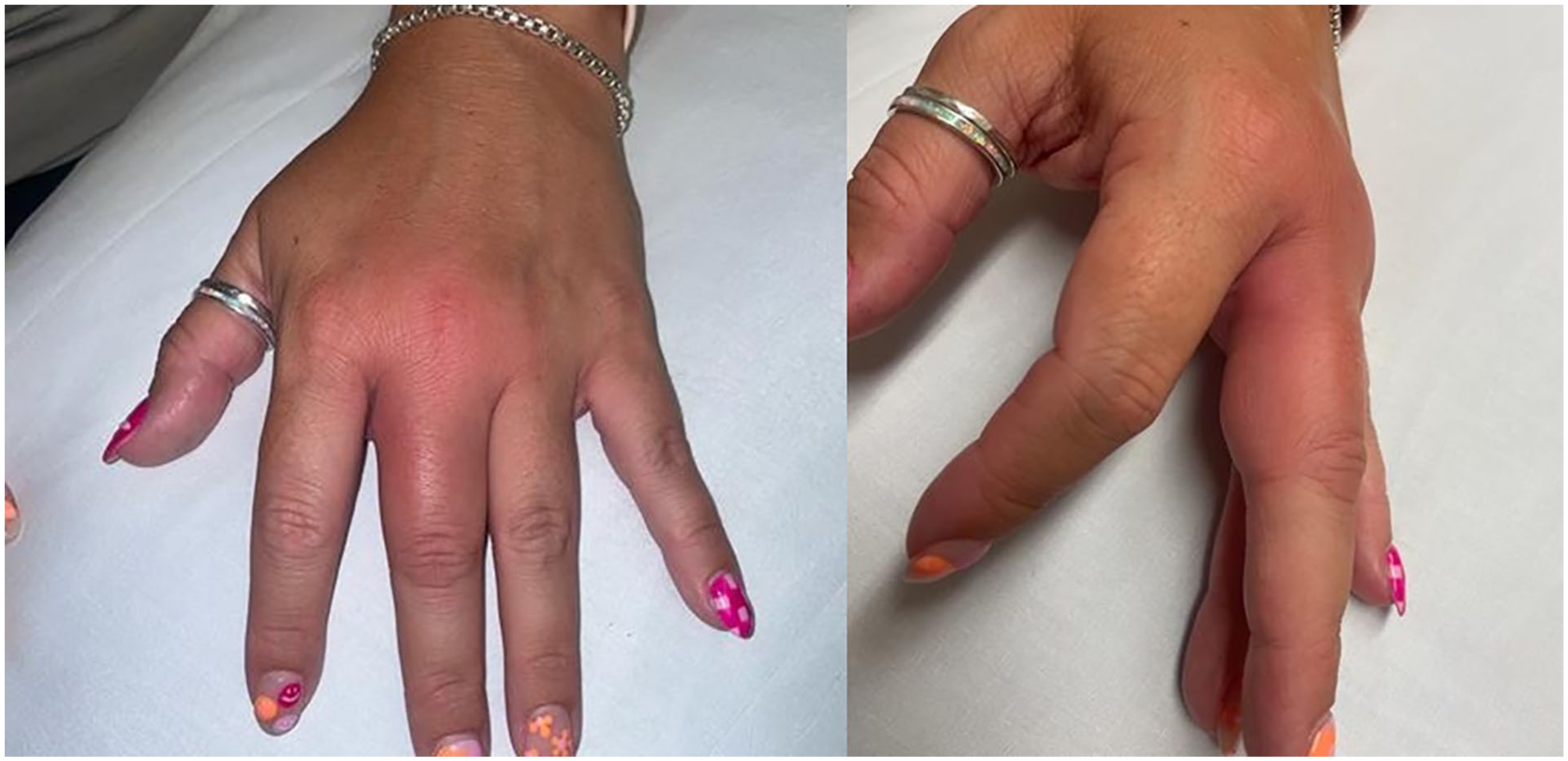
(Left): Clinical photo of affect middle finger and dorsal hand. Image courtesy of Bryngelson-Lambert, Mary, APRN, C.N.P., M.S. (Right): Clinical photo of affect middle finger, lateral view. Image courtesy of Bryngelson-Lambert, Mary, APRN, C.N.P., M.S.
She returned to clinic 4 days later for a recheck of her symptoms. She was again afebrile. The patient had reported improvement since starting the antibiotic course particularly in her systemic symptoms and the swelling and redness.
On exam, swelling and erythema was again noted on the radial aspect of the left third digit at the base with a hard palpable mass measuring 5 mm. However, there was no spreading of erythema to the palm or dorsum of the hand. A repeat point-of-care ultrasound was performed, visualizing a cyst-like structure, raising the possibility of an abscess. An I&D was performed. An #11 blade was used to make a stab incision. There was no immediate drainage of fluid after the incision was made. Therefore, a significant amount of pressure was applied to the area around the incision. Ultimately a small tan nodule was expressed as a solitary mass in entirety, with no liquid, and the specimen was sent to pathology.
The gross description of the specimen was: “0.9 cm × 0.7 cm × 0.4 cm tan-gray irregular soft tissue fragment with no grossly identifiable skin surface.” The final diagnosis from pathology “SOX10 positive spindle cell proliferation with extensive central degenerative and hemorrhagic changes” consistent with a schwannoma (Figures 2 and 3).

Hematoxylin and eosin (H&E) stain of benign schwannoma at 40× magnification.

Immunohistochemical staining shows lesional cells positive for SOX10.
The patient was not seen again in person for follow-up but did report 2 weeks later that the lesion had healed up well and that she had no further pain or symptoms.
Discussion
Peripheral nerve sheath tumors (PNST) represent a diverse group of neoplasms. Schwannomas are the most common type of PNST followed by neurofibromas and much less commonly malignant peripheral nerve sheath tumors (MPNST). 1 Schwannomas and neurofibromas make up 10% to 12% of benign soft tissue neoplasms. 1 Schwannomas may occur sporadically or as part of neurofibromatosis type 2 or schwannomatosis. 2 Peripheral schwannomas have an incidence of 0.6 per 100 000 people annually. The majority are located at upper or lower limbs and chest.1,3-6
Peripheral nerve schwannomas are usually solitary, round, smooth, slow growing, and well-encapsulated averaging 1 to 4 cm in size.2,4,5 There is not a clear correlation between initial tumor size, patient age at diagnosis, and tumor growth rate.1,2 Incidence is equal between men and women. 5 Usually, patients present in the fourth or fifth decade of life with a painless, palpable swelling. 5 There may be symptoms such as numbness, tingling, or burning. Differential diagnosis often includes ganglion cyst, lipoma, fibroma, Dupuytren’s contracture, or hemangioma. Infectious schwannomas are possible but rare and may be mistaken for an abscess or malignant tumor in the case of rapid growth. 6 Evaluation on presentation usually begins with ultrasonography identifying a solid, sharply delineated, hypoechoic homogenous mass. X-ray may be obtained to exclude bony involvement. MRI may illustrate iso-intensity or show decreased signal intensity relative to skeletal muscle on T1-weighted images and heterogeneously increased signal intensity on T2 weight images. 4
Complete surgical excision is curative and prognosis is excellent with low chance for recurrence. 5 Open biopsy before complete enucleation is recommended to avoid undertreating in the case of malignancy. Histopathology of the excised lesion is the gold standard for a definitive diagnosis. 4 Findings include classic features of schwannomas including a biphasic pattern of alternating Antoni A and B areas. “Ancient schwannomas,” which are often large and long-standing, may have other histopathologic findings including marked nuclear atypia and cyst formation, calcification, hemorrhage, and hyalinization. 7 They will stain positive for S100 and SOX10 owing to their neuroectodermal origin.5,6 MPNST arising from schwannomas are extremely rare but among all soft tissue tumors, MPNST have one of the worst prognosis with high rates of local recurrence and metastasis. 3 Therefore, it is important to be aware of their infrequent association with peripheral schwannomas.
In the above case, the initial presentation seemed most consistent with an infectious process as patient endorsed pain, redness, warmth, and subjective fevers. These features are not typical for schwannomas. Ultrasonography was utilized at the first and subsequent visit identifying a discrete, round, walled off cystic structure which was thought to be fluid filled. Cysts can be anechoic to hypoechoic on imaging as can schwannomas. Unexpectedly, on excision the mass was solid rather than fluid filled. The specimen stained positive for SOX10 helping to formally identify it as a schwannoma. This case illustrates the importance of utilizing numerous diagnostic modalities, most importantly histopathology, when dealing with soft tissue masses that do not behave as expected.
Conclusions
Schwannomas, while the most common peripheral nerve sheath tumor, are typically slow-growing and painless. Their presentation as an apparent infectious process, as seen in this case, is rare and poses a diagnostic challenge. This case highlights the importance of maintaining a broad differential diagnosis, even when initial findings suggest a more common condition like cellulitis or abscess. While point-of-care ultrasound can be a valuable tool in evaluating soft tissue masses, its findings must be interpreted in the context of the clinical picture. In this instance, the ultrasound initially suggested a fluid collection, contributing to the suspicion for an abscess. However, the subsequent lack of fluid drainage upon incision and drainage, coupled with the unusual appearance of the excised tissue, prompted pathological examination, which ultimately led to the correct diagnosis. Although schwannomas are benign and typically cured with complete excision, an atypical presentation can mimic alternative conditions. Therefore, clinicians should consider peripheral nerve tumors in the differential diagnosis of soft tissue masses, especially when the clinical course is unexpected or fails to respond to standard treatment. This case highlights the value of surgical pathology in establishing a definitive diagnosis and preventing misdiagnosis, which can have significant implications for patient management. While the incidence of malignant transformation in schwannomas is low, awareness of this possibility is crucial for long-term patient follow-up and surveillance.
Footnotes
Ethical Considerations
Ethical approval not necessary.
Consent to Participate
Informed consent for publication was provided by the participant.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
