Abstract
Objectives
To compare dual-task performance involving different cognitive-locomotor combinations between healthy controls and participants with sub-acute mild traumatic brain injury (mTBI) and to correlate dual-task performances to history of prior head injuries.
Methods
Eighteen participants having recently sustained mTBI and 15 controls performed nine dual-tasks combining locomotor (level-walking, narrow obstacle, deep obstacle) and cognitive (Stroop task, Verbal fluency, Counting backwards) tasks. Previous history of concussion was also investigated.
Results
Slower gait speeds were observed in the mTBI group compared to controls during both single and dual-tasks. Longer response times to cognitive tasks in the mTBI group further suggested the presence of residual impairments two months following injury. No combination of dual-task was more sensitive. Correlations were observed between history of mTBI and several measures of dual-task performance, underlying the need to further consider the effects of multiple injuries in relation to dual-task walking.
Conclusion
Dual-tasks using simultaneously locomotor and cognitive functions represent an ecological way for clinicians to detect residual, but subtle, alterations post-mTBI. History of previous mTBI needs to be considered as a personal characteristic which may influence dual-task walking performance.
Introduction
Mild traumatic brain injury (mTBI) can lead to different physical and cognitive symptoms that vary greatly and resolve at different rates across individuals. 1 Dynamic balance can take up to 30 days to normalize after mTBI, 2 and it has even been shown that long-term self-reported balance problems can persist up to four years post-mTBI. 3 Cognitive deficits can also persist up to several months or even years. 4
In most protocols assessing function after mTBI, physical and cognitive dimensions are usually evaluated separately and may not capture one’s performance in more complex daily situations where these dimensions are combined. Dual-task walking (DTW) protocols which combine locomotor and cognitive tasks (e.g. walking while performing an arithmetic task), have been recently proposed to more closely mimic daily life demands where locomotor and cognitive functions are often solicited simultaneously.5–7 Indeed, DTW induces an increased cognitive load, particularly on executive functions and attention, resulting in central resource competition that may affect performance on one or both tasks.8–10 Including such protocols in an assessment may prove useful to inform return-to-function decisions following mTBI.
A recent review of the literature suggested that DTW protocols show promise to detect gait abnormalities after the acute period of concussion. 11 In studies combining level walking and cognitive tasks such as spelling words, reciting months, or counting backwards, gait speed has been found to be significantly slower after mTBI up to six days post-injury.12–14 Only three studies have investigated DTW performance in the months and years post-mTBI in adults.6,15,16 These studies also found significantly slower gait speed in participants with mTBI compared to healthy controls, using either level-walking or walking over obstacles during dual-tasks. In studies evaluating obstacle crossing, individuals with mTBI show slower gait speed, more contacts with obstacles, greater clearance variability and less time in single-leg stance.6,16,17
Only a small number of studies have investigated dual-task cost (DTC) in DTW paradigms, which represents the decrease in performance compared to single-task performance for a given variable. Cossette et al. 6 found that DTC for gait speed was higher in the mTBI group, which was on average 158 days post-injury. Fait et al. 18 observed a greater DTC in elite athletes one month post-concussion for response time to a visual Stroop task during obstacle circumvention. Fino 15 also found that athletes with mTBI had higher DTC for dynamic stability.
While there is increased interest in DTW following mTBI, it remains unclear what combination of locomotor and cognitive tasks might be sensitive enough to capture potential residual, subtle deficits following an mTBI. Furthermore, little research has explored DTW performance beyond the acute period. Finally, in their recent systematic review, Fino et al. 11 have identified a clear need for further research on complex gait, such as obstacle avoidance with dual tasks, particularly in the subacute and intermediate phases following injury.
In addition, multiple mTBIs are also a major concern for young adults, particularly in sports-related contexts, but the effects on DTW performance are not clear. Some studies suggest that multiple injuries may increase the number of symptoms and length of recovery after a concussion, 19 and may also diminish executive functioning, 20 or result in conservative gait patterns. 21 Therefore, multiple mTBIs might be expected to also influence DTW performance. However, to our knowledge, only two studies have explored the relationship between mTBI history and DTW performance. Martini et al. 16 found correlations between number of mTBIs and percent time spent in single and double-leg support during gait, both in single and DTWs conditions, suggesting an increased need of balance support. Howell et al. 22 found smaller strides during DTW in participants with a history of two or more mTBIs compared to a control group, suggesting a more conservative gait.
Given the call for further research on DTW performance using more complex gait situations, 11 and the limited research related to the sub-acute phase, along with the continuing uncertainty about the effects of past mTBIs on DTW, the present study had two goals. First, to compare performance on cognitive and complex gait parameters using different DTW conditions between healthy controls and young adults with mTBI 3 to 15 weeks post-injury. We expected a slower gait speed and greater motor DTC in the mTBI group for obstacle avoidance. Second, to explore the relationship between the number of prior head injuries and DTW performance in the mTBI group. We expected the number of prior injuries to be correlated to gait speed and to DTC on locomotor and cognitive parameters.
Methods
Thirty-three individuals aged 16 to 30 years participated in the study. Participants in the mTBI group (n = 18) had received a diagnosis of mTBI from a health professional. We further verified that all injured participants corresponded to the World Health Organization’s mTBI definition. 23 Participants were recruited 3 to 15 weeks post-injury. The control group included 15 healthy individuals who reported no history of diagnosed mTBI. Exclusion criteria for both groups were: self-reported substance abuse, other neurological, musculoskeletal, balance or cognitive problems, previous moderate or severe TBI, and use of medications known to interfere with locomotion or cognition. The study was approved by the Ethics Review Board of the Centre Intégré Universitaire de Santé et de Services Sociaux de la Capitale Nationale and informed written consent was obtained for each participant.
Experimental procedure
Recruited participants were assessed for previous head injuries, symptoms, visual acuity and physiological and neuropsychological ability (see below). A separate session involved gait analysis with 3D motion analysis (Vicon Motion Systems Ltd, Oxford, UK) using four triads of reflective markers placed on the head, trunk and feet. Participants were asked to walk a 6-m straight-walkway during different combinations of locomotor and cognitive conditions. Three locomotor conditions (level-walking; stepping over a narrow obstacle – 15 cm high × 3 cm deep; stepping over a deep obstacle – 15 cm high × 15 cm deep) were combined with one of four cognitive conditions (no concurrent cognitive task; Stroop task – naming the incongruent ink colours of eight words repeating “green” “blue” and “red” projected at the end of the walkway; Verbal Fluency – producing different words beginning with a specific letter; Arithmetic task – counting backwards by 2 s). Each condition was completed four times, for a total of 48 randomized trials divided into three blocks corresponding to locomotor conditions. Different stimuli were used for each cognitive trial to avoid learning effects. Participants were instructed to walk at a natural pace while performing the cognitive task as fast and accurately as possible. Cognitive tasks were performed as single tasks while sitting at the beginning and at the end of the experiment.
Measures
The Ohio State University Traumatic Brain Injury Identification Method (OSU TBI-ID) 24 was used to identify prior head injuries. This questionnaire reviews history of impacts to the head, including diagnosed or possible mTBIs.
Self-reported symptoms experienced in the last 24 h were assessed with a French version of the Rivermead Post-Concussion Symptoms Questionnaire (RPQ). Severity of 12 symptoms was rated from 0 (never felt/no change from pre-injury) to 3 (severe problem).
Neuropsychological tests were administered to characterize executive functioning, attention, processing speed, verbal skills and working memory. These included four subtests of the D-KEFS’s, the Wechsler Memory Scale’s forward and backward Digit Span, the Brown-Peterson’s Auditory Consonant Trigrams and the WAIS-IV vocabulary subtest.
Physiological measures included grip strength using a dynamometer, balance and upper limb coordination using subtests of the SCAT3, 25 postural stability (balance error scoring system; BESS) and natural and fast walking velocity over 10 m.
During experimentation, average gait speed was calculated from the forward velocity of the trunk over the walkway. Gait fluidity (acceleration/deceleration) was calculated as the number of zero crossings of the anterior–posterior trunk acceleration. Obstacle clearance was measured as the height of the lead toe over the obstacle. Locomotor variables were averaged over trials of the same combinations. DTC for gait speed and fluidity was obtained by calculating the difference between DTW and single-task performances as a percentage of the single-task performance.
Cognitive performance measures included response time (time between presentation of stimulus and first response or total walking time in the case of no responses), answers/time ratio (total number of responses divided by the duration of the trial), DTC for answers/time ratio (percent difference between answers/time ratio during DTW and during the cognitive single-task, divided by the single-task performance), and number of errors.
Statistical analyses
For statistical analyses (SPSS, IBM, New York, USA, v.23), group characteristics were compared using t-tests. Repeated measures ANOVAs were used to analyse gait speed and fluidity (2 groups × 3 locomotor conditions × 4 cognitive conditions), obstacle clearance including only the two obstacle conditions (2 × 2×4), and cognitive variables including only the three cognitive conditions (2 × 3×3). Only group effects and interactions were examined. In case of significance (p ≤ 0.05), post hoc analyses were conducted. In the case of a significant Box test evaluating homogeneity of variance between groups, Levene’s test results were used. A Huynh-Feldt correction was applied when the Mauchly test for within-group homogeneity was significant.
For the second objective, for the mTBI group, Pearson’s correlations were computed between number of prior head injuries, including the current one, and gait speed, DTC for gait speed, response time, answers/time ratios and DTC for answers/time ratio. Considering the exploratory nature of this objective, no statistical correction was made. However, to reduce number of comparisons, statistical analyses were only conducted on DTW combined by cognitive task, regardless of locomotor conditions.
Results
No significant differences between groups were found for age, height, sex or education (Table 1). The mTBI group reported significantly (p = 0.030) more symptoms (M = 4 ± 3.73) than controls (M = 1.80 ± 1.37), with greater severity (p = 0.028). Participants were 26 to 110 days post-injury at data collection (M = 59.56 ± 24.12 days, mdn = 59). No significant differences between groups were found on standardized neuropsychological tests (Table 2; p > 0.05).
Participant characteristics.
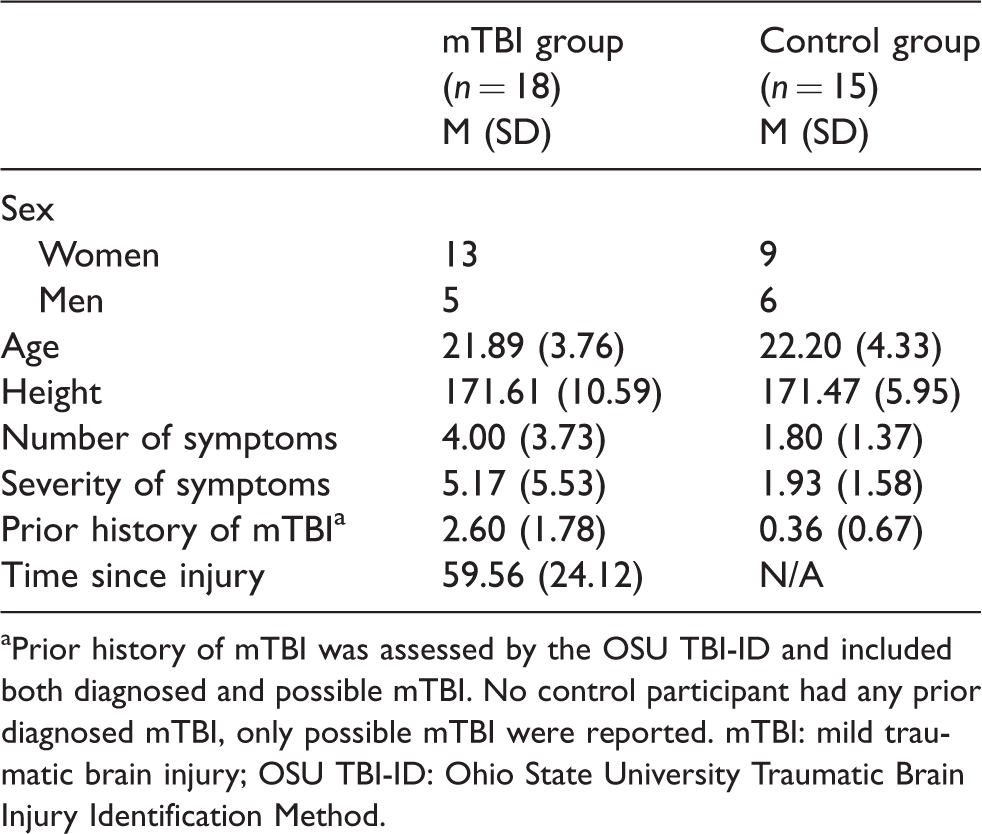
aPrior history of mTBI was assessed by the OSU TBI-ID and included both diagnosed and possible mTBI. No control participant had any prior diagnosed mTBI, only possible mTBI were reported. mTBI: mild traumatic brain injury; OSU TBI-ID: Ohio State University Traumatic Brain Injury Identification Method.
Results of neuropsychological assessment.
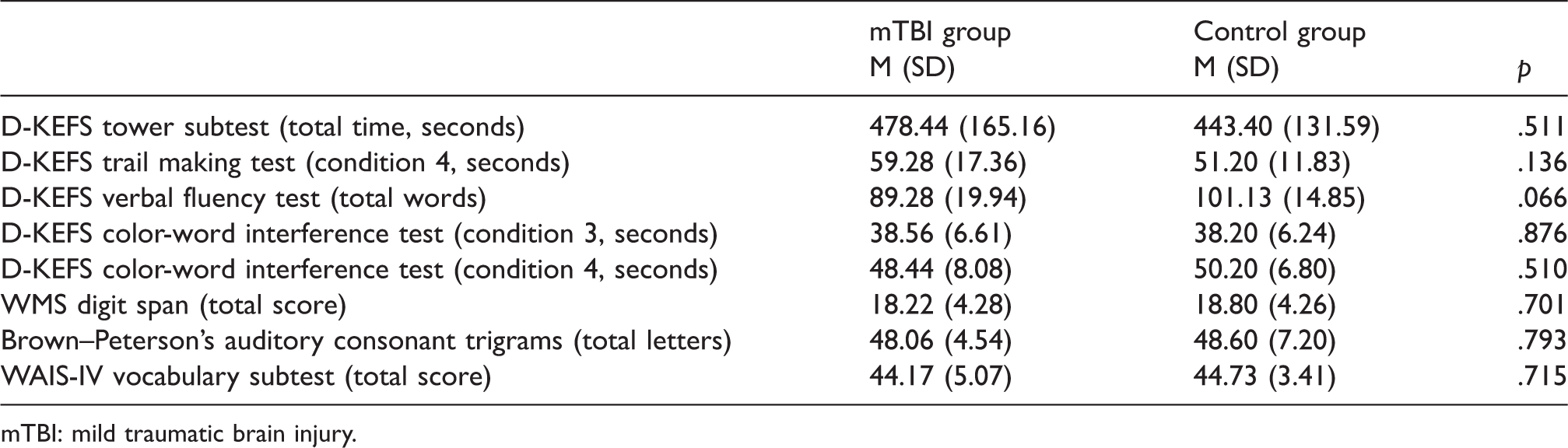
mTBI: mild traumatic brain injury.
The mTBI group was slower and more unstable than the control group for Upper Limb Coordination (p = 0.029), the 10-m Walk Test (p = 0.023) and the BESS (single-leg stance; p = 0.027) (Table 3). Outliers (>3SD) were found in one participant in the mTBI group for gait fluidity. Analyses were re-run without this participant, but yielded the same results; therefore, the initial analyses are presented.
Results of physiological assessment.
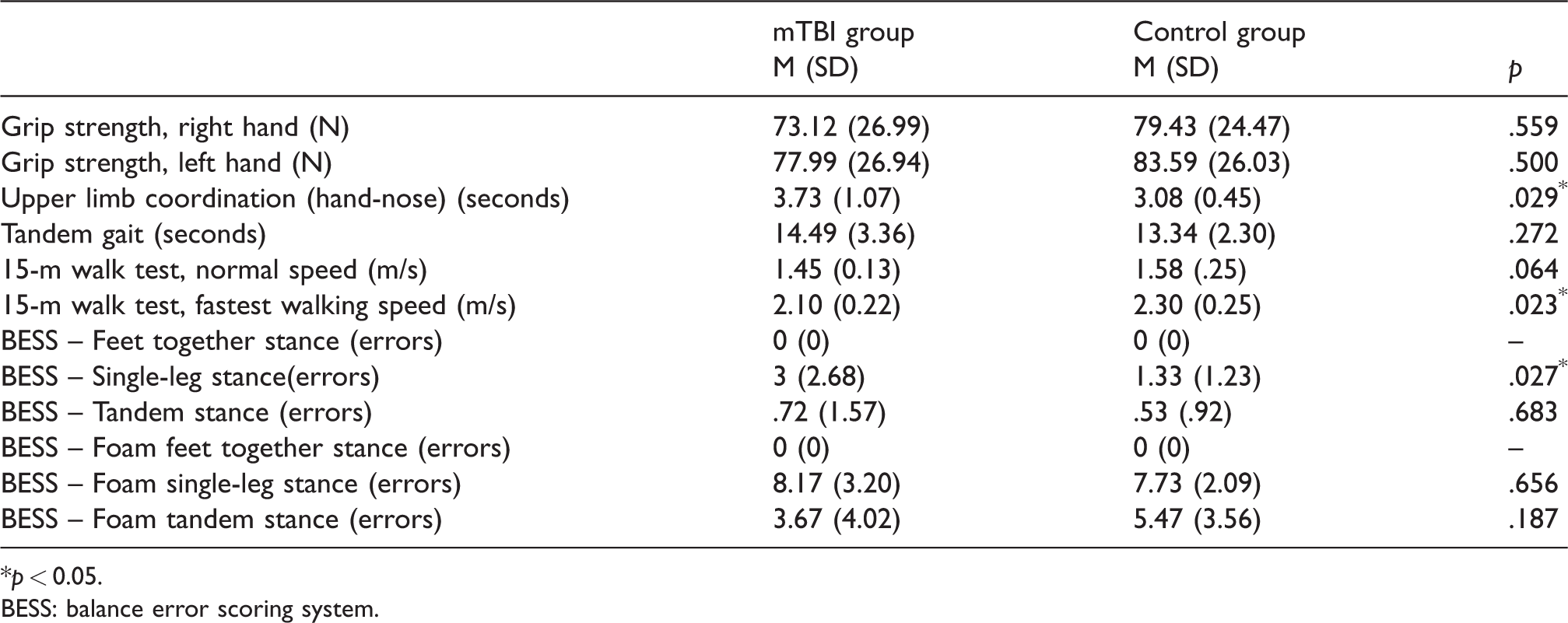
p < 0.05.
BESS: balance error scoring system.
The three-way interactions were non-significant for all locomotor variables. There was no significant group effect for gait fluidity, obstacle clearance or DTCs for gait speed and gait fluidity, but a significant group effect was observed for gait speed (p = 0.014;
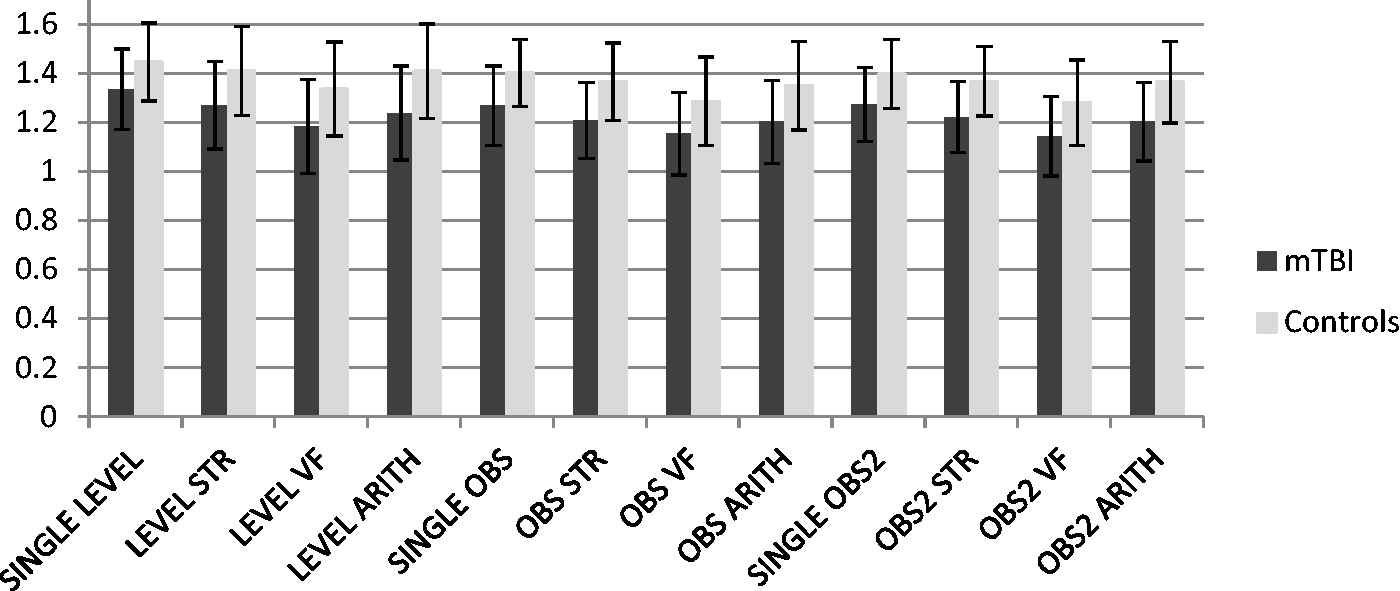
Average gait speed (m/s) during all single and DTWs for mTBI and control groups (standard deviations indicated by error bars) (STR: stoop task; VF: verbal fluency task; ARITH: arithmetic task).
Missing data led to the removal of one participant from each group for response time, and one participant in the mTBI group for answers/time ratio and errors. The three-way interactions were non-significant for all cognitive variables. A significant group effect was found for response time (p = 0.025,
Mean (SD) and total number of errors during DTW conditions for mTBI and Control groups.
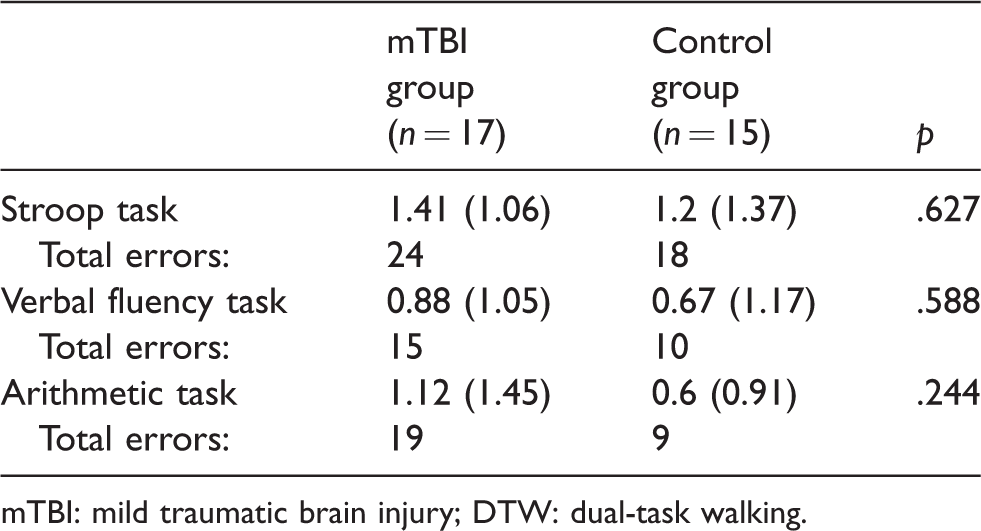
mTBI: mild traumatic brain injury; DTW: dual-task walking.
For the second objective, gait speed and DTC for gait speed were not found to be correlated with head injury history. For the DTW arithmetic task, a higher number of prior head injuries was associated with shorter response times (r = −.583, p = 0.014). For DTW with Verbal Fluency, a positive correlation between answers/time ratios and number of prior injuries (r = .487, p = 0.048) was found. A positive correlation was also found between the number of prior head injuries and DTC for answers/time ratios during the Arithmetic task when all locomotor conditions were combined (r = .560, p = 0.019), suggesting a greater decrement from single to DTW for those with a higher number of prior injuries.
Discussion
This study aimed to investigate performance across different complex locomotor and cognitive DTW conditions in the first months after mTBI and to explore the potential relationship between DTW performance and history of head injury. Subtle, but persistent residual deficits for locomotor and cognitive parameters were revealed during DTW post-mTBI. However, no specific combination of locomotor or cognitive task was found to clearly stratify groups. History of mTBI correlated with several measures of dual-task performance.
Groups did not differ on gait fluidity or obstacle clearance, but gait speed was found to be significantly slower in the mTBI group on both DTW and single task walking conditions. Previous studies have documented this finding, but mostly for the acute period post-mTBI.13,26 Two studies conducted in the longer term after the injury also found similar results. Martini et al. 16 observed slower DTW gait speed for level-walking in persons 6.3 years on average post-mTBI. More recently, Cossette et al. 6 observed slower gait speed on average 158 days post-injury, particularly for obstacle avoidance, regardless of the type of cognitive task used (Stroop, Verbal Fluency or Arithmetic). Several authors have suggested that this represents a more conservative gait pattern, in conjunction at times with a wider foot base, 16 in order to increase stability and avoid falls.8,21,27
The generally lower gait speed in the mTBI group may have masked potential differences between groups during specific dual-task conditions in both previous work 15 and the present study. Performance in both groups was affected similarly when cognitive tasks were added (Figure 1). However, when we controlled for baseline gait speed, the difference between groups for gait speed approached statistical significance suggesting that DTW may affect gait speed more for the mTBI group than for the control group. Future studies may further confirm this difference with a greater number of participants. It was uncertain, however, if a specific combination of locomotor and cognitive task would expose gait speed differences further. Our results showed that both groups were similarly affected by DTW with a decrease of gait speed, no matter what tasks were used. Future studies should perhaps focus on identifying which dependent variables are most sensitive to reveal alterations in DTW after mTBI. Further research is also needed to understand how personal factors might influence DTW performance after concussion, for example age or training received to develop particular skills.
To date, most DTW studies have focused on motor performance. The few studies that have explored cognitive performance have not found any significant group differences.13,14,16 The present study made an effort to rigorously document cognitive performance. When data from all three cognitive tasks were combined, we found average response times to be slower in the mTBI group. In a previous study, Catena et al. 26 had noted more variability for response time in the mTBI group, but no significant differences between groups. According to the capacity theory, attentional resources are limited. The fact that participants with mTBI had slower gait speed and processing speed may indicate a competition between resources, which globally slowed the completion of the dual-task. General information processing speed alone is also known to be reduced following mTBI and our results suggest that subtle differences may persist following the acute period. 28 The absence of statistical differences on other cognitive parameters (answers/time ratios, number of answers, errors and DTC for answers/time ratios) might be due to a ceiling effect due to the short duration of the trials. Most studies involving gait, including ours, use short walkways such that cognitive performance is measured over a very short period of time. Increasing walking distance and the duration of trials would allow participants to produce more answers, thereby possibly improving the detection of more subtle differences on cognitive tasks.
For some DTC results, high standard deviations were observed within both groups suggesting differences between participants within the same group in terms of cognition and gait. A possible explanation could be different prioritization strategies between individuals. The mainstream theory is that a person will prioritize an efficient posture over performance on the cognitive task in order to ensure safety. 29 However, this process appears to be much more complex and flexible, influenced not only by motor and cognitive aspects, but also by environmental conditions and individual characteristics such as skills, mood, or task complexity. 29 In the mTBI population, one study showed that prioritization was in fact quite variable across trials. 27 In the present study, participants were asked to keep a comfortable and natural gait speed while responding quickly and accurately to the cognitive task. As such, our results may reflect different prioritization patterns, some individuals giving priority to the locomotor task, others to the cognitive task, leading to presence of both positive and negative DTCs. Future studies could explore the effects of specific prioritization strategies in the context of DTW paradigms after mTBI.
Our results also suggest that a history of multiple mTBIs may affect DTW performance. The number of previous head injuries was correlated with faster response times in the Arithmetic task, higher answers/time ratios in the Verbal Fluency tasks, and greater DTC for the Arithmetic task. Although the specific mechanisms explaining these results remain unclear, the first two results may point toward a tendency to respond slightly more impulsively in persons with a history of multiple mTBIs. There is a suggested link between a history of mTBI and greater impulsivity in former athletes. 30 Our study did not show any significant correlation of prior head injury to motor variables despite two previous studies demonstrating that during both single and dual-tasks, participants with a multiple history of mTBIs show altered gait performance.21,22 However, both of these studies showed differences only when comparing persons with multiple injuires to the control group, while no significant differences were found compared to an intermediate mTBI group (1 or 2 concussions), demonstrating the subtlety of the impairment.21,22 In the present study, analyses were only carried out within the mTBI group. The need for further research investigating history of mTBI seems important considering the heterogeneity that this factor may introduce and its possible influence on performance outcomes.
The present study has several limitations including the limited number of participants, short trials potentially affecting the assessment of cognitive performance and heterogeneity in recovery periods in mTBI participants. Furthermore, our instructions may have led to various prioritization patterns, and personal abilities (e.g. arithmetic skills) could have influenced performance on cognitive tasks. Despite these limitations, this study adds further knowledge to a still sparse literature on DTW. The study also provides novel information on the relationship between DTW performance and history of concussion.
In conclusion, subtle impairments are present during DTW about one to three months post-mTBI as indicated by slower gait speed and cognitive reaction time. The functional significance of these differences remains to be studied. This suggests that combining walking and cognitive tasks is useful to uncover persisting alterations in motor or cognitive function post-acute injury. However, the optimal combination of tasks remains unclear. A history of multiple mTBIs appears to be linked to DTW cognitive performance and needs to be further considered in research and clinical practice. Although they are not yet included in routine clinical assessment, dual-tasks while walking may represent a useful paradigm to help patients and providers evaluate functionning following mTBI. However, there is a need to develop simple, more “clinic-friendly” dual-task protocols which can inform clinicians on the evolution of patients and provide guidance for return-to-function decisions.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Canadian Institutes for Health Research (Grant # CBI-127052) and from the Natural Sciences and Engineering Research Council of Canada (Grant # RGPIN/191782-2012).
