Abstract
Objective
This study aimed to synthesize existing qualitative evidence to explore the complex facilitators of and barriers to health information-seeking behavior (HISB) among cancer patients.
Methods
Guided by the PRISMA framework, a systematic search was conducted across multiple English and Chinese databases, including Cochrane Library, PubMed, Embase, CINAHL, PsycINFO, Web of Science, CNKI, and Wanfang. Study quality was appraised using the Joanna Briggs Institute (JBI) critical appraisal tools. Evidence from 12 eligible qualitative studies involving 230 patients was integrated and synthesized using the JBI meta-aggregation approach.
Results
The synthesis revealed a multifaceted interplay of factors influencing HISB. Patients’ behaviors are primarily driven by an internal psychological process, navigating a dynamic tension between acquiring knowledge to regain a sense of control and avoiding potentially distressing information to preserve hope. Furthermore, these behaviors are significantly shaped by external contexts, particularly the dynamics of patient-provider communication, family roles, and cultural beliefs, giving rise to a complementary “online preparatory search and offline verification” strategy. Ultimately, the ability to translate information-seeking intentions into effective action is closely tied to individual competencies, including health literacy, digital literacy, and accessible socioeconomic resources.
Conclusions
This review synthesizes the facilitators of and barriers to HISB, revealing a complex system shaped by internal states, external contexts, and personal capacities. Effective information support must therefore extend beyond mere information provision to incorporate dynamic, multi-level, and personalized strategies that are responsive to patients’ psychological needs, cultural backgrounds, and resource realities. The findings provide a consolidated evidence base and a holistic understanding for developing patient-centered, contextually adapted, and digitally informed health information support practices.
Keywords
Introduction
Cancer represents a critical social, public health, and economic challenge that threatens the wellbeing of global populations in the 21st century. According to the latest data from the International Agency for Research on Cancer (IARC), approximately 20 million new cancer cases were diagnosed worldwide in 2022, a figure projected to rise to 35 million by 2050. 1 Advances in screening and diagnostic technologies, combined with rising incidence and improved survival rates, have contributed to a growing number of cancer patients globally. Following a cancer diagnosis, patients often face life-changing decisions and experience substantial psychological stress, which may impair their ability to effectively access and use health information. 2 Furthermore, with the advancement of medical technologies and standardized treatment protocols, hospitals are discharging patients more rapidly after surgery or major treatments, increasing the demand for health management during the home recovery phase.
Health information-seeking behavior (HISB)—the proactive effort to obtain health-related knowledge to address needs, reduce uncertainty, and improve outcomes—serves as a central self-management and coping strategy for cancer patients. 3 Active HISB can support early detection and disease control, while also influencing prognosis through psychological and behavioral pathways. As articulated in Lazarus and Folkman's coping theory, information seeking functions as a strategy to appraise and manage stressful situations.4,5 By actively acquiring information, patients gain a better understanding of their condition, which enhances psychological adjustment, supports shared decision-making, reduces treatment-related anxiety, and strengthens self-management agency. 6 These mechanisms collectively contribute to improved treatment adherence, healthier behaviors, and better health outcomes. 7
HISB comprises diverse information-seeking modes across offline and online channels. Offline modes include consultations with healthcare providers, participation in peer support groups, and use of printed materials, while online channels encompass search engines, professional medical websites, social media, and mobile health applications. 8 These two modes differ significantly in their characteristics and functions. Online HISB offers broad accessibility, convenience, and real-time updates, supporting rapid acquisition of general knowledge, yet it is often accompanied by challenges such as information overload, variable quality, and difficulty in assessing credibility. 8 In contrast, offline HISB, particularly communication with healthcare professionals, provides greater professional credibility, contextual relevance, and personalized guidance, along with emotional support through direct interaction. 9 Rather than serving as substitutes, online and offline HISB function as complementary resources that patients strategically employ according to their specific needs and illness stages.
Existing research has largely concentrated on online HISB, identifying influencing factors such as demographics, disease-related variables, and psychosocial elements. For example, a scoping review on breast cancer patients’ online information seeking highlighted their preferences for search engines, institutional websites, and social media, alongside widespread concerns about information quality, credibility, and understandability. 9 Similarly, a systematic review by Giulia et al. 10 noted that internet information quality and digital literacy shape cancer patients’ online information behaviors, while Safa et al. 11 observed that despite technological advances, healthcare providers remain the most trusted information source, underscoring the enduring relevance of traditional channels. Cultural context also plays a key role: Sophie et al. 12 reported that Asian/Pacific Islander populations exhibit more positive attitudes toward seeking cancer-related information, and other studies have noted differences in information needs between American and Chinese patients. 13 These variations in source preference across groups likely reflect underlying cultural and contextual factors, which should be carefully considered in analyses of HISB among cancer patients.
While quantitative studies have identified various factors associated with HISB, they seldom explain the underlying “why” and “how.” Qualitative research addresses this by uncovering patients’ emotional experiences, motivations, and cultural influences. However, individual qualitative studies are often limited in scope and generalizability due to specific samples and settings. 14 Qualitative evidence synthesis can overcome these limitations by integrating findings across diverse contexts to provide a more comprehensive understanding of cancer patients’ HISB. 15 Furthermore, existing systematic reviews rely heavily on quantitative evidence from Western populations, with a notable lack of representation from distinct cultural settings such as China. Even when qualitative studies are included, analyses typically focus on online channels or isolated aspects, rather than examining the integrated experience of online and offline HISB, its underlying mechanisms, or how culture shapes information-seeking preferences and barriers.
Methods
Research aim and design
Qualitative evidence synthesis (meta-synthesis) addresses the limitations of individual studies by systematically integrating findings across diverse settings, uncovering underlying mechanisms of HISB and identifying potential intervention points. 15 Recognizing the complementary roles of online and offline channels, this review examined both modes, with particular attention to the underrepresented Chinese context. The aim was to explore factors influencing cancer patients’ HISB and identify modifiable facilitators and barriers that could inform clinical practice and supportive care strategies. The review was conducted in accordance with the Joanna Briggs Institute (JBI) Reviewer's Manual and reported following the Enhancing Transparency in Reporting the Synthesis of Qualitative Research (ENTREQ) guidelines to ensure methodological rigor and transparency.16,17 The protocol for this synthesis was prospectively registered on PROSPERO under registration number CRD42025633635.
Literature search and screening strategy
A systematic computer-based search was conducted across the following databases: Cochrane Library, CINAHL, Embase, PubMed, Web of Science, PsycINFO, China National Knowledge Infrastructure (CNKI), VIP Database, Wanfang Database, and the China Biology Medicine disc (CBM). The search aimed to identify qualitative studies investigating factors influencing HISBs among cancer patients, from the inception of each database until October 2024. Furthermore, the reference lists of all eligible articles were manually reviewed to supplement the database search. An initial limited search was performed in PubMed and CBM to identify relevant keywords and free-text terms. The specific search strategy tailored for each database is available in Supporting Information S1: File 1.
All retrieved citations underwent eligibility screening. Studies were included if they met the following criteria: (a) participants had a histopathologically confirmed malignant tumor diagnosis (screening-phase or precancerous cases were excluded); (b) the study examined facilitators or barriers to HISB in cancer patients; (c) a qualitative methodology was used, such as descriptive qualitative research, phenomenology, ethnography, grounded theory, or case studies; (d) the study was published in English or Chinese. Exclusion criteria were: (a) conference abstracts; (b) non-English or non-Chinese publications; (c) articles with unavailable full text, incomplete data, or duplicate publication. No restrictions were placed on participant age or study location. After duplicate removal, two reviewers independently screened titles, abstracts, and full texts against the eligibility criteria. Any disagreements were resolved through discussion or by consulting a third reviewer.
Quality assessment
Two researchers (WJ and YX) trained in evidence-based medicine independently appraised the quality of the included studies using the 2016 Joanna Briggs Institute (JBI) Critical Appraisal Checklist for Qualitative Research. 17 Any disagreements between the reviewers were resolved through discussion until a consensus was reached, or by consultation with a third reviewer to determine final inclusion. The checklist includes a total of 10 items, each of which was rated as “Yes,” “No,” or “Unclear.” Based on these ratings, the methodological quality of each study was classified into three levels: A, B, or C. A rating of Level A indicates that the study met all criteria, presenting the lowest likelihood of bias. Level B indicates partial fulfillment of the criteria with a moderate likelihood of bias. Studies that did not meet the criteria and presented the highest likelihood of bias were rated Level C. Finally, only studies rated Level A or B were included in the synthesis.
Data extraction and analysis
Data extraction from the included studies was performed independently by two researchers (WJ and LX). Any discrepancies were resolved through discussion or, if necessary, by consulting a third reviewer. Key descriptive characteristics were extracted using a pre-designed form, which included information such as the author(s), publication year, country, study design, sample demographics, phenomena of interest, and primary findings.
The findings were synthesized using the JBI meta-aggregation approach. 18 This method involved the following four steps: (a) extracting findings, along with supporting illustrations and participant quotes, that were directly relevant to our review objectives; (b) independently assessing the credibility of each finding by two reviewers (WJ and YH) as unequivocal, credible, or unsupported to ensure methodological rigor; (c) categorizing findings rated as unequivocal or credible based on their similarity in meaning, while excluding those rated unsupported from further synthesis; (d) developing synthesized findings by aggregating the categories. All authors reviewed the final synthesized findings for coherence, with any disagreements resolved through discussion.
Results
Literature search
The initial database search identified 7105 articles. After removing duplicates, 1887 articles were retained for title and abstract screening. Following this review, 1625 articles were excluded. The full texts of the remaining 262 articles were assessed for eligibility, resulting in the exclusion of 250 articles. Ultimately, 12 studies met all inclusion and exclusion criteria and were included in the final synthesis. The screening process and reasons for full-text exclusion are detailed in the PRISMA flow diagram (Figure 1).

PRISMA flow diagram illustrating literature search and selection.
Quality appraisal
All 12 included studies were considered of acceptable quality. One study was rated as Level A, having comprehensively described all quality assessment components. The remaining 11 studies were rated Level B. Among these, only five studies19–23 clearly articulated their philosophical perspective and methodology. Three studies23–25 demonstrated an inconsistency between the stated research methodology and the representation or analysis of the data. The cultural or theoretical positioning of the researcher was not identified in seven studies,19,21,24–28 and six studies19,21,22,24,25,29 did not address the potential influence of the researcher on the research. Additionally, one study 23 showed a lack of congruence between its methodological approach and the methods used for data collection. Despite these identified methodological limitations, all articles were retained in the systematic review as they provided valuable insights and contributions to the literature. The complete details of the JBI quality assessment for all 12 included studies are presented in Table 1.
Results of the quality appraisal.
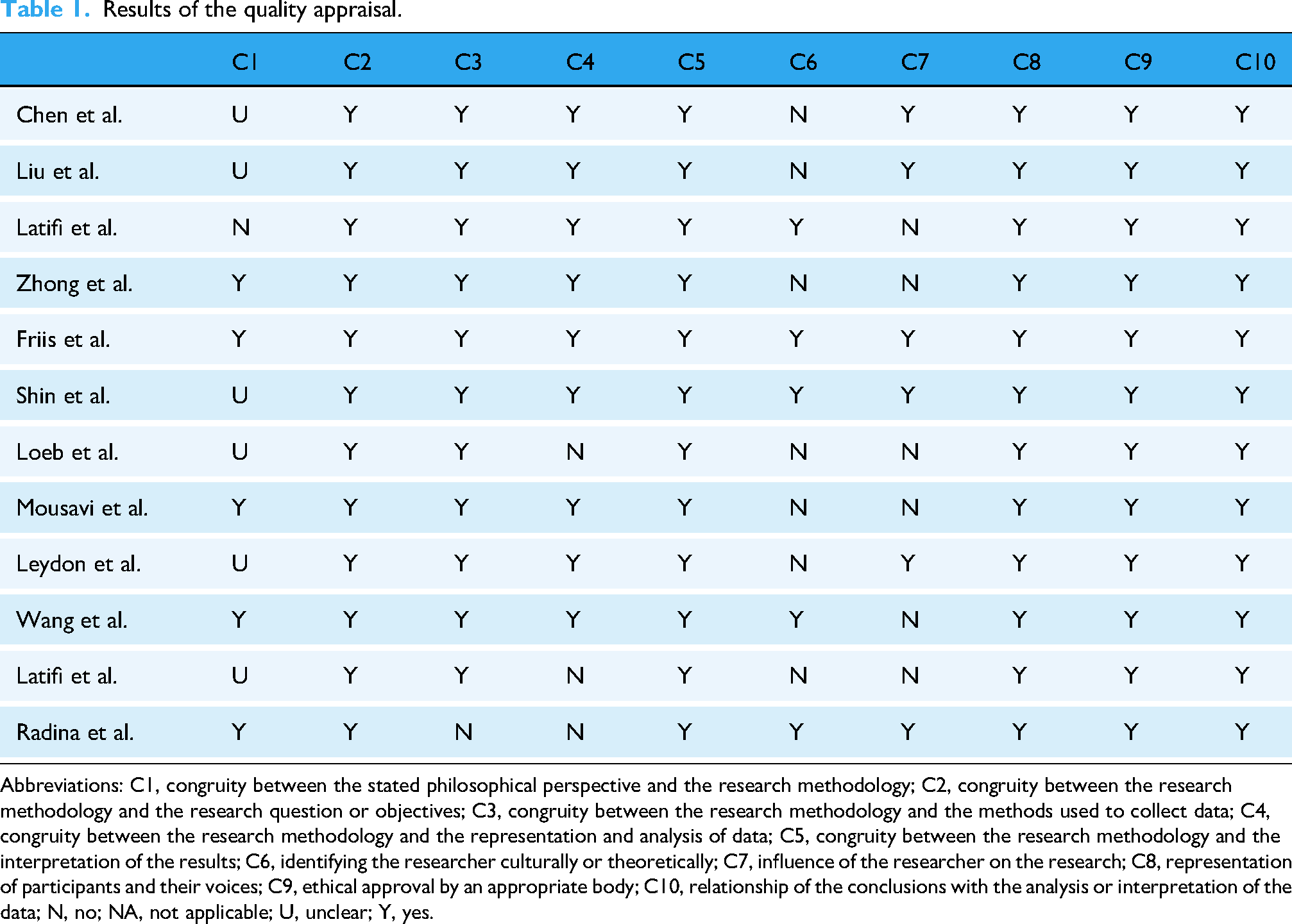
Abbreviations: C1, congruity between the stated philosophical perspective and the research methodology; C2, congruity between the research methodology and the research question or objectives; C3, congruity between the research methodology and the methods used to collect data; C4, congruity between the research methodology and the representation and analysis of data; C5, congruity between the research methodology and the interpretation of the results; C6, identifying the researcher culturally or theoretically; C7, influence of the researcher on the research; C8, representation of participants and their voices; C9, ethical approval by an appropriate body; C10, relationship of the conclusions with the analysis or interpretation of the data; N, no; NA, not applicable; U, unclear; Y, yes.
Study characteristics
Table 2 presents the characteristics of the 12 included studies. These studies, published between 2018 and 2024, were primarily conducted in China and Iran. Eight studies22–29 employed a qualitative descriptive design, while the remaining four utilized methodologies such as focus group interviews, phenomenological inquiry, and ethnography.19–21,30 In total, 238 cancer patients participated across the 12 studies, encompassing cancer types including breast cancer, colorectal cancer, head and neck tumors, leukemia, and prostate cancer. Sample sizes ranged from 12 to 35 participants.
Study characteristics.

Review findings
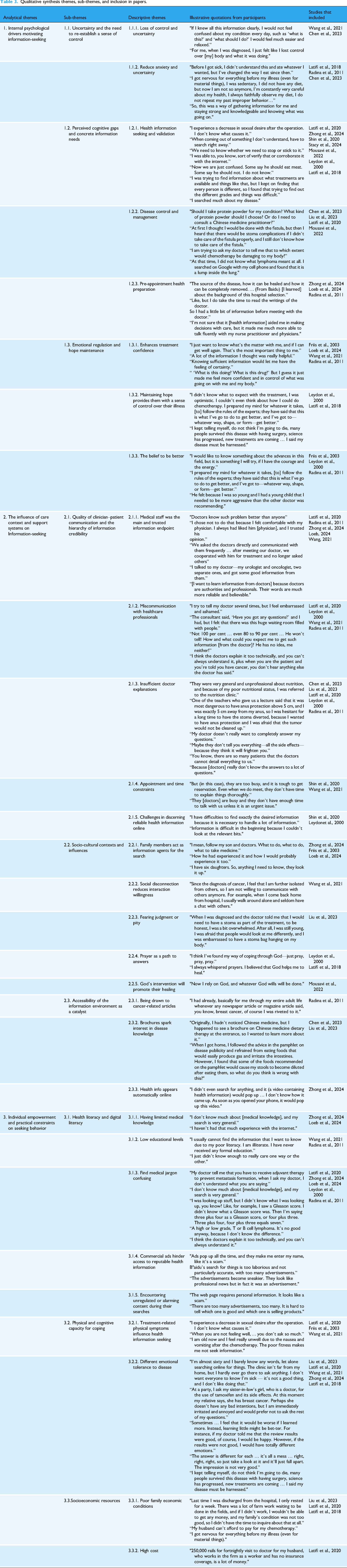
A summary of the results and synthesized findings is presented in Table 3. The synthesis process integrated 44 individual findings extracted from the 12 included studies, which were grouped into nine categories. These categories were further aggregated to form three overarching synthesized findings: (1) internal psychological drivers motivating information-seeking; (2) the influence of care context and support systems on information-seeking; and (3) individual empowerment and practical constraints on seeking behavior.
Qualitative synthesis themes, sub-themes, and inclusion in papers.
Internal psychological drivers motivating information-seeking
Uncertainty and the need to re-establish a sense of control
Uncertainty regarding disease prognosis, treatment side effects, and changes in life trajectory served as a fundamental driver for patients to seek health information. A cancer diagnosis often triggered a profound sense of losing control over one's body and life.23,25,26 To manage resultant anxiety and rebuild a sense of agency, patients actively pursued information to understand their condition, correct misconceptions, and plan for life adjustments.22,23 This process manifested differently across information-seeking channels. In online contexts, it frequently involved broad scanning for generalized information such as disease knowledge and survival statistics. In offline interactions, particularly with healthcare providers, the focus shifted toward seeking personalized, definitive answers about treatment plans and prognosis, which patients described as essential anchors for navigating their uncertainty.
Perceived cognitive gaps and concrete information needs
A distinct and targeted motivation to seek information emerged when patients perceived a gap between their current knowledge (“what they knew”) and the specific information they felt they needed (“what they wanted to know”).19,21,24,25,28–30 Patients expressed a clear desire for detailed, practical knowledge, such as the specific harms of chemotherapy, methods for nutritional assessment, ostomy care, dietary restrictions, and medical reimbursement procedures.19,23,24 This need for concrete answers often initiated a complementary seeking pathway. It typically began with preliminary online searches to gather a broad range of options and general explanations, which then informed more in-depth, personalized verification during offline consultations with their doctors. Participants indicated that seeking information served not only to fill knowledge voids but also to empower them to ask informed questions during clinician–patient communication. This active engagement was seen as a crucial strategy to enhance their sense of involvement and regain a measure of control over treatment-related decisions.21,26,27,29
Emotional regulation and hope maintenance
HISB also functioned as a critical process for patients’ emotional regulation. Accessing positive information, such as stories of successful recovery, was reported to directly instill hope, with some patients describing how maintaining hope itself fostered a renewed sense of control over their illness.19,20,22,23,25,28 Consequently, the proactive act of seeking information was perceived as a positive, forward-looking step toward recovery. Conversely, the fear of encountering negative information, such as distressing statistics about poor prognosis—triggered deliberate avoidance.19,20,27,29 Some patients adopted a mindset of “what you don't know can't hurt you,” actively shielding themselves from potentially anxiety-provoking information, particularly within the less-controlled online environment.19,20,22,24,26–29 This pattern suggests that information seeking and avoidance are two sides of the same coin, both serving the overarching goal of emotional self-protection and the preservation of hope at different stages of the illness journey.
The influence of care context and support systems on information-seeking
Quality of clinician–patient communication and the hierarchy of information credibility
Clinician–patient communication served as the cornerstone of patients’ information-seeking behaviors. When patients perceived the communication to be of high quality—characterized by sufficient time, attentiveness, and a sense that their informational needs were met—they were inclined to rely on healthcare professionals as their primary and most trusted source.19,21,23,25,29 Conversely, experiences of rushed consultations, communication gaps, or unmet needs (e.g., patients reporting that their doctors could not fully address their questions) directly motivated patients to seek information elsewhere.22,23,26–29 This dynamic established an implicit hierarchy of information credibility among patients. In-person interactions with clinicians were positioned at the top as the authoritative endpoint. Online healthcare platforms, exemplified by mainstream applications like “Ping An Good Doctor” 19 (a Chinese app providing consultations with licensed physicians), were utilized as a supplementary source for obtaining second opinions and for verification. In contrast, generalized online information and commercial advertisements were accorded lower trust and were typically used only for preliminary reference.19,26,30 Thus, deficiencies in offline communication directly drove both the frequency and necessity of online information-seeking.
Socio-cultural contexts and influences
Patients’ HISB are deeply embedded within their socio-cultural networks. In collectivist-oriented contexts, information seeking often becomes a shared family endeavor, with family members acting as information-seeking agents.25,26 While this provides essential practical and emotional support, it may also inadvertently constrain the patient's sense of autonomy. Concurrently, the stigma associated with a cancer diagnosis can lead patients to withdraw from offline social interactions, increasing their reliance on relatively anonymous online patient communities for peer support and experiential knowledge.22,27 Furthermore, culturally rooted beliefs, such as dietary therapy for health maintenance or notions of illness fatalism—shape distinctive information preferences.25,26,28 These beliefs influence how patients determine what information is valuable and whom to trust, creating a tension between relying on the authority of biomedical professionals and valuing traditional or experiential knowledge.
Accessibility of the information environment as a catalyst
The accessibility of the information environment itself could passively trigger information-seeking behavior. Encounters with readily available information, such as coming across a brochure in a clinic, receiving a browser notification for a health-related article, or receiving a recommendation from a fellow patient—often served as a catalyst, shifting patients from a state of passive reception to one of active exploration.19,23,26,27 This model of passively-initiated seeking underscores the importance of strategically optimizing information displays in physical clinical settings and the delivery of health content on digital platforms. These touchpoints can function as effective entry points to activate and support patients’ proactive engagement with health information.
Individual empowerment and practical constraints on seeking behavior
Health literacy and digital literacy
Insufficient health and digital literacy presented significant challenges for cancer patients. Limited health literacy, encompassing difficulties in understanding medical terminology and core concepts, hindered patients’ ability to comprehend, evaluate, and apply health information to self-care during both online searches and offline consultations.19,22–24,28,29 Concurrently, a lack of digital literacy directly impacted the efficiency of online searches and the capacity to critically appraise information, leaving patients vulnerable to information overload, commercial advertisements, and difficulty distinguishing between professional content and marketing.19,26,30 Deficiencies in these intertwined literacies posed a particularly pronounced barrier for older patients and those with lower levels of formal education.
Physical and cognitive capacity for coping
Treatment-related physical symptoms, such as fatigue and pain, coupled with the associated cognitive burden,20,25,29 significantly diminished patients’ overall capacity for active coping. In this diminished state, patients’ executive functions and motivation to process complex information tasks were compromised, rendering their information-seeking behavior more reactive and passive. Additionally, individual differences in emotional tolerance served as a key moderator,19,23,25,27,29 influencing whether a patient would actively engage with or potentially avoid stressful health information.
Socioeconomic resources
Financial constraints posed a direct and practical barrier to information access. Economic pressures limited patients’ ability to afford the time and costs associated with comprehensive in-person consultations, such as multiple outpatient visits or seeking second medical opinions.25,27,29 Concurrently, these constraints restricted access to quality online resources, including necessary devices, internet data, and paid professional consultations.22,23 When low socioeconomic status intersected with limited health and digital literacy, it created a compounded, more profound layer of inequality in health information access.
Discussion
This review synthesized all identified qualitative studies reporting on factors influencing HISBs in cancer patients. We employed the rigorous Joanna Briggs Institute (JBI) meta-aggregation approach, coupled with a critical appraisal of findings’ credibility, to enhance the trustworthiness, reliability, and transparency of our data synthesis. The analysis yielded three overarching synthesized findings from 12 studies, which collectively indicate that cancer patients’ HISB is influenced by a constellation of interconnected factors: the need to manage uncertainty and rebuild a sense of control; perceived cognitive gaps and concrete information needs; emotional regulation and hope maintenance; the quality of clinician–patient communication and the resultant hierarchy of information credibility; socio-cultural contexts and influences; the accessibility of the information environment as a catalyst; health and digital literacy; physical and cognitive capacity for coping; and socioeconomic resources. Our findings suggest that patients’ HISB is not a singular, linear process of either facilitation or hindrance. Instead, it represents a dynamic interaction between intrinsic psychological drives, external contextual factors, and individual capacity and resources. This systemic understanding helps reconcile seemingly contradictory findings in the literature regarding patients’ information needs and avoidance, providing a nuanced framework for offering personalized support across different contexts.
First, the findings reveal that the core dynamic driving patients toward or away from information is a quest for a dynamic balance between managing disease-related uncertainty and maintaining emotional hope. On one hand, concerns about disease risks, treatment side effects, and the future create a strong impetus for information-seeking. Patients actively acquire knowledge to rebuild a sense of control, validate assumptions, and participate in decision-making—a process consistent with the danger control process outlined in the Planned Risk Information Seeking Model. 31 On the other, aligning with the fear control process, 31 a profound fear of negative information (e.g., fearing poor prognosis statistics) and a protective need to preserve hope can lead patients to engage in strategic information avoidance. 32 This avoidance is not necessarily passive or ignorant; rather, it constitutes an adaptive strategy aimed at maintaining immediate psychological equilibrium and avoiding being overwhelmed by difficult facts, mirroring the coping style of blunters described in the Monitoring and Blunting Hypothesis. 32 Consequently, clinical assessment of an individual cancer patient's information preferences is crucial. Healthcare providers must discern whether the patient is currently acting more as a “monitor” or a “blunter”—whether they seek information for active participation or selectively avoid it to preserve hope and calm. This requires respecting patient choice and avoiding simplistic judgments that equate lower information-seeking with negative behavior. Interventions should shift focus from merely encouraging more information-seeking to supporting more adaptive information management, adopting strategies most beneficial for the patient's current adaptation.
Second, patients’ HISB is deeply shaped by their socio-cultural context, which helps explain the prevalent “online preview, offline verification” pattern observed in this review. While patients value online channels for their accessibility, a finding supported by prior research, 33 they maintain a strong trust in the authority of offline medical professionals, a perspective influenced by traditional Chinese views. 33 When clinician-provided information is perceived as insufficient, patients often turn to online sources to fill knowledge gaps and prepare questions, aiming to engage more effectively in shared decision-making during clinical visits. Within the Chinese context, family involvement is particularly salient. Reflecting collectivist norms, patients frequently delegate information-seeking tasks to family members, who assist with searching, filtering, and relaying information. 34 While this provides essential support, it may also affect patient autonomy. Cultural factors such as cancer-related fatalism and stigma further shape behavior, 35 often leading patients to seek emotional support and experiential knowledge from anonymous online communities rather than offline networks. Research notes the complex coexistence of fatalistic views and active information-seeking in some Asian populations, highlighting this nuanced dynamic. Additionally, information needs vary considerably by cancer type. 12 For specific concerns, such as functional recovery after prostate or head-neck cancer surgery—publicly available online information is often inadequate. In such cases, patients rely more on specialist clinicians or condition-specific support groups, underscoring the need for targeted, disease-specific information resources.
Finally, irrespective of motivation and context, an individual's ability to translate information needs into effective action is fundamentally constrained by their health literacy, digital literacy, and available socioeconomic resources. This review found that health information overload, variable information quality, and complex medical terminology constitute major external barriers. Internally, patients’ limitations in identifying, evaluating, and applying information act as a bottleneck for their HISB. The convergence of these internal and external barriers often leads to frustration during the information-seeking process. Repeated frustration can not only induce anxiety and erode trust in the healthcare system but may also lead patients to completely avoid information or settle for misleading content, potentially resulting in adverse health outcomes and diminished quality of life.36–38 Therefore, any future intervention must consider enhancing patients’ health and digital literacy as a foundational element, while also realistically accounting for their physical/mental state and economic circumstances.
Based on these insights, we propose the following implications. Healthcare providers should dynamically assess patients’ information preferences and psychological states, and actively recommend curated, reliable resources to make the digital environment a collaborative tool. Patient-facing platforms should adopt a patient-centered design and use profiling to deliver timely, precise information services. For patients affected by fatalism or stigma, culturally sensitive communication and family support should be encouraged. Health systems and policymakers should focus on building a reliable, comprehensible, and navigable health information ecosystem, with targeted resources for underserved cancer types and vulnerable populations. Digital platforms could integrate natural language processing (NLP) tools, such as QA systems, 39 plain-language summaries, 40 and translation—to create intelligent interfaces 41 that help patients understand information more effectively. Future research should translate the systemic factors identified here into actionable assessment tools and personalized interventions, testing their effectiveness across diverse groups and cancer types.
Limitations
This study has several limitations. First, despite stringent inclusion and exclusion criteria, the selection of qualitative studies inherently involves a degree of subjectivity. To minimize bias, disagreements were resolved by an independent, trained third researcher. Second, language constraints limited the inclusion of studies to English and Chinese, potentially excluding relevant research in other languages. Third, the inability to access original interview transcripts required synthesizing findings based on extracted quotes and researcher interpretations. Lastly, the quality assessment of included studies revealed that only one study met the highest quality rating (A), while the others were rated (B), indicating the need for higher-quality research in this field.
Clinical implications
This review's strengths include a comprehensive search strategy and rigorous application of JBI meta-aggregation with credibility assessment, which support the trustworthiness of the findings. The synthesis indicates that HISB among cancer patients is shaped by the dynamic interaction of psychological, socio-contextual, and personal-capacity factors. This integrated perspective informs several practical implications. At the individual level, clinicians should tailor information support by assessing whether patients seek control or hope preservation, rather than simply promoting information-seeking. Contextually, recognizing the influence of culture, family, and clinical relationships is essential; for example, in Chinese contexts, family networks can be constructively engaged while respecting autonomy. Providers may also guide patients to vetted online resources. At the capability level, interventions should concurrently build health and digital literacy while addressing structural barriers related to cost, education, and technology access.
Conclusion
This systematic review synthesizes qualitative evidence on factors influencing HISB in cancer patients. The findings reveal HISB as a complex adaptive process shaped by the interplay of internal psychological dynamics, external contextual influences, and individual capacities and resources. Enhancing effective HISB requires a personalized and context-sensitive approach that recognizes how these dimensions interact. Future research should develop tailored assessment tools and multi-level interventions, and examine the dynamic evolution of HISB across the illness trajectory, to better support cancer patients in managing their health and improving quality of life.
Supplemental Material
sj-docx-1-dhj-10.1177_20552076261418908 - Supplemental material for Facilitators and barriers to health information-seeking behavior in cancer patients: A meta-synthesis
Supplemental material, sj-docx-1-dhj-10.1177_20552076261418908 for Facilitators and barriers to health information-seeking behavior in cancer patients: A meta-synthesis by Wenjie Wang, Yuxing Xie, Xu Liu, Han Yan, Yujing Chen, Li Wang and Li Ning in DIGITAL HEALTH
Supplemental Material
sj-docx-2-dhj-10.1177_20552076261418908 - Supplemental material for Facilitators and barriers to health information-seeking behavior in cancer patients: A meta-synthesis
Supplemental material, sj-docx-2-dhj-10.1177_20552076261418908 for Facilitators and barriers to health information-seeking behavior in cancer patients: A meta-synthesis by Wenjie Wang, Yuxing Xie, Xu Liu, Han Yan, Yujing Chen, Li Wang and Li Ning in DIGITAL HEALTH
Supplemental Material
sj-docx-3-dhj-10.1177_20552076261418908 - Supplemental material for Facilitators and barriers to health information-seeking behavior in cancer patients: A meta-synthesis
Supplemental material, sj-docx-3-dhj-10.1177_20552076261418908 for Facilitators and barriers to health information-seeking behavior in cancer patients: A meta-synthesis by Wenjie Wang, Yuxing Xie, Xu Liu, Han Yan, Yujing Chen, Li Wang and Li Ning in DIGITAL HEALTH
Footnotes
Acknowledgments
We thank all authors who participated in this study.
Ethical approval
Not applicable.
Consent to participate
Not applicable.
Consent for publication
All the authors approved the to this journal.
Contributorship
All authors contributed substantially to study design, data collection, analysis, interpretation, and quality assessment. Study design: Wenjie Wang, Yuxing Xie, Li Ning. Acquisition of data: Wenjie Wang, Yuxing Xie, Xu Liu, Han Yan. Data analysis and interpretation: Wenjie Wang, Yuxing Xie, Xu Liu, Li Ning. Manuscript preparation: Wenjie Wang, Yuxing Xie, Yujing Chen. Manuscript review: Li Ning, Li Wang, Yujing Chen.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Zhejiang Provincial Basic Public Welfare Research Program Project (grant number LGF22H160079); Zhejiang Provincial Medical and Health Science and Technology Plan Clinical Research Application Project (grant number 2023KY178); and Hangzhou City Health Science and Technology Plan Key Project (grant number ZD20240013).
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
All data analyzed for this review are included in this published article.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
