Abstract
Retention of nurses in medical departments is complicated due to the high and stressful workload. The aim of this study was therefore to describe registered nurses’ perceptions of essential factors influencing their desire to stay in their position in a university hospital medical department. A rapid qualitative research methodology was followed. Data collection, consisting of qualitative interviews with 22 registered nurses during December 2022 and January 2023, and analysis, was guided by the Rigorous and Accelerated Data Reduction (RADaR) technique. The COREQ guidelines were used for reporting this study. The findings showed how the registered nurses collectively expressed collegial unity, flexible working hours, opportunities for development and training, the patient category and the managers’ importance as the five essential factors important for them to stay in their position. The study recommends that future research on retention has a point of departure in the local context and culture of the hospital wards.
Introduction
Nurses love nursing and consistently report that the most enjoyable aspect of their job is helping patients and families. 1 The statement ‘I love my work but hate my job’ is often the response from nurses due to the nature of nursing practice and the professionalism inherent in nursing as opposed to the dissatisfying organisational context and working conditions. 1 However, an increasing lack of nurses in hospital patient care entails dissatisfaction among the remaining nurses caused by understaffing combined with an increase of patients with complex care needs. 2 To make nurses stay in their hospital positions, retention strategies have been of extreme focus for the past years. Most retention strategies focus on the first year of employment where mentorship programmes are used to introduce newly graduated nurses to practice.3,4 The focus of mentorship programmes is on striving for a safe and thorough introduction and transition to the knowledge and skills needed to succeed in the new workplace and to the ‘socialisation’ process that helps new employees fit into the new organisation. 5 Strategies directed towards retaining experienced nurses show that retention is influenced by many factors, such as flexible scheduling, money, organisational focus on retention, work environment and retirement plans. 6 A systematic review of effective strategies for retaining experienced registered nurses concluded that no particular intervention could be implemented to influence experienced nurse retention – rather a combination of the many factors important for nurse retention would be effective. 6 Retaining experienced nurses in the workforce requires innovative approaches, including the redesigning of roles and increased attention to work hours and the physical demands of nursing practice. 7
Denmark is divided into five regions and the highest nursing shortage is found in the region of Zealand, where an optimisation of strategies to recruit and retain nurses is urgently needed. The ability to recruit and retain nurses for medical departments is additionally complicated due to the high workload and patient-to-nurse ratio,8,9 which can explain the annual nursing turnover of 30% on average. To develop the most effective retention strategies directed towards nurses in hospital medical departments, knowledge is needed on what the registered nurses experience as important in their work to remain in their job. The aim of the present study was to describe registered nurses’ perceptions of essential factors influencing their desire to stay in their position in a university hospital medical department.
Methods
Design
A rapid qualitative research methodology 10 was chosen to investigate the aim of this study. Rapid qualitative research is a comprehensive term for studies using an accelerated but structured approach for data collection and analysis.10,11 For this study, the Rigorous and Accelerated Data Reduction (RADaR) technique 11 was applied for data collection and analysis to secure quick and evidence-based references to retain nurses at medical units. We have adhered to the Consolidated criteria for reporting qualitative research (COREQ) guidelines 12 for the reporting of this study.
Participants and settings
The setting of the study comprises five units in a university hospital medical department consisting of three inpatient wards, divided into geriatrics, gastric medicine and liver illnesses, and two outpatient clinics covering diabetes and gastric medicine. The five units currently have 112 registered nurses employed and 24 vacant nursing positions, which causes specialised and complex medical patients to be admitted to departments of other specialist areas.
All nurses from the five units were recruited through convenience sampling and invited to participate by the first author. To adhere to the nurses’ busy schedule, the first author sat in each unit for a week, with time for conducting interviews. This process was decided by the research group, to provide the nurses with the opportunity to be interviewed when they had available time during their working day. A total of 22 nurses agreed to participate in the interview (Table 1).
Characteristics of participating nurses (n = 22).
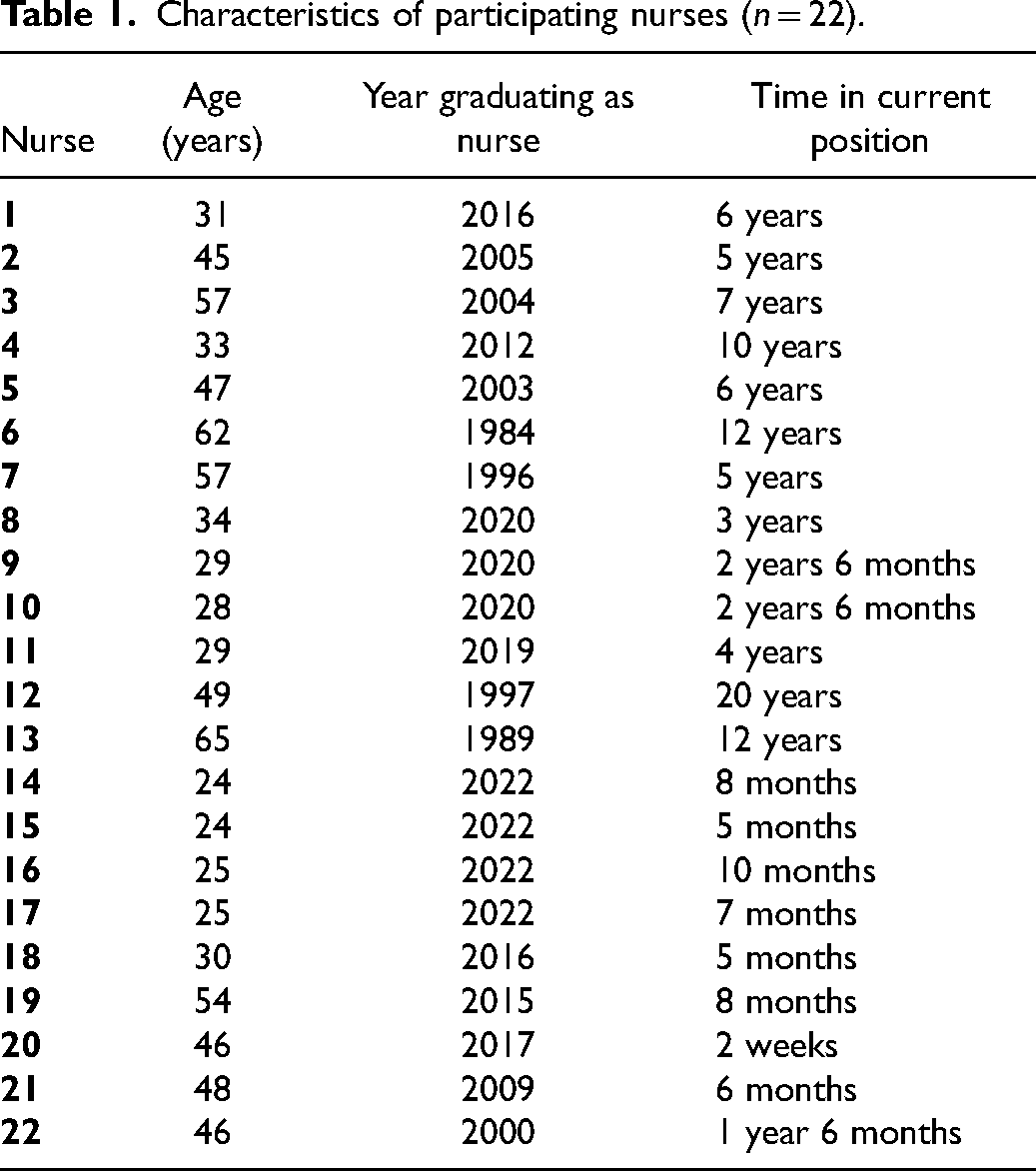
The 22 participating nurses (20 women, 2 men) had a mean age of 40 years (range 25–65 years) and had on average been educated as nurses for 12 years (range 1–39 years). The nurses had been employed in their current position for an average of 4.5 years (range 2 weeks–20 years).
RADaR data collection and analysis
Data collection and analysis were performed using the four steps of the RADaR technique (Table 2).
The four steps of the RADaR technique. 11
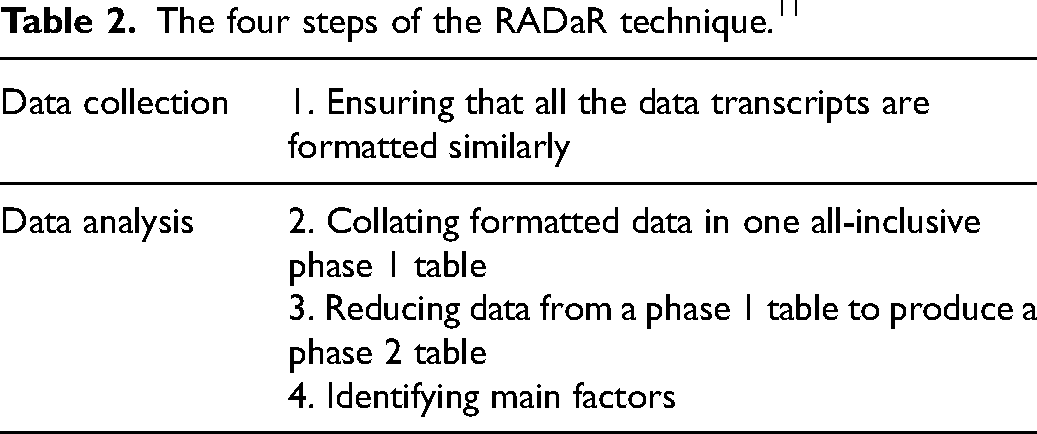
The RADaR technique is a structured method to organise, reduce and analyse qualitative data collated through interviews (Watkins). The technique is deemed rigorous due to the structured ordering of data within tables, and it accelerated due to the reduced time used for data analysis in comparison with other qualitative analysis (Watkins).
Step 1: Ensuring that all the data transcripts are formatted similarly
The 22 interviews were conducted between December 2022 and January 2023 in secluded rooms at the medical units. The interviews were directed by semi-structured interview guides consisting of questions about the participants’ sex, age, graduation year as a nurse, time in current position and the specific unit of employment as well as specific questions concerning the nurses’ perspectives on staying in their jobs at the medical units.
The questions on nurses’ intentions to stay were based on nine domains from a systematic review of factors affecting retention among hospital nursing staff. 13 The nine domains were as follows: Professional issues; Nursing leadership and management; Staffing issues; Education and career advancement opportunities; Organisational and work environment factors; Support at work; Personal factors; Demographic factors; Financial factors; and Unclassified influences. 13 An additional item to name the five factors most important to stay in the unit was applied.
To ensure that all the data transcripts were formatted in a similar manner, the interview guides were conformed to Rapid Interview Tables. 11 Notes were drafted in the Rapid Interview Table during the interviews and used as the overall data material. The interviews were not transcribed; however, they were used as verifying audio material. The 22 interviews lasted for a range of 18–72 min (mean 40 min) for a total of 14 h.
Step 2: Collating formatted data in one all-inclusive phase 1 table
In the second step of the RADaR approach, data from the 22 Rapid Interview Tables were organised according to each of the nine domains in one all-inclusive phase 1 table. This provided the authors with the opportunity to have a comprehensive view of data and of what all the participating nurses answered to each domain, e.g. How important is the factor of staffing issues for you to stay in the unit and why? The authors condensed each reply of the nine domains to a code, resulting in 414 codes from the 22 interviews. Descriptive notes were written for every code.
Step 3: Reducing data from a phase 1 table to a phase 2 table
In the third step of the RADaR approach, the phase 1 table was reduced to a phase 2 table, containing only the 414 codes, the affiliated notes and the domain of which it was collated. The phase 2 table was ordered according to the nine domains. 13
Step 4: Identifying main factors
In the final step of the RADaR approach, the authors analysed the phase 2 table to identify the main factors expressed by the nurses as essential for them to stay. To get an overview of the most important factors described by the nurses, the authors ordered the 414 codes according to those expressed by the nurses in the item: name the five factors most important for you to stay. The essential factors expressed by the nurses were not exactly similar to the nine domains as they varied between the domains. As an example, the most important factors for the nurses were collegial support and unity, which was not a specific domain but a mix between Work environment and Support of work. The second most important factor was having flexible working hours, which was a mix between the domains Personal factors, according to their work–life balance, as well as Staffing issues. The domain of Education and career advancement opportunities was described by the majority of nurses as the third most important reason to stay. The fourth most important factor was the patient category in their units, which was unmentioned in any of the nine domains, and the fifth most important factor to stay was the domain of Nursing leadership and management. No nurses mentioned Organisation environment issues or Unclassified influences; only two of the 22 participating nurses mentioned Demographic factors and Financial and monetary aspects, such as salary and bonuses – however, not as top five factors.
The analysis was conducted descriptively, and the findings are presented close to the participants’ statements according to their top five essential factors to stay in medical units. Data from phases 1 and 2, as well as the audio-recorded interviews, were used to supplement the descriptions of the findings.
Ethical considerations
All participants received written information when invited to participate as well as oral information at the time of the interview concerning the study essentials, author credentials, judicial rights and amount of participation. The participants were also encouraged to sign a consent form before their participation. The study was approved on 23 December 2022 by the Danish Data Protection Agency in Zealand Region, Denmark (REG-144-2022). Approval from the ethics committee was not deemed necessary since no biomaterial was a part of the study.
Rigor and reflexibility
The study rigour was assured by following Lincoln and Guba's 14 criteria of trustworthiness.
Credibility was assured by staying close to the participants’ statements about their perceptions of essential factors needed to stay in a hospital medical department. Even though the interviews were conducted using Rapid Interview Tables, 11 the interviews were digitally recorded for the authors to go back and look for similarities within and across the participants’ statements. The recordings made it possible to stay close to the interviews and to present relevant quotes to support our findings. Transferability was secured by presenting a thorough description of how the authors conducted the four steps of the RADaR technique. 11 Through that attempt, the authors established clarity on how to conduct a qualitative interview study using the RADaR technique, for other researchers to replicate. To secure dependability, the study was reported using COREQ 12 for other researchers to follow the decision trail used by the authors. Confirmability was assured throughout the study through reflections and discussions between the authors on the participants’ statements on what they essentially needed to stay in their positions.
Findings
The participating nurses collectively expressed the factors they experienced as essential for them to stay in medical departments. The top five essential factors particularly important for the nurses to stay, in order of priority, were as follows: collegial unity; flexible working hours; opportunities for development and education; the patient category; and the managers’ importance (Figure 1).
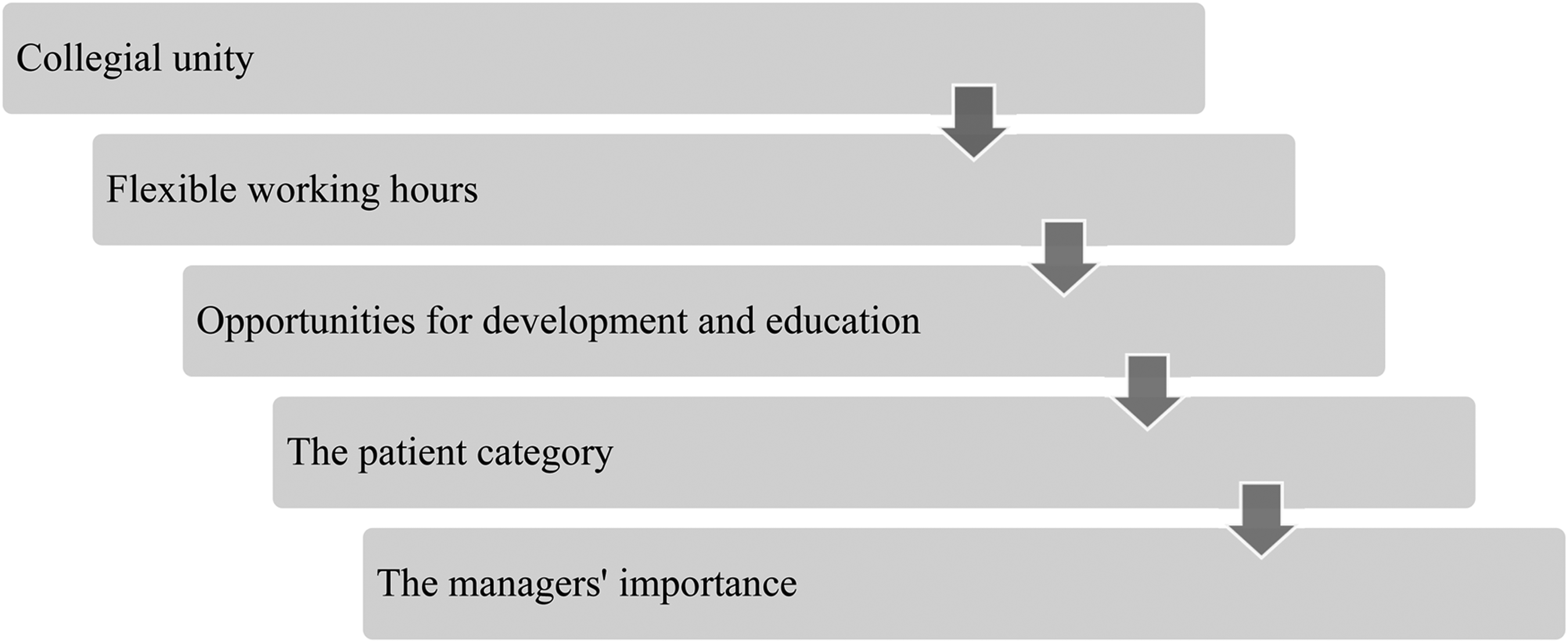
Top five factors essential for nurses to stay in the medical unit.
Collegial unity
The majority of nurses considered the feeling of unity and cooperation within the collegial group as the most essential reason for staying in the unit. The nurses described that they had a great atmosphere in their group of colleagues, which was characterised by great cooperation within the nursing care. The nurses described how everyone liked each other and treated each other properly. There was also a lot of laughing, which was of great importance in daily life in the units. The nurses described that great colleagues made it worthwhile to go to work. The interactions with my colleagues make it great to go to work and we have some good talks. It creates a great environment to be in. (Nurse 9)
On several units, the nurses participated in social events with their colleagues outside work because they simply enjoyed being together. In one unit, collegial unity was described by the nurses as being similar to family relations. They knew everything about each other, even if they didn’t see each other in private, which made the nurses very close within the unit. We are good together. Almost like a family. We are not close friends and you have not been to my house but, still, you know everything about me. It's kind of odd but very close and we share everything. (Nurse 12)
The nurses described the culture within the units as respectful, full of helpfulness and no one talked behind each other's backs. There was a mutual collaboration in making the working day run smoothly for the patients and their colleagues. The nurses also described the collaboration with other healthcare professionals in the hospital as noticeable, which was important to get the day running and get through it more easily. The nurses stated that everyone was good at asking questions and helping each other, which meant that the nurses did not feel abandoned when busy. It is always okay to ask. I ask all staff for help and everybody is welcome to. No one gets annoyed. And someone like me who is new asks a lot of questions. (Nurse 15)
The nurses emphasised that being present in a positive working environment and the positivity of their colleagues was important for them. Even though it's busy you can keep a positive attitude. (Nurse 10)
The nurses believed that everyone should prioritise coming to work with a positive mindset and with the intention that the working day was going to be great no matter what the circumstances were.
Flexible working hours
Flexibility related to the nurse's working hours was also an important factor for the nurses to stay in the medical department. It was of great importance to the nurses that the management was responsive to their wishes and needs for planning and changing shifts to fit the nurses’ private life. This meant that the nurses felt seen and heard as individuals and not as just a set of hands. She [the head nurse] is very attentive to our need for time off on certain dates and that means a lot. You just have to say it in advance. (Nurse 13)
A ‘Wish Plan’ for shifts on one of the wards was particularly highlighted by several nurses who had it in their top three important factors to stay on the ward. The Wish Plan was the nurses’ tool to write down the exact dates for shifts they wanted, which the head nurse accommodated to the best of her abilities. Here we have the Wish Plan and the head nurse does what she can to fulfil our wishes for shifts. That's the way it's always been. (Nurse 12)
The work–life balance was of extreme importance for the nurses who wanted to work but also make their home lives liveable.
Flexibility within the nursing work was also important to the nurses of the medical department. Some of the nurses experienced opportunities to plan their daily work independently and to be able to switch tasks around to fit the patients’ needs. This contributed to extra time slots where they could help and support their colleagues. It's nice to be able to plan your day. You never get stressed even though you are busy. It makes it a lot easier to move things around so you can help your colleagues. (Nurse 13)
Other nurses found a combination of positions desirable, which contributed to their opportunities to focus on different areas of interest when at work. One nurse described how a combination of working as a nurse and being responsible for the onboarding of newly employed nurses to the medical department was very fulfilling.
Opportunities for development and education
Self-development, development of the medical specialty as well as the opportunity to attend postgraduate education was an essential factor for the nurses to stay in the unit – especially for nurses employed in the unit for more than 1 year. Now they knew the patients and their colleagues and felt secure in their work and now ‘something had to happen’. Something has to happen now with my development. I have been doing the same work for 5 years and I don’t want it to be too boring. Would rather develop myself here than get a new job. (Nurse 2)
This group of nurses described that they needed constant development, of themselves and their nursing competencies, but also within the unit. However, it was important for the nurses that developmental ideas were not initiated top-down, as they needed development to be initiated from their ideas to feel engaged. I really want to develop myself and also the unit I work in. I don’t like having changes and development initiatives thrown in my face by the management. Sometimes it's like that but just as long as it is not all the time. (Nurse 13)
Several of the nurses described that it was important for them to take part in larger projects. Many of them had special responsibilities for specific areas, such as skill stations, the delirium group, student education and onboarding programmes for newly employed nurses. The nurses also prioritised being enrolled in educational programmes but only if they experienced the possibility of using their new competencies in patient care when they returned to the unit. I’m participating in a course on geriatric medicine, which unfortunately is not fully developed yet. That's one of the reasons why I’m staying – to learn more about what interests me. (Nurse 9)
A nurse described that it was important that the nurses were allowed to use their new knowledge and skills when they returned. Otherwise, they would stop and find a place where they could be used.
The patient category
A large proportion of the nurses said that the patient category in their unit and the medical specialty itself were essential factors for them to stay in the unit. This was especially mentioned by the nurses in the geriatric unit and the liver unit. Some of these nurses had decidedly chosen employment in the specific unit to take care of these particular patient groups. In their job advertisement, they wrote about elderly care, which has always been a great interest of mine. I love working with the elderly so that's the reason I applied in the first place. (Nurse 9)
Several of the nurses had previously worked with older people and had always found this rewarding. I applied for this position because of the geriatric specialty. I have always enjoyed working with old people and have also worked at a nursing home for several years. (Nurse 17)
Patients with illnesses related to the liver were special to some nurses, as they were often considered a disgraced group of alcoholics who people wanted nothing to do with. The liver patients have my interest. They are a stigmatised group of alcoholics that people stay away from – except me. (Nurse 12)
Here, the nurses could work meaningfully with a vulnerable group of people. Other nurses had chosen the medical specialty as a whole, as there was a lot to learn about nursing in general. In addition, it was also important for some of the nurses that there was semi-acute nursing care, as long as it was not all the time. The position also has some acute nursing in it and that's a great mix with elderly care. Just as long as it is not all the time. (Nurse 9)
The nurses continuously tried to optimise themselves and their knowledge so that they could do better for their patients. This was significant for them, as they wanted to stay up to date with the latest trends in care and treatment for the sake of the patients.
The managers’ importance
The nurses believed that their closest management, the head nurses of the units, was important for them to stay. This was connected with the management being visible and willing to participate in the collaboration concerning patient care, but also about the management's flexibility with shifts.
It was essential to the nurses that their head managers were visible every day. This included that the head manager had lunch with the nurses, co-created a good atmosphere and was available for questions and advice on patient care issues. I like that the management is visible every day and that she has her lunch break with us. I have had many different managers and it's not all of them who eat with the staff. (Nurse 20)
In addition, it was essential for the nurses that the head managers occasionally joined the nurses in patient care when days were busy. I enjoy that our head nurse works in shifts with us. She works every third weekend with us in patient care. That gives her a good picture of what things are like ‘out here’. (Nurse 15) She can always relate to my problems and that is truly valuable for me. I could never work with an ice-cold manager who doesn’t care. She also knows when I’m off and she comes to me when she can see that I’m not right. (Nurse 2)
It was important for the nurses that they could talk to the manager about anything. This contributed to a feeling of being seen, heard and taken care of. None of the nurses wanted an indifferent leader. It was also essential for the nurses to have a head manager who reached out to them when she could see things were bad.
When the nurses felt heard by the manager, it made them believe that the head manager was doing something active for the nurses to thrive. The nurses described how it was important to them that they had a manager who fought openly for better conditions and who stood up for the nurses.
Discussion
This rapid qualitative study aimed to describe registered nurses’ perceptions of essential factors needed to stay in a hospital medical department. The 22 interviewed nurses provided five top essential factors critical for them to stay in the medical department: collegial unity; having flexible working hours; having opportunities for development and training; the specific patient category in their unit; and the importance of connecting with their managers.
In our study, three of the five essential factors to stay were based on personal relations with colleagues or family, as in flexible working hours and work–life balance, and their managers. The priority set as an essential factor for the nurses was the feeling of being in a collegial unity. The nurses described the unity as consisting of strong work collaboration as well as personal relations, which made it more positive to go to work and manage difficult days. A cross-sectional study performed as a questionnaire study of 500 newly graduated staff nurses in Tehran, Iran, found that enjoying working with colleagues and having social support increased the nurses’ job satisfaction and intentions to stay. 15 A questionnaire survey for nurses working in a county hospital in northern California, USA, also found a correlation between collegial support with job satisfaction and retention. 16 This study furthermore identified higher mean scores for peer cohesion and co-workers perceived as friendly and supportive of each other, by nurses who stayed than by nurses who left their position. 15 The literature also showed how nurses occasionally worked past retirement age to continue having social work relations as a part of their lives. 17 As another personal aspect of the nurses’ essential factors to stay, flexible working hours were the second highest priority for the nurses related to maintaining and prioritising a family life. Through a questionnaire study of 191 nurses in public sector hospitals in Saudi Arabia, Aamir and colleagues 18 found a significant correlation between work–life balance with retention and job satisfaction. In our study, we identified how having significant contact with the nurse manager in the unit, who was visible, open to conversation and supportive, was an important factor for the nurses to stay in their position. The literature also shows how retention of nurses relies on the nurses’ perceptions and experiences of a supportive manager 16 and a manager who supports the nurses in their problems 15 as well as listening to their views. 13 As our findings show, a manager who is engaged and visible in the clinical environment and provides accessible leadership 13 is an important factor for the nurses to stay.
Besides the relation-based aspect of the nurses’ intentions to stay, they were very interested in developing themselves as well as developing the practice they worked in. Taking courses and education was a great opportunity to do both as long as the nurses were able to use their new knowledge when they returned to practice. Opportunities for development and training were also seen in the literature related to retention success when the nurses perceived education opportunities, 12 career advancement13,19 and a chance for development with supervisory support. 20 The nurses’ need to use their new knowledge in practice was related to their interest in developing patient care for the specific group of patients that were in their hospital unit. Our study showed how the patient category in the nurses’ unit was an essential factor for them to stay and that some of the nurses had decidedly chosen employment in the specific unit to take care of these particular patient groups. The literature also shows how patient-related factors are strong predictors of the nurses’ intentions to stay in their organisation and profession 21 as well as having the possibility to perform professional patient care. 22
Strengths and limitations of the study
Traditionally, rigour in qualitative research has been associated with the length of time regarding immersion with data; however, the literature indicates that rigorous findings also can be developed using the rapid qualitative research methodology.23,24 For this study, the strength of using the rapid methodology was that potentially interpretative bias was eliminated and a vast amount of time was saved on omitting the transcription of the 22 interviews. Due to the reduction of time on transcribing the interviews, the authors were able to collect more data and include more research participants within the time frame of the study. The strength therefore amounts to creating a larger density of data material. A strength could also be that the authors found a greater insight into data beyond what can be learned from reading a transcript, such as important pauses in speech and volume fluctuations. On the contrary, the study can be critiqued for not achieving the same ‘depth’ or ‘level of interpretation’ as conventional qualitative methods of data analysis. The potential loss of data if coding directly from the digital recordings or if only reliant on notes in the Rapid Interview Tables could cause a threat to the credibility of our study. However, the in-depth analysis of qualitative transcripts can be time-consuming as well, resulting in delays in the implementation of findings, 23 which was important for our study. This study intended to describe the nurses’ perceptions of essential factors needed to stay in a hospital medical department, aiming to implement the results quickly.
Implications for clinical practice
The scientific literature has profoundly and far-reached described nurses’ detailed intentions to stay21,25 or to leave22,26 their current hospital positions. In addition, a large variety of intervention studies has evaluated the effect of diverse strategies to increase retention and motivate nurses to stay in their positions.3,6 We have extensive descriptive and experimental knowledge about how to make nurses stay – so why do we still have the highest shortage of nurses and vast complications in recruitment and retention for hospital positions in history? One reason could be the effectiveness of the intervention studies performed to evaluate strategies for retention. In a systematic review, Lartey and colleagues 6 found the effectiveness of strategies for retaining experienced registered nurses in half of the 12 included studies as a direct result of the interventions. The studies were primarily non-experimental, four of the studies used a pre- and post-design to collect data and two had comparison groups. 6 Lartey et al. 6 conclude that few well-designed studies in the literature report on interventions for retaining experienced nurses in healthcare settings. In a systematic review by Brook and colleagues, 3 the authors concluded that methodological issues had an impact on which conclusions could be drawn from the 53 included studies on interventions to reduce turnover and increase retention of early career nurses. Brook and colleagues 3 conclusively argued for a future focus on standardising the reporting of interventions and outcome measures and carrying out further research with rigorous methodology. Another reason could be that increasing work intensity 27 is enlarged with too few nurses and an increase in hospital admissions can cause burnout, 28 stress and early retirement for nurses. 29 Further, balancing work and career with a private life, especially when you have a family, can be difficult. 25 The pressure and intensity of work have increased in the past decades and family life is threatened. 27
Recommendations for future research
One year after conducting interviews with the 22 nurses in this study, nine of them are no longer employed in the medical department, even though changes were made within the department to make the nurses stay. Reflections between the management group and the authors led us to considerations for future research to prevent a further increase in nurse turnover. Based on the body of evidence of our qualitative descriptive study combined with the related literature, specific strategies for the retention of nurses should be tailored for each ward, to embrace the specific context and culture present. Every hospital unit has its specific context related to the nursing history, traditions and normative culture of the specific units. Culture is a crucial part of the behaviour and actions among nurses and could be important for the nurses’ reasoning to stay. Our descriptive study was performed to gain specific knowledge about the nurses’ intentions to stay in a specific medical hospital context. Combined with two previous studies on the nurses’ intentions to leave and the newly employed nurses’ experience with a novel onboarding programme, the authors aim to use this knowledge to tailor a specific retention strategy, to be evaluated as an experimental intervention.
Conclusion
By using a rapid qualitative methodology, this study found five prioritised factors essential for 22 nurses’ intentions to stay in their current position at a university hospital medical department: collegial unity; flexible working hours; opportunities for development and training; the patient category; and the managers’ importance. Three of the nurses’ five essential factors to stay were based on personal relations with colleagues or family – as in flexible working hours and work–life balance – and their managers, which is supported by the literature to be strong predictors for retention. Although the literature holds an excessive amount of descriptive and exploratory knowledge about nurses’ intentions to stay and leave their positions within hospital organisations, no magic bullet has been identified to solve the increasing global shortage of nurses. This study recommends that future research must be based on the local context and culture of hospital wards, to tailor the intervention studies for evaluating retention strategies, to the nurses currently employed in the department.
Footnotes
Acknowledgements
We would like to thank the nurses who took time out of their busy schedule to participate in the interviews for our study and to share their thoughts on what is essential for them to stay.
Conflict of interest
The authors declare that there is no conflict of interest.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
