Abstract
Keywords
Introduction
Patient enablement is defined as the patient’s ability to understand and cope with life and illness after a consultation with a general practitioner (GP).1-4 Although the concept of enablement is not completely consistent across studies, 5 in a review by Anden et al, 6 it is regarded as 1 of the 7 main concepts used to describe and evaluate GPs’ consultations. Patient enablement is suggested to be a good patient-reported outcome measure (PROM) measuring the quality of care in primary health care.2,5-7
As a concept, enablement is paralleled with empowerment, which, in the field of health care, is seen as a process in which the patient develops, for example, skills, knowledge, and confidence in health-related decisions. 8 Empowerment is defined one of the core competencies of patient-centeredness by WONCA Europe. 9 Although empowerment is often used as a synonym for enablement, it is suggested that empowerment is an educational process, while enablement is more comprehensive since it includes managing and coping with illness. 5 Empowerment can also be achieved by the patients themselves, 10 whereas enablement is regarded more as a result of consultation.1,2,5
There are studies indicating that patient enablement leads to better clinical outcomes. In one study, enablement was positively associated with asthma balance adjustment and quality of life. 11 Among patients with type II diabetes, enablement has been associated with lower glycated hemoglobin (HbA1c) and body mass index (BMI) levels. 12
A study by Mercer et al 13 categorizes factors influencing enablement into patient, consultation, and system factors. Among patient factors, study results with regard to the patient’s age are contradictory.2,3,14,15 Patients with different ethnic backgrounds report different enablement perceptions than natives.2,3 A worse state of health 13 and the presence of a chronic illness3,13 have been associated with lower patient enablement.
A recent review of 24 studies indicated that the length of the consultation was one of the most investigated factors, being positively correlated with enablement in 8 out of 9 studies. 5 The patient’s partnership with the doctor,16,17 the GP’s communication skills,3,18,19 a more person-centered approach,15,19,20 and patient involvement in decision making19,21 may promote enablement. In addition, enablement is related to patient satisfaction. 5
When regarding system factors, continuity of care has been positively associated with enablement in several studies.2,3,15 Moreover, larger GP practice sizes 2 and poorer access to care 22 have been negatively associated with enablement.
Previous studies have shown that there could be cultural differences in terms of enablement both between different ethnic groups inside countries2,3 and between countries.23,24 To our knowledge, there are only a few studies on enablement in the Nordic countries: 2 studies have been conducted in Sweden21,25 and 1 doctoral thesis in Finland has touched on enablement in a minor way. 26
In terms of measuring enablement in general practice, Howie et al 1 have developed the Patient Enablement Instrument (PEI), a 6-item, 3-scale questionnaire about patients’ perceptions of their ability to understand, cope, and manage with their illnesses and lives after a consultation. PEI has been widely used in studies conducted in several countries.2,15,20,23-26 There is also a 3-item version of PEI available, 3 which has been used in 2 large studies.14,22 Furthermore, in the international Quality and Costs of Primary Care in Europe (QUALICOPC) study (the QUALICOPC study design was approved in October 2011 by the Ethics Committee of the Tampere Region (permission number R11153), a single question, “Think about the doctor you visited today. Do you agree the following? ‘After this visit, I feel I can cope better with my health problem/illness than before’,” was designed based on the PEI questionnaire. 27
The aim of this study was to investigate patient enablement measured by one question presented after a GP appointment at a primary health care center in Finland. We will analyze factors associated with patient enablement, and by comparing with earlier studies, we try to evaluate, if a single question method can be used to measure enablement.
Methods
We used Finnish data collected for the international QUALICOPC study, which is targeted to evaluate the primary health care systems of 31 European countries plus Australia, Canada, and New Zealand. The background and the design of the QUALICOPC study as well as the international process of developing the study questionnaires is described elsewhere.27,28 The original questionnaires were translated from English to Finnish and validated by back translation to English.
According to the QUALICOPC study design, the goal was to reach 220 GPs in each country and nine patients for each GP to fill out the Patient Experience questionnaire. The Finnish data were collected in 2012. The purpose was to get a random sample of Finnish GPs; postal questionnaire was sent to 700 GPs using the register of Finnish Medical Association. Unfortunately, the response rates were so low that complementary recruitments, that is, sending questionnaires to GP specialist trainees in Pirkanmaa Hospital District area and contacting health centers directly, were needed. The process of gathering the study sample is presented in Figure 1.

Gathering of the study sample of Finnish general practitioners (GPs) and their patients for the QUALICOPC study.
Ultimately, a total of 139 GPs (one GP per health center/station) agreed to participate in the study according to the protocol. The patients were recruited by a trained fieldworker. Over a period of 1 day, a fieldworker asked all the patients visiting the participating GP to fill out the questionnaire in printed form, immediately after the appointment. Two to 9 patients per GP were recruited, altogether 1196, with a median of nine patients and a mean of 8.6 patients.
We measured patient enablement with the question “Think about the doctor you visited today. Do you agree the following? ‘After this visit, I feel I can cope better with my health problem/illness than before’.” The answer alternatives were yes/no/don’t know. Before the analysis, “don’t know” responses were combined with the “no” responses.
Based on the existing literature on factors that may affect patient enablement, we included a large number of variables in our analyses. The questions in the QUALICOPC study questionnaire were distributed in theme groups, presented in Table 1.
Numbers of Questions in QUALICOPC Study Distributed Into Theme groups.

The themes “previous experience” and “health promotion” were designed by the authors; these were not included in the original QUALICOPC design. There is no direct research on the link between previous experience and enablement, but previous experience—particularly negative “surprises” in care—is known to influence patient satisfaction. 29 Furthermore, discussing health promotion issues with the doctor was an independent predictor of patient enablement in one study. 20
In the statistical analysis (IBM SPSS, version 23), descriptive statistics and cross-tabulation were used to find the variables showing the strongest association on patient enablement. The variables were first tested with bivariate logistic regression analysis. Next, because of the large number of variables, forward-stepwise, multivariable logistic regression analyses were performed using theme groups. All statistically significant (P < .05) factors in the theme group analyses were included in the final multivariable model, which was performed with the enter method to find the variables with an independently significant association on enablement. Finally, to consider potential variation of enablement depending on GP level, multilevel modeling was used, that is, generalized linear mixed-effect models were fitted using a function glmer in the R Software environment for statistical computing and graphics, version 2.13.0; a random intercept was used to account for the variation in the number of patients per GP.
Results
A total of 1196 patients completed the QUALICOPC Patient Experience questionnaire. The distributions of the demographic factors are presented in Table 2. The mean age of the patients was 59 years (range 18-97 years), and 51.5% were older than 65 years. In response to the item “After this visit, I feel I can cope better with my health problem/illness than before,” the patients’ answers were distributed thus: 898 patients (75.1%) selected “yes,” 36 patients (3.0%) selected “no,” 233 patients (19.5%) selected “don’t know,” and 29 (2.4%) answers were missing.
Distribution of the Demographic Factors (n = 1196).

In the bivariate analyses, 19 statistically significant factors (P < .05) were found (data not shown). Among patient factors, state of health and ethnicity/language skills were significant. Among consultation factors, significant factors included variables reflecting doctor-patient communication (4 questions), patient satisfaction (4 questions), and previous experience (1 question on health promotion, 1 question on discrimination, and 3 questions on practice safety). Among system factors, all 4 questions reflecting continuity of care were significant.
Results of the multivariate theme group analyses are presented in Table 3. All 11 statistically significant (P < .05) factors in these analyses were entered in the final multivariable model, the results of which are presented in Table 4. All models were adjusted for age and gender. In the final model, the strongest positive association was found with questions reflecting patient satisfaction and doctor-patient communication. The strongest variable reflected patient satisfaction (a “yes” answer to the question “This doctor doesn’t just deal with medical problems but can also help with personal problems,” odds ratio [OR] 3.42, 95% CI 2.40-4.85, P < .001). In addition, patient’s lower level of language skills had a negative association with the dependent variable. The interpretation of the results did not change after taking into account the clustered nature of the data by multilevel modeling.
Results of the Multivariable Theme Group Analyses on the Patients’ Perceived Enablement Measured by a Single Question, Yes/No a (All Models Include Age and Gender).
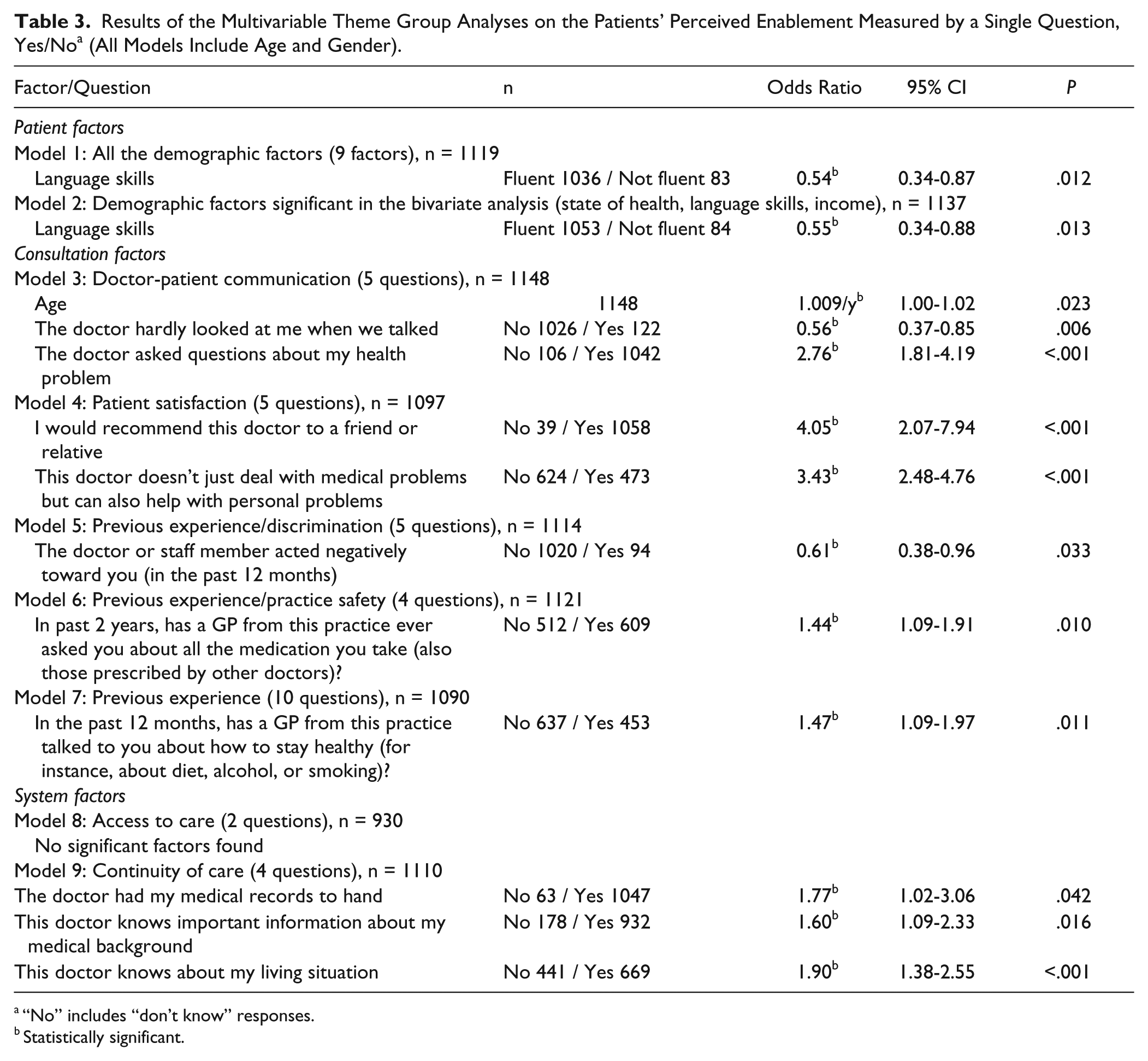
“No” includes “don’t know” responses.
Statistically significant.
Model includes factors significant in the multivariable theme group analyses, adjusted for age and gender (altogether 13 factors), n = 1081.
“No” includes “don’t know” responses.
Statistically significant.
Discussion
According to this questionnaire study using Finnish QUALICOPC data, approximately three-quarters of the respondents agreed they felt better able to cope with their health problem or illness after a consultation with a GP, reflecting patient enablement. In our final multivariable model, none of the system factors and only one of the patient factors, namely language skills, had a significant association with enablement. Of the consultation factors, aspects of patient satisfaction and doctor-patient communication had a statistically significant association with patient enablement.
In this study, many results were parallel to previous studies that used longer versions of PEI.1-5,14,18,20,26 For instance, positive answers to questions reflecting patient satisfaction (“I would recommend this doctor to a friend or a relative” and “This doctor doesn’t just deal with the medical problems but can also help with personal problems”) had the strongest positive association on enablement. This finding is consistent with previous studies that found patient satisfaction to be associated with enablement.4,5 Although the relationship between enablement and patient satisfaction is close, they are regarded as separate concepts.2,4,6 Patient satisfaction is considered to be influenced by the fulfilment of the patient’s expectations,29,30 while enablement is considered to be less dependent of expectations.18,31 A patient might feel satisfied with the care received without feeling enabled, and possibly vice versa. In addition, the patient’s perception that the doctor is able to deal with other problems than just medical ones may reflect the GP’s holistic approach and good patient-doctor partnership, which have been suggested to promote enablement.16,17,20
Furthermore, there is evidence of an association between doctor-patient communication and enablement.3,18,26 Especially doctor’s empathy has been strongly associated with enablement.13,32 In this study, the question “The doctor asked questions about my health problem” showed a rather strong positive association with enablement. It seems reasonable that if the patient feels the doctor is interested in his or her present issue, feelings of ability, confidence, and coping are more likely to be achieved. It is noteworthy that 106 patients (10.2%) answered “no” to this question. This is rather a large proportion, indicating that there may be room for improvement in doctor-patient communication during GP appointments.
When considering patient factors influencing enablement in our study, none of the demographic factors besides patient’s language skills were significant. In previous studies, patient speaking other languages have provided higher scores of enablement compared with natives.2,3 In our study, speaking Finnish not fluently had a negative association with enablement, which may imply that those patients have had difficulties when communicating with doctors. Challenges in language and communication might lead to misunderstandings between doctor and patient and thus harm the ongoing process of care.
Strengths and Limitations
The survey data were collected to examine core aspects of primary health care on a large scale. Patient enablement was not the main focus of the survey, which limits the opportunities of the investigation. On the other hand, the diverse questionnaire made it possible to take into account multiple factors influencing patient enablement. In earlier studies, one limitation in multivariable and multilevel modeling has been the large number of missing values, meaning that not all of the respondents could be included in analyses.3,33 One strength of our study is that despite the large number of variables, there were few missing values and the majority of the respondents (90.5%) could be included in the multivariable analysis. This suggests good quality data and acceptability of the questions. However, the data collection method in this survey might cause a potential cluster effect because answers could vary depending on individual GPs; we took this into account with the multilevel modeling.
This study was supposed be based on a random sample of Finnish GPs and their patients. Unfortunately, the response rate remained exceptionally low like in many other countries in the QUALICOPC study. 34 The response rate among GPs varied a lot between countries (from 6% to 79 %), and the goal of getting a random sample of GPs realized only in two-thirds of the countries. 34 Possibly GPs did not want to participate because they did not want their patients to be involved in the process. In Finland, we had to use complementary data collection techniques. The difficulties in the GP recruitment process could have distorted the sample; for example, the participating GPs might have had more positive attitude toward research.
However, the current sample of patients includes a large number of patients from both urban and rural areas. There were patients from all the age groups and the age distribution correlates well with the national register profile of all the patients who used Finnish health centers in year 2013. 35 We therefore regard that the sample represented the overall situation in Finland fairly well. Because of the completing data collection methods needed, only geographical representativeness may have suffered with emphasis placed on the situation in western Finland.
Our dependent variable (“Think about the doctor you visited today. Do you agree the following? ‘After this visit, I feel I can cope better with my health problem/illness than before’”) was a single question with no Likert-scale answer alternatives. A similar approach has been used before; Rohrer et al. measured empowerment with a single question 19 . Furthermore, Mead et al 14 used the categorization “not enabled” (PEI score 0) vs “enabled” (PEI score other than 0) in their study. Nevertheless, this question has not been used before and its validity in measuring enablement has not been tested. However, the results of our study, while comparable to earlier studies, encourage us to continue studying this question.
There is evidence that a shorter, 3-item version of PEI is as reliable as measuring enablement with the 6-item questionnaire, 3 which supports the idea that also a single question based on PEI could be used for measuring enablement. Nevertheless, our dependent question—as well as PEI itself in the Finnish context—needs further investigation to determine reliability and validity.
Conclusions
Demands and needs in health care are increasing rapidly due to growing wealth, information, and knowledge. Therefore, it is important to focus on processes and procedures that have real impacts—particularly benefits—on the patient’s life and health. It is important to find outcomes for measuring clinical practice. In addition, if the patient achieves feelings of ability and better coping after seeing a doctor, it is significant in itself. Good patient satisfaction and doctor-patient communication are associated with higher enablement. This confirms the idea that we should devote to better doctor-patient interaction, in order to achieve better patient outcomes. Because of the characteristics of the data, the findings of this study should be considered preliminary. We will continue with further investigations on enablement and its measurement by a single question.
Footnotes
Authors’ Note
The data that support the findings of this study are available from NIVEL (The Netherlands Institute for Health Services Research) but restrictions apply to the availability of these data, which were used under license for the current study, and so are not publicly available. Data are however available from the authors on reasonable request and with permission of NIVEL.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The research summarized in this supplement is part of the European QUALICOPC study, which is coordinated by NIVEL (The Netherlands Institute for Health Services Research) and funded as part of the European Commission’s Seventh Framework Programme (FP7/2007-2013) under grant agreement 242141. This study was financially supported by the Competitive State Research Financing of the Expert Responsibility Area of Tampere University Hospital (grant numbers 9N030 and 9R024). We also thank Finnish Association for General Practice (SYLY) for financing this article.

