Abstract
Worldwide, 25% to 50% of people have mental disorders. 1 Prevalence of psychological distress in Mexican primary care facilities is 66.7%, 70.6% among women and 52.5% among men as of 2011. 2 Yet there is a discrepancy between the prevalence of mental disorders and the seeking of treatment3-6: the interim between acquiring a mental illness and seeking treatment is 14 years for mood disorders and 30 years for anxiety disorders. 3 This is especially concerning to Mexican women, who are more likely than men to have psychological distress, 2 yet only seek treatment 16% of the time. 7
This underutilization is exacerbated by underfunded primary care: 70% of primary care facilities lack equipment required to diagnose mental illnesses, and Mexico is second to last place worldwide with regard to the quantity of psychiatrists per 100 000 people. 8 Additionally, primary care providers (PCPs) working in seriously underfunded health facilities are constrained to preventive and general care, limiting the services available to low socioeconomic status (SES) populations. 9 This is detrimental because PCPs who provide widespread mental health services, such as distributing treatment-promoting information, inquiring about stress or worries, and referring patients to mental health providers (MHPs) increases treatment-seeking behaviors.10-15 Consequential of poor primary care, Mexican women tend to directly seek MHPs, who offer treatments low-SES women cannot afford.3,7,16-18 Underfunded primary care tends to be the only affordable option for low-SES women.
Sociodemographic characteristics, and experiences/perceptions of services also affect mental health service seeking behaviors. The following are associated with Mexican American women seeking depression and anxiety disorder treatment: older age19-21, higher education, 22 higher income,18,23,24 and being “married” or “in a domestic partnership.”7,18 Loneliness, financial and family-related worries are also associated with seeking services. 25
Based on mental health primary service trends among Mexican women, we conducted a quantitative investigation seeking predictive factors of service utilization. We expected older age, higher income, and education, marriage/coliving, and finances, family, and loneliness worries to predict seeking mental health care5,18-25 We also hypothesized receiving mental health information, being referred by a PCP to a MHP, following doctor’s orders, and coping by talking with MHPs would predict seeking care.
The Current Investigation
The current investigation analyzed demographics and experiences among Mexico City women’s mental health treatment seeking through 3 objectives: (1) analyzing associations of seeking mental health services, (2) developing a predictive model of women likely to seek these services, and (3) providing suggestions that may increase mental health treatment.
Methods
Data was extracted from a 2-part multimethods study assessing primary care patients’ mental health beliefs and behaviors through (1) observations and 35 semistructured interviews in 19 primary care clinics and (2) questionnaires administered to convenience sample of 566 workers and 529 general health care users in 82 primary health care clinics.23,26
Participants
The current study focused on female participants, N = 456. The inclusion criteria included (1) being older than 14 years, (2) currently utilizing primary care, (3) being willing and able to share primary care experiences through the questionnaire, and (4) willingly providing informed consent. Interviewed women utilized primary care for various reasons not limited to mental health.
Procedures and Measures
Measures
Questionnaire measures from the larger study were validated for accuracy and precision through a pilot study. 24 Our mental health service usage literature led us to focus on the following measures:
Demographic variables
Age, gender, household income, number of dependents, occupation, education, and marital status data were collected.
Use of health care resources and services
Participants answered polar questions about attempts to alleviate physical and psychological ailments to operationalize health care use. Participants specified the physical or psychological ailment and the last time the resource (eg, vitamins) was used as treatment.
Experiences during the doctor’s appointment
Participants shared about the time PCPs spent with them, actions PCPs took during the consultation, and whether they followed the PCPs’ orders.
Knowledge of mental health information
Participants answered polar questions about whether they received mental health information at health centers and its content.
Attention to mental health
Participants ranked worries on a scale from 1 (primary worry) to 7 (least important worry). Only primary worries were considered for chi-square analyses. Participants answered polar questions of actions taken when worried (eg, hold it in, seek a priest, seek medical care) to operationalize personal attention on mental health.
Data Analyses
Two trained members of the research team created the coding handbook and coded the questionnaires. Two trained psychologists analyzed the data using statistical software SPSS and STATA. Missing data were removed and preliminary analyses confirmed normality. Frequencies, bivariate correlations and chi-squares analyzed scale and categorical responses. A sequential logistic regression analyzed predictors of seeking mental health services.
Ethical Considerations
The Instituto Nacional de Psiquiatría “Ramón de la Fuente Muñiz” granted the overarching study IRB approval. Ethical considerations included participants giving informed consent prior to answering the questionnaire, permission from each primary care clinic to conduct studies on their patients, and the current study being made anonymous.
Results
Descriptives
Women’s ages ranged from 17 to 79 years; 59.4% of women were younger than 40 (M = 37.56 years, SD = 15.49,). Nearly half (49.4%) of women had a household salary of minimum wage or less (minimum wage = MXP2018.70 or US$108 per month), and only 30% completed high school. Most women (68.9%) self-identified as homemakers and had M = 3.25 dependents (SD = 1.36). Most women (70.8%) were married or coliving with a significant other (see Table 1).
Descriptive Characteristics of the Sample (N = 456) and Factors Associated With Seeking Mental Health Services Using Chi-Square Analyses.
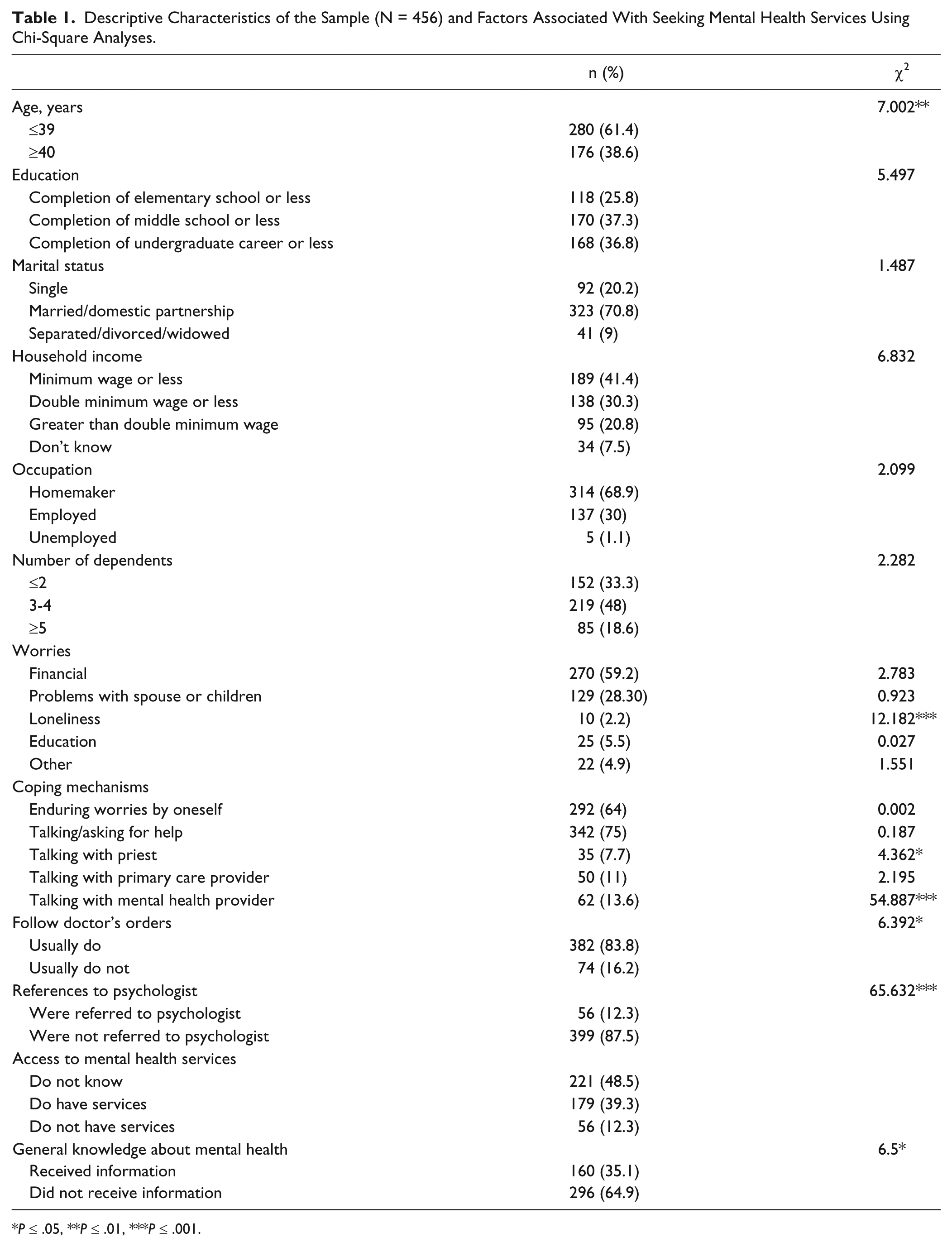
P ≤ .05, **P ≤ .01, ***P ≤ .001.
Attention to Mental Health
Only 25% of women knew their closest medical center offered mental health services and 48.5% were unsure. Moreover, 65.6% of women had never received written or verbal mental health information, although 86.4% desired it.
With regard to personal mental health, 68.2% of women reported their PCPs never inquired about their emotional problems, and only 12.3% of PCP’s prescribed medication or MHP care. Yet 45.6% of women did not agree with their MHP’s instructions and 65.8% did not entrust any medical center personnel with personal problems.
Factors Associated With Seeking Mental Health Services
Chi-square tests of independence revealed the following associations with seeking primary care mental health services: being at least 40 years old, χ2 = 7.002, P = .01, using the coping mechanisms talking with a priest (χ2 = 4.362, P = .04) or talking with MHP (χ2 = 54.887, P = .00), following doctor’s orders (χ2 = 6.392, P = .01), being referred to a psychologist (χ2 = 65.632, P = .00), and receiving general information about mental health (χ2 = 6.500, P = .01). Loneliness, compared with other primary worries, made women more likely to seek services, χ2 = 12.182, P = .00.
Predictors of Seeking Primary Level Mental Health Care
We excluded women without mental health service access and those unsure if they had it, leaving n = 169 participants. Our chi-square results and literature review guided the following factor regressions with seeking care: age, income, education level, marital status, being referred to a MHP, following doctor’s orders, receiving mental health information, worrying about loneliness, financial, or family problems, and the coping mechanisms talking to a priest or MHP.
Our model (Table 2) showed women referred to a MHP were 10 times more likely to seek mental health services (odds ratio [OR] = 10.81, 95% CI = 3.59-32.51). Women whose coping mechanisms included talking to a MHP (OR = 5.53, 95% CI = 2.10-14.53) and whose primary worry was loneliness (OR = 8.15, 95% CI = 1.20-55.10) were 5 and 8 times more likely to seek services, respectively. Finally, participants who follow doctor’s orders were approximately one-third times more likely to seek mental health services (OR = 0.28, 95% CI = 0.09-0.92).
Sequential Logistic Regression Examining Predictive Factors for Seeking Mental Health Services.
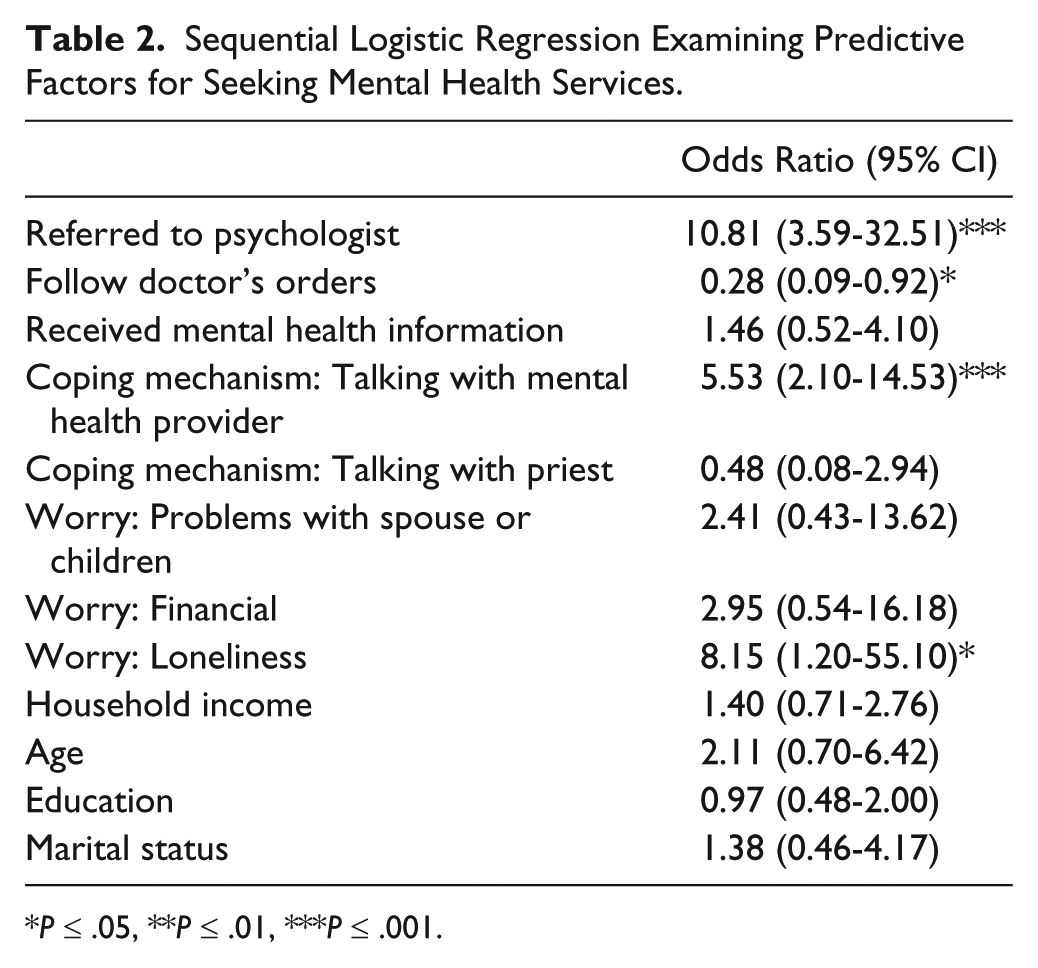
P ≤ .05, **P ≤ .01, ***P ≤ .001.
Discussion
To our knowledge, this is the first study reporting that the strongest predictive factor of primary care mental health treatment initiation by Mexican women is being referred to a MHP by a PCP. Initiating mental health treatment involves: access to appropriate treatment resources, mental health screening, referral, referral acceptance, and treatment initiation. 27 Failure at any of these steps may cause treatment initiation failure. 27 Women being 10 times more likely to initiate mental health treatment if they receive a referral from their PCP suggests that patients with primary care mental health resources that are screened for mental health maladies and referred to MHPs accept referrals and initiate treatment. We posit that the underutilization of mental health services may be a consequence of lack of primary care mental health resources, lack of mental illness recognition, and lack of MHP referrals among PCPs.
Previous research shows that patients only seek mental health services when they receive a referral if the services are integrated into their primary care facility. 27 Additionally, PCPs’ ability to identify and treat mental health problems depends on the availability of treatment resources.28-30 Thus, PCPs’ abilities to recognize mental illness and make appropriate referrals depend on the availability of primary care mental health services.
Considering only 31.8% of our participants’ PCPs inquired about emotional or personal problems and less than 10% of our participants were referred to a MHP by a PCP, we suggest future interventions should prioritize: (1) mental health service integration throughout Mexican primary care facilities and (2) training PCPs on mental illness screening and proper follow-up measures (eg, patient referrals to MHP).
Interventions involving primary care mental health service integration and PCP mental health training have been successfully implemented in Argentina, Chile, Australia, and Brazil. 31 In these countries, PCPs are trained to assess patients’ physical and mental health, treating when capable and referring to a MHP when not. 31 As a result, most PCPs in these countries are able to detect and often even treat mild cases of mental disorders. 31
Our study also showed that women who perceive loneliness to be their primary worry were more likely to seek MHPs. Additionally, loneliness for the women revealed to not refer to the absence of relationships, but to their quality because more than 90% of participants lived with a partner and each woman had 3 dependents on average.32,33 Research shows individuals with frequent feelings of loneliness tend to suffer high rates of depression. 34 Loneliness is not only a precursor to depression, but Mexican women dealing with isolation and loss of family support are also at higher risks of additional mental disorders.35-37 In Mexico, loneliness is perceived as a responsibility of the individual, being especially burdensome because of cultural expectations of family meeting one’s need for companionship.37-39 These perceptions foster the idea that one should “pick oneself up by the bootstraps” to overcome depression when lonely. 40 This may explain why women are more likely to seek mental health services when worried about loneliness. Culturally, loneliness may be perceived as out of the ordinary while other worries—finances, education, or family problems—may be perceived as quotidian and unavoidable to current Mexican society.
Future studies should also consider obtaining a larger, randomized, more representative sample size. We used a small convenience sample rather than random sample. Our study was not only limited in size, but also in gender and location, as well as in the skip logic of certain questions in our survey. Because the questionnaire was not designed specifically for this study, only participants who answered that their primary care facility included mental health services were asked whether they had ever sought such services. Future investigations should also consider patients who sought but did not find services.
Despite its limitations, this study suggests that PCPs play a fundamental role in women’s decisions to utilize primary care mental health services. This leads us to suggest that simple and specific changes (eg, ensuring an adequate amount of MHPs and training PCPs to screen for mental illness) may be implemented to improve early detection of mental illness and referrals to MHPs, as long as mental health services are integrated into the primary care facility.
Footnotes
Acknowledgements
The authors wish to express their gratitude to the Secretaría de Salud del Distrito Federal for allowing us to conduct this study within their primary care facilities, to Dr. Steven Lopez and the NIH-funded Mental Health in Research Training program (MHIRT) at the University of Southern California for providing the resources and support for the authors to conduct this research in Mexico City, and especially to the persons who shared their experiences in questionnaires and made this study possible.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The project of which this study is part was funded by the Consejo Nacional de Ciencia y Tecnología (CONACyT), Grant No. SEP-2011-C01-166588 and by a grant from the National Institute on Minority Health and Health Disparities,T37 MD003405.
