Abstract
Background and objectives:
Insertion of a intrauterine contraceptive device (IUCD) is one of the services provided at our public primary care polyclinics. We evaluate the effectiveness of a simulation workshop using low-fidelity mannequins to train primary care doctors.
Methods:
Questionnaire feedback was collected before and after the workshop. Participants rated their confidence level in performing the insertion of IUCDs using a 10-point scale.
Results:
A total of 37 out of 44 (84%) participants completed the survey. The median score for confidence level in performing the procedure increased from 2 out of 10 (interquartile range (IQR) 1 to 5) before the workshop to 8 out of 10 (IQR 7 to 9) after the workshop (p < 0.01). The increase in confidence level was most pronounced among the participants with no previous experience with the procedure and those who had inserted only one or two IUCDs before the workshop. Participants rated a median score of 9 out of 10 (IQR 8 to 10) in their interest level to perform the procedure after the workshop. The overall experience of the workshop recorded a median score of 5 out of 5 using a five-point Likert scale.
Conclusions:
Bedside procedural training has been challenging. The teaching of the procedure via a structured workshop format including a simulation of the procedure using a low-fidelity mannequin increases the confidence level of participants to perform the procedure. A similar format can be employed for training of other primary care procedural skills.
Introduction
The intrauterine contraceptive device (IUCD) is an effective and safe contraceptive method.1–4 It is a long-acting, reversible contraceptive suitable for most women including adolescents and nulliparous women.5–7 IUCD insertion is a useful and important procedural skill for primary care physicians.8–11 Bedside procedural skills training in primary care has met with various difficulties in many countries.9,12,13 Traditionally, the skill of IUCD insertion is acquired via direct observation of the procedure performed by experienced colleagues and then attempting the procedure. The first attempt of insertion is often on a real patient. This is referred to as the “see one, do one, teach one” apprenticeship approach to learning of procedural skills. Such an approach is not ideal in imparting psychomotor skills effectively.14,15 It is highly dependent on availability of both learning opportunities and supervision of these opportunities. 16 Simulation-based training in invasive bedside procedures has been shown to be effective.17–19
High-fidelity simulation training has been used in a number of disciplines such as anesthesia, surgery, obstetrics, and emergency medicine. 20 Recently, simulation training has also proven its role in undergraduate training of simple bedside procedures such as intravenous cannulation. 18 In the area of gynecology, the use of simulation training is found to increase undergraduate students’ confidence and interest in women’s health in a medical school in the United States of America (USA). 21 A study on midwifery students in Iran showed simulated patients and gynecology models are effective in reducing students’ anxiety in providing the IUCD service. 22 In an attempt to increase immediate postpartum IUCD insertion rates, a simulation workshop for gynecologists in a teaching hospital in the USA showed that it increases providers’ comfort with skills and knowledge with postpartum IUCD insertion. Rates of postpartum IUCD insertion were found to have increased post-training. 23
In the Asia-Pacific region, “on the job” training is usually employed in hospitals for specialist trainees. 24 Australia reported a structured training program for primary care physicians through family planning organizations utilizing case-based teaching and insertion in pelvic models.25,26 In the local Asian region, there is a paucity of published literature on the effectiveness of IUCD insertion training using low-fidelity, simulation-based models.
A simulation-based workshop on IUCD insertion was introduced in our institution to provide structured pre-patient training. The aim of the study was to evaluate its effectiveness in increasing confidence level in performing IUCD insertion among local primary care physicians.
Methods
This study was conducted at a single primary care training center that provides training for doctors in the nine public primary care polyclinics, serving the population in the central eastern region of Singapore. The polyclinics provide family planning services, including IUCD insertion. The workshop is a half-day session conducted by two faculty members. They are family physicians with knowledge and experience in the provision of family planning service at the polyclinics.
The workshop is designed around key components described for pre-patient training for technical skills. 14 These include cognitive knowledge surrounding the procedure, function and operation of equipment, steps of the procedure, fundamental elements needed to perform the procedure and the opportunity to perform the procedure in simulated models. Cognitive knowledge surrounding the existing literature on eligibility criteria, indications and contraindications, complications, pre- and post-procedural counseling on IUCD use3,4,6,7 was delivered in a didactic lecture format. A maximum of 12 participants per workshop allowed in-depth interactive discussion among the participants and faculty. Two low-fidelity, life-size mannequins (Figure 1) were used for each workshop. Participants were able to handle actual instruments including insertion of a speculum, visualization of the cervix, applying a tenaculum to the cervix, insertion of uterine sound and insertion of IUCD device into the uterus on the mannequin.

Low-fidelity life-size pelvic mannequin.
Following demonstration of the procedure on the mannequin by the teaching faculty, participants practiced IUCD insertion on the mannequin with one-on-one instruction and direct feedback from the faculty. They were then given time for self-directed practice on a separate similar mannequin with peer-feedback using a procedural checklist developed for the workshop. A procedural checklist was developed based on existing literature on steps for IUCD insertion, 27 published checklists,28,29,30 and the product insert of the IUCD device used for the workshop (Multiload Cu250). This was agreed on by the two faculty members to be essential steps for IUCD insertion.
Each participant was then assessed by one of the faculty for competence in providing pre- and post-insertion counseling, and insertion of IUCD on the mannequin using the same procedural checklist. Training and re-training with direct feedback was given until the participant was able to perform all the tasks listed in the procedural checklist.
A total of four workshops were conducted between July 2014 and January 2015. All doctors who were new to the Polyclinics were invited to attend the workshop. A total of 44 participants attended the workshops. This represented 28% of the total number of doctors in the nine public primary care polyclinics. Participants were medical officers and family medicine residents who were new to the polyclinics. Most had no previous experience with insertion of an IUCD. Incidentally, however, some participants who were second-year family medicine residents had already performed IUCD insertions on patients during their rotation in the hospital gynecology unit before the workshop (Table 1). A pre- and post-workshop written questionnaire was obtained.
Participants’ demographic characteristics.

Participants were asked to rate their confidence level in performing the insertion of IUCDs before and immediately after the workshop using a 10-point scale, with 1 being “not confident at all” and 10 being “very confident.” Overall experience after the workshop was recorded using a five-point Likert scale. Participants rated 1 to 5 (1 = Strongly disagree, 2 = Disagree, 3 = Neutral, 4 = Agree, 5 = Strongly agree) to the statement “overall the workshop is effective.” They were also asked to rate the helpfulness of various parts of the workshop to their learning using a five-point Likert scale (1 = Not helpful at all, 2 = Not helpful, 3 = Neutral, 4 = Helpful, 5 = Very helpful). Open-ended comments were invited for general feedback and areas of improvement for future workshops.
Statistical analysis
The Wilcoxon signed-rank test is used to compare the medians for pre- and post-workshop confidence level. Change in confidence level was assessed with number of IUCD insertions performed before the workshop using the Mann–Whitney U test. A p value of less than 0.05 was considered to be significant.
This study received a SingHealth Centralised Institutional Review Board exemption, ref: 2015/2662.
Results
A total of 37 out of 44 (84%) participants completed the questionnaire. A majority (84%) of participants had performed two or fewer IUCD insertions previously (Table 1). The median score for confidence level in performing the procedure increased from 2 (IQR 1 to 5.5) before the workshop to 8 (IQR 7 to 9) after the workshop. (p < 0.01) (Figure 2). The increase in confidence level was significantly higher among participants who had performed two or fewer IUCD insertions before the workshop than among those who had already performed more than two insertions before the workshop (change in confidence level of 5 vs 0.5 in Table 2).

Median confidence level from pre-workshop to post-workshop.
Change in confidence level for pre- to post-workshop in IUCD insertion.
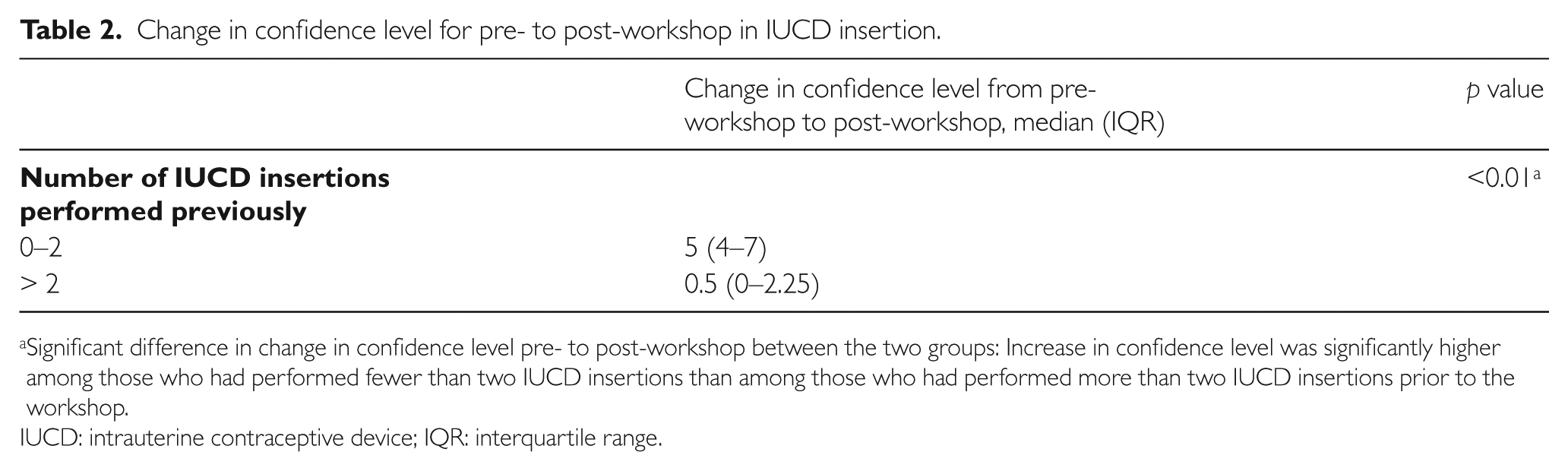
Significant difference in change in confidence level pre- to post-workshop between the two groups: Increase in confidence level was significantly higher among those who had performed fewer than two IUCD insertions than among those who had performed more than two IUCD insertions prior to the workshop.
IUCD: intrauterine contraceptive device; IQR: interquartile range.
Participants rated a median score of 9 (IQR 8 to 10) in their interest level to perform the procedure after the workshop. The overall experience of the workshop recorded a median score of 5 using a five-point Likert scale (Figure 3).
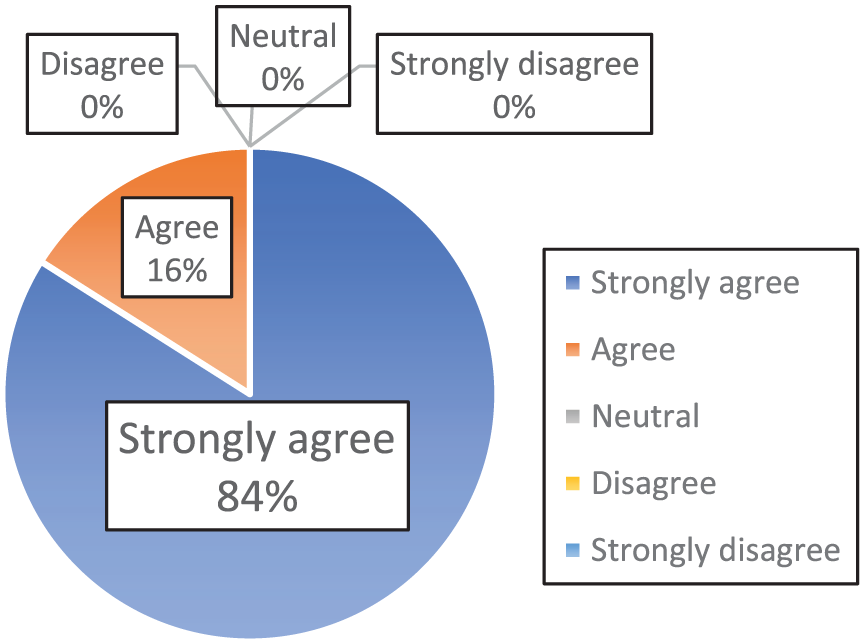
Questionnaire survey: Overall the workshop is effective.
In the open-ended comments, participants commented they found the hands-on practice session most helpful in their learning. The workshop was “interactive and clear.”
Discussion
Our study demonstrates that a simulation-based workshop on IUCD insertion is effective in improving perceived self-confidence in the procedure. Simulation training on a mannequin allows participants to repeat the procedure multiple times without causing any actual harm.
Learning and re-learning as often as required on a mannequin allowed trainees to correct mistakes, to perfect steps and fine-tune skills. 31
Mastery of skills comes with repeated practice. The psychomotor phase in procedural skills training requires repeated physical practice with correction and reinforcement. 32 Repetition is considered essential to psychomotor learning. 33 Repetitive practice and direct feedback have been identified as a key feature of successful learning in simulation-based training. 34 The simulation-based workshop on IUCD insertion allowed participants opportunity for repeated practice, direct faculty feedback, and learning and re-learning, which supports the literature on effective procedural skills training.14,32,34
Simulation-based learning is perceived to be expensive.7,35 Cost of equipment is often a practical limitation. A high-fidelity simulator using a sophisticated biomedical sensor and computerized monitoring system may cost up to a six-figure sum. 35 Such high-cost simulators may be a barrier for provision of simulation-based pre-patient procedural skills training. Our study utilized a low-fidelity, life-size pelvic mannequin for training of IUCD insertion. Participants were able to perform all steps of the procedure for IUCD insertion on the mannequin using actual instruments. The positive results from our study showed such relatively lower-cost simulation-based training can be helpful for procedural skills training too. Norman et al. concluded in a review that the relationship between simulation fidelity and learning is not linear, and that “more is not necessarily better.” 36
Practical training opportunities for primary care physicians have been limited. 24 Our study reports on using a low-fidelity mannequin for training of IUCD insertion for primary care physicians. Coupled with didactic lecture and interactive teaching, such a structured workshop in procedural training is effective in raising procedural confidence. Participants also reported interest in performing the procedure post-training.
Interestingly, we found the increase in confidence level was also significant among participants who had performed one or two procedures prior to the workshop. This is consistent with another study that found significant improvement in procedural skill in lumbar puncture even for those who reported some previously successful procedure experience. 19 Thus, doctors who have performed a few procedures in the past may still benefit from such training.
Limitations of our study included that it was a pre-post-test performance study with no comparative group on traditional teaching approach. Self-rating of confidence level may not necessarily correlate with competence. Measurement of clinical outcome such as success rates and complication rates as compared to the traditional mode of the “see one do one” approach would be helpful.
Bedside procedural training has been challenging in primary care. Procedural training with a simulation-based workshop increases the confidence level of participants to perform the procedure. A similar format can be employed for training of other procedures in primary care.
Footnotes
Acknowledgements
The authors thank the SingHealth Polyclinics Education Department.
A version of this work received a Merit Award for E-poster presentation at the 13th Asia Pacific Medical Education Conference (APMEC) held 13–17 January 2016, in Singapore
Abstract published: LP Ng and EYL Koh. Evaluation of a simulation workshop to train primary care doctors to insert intrauterine contraceptive device. Abstracts of the 13th Asia Pacific Medical Education Conference (APMEC), Singapore. Med Education 2016; 50 (Suppl 2): 29
Declaration of Conflicting Interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
