Abstract
Objective
Concussions cause microstructural damage, which we hypothesize leads to a lack of synchrony in the brain. Interactive Metronome (IM) behaviorally assesses how well an individual can maintain a steady rhythm under both unsupervised (absence of feedback) and supervised (presence of visual feedback) conditions. If concussion causes dyssynchrony, then we predict that children with concussion do worse on IM than healthy children and that the difficulty should be greatest during the unsupervised condition, when the children must self-regulate their rhythm performance.
Setting and Participants
Seventy-four children and adolescents (age range 8–17 years) were assessed on IM across two different tasks (unsupervised – “no feedback” and supervised – “visual feedback”) during a clinic visit after their concussion injury and diagnosis.
Design and Main Measures
We compared the participants with concussion to a healthy control group (N = 73, age range 15–19 years) with respect to their ability to clap on time with a steady beat using IM, calculated as ms off the beat, separately for the unsupervised and supervised conditions.
Results
Results reveal participants with concussion struggled to maintain a steady rhythm compared to the control group, particularly during the unsupervised condition.
Conclusion
These results support the hypothesis that concussion can give rise to brain dyssynchrony. IM captures this dysfunction and, we suggest rhythmic training has the potential to re-establish synchronization among neural networks that may be compromised after a concussion. Interventional studies are a necessary next step for testing the efficacy of IM training to accelerate concussion recovery.
Keywords
Introduction
A concussion is known to impact brain function while preserving neural macrostructure.1 It is often caused by a direct blow to the head, or by a hit to the body that causes the head and brain to move quickly back and forth or twist in the skull. This sudden movement generates metabolic changes,2–4 and damages to microstructural components including dendritic arbors, axons and astrocytic processes.3,5,6 We hypothesize that these changes impair communication between neurons, leading to a lack of synchrony in the brain that ultimately affects how a person thinks, learns, hears, feels, acts, sleeps, etc., and that this dyssynchrony persists throughout the recovery process.
In this study we aimed to examine the impact of concussion on brain synchrony through the lens of Interactive Metronome (IM). IM is a rhythm training and assessment program that constitutes different tasks, all requiring repeated whole-body synchronization over a steady timescale, that track how well an individual can maintain a consistent rhythm, both on their own and in the presence of a feedback. In this study we focused on the clapping hand-to-hand task, without and with visual feedback. Each of these tasks require the person to accurately perceive and understand auditory information (a steady metronome beat), select goal-directed behavior in a time-dependent manner (clapping hands in time with the beat), and in the case of the feedback condition, update their rhythmic pattern with provided information on their accuracy (adjusting the clapping based on the online visual feedback). 7
IM offers a window into not just behavioral synchrony, but also neural synchrony. Indeed, the ability to move along to a beat, a core component of IM, is linked to neural synchrony, with poorer performance on the IM task linked to poorer neural synchrony.8–12 Knowing that IM provides a window into neural synchronization, it represents an ideal assessment tool to detect dyssynchronization consequent to a concussion. If concussion causes dyssynchrony, then we expect it to be evident in behavioral rhythm tasks like IM.
In the current study, we test whether concussion causes dyssynchrony by comparing IM performance during two different rhythm-making tasks, an unsupervised task where participants are instructed to maintain their own internal rhythm at a prescribed rate and a supervised task where the participants receive within-cycle feedback on their ability to maintain that rhythm. Comparisons of performance at these tasks were made between children with concussion and a control group. We predict that the children with concussion will do worse on IM than healthy controls. Moreover, given the different nature of the two activities, we expect children with concussion to perform poorest in the unsupervised condition, where there is no feedback to help them align their clapping and they must rely on their own internal synchronization/timing abilities to maintain performance on this task.
Methods
Northwestern University's Institute Review Board approved all research procedures. Written informed assent and consent were obtained from the children and their legal guardians, and the children were monetarily compensated for their time.
Participants
Two groups participated in this study: the concussion group (mTBI) and the control group (control). The concussion group (N = 74, 43 females, mean age = 14.51 yr, SD = 2.17 yr) was recruited from the Institute of Sports Medicine at Ann & Robert H. Lurie Children's Hospital of Chicago. At this specialty clinic, physicians see the most severe and lingering cases of concussion with patients reporting symptoms for many weeks after their injury. Children in this group met clinical diagnostic criteria for a concussion established by the Consensus statement on concussion defined in the 5th international conference 13 and participated in the experiment following their medical evaluation by sports medicine physicians with expertise in concussion diagnosis and management. On average, they were evaluated 52 days after their injury (mean = 52.2 days, SD = 63.3 days, range: 2–340 days). Injuries were attributed to sports activities (58%), motor vehicle accidents (15%) and other accidental events (N = 27%).
The control group (N = 73, 34 females, mean age = 18.08 yr, SD = .703 yr) was designated based on Interactive Metronome data availability from the Auditory Neuroscience Laboratory database. It includes high-school students previously recruited from three public high schools in Chicago, Illinois. None of these students reported a history of brain injury.
The groups did not differ in sex distribution (Pearson Chi-Square = 3.029; p = .082) and music experience (Pearson Chi-Square = .824; p = .364) but were not matched by age (t = 13.343; p < .001). The age difference is taken into account in all statistical analyses by considering z-scores computed from normative data by age for both groups.
As for the music experience variable, all participants were categorized as musicians or non-musicians based on their exposure to any vocal or instrumental training in the years before enrolling in the study. Musicians were required to have more than 1 year of either vocal or instrumental training, whereas non-musicians had no past experience of structured musical training. This information was collected by a self-report questionnaire completed by the parent/guardian or the participant during the assessment session.
Rhythmic assessment with interactive metronome (IM)
This task measured participant's ability to clap in time with an isochronous pacing beat with (visual feedback IM) or without any feedback (no feedback IM). In both conditions, participants were asked to clap their hands together by moving their arms in a fluid circular motion against a hand trigger in time with a pacing tone delivered over headphones. The participant was required to stand while performing the task. All participants were assessed at no feedback IM first and then at visual feedback IM.
In the IM visual feedback condition, a visual indicator, aimed at facilitating the clapping at the correct rate and phase, was shown on a computer screen. The indicator reflected the asynchrony between their last clap and the target beat (ms ahead of or behind the beat). The ms offset indicator appeared in a colored box spatially corresponding to their offset in relation to the target. Each box represented a 30 ms window. If the participant clapped, for example, within 15 ms of the target, the offset in ms appeared in the central green box, whereas if the participant clapped 47 ms earlier, the ms appeared in the red box to the left of the target. Synchronization was performed at an IOI of 1111 ms for 3 min without any practice period for both IM conditions. Overall performance is calculated as ms off the beat and it is automatically computed and reported by the IM software.
Post-concussion symptoms scale
The Post-Concussion Symptom Scale (PCSS) is a 22 question self-report measure that records the severity of symptoms post-concussion using a 7-point Likert scale ranging from 0–6. Higher scores indicate greater severity of symptoms; the highest possible score is 132 and the lowest possible score is 0. The PCSS explores 22 concussion-related symptoms such as headache, nausea, sensitivity to light, etc. The PCSS indexes the symptom load conferred by the injury and is collected at every post-concussion visit.
Participants with concussion report an average PCSS total score of 34.51 (SD = 26.47) with a minimum of 1 and a maximum of 108. The most frequently reported symptom is headache whereas the least reported is vomiting. Fifteen of the 22 symptoms were reported by at least half of the participants with concussion. Moreover, 12 participants reported loss of consciousness and 15 documented post-traumatic amnesia.
Statistical analysis
Statistical analysis was performed with SPSS (SPSS, Inc., Chicago, IL).
Given the age difference between the two groups, to compare IM performance between the two groups we computed z-score for all participants using normative data 14 across age (Figure 1(a) and (b)).
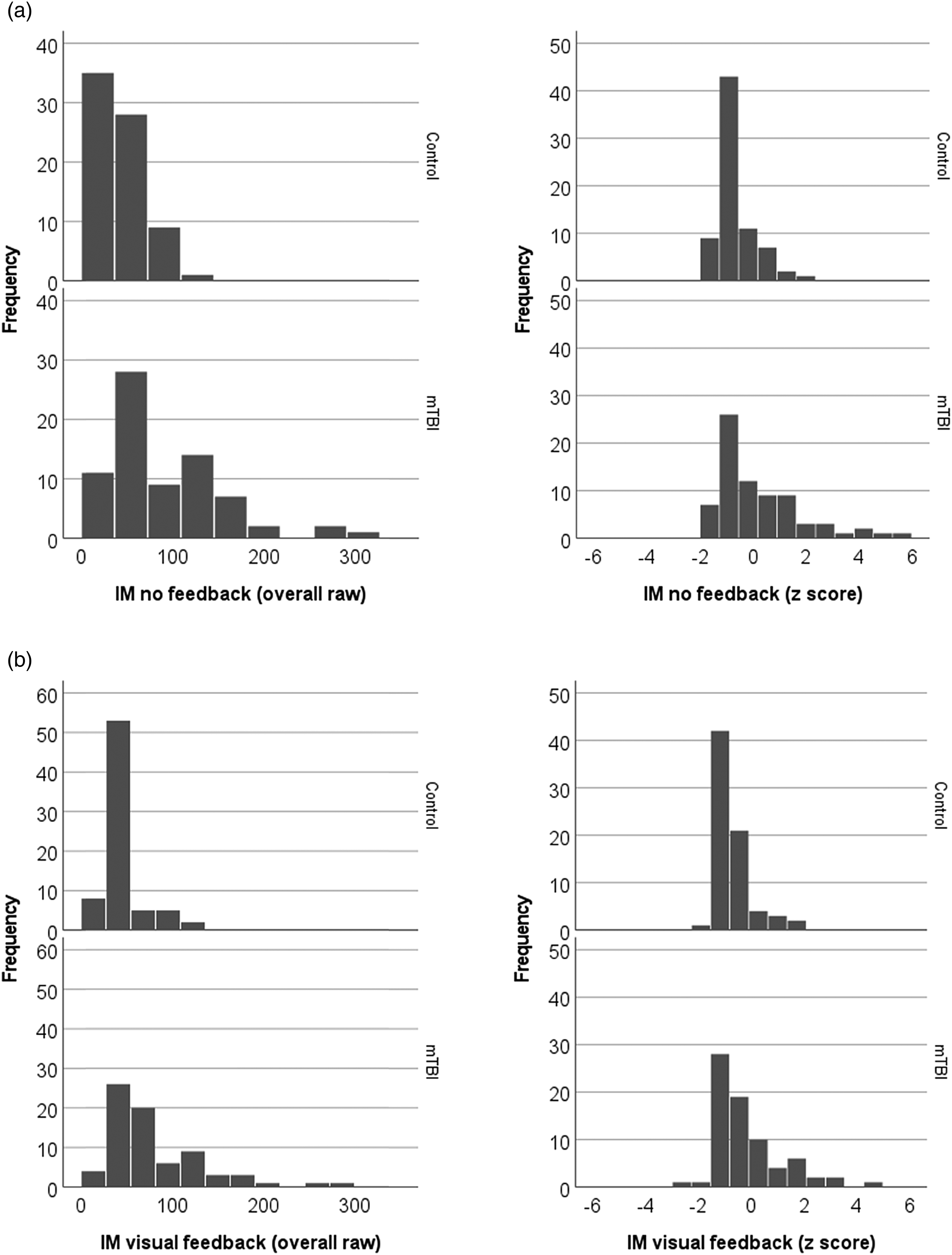
Histograms of IM performance (a. no feedback; b. visual feedback) across subjects within each group (top: control; bottom: mTBI). Left panel reflects raw data (msec); right panel reflects z scores. Lower score indicates better performance.
A repeated measure ANOVA 2*2 (IM condition*mTBI group) was computed to assess differences between the groups (mTBI and control) within the two different IM conditions.
Results
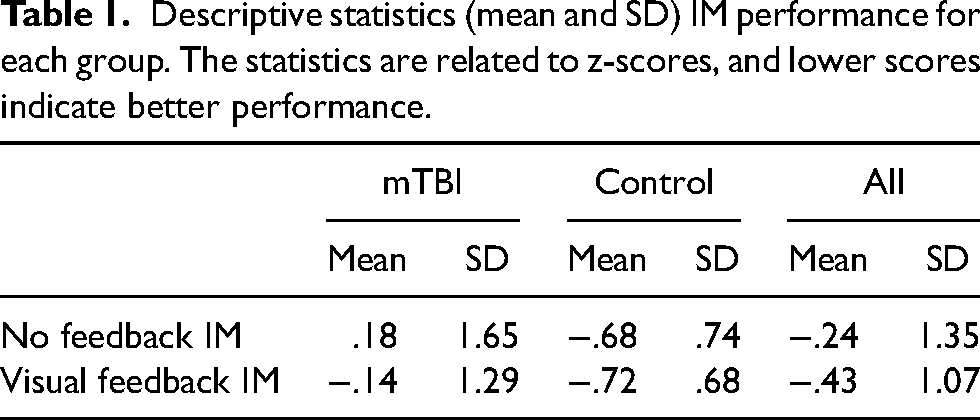
A significant main effect of group revealed that children with concussion performed more poorly than controls at IM (F = 16.267; p < .001; µ2 = .101). A significant main effect of IM condition indicated that children performed more poorly in the No feedback condition than the condition with Visual FB (F = 6.637; p = .011; µ2 = .044). The IM condition*group interaction was also significant revealing that only children with concussion exhibited a significant difference in their performance between the two IM conditions (F = 4.226; p = .042; µ2 = .028) (Figure 2). In particular, within the control group no significant difference is revealed between the two IM conditions (F = .135; p = .714; µ2 = .001) whereas within the mTBI group a significant difference is present between the two IM conditions (F = 10.800; p = .001; µ2 = .069). Table 1 reports descriptive statistics related to IM performance for each group.
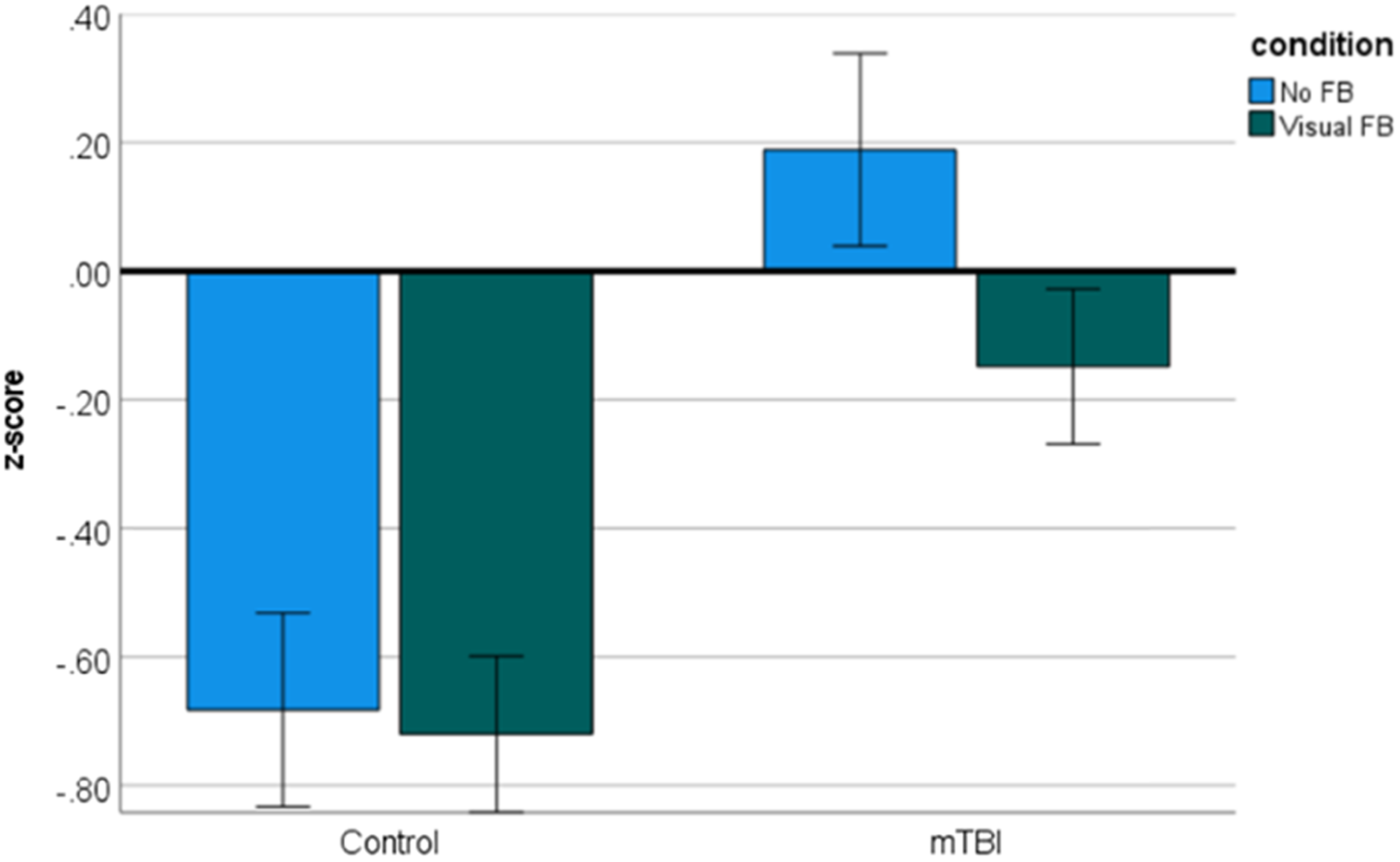
Mean IM performance across different groups and IM conditions. Lower score indicates better performance. Error bars represent ± 1 standard error of the mean.
Discussion
We compared IM performance of children with concussion to a control group of typically developing adolescents across two different Interactive Metronome activities: one where the children maintained their own rhythm and were not provided within-trial feedback on performance (unsupervised) and another condition where they received within-trial feedback on their clap timing (supervised). We found that children with concussion show poorer IM performance than control participants and that this is especially driven by a decrease in performance in children with concussion in the unsupervised condition. That is, children with concussion perform worse in the no feedback condition than in the visual feedback condition, while control participants do not differ in performance across the two IM conditions.
The difficulty that the children with concussion experienced, particularly during the unsupervised condition, supports the hypothesis that concussion causes dyssynchrony in the brain, which disrupts the internal time-keeping of an individual with concussion. When no feedback is provided, participants must rely on their own intrinsic rhythmicity to stay in time with the beat, suggesting that the poorer performance of children with concussion on that task is driven by neural dyssynchronization disrupting their intrinsic rhythmicity. With respect to the supervised condition, even though children with concussion performed worse than healthy controls when visual feedback on performance was provided, the magnitude of this group difference was smaller than in the unsupervised condition. These findings suggest that children with concussion can use an external trigger to correct their timing and further suggest rhythm training as a mechanism to restore synchrony following a concussion.
These results support the idea that IM both captures the dyssynchrony caused by concussion and ameliorates this problem by providing within-trial feedback. Thus, IM has the potential to help re-establish efficient and synchronized connections among neural networks that are compromised by a concussion. Parallel electrophysiological evidence would be needed to provide further evidence. In particular, showing data on auditory brain synchrony with respect to the two IM conditions, supervised and unsupervised, would allow to test the hypothesis that the increased synchrony is the mechanism by which performance in the supervised task was better compared to the non-supervised one for the concussed children. Even though IM has already been shown to be a promising post-concussion treatment in the context of small pilot and/or case studies,15–17 future research should investigate whether prescribing routine IM therapy to individuals with concussion can accelerate recovery from this injury, particularly in those who have a protracted recovery.
Descriptive statistics (mean and SD) IM performance for each group. The statistics are related to z-scores, and lower scores indicate better performance.
Footnotes
Acknowledgements
We thank the past and present members of the Auditory Neuroscience Laboratory for their contribution with data collection. We thank the team and the families of the Ann and Robert H. Lurie Children's Hospital who made this study possible. This work was supported by NAMM Foundation and Knowles Hearing Center of Northwestern University.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the NAMM Foundation and Knowles Hearing Center of Northwestern University
