Abstract
Keywords
Introduction
Adolescent pregnancy rates have declined in the United States, yet they remain higher than in most comparable, high-income countries. More than 600 000 adolescent pregnancies annually result in a teen birth rate of 26.5 per 1000 adolescent women aged 15 to 19 years.1,2 The majority of these pregnancies are unintended, and socioeconomically disadvantaged and minority youth are disproportionately represented in these statistics. 3 Comprehensive sexual education and timely, age-appropriate contraception counseling are essential to reduce adolescent pregnancy and its health and social consequences.
Long-acting reversible contraceptive (LARC) devices, which include intrauterine devices (IUDs) and subdermal contraceptive implants, are safe and effective methods with great potential to reduce unintended pregnancies among adolescents. The American College of Obstetricians and Gynecologists and the American Academy of Pediatrics support LARC devices as first-line contraceptive options for adolescents and recommend that pediatric providers educate adolescent patients about LARC methods.4,5
Despite these clear endorsements and evidence that adolescents will choose LARC methods when cost and access barriers are removed, 6 less is known about what adolescents in the general pediatric primary care setting know about LARC methods. Qualitative studies among adolescents in school-based and community health setting have found that many teens are fearful of intrauterine devices, particularly in relation to pain at insertion and possible complications.7-9 A few survey-based studies have examined specific determinants of adolescent knowledge gaps and negative attitudes about LARC methods, yet these studies have recruited participants from gynecology and family planning clinic settings, which may not reflect norms in a primary care environment.10-12 Our objective was to evaluate correlates of knowledge and acceptability of LARC methods among adolescent females at a primary care-oriented school-based health center.
Materials and Methods
We recruited participants for this cross-sectional, multisite study from 2 urban SBHCs in Seattle, Washington. These SBHCs are partially funded through a city levy and are operated by local health care agencies with oversight from local public health. All SBHCs in Seattle offer comprehensive primary care services, including confidential sexual and reproductive health and mental health services. A portion of these clinics—serving 3 middle and 3 high schools—began providing IUD and subdermal implant services in 2010. Gilmore et al 13 described details of this particular program previously. We chose these 2 SBHCs to include young women with varying socioeconomic backgrounds and experiences with LARC methods.
Young women eligible for participation were English speakers aged 13 to 19 years. Women younger than 18 years were eligible if they had obtained parental permission to use the SBHC for all services (ie, minors receiving confidential mental or reproductive health services without parental permission were ineligible in order to minimize the chance of their study involvement jeopardizing the confidential receipt of services). Participants were also recruited from flyers that included information about the survey and internet address to access the survey. Flyers were posted in SBHCs and given to registered female students while checking-in for SBHC visits. Prior to recruitment, the research team mailed a letter to parents/guardians of female patients who had given permission for their children to access all SBHC services with information about the study. The letter provided caregivers the opportunity to “opt-out” their child from participation. We also acquired a waiver of written consent/assent from our institutional review board prior to data collection and obtained assent/consent electronically from participants at the beginning of the survey. The University of Washington Human Subjects Division approved all study procedures.
We developed a survey instrument based on the objectives of the study, which included items on demographic information, information about medical and mental health conditions, presence of an individualized education plan (IEP) for special needs at school, sexual history, pregnancy and contraceptive history, LARC knowledge, experience, and acceptability, and overall experiences seeking care in the SBHC. After developing an initial draft, we tested the survey with 5 health care providers and 5 female adolescents from the SBHC and elicited feedback about the survey to ensure clarity. LARC knowledge questions were adapted from a previous study examining knowledge of etonogestrel implants by Bachorik et al. 10 We assessed awareness of LARC devices (eg, “Have you ever heard of an intrauterine device?”), and included generic and brand names of LARC devices in the survey to improve clarity. Among those who had never used a LARC device, we used a Likert-type scale to measure LARC acceptability. The 5-point scale ranged from “not at all” to “very much” in response to how much respondents liked the idea of having (1) a contraceptive implant and (2) an IUD for themselves. We then generated combined dichotomous outcomes for both implants and IUDs in which youth who currently had the LARC device (either IUD or implant) as well as youth who rated that device as highly acceptable (ie, participants who reported liking the idea of an IUD for themselves “very much”) were coded as “1.” Hereafter we will refer to these outcomes as “has or would like implant” and “has or would like IUD,” respectively. Our survey also included questions about the reproductive health educator providing counseling and education in the schools, specifically whether the participant had met the educator and if so, to what activities (eg, one-on-one sessions, classroom teaching) had they been exposed. Finally, we asked questions about satisfaction with the school-based health center and comfort with having an IUD or contraceptive implant placed at the SBHC.
Eligible participants completed the electronic questionnaire on tablets on the premises of the SBHC or on their personal computer, or mobile device. Data collection took place from December 2013 through January 2014. Participants received gift cards valued at US$5 for completing the survey. REDCap (University of Washington) electronic data capture tools were used to administer the survey and manage data. 14
Our primary outcomes were knowledge and acceptability of LARC devices, as represented by the “has or would like implant,” “has or would like IUD,” and “has or would like LARC device” outcomes. We calculated a knowledge score as percentage of correct responses and Cronbach’s alpha for the measure. Covariates were age, race/ethnicity (white vs non-white), family income (based on whether participant qualifies for free/reduced lunch), history of vaginal intercourse, and self-reported mental health diagnosis, all of which have been associated with unintended pregnancy and/or LARC method use in prior studies.11,12,15-18 Responses of “don’t know” or missing for prior LARC method use, mental health condition, or knowing the health educator were recategorized as a “no.” We calculated a chi-square statistic for each knowledge question, comparing youth with and without history of intercourse. We conducted univariate and multivariable linear and logistic regression, calculating regression coefficients and odds ratios respectively. We adjusted for having met the health educator during a one-on-one counseling session as a possible confounder in our multivariable regression. All analyses were conducted using STATA version 12 (Stata Corp LLC, College Station, TX). We conducted sensitivity analyses with and without the recategorization of “don’t know” to “no” for prior LARC use, mental health condition, or knowing the health educator to assess for miscategorization bias.
Results
A total of 102 participants completed the questionnaire. Based on available SBHC usage data, we estimate that approximately 120 unique female patients visited the 2 SBHCs during the recruitment period (response rate 85%). Our sample had a mean age of 16.2 years, and the race/ethnicity of the participants mirrored the diverse demographics of the student body (Table 1). More than half of participants reported a lifetime history of vaginal sex. Among 53 respondents who reported having ever had vaginal intercourse, 5 reported prior pregnancies, with 2 of these participants reporting multiple pregnancies. The majority of respondents had heard of at least 1 LARC method with awareness varying by device type. 10 participants currently had an implant and 4 had an IUD. Seventeen participants could not be categorized due to lack of response.
Participant Characteristics (N = 102).
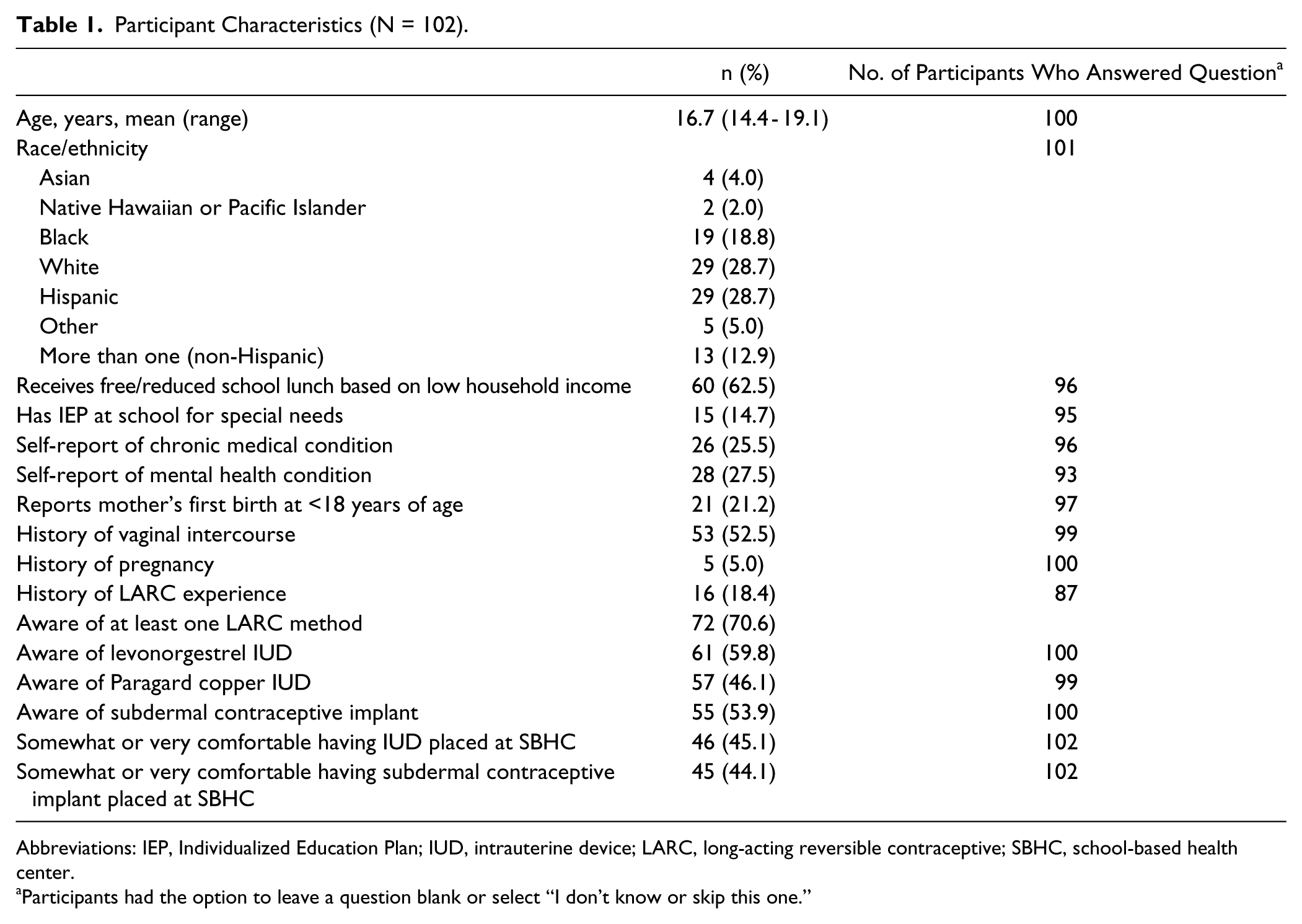
Abbreviations: IEP, Individualized Education Plan; IUD, intrauterine device; LARC, long-acting reversible contraceptive; SBHC, school-based health center.
Participants had the option to leave a question blank or select “I don’t know or skip this one.”
The mean score of correctly answered knowledge questions was 59.8% (SD = 35.4) Cronbach’s alpha for 10 items was .90. Correct responses to individual questions varied by history of vaginal intercourse (Table 2). The results of our multivariable regressions are found in Table 3. A higher knowledge score was associated with white race (regression coefficient [coef] = 26.8; 95% CI 13.3-40.4), history of vaginal intercourse (coef = 29.9; 95% CI 17.1-42.7), and having used or currently using a LARC method (coef = 22.8; 95% CI 6.5-40.0). History of vaginal intercourse was significantly associated with greater acceptability of implants as represented by our “has or likes idea of implant” (odds ratio [OR] 5.66, 95% CI 1.46, 22.0), while older age was associated with lower acceptability of IUDs (OR 0.53, 95% CI 0.30, 0.94). Only history of vaginal intercourse was associated with greater acceptability of any LARC device (coef 4.06, 95% CI 1.30-12.68). No differences in magnitude or direction of associations were found in sensitivity analyses using original and recoded variables.
Individual LARC Knowledge Question Responses.

Abbreviations: HIV, human immunodeficiency virus; IUD, intrauterine device; LARC, long-acting reversible contraceptive; STD, sexually transmitted disease.
Multivariable Regressions of LARC Knowledge and Acceptability.

Abbreviations: CI, confidence interval; IUD, intrauterine device; LARC, long-acting reversible contraceptive; OR, odds ratio.
Discussion
This survey identified low overall knowledge about LARC methods among this diverse sample of female patients in a school-based, primary care setting. We found that young women who were white as well as those with a lifetime history of vaginal intercourse were more likely to demonstrate greater knowledge of LARC methods, while only those who reported a history of vaginal sex were more likely to report that they would like the idea of a LARC device or already have one.
Our findings are consistent with other cross-sectional surveys that have identified an association between history of vaginal intercourse and knowledge and acceptability of LARC methods.11,12,16,19-21 That white race was significantly associated with greater knowledge has not previously been demonstrated in the literature. Our study is unique because it sampled from a general pediatric population attending a SBHC, rather than from those adolescents specifically seeking sexual and reproductive health services. A substantial proportion of our sample reported never having had vaginal sex, indicating that many of these individuals have not yet faced pregnancy risk but still have some knowledge about LARC methods and variable acceptability. Furthermore, we found that one-fifth of respondents reported that their mother or guardian was younger than 18 years when she had her first baby, which increases their own risk of adolescent pregnancy with possibly greater benefit from a LARC device. 17 Our findings demonstrate feasibility of conducting a survey measuring knowledge and acceptability of long-acting contraceptive methods with a school-based, primary care setting.
Interestingly, younger participants found the IUD more acceptable than older participants. This may not necessarily translate with increased IUD use, which has been demonstrated to be correlated with older age in other studies.6,22 Based on the results of a qualitative study conducted in this same setting, our findings may suggest that young women are less likely to have heard negative anecdotes from friends and family members about IUDs. 23 They may also have lower levels of knowledge about IUD placement and removal, owing to their younger age and likely less sexual experience. A more detailed exploration of school-wide IUD knowledge and acceptability among younger students may provide insight into this finding.
This study has limitations. The relatively small convenience sample excluded non-English speakers and teens younger than 18 years whose parents had not given their permission to use the SBHC. Minors with parental permission to use SBHC services, including reproductive and mental health services, may be more likely to speak with their parents about sex or contraception and thus have different levels of knowledge and attitudes about LARC. In terms of generalizability to the overall school population, SBHC users in our 2 schools comprise about one-third of the general school populations and largely mirror the racial/ethnic breakdown of the overall school populations, suggesting that teens using the SBHC may be somewhat representative of the general school population. The survey instrument was not validated before use and more research is needed to understand best measures to elicit these data from teens. In order to limit questionnaire length, we did not include questions about sexual orientation or a broader range of sexual activity questions, including gender of sexual partners or types of sexual activity beyond vaginal intercourse, thus we cannot comment on potential associations between these factors and LARC knowledge and acceptability.
Future directions for this research may include validating the survey instrument, conducting cognitive interviews with teens to determine the best way to phrase sexual health questions, expanding the survey to a larger and more representative population of teens within a school or primary care setting, including broader measures of gender identity, sexual orientation and practices, and exploring adolescents’ motivations to initiate LARC methods with qualitative methods. Results from these and related studies could be used to design and pilot a LARC counseling tool for use with sexually inexperienced and/or minority youth in school-based and other pediatric primary care settings.
Adolescents in this school-based primary care setting had variable knowledge and acceptability of LARC methods. When adjusting for other factors, a history of vaginal intercourse was the strongest correlate of LARC method acceptability. Efforts to identify unique counseling and education needs of young women from diverse cultural backgrounds and those reporting sexual activity exclusive of vaginal intercourse may be needed.
Footnotes
Acknowledgements
The authors thank Nadia Novotny and Krista Eknes for assistance with participant recruitment and a donor group of Seattle-based families who provided funding support for data collection. We also thank Elizabeth Dawson-Hahn for reviewing the manuscript.
Authors’ Note
Preliminary results of this study were presented at the American Public Health Association Annual Meeting in Chicago, Illinois in October 2015 and at the North American Forum on Family Planning in Chicago, Illinois in November 2015.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Data collection for this study was supported by a private grant from a donor group of Seattle-based families. Dr. Hoopes was supported by National Research Service Award 2T32MH020021-16 (NIH/NIMH), Leadership Education in Adolescent Health Award T71MC24210 (HRSA/MCHB). REDCap at University of Washington/Institute of Translational Health Sciences is supported by UL1TR000423 (NCRR/NIH).
