Abstract
Most sperm banks in the United States continue to process and freeze samples in “open” cryovial devices. Yet, due to growing European attention to the long-term cryostorage of gametes and embryos in an aseptic manner, we evaluated the possibility of repackaging cryovials into a sealed (i.e. closed) “CryoCocoon™”container, when distributing donor sperm vials to countries with aseptic container cryostorage restrictions. We conducted a series of controlled, prospective experiments to validate the efficacy of the CryoCocoon™ concept. Cryovials were securely repackaged within 45 s under ambient conditions while maintaining sub −100°C temperatures, before refreezing, without adversely influencing post-thaw motility. However, unique challenges in terms of container buoyancy, cryocane storage and labeling condensation had to be overcome. Although not particularly ideal to the long-term storage of pathogen-free donor sperm vials, CryoCocoons™ constitute a novel approach to the creation of an aseptic storage container for previously frozen sperm that conforms with closed-system regulations. In addition to possible short-term donor sperm cryostorage in countries implementing aseptic storage restrictions, CryoCocoons™ may prove particularly useful in clinics using sperm cryovials for the effective isolation of “pathogenically at-risk” semen samples.
Introduction
Sperm have been successfully cryopreserved and stored in sperm banks for over a half century. Beginning in the late 1970s, human sperm banks in the United States primarily adopted the use of plastic cryovials, similar to standard tissue culture laboratory practices. These cryovials are considered “open” devices because the gaskets sealing the plastic cap typically undergo thermal contraction during subzero cooling/freezing, which allows for Liquid Nitrogen (LN2) seepage into the container. However, the pathogenic cross-contamination of gametes or embryos stored in LN2 has never been documented under standard cryobanking conditions (Pomeroy et al., 2010). Nevertheless, the seminal fluid of ejaculates is known to be a significant vector for pathogens and infectious viruses (Bielanski, 2006) and represents a potential risk to contaminating LN2 when stored in open systems (Bielanski and Vatja, 2009). Furthermore, the liquid phase of LN2 is at risk of accumulating airborne contaminants overtime, placing open system containers/devices at risk of contamination (Bielanski, 2007; Bielanski et al., 2003). Thus, aseptic laboratory practices warrant continued mindfulness to minimizing potential cryostorage risk factors.
The freezing and cryostorage of bull sperm in the animal agriculture industry adopted the use of sealed 0.25–0.5 ml plastic straws, which facilitated direct, on-farm artificial insemination procedures. Secondarily, since cattle produce more concentrated, larger ejaculate volumes than men, thus the greater storage capacity of straw containers for cryobanking was more desirable. The need for an aseptic, closed container system in the agriculture industry was historically prompted by risk analyses regarding the possible spread of catastrophic disease(s) (e.g. foot and mouth disease), previously eradicated in the United States and Europe. Import–export regulations have been adopted by the United States Department of Agriculture (USDA) and the Office International des Epizooties (OIE) to prevent the widespread transmission of disease, whether by live animals or frozen gametes and embryos (Stringfellow and Givens, 2009). After a decade of growing concerns over sexually transmitted diseases (e.g. HIV, hepatitis B and C), in the mid-1990s, some European countries (e.g. France) began mandating the use of sealed plastic straws for the cryobanking of human sperm. This measure seemed particularly unnecessary in the case of the cryobanking of disease screened, quarantine tested sperm donors. Yet, the appearance of untestable disorders like Creutzfeldt–Jakob disease in Europe may have heightened concern over the need for preventive measures, whether justified or not. The latter suggested regulations have never been imposed in the United States, as the latter disease transmission concerns have never materialized or been proven. Granted, such risk assessments are warranted and justified for individuals whom test positive for sexually transmitted diseases.
In line with the European Union’s Tissues and Cells Directive, the prior laboratory guidelines supported by the European Society for Human Reproduction and Embryology (ESHRE) eluded to the use of aseptic cryo-practices and that “all gametes and embryos should be stored in specific receptacles that can be sealed effectively” (section 12.3; ESHRE; Magli et al., 2008). More recently, the latter description was modified to allow the use of “open device” systems (ESRHE, 2015), undoubtedly to accommodate proven oocyte vitrification practices. Today, specific regulations vary by country, however, most reputable fertility clinics throughout Europe strive to maintain aseptic container systems (e.g. CBS™ straws for semen), especially as it pertains to frozen semen samples. To control and alleviate concerns over the cryostorage of sperm cryovials, and to facilitate marketing efforts in Europe from the United States, we developed a secondary containment system called the CryoCocoon™ which encapsulates frozen vials and is hermetically heat sealed. The purpose of this study was to validate the safety and effectiveness of this containment system.
Materials and methods
Experimental design
A series of four prospective experiments (expt) were conducted. In expt 1, the slow warming rates of rapidly cooled cryovials at ambient temperature were determined. Using an apriori arrangement of treatment volumes (0.25, 0.5, or 1.0 ml), repeated warming temperature measurements (n = 5 replicates) were performed/treatment cryovial volume (n = 15 samples). In expt 2, the post-thaw total motility of 60 cryovials frozen in control vials (CV) or with CryoCocoon™ (CV-CC) treatments, or warmed and repackaged in a CryoCocoon™ (CC; 20 vials/treatment) was compared (Figure 1). In expt 3, six batches of sperm quality control (QC) vial lots (n = 2/lot) were placed into CryoCocoons™ post-freeze and shipped to Brussels for prospective, independent post-thaw analysis. The latter results were then contrasted to mean control QC vial results generated in a prospective external proficiency testing study (n = 13 labs; unpublished data). Finally in a fourth prospective survey, 20 more vials were sent to Brussels for further independent evaluation (n = 4 technicians) of: (1) CryoCocoon™ security on canes, (2) completeness of seals, (3) label readability (LR; post-shipment and in storage) and (4) ease of cutting CryoCocoons™ to remove the cryovial.
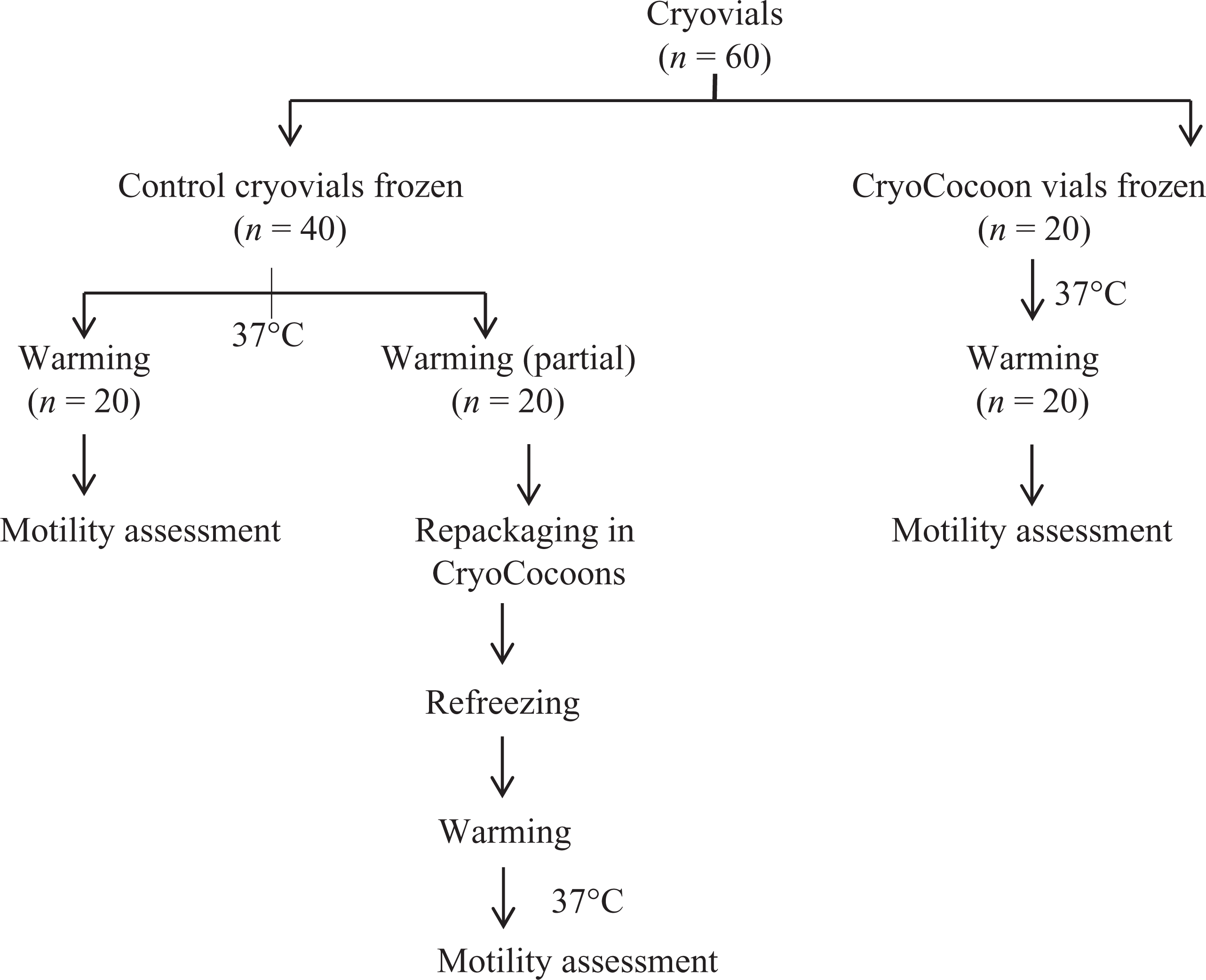
CryoCocoon™ expt 2: Assessing the influence of encapsulating cryovials before or after freezing sperm on subsequent post-thaw motility. expt: experiment.
Statistical analyses were performed with the assistance of QI Macros Excel software (KnowWare International, Inc., Denver, Colorado, USA). Analysis of variance with repeated measures was used to assess differences in temperatures (expt 1) and sperm concentrations in expts 2 and 3. Furthermore, χ 2 tests were performed to determine all differences in post-thaw motility (p < 0.05).
Control cryovial processing
Semen samples were acquired from residual potential donor samples after qualification testing in our Branch Laboratory, located in Westwood, California. All ejacuates were diluted with human tubal fluid (HTF) + 5% human serum albumin (HSA) sperm wash medium (2:1, v/v) for up to 3 h at ambient temperature on a slow rotating shaker. The pooled samples were washed on 2 ml 90% Isolate® density gradients (Irvine Scientific, Santa Ana, California, USA) for 15–30 min (centrifugation at 1500 × g). After an additional rinse and dilution wash in sperm wash medium, samples were diluted to create 15–40 vials of sperm. Samples used in expts 3 and 4 were specifically created for use in a 2012 internal/external QC study, which is the subject of a separate publication in preparation.
Prior to vialing, each 1.0 ml of sample was dropwise diluted with 0.3 ml of 26.7% glycerol/HSA-containing freeze medium (InVitro Care, Frederick, Maryland, USA) over a 7–10 min duration. All vials were labeled as QC vials, given a batch date and assigned a sequential number within batch. The vials were placed onto labeled canes within 30 min post-initial freeze medium exposure and placed into LN2 vapor phase for 30 min prior to placement in liquid LN2 storage.
CryoCocoon™ preparation and handling
In expt 1, a hole was made in the center in each cryovial cap and a wire thermocouple inserted into the base of each vial (five vials/treatment). Vials were then placed on a cane, frozen and upon warming at ambient temperature (21°C) an initial temperature (°C) was taken, followed by recording the sample temperature each 15 s for 60 s. In expt 2, two batches of 30 vials (CV#1 and #2) were prepared from diluted, washed ejaculates, and two-thirds of the vials were packaged in CryoCocoons™ either before (CV-CC; n = 20) or after (n = 20) freezing (CC), as explained in the study design. Residual QC vials were assigned to CryoCocoon™ treatment processing in expts 3 and 4.
CryoCocoon™ formation
Cryostored vials were extracted from LN2 to ambient conditions and allowed to outgas nitrogen vapor (up to 30 s), before insertion into the open end of a pre-sealed 7 cm section of polypropylene tubing (i.e. CryoFlex, Nunc; Fertility Technology Resources, Marietta, Georgia, USA), hermetically sealed and refrozen. Effective heat seals were achieved using an impulse sealer and reverse sealing technique on opposite surfaces at ambient temperature. The aseptic CryoCocoons™ were cryostored, three CryoCocoons™ per 28 cm long cane with a weighted vial (containing cooper beads) on the base to counterbalance the buoyancy of each CryoCocoon™ (Figure 2). The partially thawed CryoCocoon™ vials were then refrozen by direct exposure to LN2 and cryostored.
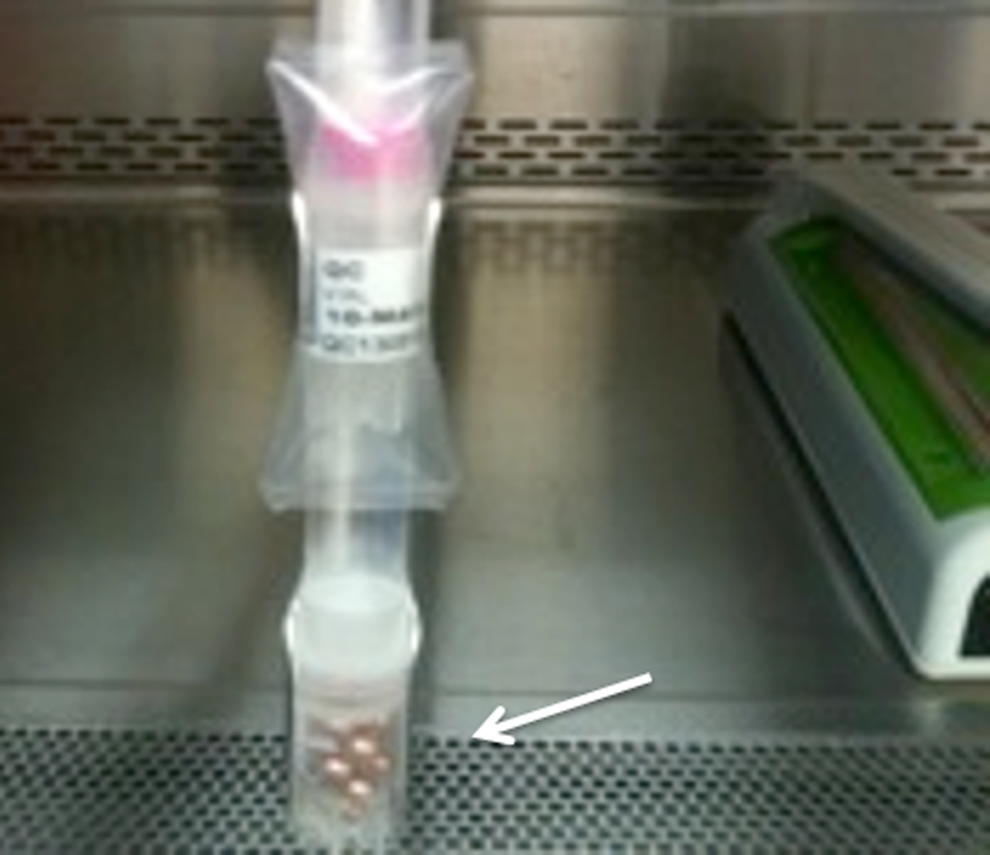
Image showing the secure placement of CryoCocoons™ attached to an aluminum cane, counterweighted with a cryovial-containing cooper ball bearings (as indicated by white arrow) to offset buoyancy in LN2 storage.
CryoCocoon™ shipment and storage
The canes were shipped in LN2 vapor tanks, via international courier, to the UZ-Brussels laboratory. Upon arrival, the CryoCocoon™ canes were stored in an empty metal canister or in between CV-cryosleeves and visotubes for secure short-term storage in a standard 35–40 l LN2 tank.
CryoCocoon™ thawing
(1) The cane was briefly exposed to ambient conditions and a CryoCocoon™ removed; (2) using a cigar cutter, the CryoCocoon™ sleeve was cut just above the label by holding it tightly with the blades while simultaneously twisting the vial 360°; (3) the vial was pulled upwards and removed from its encasement and (4) each CV was thawed in a 37°C water bath for 10 min. The CryoCocoon™ removal process can be visualized on a YouTube video (https://www.youtube.com/watch?v=2bN_kz6G9QQ).
Results
As expected, an inverse relationship between warming rates and cryovial volume was observed (expt 1; Table 1). Although the warming rate after 60 s was reduced (p < 0.05) for 1.0 ml volumes (0.93°C s−1) compared to 0.5 ml (1.14°C s−1) or 0.25 ml (1.2°C s−1), warming slowed in all groups around an estimated −120°C. In turn, all groups maintained a temperature of at least −100°C at 60 s.
Static measurements of cryovial warming (a), by volume, over a 1 min exposure to room temperature conditions (expt 1).
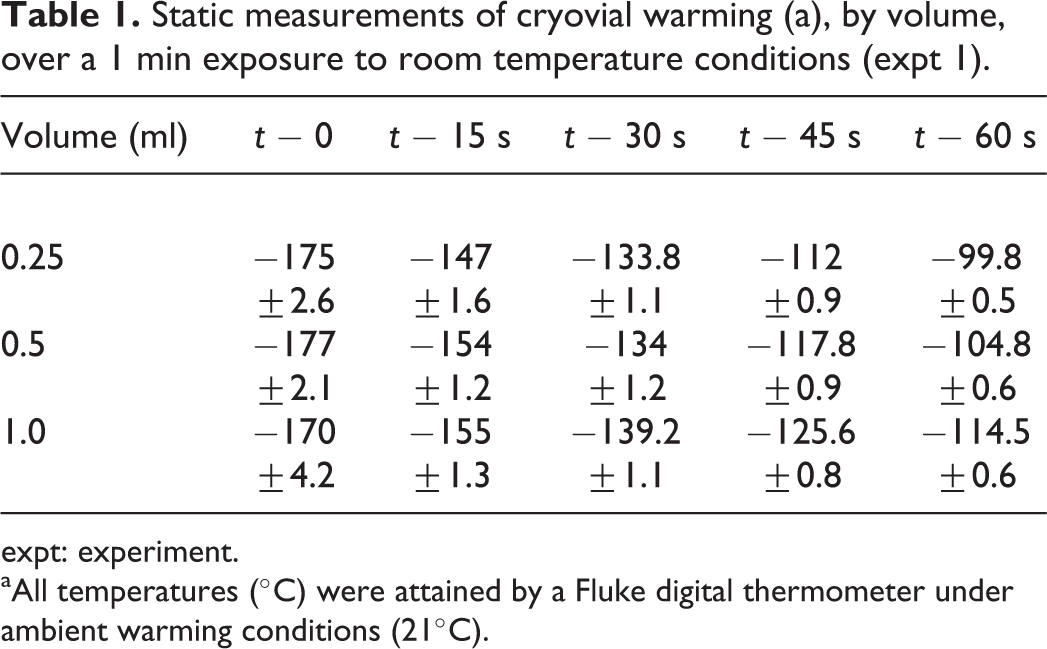
expt: experiment.
aAll temperatures (°C) were attained by a Fluke digital thermometer under ambient warming conditions (21°C).
Upon ambient temperature exposure, LN2 vapor outgassing was typically complete within 30 s. Therefore, in the preparation of frozen CryoCocoon™ vials, it took an average of 45 s to repackaged and freeze aseptic cryovials in expt 2. In contrast to control vials (CV) and ambient temperature, prefrozen CV-CC vials, no difference in the post-thaw motility of CryoCocoons™ vials was observed (53.3 ± 12.4, 52.6 ± 11.1, and 53.5 ± 11%, respectively; Figure 3). It was also determined that no inter-batch variation existed (CV#1 vs. CV#2), thus validating the combined mean assessments of both batches. In addition, no CV vaporization was observed in either CryoCocoon™ group, confirming the patency of the heat seals which prohibited LN2 seepage into vials.
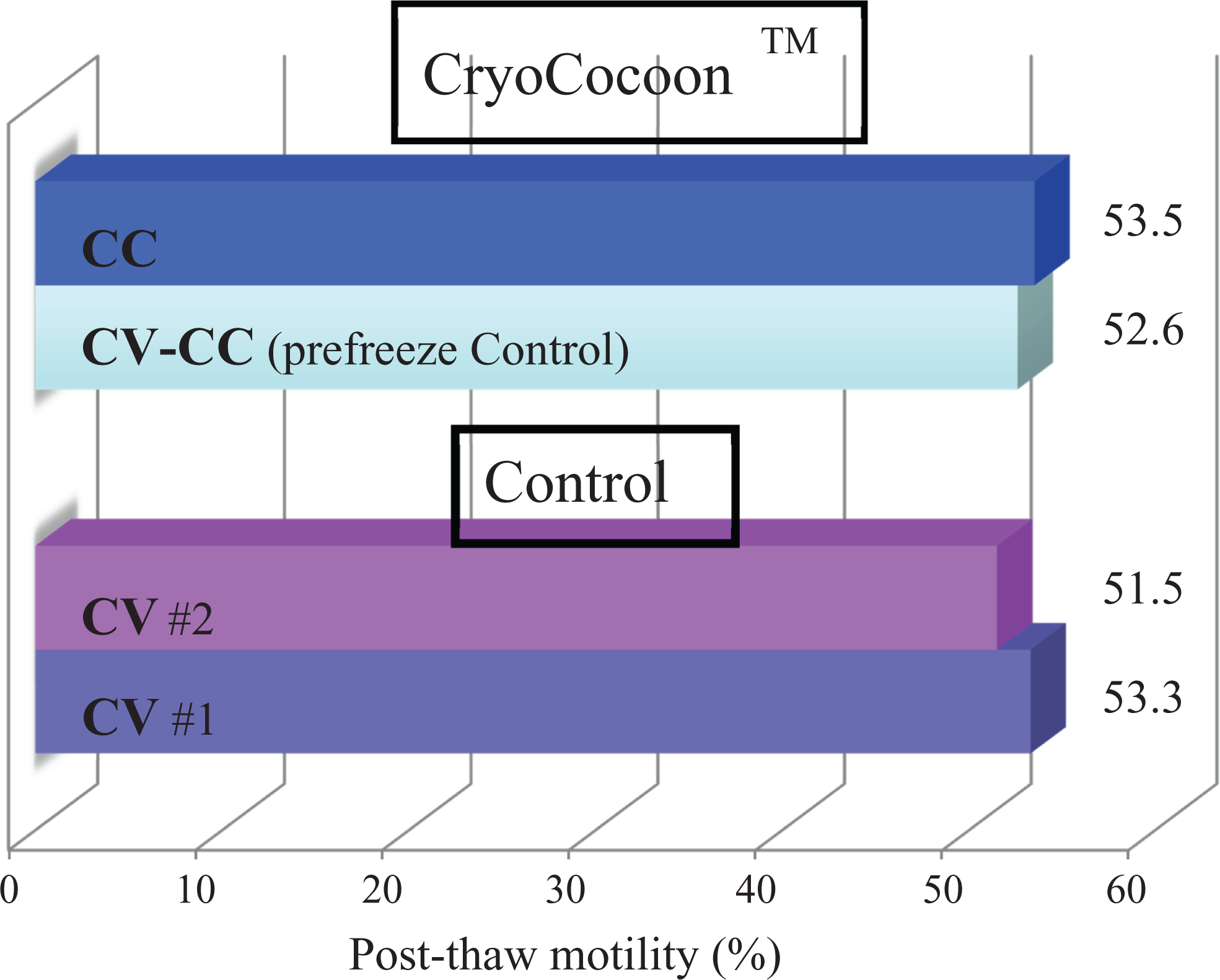
Expt 2 results exhibiting the mean post-thaw motility results of two different batches of quality control cryovials (CV), contrasted the CryoCocoon™ preparation prefreeze (CV-CC) or post-warming/refreeze (CC). No differences in sperm viability were detected between treatments.
The same pattern of CryoCocoon™ success was prospectively exhibited post-shipment by our colleagues in Brussels. Following the post-thaw assessment of 12 vials in expt 3, only one of six lots tested had a lower motility than the external controls (Table 2). Alternatively, five of the six lots favored CryoCocoon™ vials, with an overall motility SD index advantage of +0.52 for the CryoCocoons™ group. The CryoCocoon™ vials were equally viable to QC-CV controls, having a similar mean post-thaw motility (i.e. only 3.7% higher), based on assessments made by more than 20 independent evaluators. Overall, there was less than 1 standard deviation of variation for control vials repackaged in CryoCocoons™ and evaluated in Brussels for sperm concentration (−0.78) or motility (+0.52), constituting 11.8 and 5.5% variation, respectively. These results prospectively confirmed that there was no detrimental effect to CryoCocoon™ refreezing within a 45–60 s of ambient exposure.
A general lack of difference was observed between mean QC vial results attained in an external study (n = 13 sites; i.e. control group) or QC vials encapsulated in CryoCocoons, shipped to and thawed in Brussels, Belgium for evaluation (n = 4 technician assessments per QC sample).
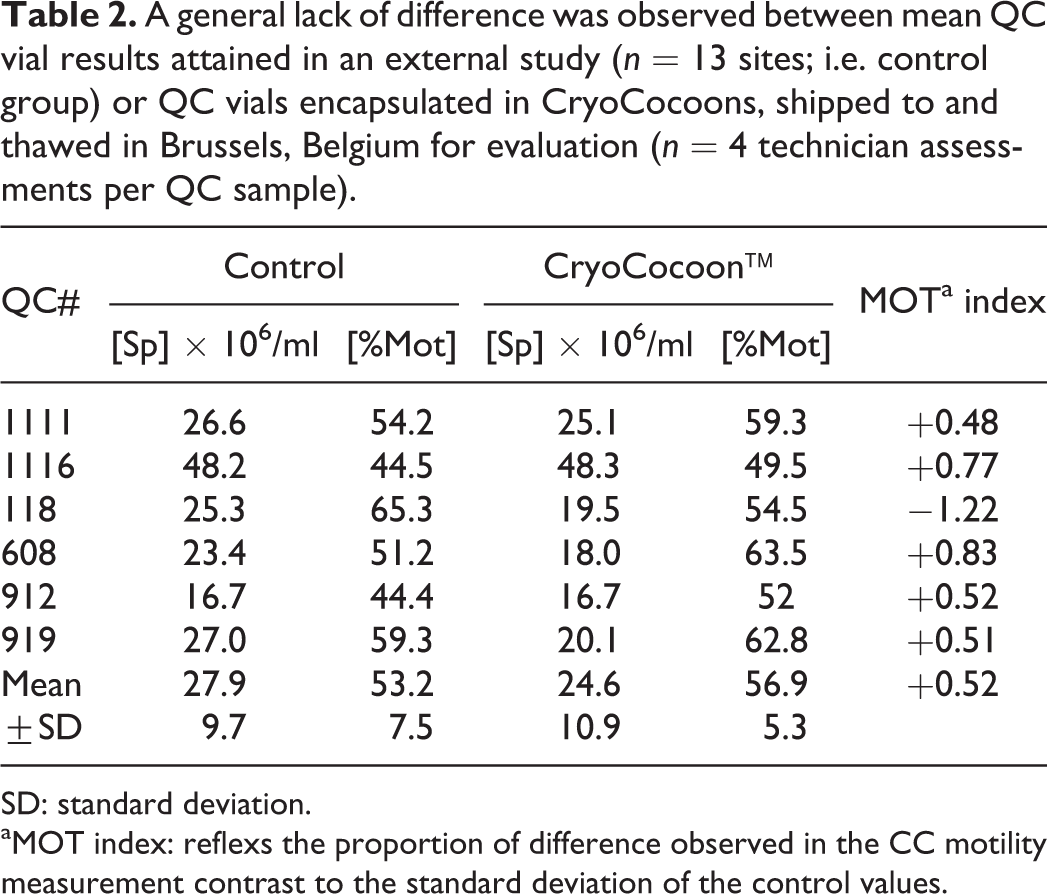
SD: standard deviation.
aMOT index: reflexs the proportion of difference observed in the CC motility measurement contrast to the standard deviation of the control values.
In expt 4, four different technicians objectively assessed the efficacy of CryoCocoon™ seals, LR, storage security and the ease of opening frozen CryoCocoon™ packaging. All CryoCocoon™ seals were complete without evidence of LN2 seepage (expts 2–4, n = 72 CC). On a scale of 1–10 (10 = clear, easy to read), mean label clarity pre-shipment was 9.0 (Figure 2), which did not change on arrival (8.9) or in storage (8.9). It was noted that a little condensation could occur at upon warming at ambient temperature but generally cleared up before vial removal from the CryoCocoons™. Ninteen of 20 vials were secure to canes post-shipment, indicating more QC of canes pre-shipment (i.e. tightening metal grip) was needed to improve reliability of storage security. Furthermore, the flanging of the heat seals limited CryoCocoon™ storage on canes as they had to fit between, not inside, cryosleeve or visotube dividers, which was deemed suboptimal. Finally, the ease of opening CryoCocoons™ varied by technician but improved with experience (ex: 4, 7, 7, 8, 9, 9, and 10). Little, if any, difficulty was experienced by most individuals after a single attempt.
Discussion
Independent of volume, frozen cryovials were surprisingly stable under ambient exposure conditions for the 45–60 s needed to aseptically repackage them in CryoCocoon™ containment. Even at low volumes (0.25 ml), samples maintained −100°C internal temperatures. A slight decrease in the warming rates of all volumes was detected around the known temperature (approximately −120°C) where ice crystal reformation begins occurring upon warming. The significance of recrystallization was proven to be negligible in 0.5 ml volumes, based on intra- and inter-facility post-thaw assessments in both expts 2 and 3, respectively. Overall, the repackaging of donor sperm vials into aseptic containers called CryoCocoons™ proved to be an excellent alternative for the safe and secure storage of unsealed frozen vials, without any change in the post-thaw motility status of sperm specimens.
Sample viability is of critical importance, but it is not the limiting factor influencing the successful implementation of CryoCocoons™ into clinical practice. Unique and challenging concerns were encountered in the handling and storage of CryoCocoons™. In the developmental phase, we learned that the outgassing of cryovials previously stored in LN2 had to be considered for quality control and safety purposes before packaging. Any attempt to quickly package and seal before vaporization of retained LN2 resulted in CryoCocoon™ gas expansion and seal rupture. Furthermore, it was unsafe to handle these vials while vaporization was occurring, if finger-tip burns were to be avoided. The next problem encountered was that without vacuum aspiration of dead airspace inside the CryoCocoon™ upon sealing, these containers are buoyant. Unfortunately, the application of heated shrink-wrapping was not a realistic option for us, as direct heat would have adversely influenced the degree of sample thawing and likely specimen viability. In turn, we choose to counterweight the cane with a vial filled with cooper ball bearings on the bottom (Figure 2). The latter measures also limited the storage capacity of CryoCocoons™ on a cane to three vials. Furthermore, the non-heat shrunken CryoCocoon™ seal created a flange, which also reduced the storage of CryoCocoons™/canes in a canister, by prohibiting their insertion into a standard cryosleeve. In contrast to the common use of straws for semen storage throughout Europe, and other parts of the world, five cryovials/cane already reduces the storage capacity of specimens in a single LN2 dewar tank. Therefore, the use of CryoCocoons™ for sperm is not ideal for long-term storage but instead is intended for the short-term storage use of active IUI and IVF cycling patients. Alternatively, CryoCocoons™ may be beneficial for pathogen containment of at-risk samples (i.e. STD positive directed donor or partner), where biosafety concerns outweigh storages issues. Obviously, if an individual is known to be an at-risk carrier of an STD, the use of weld sealed CBS™ straw containers would be preferred for long-term storage.
In the developmental phase of CryoCocoon™ packaging, we learned that LR was distinctly improved if each vial was wiped free of condensation upon outgassing, before insertion and when sealing it into a CryoCocoon™ container. The overall clarity of sample identification was considered good to excellent by all technicians, once the condensation issue identified in Study 3 had been averted. Upon warming, the simple use of a cigar cutter proved efficacious for the easy removal of cryovials from the CryoCocoons™. With increasing ease and proficiency of removal being based on experience, the learning curve proved to be minimal.
The use of CryoFlex tubing to aseptically seal and cryopreserve cryovials containing ovarian tissue has become a standard freeze preservation practice (Amorim, 2013; Dolmans et al., 2013), where the sterility of tissue preservation laboratory practices is more highly regulated compared to oocytes alone. In our study, we have now demonstrated that previously frozen sperm can be effectively repackaged in a similar manner, referred to as CryoCocoons ™. As the use of individual sperm donor samples becomes more restrictive in European countries and the availability of preferred donors reduced, the large inventory of California Cryobank sperm donors from the United States may become an attractive option. CryoCocoons™ offer an alternative approach to the aseptic shipping and short-term storage of US-produced cryovials for intrauterine or in vitro insemination in countries imposing strict aseptic storage practices.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
