Abstract
The high prevalence of no-shows in residents’ primary care clinic acts as a barrier to continuity of care, results in loss of outpatient learning opportunities, and may result in more emergency department (ED) visits. The authors seek to identify if high rates of no-shows correlate with more ED visits. In a selected primary care internal medicine (PCIM) continuity clinic, 650 patients were randomly selected, with 325 patients each from the faculty and resident practices. The number of ED visits between January 1, 2006, and December 30, 2008, was recorded. Demographic characteristics of the population were obtained, and comparisons between the faculty and resident groups were performed using Student t test. Linear multiple regression analysis was performed to compare frequency of ED visits between the faculty and the resident groups, controlling for age, interpreter requirement, number of ED visits, proportion of no-shows, and insurance type. A P value <.05 was considered statistically significant. During 2006-2008, the average number of ED visits per patient in the faculty’s practice was 2.1 compared with 4.1 in the resident’s practice (P < .001). A multiple linear regression model showed that patients who had more ED visits were likely to be younger (P = .004), had shorter duration of care in the PCIM clinic (P < .001), and had a higher proportion of no-shows to the PCIM clinic (P < .001). There was no statistical difference between faculty and resident practice after adjusting for the above-mentioned variables. Shorter duration in the PCIM clinic and higher proportion of missed appointments were associated with more ED visits, but the use of interpreters and Medicaid insurance did not result in more ED visits. Future interventions are necessary to reduce the no-show rate in the clinic as this may result in a reduction of ED visits.
Many emergency departments (EDs) are underfunded and overcrowded. 1 The Centers for Disease Control and Prevention reported that between 1993 and 2003, the number of ED visits decreased by 12.3%, but paradoxically the frequency of ED visits increased by more than 25%. 2 The increase in frequency of ED visits has been attributed to less access to primary care, higher number of uninsured patients, and general population growth. 3 The 2000 National Hospital Ambulatory Medical Care Survey found that average waiting times in the ED for nonurgent visits have increased by 33% from 3 years prior. 4 In urban EDs, longer wait times and crowded conditions are increasingly common. Overcrowded EDs can also result in decreased staff productivity, miscommunication, and medical errors.4,5
Continuity of care is considered an important component to a high-quality health care system and an essential component in the management of chronic illnesses. Continuity of care has been associated with improved outcomes and reduced costs for patients with chronic diseases. 6 When patients miss scheduled appointments, care plans are interrupted, and residents miss opportunities to see outcome of treatment plans. 7 Therefore, a high frequency of no-shows in primary care clinic acts as a barrier to delivery of continuity of care and results in poor utilization of limited medical resources.6-8 In our study, we seek to explore how the high frequency of no-show rates in a primary care clinic may be related to more visits to the ED.
Methods
One of 4 primary care internal medicine (PCIM) firms within an academic institution in the midwestern United States was selected to be the study site. The selected PCIM clinic shared a same group of office staff, but the firm is divided into 2 autonomously functioning practices comprising resident and faculty physicians. During January 1, 2006, to December 31, 2008, a total of 650 patients were randomly selected from the faculty and resident practices, with 325 patients from each group. Patients were excluded if they had less than 5 office visits during the indexed period. The total number of visits to the Mayo ED from January 1, 2006, to December 30, 2008, was recorded. Demographic characteristics of the population were obtained, and comparisons between the 2 groups of faculty and resident patients were performed using the Student t test. The patient characteristics were obtained by individual chart review. Length of affiliation with PCIM clinic was defined as the date of first visit to the PCIM clinic. A linear multiple regression analysis was performed to compare number of emergency visits between the faculty group and the resident group, controlling for age, interpreter requirement, number of ED visits, proportion of no-shows, and insurance type. A “no-show” was defined as a patient who did not call the office in advance to cancel a scheduled appointment and who did not show up for the appointment. The no-show rate was calculated as the number of missed appointments divided by the total number of appointments made. A P value <.05 was considered statistically significant. The study protocol was approved by the Institutional Review Board.
Results
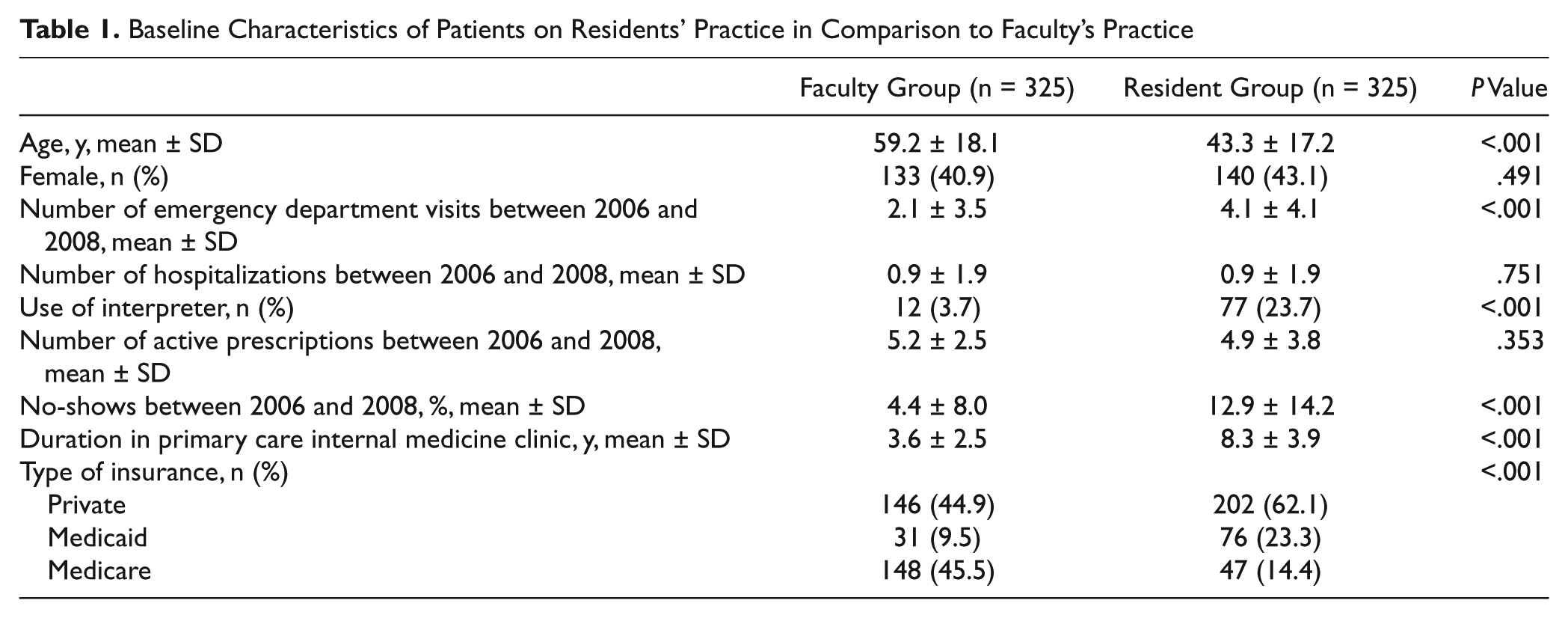
Between January 1, 2006, and December 31, 2008, the residents’ group, on average, had a higher number of ED visits compared with the faculty practice, 4.1 visits/patient compared with 2.1 visits/patient. At baseline, there appeared to be differing patient characteristics between the faculty and resident practices, as illustrated in Table 1. Patients in the resident group were younger, with a mean age of 43.3 years compared with 59.2 years (P < .001), but had a higher percentage of no-shows (12.9% vs 4.4%, P < .001), more patients with Medicaid insurance (23.3% vs 9.5%, P < .001), and more frequent use of interpreters (23.7% vs 3.7%, P < .001). The patients in the faculty practice had a longer affiliation with the PCIM clinic, with an average of 8.3 years compared with 3.6 years in the resident practice (P < .001). Despite more ED visits by patients in the residents’ practice, the number of hospitalizations did not differ between the faculty and resident groups (P = .751). The number of active prescription medications between 2006 and 2008 was used as a surrogate marker for chronic medical illnesses and medical complexity, and there was no difference between the faculty and resident groups (P = .353).
Baseline Characteristics of Patients on Residents’ Practice in Comparison to Faculty’s Practice

The multiple linear regression analysis, as shown in Table 2, showed that patients who had more ED visits were likely to be younger (β = –0.023, P = .004), had a shorter affiliation with PCIM clinic (β = –1.258, P < .001), and had a higher proportion of no-shows in the clinic (β = 7.650, P < .001). There was a trend only toward more ED visits among patients who required an interpreter (P = .067) and had Medicaid insurance (P = .059). There was no statistical difference between faculty and resident practice in terms frequency of ED visits, after adjusting for the above-mentioned variables.
Multiple Linear Regression Model Predicting Frequency of Visits to the Emergency Department (n = 650; Adjusted R2 = 0.58)


Discussion
Frequent visits to the ED are a poor utilization of limited health care resources. Schafermeyer and Asplin 5 report that longer wait times and overcrowded conditions have become increasingly common in urban EDs. Previous studies have shown that a higher proportion of ED visits may be related to a higher number of the uninsured and less access to primary care. 3 Continuity of care is considered an essential component to a primary care practice. The literature suggests that no-shows are likely a significant barrier to continuity of patient care.6-8 Continuity of care has been associated with improved outcomes and reduced costs for patients with chronic diseases. 6 Specifically, Cree et al 9 demonstrated that in asthmatic patients, improved continuity of care resulted in less ED visits.
In our selected PCIM clinic, the faculty and resident practices share similar nursing staff, appointment coordinators, and secretaries. Despite sharing the same practice parameters and staff, patients in the residents’ practice have a significantly higher number of ED visits than patients in the staff practice, with a recorded mean number of ED visits reported during 2006 to 2008 to be 4.1 visits/patient compared with 2.1 visits/patient. Despite more ED visits, the rate of hospitalization between the 2 groups was similar.
At baseline, there are differing patient characteristics between the faculty’s and residents’ practices. Patients in the residents’ practice were younger and had a shorter duration affiliated with the clinic but were more likely to require the use of a translator and had a higher frequency of no-shows. Interestingly, the number of active prescription medications, which was used a surrogate marker for chronic medical illnesses and the medical complexity of patients, was similar between the 2 groups.
The more stable nature of faculty practice may account for the older patient age population and longer primary care affiliation within this group. The population differences can also be explained by the high influx of foreign immigrants and young professionals to Rochester in the past decade, during a time when only the residents’ clinic was opened to new patient enrollment as the faculty clinic had well reached maximum capacity. Moreover, residents maintain continuity in the clinic for only the 3 years of their training, and patients may choose to seek primary care elsewhere rather than be assigned to another resident panel.
Prior studies have shown that patients who miss appointments tend to be younger, are of lower socioeconomic status, and have government-provided health care benefits.10-12 However, these reported patient characteristics, well documented in the literature, clearly correlate with higher no-show rates but do not necessarily correlate with more ED visits, as demonstrated in our study. In our patient population, English proficiency, chronic medical conditions as measured by number of prescription medications, and having Medicaid insurance did not statistically contribute to more ED visits. However, we demonstrated that the higher rate of no-shows and shorter affiliation with the PCIM clinic are independently associated with a higher frequency of ED visits in our practice.
This study is limited by our inability to disaggregate types of PCIM appointments missed (general medical examination, limited exam, subsequent visits) and type of ED visits attended (urgent vs nonurgent), and it does not account for ED visits outside of the Mayo Clinic. In addition, the distribution of ED visits was skewed rightwards, with approximately one fourth of the population having no visits to the ED, which could bias the linear regression analysis. However, several transformations were considered, but none were found that could appropriately normalize this distribution because of the large proportion of no visits.
It is also difficult to identify if reducing the no-show rate will ultimately result in a reduction of ED visits. A resident-driven quality improvement project has begun in the PCIM clinic, with multiple interventions implemented to reduce the rate of no-shows, including refining methods of appointment reminder and educating residents to closely follow-up with no-shows. A postintervention analysis to be performed in the next 24 months will help delineate if a reduction in no-shows will result in less ED visits.
For the ED to fulfill its role as a safety net provider and meet public health needs in the event of disasters, appropriate use of ED resources becomes increasingly important. Reducing the frequency of no-shows may result in improved continuity of care, which can result in reduced frequency of ED visits.
Footnotes
The authors declared no potential conflicts of interest with respect to the authorship and/or publication of this article.
The authors received no financial support for the research and/or authorship of this article.
