Abstract
Context
No prior study has examined inversion position testing in individuals who have experienced sports related concussions.
Objective
To investigate whether the inversion position testing (IPT) would un-mask symptoms in asymptomatic concussed collegiate athletes during the return to play progression assessment.
Design
Case-Control Study.
Setting
Athletic Training Room.
Participants
One hundred and thirty-nine collegiate student athletes were randomly recruited from 12 different sports belonging to National Collegiate Athletic Association Division I Conference.
Main outcome measure(s)
A baseline concussion symptom questionnaire was administered. Of the 139, 122 participants without any of the suspicious symptoms related to concussions were examined using the Concussion Symptom Inventory (CSI) in connection with IPT. Also, the 18 concussed athletes underwent the IPT when any symptom subsided.
Results
Eighteen of the 122 (16.2%) non-concussed athletes showed some post-IPT symptoms, while 5 of 12 (41.7%) concussed athletes showed some post-IPT symptoms in the baseline test. For the latter, neither the interaction (P = 0.08) nor difference in the total CSI score was observed either from pre- to post-IPT (P = 0.14) or between the baseline and post-concussion (P = 0.96).
Conclusion
This study demonstrated that symptoms could be exacerbated by the IPT in concussed athletes even when their original symptoms had subsided prior to the testing. The IPT exacerbated post-concussive symptoms may depend on a number of days required for post-concussive symptoms to subside. The innovative instrument of IPT may prove effective in clarifying the degree to which post-concussive symptoms have subsided.
Key words
Concussion, College athletes, Inversion position, Symptoms.
Introduction
The approximate numbers of athletes who suffered from sports-related concussions (SRC) have been clarified for each performance level. Among high school athletes SRCs account for 21–27% of all sport injuries. 1 For collegiate athletes, SRCs accounted for 6.2% of reported injuries with the greatest numbers of SRCs occurring among football players (36.1% of injuries), men's ice hockey (13.4%) and women's soccer (8.1%). 2 For one National Collegiate Athletic Association (NCAA) Division I Football Bowl Subdivision program, the incidence of concussion was 1.19 per 1000 athlete-exposures (AEs) in all games and practices over a nine-year period. 3 This rate was considerably higher than the overall risk of concussion, reported at 0.23 per 1000 AEs overall in sports involving those under 18 years of age. 4 Gender differences in concussion injury rates have been identified ranging from 0.07 (baseball) to 0.91 (women's ice hockey) per 1000 AEs. Females showed a 1.4 time greater incidence of concussion than males owing to greater peak head and neck angular acceleration suggested as explanations. 5 In contrast, the National Football League (NFL) reported 0.38 concussed athletes per game 6 although athletes have incurred the risk of concussion in 25.9% of the 480 NFL regular games. 7
Many healthcare providers rely on some specific form of symptom assessment protocol to evaluate SRCs in the course of return to play (RTP) decisions.8–10 One problem in RTP decisions may be that the symptom scores are often assessed using a 7-point Likert scale in connection with the Sport Concussion Assessment Tool (SCAT), a method that is by nature subjective and dependent on self-reporting. 11 Thus, self-reporting of SRC symptoms may lead to under-estimation of their severity owing to a desire on the part of athletes to RTP; 12 in any case, females seem to be more honest in their reporting than males. 5 Also, the total symptom score at baseline testing may vary in relation to fitness level while women who take oral contraceptives tend to show fewer symptoms. 13
Inversion positioning can reliably provoke concussive-type symptoms specifically causing a temporary exacerbation of such pathophysiological processes theoretically temporarily affecting vestibular function, cerebral blood pressure, and/or autonomic nervous system.14,15 No prior study has examined inversion position testing in individuals who have experienced SRCs despite the prevalence of subjective observations included in symptom check-list evaluations. Therefore, this study investigated that inversion position testing (IPT) had considerable potential as a means to induce or detect whether injured athletes have fully recovered through the identification of subtle symptoms by temporarily exacerbating the pathophysiological processes with which they are associated. Therefore, the aim of this study was accordingly to determine whether IPT could amplify, exacerbate or un-mask symptoms in concussed athletes. This study hypothesized that the testing would assist healthcare providers assessing whether athletes’ symptoms had subsided sufficiently for them to proceed further with a RTP protocol. Theoretically the practical implication of this study was the potential method to improve accuracy in identifying the concussed athlete who might still not be fully recovered and unfit for RTP, and thus decreasing the incidence and severity of permanent traumatic brain injury.
Methods
Participants
This study was approved by the university's institutional review board, and all participants read and signed the informed consent forms prior to every examination. One hundred and thirty-nine student athletes, all of whom belonged to the NCAA Division I (D1) conference, were randomly recruited from a pool of approximately 450 student athletes (30.9%). The number of participants was determined in part by the amount of time available for the athletic trainers (ATs) who examined the participants, the latter of whom were identified through a pre-participation examination.
Selection of participants
A baseline concussion symptom questionnaire was administered that consisted of 18 yes/no questions regarding current suspicious symptoms related to concussions that had occurred following head injuries that the participants had suffered (Table 1). Seventeen participants who responded positively to at least one of the questions were excluded. The remaining 122 participants, equally balanced between males and females, were examined using the Concussion Symptom Inventory (CSI) in connection with IPT across seven different days during the course of the pre-participation examination. Of the 61 male athletes, 32 played football, 22 soccer, and 7 basketball players; of the 61 female athletes, 16 were gymnasts, and 21 played soccer, 8 volleyball, 9 basketball, 3 softball, 1 diving, 1 golf, 1 tennis, and 1 water polo. Thirty-three of the 450 athletes had been diagnosed with an SRC during the course of the season (7.3%), 18 of whom again balanced in terms of gender agreed to participate in the IPT in anticipation of the physical exertion leading to RTP (Table 2).
Baseline concussion symptom questionnaire. This initial self-reported questionnaire regarding suspicious symptoms related to concussions was administrated to all subjects, who were randomly recruited prior to the inversion position testing (IPT). Any potential subject who answered any of the 18 questions with “Y” (yes) was excluded from the IPT.
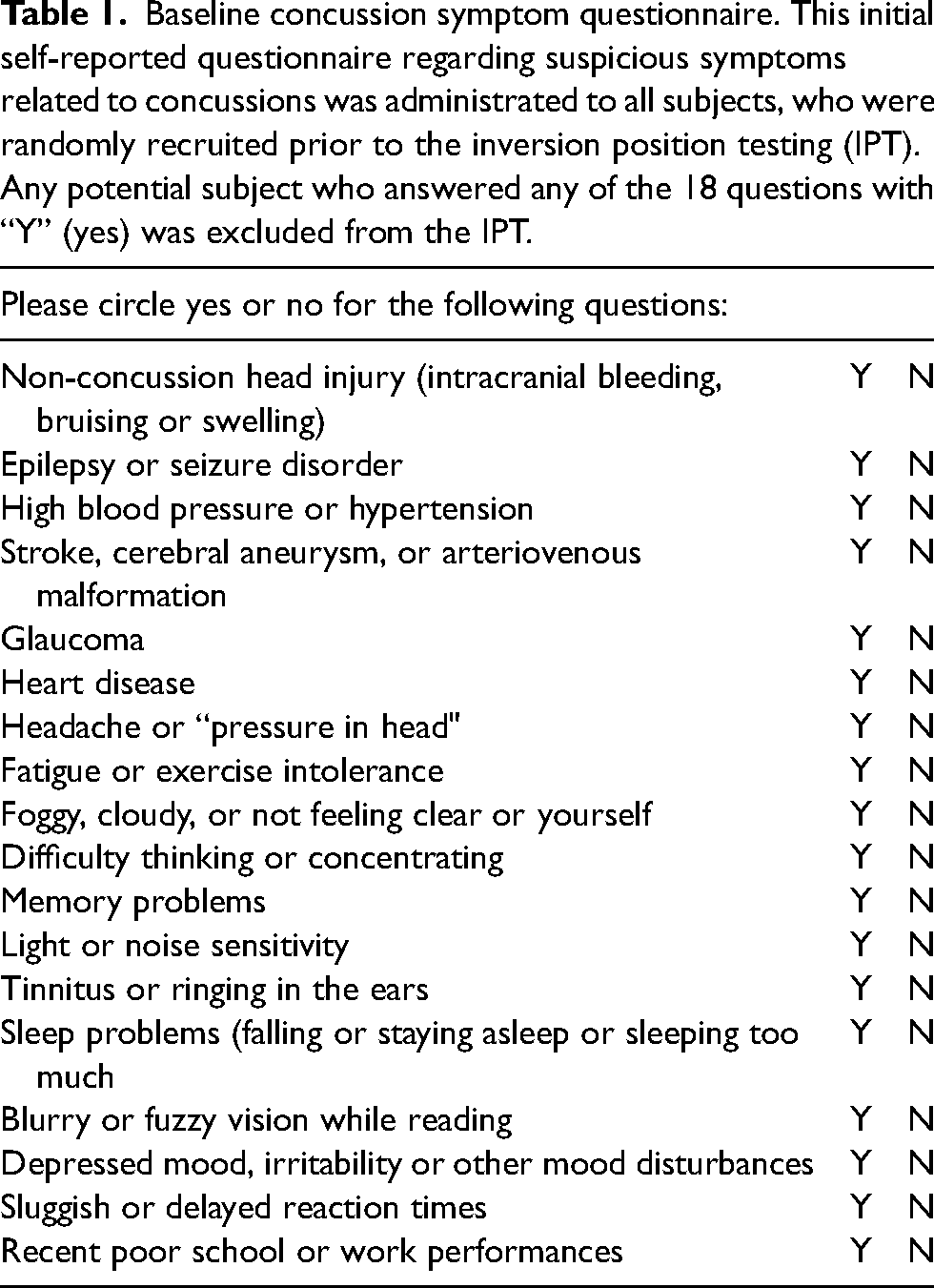
Number of concussed athletes who participated in the inversion position testing after sports-related concussions with demographics and concussion history.
Examination procedure
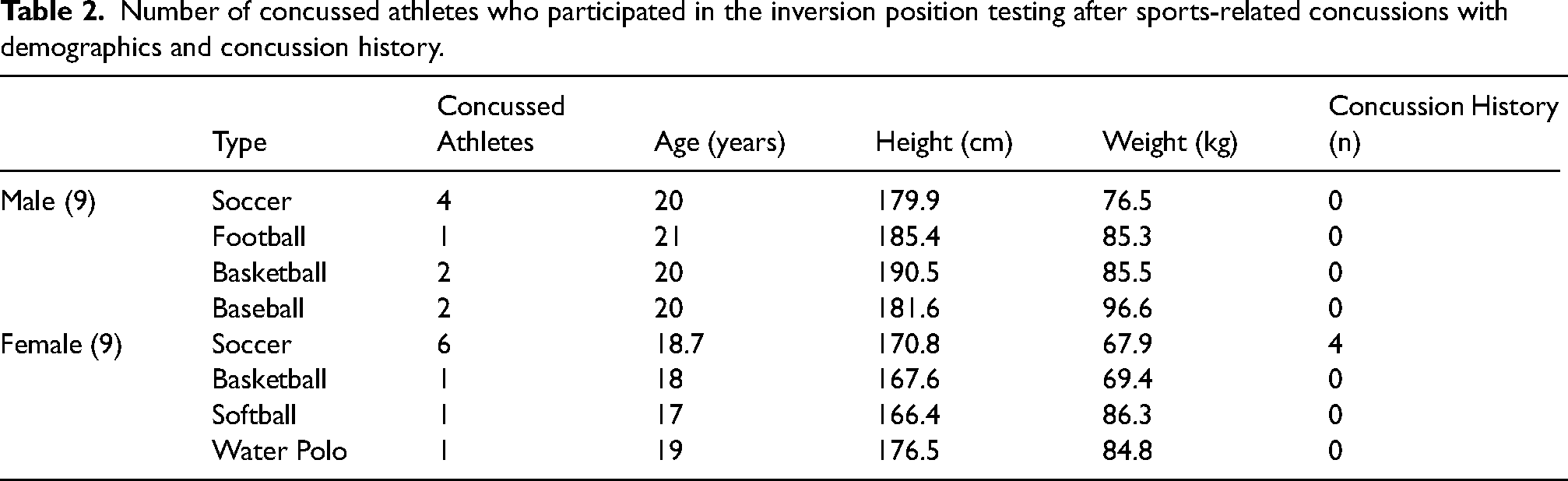
The IPT was administered for baseline purposes as a comparison to assess potential changes caused by a concussion. For the procedure, all of the participants reclined with their heads tilted upward at a 45-degree angle on a table designed for the purpose (Ironman ATIS 4000 Inversion Table, Model # 5903, Industry, CA USA). Their bodies rested against a backrest which was constructed of nylon-covered steel tubing. The participants’ feet were placed on a platform adjusted to the heights of each with an adjustable beam, which was clearly marked in centimeters and inches, serving to keep them stable. Their ankles were firmly cupped by adjustable fittings that were ergonomically shaped to hold them in place without pinching the sensitive skin. The participants were then passively inverted backward at approximately 180 degrees from vertical for 30 s while hanging by their feet (Figure 1).
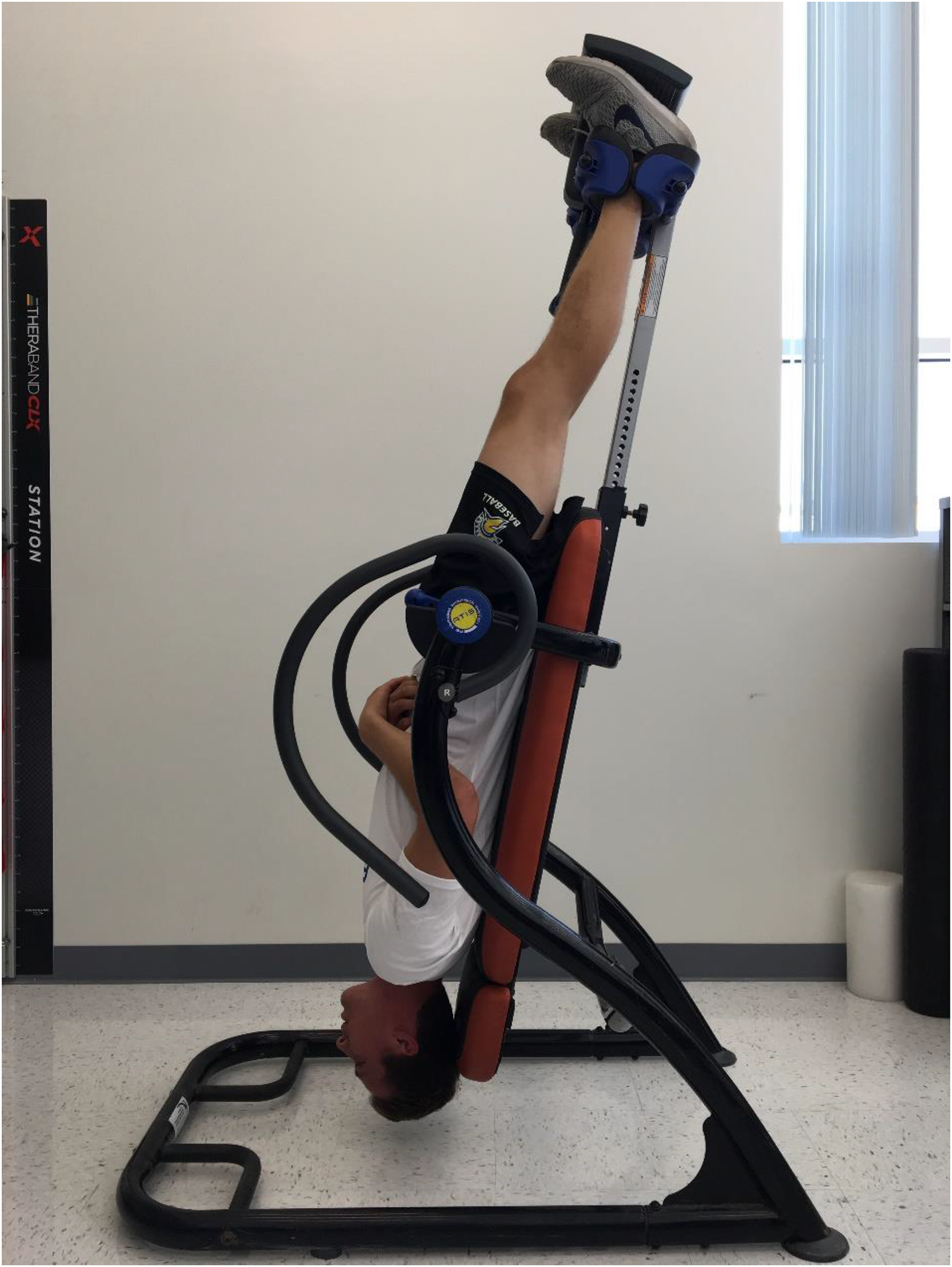
Ending position of inversion position testing. The participants were passively inverted backward at approximately 180 degrees from right angles for 30 s while hanging by the feet.
Data collection and analysis
All of the participants were asked to complete the CSI, a self-reported concussion symptom scale, listing 12 symptoms for which they rated their current status on a 7-point Likert scale. They were led through the list of symptoms by an AT each time (Figure 2). For scoring, 0 indicated the absence of a symptom, 1 and 2 relatively mild occurrence of a symptom, 3 and 4 moderate occurrence, and 5 and 6 severe occurence. 14 Immediately after having been placed in the initial position, the participants were again asked for their status using a post exam that was the same as the pre-exam.
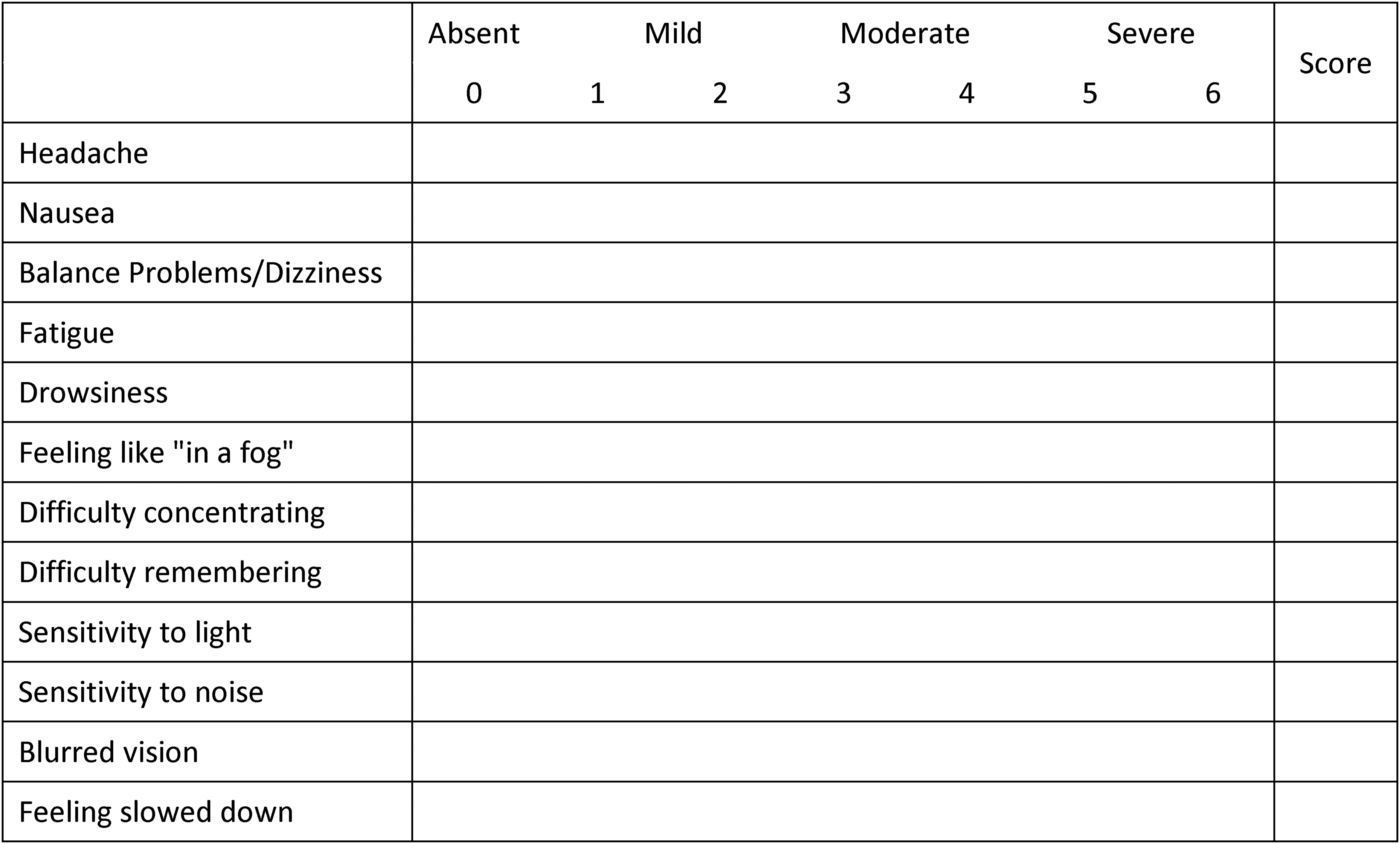
Concussion symptom inventory. A self-reported 12-item questionnaire was used to identify the status of concussive symptoms. The 7-point Likert scale ranged from 0 for the absence of a symptom, 1 to 2 for mild symptoms, 3 to 4 for moderate symptoms, and 5 to 6 for severe symptoms.
For analyses of the data represented by these CSI scores, a 2 × 2 (baseline/post-concussion x pre/post-test) repeated measures analysis of variance (ANOVA) design for the concussed athletes who had taken the IPT to serve as a baseline during the pre-participation examination. All statistical tests were performed at a 0.05 level of probability (P < 0.05).
Results
For this study 122 non-concussed athletes (61 males and 61 females) took part in the pre-participation examination. Eleven were found to have had at least one symptom prior to the IPT and have accordingly been excluded from the following description of data. Next, 18 non-concussed athletes underwent induction of some symptoms in post-IPT, amounting to 16.2% of the 111 non-concussed athletes. These 18 individuals had had no suspicious symptoms of concussion prior to the IPT (Figure 3). The total number of symptoms displayed post-IPT by the 18 non-concussed athletes ranged from 1 to 4 (mean: 1.9; SD: 1.1). The greatest number of symptoms that were induced during the post-IPT included balance problems/dizziness followed by headache and feeling slowed down.
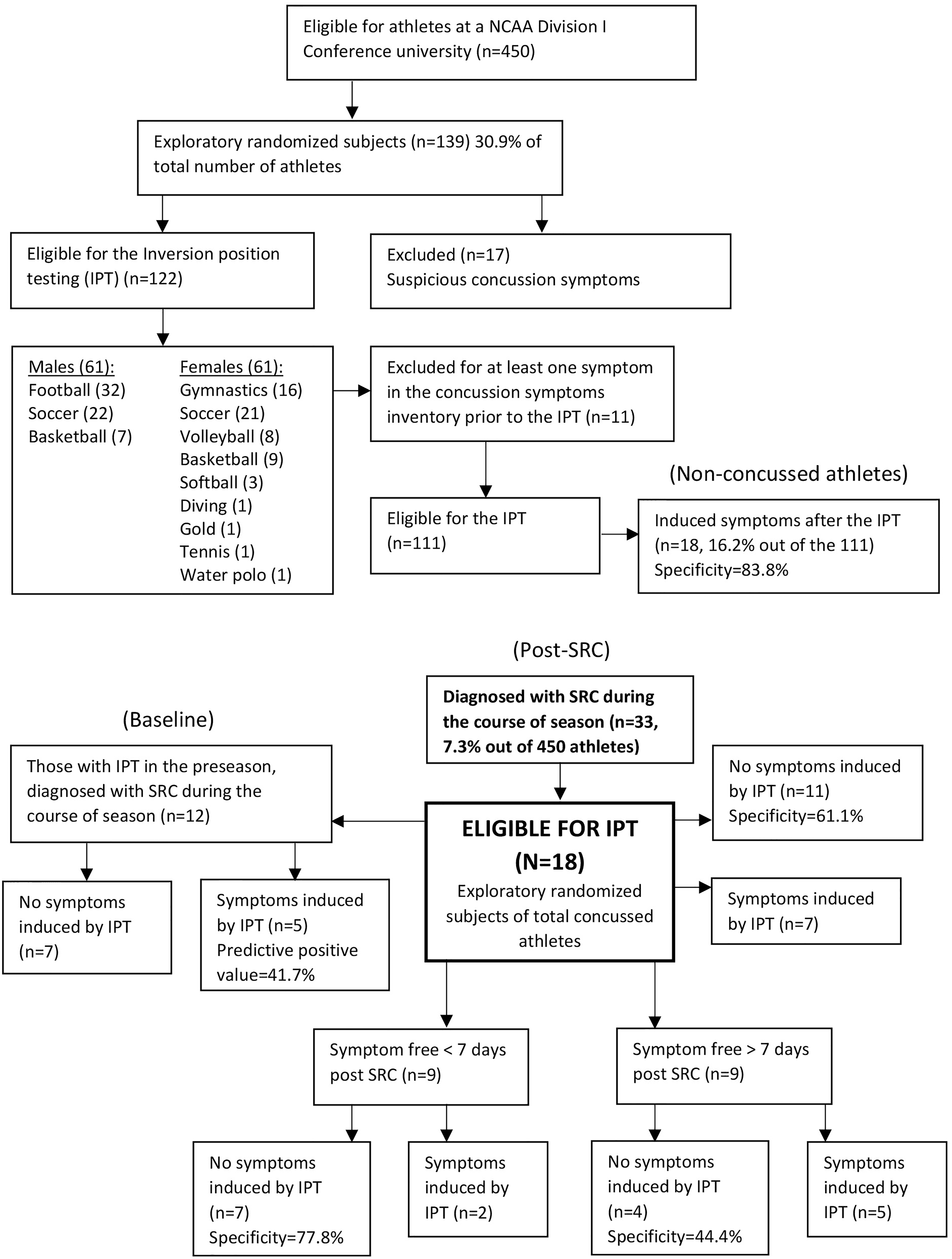
Flowchart for both non-concussive and concussive participants. Inversion position testing (IPT) was conducted on 139 non-concussed active athletes at baseline along with 18 concussed athletes. Of the 122 who underwent IPT, 111 non-concussed athletes were suitable for a comparison with the 18 concussed athletes.
The eighteen concussed athletes underwent the IPT when any symptom subsided. Eleven were identified as concussed based on the fact that their symptoms subsided in both pre- and post-IPT. The specificity was 61.1% for the post-concussed athletes (Figure 3). The false negative was thus 38.9%.
The time interval between the occurrence of a concussion and the date of examination ranged from 3 to 25 days (mean: 9.2; SD: 6.3 days) for the 18 concussed athletes. This variation was attributable to the nature of the concussion protocol, according to which a concussed athlete must be asymptomatic before the IPT, which was in turn followed by physical exertion leading to RTP. The 18 concussed athletes who participated in this study were accordingly separated into two groups, one consisting of those for whom the time interval was less than 7 days (9 concussed athletes) and the other of those for whom it was 7 days or more group (the 9 other concussed athletes). Within the former group, 7 concussed athletes showed no exacerbation of symptoms in the post-IPT; the specificity for this group was 77.8% and the false-negative rate consequently 22.2% (Figure 3). The other two concussed athletes belonging to this group did show an exacerbation of symptoms in the post-IPT, specifically headache and fatigue. Within the 7-days or more group, on the other hand, 4 of 9 concussed athletes showed no symptoms during the post-IPT. The specificity for this group was 44.4%, and its false-negative rate consequently 55.6% (Figure 3). This study could not determine whether the results of baseline test were predictable in the number of days to subside into the asymptomatic condition. In light of these findings, the intensity of the symptoms could be seen to correlate with this participant's sensitivity to IPT (Table 3).
A comparison of symptoms induced by the post-IPT for 7 concussed athletes asymptomatic after SRC: 2 athletes with symptoms subsided within 7 days, whereas 5 athletes with symptoms subsided for more than 7 days. One athlete with symptoms subsided within 7 days had the baseline test inducing symptoms: 1 moderate headache and 1 mild nausea, whereas 4 athletes with symptoms subsided for more than 7 days had the baseline tests inducing symptoms in two athletes: a mild headache for one athlete, mild nausea and fatigue for the other athlete.

Twelve of the 18 concussed athletes had taken the IPT to serve as a baseline during the pre-participation examination. Five of these 12 showed symptoms in the post-IPT during the baseline test and 7 did not. In contrast, 18 of the 111 non-concussed athletes showed some symptoms in the post-IPT, and 93 did not. Based on these observations, the positive predictive value was 41.7% (5/12) for the concussed group, whereas the specificity was 83.8% (93/111) for the non-concussed group (Figure 3). Conversely, the false-positive rate was 58.3% as type I error, and the false-negative rate was 16.2%.
A repeated 2-way ANOVA design was performed for the 12 concussed athletes who had participated in the baseline test. The mean total CSI score for the purpose of the baseline was 0.9 (SD: 1.3) prior to the IPT and 1.1 (SD: 2.0) in the post-IPT, whereas the mean total CSI score for the post-concussion was 0.6 (SD: 1.1) prior to the IPT and 1.3 (SD: 2.0) in the post-IPT. Neither the interaction (F1, 11 = 3.61, P = 0.08) nor difference in the total CSI score was observed between pre- and post-IPT (F1, 11 = 2.57, P = 0.14), nor between the baseline and post-concussion (F1, 11 = 0.01, P = 0.96).
Discussion
SRCs are not related to a pathological injury.9,16 This study identified post-SRC symptoms that had been exacerbated by the innovative assessment tool of IPT in active asymptomatic collegiate athletes. One possible mechanism for this exacerbation was the temporary modulation of cerebral blood flow. However, since the IPT lasting for 30 s, hemodynamic and vasovagal responses cannot be methodologically associated with the results of this study.17,18 Nevertheless, IPT may induce rotatory vertigo or dizziness as the head position is changed relative to gravity in what can be characterized as possible vestibular sub-type concussion. The vestibular structures, which are surrounded by the temporal bone, can be vulnerable to forces exerted on the head.19,20 In case of vestibular dysfunction that occurs following traumatic brain injury objective signs of imbalance, dizziness symptom and migraine phenotype headache all have been suggested to interactively increase.21,22 Also, head trauma often provokes benign paroxysmal positional vertigo (BPPV), a condition in which otoconial debris floats freely within the endolymph of the semicircular canal. 23 However, the head position during the IPT, which did not include any side rotations, would not induce torsional nystagmus or BPPV. Dizziness, the second most common reported symptom next to a headache after SRC, can be caused by inner ear disorders following an SRC,9,20,24,25 and IPT has potential to exacerbate dizziness or other symptoms even after post-concussive symptoms subside.
A number of assessment tools for SRCs have been investigated intensively, including those that assess the extent of post-concussive symptoms and signs, anterograde and retrograde amnesia, objective balance systems, and neurocognition.26–32 All of the assessment tools currently in use, Balance Error Scoring System (BESS) and Standardized Assessment of Concussion (SAC) can detect differences in the scores of common post-concussive symptoms between preseason baseline and post-concussion tests of concussed athletes. From the standpoint of test-retest reliability regarding the preseason baseline and the first 24 h or 7 days post-injury assessment, however, the symptom checklist has been shown to constitute more sensitive measurement of concussive injury than either the BESS or the SAC in SCAT-3. 26 Thus, IPT may help to detect concussion symptoms that remain concealed owing to their unobtrusiveness on the checklist, or essentially identify athletes post-concussion who are not truly recovered.
A comprehensive, multifaceted diagnostic approach is necessary for treating SRCs.16,33 Recently the assessment method involving oculomotor function, known as the King-Devick test has been advocated to clinicians and researchers.34,35 Such highly empirical techniques as quantitative electroencephalography and functional neuroimaging or functional MRI have been further demonstrated to provide evidence useful in the diagnosis of SRCs. 36 Previous research has extensively demonstrated ways to diagnose the transient disturbance of brain function associated with SRCs using computerized neuropsychological batteries, such as Immediate Post-concussion Assessment and Cognitive Testing (ImPACT), that are compared with a preseason baseline. Post-concussive symptoms, however, especially headache affect the level of cognition, such as reaction time and memory composites during ImPACT or field retrograde amnesia tests during the SAC.16,20,37 Athletes with mental fogginess experience diminished reaction times as well.6,37 There are further reasons to conclude that BESS is not the most effective tool for assessing concussed athletes suffering from headaches. 7 A number of post-concussive symptoms may later be concealed when the quantitative diagnosis approach is used to make RTP decisions. This study suggests that any post-concussion symptoms should be dealt with before a comprehensive diagnosis approach is employed.
Although female athletes are more prone to suffering from SRC than male athletes, reported differences in the numbers of symptoms or their severity between the two gender groups at baseline can prove controversial.1,9,13,26 The IPT in this study induced symptoms in 7 male and 5 female soccer players, 33.3% of 22 and 31.4% of 16 respectively, which was more than in any other types of athletes. Five female soccer players were actually excluded from the analysis of baseline test results because they showed some symptoms before the IPT, though none displayed symptoms suggestive of concussion. The baseline symptoms have also been shown to vary depending on the number of previous concussions, in particular three or more, 38 and age or performance level, such as high school compared with NFL players.13,31 Moreover, nearly half of the collegiate athletes showed concussion-like symptoms without a history of concussion at baseline testing.9,39 Lastly, 17–46% of youth athletes are reported to suffer from such mood disorders as anxiety, depression, and irritability. 9 Taken together, these findings suggest that collegiate players may be prone to experience the induction of symptoms as a result of the IPT.
The IPT exacerbated symptoms in 16.2% of healthy non-concussed collegiate athletes (18/111) during the pre-participation examination, whereas it induced symptoms in 41.2% of those who were later diagnosed with SRCs (7/18) during the course of season. The chance of susceptibility to SRC less than 50% cannot be concluded at all. The mechanism by which symptoms are induced in IPT has not yet been clarified, but this is consistent with a previous study in which the control group was matched with the tested concussed athlete group to demonstrate that significantly fewer symptoms were detectable in baseline testing than in the concussed athlete group based on the Graded Symptom Checklist. 30 Concussion-like symptoms can occur in association with an individual's premorbid health history, such as psychiatric difficulties, learning disorders, migraines, and other types of headaches, and motivational variables. It is reasonable to assume that athletes who have prepared for an upcoming season are at a homogeneous fitness level, especially those in NCAA D1. This study excluded anyone with concussion-like symptoms before administration of the IPT, so it remains for further studies to assess whether IPT can be effective in identifying athletes whose concussion-like symptoms are exacerbated and therefore will be relatively susceptible to SRCs in their athletic activity.
The IPT exacerbated post-concussive symptoms, which subsided in 7 of the 18 concussed athletes. Next, concussed athletes were distinguished based on whether they reported post-concussive symptoms within 7 days after an SRC, and it was found that this approach had greater specificity in identifying correctly those who had not experienced post-concussive symptoms within this period than was the case of those who had (71.4% vs. 50% respectively). With regard to time to RTP, 64% of the student athletes who were diagnosed with RTP by 9 days after an SRC; specifically the median ranged between 7 and 9 days after a concussion for male student athletes and between 3 and 6 days for female athletes. 30 Therefore, the specificity, which, it has been argued, includes understanding the symptoms of SRCs, 15 might be increased in those with post-concussive symptoms that subsided earlier than usual through the instrument of IPT. It should be noted that no difference was found in post-concussive symptom recovery time between high school and collegiate athletes; thus the same injury management protocol is used for both aged groups once symptoms subside, 30 though the number of concussions that an athlete has endured in particular a history of more than three, calls for special injury management procedures. 27
Previous studies demonstrated that the modification of cerebral blood flow and metabolism can decrease the severity of symptoms after an SRC based on the graded treadmill test in connection with the Brog's rating of perceived exertion scale, regardless of an individual's physical conditions or age.40–42 The findings presented here suggests that IPT be performed in the earlier stages of the RTP protocol. The 5-day progression includes such activities as light aerobic exercise, sport-specific exercise, and non-contact training drills.40–42 Since IPT probably is not mediated by the autonomic nervous system, those whose post-concussive symptoms were exacerbated might use it in conjunction with the graded treadmill test to determine whether the symptoms can be diminished. The period of 2–7 days post-concussion should accordingly be defined as the acute phase. IPT may thus play a role in establishing that concussion-like symptoms at baseline testing are not false negatives.
The self-reporting of symptoms in this study was completed using the CSI with a 12-item questionnaire, one different from the 22-item symptom evaluation scales used in the SCAT and the ImPACT, questionnaires. The CSI for SRC has rarely been addressed in prospective studies, 8 but this inventory was empirically derived from three other different self-reported scales, namely the Concussion Prevention Initiative, the NCAA Concussion Study, and Project Sideline, by comparing samples of 641 concussed athletes with baseline samples of 16,350 non-concussed athletes. 43 The 12-symptom CSI questionnaire can be described as a cognitive-migraine-fatigue cluster. 27 The symptom cluster in this study indicated a significant interaction between time to recovery from post-concussive symptoms and the number of concussions. No other symptom clusters, such as the somatic and sleep clusters that are included in the SCAT and ImPACT, showed differences for these variables. 27 The inventory obtained through a 12-item questionnaire therefore appears adequate to assist with decisions regarding RTP after SRC.
Few if any single SRCs are associated with long term cognitive impairment. 43 Whether post-concussive symptoms reside or subside, the result can often create confusion for healthcare providers regarding such issues as malingering, exaggeration, or magnification for various individual factors may affect a patient's self-reporting including ‘stereotype threat’, ‘loss aversion’, and ‘cheating’. 43 Conversely, many concussed athletes desire to RTP as quickly as possible. 38 In either case, IPT may prove effective in assisting ATs and other medical professionals in assessing the outcome of symptom exacerbation and thus probable recovery in accordance with an RTP protocol.
Limitations
The sample for this study was limited to college student athletes from a few cohorts, a limitation that may not allow for generalization and to other age groups. Further this study did not compare the results of symptoms exacerbated by IPT with any of the common concussion assessment tools, such as ImPACT, which again may limit the validity of the findings. Thus, further future potential studies may compare IPT with other post-concussive testing including BESS, ImPACT, or the King-Devick test. Finally, because this research took the form of a field cohort study, the duration of symptoms that subsided varied among concussed athletes, and IPT was not performed during any of the subacute phases following an SRC, which represents a further potential limit to this study in terms of understanding the mechanisms involved in the subsiding of post-concussive symptom.
Conclusion
This study demonstrated that IPT could induce some of the 18 symptoms associated with SRCs. The list of symptoms included those of 41.7% of the concussed athletes whose post-symptoms subsided as well as 16.1% of the non-concussed athletes in the baseline test. The findings also showed that collegiate soccer players were more likely than other types of athletes to experience the induction of symptoms during IPT. The results of this study provide preliminary evidence that IPT may clarify the extent to which post-concussive symptoms have subsided or conversely which post-concussed athletes who may not be fully recovered. This is the first study to investigate the exacerbation of symptoms that had subsided in concussed athletes through IPT. Further studies are warranted to investigate the validity and reliability of this innovative instrument in respect to the psychometric properties of sensitivity and specificity.
Footnotes
Acknowledgements
The authors thank Scott Shawn, MS, ATC, Hisashi Imura, MA, ATC, Shawna Bryant-Hernandez, MEd, ATC, Laura Alexander, MA, ATC, Theresa Gethins, MA, ATC, Jessica Reinhart, MA, ATC, Courtney Beverine, MA, ATC, and Kristen Pagtulingan, MA, ATC for their assistance with data collection and reduction during this study.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
