Abstract
Background
Disabled multiple sclerosis (MS) patients often need intervention of multiple specialists, resulting in a complex organization of care. How this multidisciplinary care should be organized and structured has not been studied.
Objective
The objective of this article is to address the effectiveness of an integrated multidisciplinary approach versus usual care in MS patients.
Methods
This is a prospective, randomized, controlled, monocentric clinical trial in MS patients. Two treatment strategies were compared: (i) an integrated multidisciplinary (IMD) approach, consisting of a half-day individually tailored comprehensive assessment in the MS clinic; and (ii) a standard care. The primary outcome was the impact of the strategy on quality of life (QoL) measured using the MSIS-29 scale at inclusion and after six months.
Results
Fifty MS patients were included. Median MSIS 29 score decreased over six months in the control group (−4.89) and increased in the IMD group (+2.00), with a significant difference between the two groups (p = 0.03). However, in the multivariate analysis, after adjustment of HAD-D and INTERMED score, this difference was no longer significant.
Conclusions
This prospective, randomized study is the first attempt to evaluate the multidisciplinary approach in MS patients. The results show that, contrary to our expectations, an integrated multidisciplinary approach is not superior to usual care on QoL.
Introduction
Despite major advances related to the development of immunotherapies, multiple sclerosis (MS)-related disability remains a major issue, reducing patients’ quality of life (QoL). As the clinical presentation is often complex, with motor symptoms, ataxia, cognitive difficulties, bladder dysfunction, pain, visual deficits, depression and fatigue, a multidisciplinary approach of care with different MS specialists and allied health professionals is frequently needed. Several reports have suggested the value of rehabilitation stays on disability and on some aspects of QoL. 1 However, apart from rehabilitation stays, the potential benefit of a multidisciplinary intervention has not been assessed.
An integrated intervention within a multidisciplinary outpatient clinic gathering the different team members is thought to offer the best management of MS. However, whether this multidisciplinary approach is more beneficial for the patient than more usual type of care, where interventions are not integrated but proposed through successive referrals to needed medical and allied health professionals, is unknown. This question is of importance not only for the benefit of the patient, but also for the health organization. To gain insight into this question, we set up a prospective, randomized, controlled study, aimed at comparing the integrated multidisciplinary program existing since 2001 in our MS clinic with a nonintegrated approach, using QoL as a primary endpoint.
Materials and methods
Patients
MS patients from the outpatient clinic of the Neurology Department of Pitié-Salpêtrière Hospital were prospectively enrolled in the study between March 2010 and July 2012. Inclusion criteria were: having MS (MacDonald criteria); being able to complete a questionnaire; and being in need for a multidisciplinary approach, defined by the requirement, in addition to the neurology specialist, of at least two different medical (rehabilitation specialist, neuro-urology specialist, psychiatrist) or allied health professionals (physiotherapist, occupational therapist, social worker, psychologist, and neuropsychologist). Patients who were not living independently in the community were excluded.
Previous history of MS, previous and ongoing disease-modifying treatments (DMTs), social characteristics (help of caregiver, employment, and pension of invalidity) were collected from the patients’ files at inclusion. The INTERMED score, an observer-rated instrument that scores information in four domains: biological, psychological, social, and health care, and has been used to identify patients in need of multidisciplinary care in different neurological diseases including MS, 2 was calculated at inclusion. Psychological, social and biological subscores were calculated. The total of the INTERMED score was 57.
Randomization and study design
Signed informed consent was obtained for each patient at inclusion. At the end of the inclusion visit (conducted by the evaluating neurologist not participating in the multidisciplinary team), the patient was randomized via a central Web-based randomization system. Treatment was allocated according to a computer-generated randomization list in a 1:1 ratio. Patients were then randomized in two groups depending on the treatment strategy: (i) an integrated multidisciplinary (IMD) group, consisting of an IMD approach at the Pitié-Salpêtrière MS clinic, and (ii) a control group, consisting of successive, non-integrated interventions with different specialists and allied health professionals, at different times and sites (Figure 1). For patients in the IMD group, the multidisciplinary integrated outpatient clinic was planned at our MS clinic within a maximum three-month period after inclusion. These patients received a half-day (four to six hours) individually tailored assessment by the multidisciplinary group. The schedule allowed each required medical specialist (neurologist, rehabilitation specialist, neuro-urology specialist, and psychiatrist) or allied health professional (MS nurse, occupational therapist, physiotherapist, psychologist, social worker, and neuropsychologist) to assess the patient’s status and needs. Depending on their needs, evaluated during the inclusion visit and re-evaluated during the multidisciplinary visit, patients were seen by different MS specialists and allied health professionals. This multidisciplinary assessment was followed by an integration of all team members’ evaluations and recommendations by the coordinating neurologist.
Study design.
At the end of the visit, a summary of the multidisciplinary evaluation, along with the resulting therapeutic propositions, was discussed with the patient and caregivers. For patients in the control group, interventions with the different health professionals were planned after the inclusion visit, with an explanatory letter given to the patient or directly sent to the professionals. In most cases the same health professionals were in charge of the two groups.
The study protocol was approved by the coordinator of our local (Pitié-Salpêtrière Hospital) ethics committee, and formal review by the committee was judged unnecessary.
Primary and secondary outcomes were assessed at inclusion, and after six (M6) and 12 (M12) months. The primary outcome was the change in QoL from inclusion to M6, assessed by the Multiple Sclerosis Impact Scale (MSIS-29) self-questionnaire. The MSIS-29 is a validated, reproducible and specific MS QoL scale3–5 that consists of 29 simple questions including six different subdomains (fatigue, cognitive function, urinary and bowel trouble, social, emotional and mobility). A higher MSIS-29 score corresponds to lower QoL. The questionnaire takes 25 minutes to complete.
The secondary outcomes were: (i) change in QoL from inclusion to M12, assessed by MSIS-29; (ii) change in disability from inclusion to M6 and to M12 assessed by the same neurologist by the Expanded Disability Status Scale (EDSS), which ranges from 0 (no disability) to 10 (death of the patient), with 0.5-point steps; 6 (iii) change in anxiety and depression from inclusion to M6 and to M12, assessed by the Hospital Anxiety and Depression Scale (HAD) self-questionnaire, a scale validated in chronic diseases. 7 The 14-item scale takes five minutes to complete. The global score is divided into two subscores: Part A: measuring anxiety and Part D: measuring depression. Higher scores correspond to higher anxiety or depression; (iv) change in fatigue from inclusion to M6 and to M12, assessed using the Modified Fatigue Impact Scale (MFIS) scale, a fatigue-specific self-questionnaire widely used in MS. 8 The MFIS 9 is divided into three subdomains: cognitive functioning, physical functioning and psychosocial functioning. The total MFIS score ranges from 0 to 84 with higher scores indicating a greater impact of fatigue on the patient’s activities; (v) change in bowel and urinary tract dysfunction from inclusion to M6 and to M12 measured using the QUALIVEEN, a self-administered questionnaire validated in MS, consisting of 40 questions, completed in approximately 15 minutes; 10 and (vi) patient’s subjective evaluation of the care management at M6 and M12, assessed using a visual analog scale (VAS) rating, widely used to evaluate the impact of neurological rehabilitation in MS. 11 The clinical evaluating team was masked to the treatment arm.
Statistical analyses
For the sample size, calculations were based on a preliminary study 12 including 40 MS patients. In this pilot study a mean improvement of 10 points over six months on the MSIS-29 scale in the IMD group and a mean worsening of six points in the control group was observed. The standard deviation for the change in the MSIS-29 was 14 points. With the same hypotheses, 22 patients per group were necessary to provide the study a power of 90% with a type 1 error rate of 0.05. To take into account a possible dropout rate, we randomized 25 patients per group.
Characteristics at inclusion were compared with the Mann-Whitney test for continuous variables and chi-square or Fisher’s exact test for categorical variables.
The comparisons on the variation over six and 12 months of the MSIS-29 scale and secondary criteria (HAD scale, MFIS scale, QUALIVEEN and VAS) were analyzed in intention to treat with the Mann-Whitney test.
Factors associated with the six-month variation of the MSIS-29 were studied in univariate analysis with linear regression for continuous variables (age, disease duration, baseline scores of the EDSS, HAD, MFIS, VAS, QUALIVEEN, and INTERMED) and Mann-Whitney test for categorical variables (sex; form of MS; work status, i.e. non-workers vs. others; and use of personal care aid). Univariate predictors with p < 0.05 were included in a multivariate analysis of variance. Correlations between variations of outcomes from inclusion to M6 were assessed with Spearman correlation coefficients. To perform an intention-to-treat analysis, missing data were replaced with the mean variation of the group for the comparisons of the six-month variation criteria and the analysis of predictive factors of the six-month evaluation of the MSIS-29. Concerning the other exploratory analyses (correlations between variations of outcomes and comparisons of 12-month variations), missing data were excluded. The comparison of the variation over six months of the EDSS score in progressive patients was also performed after exclusion of missing data.
All analyses were performed with the SAS software version 9.2 (SAS Institute, Cary, NC, USA).
Results
Demographical, social and clinical characteristics of the groups at inclusion.

IMD: integrated multidisciplinary approach; RR: relapsing–remitting; SP: secondary progressive; PP: primary progressive; EDSS: Expanded Disability Status Scale; HAD: Hospital Anxiety and Depression Scale; MSIS: Multiple Sclerosis Impact Scale; MFIS: Modified Fatigue Impact Scale; SD: standard deviation.
Eleven patients (five in the IMD group, six in the control group) were not evaluated at M6; eight of these had no consultation (four in the IMD group, four in the control group). At M12, 21 patients in each group were evaluated (Figure 1). A detailed analysis of the different consultations during the study period shows that patients in both groups were treated by several health professionals: in the IMD group, a consultation with the neurologist was conducted for 18 patients, with the rehabilitation specialist for 16 patients, with the urology specialist for six patients, with the psychologist for 13 patients, with the social worker for 18 patients, with the MS nurse for four patients, with the physiotherapist for two patients, with the occupational therapist for one patient, and with the neuropsychologist for one patient. For five patients, the complete evaluation by the different health professionals was not possible same day, and was therefore completed during another visit. For 16 patients, all the interventions were performed during the same day. In the control group, a consultation with the neurologist was conducted for 20 patients, with the rehabilitation specialist for 15 patients, with the urology specialist for eight patients, with psychologist for 10 patients, with the social worker for 15 patients, with the MS nurse for two patients, with the physiotherapist for one patient, with the occupational therapist for one patient, and with the neuropsychologist for four patients. This overview shows that patients of both groups received multidisciplinary care, although this multidisciplinary intervention was delivered differently as scheduled by the protocol.
Median MSIS-29 score (higher score corresponding to lower QoL) of over six months decreased in the control group (−4.89), and increased in the IMD group (+2). The difference between the two groups was significant (p = 0.03). Over 12 months changes in MSIS-29 (0 and −5 in the control and the IMD group, respectively) were not significantly different between the two groups (Figure 2). Concerning secondary outcomes, there was no significant difference between the groups at M6 and M12 (Table 2).
Change of MSIS-29 over six and 12 months. Changes of secondary criteria over six months and 12 months. IMD: integrated multidisciplinary approach; HAD: Hospital Anxiety and Depression Scale; MFIS: Modified Fatigue Impact Scale; VAS: visual analog scale.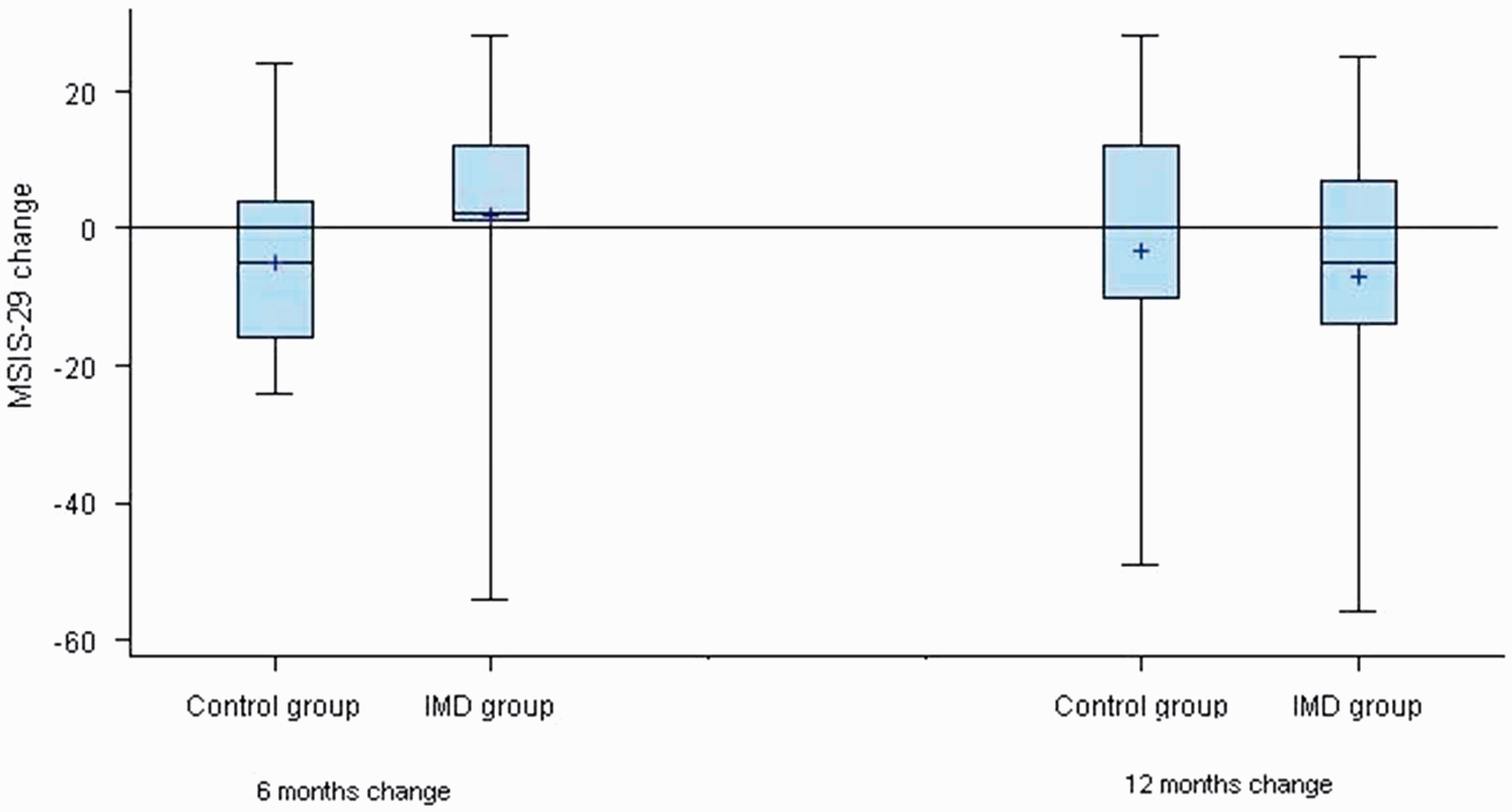

Univariate and multivariate analysis to identify potential predictive factors of MSIS-29 changes were performed at M6. The univariate analysis (taking into account age, sex, disease form, EDSS, HAD-A score, HAD-D score, MFIS, QUALIVEEN score, INTERMED score, type of therapeutic intervention, disease duration, use of personal care aid, relapses within six months after inclusion) showed that two factors only, the HAD-D and the INTERMED score, were significantly associated with the MSIS-29 change from M0 to M6. Higher HAD-D at inclusion was predictive of lower MSIS-29 score at M6 (p = 0.046). Higher INTERMED score at inclusion was predictive of higher MSIS-29 score at M6 (p = 0.04). These two factors and the type of care were entered in the multivariate analysis. After adjustment, MSIS-29 change was associated with HAD-D (p = 0.009) and INTERMED score (p = 0.01). In contrast, the type of care did not play a significant role in the variation of MSIS-29 score (p = 0.35). Taken together, these results demonstrate that MSIS-29 change from M0 to M6 is independent of the type of care but related to HAD-D and INTERMED score factors.
Correlations between MSIS 29 change (n = 39) and HAD-A, HAD-D, MFIS, QUALIVEEN changes, over six months, pooling both groups.

MSIS: Multiple Sclerosis Impact Scale; HAD: Hospital Anxiety and Depression Scale; MFIS: Modified Fatigue Impact Scale.
Discussion
MS is a chronic disabling neurological disease characterized by multidimensional dysfunction. Because of this complexity, many MS clinics use a multidisciplinary team approach to offer the best management of the multiple aspects of the disease. 13 However, how such multidisciplinary care should be delivered has not been evaluated.14,15 This study is to our knowledge the first to address this question using a randomized, controlled and prospective trial. Our results show that, contrary to our expectations, an integrated multidisciplinary approach is not superior to usual care regarding QoL (primary endpoint). These negative results were unexpected as the integrated approach was evaluated very positively in our previous pilot study, where patients were asked after the integrated outpatient clinic to score their satisfaction. In this pilot study, performed on 40 patients, more than 90% of them answered that they were extremely satisfied by this approach of care. These satisfaction auto-questionnaires, however, were completed and collected just after the outpatient clinic. We believe that although the present study was not blinded for the patients, this should not have influenced the outcomes. Indeed, it should have rather favored the integrated care group, as patients were often disappointed when selected for the control group. Interestingly, this lack of beneficial impact of integrated care on QoL was also evidenced in the subpopulation of progressive patients (which represents 84% of the whole population), although in this group, disability assessed by EDSS scores was reduced compared to the control group. This lack of correlation between QoL and disability contrasts with previous studies16–18 and is possibly explained by the fact that in our study EDSS changes were not confirmed at three or six months. Moreover, this difference in EDSS was no longer significant when missing data were excluded. Concerning the other secondary outcomes, which were not different in the two treatment groups, we noted that only depression assessed by HAD-D and INTERMED score were significantly associated with the MSIS-29 change at M6.
The INTERMED score was used at inclusion to better characterize the population studied. Among the 50 patients included in the study, the mean INTERMED score was 21. In a previous study 2 in MS analyzing 100 MS patients, mean INTERMED score was 14 (range 10–18) for the whole MS population, but increased to 18 (range 13–23) when the analysis was restricted to patients with more disability (defined as EDSS > 4), this latter population corresponding to the population analyzed in our study. Although INTERMED score allows quantifying the area of patient vulnerability, further studies will be necessary to demonstrate the clinical usefulness of this score in MS.
Only a few studies have evaluated the impact of a multidisciplinary approach in chronic neurological diseases. Among these few studies, most focused on Parkinson’s disease. A recent non-randomized study 19 comparing a multidisciplinary approach to usual care in Parkinson’s disease did not find significant difference in disability score (American Medical Center Linear Disability Score (ALDS)) and QoL (Parkinson’s Disease Quality of Life Questionnaire (PDQL)) scores used as primary outcomes. Contrary to our trial, referrals to the different health professional specialists in the “usual care” group of this Parkinson’s study were not organized. However, the overview of the different visits showed that patients in both groups were indeed referred to different specialists, and therefore had in most cases multidisciplinary care, as in our study. In contrast, positive effects on different outcomes, including QoL, were reported in a Canadian randomized study 20 of Parkinson’s disease. The differences between these two studies in Parkinson’s disease, which share a common design and assessed similarly ongoing care during eight months, were considered to be related to a lower number of patients and to the small size of the health care team in the latter study, as well as to large differences in the two groups concerning approach of care and settings.
Several methodological biases might have influenced our results: Clinical heterogeneity between the two groups was ruled out as, as shown in Table 1, these were well matched for disease severity (assessed by EDSS) and disease duration. In addition, the changes of secondary criteria were all correlated with changes in the MSIS-29, as expected. 21 Whereas we cannot totally exclude that missing data might have influenced the results, to conclude in favor of the IMD group, it should be assumed that the missing patients in the IMD group have improved, unlike missing patients in the other group. This seems unlikely.
In addition, the percentage of patients for whom referrals led to consultations was not different between the two groups, showing that, in contrast with our initial view, non-integrated care is not leading to weaker access to care.
We are aware that the size (n = 50) of the study is limited, but the number of patients was calculated based on a previous preliminary study in which a mean improvement of 10 points over six months of the MSIS-29 scale in the IMD group and a mean worsening of six points in the control group was observed
In addition, we cannot exclude that the selection of our cohort might have influenced the results: The population included into the study is not representative of the whole MS population treated in our MS clinic, and focuses on a subpopulation of disabled patients needing multidisciplinary care and willing to participate in a trial. Furthermore, most patients in our cohort had a “moderate” disability, with a median EDSS score of 6; whether our results might differ in other MS cohorts, notably in patients with a more severe handicap remains an open question.
Finally, it is important to emphasize that motivational factors and barriers strongly influence individual long-term management of MS care. This was recently demonstrated by Helland et al. 22 for MS patients applying for a stay in specialized rehabilitation centers, highlighting the need for better patient-centered communication.
In conclusion, the benefit of an IMD approach compared to usual care for disabled MS patients is not demonstrated. This result will influence our local organization. We believe that the benefit of the multi-disciplinary approach is less related to the modality of interventions (integrated or successive) than to the effective access to the resulting plan of care, which was not systematically reported in this study. Follow-up calls, notably by a dedicated MS nurse, should be organized in a systematic way, in order to assess that the patient is receiving the expected type of regular care. Further studies in which this “real-life” care is taken into account will allow us to better evaluate MS care organization.
Footnotes
Funding
This work was supported by a grant from Assistance Publique-Hôpitaux de Paris. The sponsor was Assistance Publique-Hôpitaux de Paris (Département de la Recherche Clinique et du Développement).” The research leading to these results has received funding from the program “Investissements d’avenir” ANR-10-IAIHU-06.
Acknowledgments
Statistical analyses were performed by Marie-Laure Tanguy and Laetitia. Gambotti; AP-HP, Pitié-Salpêtrière Hospital, Clinical Research Unit, Paris, 75013, France.
We thank Pr Laurent Cohen for fruitful discussion, and Sean Freeman for careful reading of the manuscript.
Conflict of interest
None declared.
