Abstract
Background
Social media applications like WhatsApp are commonly used in sub-Saharan Africa (SSA), where access to health Interventions remains limited. This study aimed to assess the effectiveness of a WhatsApp based communication on improving access of antenatal care (ANC) interventions in resource limited setting.
Methods
This was a randomized controlled trial targeting pregnant women attending a Hospital in Yaounde, Cameroon. Participants were assigned to two arms using block randomization, stratified by age and parity, at a 1:1 ratio. Women in the intervention arm in addition to routine ANC were included in WhatsApp groups where short educational videos were posted weekly for 12 weeks, with ability to discuss, moderated by facility nurses. Participants in the control arm received routine ANC. The primary outcome was the completion of at least eight ANC contacts during pregnancy.
Results
A total of 316 pregnant women were enrolled and randomized into intervention (n = 159) and control (n = 157) arms. Thirty (20.1%) participants in the intervention arm and 10 (7.0%) participants in the control group complied with the recommended eight or more ANC contacts. The intervention significantly increased the likelihood of achieving at least eight ANC contacts (20.1% vs 7.0%) with an adjusted Risk Ratio (aRR): 2.65 (95% CI [1.34–4.79]) and an aRD: 0.12 (95% CI [0.04–0.20]). The intervention significantly reduced pregnancy-related anxiety, with participants 46% less likely to experience it compared to the control group (aRR: 0.54, 95% CI [0.34–0.78]), and improved pregnancy-related knowledge (adjusted Mean Difference (aMD): 0.34, 95% CI [0.08–0.61]). While a higher proportion of women in the intervention group completed the recommended intermittent preventive treatment of malaria in pregnancy doses, the adjusted effect was not statistically significant (aRR: 1.22, 95% CI [0.96–1.46]), and no significant differences were observed in mosquito net use (aRR 1.10; 95% CI [0.84–1.34]), malaria incidence (aRR: 1.05, 95% CI [0.76–1.36]), or satisfaction with ANC services aMD: 0.14, 95% CI [−0.07–0.36]).
Conclusions
Posting short pregnancy-related educational videos in WhatsApp groups involving moderating their discussion on the shared video contributes to significantly improving ANC attendance in a resource limited setting. The consistency of these findings should be documented across different contexts to enhance access to populations in need.
Trial registration
This trial was registered at Pan African Clinical Trials Registry (PACTR) under the registration number: PACTR202306721999803, on 13 June 2023.
Introduction
Maternal health remains a major public health concern in sub-Saharan Africa (SSA). According to the World Health Organization (WHO), nearly 70% of the 287,000 maternal deaths occur in that region, 1 despite the availability of effective recommended interventions aiming to allow pregnancy to be a positive experience.2,3 This situation highlights the persistence barriers to accessing the available antenatal care (ANC) services to the population in need. 4
In this context, innovations offered by new technologies of information and communication can help the health system to boost access to health interventions including those related to ANC. In fact, in resource limited settings where access to internet, availability and utilization of smartphones is growing exponentially, information has become increasingly accessible for the population. Recent studies have presented WhatsApp as the most use messaging application in general population and among pregnant women.5,6
Previous studies have shown WhatsApp-based interventions as feasible, accepted and cost effective way 7 to enhance maternal health such as improving the number of ANC contacts, 8 the pregnancy-related knowledge9,10 and the women satisfaction with ANC services 11 and reducing pregnancy-related anxiety (PRA).12,13
However, despite these promising findings, there is limited empirical evidence from randomized controlled trials assessing the effectiveness of WhatsApp-based interventions in improving access to ANC interventions, particularly in SSA. Existing studies are often limited by small sample sizes and lack of rigorous methodological approaches. To address these gaps, this study used a rigor randomized control trial procedure with more than 300 participants to respond to the research question: can exposing pregnant women to a communication program in WhatsApp groups where weekly educational short videos are posted for 12 weeks, with nurses to moderate discussions improve access to ANC intervention? By providing robust evidence on the potential role of WhatsApp in strengthening maternal health services, this study may inform future digital health strategies to improve ANC coverage and overall pregnancy outcomes in resource limited settings.
Materials and methods
Study design
This was a two-arm, parallel and superiority randomized controlled trial where pregnant women were assigned in two arms with 1:1 ratio using block randomization stratified by age, and parity. The intervention arm consisted of pregnant women included in a WhatsApp group, where they were exposed to short educational videos posted weekly for 12 weeks with the presence of nurses to moderate discussion. In the control arm, participants received the routine ANC (i.e. scheduled face-to-face visit at the ANC clinic, where pregnant women received ANC package including education). The primary outcome was the proportion of participants who complied with the minimum of eight ANC contacts during their pregnancy and secondary outcomes were malaria prevention and incidence, pregnancy-related knowledge, participant's satisfaction with ANC service received, and PRA.
Study setting and period
This study was conducted from January to December 2024 at the ANC unit of the Centre Médical Jean Zoa hospital, a faith-based hospital in the center region of Cameroon. Based on the national data reporting system (DHIS 2), the hospital receives the highest number of pregnant women for antenatal visits in the country (averagely 413 monthly).
Study participants
Participants were pregnant women attending their first ANC visit for the ongoing pregnancy, regardless of the gestational age. They were required to have a smartphone and be a WhatsApp user.
Intervention
The intervention involved, in addition to routine ANC, including pregnant women into a WhatsApp forum where a short educational video on key aspects of pregnancy was shared weekly. Three WhatsApp groups labeled “Wise Moms” were formed and each pregnant woman assigned to the intervention group was included in one of them. When each WhatsApp group attained 50 participants, the next participant was included in the second WhatsApp group. At the end of the enrollment the three WhatsApp groups contained 50, 50, and 53 participants respectively. Two nurses and one research team member were included in each WhatsApp group. All participants in the groups were allowed to send text, voice and emoji messages and react to others message with a mutual respect. The health personnels present in each WhatsApp group were responsible for providing orientations, response to questions or worries raised by pregnant women. No consultation was allowed to be done in the group. In the case a consultation was needed, pregnant women were referred to the health facility. The members of the research team present in each group had responsibility to watch the quality of the discussion in the group and to post each week (on Monday) an educational video.
During the study preparatory phase, research team and nurses of Centre Médical Jean Zoa hospital had working sessions during which 12 topics were selected based on WHO recommendations on ANC for a positive pregnancy experience 3 and their importance for pregnancy in the local context (see Table 1). Selected topics were shared with nurses of the ANC unit who developed talking points which were therefore validated by the head of the unit. After the validation, video recordings were made where each nurse presented their topic, as if speaking to pregnant women during an education section. Each video (lasting 2–3 min) was posted with the following caption: “Dear wise Mom, Happy new week!!!! We have another opportunity to act wisely for our benefit and for the benefit of our babies. This week, we will be talking about ‘topic.’ Please, watch the video, ask your questions in the group, interact with each other. All the best!.” The video of the week was pinned in the WhatsApp conversation and two days after each video posted, a post was done in the group to remind women to listen the video, ask their questions and react to other participants’ comments. The participant's engagement was monitored by computing the number of views per video 72 h after they have been posted and the number of interactions per week.
List of the educational topics and subtopics used for the videos.
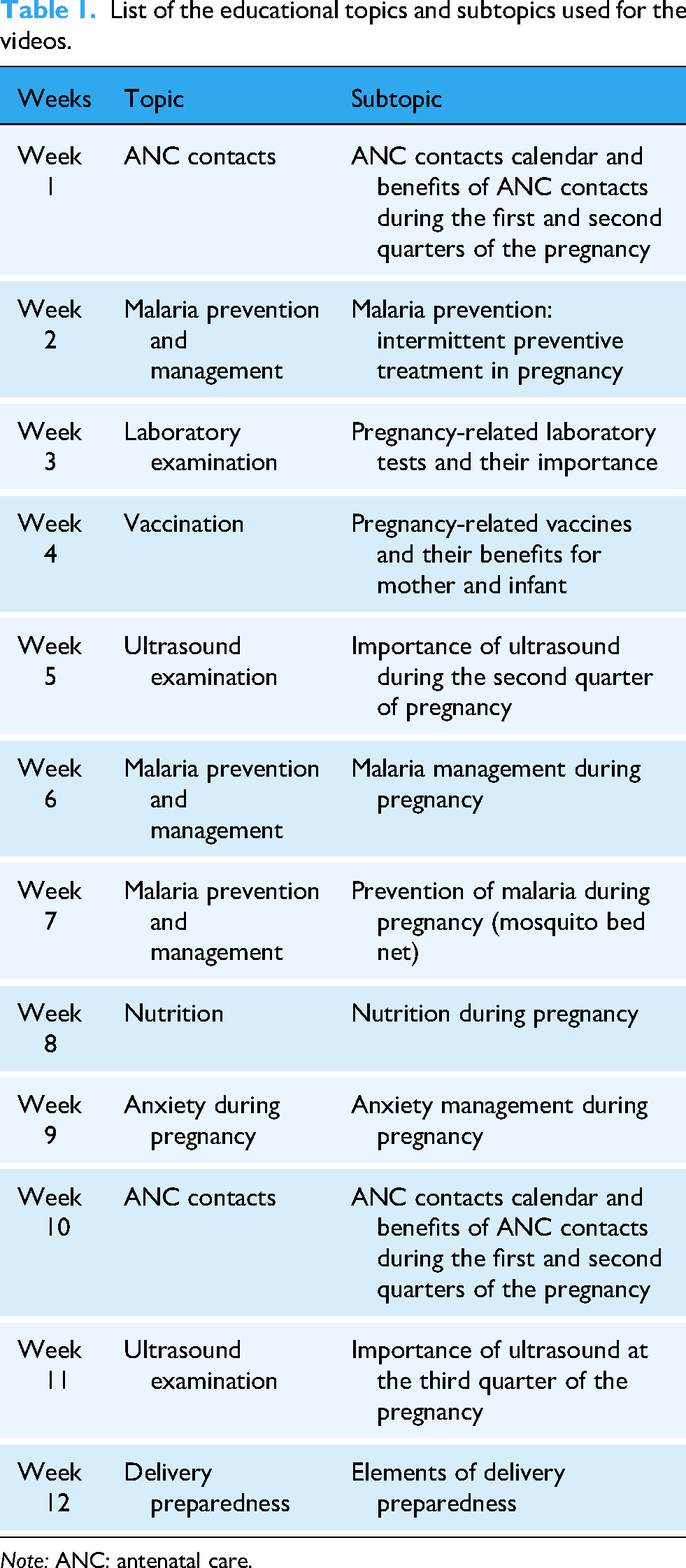
Note: ANC: antenatal care.
Control
Control groups received nationally recommended ANC package of care, that is, schedule face-to-face contacts of pregnant women with the service provider at the ANC clinic of a health facility. During each visit, pregnant women receive group education on a specific pregnancy-related topic followed by individual consultations where physical check, laboratory exams and prescription are made based on the pregnancy age and women specificities.
Outcomes
The primary outcome of this study was ANC—at least eight contacts, defined as the proportion of participants who had eight or more ANC contacts during their pregnancy from any professional health provider among pregnant women enrolled in the study. 14 In the Centre Médical Jean Zoa hospital, ANC visit appointments are given to pregnant women according to WHO directives. 3
Secondary outcomes of this study were: Proportion of pregnant women who completed the three doses of intermittent preventive treatment of malaria in pregnancy (IPTp), proportion of participants who always slept under mosquito net during pregnancy, pregnancy-related knowledge, PRA and participant's satisfaction with ANC services.
Data collection
Baseline information, initial pregnancy-related knowledge and initial PRA was collected through a semistructured questionnaire by interviewing pregnant women during their enrollment into the study. The post intervention PRA was assessed during subsequent visits, one month after the intervention. Data on the number of ANC contacts during pregnancy, and on the number of doses of intermittent preventive treatment for malaria were retrieved from the facility medical record at the end of the study. Information on the level of satisfaction, the incidence of malaria and the mosquito net use were gotten through interview of pregnant women after delivery or by phone call for those who were missed after the delivery or delivered in another hospital.
The assessment of PRA was done using the French version of PRA Questionnaire-Revised (PRAQ-R2). 15 PRAQ2 is a tool commonly used for assessing and identifying PRA in all pregnant women, regardless of parity and it demonstrated invariance across countries. 16 It is a 10 items questionnaire covering three areas: fear of giving birth, worries about bearing a physically or mentally handicapped child, and concern of own appearance. Each item is measured on five-point Likert scale as follows: 0—absolutely not relevant, 1—hardly ever relevant, 2—sometimes relevant, 3—reasonably relevant, and 4—very relevant. This scale ranging from 0 to 40 showed satisfactory internal consistency (Cronbach's alpha >.8). 17 The PRA score was then dichotomized; participants with a PRA score greater than the 75th percentile were considered as presenting PRA. 18
To assess participants’ knowledge about pregnancy, a prestudy survey was conducted to identify areas with the highest knowledge gap. From the survey, six questions arose around: number of recommended ANC visits, malaria prevention measures, nutrition during pregnancy. These questions were therefore used for the study. The women's level of satisfaction with ANC services was access with a five-point Likert scale question (1 = lowest level and 5 = highest level).
The documentation of the participant's exposition to the intervention was done by collecting the number of views of each video 72 h after it has been posted, and by counting the total number of interactions (messages, replies, emojis, …) posted by participants each week.
All questionnaires and tools used for this study were built in KoboToolbox 19 and deidentified data were entered directly in the study smartphones. Data quality review was done daily by a research supervisor and issues were flacked and corrections were made by the data collectors.
Sample size
The minimum required sample size was calculated at 292 participants (131 per arm), based on the following assumption: (i) two-sided, superiority design, (ii) 8% prevalence of eight or more ANC contacts in the control, 20 (iii) the intervention would increase the proportion to 20% in the intervention group, (iv) estimation of relative risk with a significance level (α) of .05, a power (1 − β) of 80% and 10% attrition. Minimum sample size was calculated in Stata/SE 18.0 software.
Randomization
A bloc randomization with age and parity stratification was done, using a maximum tolerated imbalance (MTI) procedure. The randomization was performed in the Clinical Trial Randomization Tool proposed by NIH National Cancer Institute. 21 The following parameters were entered in the tool: number of trial arms: 2; stratification: 2 (age; <25 and 25+; parity; primiparous and multiparous); MTI: 3. The software therefore generated an excel workbook with four sheets representing each stratum (<25_primiparous; 25+_primiparous; <25_multiparous; 25+_multiparous) and each sheet contained the allocation sequence that was used to assign participants in intervention or control groups. Due to the nature of the intervention, it was not possible to mask participants from the group allocation. Randomization sequence was generated by the statistician, participant enrollment was done by one the research assistants, and another research assistant oversaw assigning participants to intervention or control group.
Statistical analysis
The baseline data of the two study arms were initially compared using independent t-tests and Chi-square tests.
The effect of WhatsApp-based communication on achieving a minimum of eight ANC contact was estimated by calculating the Risk Ration and Risk Difference (with 95% confidence intervals (CIs)), adjusted with baseline variable that showed a significant difference between the two arms. This was done using the log-binomial regression model. The same was done for all the secondary dichotomous variables, while for continuous secondary variables, linear probability models were used to estimate risk differences (RDs) between the two study arms.
For all estimations, intention-to-treat (ITT) approach was used, and multiple imputations techniques were adopted to handle missing data. Each imputation model included the outcome variable, the intervention variable, and baseline variables that showed a significant difference between intervention and control groups in the bivariate analysis. To assess the robustness of estimations, complete-case analysis excluding participants with missing data were performed. Model assumptions, including normality of residuals and homoscedasticity, were assessed through diagnostic plots and statistical tests. Statistical significance was set at p < .05, and analyses were performed in Stata/SE 18.0.
Ethical considerations
This study received administrative authorization from the Centre Médical Jean Zoa hospital and ethical clearance from Centre Regional Committee for Human Health Research (CRERSH-Ce) under the ID number 0720/CRERSHC/2023. Sharing confidential information and posting inappropriate information in the WhatsApp groups were the major risks of this study. Appropriate measures including sensitization of participants and moderation of discussions by nurses and a member of the research team were taken to minimize these risks. A code of good conduct was signed by all participants before their introduction to the WhatsApp group. Prior to their enrollment, the research team provided the necessary explanations about the study to potential participants and informed them of their right to leave the study at any stage of the study. Participants were free to ask any study related question. After this process, all participants provided signed written informed consent that was kept at the study site.
Results
Characteristics of participants
At the beginning of the study, 758 pregnant women were reached and after enrollment, 316 (41.80%) were included in the study as presented on Figure 1. The randomization procedure used allocated 159 (50.32%) women in the intervention group and 157 (49.68%) in the control group. At the end of the follow-up, 149 (51.03%) women and 143 (48.97%) were still in the study in the intervention and control group respectively.

CONSORT diagram showing the flow of participants through each stage of a randomized trial.
The group comparison showed that there was no significant difference regarding variables used for stratification (age and parity) during randomization procedure (p > .05). For the other baseline variables, there were no difference between the two groups except for women occupation, women monthly income, spouse monthly income and history of premature birth (p < .05) as presented on Table 2. These variables were therefore used as covariates in the models.
Comparison of baseline characteristics of pregnant women attending the first antenatal care (ANC) visit at Centre Médical Jean Zoa hospital between intervention (routine ANC and WhatsApp communication) and control group (routine ANC only).
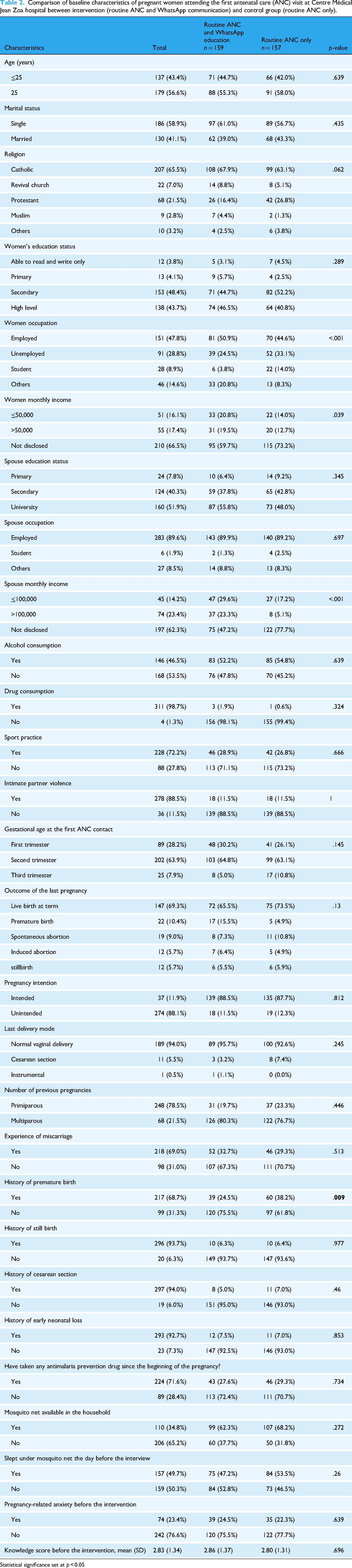
Statistical significance set at p < 0.05
Participant's exposition to the intervention
The monitoring of the participant's exposition to the intervention (as presented on Figure 2) showed that the average number of videos’ views was 140.33 (SD: 8.86), representing an average of 88.26% of participants in the intervention group who watched educational videos each week. The weekly average of interactions in the WhatsApp groups was 476.17 (SD: 30.66), corresponding to about three interactions (post, reaction to a post, emoji, …) per participant weekly.

Weekly evolution of the intervention monitoring indicator.
ANC—at least eight contacts
As presented on Table 3, 30 (20.1%) participants in the intervention group and 10 (7.0%) participants in the control group complied with the recommended eight or more ANC contacts. The crude risk ratio (RR) for complying with the recommended number of contacts with ANC services was 2.88 (95% CI [1.51–5.00], p = .002), indicating a nearly threefold increase in the likelihood of achieving the recommended number of contacts among those in the intervention group compared to the control group. After adjusting for baseline covariates, the association remained significant (adjusted RR: 2.65, 95% CI [1.34–4.79], p = .006) as presented on Figure 3. The RD analysis showed an absolute increase of 12% in the intervention group (adjusted RD: 0.12, 95% CI [0.04–0.20], p = .005) compared to control group (see Table 4). Sensitivity analysis using complete-case data yielded consistent results (RR: 2.57, 95% CI [1.29−4.68]).

Adjusted risk ratio study outcomes between WhatsApp-based intervention and control groups among pregnant women attending antenatal care visits at Centre Médical Jean Zoa hospital.
Crude and adjusted risk ratio of study outcomes between WhatsApp-based intervention and control groups among pregnant women attending antenatal care (ANC) visits at Centre Médical Jean Zoa hospital.

Statistical significance set at p < 0.05
Crude and adjusted risk difference study outcomes between WhatsApp based intervention and control groups among pregnant women attending antenatal care (ANC) visits at Centre Médical Jean Zoa hospital.

Statistical significance set at p < 0.05
Completion of three doses of malaria IPTp
A higher proportion of pregnant women in the intervention group completed the recommended three doses of malaria IPTp compared to those in the control group (59.1% vs 45.9%). The crude RR was 1.29 (95% CI [1.05–1.51], p = .019) and, after adjustment, the effect attenuated and was no longer statistically significant (adjusted RR = 1.22, 95% CI [0.96–1.46], p = .103). Similarly, sensitivity analysis using complete-case data did not demonstrate a significant effect (RR: 1.2, 95% CI [0.94–1.46], p = .139), as presented on Table 3.
Consistent use of mosquito nets and malaria incidence during pregnancy
The proportion of participants who reported always sleeping under a mosquito net during pregnancy was slightly higher in the intervention group (54.4%) compared to the control group (48.3%). However, this difference was not statistically significant, with a crude RR of 1.13 (95% CI [0.89–1.35], p = .297) and an adjusted RR of 1.10 (95% CI [0.84–1.34], p = .462).
There was no significant difference in the proportion of participants who reported having at least one episode of malaria during pregnancy between the intervention (39.5%) and control (41.3%) groups. The crude analysis suggested no meaningful difference (RR: 0.96, 95% CI [0.70–1.24], p = .754), and adjustments for covariates did not change this conclusion (adjusted RR: 1.05, 95% CI [0.76–1.36], p = .725).
Pregnancy-related anxiety
The mean of baseline PRA score was 13.43 (SD: 8.0) and the 75% percentile was 18, giving the threshold of PRA in this study. Analysis of the baseline PRA showed no difference between intervention and control group (24.5% vs 22.3%, p = .639) (see Table 2).
As indicated on Table 3, the prevalence of post intervention PRA was 20.2 percentage points lower in the intervention group (42.6%) compared to the control group (62.8%). The adjusted RR showed a significant protective effect of the intervention on PRA, with participants in the intervention group being 46% less likely to experience PRA (adjusted RR: 0.54, 95% CI [0.34–0.78], p < .001). The absolute reduction in risk was also statistically significant, with an adjusted RD of −22 percentage points (adjusted RD: −0.22, 95% CI [−0.34 to −0.09], p = .001). Sensitivity analysis using complete-case data further reinforced these findings (RR: 0.49, 95% CI [0.31–0.71], p < .001), highlighting the intervention's robust effect on reducing PRA.
Pregnancy-related knowledge
As presented in Table 2, there were no significant difference between the intervention and control groups (2.86 vs 2.80; p = .696) as pregnancy-related knowledge score was concerned at the beginning of the study. The postintervention evaluation showed a higher mean of pregnancy-related knowledge score (3.63, SD = 1.02) in the intervention group compared to the control group (3.27, SD = 1.13). The crude mean difference was 0.36 (95% CI [0.11–0.61], p = .005), the adjusted analysis yielded similar results (0.34, 95% CI [0.08–0.61], p = .011) and the sensitivity analysis using complete-case data confirmed these findings (0.34, 95% CI [0.07–0.60], p = .012) (see Table 5).
Crude and adjusted mean difference of knowledge and participant's satisfaction between WhatsApp-based intervention and control groups among pregnant women attending antenatal care (ANC) visits at Centre Médical Jean Zoa hospital.

Women satisfaction with ANC services
Although participants in the intervention group reported slightly higher satisfaction scores (mean = 4.01, SD = 0.87) compared to the control group (mean = 3.82, SD = 0.89), this difference was not statistically significant (adjusted mean difference: 0.14, 95% CI [−0.07–0.36], p = .196) as presented on Table 5.
Discussion
The aim of this study was to evaluate the effectiveness of a WhatsApp-based digital health intervention on compliance with and outcome of the recommended antenatal intervention for a positive pregnancy experience. The findings demonstrate significant improvements in achieving the recommended number of ANC contacts, increasing pregnancy-related knowledge, and reducing PRA, while also highlighting areas where the intervention had limited or no effect.
ANC utilization
This study found that the proportion of pregnant women who complied with the recommended eight or more ANC contacts was 7.0% in the control group (routine ANC), and 20.1% in the intervention group (communication via WhatsApp platform). The proportion of pregnant women receiving routine ANC who achieved eight or more ANC contacts was low (7.0%) and not different from the value pulled from the 2018 Cameroon Demographic and Health Survey. 20 The prevalence of eight or more ANC contacts remains very low in SSA despite the 2016 WHO recommendations on ANC for a positive pregnancy experience.3,20,22 Considering the positive effect of a minimum of eight ANC contacts during pregnancy on mother and child, identifying cost-effective interventions to increase the ANC uptake is critical.23–25
The findings of this study demonstrate a significant positive effect of WhatsApp-based interventions on the compliance with the recommended eight or more ANC contacts during pregnancy, with women in the intervention group being nearly three times more likely to achieve the recommended number of contacts compared to those receiving routine ANC. These results align with existing literature that highlights the beneficial effects of mHealth interventions on maternal and child health outcomes,26,27 particularly in improving ANC attendance. 28 Previous studies support the effectiveness of WhatsApp-based interventions in enhancing ANC service uptake by facilitating timely reminders, peer support, and direct interaction with healthcare providers.8,29,30 WhatsApp, being the most widely used mobile messaging application globally, 31 has also been reported as a common communication tool among pregnant women, 5 making it an effective platform for delivering health interventions. However, challenges such as maintaining participant engagement throughout the intervention and ensuring confidentiality, particularly in group discussions where sensitive personal health information may be shared have been reported as challenges during implementation of a WhatsApp-based interventions.32,33 In this study, in addition to educational videos posted in the WhatsApp groups and health providers active in the groups, proactive measures were taken to mitigate these challenges by sending regular reminder messages to participants to reinforce engagement, and by ensuring that group discussions were moderated to uphold privacy and confidentiality standards. These measures resulted to high levels engagement and adherence. Given the promising results observed in this study, scaling up WhatsApp-based interventions for ANC in diverse settings, particularly in resource-limited areas, could be an effective strategy to improve maternal and child health.
IPTp adherence
In this study, even though a higher proportion of women in the intervention group completed the recommended three doses of IPTp, the adjusted analysis did not demonstrate a significant difference between the two groups. This result aligns with previous research indicating that while mHealth interventions, including messaging platforms like WhatsApp, can enhance maternal health behaviors by improving knowledge and reminders for care-seeking, their impact on clinical adherence outcomes remains variable.26,27 Factors such as healthcare accessibility, medication availability, and individual socioeconomic conditions may have influenced IPTp completion beyond the intervention itself. Additionally, previous studies have highlighted that digital interventions may be more effective when combined with other health interventions. 34 Future research should explore potential barriers to IPTp adherence and investigate the integration of WhatsApp-based interventions with other strategies, such as direct healthcare provider involvement and community-based support mechanisms, to enhance their effectiveness.
Consistent use of insecticide-treated net and malaria incidence
No significant differences were observed in consistent mosquito net use or malaria incidence between the intervention and control groups. This contrasts with previous studies, such as the randomized trial done by Sudoi et al., which reported that mHealth interventions significantly increased insecticide-treated net use among pregnant women in Kenya. 35 However, it has been documented that behavioral interventions alone may not be sufficient to drive sustained malaria control without addressing socioeconomic and environmental factors, 36 that may have influence the results of this study. Additionally, malaria incidence is influenced by multiple external factors, such as transmission intensity and vector control measures, which were not directly modifiable by the intervention. Further WhatsApp-based intervention studies, considering socioeconomic, environmental and other external malaria incidence related factors are needed.
Pregnancy-related anxiety
This study demonstrated that the WhatsApp-based intervention significantly reduced PRA. This result is consistent with previous research. Abdelaziz et al. in their randomized control trial showed that a WhatsApp-based intervention significantly reduced tokophobia and enhanced maternal self-efficacy. 12 Other studies highlighted that tele-medicine intervention, using WhatsApp messaging can significantly reduce anxiety and depression among pregnant women.13,33 WhatsApp, being a widely accessible and interactive platform, may have contributed to reducing anxiety by facilitating instant communication with healthcare providers, delivering reassuring health messages, and fostering peer support among pregnant women. The observed reduction in PRA underscores the potential of WhatsApp-based interventions as scalable, cost-effective tools for improving maternal well-being, particularly in settings where access to in-person psychological support may be limited. Further research is needed to explore the mechanisms underlying this reduction in PRA, the sustainability of these effects, and the potential for scaling such interventions across different cultural and socioeconomic contexts.
Pregnancy-related knowledge
Before the intervention, there was no significant difference between the two groups as pregnancy-related knowledge was concerned (see Figure 4). However, at the end of the study, participants in the intervention group demonstrated a significantly higher knowledge score compared to the control group. This is in line with previous studies, which have shown that WhatsApp-based intervention can significantly increase the knowledge of pregnant women on different aspects of pregnancy such as nutrition, compliance with iron and folic acid supplementation, oral health knowledge.9,29,37 Studies have also shown that WhatsApp-based education can have positive impacts on attitudes, and self-efficacy, childbirth readiness of pregnant women physical activity, smoking cessation.9,30,37–40 The increased knowledge observed in this study may have been induced by the short educational videos that were posted in the WhatsApp groups weekly. This finding underscores the importance of accessible and engaging educational content in empowering pregnant women to make informed decisions about their health. Therefore, further studies are needed to explore the feasibility of incorporating such cost-effective interventions into routine ANC.

Adjusted mean difference of pregnancy-related knowledges and satisfaction with antenatal care between WhatsApp-based intervention and control groups among pregnant women attending ANC visits at Centre Médical Jean Zoa hospital.
Women's satisfaction with ANC services
The findings of this study indicated high level of satisfaction in both groups. Although the intervention group reported slightly higher satisfaction, the difference was not statistically significant. This result is not consistent with available literature that present a high maternal satisfaction induce by WhatsApp-based intervention. 11 Previous studies reported determinants of pregnant women's satisfaction regarding ANC services, including sociodemographic and obstetric history, hospital facilities such as clean water and latrine access, interpersonal aspects of care, such as provider communication and respect.41,42 This study was conducted at the Centre Médical Jean Zoa hospital, a faith-based health facility, which is renowned for its good care of pregnant women, justifying the fact that the hospital receives the highest number of pregnant women for ANC consultation in Cameroon. This fact can justify the high level of satisfaction observed in the intervention and control groups and the similarity between the two groups as the satisfaction level is concerned. Further study should be done in other settings to assess the effect of WhatsApp based intervention on women's satisfaction with ANC services.
Strengths and limitations
This study has several strengths, including its randomized controlled design, use of ITT analysis, and adjustment for baseline covariates. Additionally, the high engagement rates observed in the intervention group suggest strong feasibility and acceptability of digital health interventions in this setting. However, limitations exist. Self-reported outcomes, such as mosquito net use and malaria incidence, may be subject to recall or social desirability bias. Also, digital literacy, and internet connectivity could be other biases that may have affected the study results. Additionally, the study was conducted in a single hospital, which may limit the generalizability of findings to other settings. Also, the study was based on urban area where the population have more access to the internet and smart phones compared to rural areas. Conducting a study in rural areas may permit to assess the study benefits and feasibility in such context.
Implications for future research
Future research should explore strategies to enhance the effectiveness of mobile health interventions in improving other maternal health outcomes, such as adherence to malaria prevention measures and overall pregnancy satisfaction. Investigating the long-term impact of digital health interventions on maternal and neonatal outcomes would provide valuable insights. Additionally, assessing the scalability and cost-effectiveness of WhatsApp-based interventions in different healthcare settings such as rural low-income areas and different populations like vulnerable population could inform broader implementation and policy decisions.
Conclusion
This study demonstrates that a communication program with pregnant women using WhatsApp groups where weekly educational short videos were posted for 12 weeks, with nurses to moderate discussions can significantly improve ANC attendance and pregnancy-related knowledge while reducing PRA among pregnant women. These findings highlight the potential of cost-effective interventions, such as WhatsApp, to improve access to essential ANC intervention.
Footnotes
Acknowledgments
We thank all pregnant women who voluntarily participated to this study. We are grateful for the support received from all the staff of Centre Médical Jean Zoa hospital and from the research team.
Contributorship
Conceptualization and methodology: Fabrice Djouma Nembot and Jerome Ateudjieu; investigation and data analysis: Fabrice Djouma Nembot, Kakapen Deborah, and Roger Ndzana; writing—original draft: Fabrice Djouma Nembot; writing—review and editing: Collins Buh Nkum, Dora Ateudjieu, Roger Ndzana, Kakapen Deborah, Zacheus Ebongo Nanje, and Francis Duhamel Nang Nang; supervision: Jerome Ateudjieu.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability
Data are available under request.
