Abstract
Objectives:
Behçet’s disease is a chronic, relapsing, multisystem vasculitis of unknown etiology. Few reports support the hypothesis that Behçet’s disease has a primarily hereditary basis. It complicated diversified clinical features predominantly involving oral and genital ulcers, and ocular and cutaneous lesions. The clinical features of this disease have been described to be different according to geographical areas and gender. The objective of the study is to explore the demographic features and clinical aspects of Behçet’s disease in Omani patients and to compare the results with those of various reports in the region.
Methods and results:
In total, 56 Behçet’s disease patients were recruited, and clinical data parameters were recorded including age, sex, age at diagnosis, duration of symptoms till diagnosis, disease characteristics such as oral and genital ulcers, ocular manifestations, the presence of arthritis, and cutaneous lesions such as papulopustular lesions and erythema nodosum. Furthermore, other systemic involvement was studied including gastrointestinal, neurological, renal, and vascular manifestations. Laboratory tests of Behçet’s disease and treatment used were recorded in each patient. The onset was between 6 and 74 years with a male predominance. Oral ulcers were the most common manifestation, followed by genital ulcers, ocular lesions, and arthritis. Vascular lesions and gastrointestinal manifestations were less common. Cutaneous manifestations were rare in patients with Behçet’s disease. The frequency of neurological involvement was significantly high. There were no reported cardiac or urogenital manifestations.
Conclusion:
Behçet’s disease’s demographic features and clinical aspects in Omani patients showed quite significant geographical and gender differences which are comparable to other data in the area.
Introduction
Behçet’s disease (BD) is a chronic, relapsing, multisystem vasculitis of unknown etiology. Few reports support the hypothesis that BD has a primarily hereditary basis.1,2 Supported hypothesis suggests that BD has a primarily hereditary basis with complicated and diversified clinical features of mucocutaneous, ocular, vascular, articular, gastrointestinal (GI), urogenital, pulmonary, and neurological involvement. 3 The pathogenesis of BD is multifactorial involving immune, genetic, environmental, and infectious agents. 4 It is particularly prevalent along “Old Silk Road” countries from Northwest China to the Mediterranean basin. 5 The highest prevalence of BD worldwide reported in Turkey (80–300 per 100,000). 5 Conversely, the prevalence is quite low in United States (5.2 per 100,000). 6 Some clinical features of BD have been described to varies according to the geographical areas. Gender differences across BD clinical features have been reported. The majority of the reports revealed male to female predominance; however, women are affected more commonly in reports from the United States, Korea, and Northern Europe.7–11 The pathergy reaction is considered highly sensitive and specific for BD in patients originating from the Silk Road, but is often negative from patients from the West. 12 The frequency of GI involvement is much lower in the Mediterranean than that in Far East. 13 Eye involvement in BD causes serious morbidity and is a common cause of blindness in the Mediterranean basin, Middle East, and Far East. It is found in 50% of patients, but the frequency reaches 70% in young men aged <25 years. It is usually seen during the first 2 years of the syndrome and is bilateral in 70%–80% of patients.14,15 Ophthalmic manifestations, arthritis, folliculitis, and vascular involvement are more common among males, while erythema nodosum were more frequent in females. 16 The mean age at the onset of patients with the worst prognosis is younger in males. 16 HLA-B51 testing may be of significance in patients who exhibit features of BD that cannot be explained otherwise and do not fulfill the International Study Group (ISG) Criteria/International Criteria for Behçet’s Disease (ICBD).
We aimed to investigate the specific clinical features of BD patients in Oman as one of Middle East Asian countries to explore whether there are gender differences in their clinical features. We also compared the results with those of various reports in the region to find out geographical differences in clinical features of BD.
Material and methods
Subjects
Total 56 patients with BD (34 male and 22 female) who were seen in the Department of Rheumatology, Royal Hospital, Oman, between 2006 and 2013, total 46 (82.1%) (out of which 27 (79.4%) were males and 19 (86.3%) were females) fulfilled ISG criteria 17 for BD. However, all 56 (100%) patients fulfilled ICBD criteria. 18 The presence, absence, and characteristics of each clinical manifestation were evaluated by specialists of related symptoms such as neurologist for neurological features and rheumatologist for articular involvement. All skin manifestations had been confirmed with dermatologist, and few patients with no oral ulcer underwent skin biopsies to exclude other differential diagnosis. Similarly, ocular manifestations were confirmed with ophthalmologist for all patients studied. All patients consented to access their data.
Laboratory tests
Laboratory tests of all the patients with BD were carried out in the Clinical and Immunology Laboratory of Royal Hospital included erythrocyte sedimentation rate (ESR), C-reactive protein (CRP), anti-nuclear antibody (ANA), anti-double-stranded DNA (ds DNA) antibody, complements (C3 and C4), anti-extractable nuclear antigen (ENA), and serum immunoglobulin (Ig) levels.
Statistical analysis
The t-test was used to analyze the continuous variables. The chi-square test was used to analyze the categorical variables. Differences were defined as statistically significant at p < 0.05. All data were assessed on computer using a SPSS 16.0 software package.
Results
Clinical manifestations
All 56 patients with BD (34 male and 22 female: male to female ratio of 1.54) were 6–74 years of disease onset (median ± standard deviation (SD) age of 26.0 ± 8.5 years) with no significant difference (p > 0.05) between male (26.5 ± 13.1 years) and female patients (29.2 ± 12.0 years). There were 45 patients with disease onset at or below 25 years, 10 patients at 26–55 years, 1 patient at age more than 55 years. There were no significant differences (p > 0.05) between male (6.1 ± 5.3 years) and female patients (6.4 ± 7.8 years) among BD patients in duration of symptoms till diagnosis has been made. Oral ulcers were seen in 46 out of 56 patients with BD during the clinical course (82.1%) which often appeared in buccal mucosa, gingivae, tongue, lips, and soft palate. In total, 16 patients (28.6%) with BD had cutaneous lesions, frequently as pseudofolliculitis or papulopustular lesions, erythema nodosum–like lesions and erythema multiforme–like lesions. Papulopustular lesions were noted in eight patients (14.29%). Four patients (7.1%) exhibited erythema nodosum lesions and all of them were males. Four (7.1%) of 11 (19.6%) patients with BD had the pathergy test found with positive skin pathergy reaction. Of 56 patients, 40 patients (71.4%) were found to have genital ulcers commonly seen in scrotum, penis, and glans in male and labia, vagina in female. In total, 32 (57.14%) of 56 patients with BD had ocular lesions, including anterior and posterior uveitis, keratitis, scleritis, episcleritis, optic neuritis, and conjunctivitis. None of the 56 patients had retinal vasculitis.
Involvement of the joint occurred in 34 patients (60.7%), manifested as asymmetric arthritis. The most common site was knees, followed by the ankles and wrists. Joint involvement was more frequent in females (68%) than in males (55%) (p < 0.05). In total, 13 patients (23.2%) with GI involvement had the symptoms of abdominal pain, distension, diarrhea, constipation, and hematochezia. GI involvement was more frequent in male than in females (p < 0.05). In total, 17 patients (30.3%) were found to have vascular lesions, 12 (21.4%) patients were found with venous lesions: superficial phlebitis (1 patient), deep vein thrombosis (5 patients), cortical venous thrombosis (3 patients), and large vein thrombosis (3 patients: inferior vena cava thrombosis (1 patient), superior vena cava thrombosis (1 patient), and iliac vein thrombosis (1 patient)). Furthermore, five (8.9%) patients were found with arterial lesions: thrombosis (four patients: iliac artery thrombosis (one patient), popliteal artery thrombosis (one patient), subclavian artery thrombosis (one patient), and renal artery thrombosis (one patient); and pulmonary artery aneurysm (one patient)). In total, 24 patients (42.9%) were found with neurological involvement that varies from nonspecific manifestations like headache in 15 (26.8%) and dizziness in 11 (19.6%) to severe symptoms like epilepsy in 10 (17.9%), cranial nerve involvement in 3 (5.4%), and disabled cardiovascular accidents (CVAs) in 7 (12.5%). None of the patients showed brain stem involvement, cerebellar syndrome, spinal cord involvement, or peripheral nervous system manifestations. None of the patients found with renal, urogenital, epididymitis, or cardiac involvement.
Laboratory examinations
In total, 23 patients (41.1%) found with increased ESR at time of diagnosis. None of the 56 patients showed renal involvement (no abnormalities in urinalysis or 24-h proteinuria). Additional tests (C3 and C4, ANA, anti-ds DNA, Anti-ENA, and Ig level) were conducted to exclude other possible differential diagnosis in these patients. C3 and C4 levels were found normal in 10 patients (17.9%), 1 patient showed high C3 and C4 levels; whereas, in rest of the patients who presented with classical BD manifestations, test was not conducted. The positive rates of ANA found in 3 patients (5.4%), ANA found negative in 53 patients (94.6%), anti-ds DNA found positive in 1 patient (1.8%), and negative in 55 patients (98.2%). Anti-ENA were positive in 4 patients (7.1%) and negative in 52 patients (92.9%). Out of 56 patients, only 3 had both HLA-B5 and HLA-B51 typing test due to the high expense and the unavailability of the HLA typing, in which 2 (3.6%) patients were positive and 1 (1.8%) patient found with negative result for both tests. Out of 56 patients, Ig level measured in one patient who found low: IgG, IgM, and IgA. The clinical manifestations and results of laboratory examinations in 56 patients with BD are shown in Table 1.
The clinical manifestations and laboratory examination results in 56 patients with BD.
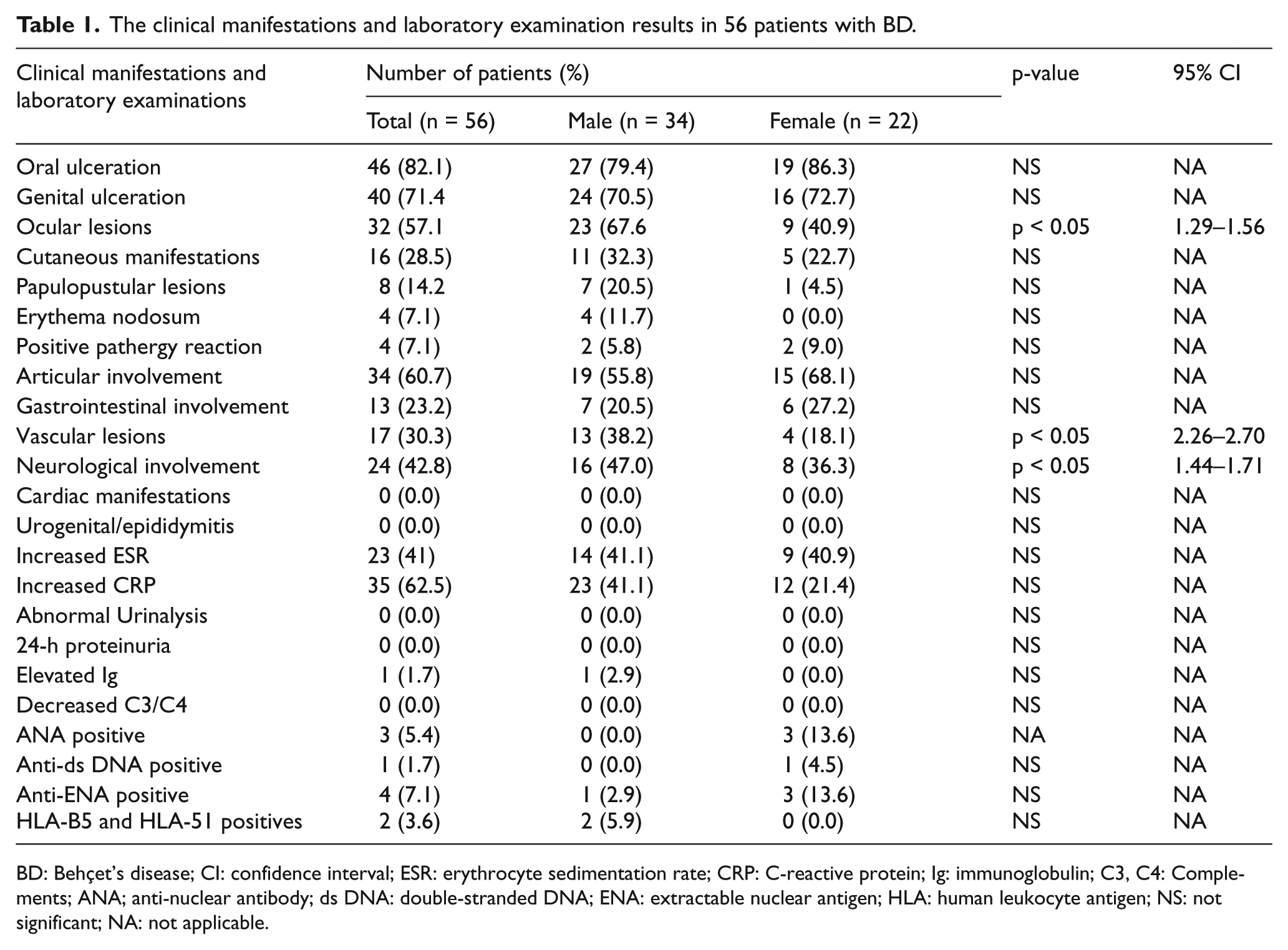
BD: Behçet’s disease; CI: confidence interval; ESR: erythrocyte sedimentation rate; CRP: C-reactive protein; Ig: immunoglobulin; C3, C4: Complements; ANA; anti-nuclear antibody; ds DNA: double-stranded DNA; ENA: extractable nuclear antigen; HLA: human leukocyte antigen; NS: not significant; NA: not applicable.
Discussion
In this study, we evaluated clinical features of BD patients in Oman, and we compared the results with those of various areas in Turkey, Iran, China, Korea, and Japan as illustrated in Table 2. In our study, recurrent oral ulceration was the commonest presentation, followed by genital ulceration, arthritis, and ocular lesions. Oral ulcerations were found in 82.1% of patients, indicating key bases of diagnosing BD. Compared with oral ulceration, genital ulceration was less significant. Cutaneous manifestations were frequent occurrence in skin lesions, followed by papulopustular and erythema nodosum–like lesions. These results differed from those in other parts of Asia.2,16 Ocular lesions were quite not uncommon with 57.1%, although rarely they developed severe. None of our patients showed retinal vasculitis unlike majority of the reports.21,22 No clear explanations could be made here, but this could be due to un-studied underlying genetic factors. Although positive pathergy reaction occurs much more commonly in Turkish and German patients, it only occurs in about 15% and 44% of Korean and Japanese patients, respectively, reducing its diagnostic value in these groups. It showed a high incidence in some regions of China, suggesting that it has a diagnostic value and is specific to BD in China. 23 In this study, no conclusion could be made on pathergy positive rate as test was done only in 11 out of 56 patients in which found 4 were positive. No cardiac, pulmonary, urogenital manifestations, or epididymitis were found among our patients. As many as 34% of patients with BD had non-destructive or deforming arthritis. Rare renal vasculitis is characterized by diffuse or focal glomerular abnormalities, more commonly mild proteinuria and microscopic hematuria with normal renal function are found. Amyloidosis and IgA nephropathy are the most frequent.24–26 None of our patient reported with renal manifestations. Epididymitis and other urogenital manifestations were not seen although other reports from South Asia reported some cases.2,16 GI involvement in BD is characterized by ulceration along the GI tract, and we found three patients with cecum ulcerative lesions, two patients with terminal ileum ulcerative lesions, four patients with gastric/duodenal ulcer, one patient with esophageal ulcerative lesion, and no rectal lesions were identified. The other three patients found with functional abnormalities. Most neurological manifestations of this group of patients included headaches and dizziness without specificity. However, a significant number of cases showed serious symptoms such epilepsy, cranial nerve palsies, and ischemic strokes while none of our patients showed brain stem involvement, cerebellar syndrome, spinal cord involvement, or peripheral nervous system manifestations. Vascular involvements were not uncommon, and both arterial thrombosis and venous thrombosis were detected. The frequency of vascular complications of BD among Omani patients was comparable to those reported around the world. 27 Some reports revealed that younger male patients with short disease duration are at a greater risk of developing thrombosis. 27 In compassion with data published in the region, more pronounced neurological and vascular manifestations noted among our group of BD patients. The diagnosis of BD has been based on clinical criteria and not on pathognomonic laboratory findings. Abnormal values such as leukocytosis, increased ESR, and elevated IgG, IgA, and IgM are often seen in disease exacerbations. 28 Despite our attempt to make wild speculations or conclusions that genetic and immunological factors might participate its aetiopathogenesis, data did not support this. However, above results helped to exclude other possible differential diagnosis in these patients. HLA-B51, the genetic marker of BD, has been reported to exhibit strong association with the disease in different ethnic groups. 28 The frequency of HLA-B51 in patients with BD was 25%–80%. 28 HLA-B5 and HLA-B51 in our study were done for minority of patients (due to test unavailability and high expenses), and data collected do not reflect actual percentage and comparison with other studies cannot be made. Our patients study group included juvenile cases, which may be interesting and unique if compared with most of the data published. Furthermore, male patients were slightly more than females and there were no differences in mean age of disease onset and mean duration between male and female patients. There was male predominance with most of the clinical manifestations like skin lesions, oral ulcers, genital ulcers, and ocular lesion. No difference could be found between males and females in positivity of skin pathergy reaction. In addition, male predominance was noted in other manifestations like GI, neurology, arthropathic, and vascular lesions. Laboratory test showed male predominance in terms of positivity and diagnostic support as noted with increased inflammatory markers (ESR and CRP) and positive HLA-B5 and HLA-51.
Clinical features of BD patients in Oman compared with those of various areas in the region.
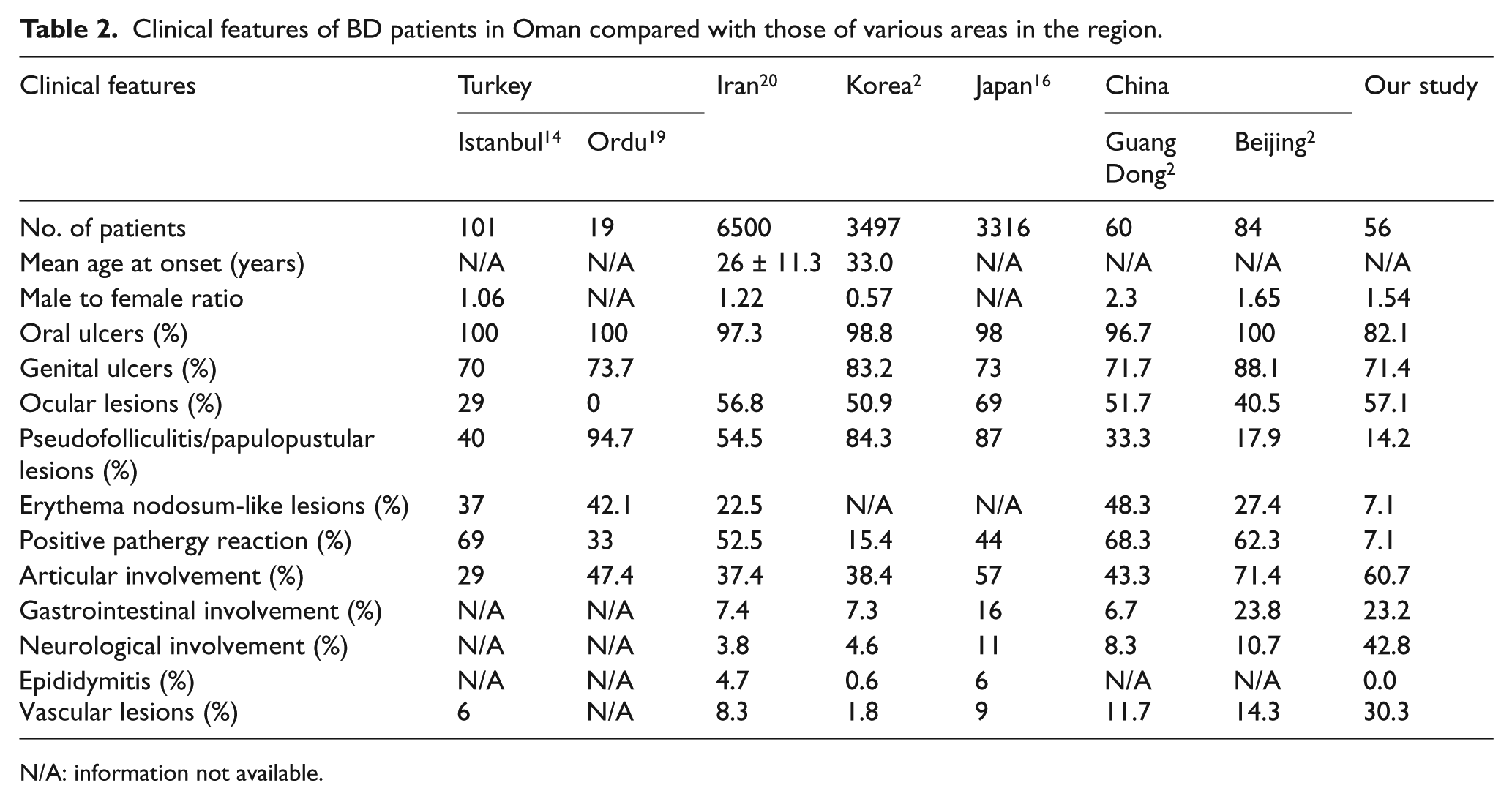
N/A: information not available.
Footnotes
Acknowledgements
The authors thank Department of research, Oman Medical Specialty Board, Muscat, Oman, for their excellent technical assistance.
Declaration of conflicting interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: The research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
