Abstract
Background
The newly adopted European directive DE59/2013 mandates adequate patient information in procedures involving ionising radiation. Patient interest in knowing about their radiation dose and an effective communication method for dose exposure remain poorly investigated.
Purpose
This study is aimed at investigating both patient interest in radiation dose and an effective method to communicate radiation dose exposure.
Material and methods
The present analysis is based on a multi-centre cross-sectional data collection involving 1,084 patients from four different hospitals ‒ two general and two paediatric hospitals. Anonymous questionnaires were administered, consisting of an initial overview of radiation use in imaging procedures, a patient data section, and an explanatory section providing information in four modalities.
Results
1009 patients were included in the analysis, with 75 refusing participation; 173 participants were relatives of paediatric patients. Initial information provided to patients was considered comprehensible. The information modality with symbols was considered the most readily understandable format by patients, with no appreciable differences in comprehension attributable to social or cultural background. The modality including dose numbers and diagnostic reference levels was preferred by patients with higher socio-economic background. The option ‘None of those’ was selected by one-third of our sample population, composed of four different clusters: female, over 60 years old, unemployed, and from low socio-economic backgrounds.
Conclusions
This study demonstrated a high level of interest amongst patients in knowing about radiation dose exposure. Pictorial representations were well understood by patients from a variety of different ages and education levels. However, a universally comprehensible model of communicating radiation dose information remains to be elucidated.
Introduction
The increased use of radiological procedures for diagnostic and therapeutic purposes has produced a heightened interest in understanding radiation dose exposure in both patients and the general population. Organisations such as the International Atomic Energy Agency (IAEA), the American College of Radiology (ACR), and the European Society of Radiology (ESR) are working to limit the steadily increasing cumulative dose of radiation. Radiation exposure is regulated by several principles outlined in the European Directive 2013/59/EURATOM of 5 December 2013. 1 These principles are based on scan justification and radiation dose optimisation in line with Diagnostic Reference Levels (DRLs). The Italian government has recently adopted (101/2020) European directive DE 59/13, which mandates the inclusion of radiation dose information in radiological reports. 1 Furthermore, the IAEA and World Health Organization (WHO) emphasise the role of radiologists in informing patients about the potential benefits of radiological procedures, as well as biological effects associated to dose exposure.2–4
This background information illustrates that the role of radiologists is crucial in properly informing patients3,5,6 about radiation dose in a way that is understood by patients, independently of their socio-economic status.
The purpose of our study is twofold, both required by European directive DE 59/13
1
: - investigating patients’ interest in knowing about radiation dose and their comprehension regarding the use of ionising radiation; - identifying the most effective method for communicating dose exposure, in relation to age and socio-economic status.
Materials and methods
Patients and study design
A multi-centre cross-sectional study was performed through a collaboration of the ‘A.O.U.P. Paolo Giaccone di Palermo’, ‘A.O.U. Careggi di Firenze’, ‘IRCCS Ospedale Pediatrico Bambino Gesù di Roma’, and ‘IRCCS Istituto Giannina Gaslini di Genova’. A total of 1,084 patients were recruited from November 2018 to December 2019.
All adult and paediatric patients undergoing planned radiological examinations were considered eligible and asked to be involved in this study on a voluntary basis. First, all patients received preliminary written information explaining radiation exposure in imaging procedures, a description of radiation dose used, and possible risks in the form of frequently asked questions (FAQ) as per ‘EUROSAFE imaging recommendation for patients,
7
(supplementary material). After the required consent forms were signed (i.e. consent for use of exams utilising ionising radiation and contrast medium, if necessary), an illustrative sample was given on how patients should fill in the questionnaire. Patients refusing to participate were excluded. The format for this survey was derived from suggestion obtained by the 2016 WHO paper on risk-benefit dialogue in communicating radiation dose.
4
Therefore, we administered an anonymous questionnaire investigating both patients’ interest in radiation dose exposure and different communication modalities. The questionnaire was distributed by radiology residents, and patients were encouraged to answer to the best of their abilities. The questionnaire was made up as follows: 1) a personal patient data section (sex, age, educational qualification, and working status); parents of paediatric patients filled in the questionnaire reporting their demographic information (supplementary material); 2) four different modalities of communicating dose exposure, as follows: (supplementary material) I) Amount: only the dose amount derived from X-ray units (mGy, DAP, CTDI, and DLP). II) Reference: the dose amount with a reference range derived from the national DRL. III) Comparison: between the dose administrated and both equivalent dose and natural background. IV) Pictorial: colorimetric scales ranging from green (low) to red (high-level radiation dose); 3) three questions (supplementary material): A) ‘Do you understand the informative text regarding exposure to ionising radiation?’, with yes/no as response categories, to assess patients’ comprehension; B) ‘Do you want to know the dose of ionising radiation received?’, with yes/no as options, to assess patients’ interest; C) ‘Which of these four modalities of dose communication do you prefer?’, with five options (1/2/3/4/none) of the four modalities proposed, to assess patients’ preference.
Ethics committee
This study was approved by the following local ethical committees: • Palermo 1, A.O.U. P - Palermo: authorization n.7 date 09/07/18; • Area Vasta Centro, CEAVC - Tuscany: authorization n.5004 date 11/12/18; • IRCCS Istituto Giannina Gaslini - Genova: authorization date 14/01/19; • Ospedale Pediatrico Bambino Gesù - Roma: authorization n.124 date 16/01/19.
Statistical analysis
The goal for this study was to assess patients’ comprehension of the informative text and patients’ interest in knowing about the dose of ionising radiation, both expressed as binary variables (no, yes). The preference for the dose communication modality was expressed using five categories (I, II, II, IV, and none of the above). Other covariates were sex, age dichotomised using the median (below or equal to 60 and above 60 years old), education (none or primary, secondary, or higher education), and working status (employed, unemployed, and non-responder). All categorical variables were summarised as counts and percentages, and their statistical association was assessed through the Chi-square or the Fisher exact test, as appropriate. Crude odds ratio (OR) and the 95% confidence interval (CI) were calculated to measure the association between study outcomes and each covariate. Logistic regression models were estimated to calculate the adjusted odds ratios (ORadj) and 95% confidence interval. Participants reporting an age of ≤ 60 years old, having received primary or no education at all, being employed, and opting for modality I were chosen as reference categories to calculate ORs and ORsadj.
The sample size was calculated to estimate the proportion of respondents that did not understand the informative text about their radiation dose, assuming an error margin equal to 0.03 and a 95% confidence level. For sample size calculation, the percentage of patients that did not understand the information about the numerical CT dose parameters was set at 66%, as suggested by a previous study from our group. 8
All statistical tests were two-sided. For each analysis, a
Results
Patients
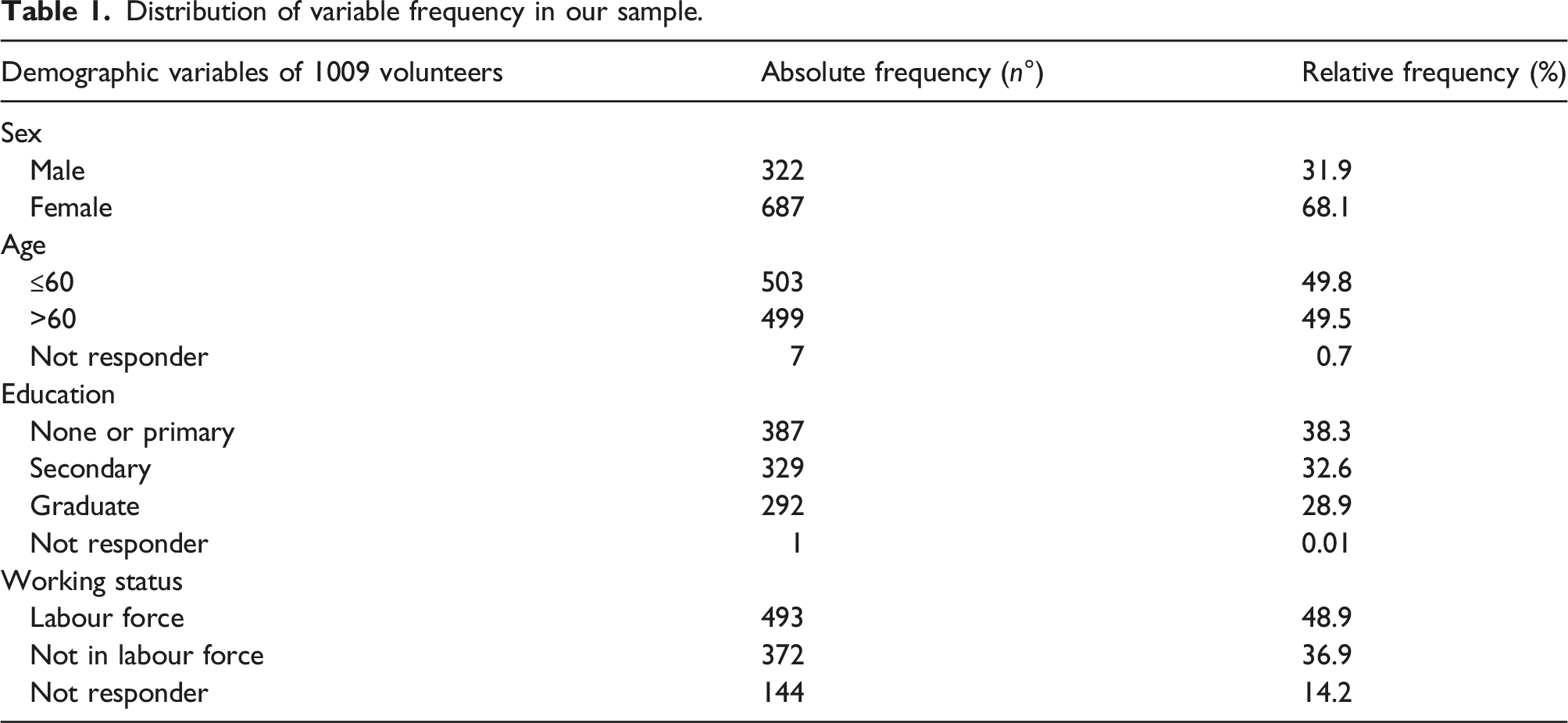
Out of 1,084 questionnaires distributed, 75 patients (7.0%) were excluded since they declined to fill in the questionnaire. The final population involved 1,009 patients including 173 (17.1%) parents of paediatric patients. X-ray examinations represented the largest group of referrals (453/60.0%) followed by CT (239/23.6%) and mammography (288/13.6%); in 29 questionnaires, the diagnostic modalities were not indicated. All participants filled the questionnaire completely except certain patients who did not declare their age (7 patients, 0.7%), education level (1 patient, 0.1%), and interest in knowing their dose exposure (2 patients, 0.2%).
Distribution of variable frequency in our sample.

Comprehension about the use of ionising radiation
The preliminary information text was understood by: - 71.7% of all participants; - 80.7% of ≤60 year-old patients and 62.7% of >60 year-old patients ( - 80.2%, 78.4%, and 76.3% of people with secondary level of education, higher education, and in employment, respectively. The multivariate analysis confirmed different levels of comprehension between patients with secondary education (ORadj = 2.44 [95% CI 1.51; 3.95]) and higher education (ORadj = 1.95 [95% CI 1.15; 3.29]) than patients with primary education. Among those respondents that understood the questionnaire, 32.9% did not express any preference between the 4 communication modalities and they showed a significantly low level of understanding (ORadj = 0.32 [95% CI 0.01; 0.11]; [ Comprehension of the information about the exposure to ionising radiation: univariable and multivariate analyses based on the answer ‘yes’ to the question ‘understanding of the informative text regarding the exposure to ionising radiation?’. *Linear regression: each variable was adjusted for the others.

Interest towards the X-ray exposure used in diagnostic examinations: univariate and multivariate analyses based on the answer ‘yes’ to the question ‘do you want to know the dose of ionising radiation received?’.

*Linear regression: each variable was adjusted for the others.
This pattern was also seen with responders currently in employment (66.7%) compared to unemployed (49.1%) (Table 3). Responders awaiting X-ray examinations showed lower levels of interest than those referred for mammography. Such differences were also confirmed by multivariate analysis (ORadj = 0.39 [0.17; 0.87]).
Interest in the X-ray dose administered and preferred method to communicate dose exposure
Interest towards the X-ray dose used in the exam for 40 people that did not choose any of the four options.

The most part of responders (652, i.e., 64.6%) expressed a preference for one of the four modalities of communication. People that did not choose any of the four options were 357 (35.4%) (Figure 1). Different preference in the communication modalities I, II, III, and IV or none of those express in percentage.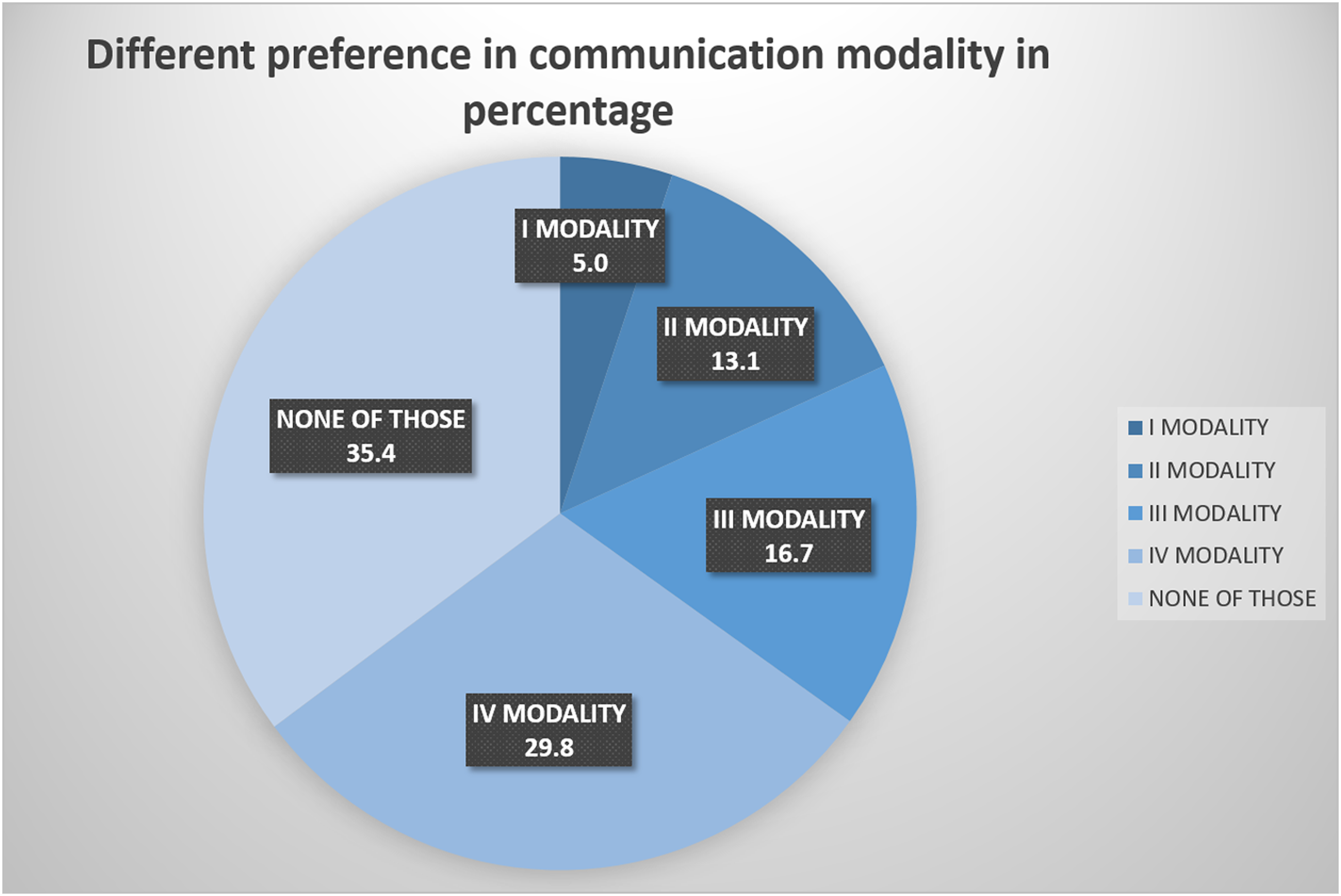
Regarding the preference of the communication tables, modalities I, II, III, and IV were selected by 51 (5.0%), 132 (13.1%), 168 (16.7%), and 301 (29.8%) subjects, respectively (Figure 1).
In detail, the different modalities were preferred by: - I (amount) was the least chosen modality (5.0%), and no statistically significant differences were found between univariate and multivariate analyses (Figure 1). - II (reference) was mainly selected by subjects ≤ 60 years old (15.3%) and with an undergraduate degree (17.8%) (Figure 2). - III (comparison) was selected by subjects <60 years old (19.8%), with secondary (21.0%) or higher (18.1%) educational level, and currently in employment (18.5%) (Figure 2). As shown by multivariate analysis, unemployed people were less prone to choose modality III compared to people in employment (ORadj = 0.60 [95% CI 0.46; 0.78], [ - IV (pictorial) was the most selected modality, being preferred by 35.0% of subjects ≤ 60 years old and 33.3% of people in employment (Figure 2). As demonstrated by multivariate analysis, patients ≤60 years old were less prone to choose this modality compared to those >60 years old (ORadj = 0.76 [95% CI 0.53; 1.11], [ - ‘None of those modalities’ was mainly preferred by responders that were >60 years old (46.7%) with a low educational level (none or primary education level, 44.4%) and unemployed (50.8%) (Figure 2). - Multivariate analysis also showed that people not in employment were more likely not to express any preference than people in employment (ORadj = 2.12 [95% CI 1.44; 3.11], [ Preferred communication modality differentiated by gender, age, level of education, and labour status. Preference for the communication modality: univariable and multivariate analyses. Preference for no one of the communication types proposed: univariable and multivariate analyses.



Discussion
Nowadays, easy access to medical imaging and the ever-increasing frequency of X-ray diagnostic examinations imply the necessity of raising public awareness on exposure to ionising radiation and related risks, allowing patients to be fully informed about medical decisions.8–10
Global and European regulatory bodies, in fact, have established more stringent criteria related to radiation dose awareness enabling patients to be informed in the best way possible.1,2
In 2013, the Patient Advisory Group was set up by the ESR with the aim of improving communication between patients and healthcare professionals working in radiology departments, thus helping raise the quality of diagnostic services through feedback and recommendations based on patients’ experiences.4,7,11 Therefore, albeit gradually, what radiations are and how they are measured will have to become common knowledge, just as it has been the case for measurement units of weights and distances. The main questions arising from this are how to start spreading these notions and how to assess that such information is fully understood by patients and relatives.12,13 Italian legislation has recently established criteria to ensure the inclusion of the radiation dose class in radiological reports and therefore provide information on what was the patients’ exposure during the examination performed. 14 Data derived from this study are prevalently from patients undergoing conventional X-ray examinations rather than computed tomography, the latter obviously representing a higher dose diagnostic modality. However, the aim of the study was to understand patient comprehension and interest in the most commonly performed examinations in diagnostic radiology departments.
Some papers in the literature13,15–19 have already explored what could be the optimal mode of communicating X-ray dose information (interviews with radiologists/radiographers or written information) and the possible level of comprehension by patients in North European countries. In their experience, Ukkola et al. 18–20 believed that communication around radiation risk is generally inadequate because it is mainly about indication, course, or radiation use, and very seldom actually involves the risks connected with radiation. In a previous experience, 8 we tried to provide written information reporting dose exposure data with the aim of improving patient understanding, noting a widespread lack of awareness around such information. 20
Ria et al. 21 demonstrated that the majority of patients, without substantial differences in terms of age and level of education, were interested in knowing about their dose exposure, and that simply including radiation dose information in the reports or verbal communication is not enough to properly inform them. Hence, they emphasised the need to find an appropriate communication strategy including the involvement of other medical professionals such as family physicians or medical physicists. Bastiani et al. 22 came to the same conclusions as the aforementioned papers,9–12 noting a high level of interest in knowing about radiation dose and the crucial need to find an optimal written modality to communicate such information. They used four modalities of communication in a way similar to our study, although no preliminary written information about radiation exposure was provided to patients. Furthermore, only quantitative information without any graphical representation was included in their study. Our series proved that quantitative information by itself can pose severe limitations to patient understanding and that every source of complexity should be avoided. The most highly appreciated representations by patients are those that are simple with immediately understandable messages and colour scales.
Our multi-centre analysis was aimed at identifying the most effective strategy to communicate risks related to ionising radiation to patients. In order to ascertain patient interest in paediatric hospital settings, we started by offering patients and relatives a preliminary written information sheet outlining the concept of ionising radiation in medical imaging. Then, further written material organised in the four different modalities reported above was provided to evaluate patients’ preference. In general, patients showed a keen interest in this study, with 93% of people interviewed actively taking part and only 7% declining to fill the questionnaires. Our results showed that the preliminary information sheet was generally comprehensible, and patients manifested an interest in developing a better understanding of ionising dose exposure related to radiological investigations. Around two-thirds of our sample understood the preliminary sheet fully and demonstrated an active interest, although most of them were young patients with a high socio-cultural level. Almost all of them preferred one of the four modalities proposed, and modality IV (pictorial or graphical representation) was found to be the most understandable irrespective of socio-cultural differences. Similar results were described by Ukkola et al.19,20 in which most of the patients preferred symbols to indicate dose exposure. Modalities II and III with more technical information such as dose reference and dose comparison were chosen especially by patients with a high socio-cultural level. ‘None of those’ was chosen by one-third of our sample, composed of four different clusters represented by female, over 60 years old, from a low socio-cultural level, and unemployed. Such results reinforce the known correlation between the level of education in a population and that of comprehension of new information. Otherwise, a widespread need of knowing about ionising radiation dose was found (647/1002 patients, 64.1%), with no significant difference in terms of sex, age, education, and occupational status.
There are some limitations to this study. First, patients were not randomised. Questionnaires were distributed only to patients that agreed filling it, potentially introducing recruitment selection bias. Lack of randomisation may be seen as a limitation, although for the design of this study, there was no other ethical way to carry it out. Secondly, the presence of medical staff during the distribution of questionnaires may influence the willingness to join the study. The option of distributing a second questionnaire to monitor patients’ level of interest after imaging results was also considered, but this strategy was deemed to be too inconvenient for patients undergoing investigations.
In conclusion, the current study showed that the written modality is simple and effective in satisfying patients’ interest in knowing more about their radiation dose exposure: graphical (pictorial-iconographic) and colorimetric representations proved to be the most easily understood. Moreover, such information could be enhanced further by combining it in a simple synoptic table, preferably preceded by a preliminary explanation to be read out in the waiting room before the examination is carried out.
Supplemental Material
Supplemental Material - Communicating radiation dose in medical imaging: How to best inform our patients?
Supplemental Material for Communicating radiation dose in medical imaging: How to best inform our patients? by Sergio Salerno, Cosimo Nardi, Mario Pace, Lidia Rabiolo, Federica Flammia, Francesco Loverre, Domenica Matranga, Claudio Granata, Paolo Tomà, and Stefano Colagrande in Acta Radiologica Open.
Supplemental Material
Supplemental Material - Communicating radiation dose in medical imaging: How to best inform our patients?
Supplemental Material for Communicating radiation dose in medical imaging: How to best inform our patients? by Sergio Salerno, Cosimo Nardi, Mario Pace, Lidia Rabiolo, Federica Flammia, Francesco Loverre, Domenica Matranga, Claudio Granata, Paolo Tomà, and Stefano Colagrande in Acta Radiologica Open.
Supplemental Material
Supplemental Material - Communicating radiation dose in medical imaging: How to best inform our patients?
Supplemental Material for Communicating radiation dose in medical imaging: How to best inform our patients? by Sergio Salerno, Cosimo Nardi, Mario Pace, Lidia Rabiolo, Federica Flammia, Francesco Loverre, Domenica Matranga, Claudio Granata, Paolo Tomà, and Stefano Colagrande in Acta Radiologica Open.
Supplemental Material
Supplemental Material - Communicating radiation dose in medical imaging: How to best inform our patients?
Supplemental Material for Communicating radiation dose in medical imaging: How to best inform our patients? by Sergio Salerno, Cosimo Nardi, Mario Pace, Lidia Rabiolo, Federica Flammia, Francesco Loverre, Domenica Matranga, Claudio Granata, Paolo Tomà, and Stefano Colagrande in Acta Radiologica Open.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
