Abstract
Background
With an increasing older adult population, the number of persons with dementia will increase as well. The most common dementia diagnosis is Alzheimer’s disease, followed by vascular dementia (WHO, 2017). Regardless of diagnosis, dementia is associated with cognitive impairments, and responsive behaviors such as such as aggression, resistant behaviors (commonly to care), wandering, and screaming. (Aarsland, 2020; Mallon et al., 2019). Persons with dementia commonly express responsive behaviors in interaction with each other, such as in care situations when personal integrity is perceived as threatened (Wang et al., 2016). Cohen-Mansfield et al. (2015) also suggest that responsive behaviors are associated with loneliness, boredom, discomfort, and a need for meaningful activities.
Antipsychotic or antidepressant medications may be used to manage responsive behaviors. However, the use of pharmacological treatments is questioned due to the side effects, such as low blood pressure, risk for falls, and risk of stroke (Macfarlane & O’Connor, 2016), and it has been found that only 10% of such medications are in fact successful in minimizing responsive behaviors (van der Spek et al., 2016). They may also be associated with an increased risk of mortality (Gardette et al., 2012; Marcinkowska et al., 2020), and these risks are considered to outweigh the benefits; thus, nonpharmacological treatments should be considered first (Dyer et al., 2018; Radue et al., 2019; Sikkes et al., 2021). Nonpharmacological treatments have great potential to reduce the responsive behaviors (Abraha et al., 2017; Legere et al., 2018; Scales et al., 2018), but research with robust methodologies needs to be performed to fully evaluate the strength of evidence (Abraha et al., 2017).
There are various types of nonpharmacological therapies, such as aromatherapy, massage/touch therapy, light therapy, validation therapy and music (Leng et al., 2020; Scales et al., 2018). Different kinds of music activities are common and have been utilized due to their effects. In a review, Skingley et al. (2020) revealed that music interventions may improve cognition and well-being and decrease responsive behaviors of people with dementia and improve the experience and engagement of carers, as communication between patients and caregivers increases. Van der Steen et al. (2017) found in a Cochrane review that music activities and music therapy reduced expressions of responsive behaviors in people with dementia, and Pedersen et al. (2017) showed that agitation was decreased in music therapy sessions. Lineweaver et al. (2021) found that individual music listening had a short-term effect on decreasing responsive behaviors. Other studies have focused on singing, and Evans et al. (2017) showed that group singing increased social interactions and engagement in the activity during the sessions. Cho (2018) also revealed that singing sessions, compared to music listening sessions, were more favorably related to quality of life and increased positive affections. In sum, studies of music activities have been shown to have positive effects on persons with dementia as well as on caregivers, and it is suggested that future studies need to focus on long-term effects and positive outcomes, such as well-being and positive emotion (Clare & Camic, 2020; van der Steen et al., 2017). Reasons for responsive behaviors are multiple and include biological, psychological, and environmental variables (Tible et al., 2017), but responsive behaviors commonly appear during care situations involving interactions with caregivers, interventions that decrease the and facilitate care situation are a priority (Burley et al., 2022; Gutman et al., 2021).
Singing during care has been studied for decades, with a focus on facilitating care situations. In 2000, Götell et al. (2000) performed a residential context study on singing during caring, music therapeutic caregiving (MTC) or caregiver singing (CS), which is defined as “when the caregivers are singing for or together with persons with dementia during caring” (thereby named caregiver singing). Subsequently, several studies were conducted that focused on morning care situations, as responsive behaviors are common during these situations. The results revealed that morning care was facilitated as communication and cooperation increased while responsive behaviors decreased, and positive emotions such as laughing, smiling and singing increased (Engström et al., 2010, 2011; Götell et al., 2002, 2009; Hammar et al., 2010a, 2010b, 2011a, 2011b; Swall et al., 2020). In addition, the caregivers were influenced by singing (CS), as they described themselves as more relaxed and happy and less anxious of having to deal with possible aggression from the persons they cared for (Hammar et al., 2011c). Multiple studies focusing on different kinds of music interventions suggested that interventions should be person-centered (McCormack, 2004), which means that the music that is played or sung should be based on the person’s preference, and preferably from his or her youth, as persons with dementia tend to remember that kind of music (Spiro, 2010). Studies focusing on CS have included both persons with Alzheimer’s disease and persons with vascular dementia, but no studies have focused on possible differences regarding these diagnoses. As disabilities and symptoms may be similar in the diagnosis, there also differences. In Alzheimer’s disease, speech, time perception and hallucinations are common, while in vascular dementia, the symptoms depending on which part of the brain is affected, and the abilities of initiatives and to plan and perform different activities are decrease (Morley, 2018). Considering the differences, CS may have different effects and thus, the response to CS may differ in terms of expressed emotions and responsive behaviors such as resistance in different diagnosis. Therefore, this study will focus on possible differences depending on diagnosis, with aim to describe expressed emotions and resistiveness to care during CS to detect possible differences among persons with vascular or Alzheimer’s disease in residential care facilities.
Research Approach and Methodology
Design
A quasi-experimental design with pre-intervention and intervention measurements.
Sample and Setting
The participants were persons with Alzheimer’s and vascular dementia living at two residential facilities for persons with dementia in an urban area of Sweden. During an 8-week study period, (4-week preintervention and 4-week intervention), video recordings were made once a week of the interaction between each of the persons with dementia and their caregiver during morning care situations, yielding a total of 80 video observations capturing approximately 20 h of 10 to 20 min sequences. Focus was possible influences of CS on expressed emotions and resistance to care among persons with dementia focusing on possible differences regarding those diagnosed with Alzheimer’s disease and those with vascular dementia. The data has been used in several studies with different aims and the study protocol was described by Hammar (2011).
Participants
Study participants included persons with dementia and their professional caregivers. The head nurse in both of the facilities recruited 12 persons with dementia based on our criteria of having a dementia diagnosis in the severe stage (<12 in MMSE test) (Folstein et al., 1975) and expressing responsive behaviors. The inclusion criteria did not include the different diagnosis, as the data was initially for other studies. It was a coincidence that the participants had the different diagnosis, which evoke the research question for this study. The participants did not have the capacity to consent; therefore, proxy consent was obtained from relatives. During the study, two persons with dementia passed away. Among the 10 persons with dementia who completed the 8-week study, five persons were diagnosed by a physician with vascular disease, and five were diagnosed with Alzheimer’s disease.
The director of nursing in both facilities recruited six caregivers (three at each facility) who cared for the participating persons with dementia at baseline and during the intervention. The same dyads of person with dementia and caregiver participated during the baseline and intervention.
Preintervention – Caring the “Ordinary” Way
The baseline situation comprised an “ordinary” morning care situation, where caring was performed the usual way with no CS.
A typical morning care situation involved the caregiver helping the person with dementia from the bed into the bathroom, and the person sat down on the toilet and had their nightclothes taken off. The faces of the persons with dementia and their upper bodies were washed, and deodorant and skin lotions were applied. Clothes were placed on the upper body, and the lower body was washed (not video observed). Socks and shoes were put on, and the persons with dementia were led to the sink (three of them in wheelchairs) and directed toward the mirror. At the sink, their teeth were brushed (four of them by themselves), and their hair was combed (two of them by themselves). The morning care situation ended when the persons with dementia left the bathroom.
Preintervention Education
The education component took place two weeks before the intervention started. The six caregivers were all educated in caregiver singing with the same curriculum. The caregivers could either enroll in a university course and earn academic credit or complete the course without earning academic credits. The course curriculum included instruction on how to communicate with persons with dementia through singing, a good singing posture and how to be creative about determining the favorite songs of persons with dementia. The caregivers were taught to personalize the selection of songs so that they resonated and had personal meaning for the persons with dementia, for example, popular songs from their late teens and 20s, religious songs or typical Swedish sing-along songs. A booklet with different song texts and a CD with songs of different genres were provided to all caregivers.
Intervention
The intervention was developed after input from an advisory group with recognized experts in non-pharmacological interventions from academic institutions and healthcare professionals for persons with dementia from dementia care facilities with the purpose of identifying unmet needs in a field of music interventions, selection of songs, and length of the intervention. When the study protocol (Hammar, 2011) was developed it was reviewed by the same advisory group and also by two caregivers (not participating in the larger project) in residential care facilities for persons with dementia. Minor revisions were done; additional songs were included.
The singing intervention was carried out by the caregivers once per week for a four-week period. The same procedures as during pre-intervention situations was done with the exception that the caregivers were singing continuously for or with the persons with dementia while caring for them; that is, they practiced caregiver singing. The caregiver started to sing when he or she and the persons with dementia entered the bathroom, and the singing lasted until they left the bathroom. The caregivers chose which songs they preferred to sing.
Data Collection and Analysis
Two instruments were used to analyze the 40 preintervention and 40 intervention video recordings: the Observed Emotion Rating Scale (OERS) (Lawton et al., 1999a, 1999b) and the Resistiveness to Care Scale (RTCS) (Mahoney et al., 1999).
The OERS rates two positive emotions (pleasure and general alertness) and three negative emotions (anger, anxiety or fear, and sadness). Over a 10-min period, the rater chooses one of six possible defined time intervals (never, <16 s, 16–59 s, 1–5 min, >5 min, and not in view) to examine whether a person with dementia displays each of the five emotions.
The RTCS rates 13 observable behaviors (move away, pull away, push away, push/pull, grab object, grab person, adduct, hit or kick, say no, cry, threaten, scream or yell and clench mouth). Over a 10-min period, the rater chooses one of five defined time intervals (never, <16 s, 16–59 s, 1–2 min and >2 min) to examine whether a person with dementia displays each of the behaviors.
The video recording was independently analyzed by the first author and last author in three steps: 1) the PI analyzed all 80 recordings; 2) 10 days later, the PI reanalyzed the 80 recordings and tested the reliability/retest (agreement minus disagreement divided by the total observations yielded a reliability of 0,97); 3) the Co-PI analyzed all 80 recordings, and the PI and Co-PI results were compared. Out of the 80 observations, a disparity in the time interval scoring between the PI and Co-PI occurred for 15 observations (general alertness n = 5, anxiety/fear n = 3, pull away n = 4, adduct n = 2) (0.62) after reviewing the recordings together.
Statistical Analysis
The frequency and duration of each observable behavior and emotion were scored. Statistical analyses were performed using the IBM Statistical Package for the Social Sciences, version 27 (SPSS, IBM Corp, Armonk, NY, USA). Student’s t-test was performed to examine the differences in sample characteristics (age, length of nursing home stay) between the dementia diagnosis groups. All p values below .05 were considered indicative of statistical significance.
The study was approved by the Regional Board of Research Ethics in Uppsala.
Results
The sample consisted of six women and four men. The mean age for persons with Alzheimer’s disease was 79.8 years (SD 9.91), ranging from 66 to 92 years, and that for persons with vascular disease was 82.8 years (SD 6.97), ranging from 71 to 88 years (p = .595). The average length of nursing home stay was 23.0 months (SD 24.69), ranging from 1 to 60 months, for persons with Alzheimer’s disease and 27.8 months (SD 23.13), ranging from 5 to 66 months, for persons with vascular disease (p = .759). According to the Mini-Mental State Examination (MMSE) test (Folstein et al., 1975) administered prior to the preintervention period, four of the five persons diagnosed with Alzheimer’s disease had severe dementia (MMSE <9), and one had an MMSE score of 12, indicating moderate dementia (mean 4.2, SD 5.02). All persons with vascular disease had severe dementia, with MMSE scores <9 (mean 2.4, SD 3.59).
Figure 1 and Table 1 illustrate the OERS positive emotions during the morning care situation. Preintervention and during the intervention, positive emotions were more common among persons with Alzheimer’s disease than among persons with vascular disease. Among persons with Alzheimer’s disease, positive emotions during at least 1 min increased from 17 observations during the preintervention period to 30 observations during the intervention, in contrast to an increase from 10 preintervention observations to 19 observations during the intervention among persons with vascular disease.
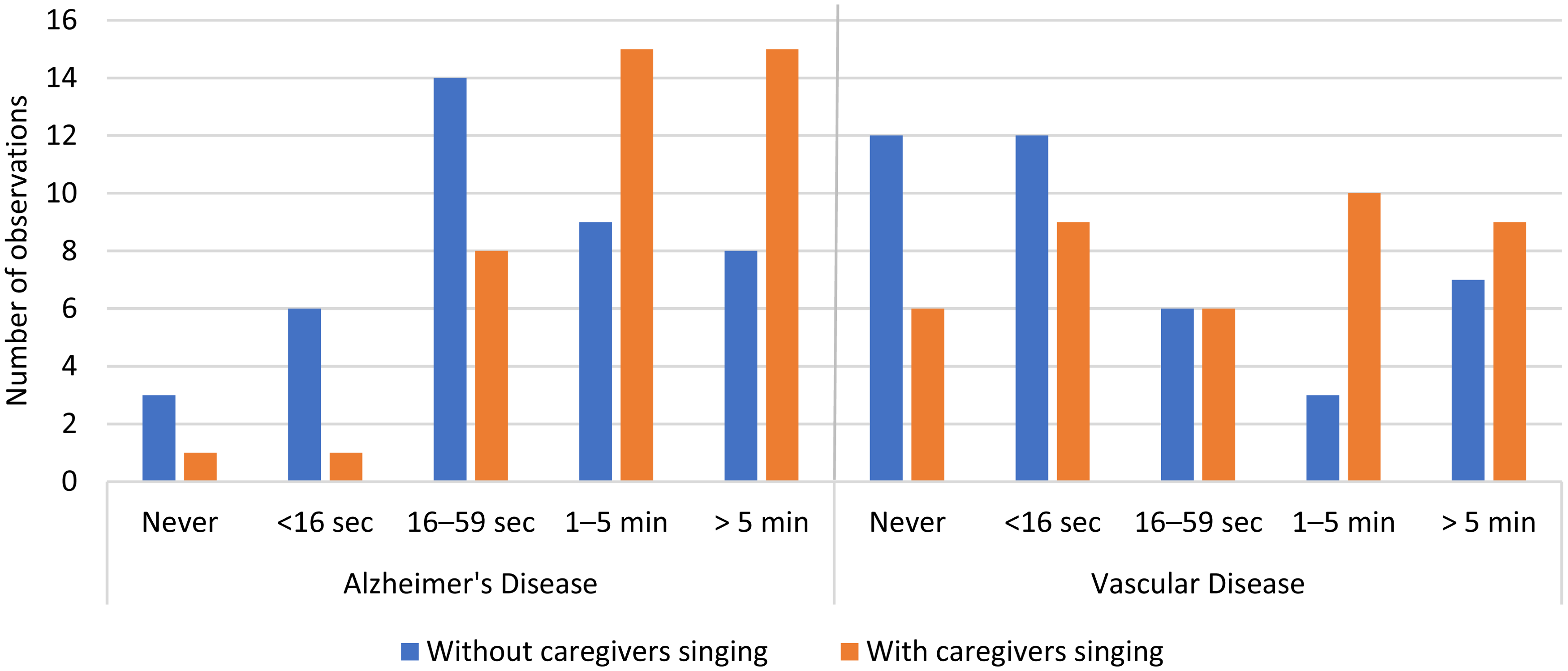
Number of positive emotions during morning care situations with and without caregiver singing in persons with Alzheimer’s and vascular disease.
Number of observations per score level during morning care situations with and without caregiver singing in patients with Alzheimer’s and vascular disease.
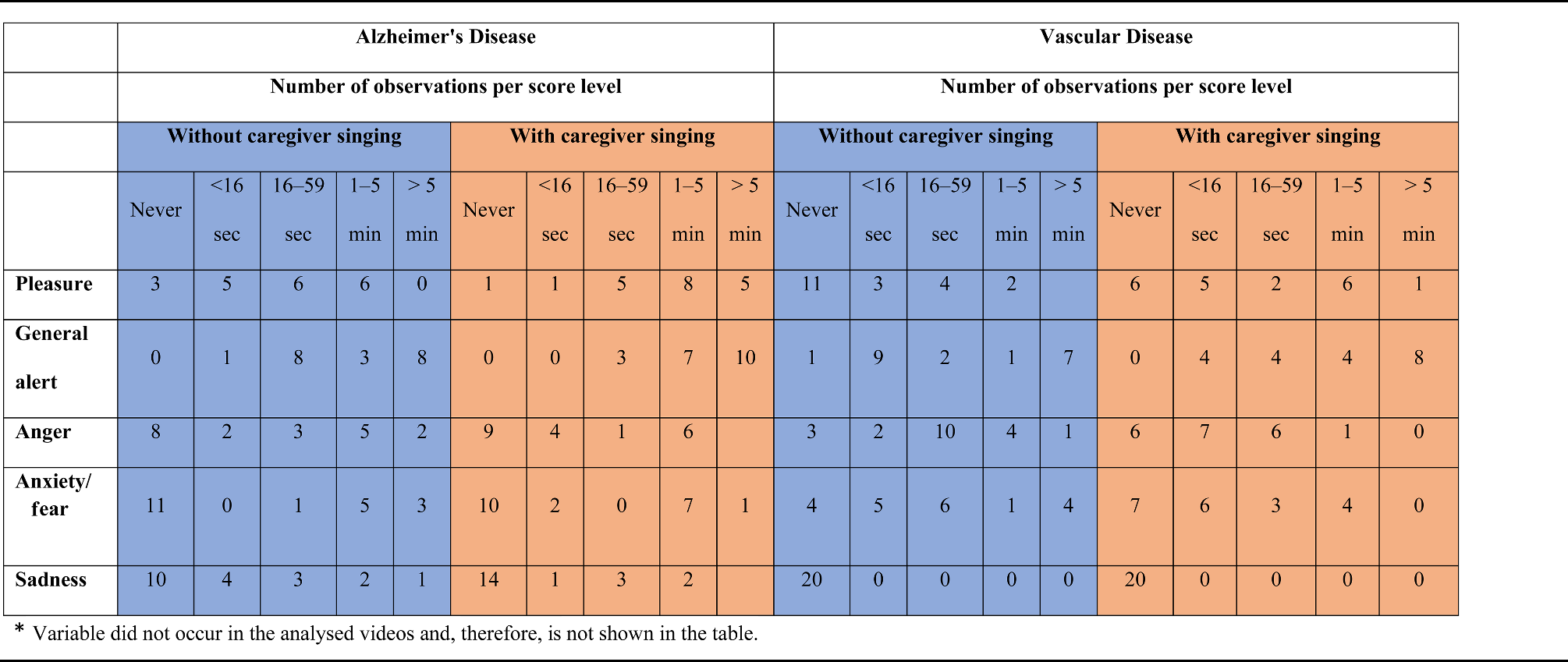
Caregiver singing interventions were associated with decreased negative emotions in the two dementia diagnosis groups. Among persons with vascular disease, for periods lasting at least 5 min, the negative emotions anger and anxiety were experienced during the preintervention period but never during the intervention, and the number of observations decreased from 6 to 1 for persons with Alzheimer’s disease (Figure 2

Number of negative emotions during morning care situations with and without caregiver singing in persons with Alzheimer’s and vascular disease.
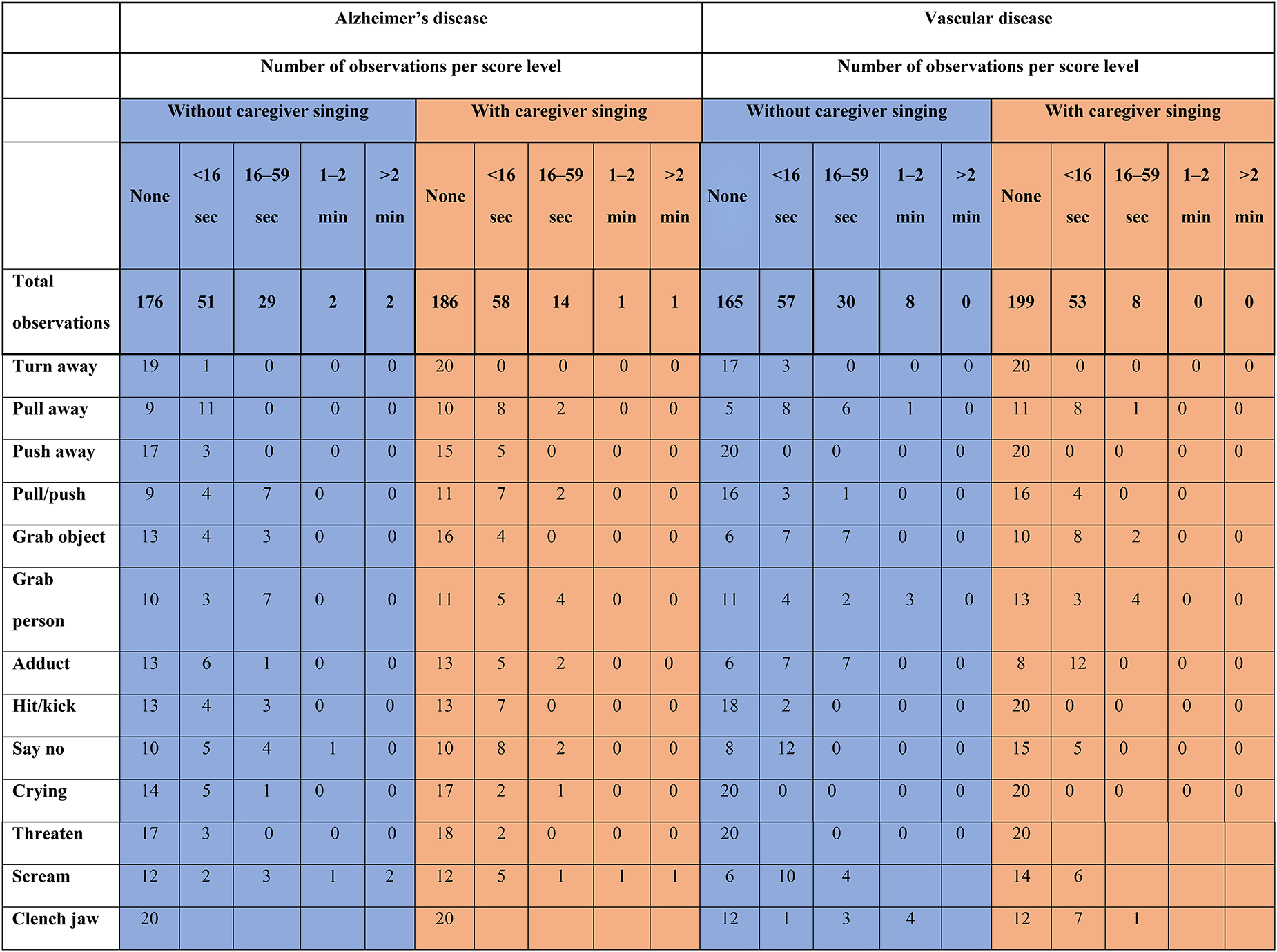
Table 2 illustrates the 13 observable RTCS behaviors during morning care situations. During the preintervention period, persons with vascular disease were observed to have a higher frequency and longer duration of negative behaviors than persons with Alzheimer’s disease. During the intervention, the reduction in negative behavior observations was greater for persons with vascular disease (from 95 to 61) than for persons with Alzheimer’s disease (from 84 to 74). Among persons with vascular disease, for periods of at least 1 min, the negative behaviors pull away, grab person, and clench mouth were not observed during the intervention.
Number of observations per score level during morning care situations with and without caregiver singing in patients with Alzheimer’s and vascular disease.

Discussion
Despite there being different dementia diagnoses, persons with dementia are commonly identified as a single group. There are of course many similarities such as communication difficulties, anxiety, confusion etc. (Morley, 2018), but as symptoms may also differ, so may responses to treatment. Our results revealed that persons with Alzheimer’s disease and vascular disease differed in expressed emotions and resistiveness to care both at baseline and during a CS intervention. During CS, positive emotion increased for both groups; however, far longer intervals of positive emotions were observed among persons with Alzheimer’s disease. Previous research did not focus on differences between dementia diagnoses, but much research has involved persons with Alzheimer’s disease, as it is the most common diagnosis. The benefits of music have been described previously regardless of diagnosis and confirm our findings, for example, Skingley et al. (2020) and van der Steen et al. (2017), as has other research on CS (Hammar et al., 2011a; Hammar Marmstål, 2011; Swall et al., 2020). These studies also confirm our findings on the decrease in resistance and expression of negative emotions, which was seen in both groups. In term of differences between the two groups, those with vascular dementia showed a decrease in expression of negative emotions and resistance to a greater extent than those with Alzheimer’s disease. However, which is better is debatable: the occurrence of negative emotions for shorter periods but at a higher frequency or the occurrence of negative emotions less frequently but for longer periods. Nevertheless, negative emotions were reduced to a greater extent for those with vascular dementia, and thus this might be a valuable consideration when planning care and using CS to facilitate care situations.
For both persons with Alzheimer’s and those with vascular disease, positive emotional pleasure was never observed during the morning care situation without CS, while with CS, emotional pleasure increased five times for persons with Alzheimer’s disease for periods of more than 5 min. Furthermore, the positive emotion general alert occurred at a higher frequency and for longer periods of time during morning care situations with CS for persons with Alzheimer’s disease than for persons with vascular disease. At baseline, the caregivers communicated using normal speech; however, O’Callaghan (1993) and Stewart et al. (2006) suggested that music gain access to different parts of the brain based on the elements involved, such as rhythm and melody. Language is a function of the left hemisphere, and a combination of language and music, as in singing, offers a greater chance of activating intact neurological pathways than using language alone (Stewart et al., 2006). This may explain our results. Previous studies of CS revealed that interaction was increased and that caregivers as well as persons with dementia experienced more positive emotions (Hammar et al., 2010a, 2010b, 2011a, 2011b). Thus, an increased interaction of the dyad may have in turn decreased negative emotions and increased positive emotions in our present study.
In sum, the effects of CS observed confirm the findings of previous studies of CS as described previously, as well as the literature on music activities with persons with dementia (Evans et al., 2017; Pedersen et al., 2017; van der Steen et al., 2017). However, Cho (2018) found that singing was preferable to music listening, as did Swall et al. (2020). Previous studies (Engström et al., 2011; Hammar et al., 2010a, 2010b, 2011a) also found increased communication and cooperation between persons with dementia and their caregivers during CS, which is important as it facilitates the care situation. Future studies may also focus on differences in interactions during CS according to diagnosis, as CS may work better or worse depending on the diagnosis.
Our results also showed a decrease in the variable grabbing person, and hitting/kicking disappeared completely during CS, confirming previous findings of caregivers describing that during CS, they did not have to defend themselves as aggression from the persons with dementia was decreased or stopped (Hammar et al., 2010a, 2010b, 2011a, 2011b, 2011c; Swall et al., 2020). This study thus adds to the growing body of literature that identifies caregiver working situations, and CS could be suggested as an easily accessible but powerful tool, both in terms of increasing moods and interaction with the person with dementia and in terms of facilitating the work situation with a focus on personal actions.
Methodological Considerations
A strength of this study is that although the behaviors and emotions of persons with dementia can vary between and within days, morning care routines occurred at the same time for the pre- and intervention assessments. We also had the same dyad of persons with dementia and caregivers to avoid any differences regarding their interactions. Other strengths are that the persons with dementia served as their own controls, with four separate baseline and four separate intervention observations, and that the scoring of the observations was done by several researchers on several occasions.
A limitation of the study is that the head nurses of the recruited care facilities requited the persons with dementia of the study. However, the head nurses were only asked to select them based on the severity of their dementia and that they expressed responsive behaviors. Based on our experience, we think that a head of nursing is an appropriate person to perform recruitment of the persons at residential care facilities we included in the pilot study, as they meet and interact with the persons with dementia and have good knowledge of their responsive behaviors.
The major limitation of this study is the small number of participants in each dementia diagnosis group. Future studies should include a larger number of participants and additional care situations such as meal-time situations, to see if CS effectively improves behaviors and emotions and reliable conclusions can be drawn. This study is a pilot study and as a basis for designing future larger studies, and thus no general conclusions may be drawn from its findings. Another limitation is that in the later stage of the disease for the participants in this study, Alzheimer’s disease and vascular dementia may develop similar symptoms, and thus it may not be valid to compare the diagnosis. Thus, it may be more interesting to conduct studies with CS involving persons in the earlier stage of the diseases in the future.
Implications
Knowledge about the benefits of CS is generally low among staff and at the managerial level, as CS is commonly interpreted as a pleasant activity and not a tool to increase interaction and facilitate caring. Thus, organizations would benefit from increased knowledge about CS and its benefits. Thus, CS should be included in nursing training at different levels, and awareness of this affordable and powerful tool should be raised. However, as our study found differences in the expressions during CS regarding the different diagnosis, larger studies should be done to further analyze this and if our results are confirmed it may be a useful implication when using CS in the care of persons with dementia
Conclusion
The results of this pilot study confirm the large body of literature on the positive effects of music activities and CS and the possibilities of CS as a tool to facilitate challenging situations. We can conclude that regardless of dementia diagnosis, CS reduces negative behaviors and emotions and increases positive behaviors but showed potential to have greater benefits on those with vascular disease. The effects of CS for persons with different dementia diagnosis are worthy of further examination and development.
Supplemental Material
sj-docx-1-mns-10.1177_20592043221120386 - Supplemental material for Caregiver Singing Intervention: Do Expressions of Emotion and Resistance Differ Between Persons with Vascular Dementia and Those with Alzheimer’s Disease? A Pilot Study
Supplemental material, sj-docx-1-mns-10.1177_20592043221120386 for Caregiver Singing Intervention: Do Expressions of Emotion and Resistance Differ Between Persons with Vascular Dementia and Those with Alzheimer’s Disease? A Pilot Study by Lena Marmstål Hammar, Sanne Messelt Wickberg, Marie Skogsbäck and Gabriella Engström in Music & Science
Footnotes
Acknowledgements
We wish to thank the persons with dementia that participated in this study. We also wish to thank Associate Professor emerita Eva Götell, who was the primary investigator of the project where this study was executed.
Action Editor
Orii McDermott, University of Nottingham, Institute of Mental Health, School of Medicine.
Peer Review
Becky Dowson, University of Nottingham, Institute of Mental Health.
Kendra Ray, NYU Langone, Department of Rehabilitation Medicine.
Contributorship
Study design: LMH, SM, MS, GE; Data collection: LHM, GE; Data analysis: GE, SM, MS, Drafting of the article: LMH, SM, MS, GE.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Supplemental Material
The supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.