Abstract
Background
Innovations are essential to meet the needs of people with MS (PwMS), particularly in addressing delays in diagnosis and treatment, and in supporting patient self-management.
Objectives
To evaluate the real-world use and outcomes of digital technologies and holistic management strategies for MS at a UK Centre.
Methods
Digital tools for PwMS included Patients Know Best (a personal health record) and CONNECTPlus® (an educational app). Tools for healthcare professionals included Infoflex (a clinical database with MSProDiscuss for assessing disease progression). A Healthy Lifestyle Clinic was introduced to promote brain health. The impact of these interventions on time-to-diagnosis, time-to-disease-modifying therapy (DMT) initiation, non-elective admissions, and hospital costs was evaluated retrospectively from 2018 to 2023, comparing pre-intervention (2018–2019) with post-intervention (2020–2023) periods, while accounting separately for COVID-19 years (2020–2021).
Results
Trends indicated a higher likelihood of disease progression in patients with delayed MS diagnosis (p < 0.001), and a reduction in time from diagnosis to DMT initiation, from an average of 23.5 to 5.8 months (p = 0.024), post-MS Infoflex disease management database implementation. Non-elective admissions and healthcare costs also decreased compared to neighbouring hospitals.
Conclusions
Digital and holistic interventions were associated with positive trends in MS care delivery. Further research is needed to validate these findings.
This is a visual representation of the abstract.
Keywords
Introduction
Multiple sclerosis (MS) is a multifaceted disease with a high degree of inter-patient variability. 1 Due to its complexity, there is no ‘one size fits all’ approach to disease management and a tailored approach is required for people with MS (PwMS); however, many healthcare systems cannot afford the necessary time and/or resources required to provide close, personalised care. 2 The findings of a national UK audit of 70 MS services revealed that most were struggling with expanding caseloads and staffing shortages. 3 These challenges have cost implications, such as emergency department/non-elective visits by patients increasing healthcare resource utilisation.
Despite large treatment advances over the last 20 years, unmet needs in the management of MS remain, including prompt diagnosis, treatment optimisation, timely identification of treatment failure and accurate reporting of symptoms and relapses by patients.4,5 The preservation of neurological reserve in PwMS is of the utmost importance, since ‘time is brain’ and a delay in diagnosis or treatment initiation can lead to irreversible neuronal deficits for patients. 6 Innovations to increase service efficiency and save money whilst supporting patients through addressing unmet needs are greatly required.
The NICE guidelines, and others, recommend a comprehensive review of care by a neurologist at least once per year for PwMS.7–9 Consequently, PwMS must manage many aspects of their disease day to day 10 ; however, some may lack the knowledge, skills and confidence to manage their health and well-being on a daily basis. 11 Self-management interventions can support patients and are associated with reduced disease burden, improved quality of life for patients,10,12 lower healthcare utilisation and less wasteful resource use across primary and secondary care. 13 With the ever-evolving treatment landscape in MS, there is a pressing need to make the best use of innovations that support healthcare systems and enable PwMS to become advocates of their own MS care. 2 Furthermore, beyond disease-modifying therapies (DMTs), it is essential that PwMS receive support for a more holistic approach to disease management. 14 Provision of lifestyle information and education to patients can support their self-management journey to living well with MS. Healthy living – through diet, exercise, reduction of modifiable risk factors and improvement in overall well-being – is known to be important, not only in the general health of PwMS but also on their brain health and MS progression.14–19
Digitisation of healthcare has enabled new dimensions of self-care for people with chronic conditions, and is becoming increasingly relevant for HCPs in the management of MS.20,21 Digital healthcare for PwMS may include mobile phone apps targeting self-management, such as medication reminders and reporting of side effects 20 and wearable technology to assess sleep quality, mood and fatigue, and measure activity levels, gait, balance and lower/upper limb function, enabling passive collection of patient data and patient-reported outcome measure (PROM) data for a more comprehensive, representative assessment of patients outside of the clinic.20–22,23 For HCPs, these technologies have the potential to improve disease assessment, allowing remote tracking of patient symptoms and better monitoring of lab results, thus facilitating patient–clinician communication and supporting more efficient and personalised disease management. 24
In this article, we describe real-world application and resulting outcomes of cutting-edge digital technologies (integrated with existing electronic health records) and holistic disease management approaches, aimed at enhancing personalised MS patient care within the Torbay and South Devon National Health Service (NHS) Foundation Trust, in the United Kingdom.
Methods
This was a retrospective service evaluation conducted over a five-year period from 2018 to 2023 at Torbay and South Devon NHS Foundation Trust. The study period was divided into a pre-intervention baseline (2018–2019), an early implementation phase with the introduction of digital tools in 2020, and a post-intervention period (2020–2023) to evaluate longer-term outcomes. The COVID-19 pandemic (2020–2021) was accounted for separately to isolate any potential effects on healthcare delivery. The study flow is illustrated in Figure 1.
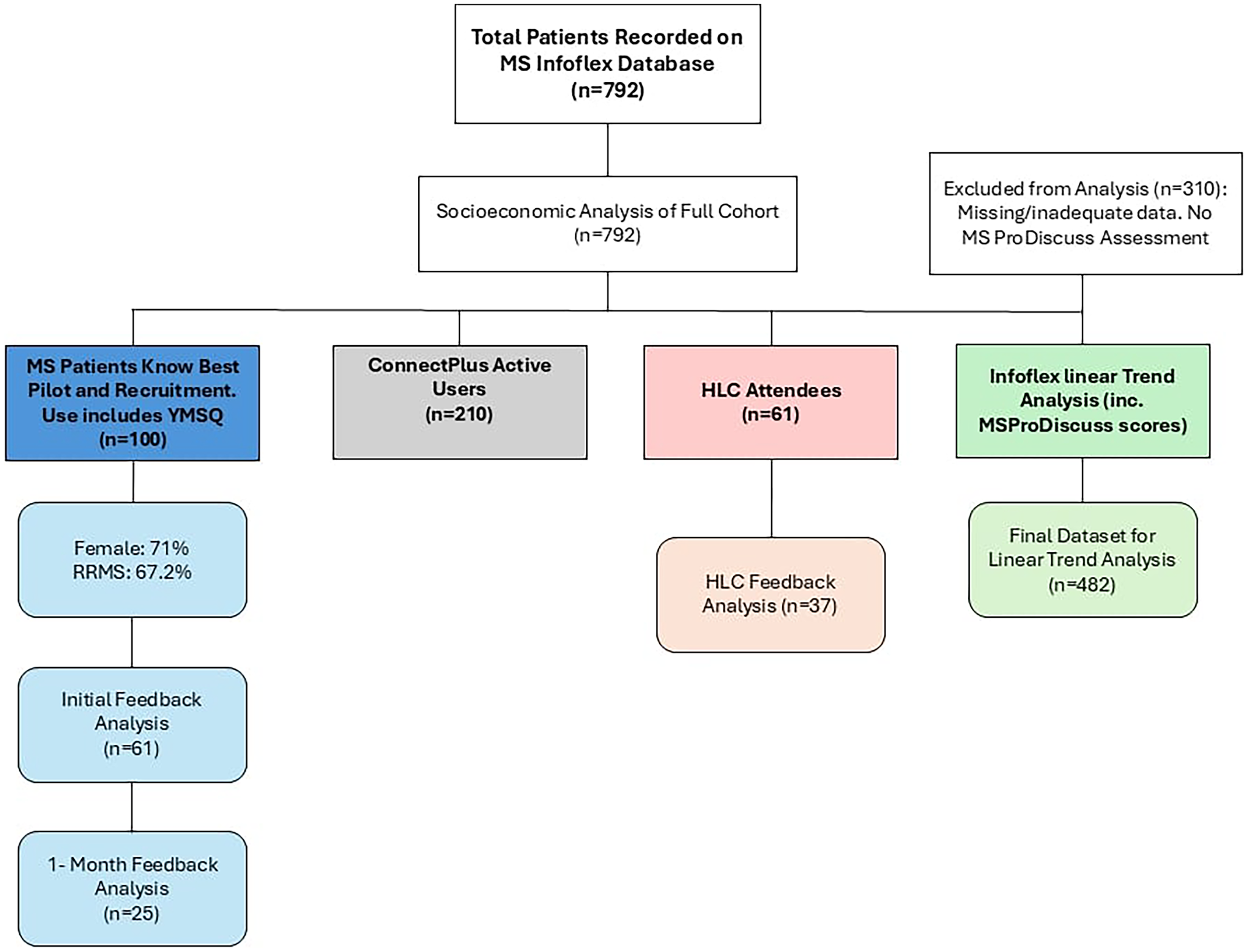
Flowchart for study participants.
Patient digital tools
MS Patients Know Best (PKB): PKB is a personal health record system for PwMS, that provides a single access point for their health information, allowing users to share selected information with healthcare providers (HCPs), family, and carers. 25 Key features of PKB are summarised in Table 1.25,26 Integrated with the NHS app, PKB enables entry of patient-reported outcome measures for ongoing monitoring of disease status (Supplementary Figure 1). 25
Summary of the digital and holistic interventions implemented for care of PwMS.

HCP: healthcare professional; HLC: healthy Lifestyle Clinic; NHS: National Health Service; PKB: Patients Know Best; PROM: patient reported outcome measures; PwMS: people with MS; YMSQ: your MS questionnaire.
A trial of PKB involving 100 PwMS over a 3-month period in 2021 demonstrated initial engagement, with a dedicated coordinator assisting in platform facilitation. Following this time, these 100 registered users were allowed and encouraged to continue using the platform.
CONNECTPlus® App: The CONNECTPlus® app offers video information, mindfulness and well-being podcasts, hospital contact details, and virtual appointments for PwMS, supporting remote self-management and access to care (Supplementary Figure 2). 27 Key features are summarised in Table 1.
Healthcare professional digital tools
MS Infoflex: This clinical management database provides a comprehensive, real-time view of patient information, replacing paper-based systems and supporting clinical decision-making with automated alerts. Key features are provided in Table 1. 28
MSProDiscuss on InfoFlex: MSProDiscuss, integrated within Infoflex, is a validated digital tool that assesses patient relapses and symptom impacts over the past 6 months (Supplementary Figure 3). It uses a traffic light system to predict disease progression risk, aiding in proactive management. Red indicates a patient likely showing signs of progression; ‘amber’, a patient who could possibly be showing progression signs; and ‘green’, a patient unlikely to be showing signs of progression, at a given point in time (Table 1).29,30
Healthy lifestyle clinic (HLC)
A Healthy Lifestyle Clinic, introduced in 2019, educates newly diagnosed PwMS and their families on disease management and healthy living. During COVID-19, HLC sessions were conducted online. The clinic received the Brain Health Team Award in 2022. Key features of the HLC are provided in Table 1.
Data analyses
All service evaluation data were collected retrospectively. The analytical approach was primarily descriptive, complemented by robust quantitative assessments. The study period was divided into a pre-intervention baseline (2018–2019), the introduction of digital tools in early 2020, and a post-intervention period (2020–2023). The potential effects of the COVID-19 pandemic on healthcare delivery were accounted for separately, covering the years 2020 and 2021.
Utilisation and satisfaction metrics for MS PKB were derived from site-specific data, encompassing user counts, demographics, login frequency, and feedback collected after first use and again one month later. The impact of digital interventions on patient outcomes was evaluated with respect to time from official diagnosis to DMT initiation, variations in MSProDiscuss scores relative to the time since diagnosis, and non-elective admission rates, along with associated cost implications, before and after digital tool implementation within the Trust.
To quantify the effectiveness of these interventions, a linear trend model was applied to a dataset of 482 modelled observations using Tableau (v2023.2), analysing the time from symptom onset to diagnosis against the sum of standardised total MSProDiscuss scores. Additionally, a Chi-squared test was carried out in Python (v3.11) to assess differences in time to DMT initiation between the pre- (2018–2019) and post-Infoflex (2020–2023) periods. A two-tailed analysis was conducted with an alpha value set at α = 0.05.
Admissions and the causes of admissions for PwMS, as well as the associated costs, were assessed using the Hospital Episode Statistics (HES) data service from NHS hospitals. This focused on healthcare utilisation and hospital admissions related to Multiple Sclerosis (MS) and Urinary Tract Infections (UTIs). HES data provided comprehensive records on hospital admissions, readmissions, and healthcare costs, covering both MS and UTI-related episodes. Costs were calculated based on hospital admissions, including diagnostics, treatments, and length of stay, with adjustments made using NHS reference costs. DMT costs for MS patients were included, reflecting both inpatient and outpatient treatments. Inflation adjustments were made to account for cost differences over the five-year period.
Ethical statement
This service evaluation was judged by the Torbay and South Devon NHS Foundation Trust institutional review board to be exempt from requiring ethical approval. Data has been compiled from current databases and there was no direct patient participation. Patients volunteered and gave written, informed consent to the collection of opinions, user metrics and anonymised data.
Results
Implementation and utilisation of digital tools at Torbay and South Devon NHS Foundation Trust
MS patients know best (MS PKB)
Following the PKB platform Pilot launch and demonstration in July 2021, 100 PwMS registered, with most accessing the platform via the NHS App. At registration, the majority of patients were female aged 55–64 years, followed by female patients aged 45–54 years (Supplementary Figure 4). The most common diagnosis among the users was relapsing remitting MS (67.2%) followed by progressive relapsing MS (14.8%) and secondary progressive MS (9.8%).
During the 3-month pilot, there was a peak in the number of logins and unique users for PKB; post-pilot, there has been a consistent number of logins, with active users ranging from 20 to 39 per month (Figure 2(a)).

(a) Number of monthly active users (>1 login) of the MS PKB tool during 2021 and 2023, following a 3-month pilot period between July and September 2021, out of a total of 100 registered users. (b) Number of users and sessions of the CONNECTPlus® App between October 2022 and August 2023, out of a total of 210 active users.
Patients were polled for their initial feedback following attendance at a demonstration event, and then again following one month of use. On first impressions, over 96% of patients agreed or strongly agreed that PKB looked like a helpful platform. Over 93% of patients strongly agreed or agreed that Your MS Questionnaire (YMSQ), a tool to help them prepare for their consultations, would help with discussion of their disease activity and symptoms (n = 60). Additional initial patient feedback is provided in Supplementary Box 1.
Following one month of use, 44% of patients strongly agreed or agreed that using MS PKB had given them more confidence in self-managing and living with MS (n = 25), and 76% would recommend using it over to other PwMS. For most patients, the YMSQ took less than 10 min to complete (n = 22), and 73.9% strongly agreed or agreed that YMSQ would help towards better discussion of symptoms and disease progression with their HCP. Additional patient feedback on MS PKB following 1 month of use is provided in Supplementary Box 2.
The most frequently accessed and utilised parts of the PKB platform by patients include ‘Lab Results’, ‘Messaging or Consultations’, ‘Measurements’ and ‘Care Plan’ (Supplementary Table 1).
CONNECTPlus® app
Since its launch in April 2021, 900 PwMS have registered to use the CONNECTPlus® app; of these 33% are aged 35–44 years, 50% are aged 45–54 years and 17% are aged 55–65 years. Most patients (92.7%) use the app via a mobile phone device rather than a tablet. Since its launch, there has been a consistent number of users and logins/sessions (Figure 2(b)). Overall, patient opinion of the CONNECTPlus® app was positive (feedback is given in Supplementary Box 3). Between October 2022 and August 2023, there were 210 active users from Torbay and South Devon Healthcare Trust, with an average of 3.1 sessions per user. The most popular content during this time was videos, ‘Learn About’ articles, podcasts and blogs, and other articles relating to exercises and self-management (Supplementary Table 2).
Healthy lifestyle clinic (HLC)
Patient and family feedback on the HLC was positive. In a poll of 37 attendees (29 PwMS and 8 family members), 100% stated that the amount of information provided and the length of the clinic, were “just right”. Additional feedback included: “the clinic made me think of more ways I can help myself in the way I live”, “I feel positive about making healthier lifestyle choices”, “I don’t feel so alone”, “meeting everyone that has MS and also others caring for someone with MS was really good and makes you feel part of something”, “it was really useful to have different professionals talking about MS together”, and “it was very informative”.
Impact of digital technology and holistic care
Trends towards improved patient management and early detection
The MS Pro Discuss score provides an idea of the likelihood of disease progression in an individual patient. Real-world data collected via MSProDiscuss on MS Infoflex database shows a correlation between score and increased time from symptom onset to diagnosis (Figure 3). Applying a linear trend model to a dataset of modelled observations showed statistical significance (p < 0.0001, r = 0.06), suggesting a higher likelihood of disease progression (red scores) in patients with a delayed MS diagnosis (Table 2). Assessment of the long-term impact of these interventions was not possible due to insufficient follow up duration.
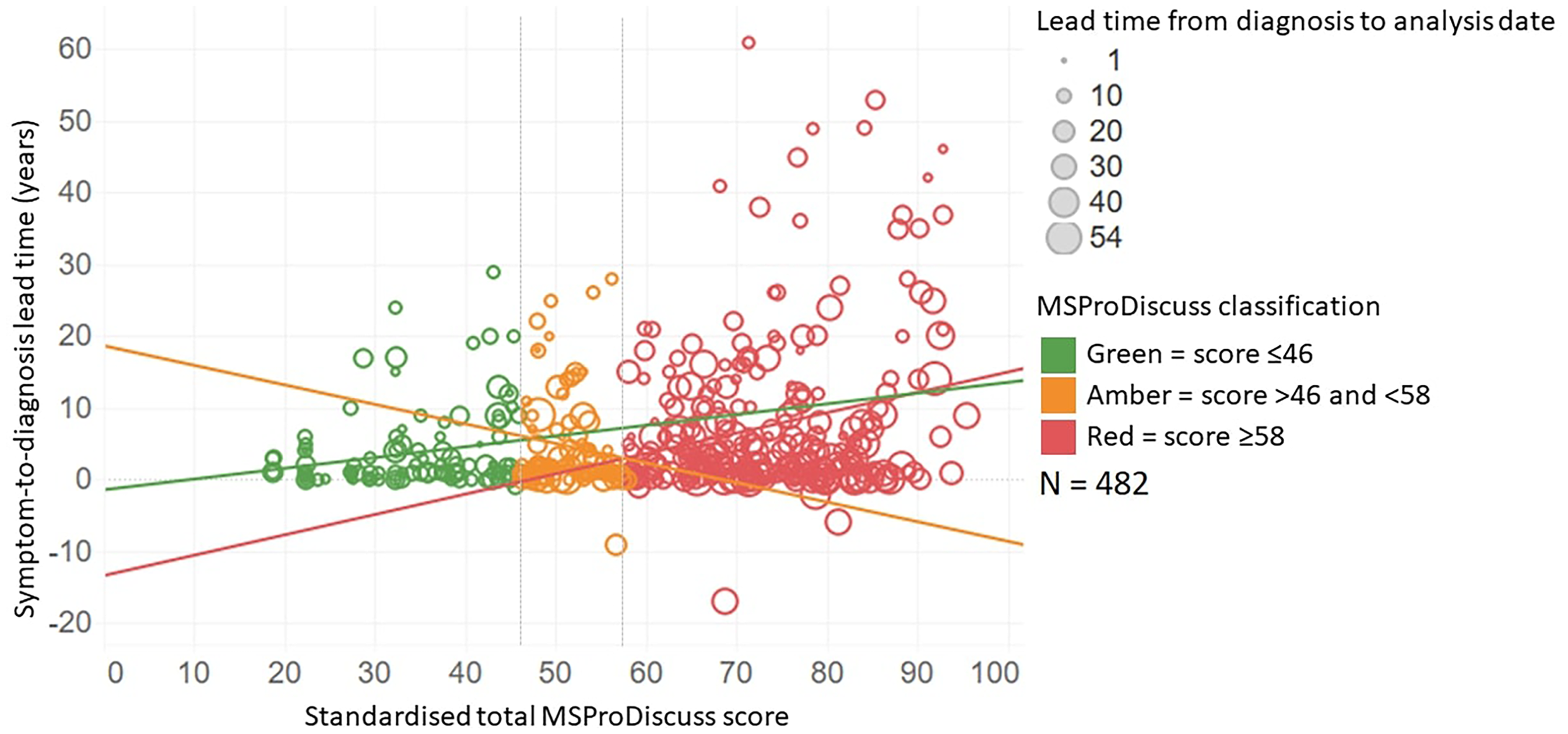
Impact of Symptom-to-Diagnosis Lead Time on Disability (n = 482).
Linear trend model statistical analysis to investigate the impact of diagnosis delay on disease progression, following collection of MSProDiscuss scores on the Infoflex database.

Since launching the MS Infoflex database and integrated MSProDiscuss assessment, the average time from diagnosis to initiation of DMTs has decreased from 18 months prior to use of Infoflex to 0.7 months (green scores). This trend is true for patients with all MSProDiscuss scores (Figure 4; p = 0.024).

Time between diagnosis and initiation of DMTs in PwMS by MSProDiscuss score, pre- and post-launch of MS infoflex database (n = 156).
Trends towards reduction in non-elective admissions and cost savings
We observed a reduction in total non-elective admissions and resulting costs for Torbay and South Devon Trust versus other neighbouring healthcare trusts. Furthermore, in the year 2021–22, there was a cost saving of almost 18% on the previous year (Figure 5(a)). Neighbouring Trusts had costs related to non-elective admissions that were the same or more than the previous years. In the year 2022–23, there was a small increase in costs related to non-elective admissions of around 5% for Torbay and South Devon Trust versus the previous year (Figure 5(b)). Other neighbouring Trusts experienced much larger increases in costs related to non-elective admissions versus the previous year, of around 20–30% more.

Cost of non-elective admissions in (a) 2021–22 (N = 15,620) and (b) 2022–23 (N = 18,360) for Torbay and South Devon versus neighbouring healthcare trusts.
Trend towards reduction in Emergency Department (ED) admissions for healthy lifestyle clinic attendees
With attendance to the HLC for newly diagnosed patients, there was a trend towards a reduction in ED admission for these patients, during the same period, however, the time frame did overlap with the COVID-19 pandemic (Figure 6).
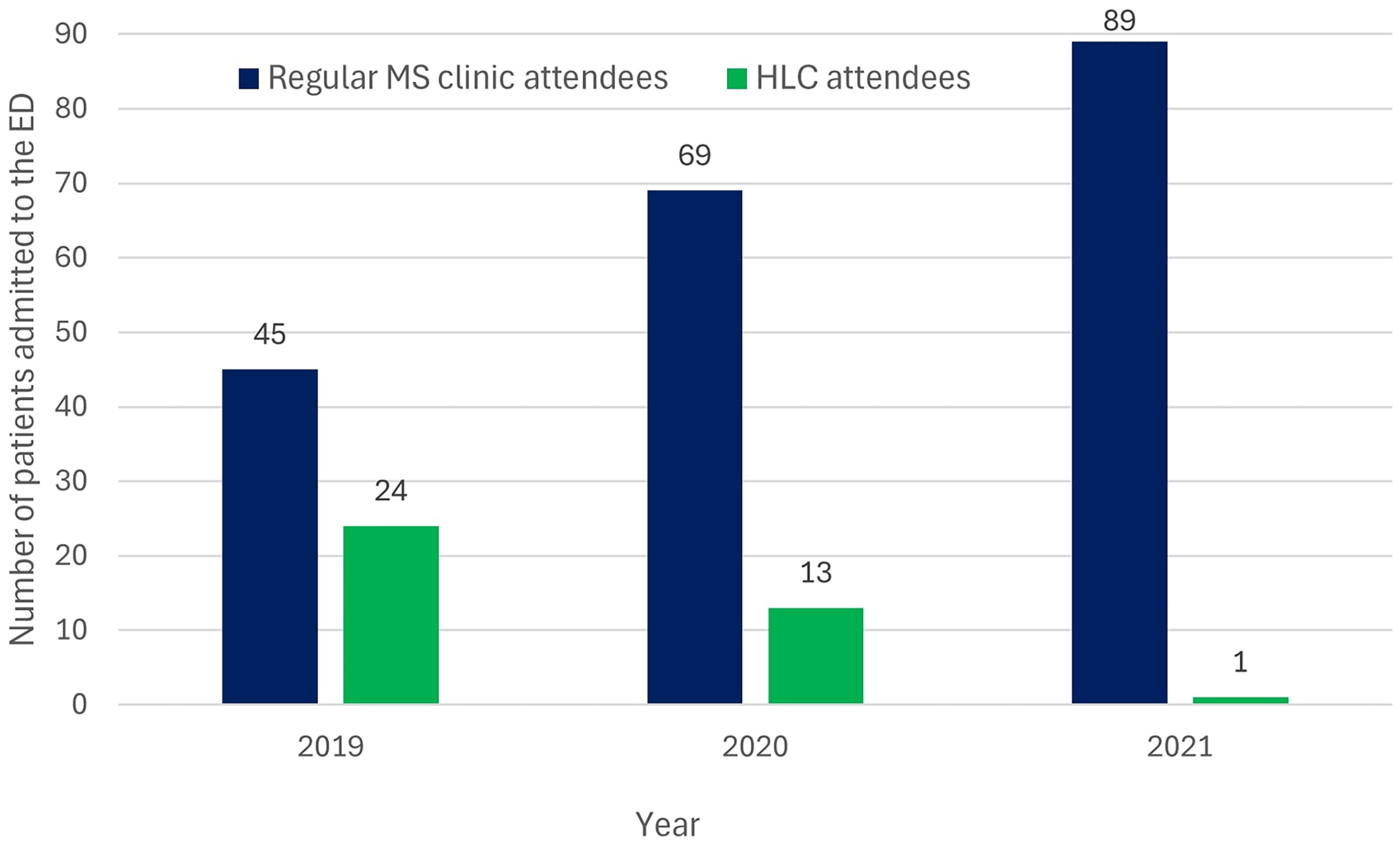
Number of HLC patient attendees who were admitted to the ED over time (total HLC patient attendees = 61).
Discussion
The implementation of innovative, integrated digital technologies and a holistic Healthy Lifestyle Clinic (HLC) at South Devon and Torbay Healthcare Trust has shown early promise. Initial trends suggest these new approaches may help address some persistent challenges in MS management, such as improving the accuracy of symptom and relapse reporting by patients and supporting PwMS in self-managing their health and well-being more effectively. This retrospective evaluation spanned five years (2018–2023), with a pre-intervention baseline (2018–2019), the introduction of digital tools in early 2020, and a post-intervention period (2020–2023), allowing a comprehensive assessment of these interventions. The COVID-19 pandemic (2020–2021) was considered separately to account for its potential impact on healthcare delivery.
While digital technology has the potential to revolutionise healthcare, it is important to not use technology merely for technology's sake and ensure that innovations are implemented for the right reasons in the right way. Evaluation of patient opinions is an important part of assessing the effectiveness and satisfaction of new technology. Tools should not be overwhelming or complicated. Indeed, the aim is not to add unnecessary steps or bureaucracy, but to simplifying lifestyles and healthcare routines through clever utilisation of time and resources. In South Devon and Torbay, the integration of new technologies seems to have supported implementation, aiming to simplify processes and reduce the risk of overwhelming patients. Early user feedback on the use of MS PKB, the CONNECT app, and the HLC has been positive, with several patients suggesting that these tools may enhance their healthcare experience. Given that PwMS sees their neurologists around once per year, it is important that they make the most out of their face-to-face appointment time. 31 The YMSQ helps facilitate conversations between patients and HCPs, is relatively quick to complete, and can guide discussions towards what is most important for the patient. It may also save time for HCPs by helping to identify quickly key areas to focus on during the consultation.
The introduction of MS Infoflex has helped HCPs save time and may enhance safety monitoring. Introducing the assessment of longitudinal data, it could further support earlier interventions with DMTs and assist in identifying potential treatment failure, adherence, or safety concerns in a timelier manner. With the integration of MSProDiscuss into Infoflex, there is a potential trend towards earlier initiation of DMTs for more patients, which may help preserve brain health and possibly slow disease progression in the longer term. The preliminary findings suggest that if people are in the green scoring range, but were formally diagnosed 10 years after the onset of MS symptoms, there is a higher likelihood that they will move into the red scoring range and progress further. This supports evidence that delayed MS diagnosis and treatment causes more disability over the time.32–35 Early diagnosis and intervention is crucial to preserve brain health, and perhaps digital technology can assist with this further.
Following the MS PKB pilot, future directions for the Trust include a wider roll-out of the platform. Use of MS PKB plateaued following the pilot, demonstrating that dedicated coordinated support is required for efficient engagement to such digital platforms. The Trust is also implementing the use of augmented reality (AR) for PwMS and the HCPs involved in their care. The AR-MagicLeap 2 technology involves a head-mounted display unit, allowing the creation of AR MS clinics. Nurses can visit PwMS in the comfort of their own home but connect to the consultant neurologist in real time, enabling them to work collaboratively to review the patient, conduct assessments (upper and lower limb function, saccadic eye movements, speech, cognition and fatigue), and communicate with their patients at home. Patients will be able to view their own MRI scans in 3D, and HCPs will be able to view a patient in 3D, to analyse gait and assess the domestic environment, thus helping to identify individuals at risk of hospitalisation and falls. 36 Ultimately, there is the potential to feed raw data into artificial intelligence (AI) applications. It is thought that machine learning algorithms can be taught to identify patterns and alterations in patient data, analyse MRI scans and predict relapses and disease trajectories, allowing personalisation of disease treatment and intervention monitoring. Ultimately, it is possible that the patient journey could be coordinated by doctor's AI assistants (Supplementary Figure 5).
Limitations of the current work include that this was a service evaluation rather than a formal research study designed to detect statistical significance, meaning only trends in the data can be observed rather than definitive conclusions drawn. The simultaneous introduction of several digital tools and holistic strategies makes it difficult to isolate the specific impact of any one intervention. Additionally, the lack of longitudinal follow-up data limits the ability to assess the long-term benefits of these innovations. Furthermore, the potential influence of the COVID-19 pandemic on healthcare delivery may have affected the outcomes, making it challenging to differentiate the impact of the pandemic from the interventions studied.
However, the study's strengths lie in its real-world application of these technologies in a clinical setting, offering practical insights. The evaluation spans a five-year period, providing a comprehensive view of the impact on MS care, even accounting for the pandemic's disruptions. Initial trends suggest that digital tools like MS PKB, CONNECTPlus, and Infoflex may help reduce the time to diagnosis and DMT initiation, contributing to enhanced patient care. Although further validation is needed, the findings point to the potential for these innovations to improve MS service efficiency and patient outcomes.
In conclusion, preliminary the use of holistic disease management and innovative digital technologies at Torbay and South Devon Trust has better enabled personalised care for PwMS, in a more timely and cost-effective manner, with positive outcomes for patients. However, further validation is necessary to confirm these findings, especially concerning long-term outcomes and broader applicability. Future research should focus on extended follow-up periods and explore the potential impact of digital tools in a formal controlled study.
Supplemental Material
sj-docx-1-mso-10.1177_20552173251317020 - Supplemental material for Evaluating patient care in multiple sclerosis: Impact of combined digital tools and holistic management strategies
Supplemental material, sj-docx-1-mso-10.1177_20552173251317020 for Evaluating patient care in multiple sclerosis: Impact of combined digital tools and holistic management strategies by Agne Straukiene, Sarah Hughes, Jon Grundy and Finn Moxon in Multiple Sclerosis Journal – Experimental, Translational and Clinical
Footnotes
Acknowledgements
The authors would like to thank Emma East of Emma East Medical Writing, for writing and editorial assistance. The authors would also like to acknowledge Biogen Idec for support with the HES analysis data, and Rob Radmore, an analyst at Torbay, for additional data analysis support.
Data-sharing statement
The anonymised data that support the findings of this study are available from the corresponding author (AS), upon reasonable request.
Declaration of conflicting interests
Funding
A writing grant from Novartis Pharma AG supported the publication of this article; however, they had no influence on the manuscript content.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
