Abstract
Racial disparities in health outcomes in the United States are well documented. 1 The effect of neighborhood characteristics on health and racial differences in access to care are thought to contribute to these disparities.2,3 Access to primary care is of particular concern because of its role in prevention, chronic disease management, and as an overall entry point to the health care system. 4 We previously examined one dimension of access 5 —spatial accessibility—in a large urban center (Philadelphia, PA) and found that neighborhood racial composition more than any other factor was associated with large variations in neighborhood-level primary care supply. 6 After adjusting for other demographic factors and insurance coverage rates, the odds of African American predominant neighborhoods (>80%) being in a low access area were nearly 50 times greater than the odds in neighborhoods with few African Americans (<20%).
The Patient Protection and Affordable Care Act (ACA) has led to historic gains in coverage with low income and minority populations experiencing the largest increases. 7 However, there is concern that despite being insured, individuals living in areas with less primary care could face long wait or travel times.8,9 Community health centers (CHCs) are federally funded primary care centers located in medically underserved areas or near medically underserved populations. The ACA increased funding for CHCs to help meet the goal of increasing primary care supply in shortage areas. Past work has shown that CHCs improve access to high quality primary care for at-risk populations, while decreasing hospitalization rates and use of emergency departments in the states and counties that they serve.10-12 Furthermore, states with more CHCs have lower racial disparities in health outcomes. 13 Despite these observed associations, the contribution of CHCs to reducing racial disparities in spatial accessibility is not well described.
Given the growing role of CHCs in the United States and racial disparities in primary care access,
14
we sought to understand the geography of primary care in a large urban area. Our objectives were to (
Methods
As previously described, 6 we developed an inventory of all adult primary care practices in Philadelphia County and neighboring zip codes. A trained research assistant called each practice and administered a short survey to measure the number of primary care providers (PCPs) including nurse practitioners and physician assistants and approximate hours worked by each. CHCs were identified from lists provided by the Philadelphia Department of Public Health and two Philadelphia-based organizations representing Federally Qualified Health Centers (FQHCs).
We calculated population-to-provider ratios for each census tract. Census tracts were used as the unit of analysis because they represent the smallest geographic unit that corresponds to neighborhoods and they also allow for the use of important health insurance variables from the American Community Survey. Drive times from the centroid of each census tract to every full-time equivalent provider were retrieved from the Google Maps Distance Matrix API 15 and based on optimal driving conditions (ie, not limited by traffic congestion). Adult population data from the American Community Survey 2008-2013 5-year estimates were used to calculate 5-minute drive-time provider-to-population ratios. Using these ratios, we identified low-access clusters, areas with 5 or more contiguous census tracts in the highest quintile of adults-per-PCP ratios (lowest supply). This is a relative rather than absolute measure as there is no empirically derived or consensus definition of the optimal supply of primary care. Additionally, a binary variable was created to indicate whether or not a census tract was within a 5-minute drive of any CHC. We elected to use a relatively short (5-minute) travel time for several reasons. First, though the optimal or maximal distance to primary care is unknown, convenient access to primary care is thought to be important. Second, the travel times in our study do not account for traffic congestion or differential modes of transportation, which could substantially increase travel times in an urban area. A drive time of 5-minutes corresponded to approximately 1.4 street miles. In this article, we define “close proximity” to a CHC as less than or equal to a 5-minute drive time.
Census tract characteristics, including median age, percent African American, percent Hispanic, percent of adults 18-64 without insurance, and percent of adults aged 18 to 64 years with public insurance were derived from the American Community Survey 2008-2013 5-year estimates. Demographic variables were categorized based on the underlying population distribution for the study area.
The number of CHCs and providers at CHCs were calculated. Descriptive statistics were used to assess the characteristics of census tracts in close proximity to a CHC compared with those that are not. We then assessed adjusted associations between proximity to a CHC and neighborhood characteristics using multiple logistic regression. Models included the sociodemographic characteristics of census tracts as well as insurance coverage rates (ie, public insurance rates among adults younger than 65 years and uninsured rates). We excluded median income from models due to high correlation with insurance coverage rates.
Descriptive statistics and multiple logistic regression were then used to assess the association between close proximity to a CHC and risk of being in a low access cluster. In order to determine whether the effect of proximity to a CHC on being in a low access cluster varies by a tract’s racial composition, we also tested a model that included an interaction term between census tracts’ proportion of population that is African American and being in close proximity to a CHC.
This study was approved by the University of Pennsylvania Intuitional Review Board.
Results
We identified 472 primary care office sites. At these sites, there were 1665 full-time equivalent (FTE) primary care providers. Of these, 35 offices (7.4%) were CHCs, with 189 (11.4%) primary care provider FTEs. The median adult per PCP ratio for census tracts in Philadelphia was 823:1.
In unadjusted analyses (Table 1), census tracts with higher rates of uninsurance and public insurance (Figure 1), larger proportions of African American or Hispanic residents, higher population density, and lower median age were more likely to be in close proximity (<5-minute drive time) to a CHC. However, in adjusted analyses only insurance rates (public insurance, uninsured) and population density were associated with proximity to a CHC. Census tracts with high rates of public insurance were more likely to be in close proximity to a CHC (30%-39% vs <10%, odds ratio [OR] = 7.84,
Unadjusted and Adjusted Associations of Census Tract Characteristics and Being in Close Proximity to a Community Health Center (CHC). a
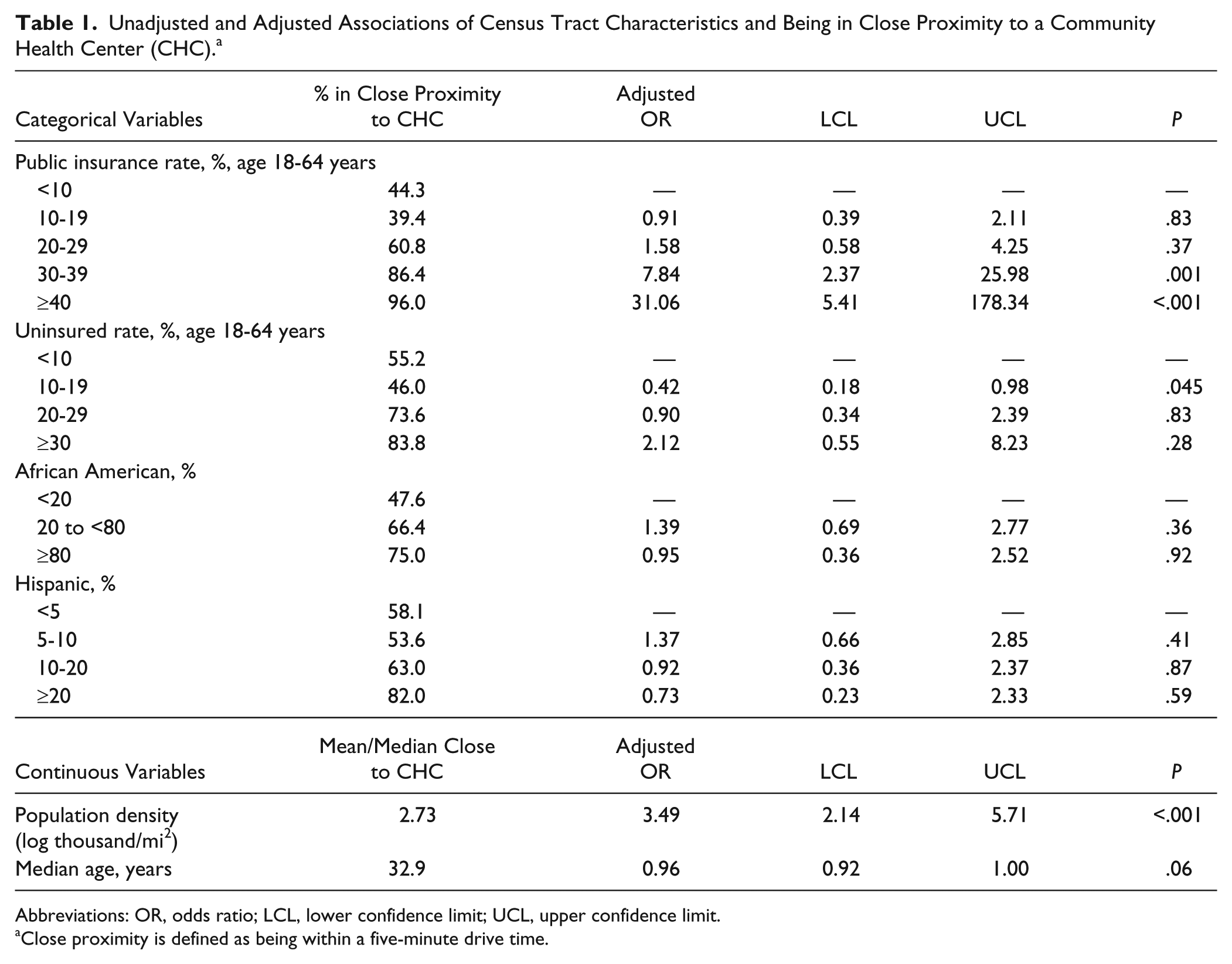
Abbreviations: OR, odds ratio; LCL, lower confidence limit; UCL, upper confidence limit.
Close proximity is defined as being within a five-minute drive time.
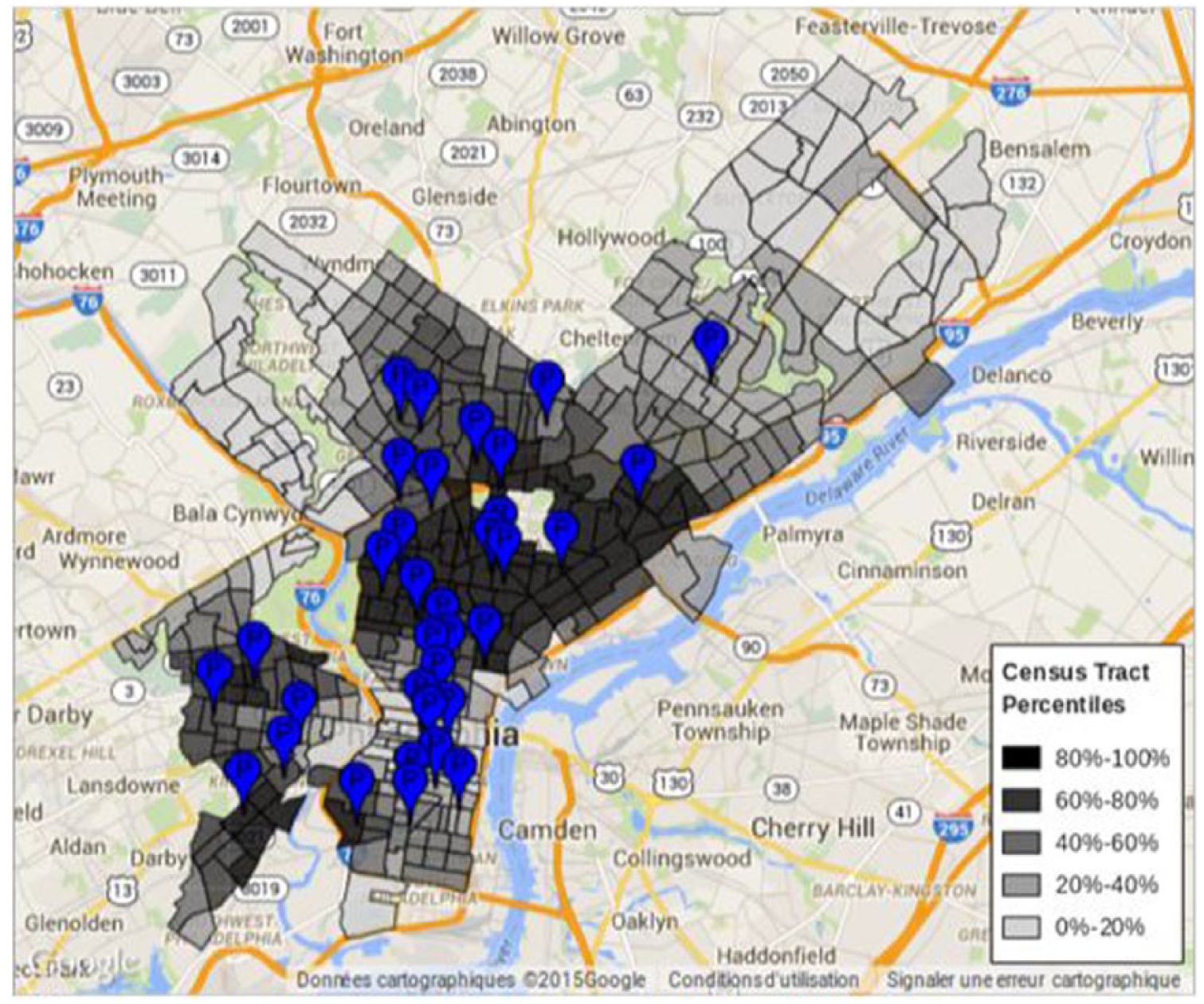
Location of Community Health Centers Relative to Public Insurance Rates. Flags represent the location of community health centers. Census tract colors correspond to public insurance rate percentile.
We previously identified low access primary care areas in Philadelphia.
16
These were areas with 5 or more contiguous census tracts in the lowest quintile for population-to-primary care provider ratios. In adjusted analyses, (Table 2), census tracts that were in close proximity to a CHC were less likely to be in a low access area (OR = 0.11,
Adjusted Associations of Proximity to CHC and Low Access Cluster With and Without Interaction.
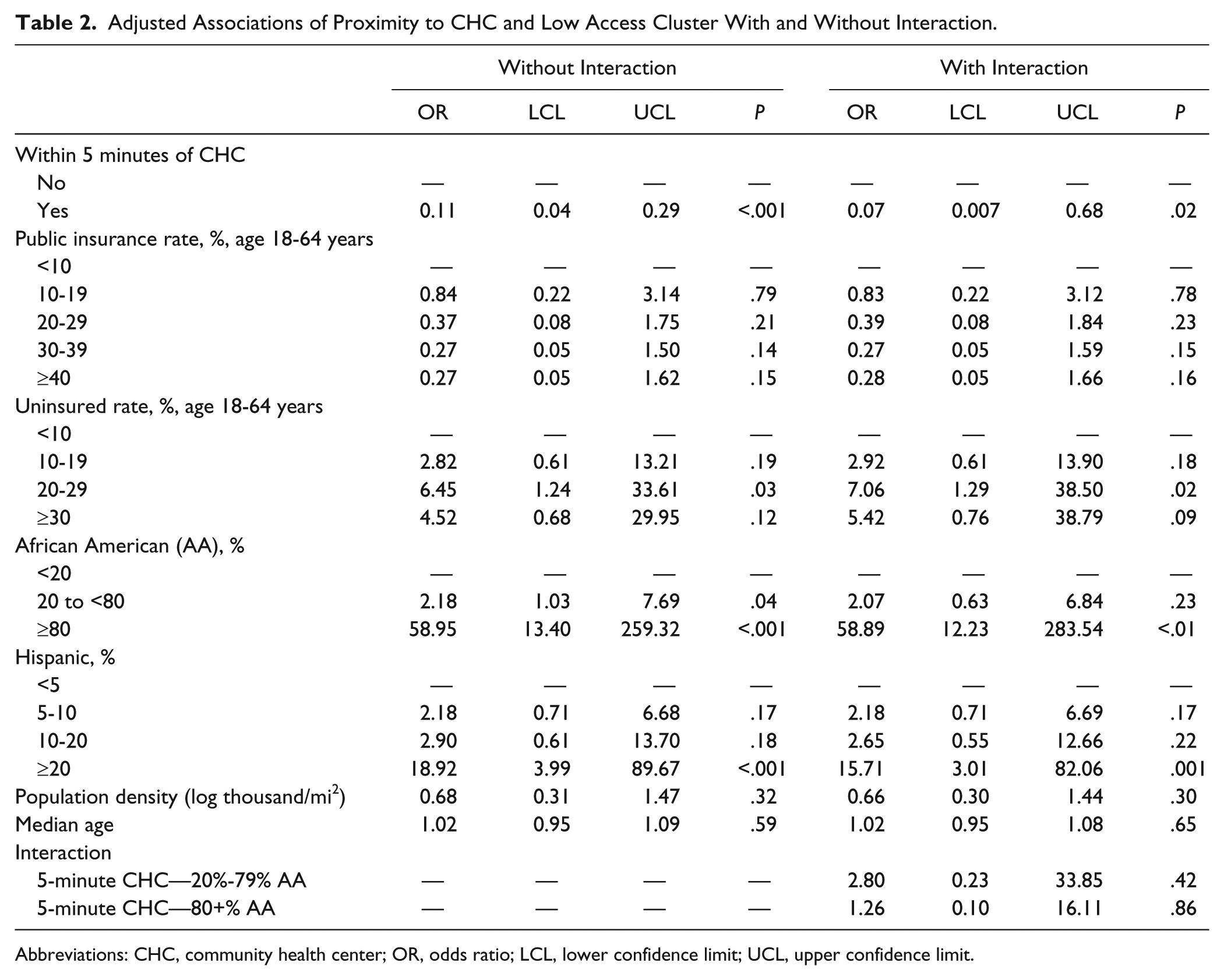
Abbreviations: CHC, community health center; OR, odds ratio; LCL, lower confidence limit; UCL, upper confidence limit.
Discussion
Overall, CHCs represented 7.4% of all primary care sites and 11.4% of primary care providers in this major urban center. We found that the location of CHCs was associated with population density and public and uninsurance insurance rates but not with the racial composition of the surrounding neighborhood. These results indicate that CHCs are more likely to be in areas with a greater fraction of racial minorities; however, that seems to be influenced by public insurance rates rather than race itself. Furthermore, although we found that proximity to a CHC was associated with decreased risk of being in low access areas, that effect did not vary by a tract’s racial composition. Thus, while CHCs undoubtedly improve access to care, neighborhoods with high fractions of racial minorities remain at greater risk of lower primary care supply.
It is not surprising that CHC location would be influenced by public insurance rates rather than the racial composition of the surrounding area. Financial sustainability for CHCs depends on having a high proportion of publicly insured patients, as opposed to uninsured patients. The Prospective Payment System (PPS) reimburses FQHCs at a higher rate than other Medicaid providers in part to improve financial sustainability. In addition, applying for FQHC status requires demonstration of financial sustainability. Thus, it is it natural that FQHCs would specifically focus on locating in areas with high rates of public insurance rather than specifically focus on areas with high proportions of racial minorities. The special populations targeted by CHCs include migratory and seasonal workers, the homeless, and residents of public housing. These programs include outreach appropriate to these populations. If policy makers hope to target racial disparities in access to care, identifying neighborhoods with high fractions of racial minorities and poor spatial access to primary care is a first step. However, creating new incentives for CHCs to locate in these areas, and thus provide protective effects for these neighborhoods, will be a critical second step.
There are several limitations to these results. These findings are in the context of a large, racially diverse urban center with multiple CHCs and high overall primary care supply. The effect of CHCs may differ in a location with low levels of primary care supply or in rural areas. CHCs’ role in reducing racial disparities may also differ in areas with a lower percentage of African Americans overall. Furthermore, based on available data, this study did not account for alternative modes of transportation such as walking or public transit which may be particularly important to the populations that are a priority for CHCs. Future studies should examine how spatial accessibility differs based on mode of transportation and the implications for racial disparities in access. Finally, our study did not examine how spatial accessibility translates to utilization of care and health outcomes. Prior studies examining this relationship in urban areas have found mixed results which could in part be explained by the multitude of factors influencing how patients access care and preferences for different types of providers. 17
Reducing racial disparities in health outcomes is a national priority. Ensuring access to primary care is an important step toward reducing these disparities. While federal programs that support CHCs can go a long way toward improving access in low-income communities, a more explicit focus on racial disparities may be needed to reduce racial disparities in access in areas where current incentives based on public insurance rates fall short. In order to address identified racial disparities in spatial access to primary care, areas with higher proportions of racial minorities would need to be prioritized in decision making regarding the placement of primary care sites, including CHCs. These findings further demonstrate the benefit of CHCs on spatial access to care and may be a strong tool in ensuring access in the most at-risk communities.
Footnotes
Acknowledgements
The authors thank the Independence Foundation (Philadelphia, PA) for their financial support of this work.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was financially supported by the Independence Foundation (Philadelphia, PA). JWS is funded through the Boston University Reproductive, Pediatric, and Perinatal Epidemiology predoctoral training grant.
