Abstract
A 78-year-old man presented with exertional dyspnea and lower leg edema for 3 months. He had a 25-year history of the exposure to asbestos, and pulmonary asbestosis was diagnosed 3 years ago. An echocardiogram and cardiac catheterization were compatible with constrictive pericarditis. He underwent pericardiectomy. On the right ventricle, the pericardium was firmly attached to the epicardium. Pathological examination confirmed the thickness of the pericardium and epicardium without specific findings indicating pathogeneses.
Introduction
Constrictive pericarditis originates from any causes such as tuberculosis and connective tissue diseases, and it can be secondary to cardiac surgery and radiation therapy. Herein, we report a case of asbestos-related constrictive pericarditis.
Case report
A 78-year-old man presented with exertional dyspnea and lower leg edema for 3 months. He had a 25-year history of exposure to asbestos while he worked for a building company handling insulation materials, and pulmonary asbestosis was diagnosed 3 years ago.
On examination, normal heart sounds and fine crackles on bilateral lung fields were audible. Moderate pretibial pitting edema was recognized with a slightly enlarged liver with moderate ascites. White and red blood cells and platelets were within normal limits. The C-reactive protein level was 25 mg L−1. The blood urea nitrogen level was 250 mg L−1 with a creatinine level of 8.6 mg L−1. The total bilirubin level was 21.3 mg L−1 without an elevation of hepatic deviation enzymes. Anti-nuclear and anti-centromere antibodies were negative. Perinuclear and cytoplasmic anti-neutrophil cytoplasmic antibodies were also negative. Tumor markers of cytokeratin19 fragment, pro-gastrin-releasing peptide, squamous cell carcinoma antigen, neuron-specific enolase, and carcinoembryonic antigen were within normal limits. Pericardial effusion was negative for tuberculosis with a negative tuberculosis-polymerase chain reaction. Rate-controlled atrial fibrillation was observed by electrocardiogram. Chest X-ray and computed tomography revealed bilateral pleural thickness and slightly damaged lower lung fields with a widened cardiothoracic ratio of 71% (Figure 1). An echocardiogram showed pericardial thickness with a moderate pericardial effusion, the dilatation of the inferior vena cava, and a left ventricular ejection fraction of 52%. Cardiac magnetic resonance imaging indicated the thickness of the epicardium (Figure 2). Cardiac catheterization showed a typical dip and plateau phenomenon in the right ventricle and a central venous pressure of 20 mmHg.
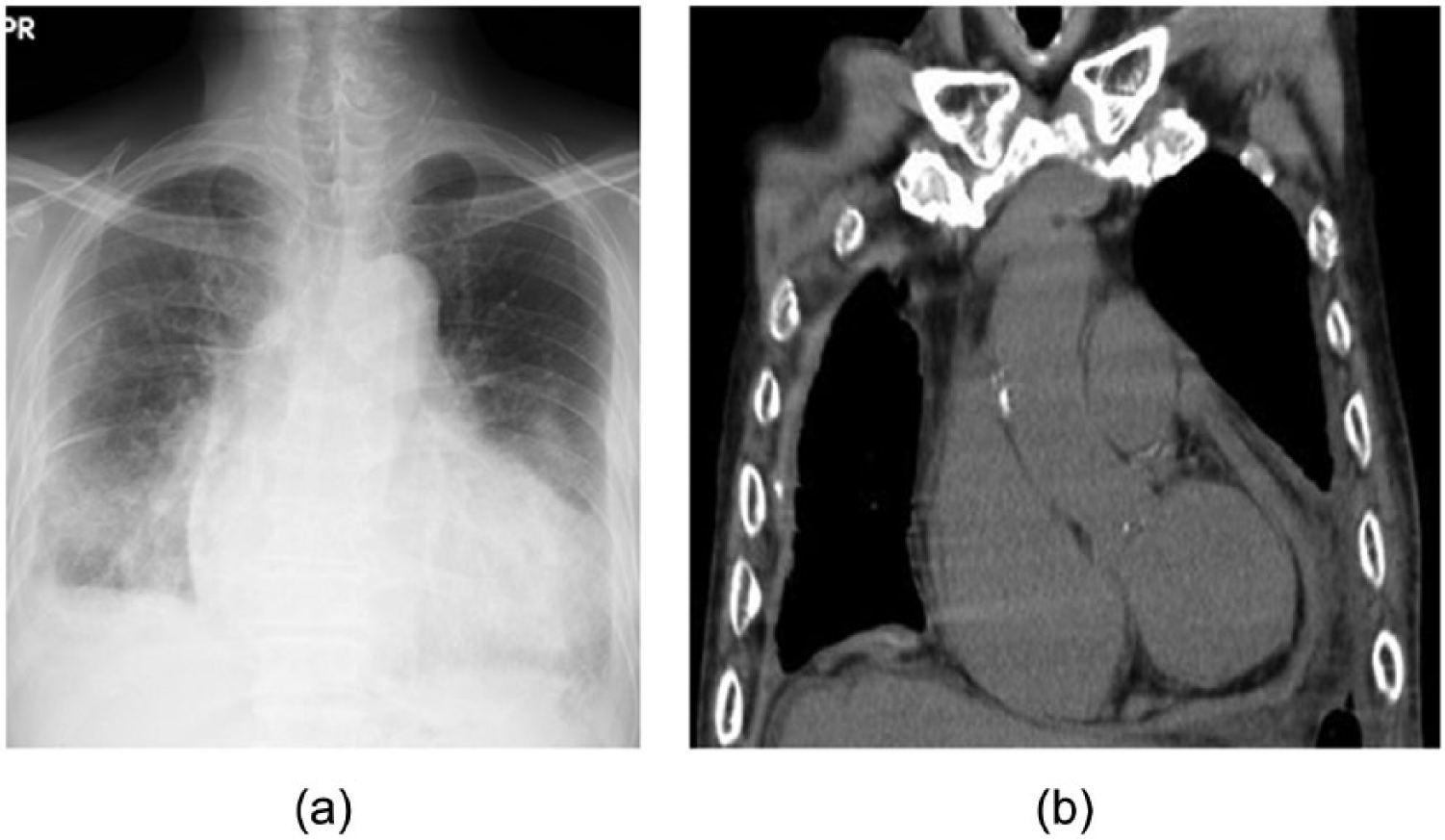
Preoperative chest X-ray and computed tomography. (a) Bilateral pleural thickness and an enlarged cardiothoracic ratio of 70% can be seen. (b) The pleura of the right lung is thicker than that of the left lung, and a pericardial effusion can be seen.
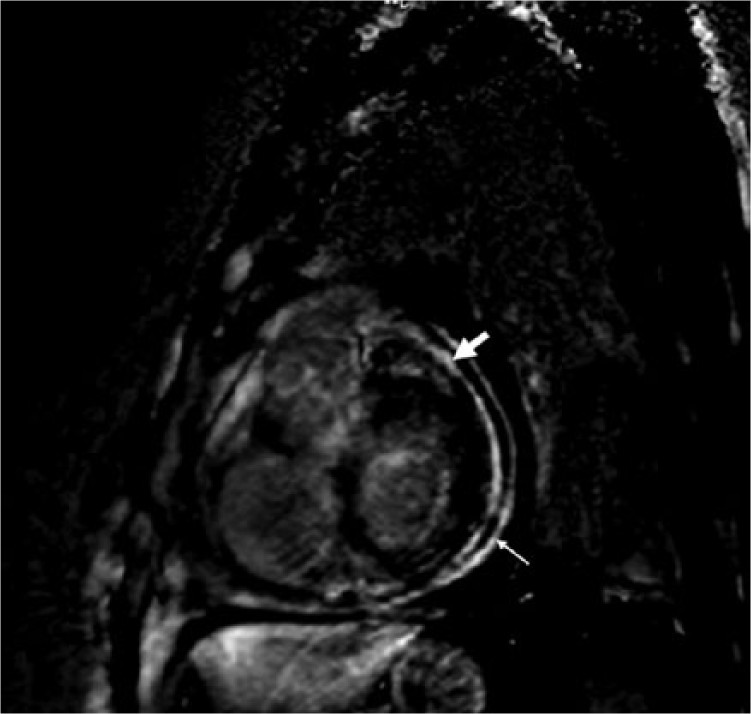
Preoperative cardiac magnetic resonance imaging. A thickened epicardium (wide arrow) is visible and is associated with a thickened pericardium (narrow arrow).
The patient underwent pericardiectomy through a median sternotomy. The pericardium between the right and left diaphragmatic nerves was removed. On the right ventricle, the pericardium was firmly attached to the epicardium, and it was also resected. The central venous pressure dropped to 14 mmHg on the fifth operative day, and the peripheral edema gradually regressed. A pathological examination confirmed the thickness of the pericardium and epicardium without specific findings indicating pathogeneses (Figure 3). The patient was doing well after 6 months of operation without ascites and pretibial pitting edema.
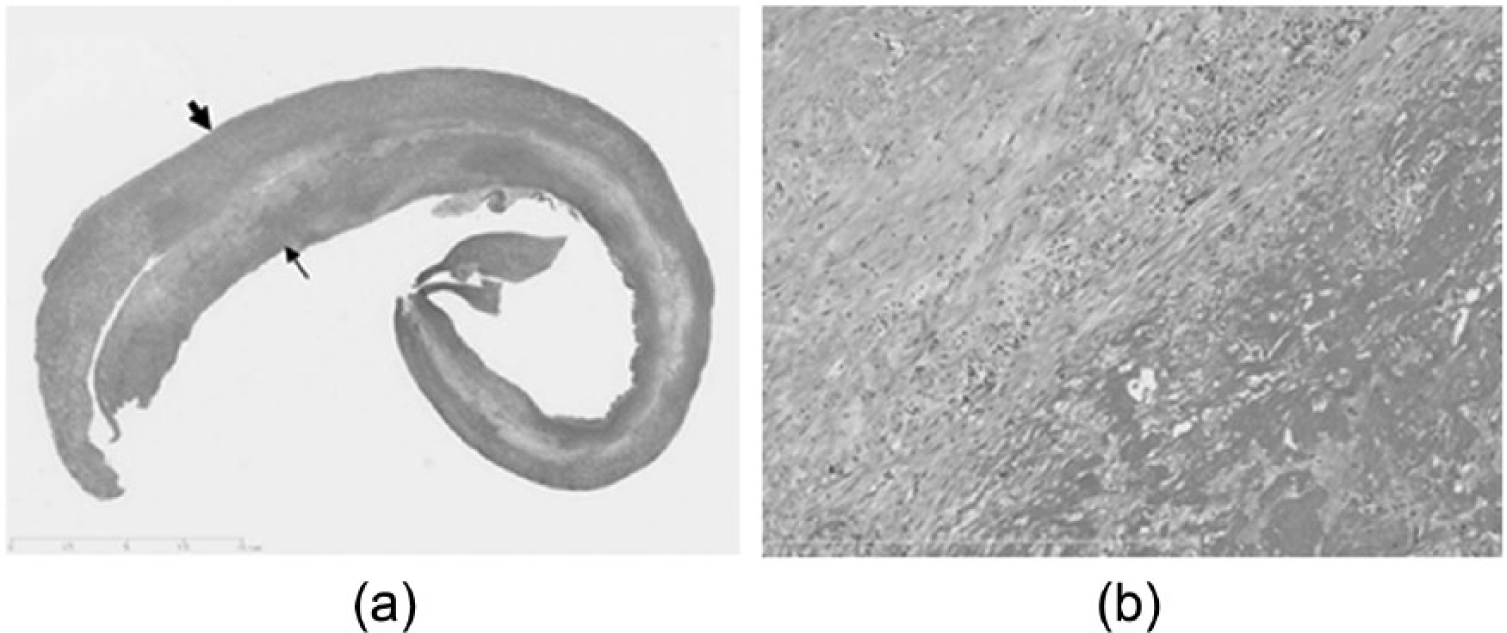
Pathology of the resected pericardium and epicardium (hematoxylin and eosin stain). (a) Loupe image. The upper layer is the pericardium (wide arrow) and the lower layer is the epicardium (narrow arrow). (b) Lymphocyte infiltration can be seen without specific findings indicating pathogeneses (magnification, 20×).
Discussion
Constrictive pericarditis originates from different causes such as tuberculosis and connective tissue diseases, and it might be secondary to cardiac surgery and radiation therapy. Asbestos-related constrictive pericarditis has rarely been reported.1 –4 Asbestos-related diseases are not limited to the thoracic cavity but to the pericardium. 5 Some investigators reported cases with non-constrictive asbestos-related pericardial effusion or malignant mesothelioma of the pericardium.6 –8 However, the diagnosis of asbestos pericarditis is never conclusive, and it is just done by approximation or exclusion.
In 1988, Fischbein et al. 1 showed a pulmonary asbestosis patient who had constrictive pericarditis. A long history of asbestos dust exposure without evidence for tuberculosis led to the diagnosis of asbestos-related pericarditis. Davies et al. 2 reported three cases of pulmonary asbestosis with constrictive pericarditis. One patient was treated by pericardiectomy, and two died. They concluded that asbestos produces progressive fibrosis of the pericardium similar to diffuse pleural thickening and that this condition may develop after relatively short or light exposure.
Rudd referred to the relations between asbestos exposure and benign pericardial effusion, thickening, and calcification, which are analogous to the effects of asbestos on the pleura. 9 The author has pointed out the usefulness of magnetic resonance imaging for the diagnosis of the pericarditis.
Abejie et al. 10 also presented a case with a 30-year exposure to asbestos. A high-resolution computed tomography scan of the chest demonstrated dense calcification in the pericardium associated with pleural thickening and nodularity consistent with pleural asbestosis in their case.
These above-mentioned authors diagnosed asbestos-related pericarditis based on the patients’ history of asbestos exposure, clinical evidence of both pleural asbestosis and pericarditis without tuberculosis, and other possible causes for pericarditis. In our patients, long-term exposure to asbestos, a history of pleural asbestosis, clinical constrictive pericarditis, and nonspecific pathological findings led to the diagnosis of asbestos-related constrictive pericarditis. Pericardiectomy should result in effective clinical results for any constrictive pericarditis.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
