Abstract
The nursing profession is close to clinical practice and vital to the student's professional development. Innovative learning activities and models are sought to improve clinical placements. A student-centered supervision model based on patient-oriented care was introduced in a medical ward. The aim of this study was to describe nursing students’ experiences of learning with a student-centered supervision model based on patient-oriented care during their clinical placement. A qualitative descriptive study involving interviews with 12 nursing students analyzed through inductive qualitative content analysis was conducted in accordance with COREQ. The findings revealed that the nursing students viewed learning as personal, knowledge, and professional development. Their learning experiences can be seen as a process in which the scaffolding is gradually reduced in line with each student's ability to act independently and establish a professional identity. The model can enhance structure and support in the practice setting to maximize learning.
Keywords
Introduction
Clinical placement constitutes a significant part of developing a professional identity and an essential bridge to future professional work as a registered nurse. 1 The shortage of registered nurses is extensive and will increase in Sweden as well as internationally. 2 In the long term, it means a shortage of supervisors for nursing students during their clinical placement. This can hinder the students’ learning process. According to Papastavavrou et al., 3 continuous meetings with a supervisor can be considered positive for student learning and when supervision models were used, they narrowed the gap between theory and practice, thus students perceived supervision as positive. 4 Time for reflection, discussion, and feedback during supervision contributes to students’ learning. 5 Research shows a need to build a clinical teaching atmosphere that promotes opportunities for theoretical and practical connections. Effective feedback mechanisms can enable students to experience a meaningful clinical learning environment on which to build their professional roles and competencies, thus helping to enhance their willingness to pursue nursing careers in the future. 6 This study is about nursing students’ experiences of learning with a student-centered supervision model based on patient-oriented care during their clinical placement.
Background
The nursing profession is close to practice, hence clinical placement constitutes an important part of the students’ development of a professional identity. Developing a professional identity means that students acquire the ability to perform professional work and identify themselves as a registered nurse, with insight into ethical principles and values. The integration of ethics strengthens the student's responsibility in clinical settings. 7 A well-organized clinical placement is characterized by opportunities for the supervisors to give the nursing students support and responsibility. 3 There are different forms of supervision. In traditional supervision, the student usually follows the supervisor during the course of the work, where the focus is on teacher-driven learning. 8 Another form is student-driven supervision with examples of models for collaborative learning, such as Peer Learning, which has been introduced in several contexts. 9 Collaborative learning cultivates a safe learning environment, improved self-confidence among students, and prepares them for their coming profession. 10
A good learning environment is characterized by a feeling of belonging and the opportunity for support. Students need to be able to discuss and reflect on their practical experiences with their academic teachers as well as their supervisors and fellow students. 11
Research emphasizes the importance of clinical supervisors as role models for students’ development of professional identity during clinical placement. 12 The supervisor function is complex as they must be able to support the students’ ability to translate theoretical knowledge into the actual problems encountered in a specific care context. 13 The relationship between student and supervisor is an important part of student learning. According to Jack et al., 14 individual, goal-oriented supervision increases the learning and sense of belonging among students. This result is consistent with the study by Gusar, 15 which shows that students who received individual supervision were better able to achieve the learning outcomes, thus strengthening their professional development. Students experienced supervision as positive when the supervisor considered the education important and designed structured learning plans with them. Students with negative experiences reported that the supervisor did not consider education important and the communication between the supervisor and the university was poor. 16
The student-centered supervision model based on patient-oriented care
A supervision model was introduced at a hospital in Sweden. In this student-centered pedagogical model, the nursing students follow the patient closely during their clinical placement with a focus on learning and activity. It was developed in collaboration between healthcare staff, hospital educators, teachers from the university, and many students to ensure the quality of clinical placement for nursing students despite high staff turnover. Student-centered learning implies that the student has responsibility for and takes part in learning activities. It involves participation, involvement, and reflection. 17 The relationship between the student and supervisor becomes more equal, as well as promoting and developing. The model is based on Cajvert's 18 description of integrated learning and focuses on how the supervisor can help students to reflect on their work, i.e. nursing activities, connect the practical tasks to different nursing theories and conceptualize their work. The university teacher’s role in the model is to provide support to supervisors in connecting the supervision with the learning objectives of the courses. The content of the model is based on the learning objectives specified in the curriculum of the course in which the student is enrolled, i.e. the year of the nursing program. A specific tool included in the model is Gibbs’ 19 reflective cycle model, which is a framework with a focus on structuring the learning process from experience by means of six stages: description; feelings; evaluation; analysis; conclusion; and action plan.
The supervision model gives nursing students opportunities to take responsibility for their learning and to follow the patient's care trajectory. The model's task is to stimulate each student's ability to create deep care relationships and be prepared for their future profession as a registered nurse by training involving daily work, responsibility, reflection, critical thinking, and cooperation. The supervision model implies that instead of merely following the supervisor's work, students follow selected patients during their clinical placement. Hence students follow a particular patient from admission via treatment and care to discharge. The number of patients for which they are responsible increases over time. While the student is not connected to one particular supervisor, one nurse is assigned as the main supervisor. The main supervisor is responsible for ensuring each student's progress by means of regular reflective meetings with the student. In other words, although there is a head supervisor, the students can meet different supervisors during their clinical placement.
Each student's learning is followed via documents stored in a personal folder, which can also be digital. A document outlining each student's expected development based on the learning outcomes is contained in the student's folder. The documents give the supervisor an overview of each student's development and provide students with clarity about what is expected. During the week, each student's learning is documented together with the supervisor who supervised during the work shifts. On selected occasions, the students meet the main supervisor and together plan nursing activities for learning, reflect on, and follow the development of the learning in relation to the learning outcomes. The model's task is also to create security for the student through a structured working method. In this way, it can reduce the gap between academic thinking and practical experience, thus creating powerful knowledge with the help of reflection.
Theoretical framing
According to the sociocultural perspective, 20 the learning process requires communication, interaction, reflection, and meaning-making to be successful. The clinical environment connects and encourages learning for a future professional function. The student-centered supervision model based on patient-oriented care can also be seen as a form of work-integrated learning (WIL), as it is designed in collaboration between academia and the healthcare organization. WIL means integrating practical experiences with academic learning. 21 The integration of theoretical and practical knowledge drawn from learning contexts in both education and working life is necessary for inclusive and sustainable knowledge. WIL is used as a teaching method and model combined with theoretical studies and practical work, i.e. clinical placement. 22 Clear goals, active supervisors, and motivated fellow students who enable the sharing of experiences and linking of academic learning with practical knowledge are required for the model to be effective,23–25 but also to ensure patient safety. 26 The aim of this study was to describe nursing students’ experiences of learning with the student-centered supervision model based on patient-oriented care during their clinical placement.
Methods
The research adopts a qualitative descriptive design, chosen for its appropriateness in delving deeper into the human experiences 27 necessary for understanding students’ learning experiences of learning with a student-centered supervision model based on patient-oriented care. The data comprised semi-structured interviews, 27 analyzed by inductive qualitative content analysis, focusing on both manifest and latent content. 28 This study adheres to the consolidated criteria for reporting qualitative research (COREQ). 29
Setting
The student-centered supervision model based on patient-oriented care was implemented in 2018 and applied by supervisors at medical departments for older people and they had worked with the model for approximately 2 years. The departments served individuals aged 75 years and older with multiple morbidities in need of extensive care. On each shift, a registered nurse was tasked with overseeing approximately nine patients. The staff worked inter-professionally based on the Comprehensive Geriatric Assessment (CGA) model. 30 The CGA model consists of integrated structured care for older people, where the team formed an integral part of the unit's operation.
The team consisted of registered nurses, physicians, occupational therapists, physiotherapists, counsellors, and enrolled nurses. They addressed illnesses, conducted diagnostic and physical tests, and collaborated with other healthcare providers like healthcare centers and municipalities to plan for patients’ future needs.
Participants and recruitment
The present study was conducted with 12 nursing students recruited from a university located in a medium-sized city, in Sweden (Table 1). The nursing program comprises a 3-year education (180 Higher Education Credits [HEC]), which leads to both a professional degree and a bachelor's degree and prepares the student for future professional work as a registered nurse.
Information about the participants (n = 12).

Participants who were recruited were considered to have a great deal of experiences to express. 27 Therefore, students who had worked with the supervision model during their clinical placement were selected. All students were recruited by registered nurses at the clinic. The students who agreed to participate contacted one of the authors (JSM) by email for more information and an appointment for the interview. They received both oral (in connection with the interview) and written (email) information and gave written informed consent (via letter, a scanned document, or in connection with the interview).
Data collection
The data collection took place between November 2020 and November 2021 and involved semi-structured interviews. An interview guide was used as support (Table 2). The question areas had been purposively designed as recommended by Polit and Beck 27 and contained items about learning experiences from the student-centered supervision model based on patient-oriented care.
Interview guide.

The nursing students were allowed to choose the form, time, and place for the interview. The COVID-19 pandemic was rampant during the data collection period, thus seven students opted to be interviewed using the Zoom videoconferencing program, which is recommended as a tool for research purposes as it supports real-time audio and full-motion video.31,32 The participants, who were asked to find a quiet place for the interview to ensure privacy, reported that it was easy to use the downloadable version. The videos were later erased and the audio recordings transcribed. However, five students chose a face-to-face interview, which took place in a conference room close to the ward and was recorded using a Dictaphone. To ensure privacy, the door was closed and marked occupied. Both the Zoom and the face-to-face interviews lasted approximately 25–50 min.
The first four interviews were conducted by two interviewers (AJ, JSM) to ensure coherence, after which AJ performed a further five interviews and JSM conducted the other three. After each interview, the interviewer verbally summarized the content with the student to ensure accuracy.
Data analysis
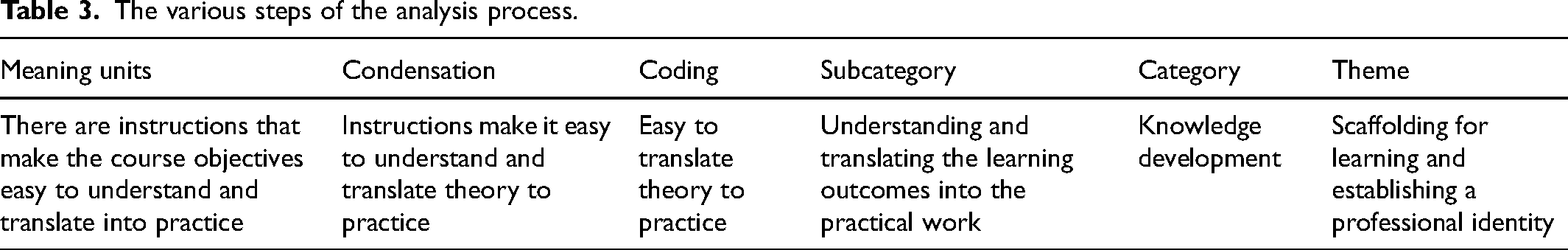
The data analysis was conducted using qualitative content analysis with a focus on both the manifest and latent content. Manifest content pertains to the observable, evident aspects of the text, whereas latent content involves an interpretation of the implicit message conveyed in the text.33 The authors transcribed the interviews in a word-for-word manner (AJ, JSM), after which they were read and reread by all authors. Meaning units were identified based on the aim of the study, which is to describe nursing students’ experiences of learning by means of a supervision model based on close patient-related work during clinical placement. The meaning units were documented in computer tables, condensed into a descriptive text, and labeled with a code (Table 3). The codes were grouped according to similarities in accordance with Graneheim and Lundman. 28 After identifying subcategories, they were grouped into categories, and finally, derived a theme that captured the overall meaning of the statements. Throughout the steps, a back-and-forth movement between the data and the categories took place. All authors continuously discussed the data analysis and emerging content categories until an agreement was reached. To confirm the interpretation of the students’ descriptions, quotations were included in the results section.
The various steps of the analysis process.
Ethical consideration
In accordance with the ethical principles of the Declaration of Helsinki,34 the participants received both verbal and written information about the study's aim, method, and how the results will be used. Before the participants provided their informed consent, it was stressed that participation was optional and individuals could choose to withdraw at any point. To avoid the risk of identifying the participants, information in the quotations that could possibly be linked to a participant was deleted and the interviews were coded and not numbered in the quotations in the order in which they were conducted. The confidential information gathered in the study was stored securely to prevent unauthorized access. According to Swedish law §3 (SFS 2003:460), 35 no ethical approval is needed for this type of study as it does not contain sensitive personal data.
Findings
In the analysis, the main theme ‘A scaffolding for learning and establishing a professional identity’ was identified, which implies that learning with the model can be likened to scaffolding. The three categories could be understood as a process for nursing students’ learning in which the scaffolding was gradually reduced in line with their ability to act independently and establish a professional identity. The subcategories represent the different strategies used by the students. The results present the students’ insights and understanding as a continuous interlinked process for establishing a professional identity (Figure 1).
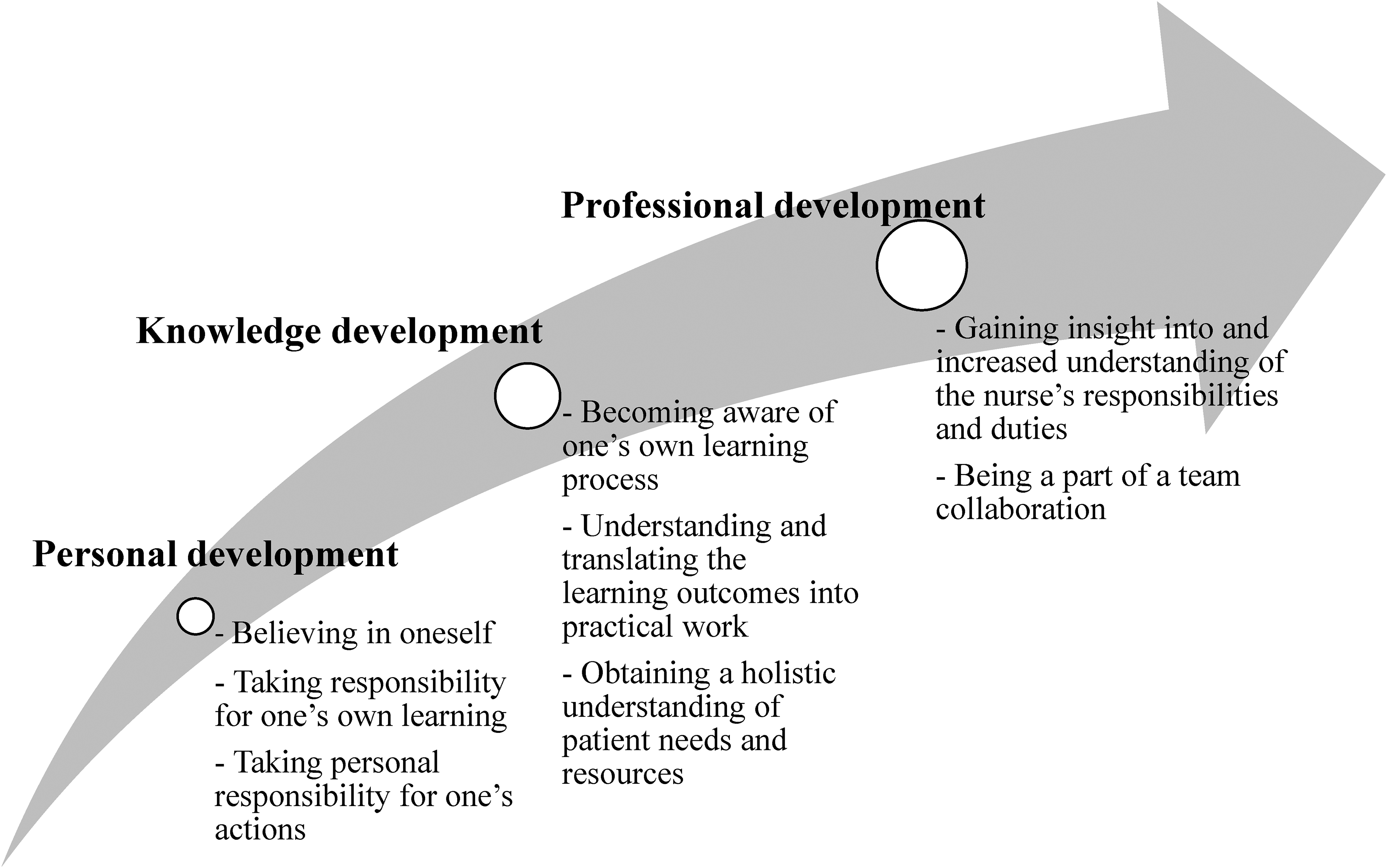
Presentation of learning with a student-centered supervision model based on patient-oriented care as a scaffolding for learning and establishing a professional identity.
Personal development
Personal development meant that the students’ self-confidence increased and that they became aware of and took personal responsibility for their studies.
Believing in oneself
Overall, the nursing students expressed that practical experiences and the structure of the model had given them the strength to believe in themselves and their work. They felt safe when working with the instructions in the folder and gained increased self-confidence because they knew what was expected of them. The model could reduce tension and they began to trust themselves and what they could accomplish in accordance with their responsibilities. The students felt that they could work independently, while supervisors were close at hand when needed. They also expressed that they had grown as a person, dared more, and could take more initiatives. Yes, above all, I have gained a lot of confidence about learning with this model. I have grown in my role by using my own initiative to follow the patient. Yes, I have grown as a person and dare to take the initiative. (Interview 1)
Taking responsibility for one's own learning
Based on the learning objectives, the folder contained instructions and tasks written as a plan of what to practice. The students expressed that the plan made them take responsibility for their own learning, which they liked and thought was fun. Their wish to develop was stimulated by reading, practicing, performing various tasks, reflecting, and documenting. In cases where they needed more help, they first observed the supervisor performing the task, after which the supervisor demonstrated it and provided instructions before they tried and practiced it themselves. I want to move on, learn more, develop, become independent and confident. That there is a good plan for how to get there is great. I have not felt that in my previous clinical placement. (Interview 8)
Taking personal responsibility for one's actions
The students stated that the supervision model was clear, simple, and gave them a structure to follow. They described that working with the model helped them to gradually increase responsibility until they were autonomous with full responsibility for their own actions. Yes, you get a patient first and then get more responsibility each week, like a staircase. Then I started to make my own decisions but double-checked with the supervisor for the sake of patient safety. (Interview 5)
The work became concrete. The students could plan the day in the patient's room together with the patient and other staff. Knowing that supervisors were nearby made them feel safe and they became self-sufficient more quickly and took responsibility for their actions. I am responsible for the patient and my actions. Yes, for example, I call the doctor myself, if necessary, do not ask my supervisor first. (Interview 12)
Knowledge development
Knowledge development involves students’ awareness of their learning process, as well as understanding and translating the learning outcomes into practical work.
Becoming aware of one's own learning process
The students explained that they became aware of their own learning process with the help of the documentation in the folder, reflection, and making notes. Their knowledge development, what they learned, and what they needed to practice became clearer. The model has had a positive effect on my learning. I see my own development. Yes, with examples of what I have experienced. I have a clear picture of what I have learned. (Interview 4)
An important part of the students’ learning process was reflection with a supervisor and fellow students. The supervisors were always close but not necessarily the same person for every reflection. The experiences of different supervisors were seen by the students as a strength, while the reflection and learning were based on the students’ own experiences and knowledge. In the interviews, the students often highlighted the significance of reflection for their learning process. We used to talk and reflect after we took care of our patients. Yes, the supervisor and I reflected on how it had gone and what we had done. We reflect every day. It is interesting to listen and reflect with different supervisors as they have diverse experiences to share. (Interview 7)
Understanding and translating the learning outcomes into practical work
During the clinical placement, the students experienced the content of the model as a pedagogical tool to help them translate the learning outcomes into practical work. It became clear what would be learned, as well as how and why. The importance of theory for practice became more understandable. The model has been helpful in achieving the course objectives. The goals became clear as there is so much to do in this ward. All course objectives could be met, yes, through participation, a holistic approach, security and all the work steps. I can see the connections between the goals and the actions. (Interview 10)
Obtaining a holistic understanding of patients’ needs and resources
The students followed the patients through the whole care chain and looked after all patients to whom they were assigned. The art of caring for the patient was enhanced. They expressed that they gained a holistic understanding of patient needs and resources. The students stated that the tasks helped them to understand both the parts and the whole, providing knowledge about everything concerning the patients, such as blood tests, wound care, documentation, communication, and nursing. I followed the patients from the time they came to the ward until they went home. The patients came in very poor condition, I was involved in the care process by doing assessments, knowing why you do such examinations, seeing what they show, being with the patients during the examinations, communicating to the patients when their health improves, and being involved with relatives’ questions and worries as well. Yes, I see how the patient gets better and if new needs arise in the meantime. Yes, I know a lot about patient care now, the holistic aspect. (Interview 9)
Professional development
Professional development means that the students gain insight into and increased understanding of nurses’ professional work.
Gaining insight into and increased understanding of the nurse's responsibilities and duties
The students expressed that during the clinical placement, they became closer to their profession as registered nurses. They gained insight into and increased understanding of a nurse's responsibilities and duties. When they needed to plan the day themselves the duties became more visible. Instead of only making efforts now and then, they followed all the nurse’s duties throughout the day. They felt that they grew in the role of a nurse, the care process became clear to them, and they also found it easier to organize the work on the ward. I automatically perform check-ups, for example, in those places with a risk of pressure ulcers. Because it is important to check those places. I also now see the importance of nutrition and fluid lists. All that kind of thing started to fall into place, and I really began to understand the nurse's duties and responsibilities. (Interview 5)
Being a part of team collaboration
The students described wanting to be part of team collaboration and the environment stimulated them to interact with other professions, for example, physicians, physiotherapist, occupational therapist, counsellor, and enrolled nurses, but also fellow students. They stated that collaboration is an important part of the nurse's profession for ensuring high-quality patient care. I have gained experience of healthcare itself… and learned the importance of teamwork. Collaboration is very important in many different situations for the patient to feel as good as possible. (Interview 4)
Discussion
The aim of this study was to describe nursing students’ experiences of learning from a student-centered supervision model based on patient-oriented care during their clinical placement. The key findings showed that the model is an uncomplicated pedagogical tool that serves as a scaffolding for learning and establishing a professional identity. Scaffolding was an important part of professional development and the higher the knowledge development, the less scaffolding is needed. According to Vygotsky's sociocultural perspective, 20 scaffolding is a type of educational tool that supports a person's learning, a kind of help that facilitates self-help. The scaffolding creates meaningful social relationships with the aim of developing a learning process based on reflection and progression of knowledge.36 This means that by using reflection supported by supervisors as well as fellow students, the nursing students could make significantly more progress. By practicing in a supported way, they extended their knowledge and formed new habits. Then, when the support was gradually removed, the students learned to use their knowledge independently. Student learning was thus seen as a process in which the scaffolding was gradually removed in line with the students’ ability to act independently and create a professional identity. Being able to discuss and reflect on their practical experiences was helpful for structuring the process of learning from experience. 19 This learning process includes reflection, which is in line with previous research. 11
The result showed that work-integrated learning (WIL) is a possible way to strengthen the pedagogical learning environment during clinical placement. WIL concerns creating conditions for student learning that enable better understanding and performance. 21 The application of theoretical knowledge in clinical placements can aid the learning process through WIL.37 The model can be seen as a form of WIL, as it was designed in collaboration between the university and the healthcare organization. By creating bridges between learning and application, the application becomes a natural part of learning. The goal is to bridge the gap between theory and practice by shaping an environment where both perspectives can work together.38 Integrating theoretical and practical knowledge is important for the students’ personal, knowledge, and professional development. The potential lies in the opportunity to discover and take advantage of collaboration, as WIL is a process that takes place between working life and university. Knowledge drawn from learning contexts in both education and working life is necessary for inclusive and sustainable knowledge.
The result revealed that nursing students’ experiences of learning became a process of personal development. They felt safe, believed in themselves more, and experienced taking more responsibility for their own learning and actions. The model is well-designed and instructive. In research, it has been stated that a well-organized clinical placement provides the students with support and responsibility. 3 Professional identity development requires a supportive learning environment that facilitates reflection on theories and underlying practice. 1
In student-centered learning the supervisor becomes a facilitator and a resource person, while the student sees her-/himself as an independent person. 17 Working with the instructions contained in the folder, being given responsibilities, following the care path of assigned patients together with instruction and reflection seem to be a good concept for learning, but also contribute to a more holistic understanding of patients’ needs and resources. The model content has a balance between task and process orientation, which constitutes different kinds of challenge for students. Communication, reflection, and feedback are important components of the model and previous research has demonstrated that this contributes to student learning. 5
The result showed that the model ensures the achievement of learning outcomes and the creation of a pedagogical learning environment during the clinical placement. By working with the tasks, i.e. nursing activities, the nursing students better understood and could translate the learning outcomes into practical work with the patient. Instead of only specific interventions for the patient, they considered the whole life situation. Being present with the patient is the most effective way to develop ethical competence and professional identity through focusing on nursing care and the patient's needs. 1
In this way, the student also became aware of her/his own learning process as the learning started from the student. The student knew what was expected from her/him. Gusar 15 claims that if students receive supervision based on their own situation, they are in a better position to achieve the learning outcomes.
By following the patient and being responsible for specific care rooms at the ward, the students expressed that they gained a holistic perspective on patient care, which can enhance the quality of nursing. The learning is followed up regularly and planned in a structured way. The method also benefits the care providers, as the responsibility for the students’ supervision and development is distributed to more than one person, which reduces the risk of having no supervisor due to, for example, illness or if the supervisor changes workplace.
The three categories with subcategories present the students’ insights and understanding as a continuous process with interlinked strategies for establishing a professional identity. In the first category, the students learned to believe in themselves and take responsibility for their own learning and actions. In the second category, the students became aware of their learning process. They were able to understand and translate the learning objectives into practical work and thus more easily gain a holistic understanding of patient needs and resources. In the third category, the students gained increased knowledge of and insights into the nurse's work and responsibility as well as the importance of team collaboration in a professional context. The model ensures the students’ development of a professional identity by providing them with insight into and increased understanding of the nursing profession.
The clinical placement is a crucial part of the development of professional competence and constitutes a bridge to future professional life.39 The clinical setting is crucial for nurse education, but it undergoes continuous changes due to challenges in the healthcare system. These challenges include factors such as a growing number of students and limited availability of clinical placements and supervisors.
There are different forms of supervision. In traditional supervision, the student usually follows the supervisor during the course of the work, where the focus is on teacher-driven learning. 8 Another form is student-driven supervision with examples of models for collaborative learning, for example, Peer Learning, which has been introduced in several contexts. 9 Collaborative learning cultivates a safe learning environment, improved self-confidence among students, and prepares them for their future profession. 10
There are various supervision models, as outlined in the background.8–10 A distinguishing feature of this particular model is its focus on the entire care of selected patients instead of merely following the supervisor's tasks. This reduces the student's reliance on a single supervisor during practical training, proving advantageous in a constantly changing clinical environment. The supervision model provides a greater opportunity to enroll more students in the departments but, if so, more equipment is needed, such as medicine handling assistance and other devices that are a prerequisite for flexible care. It is also important that ward staff understand that education is a natural task for nurses and supervisors. Research about supervisors’ perspectives on working with the model is necessary and has been planned, to provide more information about the model.
Methodological considerations
The following methodological considerations ought to be discussed. Although the small number of interviews can be seen as a limitation, the purpose of qualitative content analysis is to highlight individual experiences, not to generalize. 27 The amount of data provides enough patterns and categories to answer the research question. The fact that half of the participants were from semester 6 may impact the results due to them having more experiences. However, students from other semesters expressed similar views on the learning environment in the ward. If only semester 6 students participated, we could not be certain about various results, which might be due to their earlier experiences. Nevertheless, they have had experiences of other models and find the present one beneficial for their learning.
The fact that the results are based on statements from Sweden raises questions about their generalizability. Despite the ongoing COVID-19 pandemic, the authors attempted to conduct their interviews in a similar manner and frequently discussed how to ensure that they were as similar as possible. The participants all expressed satisfaction about having the opportunity to choose the time and location of the interview and whether it should be face-to-face or via Zoom. An oral summary at the end of each interview gave the participants an opportunity to add or change information. This procedure makes it possible to confirm the validity of the participants’ answers. 27
The interviews were transcribed verbatim to increase reliability. All researchers read the interviews and thereafter discussions were held until agreement was reached about the subcategories, categories, and themes. A back-and-forth movement between the data and the categories took place throughout the analysis process. 28 Quotations from the interviews are presented to strengthen credibility,33 which enables readers to assess the degree to which the results are credible and transferable to other settings. The results can contribute to a deeper understanding of the student-centered supervision model for patient-centered care and continue the discussion about supervision during clinical placement for nursing students.
The researchers have professional experience as nurses and nursing teachers, which can be seen as a strength as it facilitated their understanding of the participants’ experiences of learning from a student-centered supervision model based on patient-centered care. However, experience and pre-understanding can constitute an obstacle, 27 as they can lead to an unconscious bias. To prevent this, the researchers used an interview guide and had a critical attitude during the analysis to avoid over-interpreting the material.
Conclusion
The findings illustrate the process of nursing students’ learning of patient-oriented care based on the supervision model, which was described as accessible, clear, simple, and gave them a structure to follow. They described working with the model as reducing tension and anxiety, which enabled them to focus on learning. The supervision model is a scaffold for learning, in which the scaffolding is gradually reduced in line with the student's ability to act independently and establish a professional identity.
Relevance to clinical practice
In healthcare, there is a need for new innovative approaches to enhance clinical learning for nursing students. It is essential that the students learn with and from each other in collaboration with other professions for a working life as a registered nurse. The present study indicates that a student-centered supervision model based on patient-oriented care can enhance the students’ experiences in the practice setting and help maximize opportunities for learning and support quality nursing. Therefore, this model seems to have the potential as an educational approach that supplements the more conventional of supervision methods in clinical practice.
Footnotes
Acknowledgments
We acknowledge Monique Federsel for reviewing the English language in this manuscript. We would like to thank Ann-Charlotte Nilsson for her work with the development of the model and the nursing students for their participation.
Author contributions
All authors (AJ, JSM, SP) made contributions to the study's design. AJ and JSM gathered the data and all authors participated in the analysis and interpretation. All authors participated in drafting and critically revising the article for intellectual content.
Availability of data and materials
Additional data files in Swedish are available upon request to the corresponding author. The data are not publicly available since they contain details that may jeopardize the confidentiality of the research participants.
Conflict of interest
The authors declare that there is no conflict of interest.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
