Abstract
Background
Electronic health records (EHRs) are essential to modern nursing practice, enhancing patient care and safety. However, their adoption among nurses in Africa remains limited. Thus, this study aims to map evidence about nurses’ adoption of EHRs in Africa.
Source of Evidence
Guided by the Levac framework, this review thoroughly analysed scholarly publications. Searches were conducted across six databases – CINAHL, Emcare, Medline, PsychINFO, Scopus and Web of Science – covering publications from 2014 to 2024. A manual search was conducted using Google and Google Scholar. A total of 12 studies met the inclusion criteria. The majority of studies were quantitative (n = 6), followed by mixed methods (n = 5) and qualitative (n = 1). Furthermore, of the 12 studies, five adopted interventional designs that introduced training programs in EHRs and decision support tools. Geographically, the research is primarily focused on sub-Saharan Africa, with South Africa contributing the highest number of studies (n = 5), followed by Nigeria (n = 4), Kenya (n = 2) and Ghana (n = 1).
Results
The findings highlighted the suboptimal adoption of EHRs by nurses across Africa. Studies from Nigeria revealed minimal usage of EHRs despite the availability of infrastructure, while those from South Africa showed inconsistent progress. Kenya faced adoption barriers due to funding and infrastructure gaps, especially in rural areas. Eight studies emphasised the importance of standardised digital tools for nursing efficiency and patient care, yet reliance on paper records persisted. Key barriers included insufficient training, workflow disruptions, outdated technology, connectivity issues and resistance to change. Effective strategies involved targeted computer skill training, robust policies and organisational support, with usability optimisation crucial for boosting confidence and adoption.
Conclusion
The integration of EHRs among African nurses is still in its early stages, with a significant reliance on paper-based systems. Developing tailored training programs and exploring sustainable implementation strategies are essential for success.
Background
The incorporation of digital technologies into healthcare delivery has profoundly transformed clinical practice, particularly in the domains of documentation, decision-making and patient management.1,2 Amidst ongoing technological innovation, electronic medical records (EMRs), electronic health records (EHRs) and clinical decision support tools (CDSTs) are integral components of digital healthcare, each contributing significantly to the enhancement of quality, safety and efficiency in patient care.3–6 EMRs and EHRs provide digital frameworks for managing patient information, while CDSTs are embedded within these systems to facilitate clinical decision-making.3,7 The integration of CDSTs into EMRs/EHRs yields benefits such as optimised medication prescribing, reduced errors and improved management of chronic conditions like diabetes. 8 An EHR is a digital collection of patient health information, similar to a patient's paper chart. 9 Furthermore, EHRs encompass numerous potential capabilities, including CDSTs, computerised physician order entry (CPOE) and health information exchange (HIE). 10 Nevertheless, challenges, including the organisational structure and governance processes of the EHR, interoperability issues, system capabilities and skills and attitudes of healthcare professionals (HCPs) may impede their efficacy.3,7,11,12 Due to the importance of EHRs in nursing practice,12–14 this study maps evidence about nurses’ adoption of EHRS in Africa. For the purposes of this scoping review, the term EHRs is consistently used to denote digital health information systems. It is essential to acknowledge that related terminology, including EMRs and CDSTs, is employed within the literature and referenced as appropriate according to their specific contexts, with EHRs serving as the overarching concept throughout this review.
EHRs have become a fundamental component of nursing practice, potentially enhancing the quality of care and documentation.15–17 However, nursing professionals frequently encounter difficulties related to user interface and the comprehensiveness of the data provided. 15 Furthermore, the lag in integrating newly established evidence-based practices into EHR systems remains a prominent challenge. 12 EHRs are pivotal in the digital transformation of healthcare. 18 EHRs are digital systems that store patient health information, offering advantages over paper-based records in efficiency and security. 19 EHRs aim to enhance clinical documentation, data quality and the portability of health records. 20 EHRs provide a comprehensive overview of a patient's health status and care history, allowing for secure sharing among healthcare providers. 21 EHRs offer multiple advantages, such as increased patient safety, improved efficiency and enhanced effectiveness in healthcare delivery.22,23 Additionally, EHRs support quality improvement through features like clinical decision support tools, CPOE systems and HIE. 24 EHRs have positively impacted financial and clinical outcomes in healthcare settings. 25 They can enhance clinical documentation, standardise record-keeping and streamline patient care. 26 In low- and middle-income countries, EHRs have improved chronic disease management and healthcare system efficiency.27,28 While EHRs have improved healthcare delivery and research capabilities, they present challenges in interoperability, privacy and data quality.29,30 To enhance EHR usage, comprehensive interventions that tackle organisational, individual nurse and information technology aspects are essential. 31
Africa has made significant progress in implementing EHRs/EMRs, necessitating an understanding of the utilised health information systems, frequently comprising open-source platforms such as Open Medical Record System (OpenMRS) and District Health Information Software 2 (DHIS2),32–34 as well as national systems, like Kenya Electronic Medical Records (KenyaEMR), 35 and Rwanda Health Information Exchange (RHIE).36,37 These systems are often customised to address specific healthcare requirements and infrastructural limitations unique to the continent. OpenMRS is the leading open-source EHR platform in sub-Saharan Africa, particularly in countries such as Kenya, Rwanda, Nigeria, Mozambique, Malawi and Ethiopia.33,34 OpenMRS has been widely implemented in Africa, particularly for HIV and maternal and child health care. 34 For instance, in Rwanda, it has been utilised to enhance clinical record-keeping and support HIV epidemiology studies.33,38 The system has been deployed in over 62 countries, with implementers reporting positive impacts on healthcare delivery, data quality and decision-making. 34 During the 2014–2016 Ebola epidemic in West Africa, OpenMRS was adapted to create OpenMRS-Ebola, an EHR system for Ebola Treatment Centers in Sierra Leone.39,40 DHIS2 is another widely adopted, open-source health management information system that facilitates the aggregation of public health data, disease surveillance and immunisation tracking across numerous African nations.32,41 DHIS2 is critical for national health data reporting and monitoring, often enhanced by EHR systems at the facility level, and it a system that provides a near-universal coverage of key indicators, including maternal and child health outcomes within health facilities, infectious diseases, antenatal care and vaccination rates. 32
EHR-integrated CDSTs enhance clinical decision-making and patient care by generating alerts for drug interactions, supporting accurate diagnoses, offering evidence-based treatment recommendations and enabling proactive disease surveillance.3,42,43 A study by Stipelman et al. 43 found that CDSTs were implemented in primary care outpatient settings to enhance screening and treatment and their functionalities included point-of-care alerts, order facilitators, workflow support, information displays, expert systems and medication dosing support. The use of CDSTs is associated with improved patient safety, increased adherence to best practices and a reduction in medical errors. 3 In Africa, clinical decision support systems, such as the Electronic Integrated Management of Childhood Illness (eIMCI), have been developed to enhance the quality of care for pediatric patients in primary healthcare settings.44–47 Feasibility and impact studies in South Africa and Burkina Faso demonstrate that eIMCI was well-received by healthcare providers and caregivers, enhancing the comprehensiveness and efficiency of clinical care.46–48 However, implementation challenges were noted, including limited computer literacy among healthcare personnel, technical issues and concerns about prolonged consultation times.44,45
In nursing, adopting electronic decision tools such as standardised nursing care plans (SNCPs) and standardised nursing languages (SNLs) is crucial for enhancing the quality of nursing documentation and patient care.49–51 SNCPs are evidence-based, pre-prepared documents that are structured according to the nursing process, whereas SNL represents an established set of terms that systematically categorises, defines and encodes nursing care in the form of nursing diagnoses, nursing interventions and/or nursing outcomes.49,50 Research indicates that SNCPs, in both electronic and paper formats, significantly improve documentation quality. 51 However, challenges in sustaining their use arise from limited SNL knowledge, staffing shortages and low nurse motivation. 52 In healthcare settings, the adoption of standardised care plans is influenced by nurses’ perceptions of their utility, implementation issues and personal preferences. 53 Despite favourable attitudes in South Africa, adopting an electronic clinical decision support system was limited due to inadequate computer proficiency and technical assistance. 45 To maximise advantages and mitigate risks, evidence-based strategies for the design, implementation, evaluation and maintenance of CDSTs are critical. 42 In Kenya, technical elements such as information and communication technology (ICT) infrastructure and internet availability substantially impacted EHR adoption rates. 54 Notwithstanding infrastructural constraints, EHR systems were generally embraced in Rwanda, with enhanced iterations contributing to increased perceived utility. 55 As healthcare systems across Africa adopt digital technologies, nurses play a crucial role in implementing and utilising EHRs. Thus, this scoping review aims to map evidence about nurses’ adoption of EHRs in Africa.
Methods
This study was guided by the framework of Levac et al.
56
This framework provides guidelines for conducting scoping review studies and is comprised of the following steps:
identifying the research questions identifying relevant studies study selection charting the data collating, summarising and reporting the results
Step 1: Identifying the research questions
Applying the Levac et al.
56
framework to map studies about nurses’ adoption of EHR in Africa involved clearly defining and refining the research question. This scoping review is informed by three research questions that were systematically developed based on insights from the existing literature. These research questions aim to provide a comprehensive understanding of nurses’ engagement with EHRs in Africa. Specifically, they seek to investigate how nurses utilise EHRs in clinical practice, identify perceived barriers to their adoption and explore strategies for successful implementation and utilisation. Examining the experiences and perspectives of nurses is crucial for addressing knowledge gaps, informing evidence-based policy and developing contextually relevant approaches to enhance digital health integration in resource-constrained healthcare systems.
How do nurses utilise EHRs in their practices in Africa? What barriers do nurses perceive as hindering the adoption of EHRs in Africa? What strategies would facilitate the successful implementation and utilisation of EHRs among nurses in Africa?
Step 2: Identifying relevant studies
A comprehensive literature search was conducted on 11 October 2024 and 12 October 2024 across six databases, covering publications between 2014 and 2024: CINAHL, Emcare, Medline, Psychinfo, Scopus and Web of Science. The review considered both primary research studies and grey literature. The grey literature sources include government publications, healthcare policies and conference proceedings. Additional sources were obtained through manual searches from Google and Google Scholar. The following keywords were used: ‘nurses’, ‘electronic health records’ and ‘Africa’. The search strategy was iterative, with adjustments based on the databases and initial results to ensure all relevant studies were included. Table 1 presents a customised search string per database.
Customised search string per database.

Step 3: Selection of studies
Inclusion and exclusion criteria were established to guide the selection process. 56 Studies focusing on nurses’ adoption of EHR in African countries were included regardless of study design, while those not specific to nursing or nurses or conducted outside Africa were excluded. Studies were published between 2014 and 2024, and the English language was an inclusion criterion. The Mixed Methods Appraisal Tool (MMAT) 57 was used to evaluate the methodological quality of the studies included in the scoping review. Each study was assessed according to the appropriate MMAT criteria for its design, and the results were summarised descriptively to emphasise both the methodological strengths and limitations. Furthermore, the research questions guided the selection of relevant studies. A researcher and an expert in the scoping review screened titles and abstracts, followed by a full-text assessment of qualifying articles. Any disagreement was solved through consensus. 56 Reasons for excluding studies were documented to maintain transparency.
A total of 2107 records were identified, of which 1994 were retrieved through database searches, specifically CINAHL (n = 110), Emcare (n = 43), Medline (n = 137), PsychInfo (n = 100), Scopus (n = 606) and Web of Science (n = 998). An additional 113 records were acquired through manual searches. Following the removal of duplicates, 1534 records remained for screening. Of these, 1480 records were excluded based on title and abstract screening. The remaining 54 full-text articles were evaluated for eligibility, leading to the exclusion of 42 articles for various reasons, including being non-empirical (n = 2), involving the incorrect population (n = 10) or falling outside the study's scope (n = 30). Ultimately, 12 studies met the inclusion criteria and were included in the data extraction and thematic analysis, comprising one qualitative study, six quantitative studies and five mixed-methods studies. A PRISMA flowchart was developed to display the final number (Figure 1).
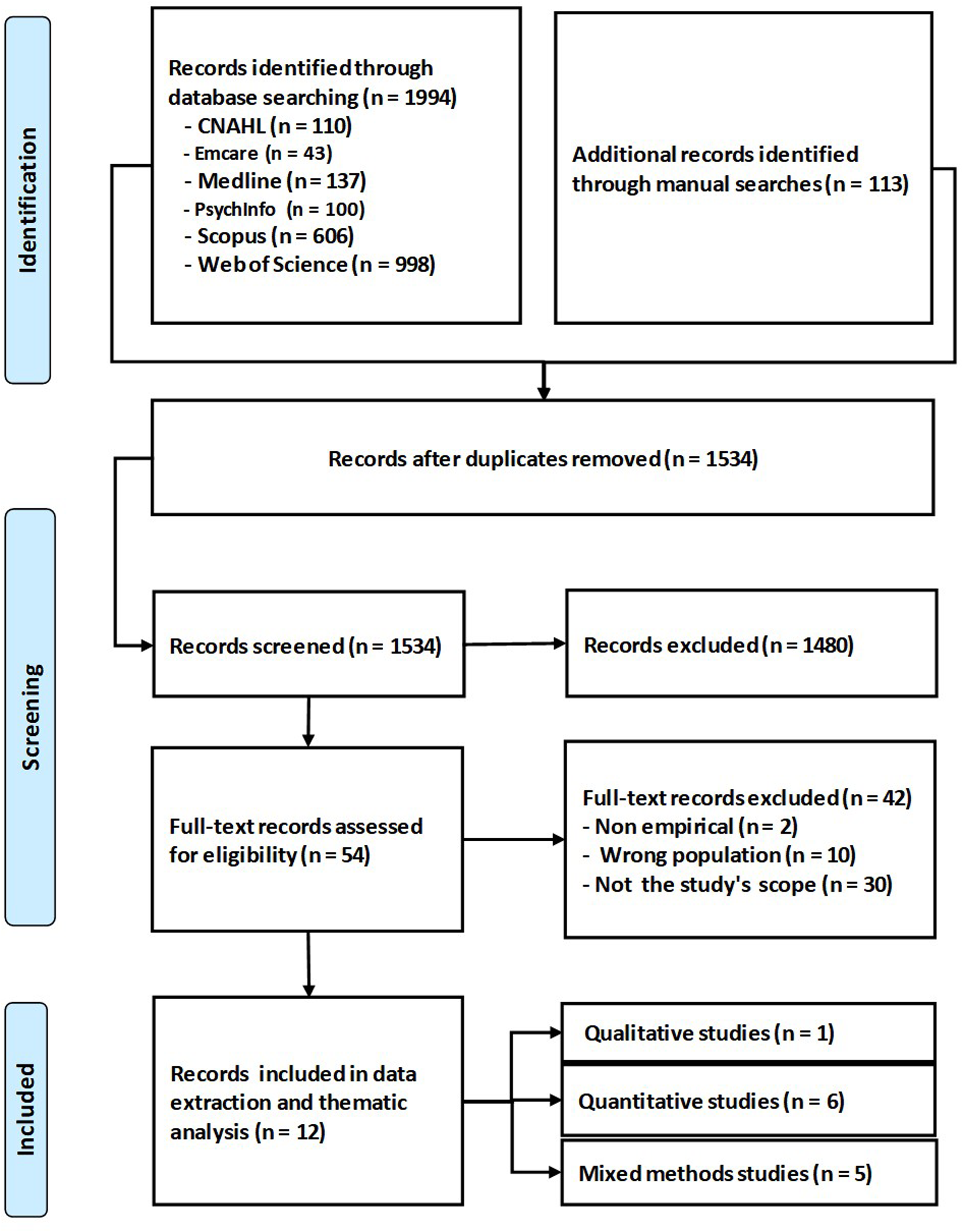
A PRISMA flowchart.
Step 4: Data charting
A standardised form was used for data extraction to ensure consistency and completeness. 56 Data points included study details, authorship, publication year, country of origin, population, study design/ intervention (if applicable) and key findings (Table 2). A total of 12 articles met the inclusion criteria and were included in the data extraction and synthesis.
Overview of the selected studies.
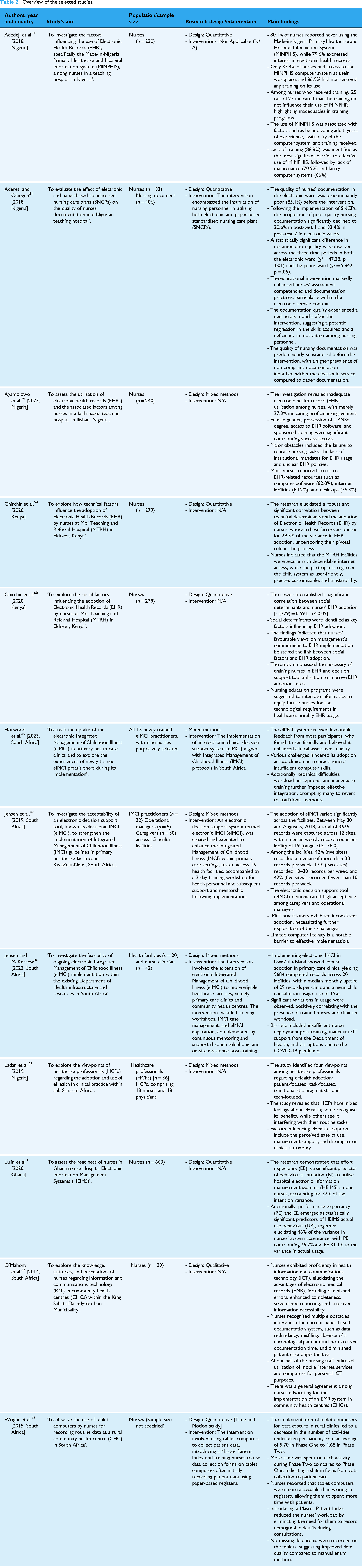
Step 5: Collating, summarising and presenting the findings
After data charting, data analysis followed a six-phase thematic framework from Braun and Clarke. 64 This framework provided a structured and systematic approach that promoted consistency and reliability throughout the analysis. The division into distinct phases enabled researchers to focus carefully on each step, thereby minimising the risk of overlooking important details. The first phase involved iterative readings of the data for familiarisation. In the second phase, researchers developed initial codes by systematically identifying significant features. The third phase aggregated related codes into potential themes. The fourth phase reviewed and refined these themes to ensure they accurately represented both coded segments and the complete dataset. In the fifth phase, themes were defined and labelled to encapsulate their essence and scope. The final phase (Sixth) involved composing the analysis to produce a coherent narrative that directly addressed the research questions. Furthermore, quantitative and qualitative data were combined to provide a comprehensive understanding. Findings were interpreted in line with the research question. The scoping review outcomes were reported following PRISMA-ScR guidelines from Tricco et al. 65
Results
Characteristics of the studies
Twelve studies were included in this scoping review. Geographically, the research is primarily focused on sub-Saharan Africa, with South Africa contributing the highest number of studies (n = 5),45–47,62,63 followed by Nigeria (n = 4),51,58,59,61 Kenya (n = 2)54,60 and Ghana (n = 1). 13 The aims of the included studies varied by country, reflecting the unique challenges and priorities influencing EHR adoption among nurses in sub-Saharan Africa. In Nigeria, research focused on the utilisation of EHR, associated factors and the effect of electronic and paper-based SNCPs on the quality of nurses’ documentation. Studies in South Africa assessed the implementation of digital tools, such as eIMCI, and highlighted the disparities between rural and urban areas. Kenyan research explored the technical and social barriers that hinder adoption in under-resourced settings. In Ghana, the emphasis was on nurses’ readiness and behavioural intentions, utilising the Unified Theory of Acceptance and Use of Technology (UTAUT) model. Methodologically, the majority of studies were quantitative (n = 6),13,51,54,58,60,63 followed by mixed methods (n = 5)45–47,59,61 and qualitative (n = 1). 62 Furthermore, of 12 studies, five adopted interventional designs introducing training programs or digital tools like SNCPs and the eIMCI electronic decision-support tool to improve EHR usage.45–47,51,63
The selected studies revealed several common themes, including the adoption of EHRs by nurses, barriers and strategies affecting the adoption of EHRs by nurses.
Adoption of EHRs by nurses
Of the 12 studies included in this review, seven studies indicated suboptimal engagements with EHRs among nurses.45,51,58–62 In Nigeria, EHR utilisation is notably poor,51,58,59,61 with 80.1% of nurses never using the Made-In-Nigeria Primary Healthcare and Hospital Information System (MINPHIS) and 92.7% not employing it for patient tasks. 58 Despite the availability of infrastructure, EHR usage is only 27.3%, 59 although Ladan et al. 61 identified a slight upward trend. In South Africa, EHR adoption is rising but remains inconsistent.45–47,63 The implementation of the electronic Integrated Management of Childhood Illness (eIMCI) demonstrated strong adoption,46,47 though urban areas benefited disproportionately compared to rural regions. 45 Similarly, in Kenya, EHR adoption is poor, especially in rural regions, primarily due to infrastructural and funding limitations. 54 In South Africa, O'Mahony et al. 62 reported minimal EHR implementation in community health centers.
Nine studies established a link between EHRs adoption and nursing documentation.13,45–47,51,58,59,62,63 Adopting EHRs enhances documentation accuracy, healthcare quality, minimal errors, data management and data security.45,47,51,59,62 Two studies from Nigeria found that despite a preference for EHRs, actual usage remained limited.58,59 In Nigeria, although 79.6% of nurses preferred EHRs, 93.7% used paper-based systems. 58 A study conducted in South Africa by O’Mahony et al. 62 reported that the reliance on paper-based records resulted in increased workloads and errors, underscoring the necessity for electronic systems. Studies in Nigeria and South Africa reported that the persistence of paper-based records compromised documentation quality.58,62 Furthermore, Adereti and Olaogun 51 argued that inadequate training and equipment contribute to poor documentation. In Ghana, effort expectancy significantly influenced nurses’ intent to utilise hospital electronic information management systems. 13
Barriers to nurses’ use of EHRs
Barriers to nurses’ adoption of EHRs are multifaceted, encompassing inadequate computer literacy and training deficiencies, technological infrastructure issues, institutional challenges and resistance to change. Eight studies identified inadequate computer literacy among health professionals, particularly nurses, as a significant issue affecting the use of EHRs.45–47,51,54,58,61,62 The lack of computer skills among practitioners significantly hindered the implementation of EHRs in Nigeria, Kenya and South Africa, affecting their ability and confidence to use the system effectively.45,47,54 In Nigeria, training deficiencies exacerbated this issue, with 88.8% of nurses in one study citing inadequate training as the primary obstacle. 58 In Kenya, Chirchir Chirchir et al. 54 also noted that poor digital skills hinder adoption, particularly in rural areas. South African studies45–47 found that even after training, many nurses felt unprepared for full EHR adoption, with the lack of post-training support and mentorship exacerbating the problem. This lack of preparation and support reduces nurses’ confidence and fosters resistance to adoption.
Technological issues were reported in six studies from Kenya, Nigeria and South Africa and included inadequate computer availability, unreliable internet access, outdated hardware and frequent power disruptions, all of which impede effective EHR use.46,54,58,59,61,62 In South Africa, security concerns, hardware theft and system failures further compound these challenges.46,62 Additionally, insufficient IT support, slow equipment replacement processes and inadequate technical support from management frustrate nurses attempting to use these systems. 46 In Nigeria, complex EHR software designs were reported to create usability issues, particularly for nurses unfamiliar with advanced technology. 59
Studies indicated a lack of formal policies and ineffective management practices as critical barriers to EHRs.46,58,59 The absence of robust policies and enforcement mechanisms results in inconsistent EHR implementation and utilisation. 59 High patient-to-nurse ratios and heavy workloads limit the time available for nurses to learn and effectively use EHRs, while frequent staff rotations disrupt continuity and training.47,59 The dual burden of maintaining both electronic and paper records exacerbates workflow disruptions, making EHR systems appear cumbersome and inefficient.45,47 Studies from Nigeria and South Africa reported that some nurses perceived EHRs as an additional burden rather than a tool that seamlessly integrates into their daily practice, deterring adoption.61,62 In Nigeria, Ladan et al. 61 reported that some nurses viewed eHealth technologies as a burden rather than a clinical asset. Concerns regarding job displacement, increased workloads and the perception that EHR systems complicate workflows contributed to resistance to transition from paper to digital systems.45,61 Two studies indicated an association between age and the adoption of EHRs58,62 and older staff were prone to resistance to change. 62
Strategies to enhance nurses’ use of EHRs
Strategies to enhance nurses’ use of EHRs are multifaceted and focus on training, standardised documentation, clear policies and organisational support. Studies from Kenya, Nigeria and South Africa have highlighted the importance of comprehensive training and capacity building to equip nurses with the skills needed to effectively use EHRs, addressing a significant barrier to their adoption.45–47,51,58–60,62,63 Interventional studies have shown that structured training, mentorship and the integration of digital tools into nursing workflows can enhance confidence and competence in EHR use.45–47,51,63 Studies from Nigeria emphasised the importance of training in enhancing nurses’ ability to effectively use EHRs.51,58,59 Adereti and Olaogun 51 conducted an intervention in Nigeria to train nursing personnel to use electronic and paper-based SNCPs, using a structured training package employing SNLs, emphasising the integration of standardised care protocols with EHR systems. Adedeji et al. 58 underlined the need for comprehensive training programs to address the skills gap and confidence deficits in EHR utilisation, which hinder effective implementation. Similarly, Ayamolowo et al. 59 highlighted the importance of ongoing training to improve nurses’ competence and confidence in EHR usage.
In South Africa, various interventions have targeted EHR implementation and nurse training.45–47,63 Horwood et al. 45 introduced an electronic clinical decision support system (eIMCI) that follows the Integrated Management of Childhood Illness (IMCI) protocols. This intervention encompassed structured training in computer literacy, practical application in clinical settings and ongoing mentorship to encourage effective adoption and sustained use by healthcare providers. 45 Similarly, Jensen et al. 47 and Jensen and McKerrow 46 conducted eIMCI workshops, emphasising the necessity of continuous support and digital literacy for sustained EHR utilisation in clinical environments. Wright et al. 63 optimised nursing workflows through the introduction of tablet computers for data collection, facilitating the transition from paper-based to electronic systems, highlighting the critical role of adequate training in EHR implementation. Collectively, studies from Nigeria51,58,59 and South Africa45–47,63 confirm that continuous and structured training is essential for overcoming challenges and ensuring the successful adoption of EHR systems in Nigerian healthcare settings.
Eight studies highlighted the crucial role of standardised electronic documentation systems in improving nursing efficiency and patient care outcomes.13,45,47,51,58,59,62,63 Various electronic systems, including EHRs, EMRs and Hospital Electronic Information Management Systems (HEIMS), are recognised for their ability to enhance documentation accuracy and streamline workflows. In Nigeria, Adedeji et al. 58 and Adereti and Olaogun 51 emphasised the transition to EHRs and SNCPs to improve structure and efficiency, while Ayamolowo et al. 59 advocated for the adoption of EHRs, highlighting their capability to provide comprehensive digital patient records. Studies from South Africa62,63 reported that EMRs and EHRs were effective in reducing documentation errors and redundancy while also improving accessibility. Additionally, studies from Ghana 13 and South Africa45,47 have indicated that optimising digital tools before implementation was essential, as usability could significantly enhance nursing confidence and efficiency.
Three studies reported that well-defined policies are essential for promoting EHR adoption in healthcare settings.51,59,61 Two studies highlighted the importance of involving HCPs in policy development, ensuring system interoperability and establishing a unified legal framework to address barriers to EHR utilisation.51,59 Ladan et al. 61 identified the lack of comprehensive policies as a significant challenge in Nigerian healthcare institutions, leading to inconsistent adoption practices and unsustainable local policies. Moreover, insufficient managerial support hindered adherence to these policies. 61 Ayamolowo et al. 59 emphasised the need for clear written guidelines, advocating for system interoperability and nurse engagement during implementation. Adereti and Olaogun 51 further stressed the importance of standardised care plans and protocols in improving documentation practices. Studies indicated the necessity for structured, legally enforced EHR policies to enhance adoption and improve patient care.51,59,61
Organisational support is crucial for the successful adoption and use of EHRs by nurses, as evidenced by seven studies.45,47,58–62 Essential resources, including operational computer systems, reliable electricity and internet access, are vital for EHR implementation.58,59 Strong management commitment and stakeholder collaboration help address social factors such as staff attitudes and skills.58,60 Leadership and resources mitigate barriers like heavy workloads and resistance to change.45,60 Incentives, IT support and mentorship further facilitate the transition.47,62 Without adequate support, EHR adoption faces resistance and underutilisation. 61 A multi-level approach ensures EHR effectiveness.58–60
Discussion
The reviewed studies highlight the suboptimal usability of EHRs among nurses in Africa. While nurses show positive attitudes towards EHRs, the continued reliance on paper-based documentation reflects a global trend of low EHR usability ratings. Similarly, Melnick et al. 66 reported that US nurses rated EHR usability in the lowest 24% of systems assessed. Complex interfaces challenge workflow efficiency and impede nurses’ effective access to patient information.67,68 Additional factors such as low digital literacy, stress, burnout, cognitive load and the risk of errors exacerbate these challenges, underscoring the necessity for management support and targeted, ongoing training for nurses.31,68–70 Data privacy, security and integrity concerns persist, necessitating robust policies and strategies to address these barriers.71–73
African nurses encounter unique challenges, including limited computer literacy, insufficient training, and EHR systems that lack user-friendliness, completeness, and integration.45,46,51,74 Furthermore, there is resistance to EHR adoption, primarily associated with concerns regarding job displacement and increased workload, particularly among older personnel. 75 Established workflow patterns and discomfort with EHR implementation further intensify resistance. Nevertheless, adequate training and confidence-building initiatives can alleviate these challenges. 75 Organisational support, including the provision of resources and training, is vital for overcoming resistance, although it may not be solely sufficient. 75 Enhancements in EHR usability and the work environment can improve nurse and patient outcomes.70,76
Institutional policy gaps significantly hinder EHR adoption. Ayamolowo et al. 59 highlighted that policy deficiencies increase nurses’ workloads during EHR implementation, often persisting for years. 77 Comprehensive frameworks to promote digital health and government investments are essential. 78 In South Africa, initiatives like the National Digital Health Strategy and the Health Normative Standards Framework aim to enhance digital health but lack actionable guidance for implementation. 78 Effective leadership, governance, and policy adaptability are critical for addressing diverse regional needs. 78
Strategies for facilitating EHR adoption encompass user-centred system designs, policy support, and structured organisational frameworks. Training and capacity-building initiatives are crucial for effective EHR utilisation.79,80 Access to computing resources and enhanced digital literacy are also essential.80,81 Governance, leadership and end-user participation are fundamental to successful implementations. 82 Context-aware technical support and robust system functionalities further enhance sustainable adoption.79,83 Furthermore, continuous, specialised in-service training tailored to nursing requirements is imperative. 51 Incorporating health informatics into nursing curricula will better equip future professionals60,84,85 Wright et al. 63 and Harerimana and Mtshali 86 advocate for integrating familiar mobile technologies into formal training programmes. User-friendly system designs featuring touch-screen interfaces and intuitive functionalities can enhance usability.59,62 The embedding of standardised nursing terminologies (SNTs) can improve documentation accuracy and streamline care processes. 58
Addressing technical infrastructure through strategic ICT planning, private-sector collaboration, and robust support systems is critical.13,46,54 Successful EHR adoption also relies on established policy frameworks and stakeholder engagement. Ladan et al. 61 emphasised the necessity of involving HCPs in eHealth decision-making to foster ownership and mitigate resistance. Clear policies that endorse EHR implementation are essential. 59 Aligning EHR tools with healthcare workflows through formative research can enhance user acceptance. 45 Ongoing mentorship, supervision, and monitoring and evaluation frameworks are pivotal to ensuring sustained EHR efficacy.47,51,58
The adoption of EHRs among African nurses remains nascent, as paper-based systems prevail due to infrastructural and technological constraints. A comprehensive strategy incorporating advanced EHR systems, technological upgrades, targeted training, robust policies, and informatics integration into nursing education is crucial for transforming nursing practice and enhancing care standards. These interventions must comprehensively address technical, educational, and human-centric dimensions to establish a sustainable, user-friendly EHR ecosystem.
Limitations of the study
The limited number of the included articles highlights the niche or emerging nature of the topic, limiting the generalisation of the findings and indicating a need for further exploration in this field. Furthermore, the studies used diverse methodologies, which complicate comparisons. Additionally, inconsistent interventions and limited follow-up obscure their long-term impacts. Future research should address these gaps using standardised methods and longitudinal studies, which are essential for assessing interventions’ sustainability and long-term effects and ultimately ensuring lasting improvements in healthcare practices.
Implications to nursing practice and policy
The adoption of EHRs enhances patient care and safety by facilitating rapid access to comprehensive patient data, standardising documentation and minimising errors. Effective training is crucial for equipping healthcare personnel with the skills necessary for proficient system use. Research is required to evaluate various training models, create user-friendly EHR systems aligned with nursing workflows, and assess their long-term impacts on practice. Comparative studies across African healthcare systems can identify scalable solutions, while investigations into EHRs’ effects on workload can facilitate integration. Policymakers must prioritise EHR integration into national healthcare strategies through supportive policies, adequate funding, and access to technology, particularly in underserved regions. Emphasis on interoperability among systems is essential to enhance care coordination while ensuring data security. Sustainable EHR adoption necessitates leadership, training, and resource allocation, ultimately leading to improved health outcomes and more efficient healthcare delivery.
Conclusion
This scoping review examined nurses’ use of EHRs in Africa, along with the barriers and strategies influencing their adoption. EHRs enhance healthcare delivery by improving data accuracy, patient safety and workflow efficiency. However, implementation challenges include inadequate infrastructure, limited digital literacy, resistance to change and insufficient training. Adoption is more advanced in urban areas, while many rural regions still rely on paper-based systems. Despite these challenges, there is growing awareness of the benefits of EHRs for nursing documentation and patient care, along with an increasing willingness among nurses to adopt these technologies when adequate support is provided.
Coordinated efforts from policymakers, healthcare leaders and practitioners are essential to expedite EHR adoption. Investments in infrastructure, particularly in underserved regions, and the development of user-friendly systems that cater to local contexts are critical. Continuous training programs to enhance nurses’ digital literacy and emphasise data accuracy, patient confidentiality and information security are necessary. Integrating informatics education into nursing curricula and professional development will empower nurses to utilise EHRs effectively. These initiatives will enhance nursing practice and bolster healthcare delivery across Africa, facilitating evidence-based policymaking and improved patient outcomes.
Footnotes
Author contributions
Conceptualisation was done by AH, KW, NB, KY, JP, GM.
Data collection was done by AH.
Data analysis was done by AH, JP, GM.
Study supervision was done by KW, NB, KY, JP, GM.
Manuscript writing was done by AH, KW, NB, KY, JP, GM.
Critical revisions for important intellectual content were done by AH, KW, NB, KY, JP, GM.
Funding
The authors disclosed receipt of the following financial support for the research, authorship and/or publication of this article: This research is funded by the Harnessing Talent (HANT) Post Doctoral Fellowship (PDF) award from the Durban University of Technology (DUT), in Durban, South Africa.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Guarantor
Primary Author: AH.
