Abstract
Background
Telepharmacy is becoming an inevitable trend in the field of pharmaceutical care, especially in the Fourth Industrial Revolution. The use of telepharmacy systems in pharmaceutical consulting services has the potential to offer many benefits. However, a clear and comprehensive evaluation is necessary to ensure an optimal telepharmacy system. The study was conducted to assess the effectiveness of telepharmacy (www.telepharmacy.vn) in pharmaceutical consulting services for outpatients at Le Van Viet Hospital in Ho Chi Minh City. The MAST (Model for Assessment of Telemedicine) model was used to evaluate the effectiveness of the telepharmacy system.
Methods
This is a cross-sectional study evaluating the effectiveness of telepharmacy system (www.telepharmacy.vn) in pharmaceutical consulting services for outpatients at Le Van Viet Hospital, Ho Chi Minh City, in 2024, using the MAST model.
Results
The total number of participants was 51. According to the survey, 48 out of 51 patients (94.1%) reported satisfaction after consultation, with significant support from the hospital staff. Most of the evaluations on various aspects of the system according to the MAST model supported the application of this system in medication consultation activities at the hospital.
Conclusion
The positive feedback has encouraged the hospital's administration to widely implement this new system to improve and enhance the quality of outpatient care services.
Keywords
Introduction
Telepharmacy is a part of telemedicine that involves the provision of services by pharmacists through a remote system, without the need to meet patients or healthcare professionals in person.1,2 These services include selecting medications, reviewing prescriptions, offering patient consultations, and providing clinical services by using technological applications.3,4 Many studies have demonstrated that telepharmacy can improve the quality of healthcare services, reduce errors, increase patient access to services, detect drug side effects, improve healthcare professionals’ satisfaction, reduce costs, and enhance pharmacist training. 5
A study conducted in Spain during the COVID-19 lockdown showed that telepharmacy eliminates the need for a 122 km, 90-min commute to reach a healthcare facility, and increased patient satisfaction levels to 9.88/10 points. 6 Another study published in September 2024 found that the average annual growth rate of telepharmacy studies is 8.07%. 7 Emerging from the COVID-19 lockdown, telepharmacy was strongly promoted in Vietnam, with up to 86.7% pharmacists using this technology. 8 However, since the pandemic ended in 2023, telepharmacy growth has slowed down compared with 2021. 7
Le Van Viet Hospital is one of the public hospitals in Thu Duc City that actively applies information technology to pharmaceutical management. The hospital has hundreds of beds and receives thousands of patients daily. The hospital leadership, particularly in the Pharmacy Department, is very interested in improving the pharmaceutical consulting services, specifically drug consultation, where the application of telepharmacy is one of the priorities to optimize resources and meet patient consultation needs. A recent study was conducted to detail the current situation of pharmaceutical consultation needs at Thu Duc City Hospital, Ho Chi Minh City. 9 The results show that the demand for drug consultation through telepharmacy among patients was as high as 60.3%. 9 However, expanding and fully deploying this service still faces many challenges.
The MAST (Model for Assessment of Telemedicine) model is a comprehensive evaluation framework for telemedicine that includes all relevant medical, social, economic, and ethical factors. The model has been applied in multiple countries globally. 10 The MAST model, with its comprehensive approach, covers all aspects of the telemedicine system, proving its credibility in evaluating effectiveness and identifying areas for improvement. Applying the MAST model can enrich discussions on the evaluation of emerging technologies in the healthcare sector, such as mobile applications. 11
With the main goal of increasing healthcare benefits for the population, providing quick and timely access to medical services, and reducing the burden on medical facilities, the Vietnamese government has issued critical directives promoting telemedicine. These directives outline the importance of digital transformation in the health sector through strong applications of digital technology.
In the context of promoting the application of information technology in regard to the medical field, hospital conditions, and the current situation of various patients’ drug consultation needs, we have begun deploying telepharmacy in pharmaceutical consultations for patients at Le Van Viet Hospital, Ho Chi Minh City. By applying the MAST model, all aspects surrounding telepharmacy will be fully considered and weighed. This will allow for the expansion and more effective deployment of remote drug consultations for patients.
Method
Study design
This is a cross-sectional study conducted from January 2024 to June 2024. Study participants were selected by convenience sampling and included patients over 18 years of age who agreed to participate in the study and use pharmaceutical consultation services through the telepharmacy system (www.Telepharmacy.vn) built and developed by the research team of Saigon Pharmaceutical Science and Technology Center. To avoid ethical and legal issues, it was necessary to exclude individuals under the age of 18. In addition, telepharmacy consultations may require additional consent from parents or guardians for minors.
Exclusion criteria
Emergency patients
Patients receiving controlled medications
Patients who did not consent to participate in the survey
Patients who did not complete the survey
The consultations were conducted by clinical pharmacists of Le Van Viet Hospital via telepharmacy software. There were 51 patients participating.
Another survey was conducted for the Board of Directors, Pharmacy Department Leadership, and Medical Staff to assess the economic viability from the perspective of hospital staff. This survey included 1 deputy director of the hospital, a head of the Pharmacy Department, and 13 pharmacists from the Pharmacy Department. These individuals were selected through convenience sampling based on their availability and role in hospital operations. While they did not directly participate in the telepharmacy consultations, their insights were valuable in evaluating the system's feasibility.
Study instruments
To conduct the study, several tools were employed to evaluate and implement the use of telepharmacy services. One critical tool was the telepharmacy computer software (www.telepharmacy.vn) that allowed users to schedule drug and pharmaceutical consultation sessions, send messages, and make voice and video calls after successfully scheduling an appointment. The software also enabled users to purchase medications, fill prescriptions, make online payments, and access medical news. Consultations were conducted by clinical pharmacists from Le Van Viet Hospital through video calls, voice calls, or messaging. Each session followed a structured protocol. Started by reviewing medical history and prescription details; then provided medication counseling, including proper usage, dosage adjustments, and potential drug interactions; and concluded by advising patients on further actions if needed.
After using this application, patients were surveyed using a standardized questionnaire, in which the first part gathered information on the patient's demographics and medical conditions that required drug use consultation, then documented patients’ opinions and satisfaction levels. The questionnaire was reviewed by clinical pharmacists to ensure clarity and relevance before being administered to patients. While expert-reviewed, no formal validation study was conducted. A separate questionnaire was designed for the Board of Directors, Pharmacy Department Leadership and Medical Staff on the cost-effectiveness of telepharmacy consultation.
The evaluation process has followed the sequence of steps according to the MAST model obtained from Kristian Kidholm et al. including the following 10 : The evaluation sequence used in this study follows the three-step structure of the MAST model in Figure 1. The MAST framework consists of three sequential steps: (1) Preliminary assessment of the telemedicine application; (2) Multidisciplinary assessment across seven domains—health problem and characteristics of the application, safety, clinical effectiveness, patient perspectives, organizational aspects, economic aspects, and sociocultural, ethical, and legal aspects; and (3) Transferability assessment. This structure ensures a comprehensive and policy-relevant evaluation of telehealth interventions (Figure 1).

Evaluation sequence in Model for Assessment of Telemedicine (MAST) model. 10
Data collection method
The data collection tools included five structured instruments: (1) Consent form to participate in the study (Appendix 1); (2) Preintervention questionnaire for patients on their demand for drug use counseling (Appendix 2); (3) Questionnaire for the Board of Directors and pharmacists on current demand and organizational readiness for pharmaceutical counseling (Appendix 3); (4) Patient satisfaction survey after receiving pharmaceutical consultation via the Telepharmacy system (Appendix 4); and (5) Questionnaire for the Board of Directors and pharmacy staff evaluating the cost-effectiveness of pharmaceutical consultations via the Telepharmacy platform (Appendix 5).
During the survey process, researchers also collected contact information from patients so that the hospital's clinical pharmacists could provide further guidance on installing the telepharmacy software and offer consultations. After the consultation, the researcher contacted the patient to conduct a survey on their opinions and satisfaction level. The researcher observed and evaluated the system according to the MAST criteria.
The collected information was processed and analyzed to support the evaluation, alongside descriptions of the characteristics of the telepharmacy system. The steps of the MAST model assessment were conducted following the guidelines of Kristian Kidholm et al., including preceding considerations, multidisciplinary assessment, and transferability assessment. 10
Data analysis
The collected data were analyzed using IBM SPSS Statistics 27 statistical software. The results were presented in the form of charts, tables, and using descriptive statistics with frequencies and ratios (expressed in %). The univariate analysis calculated the odds ratio (OR) and 95% confidence interval (CI) to examine the association between independent variables and the need of using these pharmaceutical consultation services at the next visit. Independent variables included demographics, patient's feedback on satisfaction and money-saving aspects, and their willingness in paying for the consulting services if the service was chargeable.
Results
General characteristics among the 51 patients surveyed after using the medication consultation through the telepharmacy application, 26 out of 51 participants were female, accounting for 51.0%. The median age is 49 with the youngest participant being 19 and the oldest 73. The most common age group is 18–30 years, with 20 participants (39.2%). Details are presented in Table 1.
General characteristics of survey subjects after drug use consultation using telepharmacy (n = 51).

College/University educational level has the largest sample size, comprising 43.1%, while the lowest is Primary school or below, at 5.9%. The highest income group was those earning 10–20 million VND per month, accounting for 19 participants (37.3%). Unemployed subjects, such as students or those of working age/retired, account for 15.7% and 19.6%, respectively. The distribution of 51 patient's treatment in 6 different departments is shown in Figure 2. However, the relatively small sample size (n = 51) poses limitations on the generalizability of the results. This limitation is common in exploratory telepharmacy studies, suggesting future research in Vietnam should aim for broader sample inclusion to enhance external validity.

Disease groups recorded from outpatient treatment.
In this study, chronic disease groups such as cardiovascular and endocrine diseases accounted for the highest proportion of patients seeking treatment at the hospital, 31.4% and 27.5%, respectively. The 51 patients participating in the medication consultation via the telepharmacy system also belonged to these two major disease groups. The result of patients’ opinions as well as satisfaction level after medication consultation via telepharmacy system is shown in Table 2.
Survey of patients’ opinions after pharmaceutical consulting services via telepharmacy software.
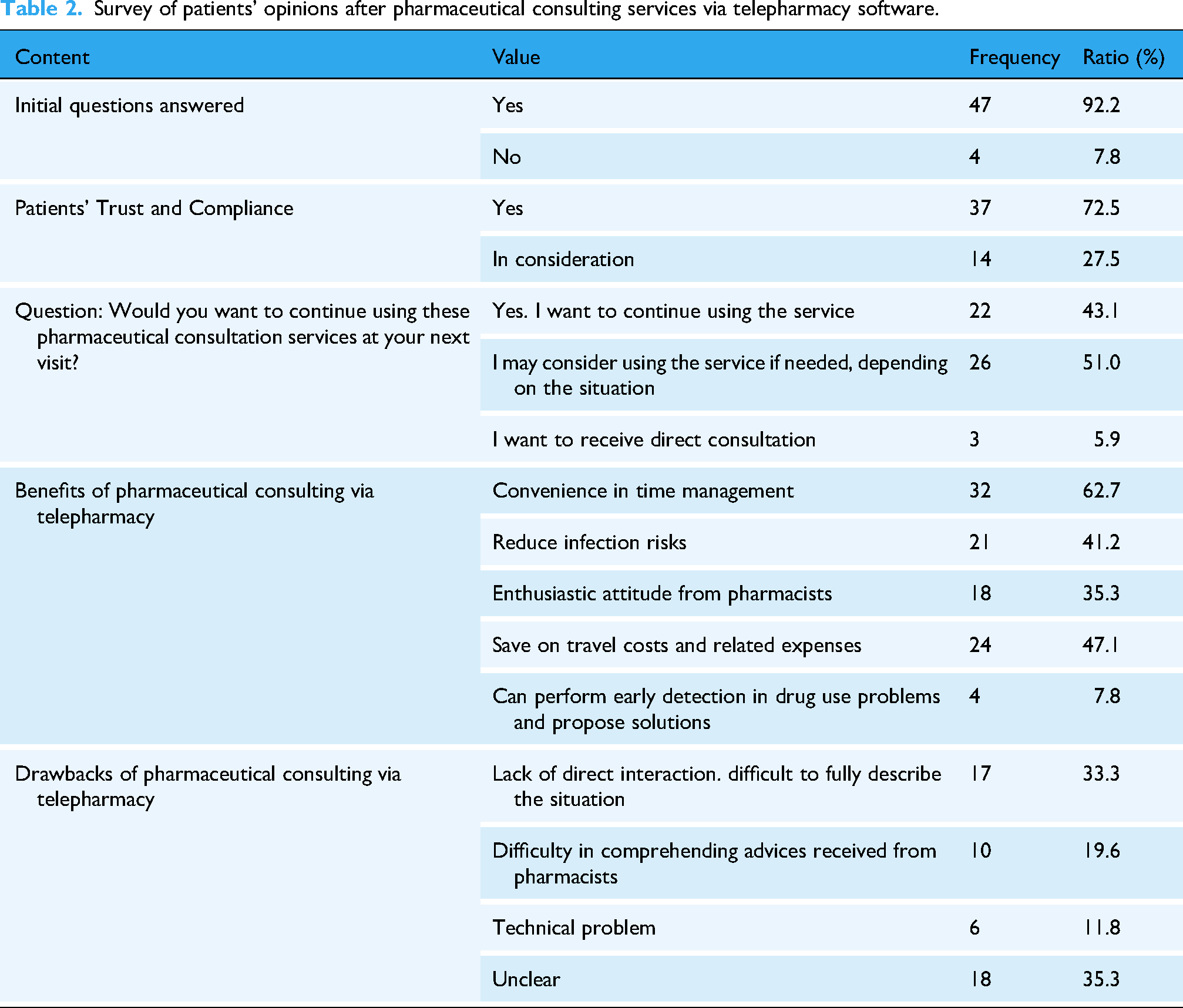
Forty-seven out of 51 patients (92.2%) reported that all questions related to their disease/drug use were satisfactorily answered, and 37 out of 51 patients (72.5%) demonstrated a high level of trust and compliance, as shown in Table 3.
Patient satisfaction level after consultation via the telepharmacy system on the 5-point Likert scale.

The level of patient satisfaction after consulting via telepharmacy system was measured using a 5-point Likert scale. The consulting service received high ratings, with a satisfaction rate of 41 out of 51 participants (80.4%) rating ‘Satisfied’ or ‘Very Satisfied’. Twenty-five out of 51 participants (51.0%) expressed willingness to recommend the service to relatives and friends. The primary advantages cited were the convenience of scheduling consultations and the savings on travel costs. In this study, economic perspective was evaluated by patients’ willingness to pay and opinions on cost benefits of telepharmacy pharmaceutical consulting services. The results are shown in Table 4.
Survey of patients’ willingness to pay and opinions on cost benefits of telepharmacy pharmaceutical consulting services.
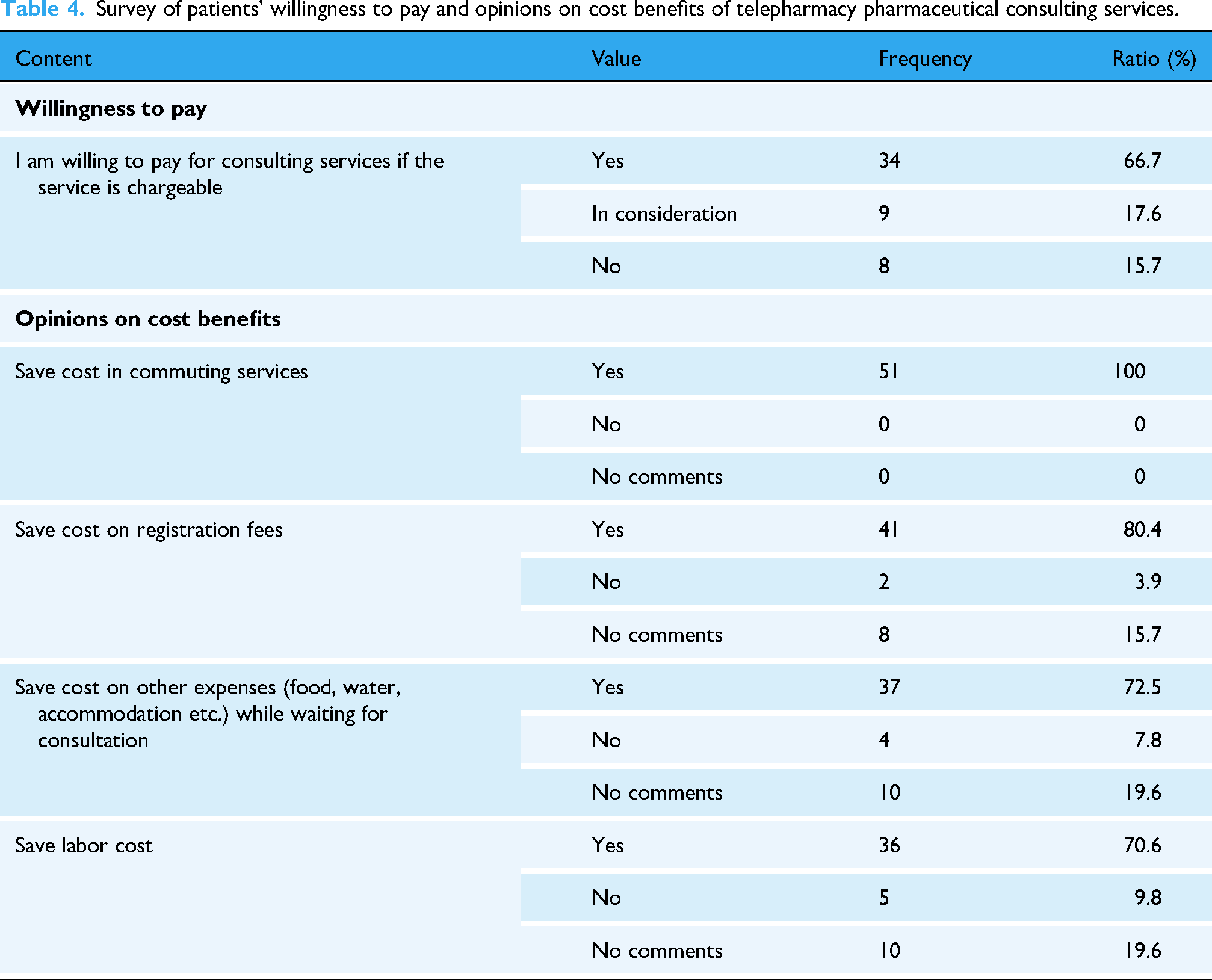
Table 5 compares the association between independent variables, such as patient satisfaction, cost-saving factors, and willingness to pay, and the expressed need to use pharmaceutical consultation services at the next visit. There was a statistically significant association between the expressed need and several factors. Notably, patients who reported dissatisfaction after consultation were significantly more likely to express the need to use the service again (OR: 4.82; 95% CI: 1.31–17.79; p = 0.018). Similarly, patients who did not save on other expenses (such as food, water, and accommodation) showed a much higher demand for the service (OR: 7.06; 95% CI: 1.38–36.05; p = 0.019). Additionally, those who did not save on labor costs also demonstrated a significantly higher need (OR: 4.47; 95% CI: 1.08–18.58; p = 0.039). Although willingness to pay showed a borderline association (OR: 3.66; 95% CI: 0.99–13.52; p = 0.052), other variables such as gender, age, education, and income were not significantly associated (p > 0.05).
Some factors related to need using these pharmaceutical consultation services at your next visit.

Note. The bold values in Table 5 indicate statistically significant results (p < 0.05).
Regarding the opinions and perspectives from the Board of Directors, Pharmacy Department Administration, and Medical staffs on the cost benefits of telepharmacy consultation, the results are recorded in Table 6.
Survey of board of directors, pharmacy department leadership and medical staff on the cost benefits of telepharmacy consultation.

One hundred percent of the surveyed subjects agreed that consultation via the telepharmacy system brings at least one cost benefit to both the patient and hospital staff. The most common response was reducing the cost of handling cases of noncompliance with treatment plans, with 28.6% agreement.
Table 7 summarizes the assessment of the telepharmacy system using the MAST model. The evaluation includes 12 components across three major domains: preceding considerations, multidisciplinary assessment, and transferability assessment. These criteria reflect a comprehensive analysis of telemedicine services, covering clinical effectiveness, patient perspectives, safety, and economic and organizational considerations. This summary provides an essential basis for discussing the current status and future potential of the telepharmacy system being piloted.
Telepharmacy system assessment checklist using MAST model.

MAST: Model for Assessment of Telemedicine.
Discussion
Preceding considerations
The pharmaceutical consulting services offered through the telepharmacy system were first implemented in Vietnam at Le Van Viet Hospital and Thu Duc City Hospital, Ho Chi Minh City in March 2022. 9 This is a model that helps to shorten the distance between patients, pharmacists, hospitals, and reducing difficulties in treatment compliance. The operation procedures are simple, with specific steps for patients. First, patients arrange an appointment for consultation and purchase a prescription online via text message, voice call, or video call. A pharmacist then provides instructions on drug usage and potential adverse reactions, and patients can also proactively schedule a follow-up appointment. 9
On January 9, 2023, the Vietnamese National Assembly issued Law 15/2023/QH15 allowing remote medical examinations and treatment activities, including telepharmacy. In addition, the Ministry of Health has deployed the “Vietnam Healthcare Network” platform within the National Digital Transformation Program, with the main goal of creating an internal network connecting all medical staffs nationwide. As a result, the implementation of this telepharmacy system does not encounter legal obstacles since the Ministry of Health initiated the “Vietnam Health Connection Network.” Payment for online prescriptions through insurance agencies has not yet been specifically regulated. However, current users do not incur any costs upon usage of the system.
According to our preceding considerations, the telepharmacy application is suitable for use in pharmaceutical consulting services at the hospital, as the technical characteristics and implementation process have proven to be convenient and simple. The positive expectations for both patients and the hospital are significant, aligning with the survey responses from patients as well as the Board of Directors and staff at the hospital. The implementation process proceeded smoothly, without serious problems or legal issues. However, raising awareness and promoting the application to more potential users is still necessary.
Multidisciplinary assessment
In this study, a majority of patients had existing cardiovascular and endocrine diseases. Most patients own smartphones, a popular and convenient tool for telepharmacy consultation, especially for chronic patients. 12 According to the survey, this service promises to improve the quality of care by saving time, reducing travel costs, minimizing the risk of infection, and helping to detect drug-related issues early. However, some disadvantages persist, such as difficulties in interacting and receiving information due to environmental or technical problems; 66.7% of users were willing to pay for the service, which was lower than a similar study conducted in Nam Tu Liem District, Hanoi, Viet Nam, accounting for around 69.2% to 74.1%. 13
Additionally, communication with patients regarding drug use is conducted by calling through the telepharmacy system, as calling is frequently reported as a common communication channel for remote healthcare. 14 At the pharmacy, this software is also used to connect third parties with the pharmacy, offering many specialized features. Patients can also send prescriptions to receive advice and have them filled according to the available product list in the telepharmacy system.
The study uses telephone consultation software to guide patients on drug use without affecting their disability or morbidity. This software is implemented by experienced clinical pharmacists and ensures patient information confidentiality. The purpose of the software is to support patients in resolving problems and questions related to drug use and to monitor their satisfaction level.
The main advantages of using the service include the convenience of scheduling and savings in travel costs. However, some limitations, such as the lack of direct interaction and difficulty in describing one's condition, were also noted. The study also suggested measures to improve the service, such as enhancing the quality of voice and transmission.
At Le Van Viet Hospital, the operation process of the telepharmacy software for consultations has not encountered any errors or significant technical shortcomings. In this study, with only two clinical pharmacists in charge of drug use consultations for outpatients, it is challenging to ensure consultation efficiency for all patients participating in the study. However, patients receive consultation according to their personal schedules. The study recorded that over 80% of appointment times were outside regular business hours, with an average contact time of 7–10 min. This is quite short in comparison with research done by Leshem-Rubinow et al., where the majority of calls lasted between 15 and 60 min (47.8%). 15
Patients are also willing to pay for the service if a fee is introduced to reduce other costs. Therefore, telepharmacy is considered an effective solution to help reduce the burden of medical costs for patients, especially in the context of rising healthcare expenses. 16 At the same time, it also helps reduce the number of patients coming for direct examinations, saving costs and improving operational efficiency according to the hospital management team. 4
Transferability assessment
The results obtained from our study are quite comprehensive and can serve as a foundation for future research. This could enable medical facilities to generalize and evaluate other services in the field of telemedicine.
Based on the multidisciplinary assessment, telepharmacy software has been partially proven to be an effective and convenient solution for pharmaceutical consulting services, providing numerous benefits to both patients and the healthcare system. This is also the first study in Vietnam to apply the MAST model to evaluate the effectiveness of telepharmacy software in drug use consultation for outpatients. As there has not been a similar study to compare its effectiveness, it is essential to conduct additional research on the same topic to provide a more thorough evaluation of the software.
Legally, the implementation of telepharmacy in Vietnam is supported by the Law on Medical Examination and Treatment No. 15/2023/QH15. This law officially recognizes and regulates remote medical services, including telepharmacy. Additionally, the Ministry of Health has emphasized the importance of digital transformation and telemedicine in its national health strategy. Policies encouraging remote consultation systems at the grassroots level district and commune healthcare facilities provide a legal and administrative foundation for expanding telepharmacy applications, especially in primary care settings.
As this is the first study in Vietnam applying the MAST model to evaluate telepharmacy services, it inevitably faces certain limitations, such as modest sample size, limited resources, and lack of standardized tools. However, in the context of Vietnam's growing focus on strengthening primary healthcare at the district and community levels, and the government's emphasis on digital transformation in health, this research plays a foundational role. It provides a starting point for future evidence-based telepharmacy interventions and serves as a reference for scaling up remote pharmaceutical services across other regions of the country.
Some limitations we encountered during the study include the small sample size, which may reduce representativeness and make it difficult to draw concrete conclusions about the effectiveness of telepharmacy. This is because many patients at the hospital were hesitant to participate in new technologies like telepharmacy, leading to a high refusal rate. Additionally, some patients’ unfamiliarity with technology may have affected their evaluation of the experience. Overall, these factors restricted our study to a certain population group in Le Van Viet hospital. Therefore, future studies should implement corrective measures, such as expanding the sample size, raising patient awareness, and providing more technical support before and during participation in telepharmacy.
Conclusion
The telepharmacy application is well-suited for pharmaceutical consulting services in hospitals due to its convenience and user-friendly features, bringing significant administrative benefits. Although the implementation process has not encountered significant errors, it is important to raise awareness and promote this form of consultation more widely.
Evaluation steps according to the MAST model show that most of the content meets the necessary requirements, suggesting that the hospital can consider widely deploying the pharmaceutical consulting services via telepharmacy software for outpatients. This expansion not only enhances treatment efficiency but also optimizes the healthcare process, contributing to an improved patient experience. However, as this is the first study in Vietnam to apply the MAST model, there are no comparable studies to assess its effectiveness. Therefore, more studies in the future are needed to evaluate the software more comprehensively and accurately.
Supplemental Material
sj-docx-1-dhj-10.1177_20552076251347734 - Supplemental material for The use of MAST in telepharmacy assessment: First report in Vietnam
Supplemental material, sj-docx-1-dhj-10.1177_20552076251347734 for The use of MAST in telepharmacy assessment: First report in Vietnam by Truong Van Dat, Thai Minh Hoang, Ha My Ly, Nguyen Thi Thu Ha, Nguyen Ngoc Trung, Luong Bao Khanh, Luong Thi Thu Tham, Tran Dinh Trung, Bui Van Nhieu, Nguyen Vu Hung and Vo Linh Tu in DIGITAL HEALTH
Footnotes
Acknowledgements
The authors thank Le Van Viet Hospital and the participating patients and pharmacists for their valuable collaboration.
Ethics approval and consent to participate
The study was approved by the Ethics Council in Biomedical Research, University of Medicine and Pharmacy, Ho Chi Minh City, according to document No. 650/HĐĐĐ-ĐHYD. Written informed consent was obtained from all participants prior to enrollment. For participants under 18, consent was provided by legally authorized guardians.
Author contributions
Truong Van Dat (Dat TV) contributed to study conception and design, data acquisition and interpretation, initial drafting of the manuscript, critical revision for intellectual content, and final approval. He agrees to be accountable for all aspects of the work in ensuring the integrity and accuracy of the research. Thai Minh Hoang contributed to study design, data acquisition, analysis and interpretation, and initial manuscript drafting. Ha My Ly and Nguyen Thi Thu Ha participated in drafting the manuscript and contributed to early-stage documentation. Nguyen Ngoc Trung and Vo Linh Tu contributed to interpretation of findings and manuscript drafting. Luong Bao Khanh and Dinh Trung Tran contributed to data interpretation and critical revision of the manuscript. Luong Thi Thu Tham and Nguyen Vu Hung participated in data analysis and manuscript preparation. Bui Van Nhieu contributed to data analysis and interpretation, and participated in manuscript drafting. All authors have read and approved the final manuscript and agree to be accountable for all aspects of the work.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Department of Science and Technology in Ho Chi Minh City (DOST HCMC), (grant number Decision 1362/QD-SKHCN and Contract no. 99/2020/HD).
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
Data available from the corresponding author upon reasonable request.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
