Abstract
Keywords
Background
Although rates have recently declined, the United States maintains one of the highest rates of teen pregnancy in the developed world. 1 According to Youth Risk Behavior Surveillance System data from 2011, nearly half (46%) of high school girls have had sex, 34% are currently sexually active, and 15% have had sex with 4 or more partners. 1 Consistent and early use of contraception remains one of the best ways to prevent unintended pregnancy in this at-risk population. 1 The American Congress of Obstetricians and Gynecologists (ACOG), the American Academy of Pediatrics (AAP), and the Society for Adolescent Health and Medicine (SAHM) all recommend use of long-acting reversible contraception (LARC) as first-line contraceptives in sexually active adolescent females.2-4 Despite this support, the United States has lower rates of LARC use as compared with other developed countries 5 ; as of 2010, although 57% of women aged 15 to 19 years reported a history of vaginal intercourse, fewer than 5% were seeking LARC.6,7
Parents and teenagers have cited discomfort as a key barrier to discussing reproductive health. 8 Parents also feel undereducated and embarrassed to discuss reproductive health with their teenagers and are often unaccepting or altogether unaware of their daughters’ sexual maturation.8,9 Unfortunately, and in spite of evidence to the contrary, parents still have concern that confidential reproductive care, education, or simply conversation can promote sexual activity in their teenage daughters and are reluctant to allow it for their teens.8,9
In addition to their parents, adolescent females seek medical information from a primary care physician, often their pediatrician, for recommendations regarding sexual health. However, providers express discomfort with sexual health counseling and often do not offer counseling on contraceptive options. 10 Furthermore, there are multiple myths regarding LARC that contribute to fear and underutilization. 11
Given this scenario, adolescents and their parents often turn to other sources, particularly the Internet, for sexual health information.12-14 The Internet does not adhere to the same standards as medical associations and therefore may offer misleading, outdated, or inaccurate information. Studies have shown medical information obtained via Internet searches may not provide patients with accurate information and leave many patients uncertain when making medical decisions. 15
The primary goal of this study was to describe the availability of LARC information on the Internet and to assess whether (1) information was up to date with current literature on adolescent LARC recommendations and (2) websites with and without LARC information met quality standards as described in a prior study. 14
Methods
A web search was conducted using a combination of terms related to adolescents and contraception initiation between December 2013 and January 2014. To mimic real searches, an informal survey was conducted with 8 parents of adolescent patients receiving care at a teen clinic to determine search terms. The results were summarized into 5 searchable phrases: teenage birth control, birth control appropriate for teenager, pros and cons of birth control for teens, teenagers on birth control, teenagers starting birth control. Two researchers (KH, KW) collected data by querying the 3 most common search engines: Google, Microsoft/Bing, and Yahoo 16 using these search phrases. The first 10 websites resulting from each search engine were recorded and websites that were found on at least 2 of the 3 search engines were evaluated.
Following the methods of Borzekowski et al, 17 this first list of included websites was considered the first generation dataset. 17 A third researcher (KB) then identified viable links from the first-generation data set to develop a list of second-generation sites. Sites were included in the second-generation data set if they included the terms “birth control,” “contraception,” or listed a specific form of contraception (ie, condom, intrauterine device, cervical cap, spermicide, abstinence, etc). All unique websites related to contraception were included in analysis unless they were an advertisement, headline information and/or had incomplete text. In addition to these exclusions, headings, side bar information, pictures and captions, tables, videos, bibliographies or references, and advertisements included within websites were not evaluated. First- and second-generation websites made up the data set for the directed content analysis. 18 The data set was assessed by 2 coders (KB, KW) independently for 11 a priori themes related to LARC (Table 1). Themes were formulated prior to analysis by reviewing the recent guidelines on adolescent contraception put forth by the ACOG, AAP, and SAHM.2,4,19
List of 11 Content Themes Used for Coding.

For websites that discussed LARC, content was evaluated for accuracy regarding health benefits and adverse effects of using LARC. Additionally, inaccurate information to dissuade adolescents from using LARC was coded.
In conjunction with the content analysis, quality of each website was reviewed. Referencing a 2010 study by Buhi et al, 14 websites were assessed for the presence of 15 quality measures (see Table 2). Each measure present received 1 point, with a total of 15 points possible. Top-level domain (eg, “.com”) was also recorded for each website. The first 10 websites were coded by 2 researchers (KB, KW) and discrepancies were discussed and reconciled by a third researcher (KH). The remaining websites were coded for quality by a single researcher (KH) with a second researcher (KW) performing fidelity checks on every 10th website. All content and quality coders were pediatricians.
The 15 Criteria Used for Quality Analysis as per Buhi et al. 14

Analysis
Data were summarized using proportions and means. Data were compiled into the following groups: sites that discussed LARC, sites that discussed LARC use in adolescents, and sites that discouraged LARC use in adolescents. Categorical data were evaluated using Fisher’s exact test and sum quality scores were evaluated using analysis of variance. Analyses were performed using IBM SPSS (Version 20.0).
Results
The 11 content themes applied to 238 websites resulted in 2618 codes for analysis. Of the websites analyzed 77% (n = 183) made no recommendation of LARC for adolescent females. Of the 55 websites that did recommend LARC, only 40% (n = 22) specifically discussed its use in the adolescent population. Of note, 16% (n = 9) of websites recommending LARC discouraged their use in adolescents. When a reason for deterrence was listed, these included nulliparity (n = 2), increased pain with insertion (n = 2), increased expulsion risk (n = 1), and increased risk of sexually transmitted infections (n = 2).
Relatively few websites listed side effects (24%, n = 13) or health benefits other than contraception (2%, n = 1). Only 4% (n = 2) of LARC-discussing websites correctly stated that contraception can be prescribed to teenagers without a pelvic examination.
Quality varied among LARC-discussing websites, ranging from 3 to 13 of the criteria assessed (Table 3). Most websites had a “.com” domain, only 1 website was found with a “.edu” domain. The average sum quality score was 9.5 (SD = 3.8). Quality scores did not differ based on whether sites were incorporating inaccurate information; nor did scores differ by top-level domain.
Results of Quality Review of Websites.
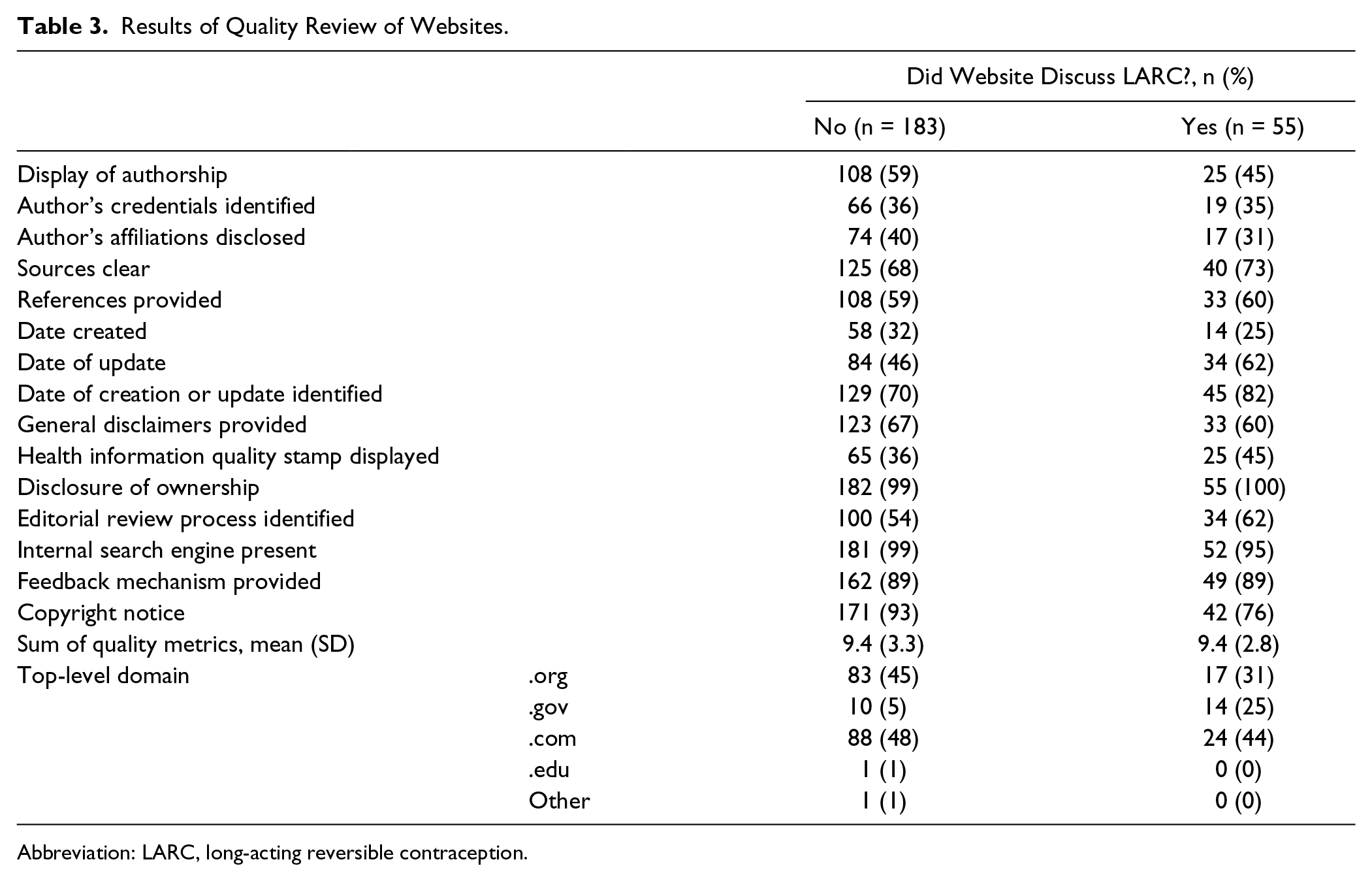
Abbreviation: LARC, long-acting reversible contraception.
Discussion
The Internet provides a safe and comfortable way to obtain information that users may otherwise not seek. It has been, and will continue to be, a readily accessible venue for health information for teenagers and their parents. As noted in previous studies, there are multiple barriers that preclude LARC counseling and utilization by adolescents.5,10,11,20 These barriers, especially discomfort in discussing contraception, make the Internet a prime location to harvest such medical recommendations. Although its ease of access is appealing, this study illustrates that Internet information is often not up to date with medical society recommendations and may offer inaccurate medical opinion.
The AAP, ACOG, and SAHM are clear in their recommendations for LARC as first-line contraceptives for teenagers, but the information available on the Internet fails to convey this recommendation to its users. Some websites go as far as to dissuade teens from using LARC. In addition, the quality of websites accessible to parents and teens is not high. It is crucial that providers understand the potential misinformation provided by websites related to LARC use and address it in the clinical setting.
While the results identified few websites promoting current information and recommendations related to LARC, it is important to recognize the limitations of this study. The Internet is a dynamic and ever-changing source of information so the assessments of these websites only represent a snapshot of a single moment. The relative paucity of websites discussing LARC may imply that more narrowed search terms would be needed to fully survey information available to teens via the Internet. In addition, it is possible that our search strategies and methodology resulted in missing relevant websites that may have changed our results. However, every attempt was made to mimic real-life searching patterns of parents of adolescents.
The AAP, ACOG, and SAHM continue to encourage good dialogue between patients and physicians, particularly in the area of sexual health.21,22 Despite discomfort in addressing contraception, it is imperative that providers, at a minimum, provide patients and parents with up-to-date and accurate sources to access regarding contraception and specifically LARC. If left to their own Internet searches, patients will often not find medically accurate information. By promoting accurate sources, providers can give parents the knowledge and tools necessary to increase their comfort in discussing and facilitating reproductive health care for their daughters. Last, this study should further encourage providers to be aware of the inaccurate recommendations regarding contraception for teenagers and reinforce the importance of having a comprehensive dialog with teen patients about safe and effective contraception.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
