Abstract
Background
Nutrients may have implications following concussion, such as inflammation reduction or neuroprotection. The purpose of this study was to describe nutrition practices of athletic trainers (AT) and dietitians for patients regarding sport-related concussion, with respect to prevention, recommendations, and barriers to implementation.
Hypotheses
Due to the descriptive nature of this study, hypotheses were not warranted.
Study Design
Mixed methods.
Level of Evidence
Level 3.
Methods
A survey was distributed through professional memberships and included multiple-choice and open-ended items about nutritional practices regarding concussions. Participants included 1465 ATs and 51 dietitians accessing the survey (AT: age = 35.7 ± 11.4 years, females = 43.1%; dietitians: age = 31.8 ± 8.17 years, females = 45.1%). Open-ended survey responses regarding nutritional practices for concussion prevention, recommendations, and changes following concussion were analyzed by identifying key words or repeating phrases, theme development and categories into an initial codebook, using the codebook on responses, and coding all responses with the finalized codebook. Barriers to implementation was analyzed with descriptive statistics.
Results
Themes were identified for prevention strategies, and recommendations and changes following concussion. For concussion prevention, ATs noted overall health, specific target nutrients, barriers and limited research support, while dietitians identified overall health, specific target nutrients, recommendations/guidelines as themes. Post-injury themes for patient recommendations and changes were noted as overall health, specific target nutrients, resources, interprofessional collaboration by ATs, whereas dietitians identified overall health, specific target nutrients, interprofessional collaboration. ATs and dietitians noted numerous barriers including the lack of clinician knowledge and athlete compliance.
Conclusions and Clinical Relevance
ATs and dietitians are utilizing nutritional practices regarding concussion in numerous ways by focusing on use for whole body, brain health and specific targets such as omega fatty acids, hydration, micronutrients/supplements, and macronutrients. With these findings and the barriers listed by respondents, we can use this information to design focused research to influence evidence-based nutritional practices and concussion.
Introduction
Concussions represent a significant public health concern. 1 As such, prevention models have been applied in order to influence this injury. Prevention can be categorized into primary, secondary, and tertiary models. Primary prevention aims to prevent the injury from occurring in the first place, 2 with strategies such as rule changes3,4 and contact restrictions 5 reducing the incidence of concussion. Secondary prevention efforts are those aimed at reducing or limiting long-term disability or re-injury following concussion, 2 including legislation,6,7 education, 8 and early identification and management. 9 Lastly, tertiary prevention strategies aim to limit or lessen the long-term effects of a concussion on function or quality of life, 2 such as the inclusion of early aerobic exercise to improve recovery time.10,11 Efforts to determine ways to prevent concussions through primary, secondary, and tertiary prevention strategies have been of great interest.
One proposed prevention strategy for concussion or post-injury sequelae is nutrition, through food or supplements. The nutrients of omega-3 fatty acids, magnesium, riboflavin, curcumin, vitamin D, and melatonin may potentially be beneficial in brain health to prevent or aid in the recovery of concussion, however that list is not exhaustive. Additional nutrients in both food and supplements that are proposed to potentially also play a role are vitamins B3, B6, B9, C, and E, n-acetyl cysteine, resveratrol, ginseng, gingko biloba, zinc, and creatine.12,13 However, many of these nutrients have been examined in rat models, preclinical settings, or not in individuals with concussions, but rather in the larger spectrum of traumatic brain injuries.12,13 This leads to some discrepancies in the clinical recommendations regarding nutrition following concussion. For example, the National Athletic Trainer's Association (NATA) Position Statement suggests that patients should avoid alcohol and eat a well-balanced, nutritious diet high in carbohydrates. 14 In contrast, the American Medical Society for Sports Medicine position statement suggests that while there is emerging evidence in animal models that supplements may protect or speed recovery, the recommendation to include nutraceuticals in concussion management is tempered due to non-Food and Drug Administration (FDA) regulation of supplements and limited evidence. 15
While the literature is inconsistent with what benefits various nutraceuticals may provide to patients following sport-related concussion, basic science research supports the notion that some nutrients from food and supplements are able to pass the blood-brain barrier, which could aid in improving the neuropsychological process following injury.12,16,17 The neuropathological process that occurs after a concussion is largely examined in rat models and includes a neurometabolic cascade that begins with an impact either directly or indirectly to the head. 18 During the neurometabolic cascade following injury, there is an efflux of potassium, and calcium and sodium enter the cell. 18 The neuron works over time in order to maintain equilibrium which requires adenosine triphosphate. However due to a decrease in cerebral blood flow the cell experiences an energy crisis. 18 The neurometabolic cascade following concussion creates many theorized opportunities for food and supplements to influence this process, and thus aid in recovery.
Anecdotally, clinicians are often recommending both food and supplement as a primary prevention strategy or following a concussive injury, but to date these practices are often not documented. As such, it is important to examine how clinicians and dietitians are implementing nutrient changes, from both food and supplements, to prevent or manage a concussion in humans. Therefore, the overall purpose of this study was to understand primary and secondary nutrition prevention practices, among athletic trainers and dietitians. Specifically, we aimed to 1) describe nutrition (e.g., food and/or supplements) practices of athletic trainers and dietitians for patients sustaining sport-related concussions, and 2) describe barriers perceived by athletic trainers and dietitians who are not implementing nutrition (e.g., food and/or supplements) recommendation practices for patients regarding sport-related concussions. Due to the descriptive and exploratory nature of this inquiry, hypotheses are not warranted and were not developed to minimize researcher bias.
Methods
Strategy
This study was determined to be exempt from A.T. Still University's Institutional Review Board (Exempt protocol #2020-118). Data collection for this study was prospective, featuring a mixed methods approach, specifically a concurrent nested design. We chose a convergent parallel design with qualitative and quantitative research methods to obtain a deeper, more comprehensive understanding of a phenomena. 19 Aim 1 was conducted using qualitative research methods guided by a consensual qualitative research (CQR) tradition and aim 2 was cross-sectional. CQR was chosen to guide this research because it is rooted in phenomenology, 20 grounded theory, 21 and comprehensive process analysis.22–24 CQR includes the essential components of: (a) open-ended questions; (b) a data collection process that includes multiple researchers across the analysis process to ensure multiple perspectives; (c) arriving at consensus to judge the meaning of the data; (d) at least one formal auditor to assess the work of the main team of judges and to minimize the potential effects of group bias within that team; and (e) domains and core ideas within the data analysis. 22
Participants
The inclusion criteria for this study included those who were athletic trainers or dietitians and members of their respective professional organizations. Athletic trainers and dietitians were recruited from convenience samples through their respective professional organizations, the NATA's and Collegiate and Professional Sports Dietitians Association (CPSDA). We initially contacted 20,000 athletic trainers in the secondary school, college/university, professional, and clinic/hospital settings through the NATA's Research Survey Service. Dietitians were recruited through the CPSDA listserv. We contacted dietitians via the CPSDA by posting on their professional discussion board for a potential participant pool of approximately 1400 members. We also posted the survey link to social media outlets in order to increase recruitment. The exclusion criteria included those who were not athletic trainers nor dietitians, or not members of the NATA or CPSDA.
Instrumentation
Following an extensive literature search, it was determined that no validated surveys exist aiming to explore athletic trainers’ and dietitians’ practices regarding nutrition changes and recommendations for concussion. The survey was developed by the research team to include multiple-choice items (Aim 1) but also open-ended items (Aim 2), regarding supplement practices related to concussion (31 items total). Participants also answered specific demographic items. Face and content validity were assessed by two concussion experts who are also ATs and three sports medicine dietitians. To assess face and content validity, experts and clinicians were provided an initial survey draft and asked to provide their feedback regarding survey flow, feasibility, item clarity and relevance, and if any topics were not included in the survey that should be. Because the survey was used to describe nutritional practices for prevention prior to and management following concussions, it was determined from a statistical consultation that a reliability analysis was not warranted.25,26 Eligible participants answered items about specific food and supplementation in concussion practices such as if the respondent uses food and supplements as a preventative measure for concussions, recommendations regarding food and supplements following concussion, and any actual changes of food and supplement practices following concussion. If participants endorsed those practices, they were then asked to answer questions regarding each of those practices (i.e., which nutrients are targeted, specific instructions, dosage, frequency, duration), the reasoning behind these nutrient changes, and perceived effectiveness. If participants did not use food or supplements for preventative measures, offer nutritional advice or change nutrition following concussion, we followed up with questions regarding reasons why they do not implement these changes.
Procedures
Participants who met inclusion criteria were contacted via the NATA Research Survey Service, CPSDA discussion board, or asked to click on a link solicited via social media. The survey was expected to require 20 min for each participant. Voluntary written consent was implied when the participant opened the survey link, clicked the “next” arrow and voluntarily provided survey information. A weekly reminder message or the survey link was posted weekly following initial distribution to those who have not yet completed the survey. The survey was open for one month. Participants were entered into a drawing for one of six $50 Amazon gift cards following the completion of the survey and if they voluntarily provided their contact information. While the survey was anonymous, participants were taken to a separate survey link automatically following data collection to provide their contact information. Contact information was kept separate from survey responses.
Data analysis
Descriptive statistics including means, standard deviations, and frequencies were calculated for demographic variables such as age, sex, setting, profession, etc. Aim 1 was analyzed generally using a content analysis in examining the open-ended responses by participants. Data analysis included five stages: 1) identification of key or repeating words or phrases; 2) development of key words into themes and categories into initial codebook creation; 3) using the initial codebook to code, codebook finalization; 4) coding participants’ responses using the finalized codebook; and 5) final coded participant responses counted, and gathered into one document.22,23 Dependability and confirmability of the data was assessed by an external reviewer served as qualitative data auditor. 27 We sent the auditor a small number of responses from each participant group, the corresponding coded responses, all finalized codebooks, and the survey. For each participant group, the auditor read 50 randomly selected responses from ATs and all responses for dietitians, created a codebook, and determined whether there was agreement among their codebooks and the codebooks created by the research team. Aim 2 was analyzed using descriptive statistics including frequencies.
Results
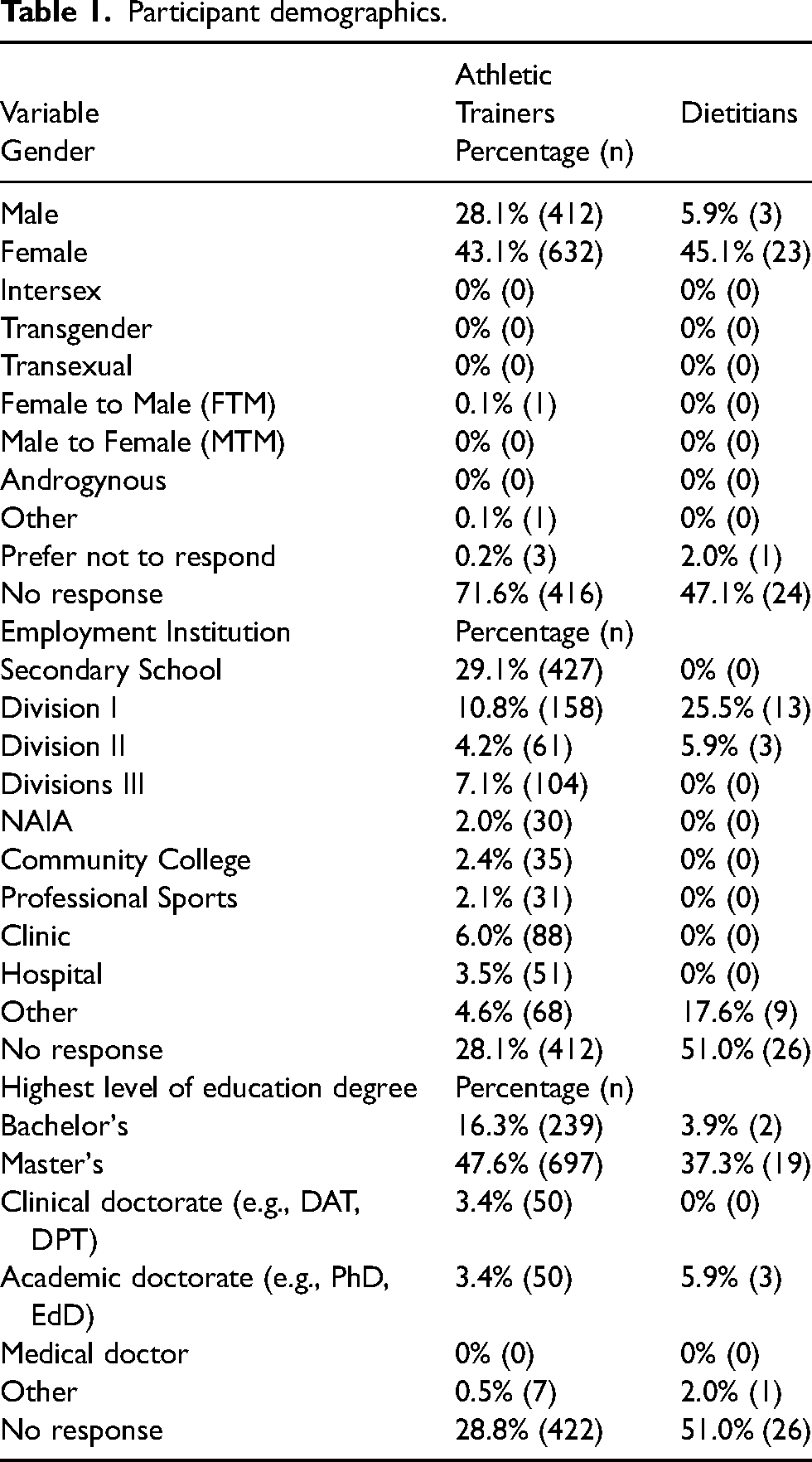
Overall, 1465 AT respondents accessed the survey (access rate = 7.3%, n = 1465/20000) with 1048 AT respondents completing the entire survey (completion rate = 71.5%, n = 1048/1465). Fifty-one dietitians accessed the survey (access rate = 3.6%, n = 51/1400) with 25 dietitian respondents completing the entire survey (completion rate = 49.0%, n = 25/51). The average age for AT respondents was 35.7 ± 11.4 years (n = 1050) and 31.8 ± 8.17 years (n = 27) for dietitian respondents. AT respondents had worked an average of 8.1 ± 8.4 years (n = 1034) in their current clinical setting, however had been practicing clinically as an athletic trainer for an average of 12.3 ± 10.6 years (n = 1032). While dietitians worked an average of 4.3 ± 3.7 years (n = 25) at their current position, however had been practicing for an average of 7.0 ± 7.8 years (n = 25). The average number of patients with concussion managed per year for ATs was 14.8 ± 14.7 cases (n = 1011) and 9.1 ± 5.8 cases (n = 25) for dietitians. All other demographic variables are included in Table 1.
Participant demographics.

Nutritional practices description
From our sample, 2.7% ATs and 33.3% dietitians currently use nutrition as a preventative measure for concussions, while 5.5% ATs and 13.7% dietitians
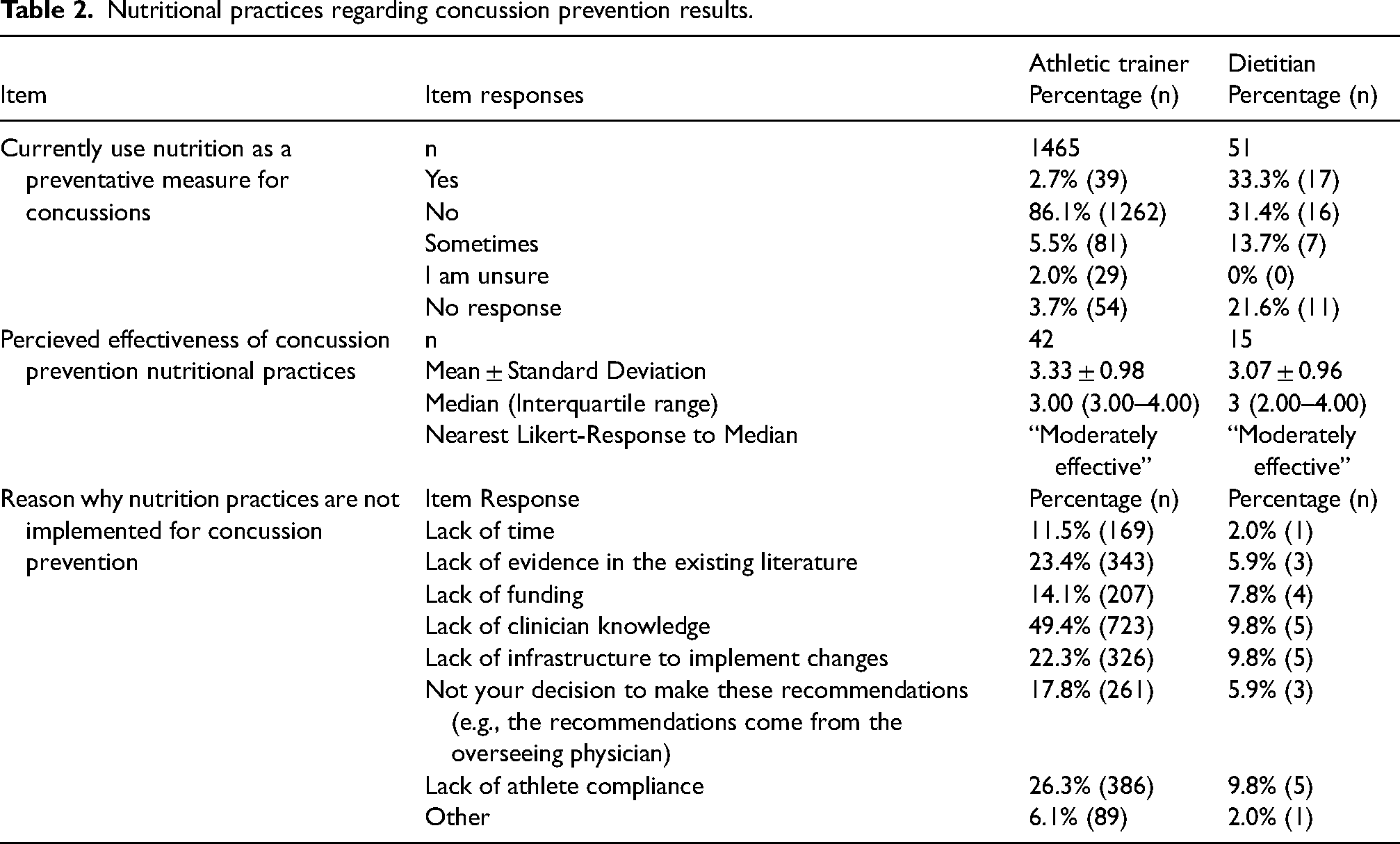
Nutritional practices regarding concussion prevention results.
Due to differences in AT and dietitian responses, two codebooks were developed. From the qualitative data analysis for ATs, four themes emerged for use of nutrition for concussion prevention including overall health, specific nutrient targets, barriers, and limited research support (Figure 1). The discovered subthemes of overall health included (1) brain, whole body health, (2) performance and (3) balanced diet. Participants often noted using nutrition prevention practices for brain, whole body health stating “I use proper nutrition for preventing all injuries” and “healthy foods lead to better overall health and may aid in preventing concussions.” For the performance subtheme, participants noted “…poor nutrition decreases performance physically and mentally thus increasing risk of injury” and “to feed the brain good nutrition for optimal performance.” Lastly, participants often stated using “balanced diet” with the words themselves to promote health and also noted “I try to just encourage athletes to eat a healthy, well rounded diet to prevent injury and stay healthy.”
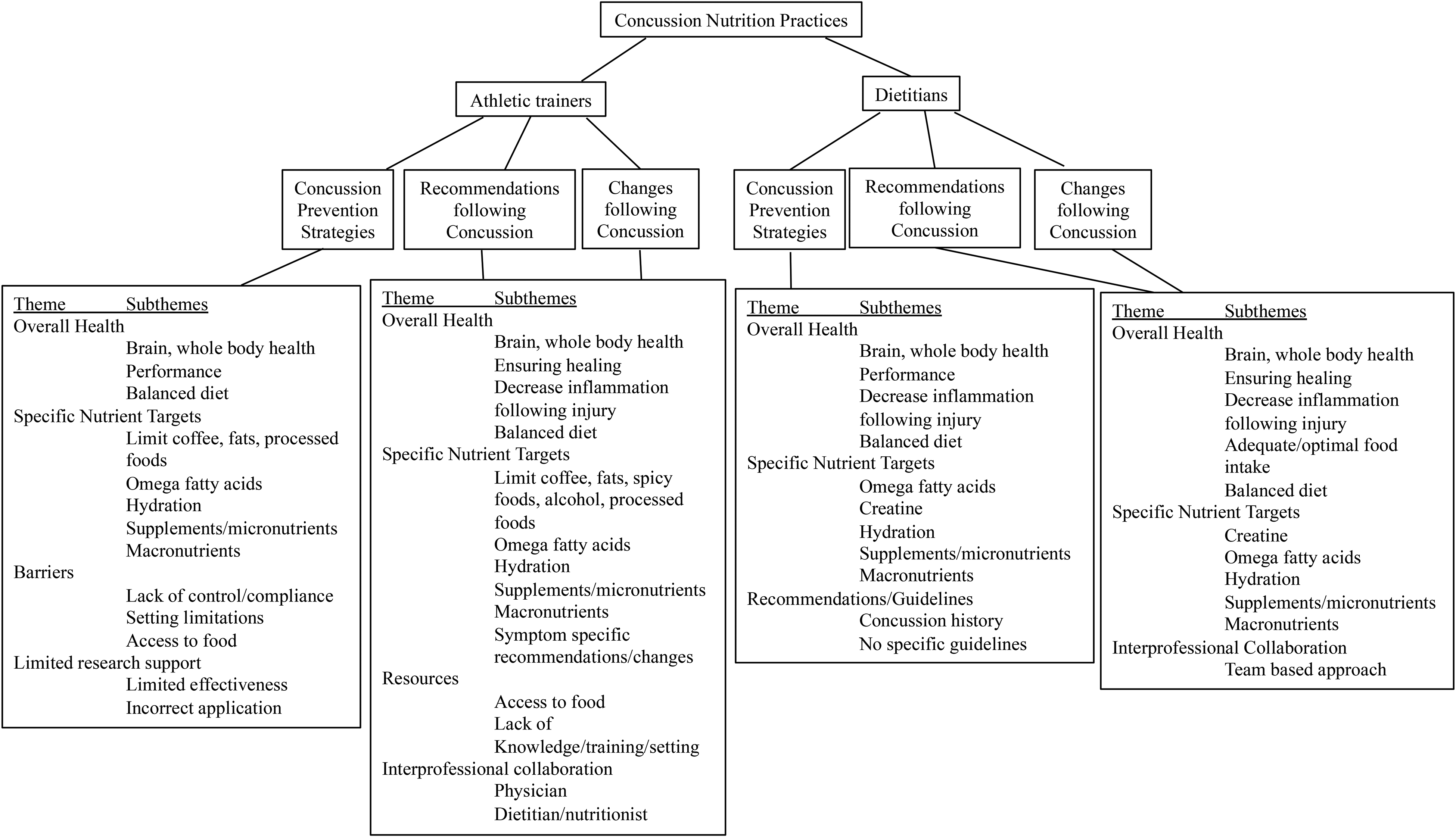
Concussion nutrition practice themes and subthemes for athletic trainers and dietitians.
The subthemes for specific nutrient targets included five subthemes. For the subtheme of limiting coffee, fats, processed foods, alcohol, participants would often state just that noting “Advise athletes to avoid caffeine alcohol, sugary and salty, and fried foods” or “no junk food.” Omega fatty acids subtheme was among the most frequently utilized code for using nutrition for concussion prevention practices with statements such as “fish oil supplementation” or recommending patients eat fish for the omega-3 fatty acids as well. The hydration subtheme was also a common utilized code with participants simply noting that hydration targeted for concussion preventions nutritional practices. Participants noted numerous supplements and micronutrients for concussion prevention including L-carnitine, vitamin B/riboflavin, magnesium, vitamin C, collagen, vitamin D, vitamin E, electrolytes, potassium, multi-vitamins, among others. For the last subtheme of macronutrients, participants often noted the use of “lean proteins,” “healthy fats and carbs.”
ATs noted many barriers to using nutrition in prevention of a concussion including the three subthemes of lack of control or compliance, setting limitations, and patients’ access to food. Evidence to support the lack of control or compliance subtheme included participants stating “I deal with high school athletes, so I cannot force patients to provide this or control what they eat” and “…try to advise, but they don’t always listen.” ATs described their setting limitations due to setting in this area stating “As an athletic trainer at my work setting, I am not allowed to directly provide nutritional direction to patients.” Finally, patients’ access to food was also described: “Not all patients or athletes can afford creatine, and we don't always have contact with them before a concussion happens.”
The subthemes that emerged for the limited research support theme included (1) limited research support, and (2) incorrect application. Participants described that there was limited research evidence to implement nutrition for prevention of a concussion by writing “None of this will PREVENT a concussion- just helps with overall brain and body health.” As we were coding, we also noted the incorrect application or use of supplements in regards to brain health including participants simply listing that both collagen and vitamin A would be utilized to prevent a concussion.
For the dietitians we discovered three themes of overall health, specific nutrient targets, and recommendations/guidelines (Figure 1). The subthemes for overall health and responses for these subthemes were similar to AT subthemes including brain, whole body health, performance, and balanced diet. However, one additional subtheme was discovered: decreasing inflammation following injury. Sample responses for this subtheme included having an “anti-inflammatory meal,” and “[The] potential role of DHA, EPA to reduce brain tissue inflammation.”
The following subthemes emerged for the specific nutrient targets theme including omega fatty acids, hydration, supplements/micronutrients, and macronutrients. However, an additional subtheme discovered for dietitians included creatine. Dietitian respondents noted “Per NCAA bylaws, we are not allowed to provide creatine to athletes, but I offer recommendations for intake.”
Two subthemes were discovered for the recommendations/guidelines theme of concussion history and no specific guidelines. Participants noted they would recommend nutrition practices for prevention of a concussion for “…[student-athletes] with history of multiple concussions…” Lastly, respondents noted they have no specific guidelines for nutrition and concussion prevention practices but nonetheless use nutrition to prevention concussions.
Recommendations and changes following concussion
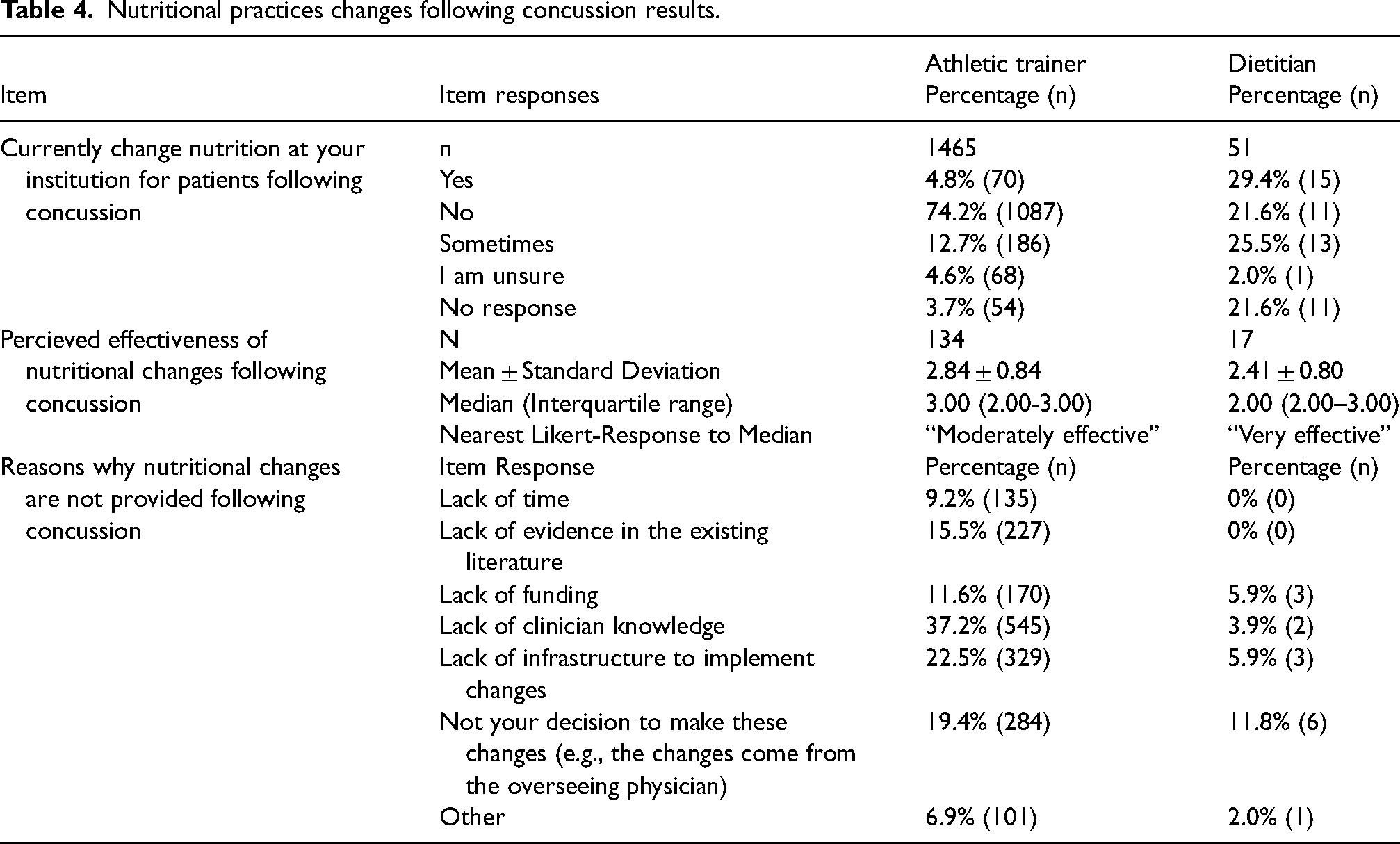
Descriptive results regarding nutrition recommendations provided following a concussion from ATs and dietitians are provided in Table 3, while descriptive results for those clinicians making actual changes are presented in Table 4. From our sample, 28.5% of ATs and nearly 60% of dietitians offered nutritional recommendations to patients following concussion with ATs believing those changes were “moderately effective” and dietitians believing changes were “very effective” (Table 3). While only 4.8% of ATs and 29.4% made actual nutritional changes at their institution for patients following concussion, with ATs believing the changes made were “moderately effective” and dietitians believing said changes were “very effective” (Table 4).
Nutritional practice recommendations following concussion results.
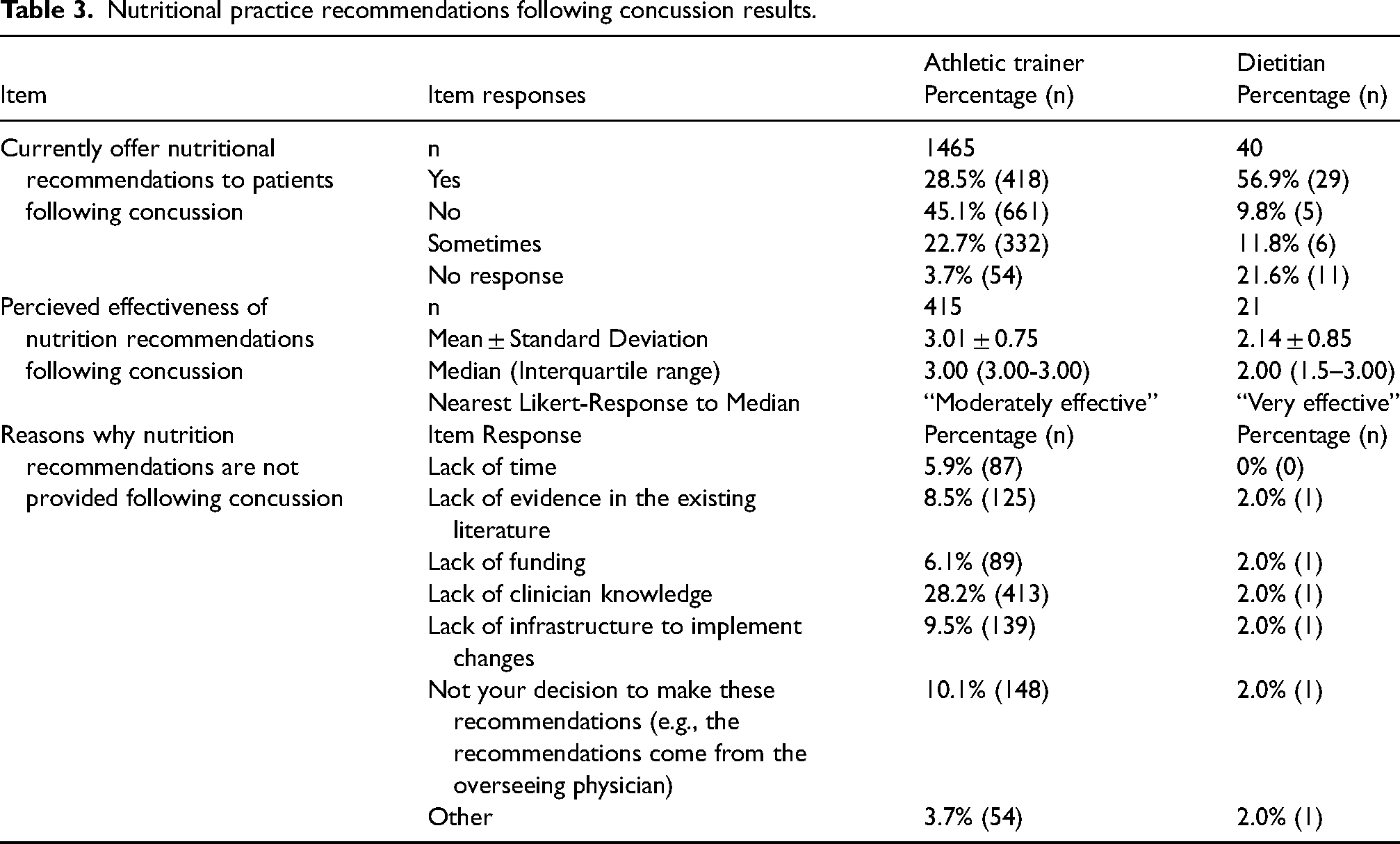

Nutritional practices changes following concussion results.
While the items for nutritional recommendations and changes were coded separately the same codebook was utilized and therefore, the results are presented together. Four overall themes were discovered for ATs who recommend and change nutrition following a concussion, which included overall health, specific nutrient targets following concussion, resources, and interprofessional collaboration.
The overall health theme had four subthemes including 1) brain, whole body health, 2) ensuring healing, 3) decreasing inflammation following injury, and 4) balanced diet. ATs noted they would again provide nutrition recommendations and changes following a concussion for brain, whole body health noting “I recommend certain foods that will help improve brain functioning…” ATs also describe recommending and changing nutrition following concussion in order to ensure the brain was healing during the injury: “To provide the optimal environment for healing.” Participants often noted simply stating using nutrition to “decrease inflammation” following injury or even recommending or changing to an “anti-inflammatory diet.” Lastly, as with above, participants described recommending and changing nutrition following injury for a “balanced diet,” often using that exact terminology.
ATs noted similar specific nutrient targets following concussion including the subthemes of 1) limiting, coffee, fats, spicy foods, alcohol, processed foods, 2) omega fatty acids, 3) hydration, 4) supplements/micronutrients, 5) macronutrients, 6) symptom specific recommendation and changes, and 7) prolonged recovery. One respondent even described multiple subthemes by stating: “…decrease the processed foods, no junk food, stay away from high sugary foods, and most importantly to hydrate with the appropriate hydration choices.” Evidence of the omega fatty acids and supplements/micronutrients recommendation or change following concussion included “Provide fish oil, magnesium and Vitamin B supplements for concussion patients.” The macronutrient subtheme was utilized for respondents who noted to “increase protein,” “focus on health fats” and include a “carb-rich diet.” ATs noted using specific nutritional recommendations or changes based on the symptoms the patient was experiencing stating “Might consider magnesium [once a day] for headache/migraine management,” “melatonin for sleep difficulty…” or “try to limit outside factors that may provoke symptoms (e.g., hunger, dehydration).” Lastly, many of these recommendations would be changed if the patient is having a “prolonged” or “slow recovery.”
We discovered two subthemes for the overall theme of resources, including 1) access to food and 2) lack of knowledge, training, or setting limitations. One participant stated: “At the secondary school I am at, the most basic nutritional information I give patients regardless of injury is suggesting a well-balanced diet. Many of my patients are on [free and reduced] lunches and/or breakfast. Giving suggestions of nutritious and relatively inexpensive foods is the best I can hope for.”
Lastly, ATs often noted interprofessional collaboration with physicians, and dietitians and nutritionists. One participant described “These recommendations come from our physicians or dietitian, but there have been recommendations to take fish oil and to limit gluten.” Another example includes a participant noting “I make the recommendations and reach out to nutritionist, but I do not get follow-through from the student-athlete or nutritionist.”
Three overall themes were identified for dietitians of overall health, specific nutrient targets following concussion, and interprofessional collaboration. For the overall health theme, similarly subthemes were discovered as the AT respondents of 1) brain, whole body health, 2) ensuring healing, 3) decreasing inflammation following injury and 4) balanced diet. However, an additional theme of adequate or optimal food intake was also discovered. Dietitian responses noted recommending or changing nutrition to “maintain weight,” provide “…education on consistent calorie intake,” or “…optimize appetite.”
For the second theme of specific nutrient targets following concussion, we discovered five subthemes mostly similar to AT responses too of omega fatty acids, hydration, supplements/micronutrients, macronutrients, and creatine. The discovery of creatine as a subtheme varied to AT responses. Dietitians stated “For those [greater than] 18 years old, [I] will recommend creatine dosing…” or simply listing recommendation or changes in creatine.
Lastly, dietitians also noted interprofessional collaboration in that respondents described a team-based approach. One respondent described “Recommendations are all done alongside support from multidisciplinary personnel ([athletic trainer], physiotherapist, sports medicine [physician] and [strength and conditioning]) throughout return to play and/or return to learn programs.”
Barriers
For those not using nutrition for concussion prevention measures or post-concussion recommendations or changes, AT respondents most frequently noted lack of clinician knowledge as the most common barrier (Tables 2, 3 and 4). Additional reasons ATs cited for not implementing nutrition practices for concussion prevention were athlete compliance and evidence in the existing literature (Table 2). The most common reasons why ATs did not implement nutritional recommendations and changes following concussion was because they believed this fell outside of their scope and a lack of infrastructure (Tables 3 and 4).
Dietitians also noted lack of clinician knowledge, infrastructure to implement changes, and athlete compliance as the most frequently endorsed reasons as to why nutrition was not used for concussion prevention (Table 2). Reasons dietitians endorsed for why nutrition recommendations are not provided following concussion included all responses, except for lack of time and lack of evidence in the existing literature, however responses were from one participant (Table 3). Dietitians noted barriers to making nutritional changes following concussion as not their decision to make said changes, lack of funding, and infrastructure (Table 4).
Discussion
Having a better understanding regarding nutrition practices of medical providers and dietitians with respect to sport-related concussion prevention and post-injury recommendations is an important first step in this area of research. We noted that few ATs are using nutrition for sport-related concussion purposes either in prevention, recommendations alone, or changes following the injury itself. However, dietitians in our sample were more frequently using nutrition for concussion prevention, recommendations, and changes than not. In both groups, nutritional practices were often used for brain or whole body wellness, and often injury practices including omega fatty acids, hydration, micronutrients and macronutrients managed with interprofessional collaboration.
While the FDA outlines there is no scientific evidence supporting that nutrition changes to prevent concussion or influence return to play such that would allow athletes to return to activity sooner, 28 some ATs and dietitians are implementing said changes. Many micronutrients and supplements were listed from our participants for a variety of reasons including neuroprotection, decrease inflammation, headache aid, and for sleep disturbances. Omega fatty acids, vitamin D, curcumin, and melatonin are believed aid in neuroprotection and inflammation. Omega fatty acids were often discussed by both ATs and dietitians for concussion prevention, and recommendations and changes following the injury. Use of omega-3 fatty acids is grounded in basic science 29 since omega-3 fatty acids prevent axonal damage following injury 13 and reduce inflammatory cytokines. 30 Although vitamin D, curcumin nor melatonin were discovered as themes or subthemes, each have neuroprotective effects, vitamin D deficiency may influence the increase in inflammatory damage following injury as cells in the “central nervous system have vitamin D receptors that module gene transcription responsible for neuronal proliferation and maintenance of calcium homeostasis.”12,31 Additionally, curcumin is a flavonoid found in turmeric, 12 and flavonoids may have neuroprotective components, suppress neuroinflammation, 32 and may promote cognitive function. 33 While there has been a human study examining docosahexaenoic acid (DHA; a type of omega-3 fatty acid) levels amongst football athletes, individuals who were injured, including those with concussions, were excluded. 34 In a review, early evidence supporting vitamin D supplementation for reduced inflammation and neuronal injury in rats with traumatic brain injury was noted. 35 In line with the International Society of Sports Nutrition, creatine was a specific nutrient target recommended and changed by dietitians following injury. 36 Creatine is theorized to improve cognitive processing, 37 which may be impaired following a concussion. However, authors conclude that creatine use and cognitive function requires further investigation as several gaps still exist. 37
ATs noted using nutrition for symptom specific needs, including headache and sleep, post-injury. Both magnesium and riboflavin have been found useful in individuals with migraine headaches,38,39 which may aid in headaches, especially migraine headaches, following concussion however this has not been examined. Additionally, magnesium and riboflavin (vitamin B2) both influence brain energy metabolism as magnesium makes adenosine triphosphate biologically active and riboflavin is a co-factor in oxidative metabolism, 40 which makes both nutrients potentially useful during the energy crisis following concussion. Sleep disturbances are often experienced following concussion, 41 melatonin and caffeine may influence concussion recovery and prevention. Findings from a systematic review concluded that melatonin was effective at improving sleep disturbances in patients following a traumatic brain injury, 42 however more recent randomized controlled trials have found no effect or mixed findings in melatonin supplementation and concussion recovery.43,44 Caffeine is a stimulant inhibiting adenosine 1 and 2a receptors which may lead to suppression of glutamate release and inhibition in production of inflammatory cytokines. 45 Caffeine has been largely examined in rat models,45–49 however some studies have shown acute caffeine ingestion positive and negative outcomes in rats with traumatic brain injury.45,48 Our participants noted limited caffeine specifically prior and following concussion. While limiting caffeine for the neuropathologic reasons as listed above is noteworthy, recommending an athlete to limit or exclude caffeine when they are used to a certain caffeine intake may also have detrimental effects such as an increase in headache. It may be beneficial for clinicians to suggest the athletes’ regular amount of caffeine following injury, however future research should examine caffeine intake and concussion recovery specifically.
Due to the energy crisis following injury, it is also theorized that macronutrients, particularly carbohydrates, may aid in the concussion healing process. Respondents in our study often noted all three macronutrients of carbohydrates, proteins, and fats. A recent pilot study concluded that whole body metabolic rate after concussion did not change,50,51 indicating the source of energy either through carbohydrates, proteins, and fats did not change following injury. However, authors found an inflated resting-state metabolic response in those with a prior concussion history. 50 Secondly, in another pilot study examining the ketogenic diet for post-concussion syndrome patients, authors found an improvement in visual memory, but no other concussion assessment, after two months of dietary intervention (≥70% fat, ≤10% carbohydrates, and the remaining protein). 52 For both macronutrients and micronutrients, respondents often noted that these nutrients should be provided through whole foods and not just supplements. Given the current literature findings, it is clear much more work should be done in this area to determine if macronutrient or micronutrient focus, either through foods or supplements, impacts concussion prevention or recovery.
Authors have hypothesized that dehydration may influence the neurophysiologic process following concussion 53 and this was too noted in our findings in both AT and dietitian respondents. In a study of dehydration on mental status, balance, symptoms, and neurocognition, Patel, Mihalik 53 found that moderate dehydration increased the number and severity of concussion symptoms and worse visual memory, but no other concussion assessments differed based on hydration in those with a concussion. Similarly, in a study of individuals without concussions, symptoms associated with concussions were also increased in those who were dehydrated from mild exercise as oppose to when rested and euhydrated. 54 With respect to recommendations regarding hydration, water is best, as sports drinks include other nutrients and were considered to be supplements based on the recommendation of our dietitian research team members with respect to our coding. It is important for clinicians to understand that concussion symptoms may be influenced by hydration status and if dehydration is suspected to rely on other concussion assessments or delay return-to-activity decisions until euhydration can be reached.
Dietitians noted they do not have specific protocols nor guidelines for concussion prevention. This approach may be the most beneficial as the state of the literature does not support nor use for concussion prevention and post-injury. This was highlighted as ATs noted a lack of research support for concussion prevention and nutrition in our findings. Given this, it is also unsurprising the differing perceptions of effectiveness using nutrition in concussion prevention and management. Optimal food intake and nutrient supplementation is already a common consideration for athletic performance 55 and the recovery of injuries. 56 Until more is known regarding the effectiveness of concussion prevention or recovery and nutritional practices, it may be worthwhile to focus nutritional efforts on athletic performance and injury recovery globally.
Numerous barriers to nutrition practices and concussion were described in both our qualitative and quantitative findings. A lack of clinician knowledge and athlete compliance was often noted by athletic trainers. ATs providing athletic health care at the secondary school setting, as most in our sample, have many duties and demands on them. Clinicians in this setting also provide care to numerous patients from a variety of socioeconomic backgrounds, therefore it is unsurprising AT respondents noted a lack in athlete compliance and access to food as barriers for this population. Additionally, research and clinical use of nutrition and concussion is fairly new, and therefore is also understandable ATs and dietitians may not believe they have the knowledge to successfully advocate for. In a study of ATs and athletic training students providing care at the Division I setting, respondents answered 66% of nutrition knowledge items correctly. 57 It is noteworthy dietitians noted barriers such as a lack of funding and infrastructure when the majority of our sample included Division I dietitians. Division I athletics often have robust nutritional services for athletes. These findings in conjunction with ours continue to emphasize the great need to examine social determinants of health, including access to quality food, in regards to concussion prevention and care. ATs and dietitians are well suited to collaborate on nutrition and concussion following injury. ATs have strong concussion knowledge and dietitians have strong nutritional knowledge. This collaborative relationship may mitigate some of the barriers experienced by respondents in this study. However, we again acknowledge the challenges of establishing these relationships given several social determinants of health including transportation, access to quality food, socioeconomic status, health care access, among others.
Limitations
This study was cross-sectional, and descriptive in nature, and therefore would benefit from longitudinal studies that examine nutritional interventions for individuals at risk for concussion and following the injury itself. Further, since concussion is a multidimensional injury, understanding which nutritional interventions benefit patients with various concussion clinical presentations may be warranted. A comparison analysis of which clinicians are using which nutritional approaches should also be examined in future research. Secondly, our study had a limited sample of dietitians. While not ideal, we believe the dietitian results highlight a useful perspective but future research should aim to explore dietitian nutritional practices for concussion in a larger sample.
Conclusions
Identifying ways to prevent a sport-related concussion or positively impact concussion recovery is an important, emerging area of research. Some nutrients from food and supplements are able to pass the blood-brain barrier, which could aid in improving the neuropsychological process following injury.12,16,17 Specifically, our results highlight that ATs and dietitians are currently approaching nutritional practice and sport-related concussion holistically for whole body, brain health but targeting numerous specific nutrients including omega fatty acids, hydration, micronutrients/supplements, macronutrients, among others. Numerous barriers were often noted such as lack of clinician knowledge and athlete compliance. Our approach in examining nutrition and concussion enables a clinician-driven and practice-based approach by including clinicians and dietitians to outline what may be examined in future intervention studies. We can utilize the findings from this study and target specific nutrients to determine effectiveness and influence evidence-based concussion prevention and management.
Footnotes
Acknowledgements
We would like to acknowledge Ms. Jana Heitmeyer for her work on codebook creation and Dr Erica Beidler for serving as an external reviewer.
Declaration of conflicting interests
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was supported by A.T. Still University Warner/Fermaturo Fund.
Ethical approval
This study was determined to be exempt from A. T. Still University’s Institutional Review Board (Exempt protocol #2020-118).
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the A.T. Still University Warner/Fermaturo Fund.
