Abstract

Toxic epidermal necrolysis (TEN) is a rare, acute life-threatening mucocutaneous disorder that is characterised by epidermal loss/exfoliation exceeding 30% total body surface area (TBSA) and is on a spectrum that includes erythema multiforme and Stevens–Johnson syndrome (SJS). It is estimated that 80% of TEN cases are related to medication reactions; the association based on the recognition that TEN usually develops 1–3 weeks following administration of the suspect drug. It is agreed that primary treatment consists of prompt withdrawal of causative drugs and transfer to a regional burn unit. Transfer to a burn unit, no more than 7 days after onset of symptoms, has been acknowledged as reducing the risk of infections, hospital length of stay and infection-related mortality. Due to the uncertainty surrounding TEN pathogenesis, several different modalities have been proposed for the treatment of TEN, including high-dose intravenous immunoglobulins, plasmapheresis, cyclophosphamide, cyclosporine and systemic steroids; however, these therapies are relatively ineffective. The use of systemic corticosteroids for treatment of TEN has in particular been deemed controversial due to associations with increased infections leading to greater length of hospital stay and increased mortality.
Granulomatosis with polyangiitis (GPA), formerly known as Wegener’s granulomatosis, is a rare relapsing-remitting disorder of unknown aetiology, characterised by granulomatosis inflammation and necrotising vasculitis predominantly affecting small- to medium-sized vessels. While a 5-year survival rate of 75–83% is now realised, relapse and associated morbidity is of concern.
The established treatment for GPA follows the recommendations of the French National Authority for Health (HAS) for systematic necrotising vasculitis. With induction treatment, it is recommended that GPA be treated with a combination of systemic corticosteroids and immunosuppressants.
A review of the literature failed to identify any previous case where both of these conditions coincide. Our search was conducted through databases which included MEDLINE, PubMed, Scopus, AMED, CINAHL and EMBASE, using keywords: toxic epidermal necrolysis, Wegener’s granulomatosis, granulomatosis with polyangiitis. We submit the rare case of a 22-year-old woman who presented to our regional burn unit with both GPA and TEN, and we discuss the presentation, investigation and multidisciplinary management of the patient, as well as reviewing the literature regarding these two conditions.
Lay Summary
Toxic epidermal necrolysis is a potentially fatal condition where there is a large area of skin exfoliated after the body’s reaction to a particular medication. Its treatment is largely by stopping the medication that is thought to have caused this reaction and also by regular dressings, thus keeping the area clean from any infection. Granulomatosis with polyangiitis, also known as Wegener’s granulomatosis, is another potentially fatal condition. Its treatment is very specific; however, this treatment may be harmful to a patient with toxic epidermal necrolysis. We describe the management of a patient who presented with both conditions, which is an extremely rare event. We describe the diagnosis and treatment during the patient’s inpatient stay at a regional burns unit. From this case report we have shown insight into the multidisciplinary management needed to manage such a complex patient, who made a full recovery.
Keywords
Case report
A 22-year-old woman was referred by the critical care team of a district general hospital (DGH) to our regional burns unit with 100% TBSA involvement following toxic epidermal necrolysis (TEN) on the background of GPA. The patient initially presented to the DGH with a fever, shortness of breath and feeling generally unwell. A chest X-ray demonstrated multiple opacities and on computerised tomography (CT) of the chest and abdomen, she was found to have multiple cavitations, a pulmonary embolism and a femoral thrombosis. Granulomatosis with polyangiitis (GPA) was confirmed and the patient was commenced on warfarin, rituximab, methylprednisolone, Immunoglobulins (IgG) and fluconazole, to which she responded well. As part of this regime she had a second and third infusion of rituximab and prophylactic co-trimoxazole.
Three days following co-trimoxazole, she presented back to the DGH with angioedema and had developed a rash with an estimated 90% total body surface area (TBSA), involving the oral and ophthalmic mucosa. Fluconazole and co-trimoxazole were immediately stopped and the steroids increased with the initial suspicion of Stevens–Johnson syndrome (SJS). The patient deteriorated, progressing to 100% TBSA, and required significant support from the critical care team. TEN was suspected and subsequently confirmed by skin biopsy. She had an initial SCORTEN (SCORe of Toxic Epidermal Necrosis) score of 3, predicting a 35.3% mortality risk, and was accordingly referred and transferred to our specialist burns centre for management of her extensive wounds. Figure 1a and b show the large extent of the TBSA involved in this patient.
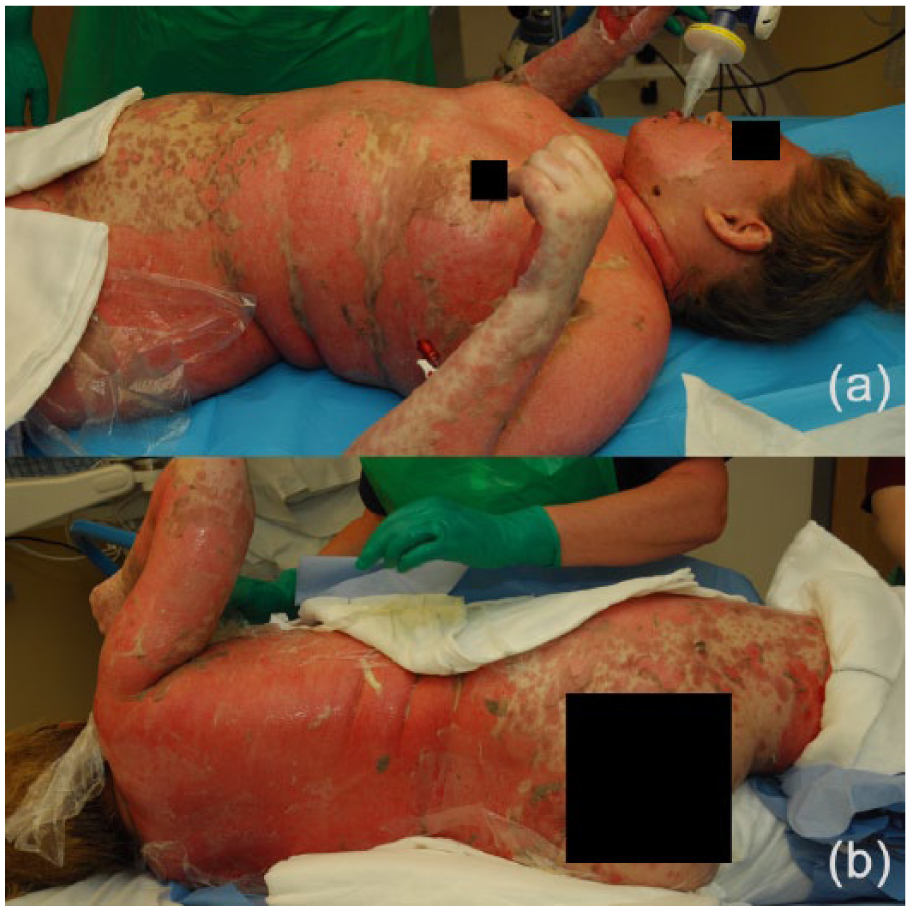
(a) Anterior view of patient with 100% TBSA of toxic epidermal necrolysis, including the head and neck. (b) Posterior view of the patient.
Piperacillin/Tazobactam (Tazocin) and Vancomycin antibiotics were commenced following sputum and wound swab sensitivities. One week following admission, prednisolone was reduced to 40 mg daily. After 10 days of treatment, there was good re-epithelisation of the skin. The patient was discharged at 3 weeks following a period of physiotherapy.
Discussion
GPA is a serious disease, with a fatal outcome in the absence of treatment. Fortunately, with therapeutic approaches that are increasingly standardised and the emergence of new biotherapies, 90% of patients go into remission, and the survival rate is approximately 75–83% at 5 years. The current treatment is based on a first phase, known as the induction phase, which aims to put the disease into remission, and lasts about 3–6 months according to the clinical response. A second phase, known as the maintenance phase, must then consolidate the remission and limit the risk of relapse and generally lasts 12–24 months. The intensity of the initial therapeutic approach must be adjusted for each patient and for the type and seriousness of GPA in order to avoid two pitfalls: excessive treatment associated with a significant risk of side effects, or insufficient treatment with a risk of failure or early relapse. With induction treatment, it is recommended that GPA be treated with a systemic corticosteroid and immunosuppressant combination. Oral prednisone is recommended at a daily starting dose of 1 mg/kg. For severe or refractory forms, oral corticosteroid therapy is preceded by an intravenous bolus of methylprednisolone at a dosage of 7.5 mg to first flare up or relapse (results under publication). Rituximab has a lower risk of relapse compared to azathioprine at 28 and 44 months after the start of the maintenance treatment (rate of major relapses at 44 months: 18.2% in the rituximab arm vs. 51.9% in the azathioprine arm). Treatment with co-trimoxazole (sulfamethoxazole/trimethoprim at a dose of 400 mg/80 mg) per day is systematically given for the prevention of relapse and of Pneumocystis jirovecii infections. The treatment regimens are increasingly adapted to the expression of the disease and to its course; relapses remain frequent, however, and the maintenance treatment methods warrant better standardization. 1
Glucocorticosteroids are prescribed in conjunction with induction therapy immunosuppressants and are not prescribed as monotherapy to induce clinical remission in GPA. Corticosteroids are prescribed at high doses while the disease is active then gradually tapered to the lowest dose of corticosteroid required to maintain remission with concomitant immunosuppressive drugs.
Although guidelines have been proposed regarding the treatment of TEN,2,3 its rarity hinders the establishment of treatment based on large prospective studies, and subsequently management standards have not been widely accepted. 4 It is, however, agreed that primary treatment consists of prompt withdrawal of causative drugs 5 and transfer to a regional burn unit. Transfer to a burn unit, no more than 7 days after onset of symptoms, has been acknowledged as reducing the risk of infections, hospital length of stay and infection-related mortality.6–9
TEN management focuses on resuscitative, symptomatic and supportive strategies, and comprises fluid resuscitation and electrolyte replacement, nutritional support, as well as suitable and targeted wound care.7,10 With sepsis being recognised as the leading cause of mortality in the TEN population,5,11 increased attentiveness towards skin care is warranted and includes prevention, early detection and treatment of infection 10 achieved by frequent skin, blood and urine cultures. 12 Emphasis must also be placed on the role of analgesia, deep vein thrombosis/pulmonary embolism and erosive gastric ulcer prophylaxis, and regular physiotherapy. 11
Due to the uncertainty surrounding TEN pathogenesis, several different modalities have been proposed for the treatment of TEN, including high-dose intravenous immunoglobulins, plasmapheresis, cyclophosphamide, cyclosporine and systemic steroids; however, these therapies are relatively ineffective.13,14 The use of systemic corticosteroids for treatment of TEN has in particular been deemed controversial due to associations with increased infections leading to greater length of hospital stay and increased mortality.15-20 In a study by Halebian et al., 15 15 consecutive patients with TEN or SJS managed without corticosteroids after transfer to the burn centre (group 2) were compared to a previous consecutive group of 15 patients who received high doses of these drugs (group 1). Group 2 had a 66% survival, which was a significant improvement compared to the 33% survival in group 1 (P = 0.057). In group 1, mortality was associated with loss of more than 50% TBSA skin loss. In group 2, mortality was related to advanced age and associated diseases. Non-steroid (group 2) management was associated with a decreased incidence of ulceration of gastrointestinal columnar epithelium, Candida sepsis, and an increased survival after septic complications.
Conclusion
TEN with GPA are both life-threatening illnesses. Treatment for GPA is well established and steroid use is part of this treatment in both the induction as well as the maintenance phase stages. Robust evidence for or against the use of steroids in the treatment of TEN is unavailable, but available published literature suggests that they can be harmful. We present an exceptionally rare case where both of these diseases occurred concurrently and raise awareness to the controversial role of steroid use in TENs. We also emphasise the importance of a multidisciplinary team approach for the management of such a complex case.
Footnotes
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Ethical approval
The authors confirm that the necessary written, informed consent was obtained from patients for this article.
