Abstract
Objective
To identify and synthesise research evidence regarding psychometric properties and clinical utility of the Buffalo Concussion Treadmill Test (BCTT) and Buffalo Concussion Bike Test (BCBT) for use with patients with acute concussion, post-concussion syndrome (PCS) or physiological post-concussion disorder (PPCD).
Data sources
ProQuest (ProQuest Central), PEDro, Medline (Ovid), Emcare (Ovid), EBSCOhost (Health collection) and Google Scholar, searched September 8th-12th, 2020.
Study selection
Two authors independently selected studies that met eligibility criteria. Studies were selected if they were original research of any design, that investigated the properties of the testing protocols in either concussed or uninjured participants. Articles not published in English, that were not original research or that used significantly different testing protocols were excluded. The search yielded 250 articles, 11 of which were eligible and included in this review.
Data extraction
Included studies were critically appraised independently by two authors, using the Mixed Methods Appraisal Tool (MMAT). Data relating to study characteristics and key findings were extracted from the studies, documented in tables, and used to inform a critical narrative synthesis of findings.
Data synthesis
To provide recommendations relating to each aim of the review, a strength of evidence scoring system was used. Available evidence supported use of the BCTT, with strong evidence supporting the safety and construct validity of the test and moderate evidence supporting its prognostic value. There has been very limited research investigating use of the BCBT.
Conclusion
The findings support a recommendation for use of the BCTT in clinical settings for management of acute concussion, PCS and PPCD. There is limited evidence available for the BCBT. Additional studies are needed of both tests to further establish their clinical value.
Introduction
Concussion is a type of mild brain injury induced by biomechanical forces applied to the body, head or neck, with transmission of impulsive forces to the brain.1,2 Spontaneous recovery occurs in an estimated 70–90% of concussions,2–5 however a proportion of individuals will develop persistent symptoms – termed Post-Concussion Syndrome (PCS) if symptoms persist for longer than 14 days or Persistent Post-Concussion Syndrome (PPCS) if symptoms persist for longer than 3 months.6,7 A common and debilitating symptom of acute concussion, PCS and PPCS is exercise intolerance8–10 – the inability to exercise to one’s age-expected maximum heart rate without symptom exacerbation. Further classification of PCS and PPCS has been proposed and those with exercise intolerance may be classified as having Physiological Post-Concussion Disorder (PPCD). 11 In those with acute concussion, PCS, PPCS and PPCD, exertional testing has emerged as a tool for identifying exercise intolerance or provoking more subtle symptoms that are not obvious at rest.10,12–15 Additionally, exertional testing provides objective information and reduces the reliance on subjective symptom reporting, which can be unreliable, 16 with symptoms underreported. 17
The Buffalo Concussion Treadmill Test (BCTT) is a progressive exertional test that has been developed to support assessment and management of this population. More recently, the BCTT has been adapted to a cycle ergometry mode 18 to prevent potential symptom provocation from vestibular or cervicogenic origin. This can be accomplished by enabling the maintenance of a more stationary head/neck position than is possible when walking/running on a treadmill 19 ; this adapted version of the test is termed the Buffalo Concussion Bike Test (BCBT). 18
Linked with the evolving management of concussions, research surrounding the BCTT and BCBT has progressed rapidly. The BCTT was first implemented in people with persistent concussive symptoms and demonstrated it can be used to successfully identify symptoms, guide prescription of an exercise program and confirm recovery. 8 Research has continued to investigate similar applications, consistently showing positive value of the BCTT in both acute and persistent concussion.
One systematic review has been published investigating a range of testing modes and protocols for exertional testing amongst patients after mild traumatic brain injury. 20 However, the BCBT was not included in this review and the BCTT was not focal to the investigation. While primary research has produced information that could potentially contribute to assessment of the psychometric properties of the BCTT and BCBT and aspects of their clinical utility, no reviews have yet aimed to synthesise these findings systematically. No systematic review has been conducted to synthesise and evaluate the existing research literature on the BCTT and BCBT, specifically, and their use in management of concussion. There is therefore limited guidance and information available regarding application and value of these tests.
The purpose of this systematic review is to provide clinicians with clarity in relation to the application and value of the BCTT and BCBT for guiding management of acute concussion, PCS and PPCD in the clinical setting. With this in mind, the primary aim of this systematic review was to identify and synthesise research evidence regarding the BCTT and BCBT (or equivalent exertional testing protocols) and their use for patients with acute concussion, PCS or PPCD. Specifically, the review was designed to: (i) assess the psychometric properties of both tests in this population; (ii) investigate the safety, utility, feasibility and acceptability of both tests in the clinical setting; and (iii) generate clinical and research recommendations for the implementation of the BCTT and BCBT in the management of patients with either acute or persistent concussion, while considering the strength of available evidence.
Methods
Research design
This systematic review was registered with PROSPERO (ID number: CRD42020201173) on the 28th of August, 2020, and it’s design and reporting were informed by the PRISMA Statement. 21 Two changes were made from the research protocol registered with PROSPERO. Firstly, the MMAT was used to critically appraise included studies instead of the tool originally proposed because it allowed appraisal of a variety of study designs using a single tool. Secondly, a strength of evidence assessment was conducted to add further rigour to the assessment of the strength of the available evidence.
Data sources and search strategy
A literature search was conducted in the period September 8th-12th, 2020, using the following databases: ProQuest’s ProQuest Central collection, PEDro, Medline (via Ovid), Emcare (via Ovid) and EBSCOhost’s Health collection. An advanced Google Scholar search was also conducted. All databases were searched using the following search terms: (“Buffalo Concussion Treadmill Test” or BCTT or “exercise test*” or “exertional test*” or “aerobic test*” or “treadmill test*” or “buffalo concussion bike test” or “buffalo concussion cycle test” or “Balke protocol”) AND (concuss* or “sports-related concuss*” or SRC or “mild traumatic brain injur*” or “Mild tbi” or mtbi or “post-concussion syndrome” or PCS or “Post-concussion disorder” or PCD) NOT (“physical component summary”) NOT (“Physical component score”). No search limits were placed on the year of publication. The reference lists of all identified studies were also screened to identify any further eligible research.
Study selection and critical appraisal
Following completion of the search, citations of identified articles were imported into Endnote X9 software (Clarivate Analytics), where duplicates were removed. One author (AJ) then screened titles and abstracts of the remaining articles, and articles that were clearly ineligible for inclusion in the review were excluded in this process. Full-texts of the articles retained after screening were then assessed for eligibility by two authors (AJ & NR), independently, and disagreements were resolved by discussion and consensus, or mediated by the third author (RP) if consensus was not reached.
Articles were included if they: (i) were reports of original research using any type of study design; (ii) investigated the BCTT, BCBT or similar test protocol (as judged by the authors through careful comparison); and (iii) investigated the use of the test with either patients who had experienced a concussive event or uninjured participants, for purposes of investigating properties of the test Articles were excluded from this review if they: (i) were not published in English; (ii) were a literature review, protocol only, abstract only or not original research; or (iii) utilised a testing protocol or mode significantly different from the BCTT or BCBT. The results of the search, screening and selection of studies were recorded in a PRISMA flow diagram. 21
The methodological quality of all included studies was critically appraised using the Mixed Methods Appraisal Tool (MMAT), 22 by two authors (AJ & NR), independently. Any disagreements in quality appraisal findings were once again resolved by discussion and consensus between the two authors appraising the studies or mediated by the third author (RP). The MMAT has five criteria by which methodological quality is assessed, for each of the five categories of study designs it covers. 23 A scoring system was developed by the reviewers to grade the quality of evidence and to assist with data analysis and synthesis. Meeting 0-2/5 criteria would indicate low methodological quality, 3-4/5 criteria met would indicate moderate quality, and 5/5 would indicate high methodological quality. The appraisal findings were further detailed and highlighted pertinent limitations and strengths of each study, to inform the data synthesis.
Data extraction, analysis and synthesis
Data relating to study characteristics and key findings were systematically extracted from each of the included studies by one author (AJ), documented in tables, and used to inform a critical narrative synthesis of findings from the included studies. Only key findings clearly relevant to address the aims outlined for this review were extracted. For example, adverse responses to testing, to assess the safety of either test Meta-analysis was not conducted due to excessive heterogeneity across the included studies. Instead, a strength of evidence assessment was made for the key findings, as described below.
The strength and consistency of evidence across studies were explored in detail, and assessments of the overall strength of evidence were developed, with consideration of each research aim. To provide recommendations, a strength of evidence scoring system, 24 as adapted by Prowse et al., 25 was employed to indicate the strength of evidence available to address each aim of the review. Available evidence was assigned a strong, moderate, limited or “conflicting” strength of evidence categorisation. Strong evidence was indicated by consistent findings from 3 or more high quality studies. A moderate strength of evidence was indicated by consistent findings from 1–2 high quality studies or 1 high quality study and 1 or more low quality studies. Evidence was categorised as limited if it came from 1 or more low quality studies with consistent findings or only 1 study. If findings were inconsistent across studies, the evidence was considered conflicting regardless of the number of studies or their quality. If evidence was not available on a particular test property, strength of evidence was not considered in relation to that property, but the lack of evidence was discussed in the narrative synthesis.
Results
Study selection
The results of the search, screening and selection processes are depicted in Figure 1. A total of 250 articles were identified using the planned search strategy. Following the screening process, 11 articles were deemed to have met the study eligibility criteria and included in this review. Based on the study categories used by the MMAT, one of the included studies was a randomised controlled trial, 26 five were quantitative non-randomised studies (with four being case-control studies),10,15,18,27,28 and five were quantitative descriptive studies (case-series studies).8,12,29–31
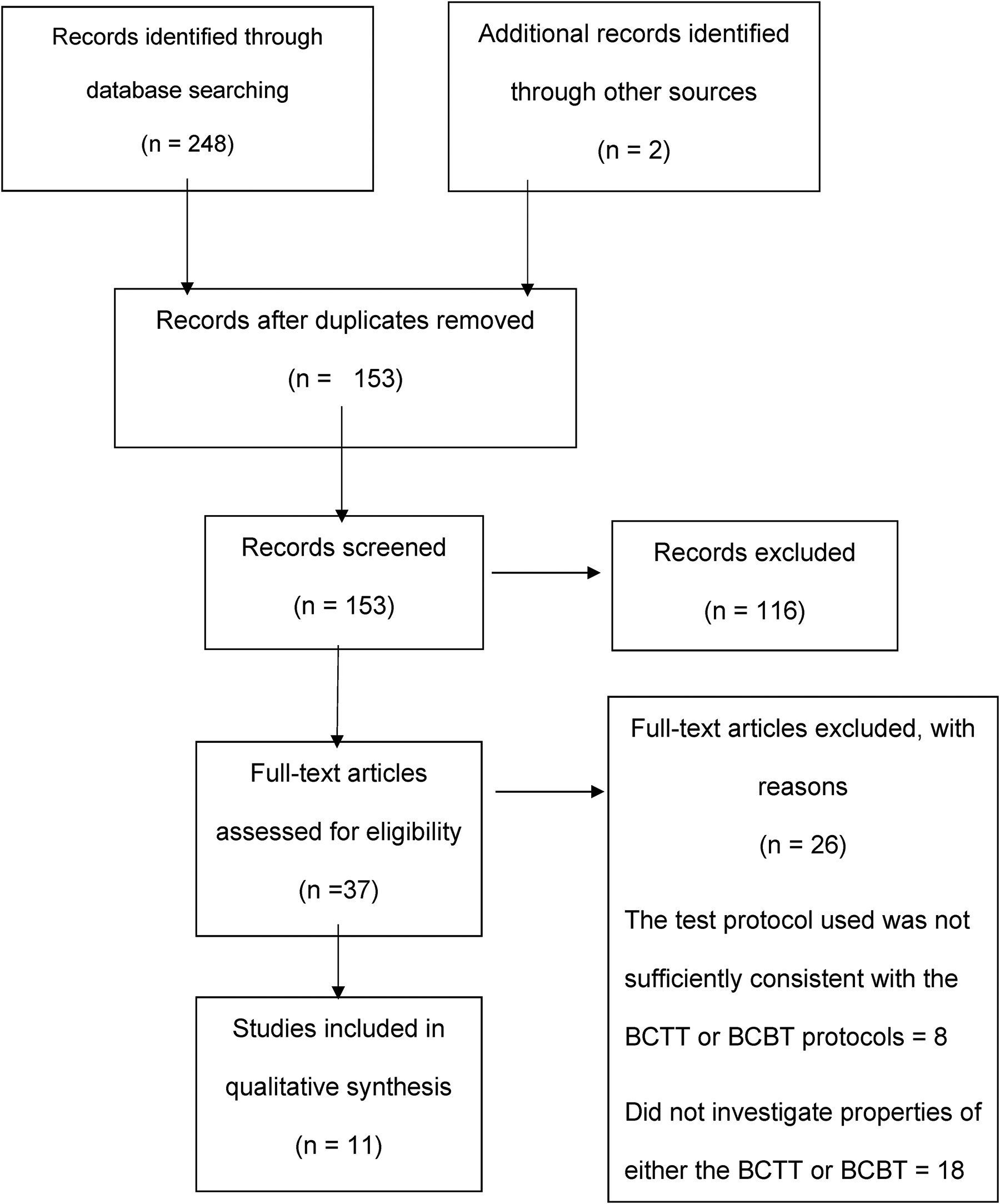
PRISMA flow diagram (Page et al., 2021).
Quality appraisal
The results of the appraisals of methodological quality are presented in Table 1. The one included randomised-controlled trial was determined to be of high methodological quality, scoring 5/5 on the MMAT. The average MMAT score of all five included quantitative non-randomised studies was 4.6/5, indicating moderate-to-high methodological quality. The average MMAT score of all five included quantitative descriptive studies was 4/5, indicating moderate methodological quality.
Critical appraisal (MMAT) results.
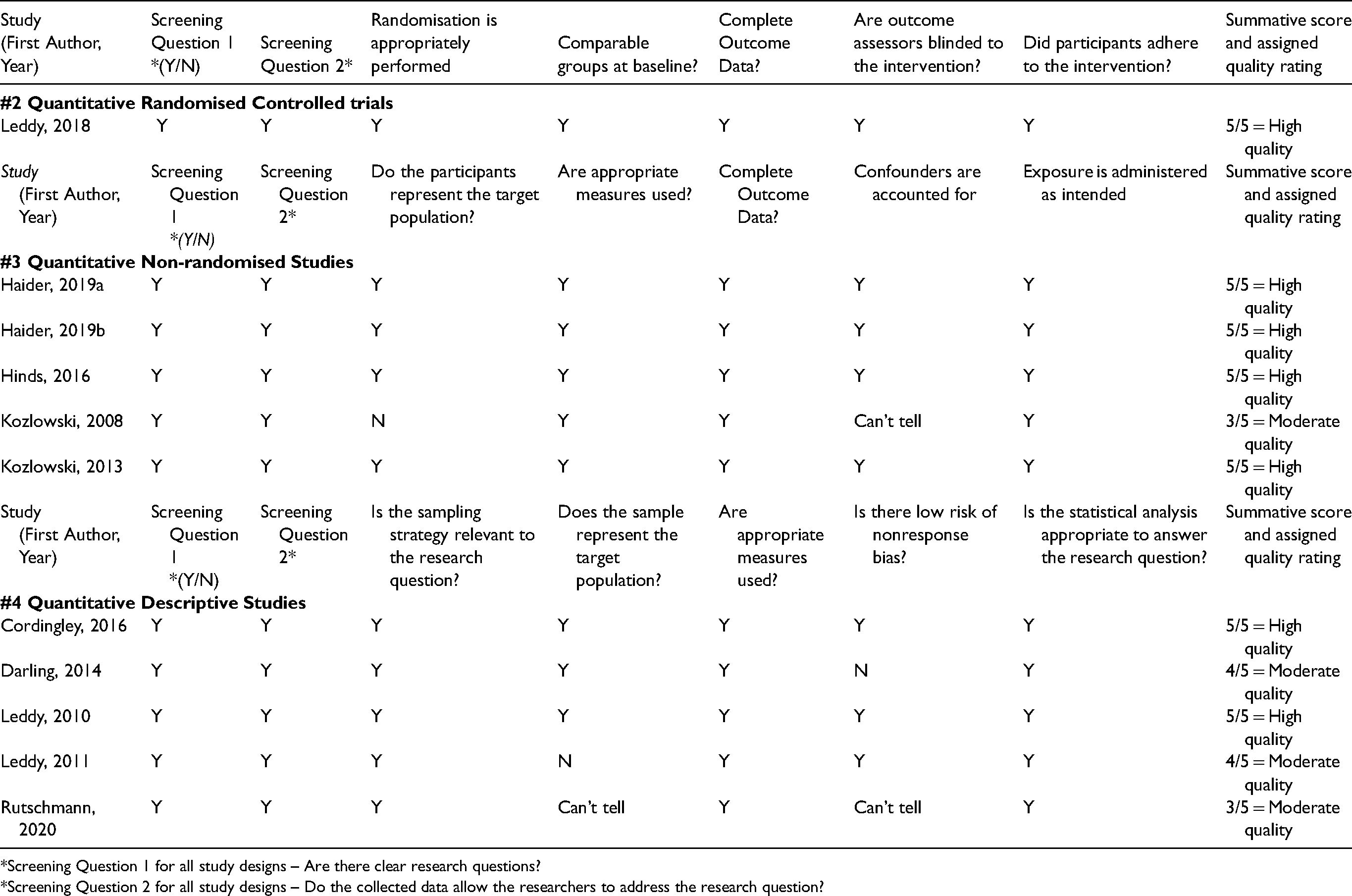
*Screening Question 1 for all study designs – Are there clear research questions?
*Screening Question 2 for all study designs – Do the collected data allow the researchers to address the research question?
Study characteristics
The characteristics of the included studies are presented in Table 2. Four of the included studies investigated use of the BCTT or BCBT with acutely concussed participants,18,26–28 with another four studies involving patients experiencing PCS,8,10,15,30 and three involving a mixed patient sample, including both acute concussion and PCS.12,29,31 Only one study investigated the BCBT. 18 None of the included studies investigated the use of either test solely with adults; six studies investigated use of the tests in adolescents12,18,26–29 and five included people of ages ranging from adolescence to older age (50 + years).8,10,15,30,31 The youngest participant across all studies was 11 years old and participated in the BCTT. 12
Study characteristics.
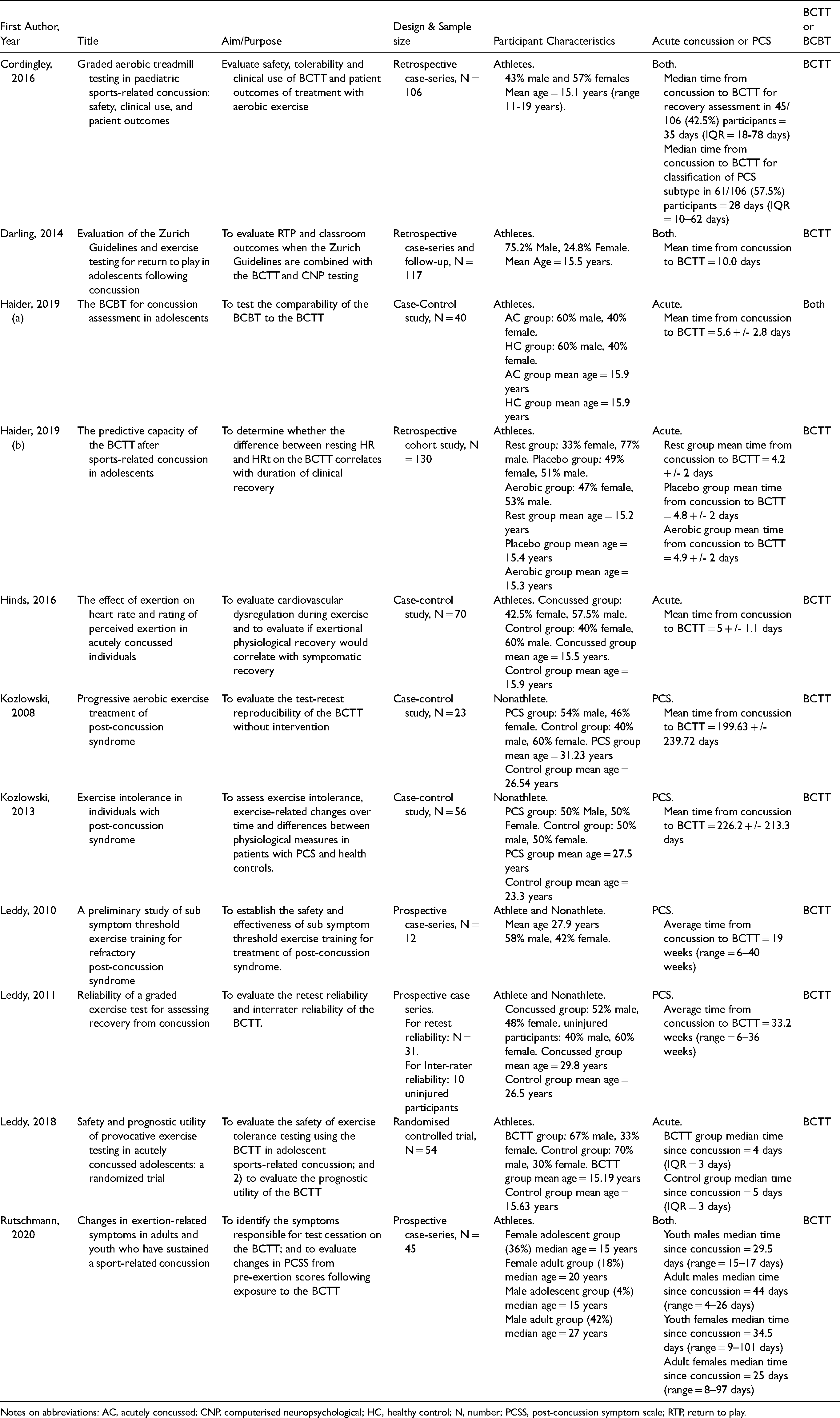
Notes on abbreviations: AC, acutely concussed; CNP, computerised neuropsychological; HC, healthy control; N, number; PCSS, post-concussion symptom scale; RTP, return to play.
Test reliability
The key findings from the included studies are presented in Table 3. Two studies were identified that examined the reliability of the BCTT in patients with PCS.15,30 Both investigated the test-retest reliability of the BCTT. In patients with PCS assessed using the BCTT, Kozlowski 15 found moderate but significant positive correlations between repeated tests in heart rates (HR) (R 2 = 0.647, p = 0.008) and in ratings of perceived exertion (RPE) (R2 = 0.558, p = 0.024) that corresponded with symptom exacerbation. However, information provided on study methods by Kozlowski 15 was deemed insufficient to allow determination of whether potential confounding factors were adequately controlled or accounted for, and the small sample size was also of concern. Similarly, Leddy et al. 30 demonstrated a moderate level of agreement between repeated tests only for heart rates (HR) corresponding with symptom exacerbation (ICC = 0.79, 95% CI, 0.55–0.91).
Key findings.
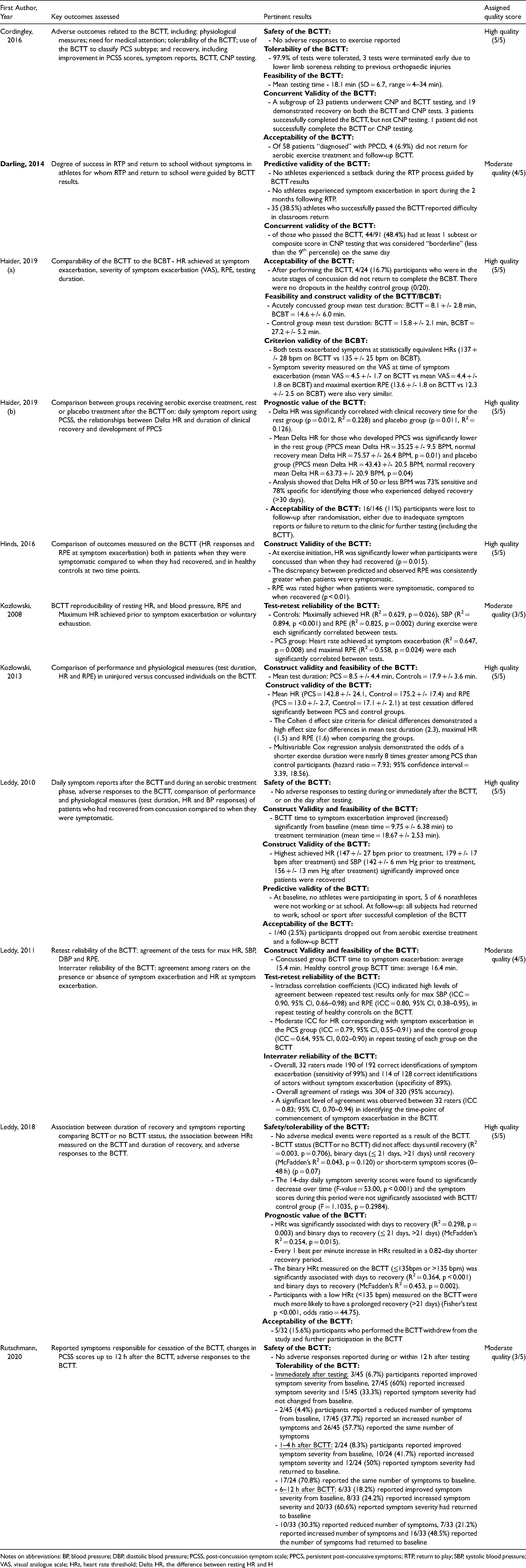
Notes on abbreviations: BP, blood pressure; DBP, diastolic blood pressure; PCSS, post-concussion symptom scale; PPCS, persistent post-concussive symptoms; RTP, return to play; SBP, systolic blood pressure; VAS, visual analogue scale; HRt, heart rate threshold; Delta HR, the difference between resting HR and H
The study by Leddy et al. 30 also investigated inter-rater reliability of the BCTT. The study found a good level of agreement between 32 raters (intraclass correlation coefficient (ICC) = 0.83; 95% CI, 0.70–0.94) in identifying the time-point of commencement of symptom exacerbation in the BCTT. 30 However, a sample of actors portraying patients with PCS was used, and the raters were also not able to interact with the participants.
Test validity
Four studies examined the extent to which the BCTT actually assesses the primary construct it was designed to assess - exercise tolerance/intolerance8,10,18,30 (Table 3). All of the four studies supported the construct validity of the BCTT, by demonstrating reductions in exercise duration achieved in the BCTT in either acutely concussed patients 18 or patients with PCS.8,10,30 In each population, exercise tolerance or duration was limited by symptom onset and significantly more limited in participants with acute concussion or PCS than in healthy controls or the concussed patients themselves once recovered. For example, Leddy et al. 8 found that exercise duration on the BCTT significantly improved in participants that had recovered from PCS (mean time = 18.67 + /- 2.53 min), when compared to those same participants at baseline testing (mean time = 9.75 + /- 6.38 min). Both Leddy et al. and Kozlowski et al. 10 found that participants with PCS had shorter testing durations on the BCTT, when compared to healthy controls. Similarly, Haider et al. 18 demonstrated differences in testing duration between acutely concussed participants (mean time = 8.1 + /- 2.8 min) and healthy controls (15.8 + /- 2.1 min).
Three other studies investigated the construct validity of the BCTT by examining RPE and HR responses to exertion during the BCTT.8,10,28 Firstly, Kozlowski et al. 10 demonstrated that the highest achieved HR prior to test cessation on the BCTT was lower in patients with PCS than in healthy controls and this HR in patients with PCS corresponded with a lower reported RPE. Leddy et al. 8 did not investigate RPE responses on the BCTT, but demonstrated lower peak HR on the BCTT in individuals with PCS whilst symptomatic compared to when they had recovered. Hinds et al. 28 examined the response to the BCTT in acutely concussed participants over the first nine minutes of the test, finding that the HR at exercise initiation was significantly lower when participants were symptomatic compared to when they had recovered. Hinds et al. 28 found that the average HR during the test was lower when participants were symptomatic, however this finding was not statistically significant. In contrast to Kozlowski et al., 10 Hinds et al. 28 also found that RPE scores were higher for comparable levels of work when participants were symptomatic compared to when they had recovered. From the available evidence, it appears the HR and RPE responses to exercise on the BCTT differ in individuals who are exercise intolerant after a concussion or those suffering from PCS. It is not clear however, if the RPE responses are exacerbated due to increased levels of perceived difficulty or dampened due to an inability to complete a greater workload.
With regard to the criterion validity of the BCBT, Haider et al. 18 investigated the comparability of results from the BCBT to those from the BCTT. Both tests found concussion symptoms were exacerbated at an equivalent heart rate and they also yielded very similar results for symptom severity and maximal RPE achieved at time of symptom provocation. No other studies were identified that compared outcomes of interest from either the BCTT or the BCBT, to equivalent outcomes from another exercise tolerance test
Two studies examined the prognostic value of the BCTT, as another indicator of test validity.26,27 Both studies demonstrated significant correlations between HR measures at point of symptom provocation in the BCTT and subsequent recovery periods in adolescent participants first tested in the acute stages of concussion. Leddy et al. 26 found that a heart rate threshold (HRt) (the average heart rate over the final minute of the BCTT) of less than 135 beats per minute (BPM) was significantly associated with recovery requiring more than 21 days. Haider et al. 27 found that a Delta HR (the difference between resting HR and HRt) of less than 50 BPM was both sensitive (sensitivity 73%) and specific (specificity 78%) for early identification of those at risk of delayed recovery (defined as more than 30 days). However, statistical analysis in that study was not possible in the group treated with aerobic exercise, as only 2 participants developed PCS. Therefore, the findings were only applicable to those who received rest or placebo treatment.
Two studies investigated whether the ability to exercise to maximum volitional exhaustion on the BCTT confirmed readiness to return to school, work and sport.8,29 In the study conducted by Leddy et al., 8 all participants achieved this test outcome and had made successful returns to school, work and/or sport at 3-month follow-up. After a minimum follow-up period of 2 months, Darling et al. 29 found that no athletes experienced symptom exacerbation in sport if recovery had been confirmed on the BCTT. However, in both studies participants were held back from athletic activities until they had successfully completed the BCTT and so no comparisons of outcomes were made with individuals who had not passed the BCTT. Nevertheless, 35 (38.5%) of the athletes for whom recovery was confirmed on the BCTT reported new difficulties in classroom return. It should be considered, however, that the small sample size used by Leddy et al. 8 is of concern and Darling et al. 29 was deemed to be at risk of non-response bias.
Clinical utility
Safety and adverse events
No studies were identified that reported on the safety of the BCBT. Reports of adverse events experienced during the BCTT were documented in four studies.8,12,26,31 None of those studies reported any adverse events associated with performing the BCTT. The participants in these studies varied in clinical presentation (acute concussion and PCS) and age, with the youngest participant reported as being 11 years old. 12 Leddy et al. 26 was the only study to report solely on acutely concussed participants and the only study to report on participants who were tested within 7 days of the concussion event; the study included participants as early as 1-day post-injury (median = 4 days, interquartile range (IQR) = 3). The largest study that reported on adverse events involved 106 participants 12 and so the power of these studies to detect safety concerns, and particularly any that might occur infrequently, was limited.
Two studies investigated the impact of the BCTT on symptom severity for periods after test cessation. Rutschmann et al. 31 found immediate increases in symptom severity and number of symptoms, whereas Leddy et al. 26 found no impact on symptom severity within 48 h of testing. However, in the study of Rutschmann et al., a majority of the symptoms reported improved to baseline within 6–12 h after testing.
Feasibility, acceptability and tolerability
No studies were identified that specifically aimed to assess the feasibility of the BCTT or BCBT. However, five studies were included that may contribute useful information regarding the time needed to complete the BCTT.8,10,12,18,30 For patients with symptom-limited exercise capacity, test duration varied from a mean of 8.1 min, 18 to an average of 15.4 min. 30
No studies were identified that specifically aimed to assess the acceptability of the BCBT or BCTT. One study reported on tolerability of the BCTT and found that 3 out of 141 tests were terminated early due to lower limb soreness relating to previous orthopaedic injuries. 12 No specific investigations were undertaken by any study on attrition rates after the BCTT or BCBT. However, five studies provided brief reports of participants who performed the BCTT and then withdrew from either repeating the BCTT8,12,26,27 or subsequently performing the BCBT. 18
Strength of evidence
The strengths of evidence relating to specific BCTT and BCBT properties are presented in Table 4. These gradings of strength of evidence24,25 indicate the strength of evidence available to address each aim of the review and are further described in the Methods. Strong levels of evidence were found in relation to assessments of safety of the BCTT when it was conducted more than 7 days post-concussion, and in relation to the construct validity of time to symptom exacerbation on the BCTT, as a means of assessing levels of exercise tolerance or intolerance. Moderate levels of evidence existed in relation to the prognostic value of the BCTT and the construct validity of the measures of RPE and HR responses to exercise on the BCTT, which have been found to differ between concussed and healthy participants. The available evidence was limited in relation to inter-rater reliability and test-retest reliability of the BCTT, criterion validity of the BCBT when compared to the BCTT, safety of the BCTT within 7 days of concussion, and in relation to the construct validity of testing duration to symptom exacerbation on the BCBT, as a means of assessing levels of exercise tolerance or intolerance. Conflicting evidence was found regarding the impact of the BCTT on short-term symptom severity, and the extent to which exercise tolerance assessed using the BCTT is indicative of readiness for return to school, work, and sport.
Strength of evidence.

Discussion
This review aimed primarily to identify and synthesise evidence on the properties and utility of the BCTT and BCBT and their use in acute concussion, PCS and PPCD. The secondary aim of this review was to use the available evidence to generate clinical and research recommendations for the BCTT and BCBT. This is the first systematic review to investigate the properties and utility of the BCTT or BCBT. Overall, the findings of this review indicate the BCTT is safe and well tolerated, that it has utility in assessment of exercise tolerance following concussion, and that it possesses construct validity and prognostic value. However, much less evidence is available regarding the BCBT and the reliability, feasibility, and acceptability of the BCTT.
The evidence that is available on BCTT properties tend to support its clinical value, and in particular indicates the BCTT is safe to conduct for patients with PCS and is a valid measure of exercise tolerance/intolerance, while probably also having good prognostic value (Table 4). However at present, there is generally not sufficient evidence to draw strong conclusions regarding other properties of the BCTT. In another systematic review, 20 the authors stated that there is little research to support the validity and reliability of any exertional testing protocol. Although the BCTT appears to be the most researched and consistently used test, the findings of this review are mostly in agreement with the findings reported by Quatman-Yates et al., 20 though with the exceptions noted above for safety, validity as a measure of exercise tolerance, and prognostic value.
The research investigating the reliability of the BCTT is quite limited. For test-retest reliability of the BCTT, the available evidence suggests that the HR achieved at time of symptom exacerbation in PCS patients is the most reliable measurement to use in the clinical setting. This is reassuring given the importance of measuring the HR at symptom exacerbation, as it is used in practice to prescribe progressive sub-symptom aerobic exercise.8,12,32–34 The findings also suggest that RPE and SBP could be further reliable measures in the BCTT, however the findings for these were generally less consistent and statistically significant than those for measures of HR.
It is nevertheless recommended that clinicians remain cautious when interpreting measures taken on the BCTT, as the reliability of measures taken during the test is yet to be established.
The construct validity of time to symptom exacerbation on the BCTT, as a means of assessing exercise tolerance or intolerance, was consistently demonstrated in included studies. This measure on the BCTT was able to differentiate healthy individuals from those who had experienced concussion. Although the validity of this construct is well evidenced, the interpretation of the BCTT results should not be based solely on time to symptom provocation. Exertional testing has been shown to produce symptoms similar to those experienced post-concussion in apparently healthy individuals30,35 and the rate at which this occurs on the BCTT is not well understood. To strengthen the clinician’s confidence in BCTT results, other objective data must also be considered. The construct validity of measures taken during the BCTT was also supported by three studies that found altered HR and RPE responses to the BCTT, as further measures of exercise intolerance.
HR measurements on the BCTT also had prognostic value in acutely concussed patients. Both studies demonstrate that HR measured on the BCTT provides prognostic information, however, the Delta HR may be more clinically useful. It is recommended clinicians consider the Delta HR when interpreting results from the BCTT, as this may better identify those who are at risk of prolonged recovery and indicate a need for early intervention. Further research should aim to replicate the findings regarding use of the Delta HR, with larger sample sizes. Due to the limitations of the participant sample and statistical analysis in the study by Haider et al., the results were only confirmed for those patients who received rest and placebo treatment and could not be confirmed for those who received aerobic exercise treatment. Future research should also ascertain if the Delta HR predicts development of PCS independent of intervention type.
The BCTT may also have prognostic value. However, there were only two studies available that examined this property and the results of the critical appraisal of those studies should also be considered.8,29 After successful completion of the BCTT, there was no evidence that participants had difficulty with return to sport or return to work.8,29 The study by Darling et al. 29 found more conflicting results for successful return to school. However, due to the design of those studies, no comparison can be made between those who were deemed to have recovered and those who were not.
A concussion has the potential to affect numerous brain regions and neurological functions, so a patient will seldom present with an isolated deficit.14,36,37 Therefore, one test is unlikely to be sufficient to determine recovery for all patients and the BCTT should be reserved for determining recovery from exercise intolerance and readiness for return to physical activities. It may also be hypothesised that the BCTT has limited value for assessing readiness for return to school.
Noting the available evidence, it is not recommended to use the BCTT in isolation for decision-making regarding readiness for return to sport, work or school. For return to play decisions in the clinical setting, it is recommended to combine the BCTT with the Zurich guidelines return to sport strategy, 2 and other clinically relevant tests. Larger cohort or case-control studies are recommended to further investigate the predictive validity of the BCTT, as this test property could prove to be clinically valuable in determining safe and successful return to activities. Further research comparing the BCTT to other testing protocols is also recommended. Comparing the BCTT to the Bruce testing protocol may provide valuable information on properties of the test such as; criterion validity, acceptability and safety. The Bruce protocol consists of a less conservative intensity progression that lasts for 3-min stages as compared to 1-min on the BCTT. 38
For any assessment tool to be clinically valued, research must not only investigate its psychometric properties, but also its utility when applied. The feasibility, acceptability and safety of the test are important factors to consider before implementing the BCTT in the clinical setting. There was no evidence specifically investigating the feasibility or acceptability of the BCTT, and there was limited evidence provided by the included studies for the safety of the BCTT within the first week of concussion.
The research on the safety of the BCTT was considered in respect to both the time since concussion and the age of the participants. There was conflicting evidence found in the included studies for the impact of the BCTT on short-term symptom severity. Dematteo et al. 39 has also examined symptom severity after exertional testing on a stationary bike and found that symptom severity improved immediately after testing (at 5- and 30-min) and 24 h after testing. Further research is recommended to investigate the changes in symptom severity that occur after performing the BCTT, particularly within the first 24 h.
The one study that investigated the safety of the BCTT within seven days of a concussion 26 was deemed to have high methodological quality and its findings were supportive of the safety of the BCTT. It is difficult to extrapolate findings regarding patient responses on other exertional tests to use of the BCTT in the acute stages of concussion, as much of the literature has investigated participants in the sub-acute and chronic phases of concussion. 20
More evidence was available regarding the safety of implementation of the BCTT after a seven-day period following a concussion8,12,31 and the findings consistently demonstrated no adverse responses to testing. It can therefore be concluded that the BCTT is safe to implement after a seven-day period. Further research into the safety of implementing the BCTT within the first few days after a concussion is recommended.
Multiple studies reported on the time taken to complete the BCTT.8,10,12,18,30 Patients will commonly present with a range of concussive symptoms.14,36,37 The BCTT is therefore unlikely to be the only test used during an assessment, so testing times are an important factor to consider when examining the applicability of the BCTT to the clinical setting. With this in mind, the reports given on the time taken to complete the BCTT may limit its feasibility. Dependent on the degree or presence of exercise intolerance, the BCTT could take as long as 18 min to complete. 8
Further studies are recommended to investigate a variety of aspects relating to the feasibility of the BCTT. Important factors to further consider may be the time taken, the equipment required, the cost, and the perceived ease of implementing the BCTT for clinicians of different professions and levels of expertise.
It is expected that exertional testing will temporarily exacerbate concussive symptoms, but this symptom increase is generally expected to return to, or below baseline within 24 h.26,31,39 Fear avoidance has been reported in those suffering from PPCD,40,41 and exercise testing that exacerbates symptoms may therefore incur high attrition rates and affect adherence to further treatment. Further research is recommended to investigate the attrition rate of participants after completing the BCTT, and this may also be compared with that for those attempting other testing protocols (e.g., the Bruce protocol). 38
One important finding of the review was the limited evidence found on protocols consistent with the BCBT, despite the potential for it to be a valuable clinical tool. The results reported by Haider et al. 18 suggest the BCBT is comparable to the BCTT and are supportive of the construct validity of time to symptom exacerbation on the BCBT, as a means of assessing exercise tolerance/intolerance.
Other research has been conducted with concussed patients using different protocols on a stationary bike.14,42 These studies appear to have found the stationary bike useful in the assessment and management of patients experiencing concussion symptoms. Vestibular impairment resulting in dizziness and balance dysfunction has been reported as a common symptom following concussion and head injury.36,43 As a result, head movements associated with walking on a treadmill may produce false-positive symptom reports in the BCTT that are not due to true exercise intolerance, and so the stationary bike may be a valuable alternative, since it may better enable maintenance of head stability.
The available evidence does not provide sufficient information to establish the properties or value of the BCBT in clinical assessments. Based on the findings of this review, it is not yet recommended to use the BCBT in place of the BCTT unless head stability is deemed imperative, or other limitations (e.g., lower limb injuries limiting mobility) are present.
Limitations
The strength of conclusions drawn from this review is somewhat limited due to the small number of eligible studies. Due to the anticipated heterogeneity of the research, a broad search strategy was used and thus research that investigated the tests and their use for multiple purposes were included. Consistency and comparison of findings across studies was limited for this reason and this may also limit the strength of conclusions. Non-English articles were excluded as per the selection criteria, so language bias is also possible.
Conclusion
The results of this review indicate that the BCTT appears to be safe, though there was conflicting evidence regarding whether it might temporarily increase symptoms for 6–12 h post-testing. There was strong evidence to support the construct validity of measures used in this test. Additionally, the BCTT may have good prognostic value in the early assessment of acutely concussed patients. Although there was limited evidence for some of the properties of the BCTT, the test is recommended for clinicians to use in the assessment of exercise tolerance/intolerance in individuals suffering from acute concussion, PCS or PPCD. It is recommended that further research investigate properties of the BCTT by comparisons to other testing protocols. There is very limited research available on the BCBT, however it may be useful for the clinical assessment of patients suffering from concussion symptoms, particularly where symptoms of vestibular origin are present. Further research is recommended to establish the validity, reliability, and application of the BCBT.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article
