Abstract
Modern healthcare is experiencing a significant transformation, utilizing technology to improve patient outcomes and make processes more efficient. Breast cancer, being the most commonly diagnosed cancer in women globally, requires innovative approaches for effective management. Digital Therapeutics (DTx) and Clinical Decision Support Systems (CDSSs) have emerged as pivotal technologies, offering personalized, patient-centered care and optimizing clinical decision-making. This review provides a comprehensive analysis of the applications, benefits, and challenges of these digital tools in breast cancer treatment. We examine DTx tools’ ability to offer real-time symptom monitoring, treatment adherence, psychological support, and lifestyle modification guidance. Simultaneously, the role of CDSSs in providing personalized treatment recommendations, early detection, data analysis, and enhancing multidisciplinary collaborations is evaluated. The challenges of implementing these technologies, such as data privacy, interoperability, and accessibility are also discussed, along with potential solutions. By exploring the current research findings, the review underscores the significant impact of DTx and CDSSs on patient outcomes, treatment efficiency, and overall quality of life. This manuscript concludes with a forward-looking perspective, emphasizing the importance of collaborative efforts to overcome obstacles and unlock the full potential of digital innovations in breast cancer oncology. Our analysis suggests that adopting these digital tools can lead to more holistic, efficient, and patient-centric cancer care, marking a significant shift in the paradigm of breast cancer management.
Keywords
Introduction
In the rapidly evolving landscape of modern healthcare, there is a clear and pressing shift towards leveraging technology to enhance patient outcomes and streamline medical processes. For years, the global health sector has navigated the complex challenge of rising demand, often surpassing available resources. Now, with the advent of digital solutions, there is an opportunity to reshape this scenario.1–3 Among the proliferation of digital advancements, Digital Therapeutics (DTx) tools and Clinical Decision Support Systems (CDSSs) emerged as pioneers in contemporary healthcare, and their integration with traditional medical practices is reshaping the paradigms and methodologies of modern care. 4 These technological interventions promise to enhance the standard of care, expand accessibility, improve patient experiences, provide personalized treatments and optimize both treatment adherence and cost efficiency.3,5,6
Within the field of oncology, breast cancer is the most commonly diagnosed cancer in women worldwide, with more than 2.2 million new cases every year. 7
Despite advancements in early detection methods, more effective treatments, and supportive care that have led to significantly improved patient survival rates,7,8 managing breast cancer remains complex.7,9 Furthermore, a breast cancer diagnosis profoundly affects patient's lives, making it essential to equip them with the right tools to manage their condition effectively. 10 As breast cancer treatments become more sophisticated, there is an increasing emphasis on a technology-driven, personalized approach to ensure optimal patient outcomes, cost-effectiveness, and improved quality of life. 5
From this context, there is an urgent need to provide both physicians and patients with digital solutions to navigate this scenario. Digital innovations represent a crucial bridge between current medical practices and a futuristic, patient-focused approach. Despite several digital tools being readily accessible to both patients and healthcare professionals, numerous applications and platforms will be designed to provide patients with critical information and personalized support during their unique journey. These resources will include real-time access to health data empowering patients to be active participants in their curative process. On the other hand, clinicians will be able to make informed decisions based on a synergy of data and advanced algorithms, ensuring a comprehensive integration of each patient's unique health profile. DTx tools, which are anchored in evidence-based software, and CDSSs, which offer immediate insight and recommendations derived from patient-specific data, have distinct roles. However, their combined effect highlights a transition from one-size-fits-all treatments to personalized approaches that prioritize overall well-being. Table 1 compares DTx and CDSSs by highlighting key aspects such as their primary purpose, method of intervention, regulatory requirements, target users, and their integration within healthcare systems or workflows. DTx tools are designed to directly manage, treat, or prevent medical conditions through patient-focused interventions, often requiring regulatory approval. By contrast, CDSSs assist healthcare professionals by providing decision-making support through patient-specific information and guidelines. Together, DTx and CDSS can be synergistic: DTx engages patients in managing their own health, while CDSS enhances clinical decision-making, allowing for a comprehensive approach to patient care.
Differences between digital therapeutics and clinical decision support system. Digital therapeutics are primarily therapeutic interventions, and clinical decision support system are decision aids for clinicians. Both leverage technology to enhance healthcare outcomes and play essential roles in the rapidly evolving landscape of digital health.

Through this review, we aim to delve into the nuances and complexities of DTx and CDSS and explicate their roles and potential in the evolving digital healthcare scenario in breast cancer.
Methods
We conducted a comprehensive literature search across three major medical databases, over the last decade, from 2014 to 2014. Our search strategy included keywords such as “digital health,” “digital therapeutics,” “clinical decision support system,” and “breast cancer”.
The initial search identified 557 papers from PubMed/MEDLINE, EMBASE, and Elsevier Scopus. After removing duplicates, screening for relevance to breast cancer and alignment with our research question, 31 articles were selected for inclusion in the review.
Digital therapeutics (DTx)
Role of DTx in breast cancer
DTx tools represent a separate category within digital medicine, which itself is part of the broader realm of digital health. These tools use digital means to treat, manage, or prevent diseases. Unlike traditional therapies that rely on drugs, DTx employs software and algorithms as its therapeutic agents. 6 Although both traditional medications and DTx often demand clinical validation and prescriptions, their developmental pathways, regulatory processes, and post-release management differ considerably. DTx development is generally faster and more cost-effective, requiring no further production costs once developed. Instead of navigating the complex drug distribution network, DTx directly reaches patients via digital platforms. A significant advantage of DTx is its minimal occurrence of adverse events, as it does not entail any medication toxicity.
DTx tools operate by facilitating a dynamic interaction between software and patients, thereby fostering patient engagement, which has been identified as a critical factor for achieving successful results. 6 This engagement has the potential to significantly impact patient behaviors and ultimately influence the outcomes. 9
Given their capacity to impact outcomes, DTx tools warrant evaluation as rigorous as that applied to traditional drugs. 6 Their journey from initial software development through clinical trials to post-marketing evaluations reflects the usual trajectory of conventional medicines. For this reason, regulatory authorities must evaluate their safety and advantages within clinical studies for approval. 12
Examples of DTx in breast cancer
Despite the majority of DTxs available today in medicine addressing psychiatric or neurological disorders, 13 their application in other medical domains, such as oncology, is increasing. The potential of DTx in the management of patients with breast cancer is promising and offers innovative approaches.9,12
DTxs in breast cancer management encompass both web-based and smartphone platforms. Kirsch et al. demonstrated that these digital tools significantly enhance patients’ education, reduce anxiety and depression, alleviate symptom burden, and aid in treatment decision-making. However, further research is needed to confirm these benefits across broader patient populations and evaluate the impact of digital health on healthcare resource utilization in breast cancer management. 14
Areas of intervention for DTx in breast cancer range the entire patient journey, from prevention to survivorship (Table 2).
Digital therapeutics tools in breast cancer. This table delineates the different application fields of digital therapeutics in breast cancer, highlighting their specific effects and providing illustrative examples for each domain. It offers an overview of how digital tools are revolutionizing various stages of breast cancer care, from prevention to survivorship.
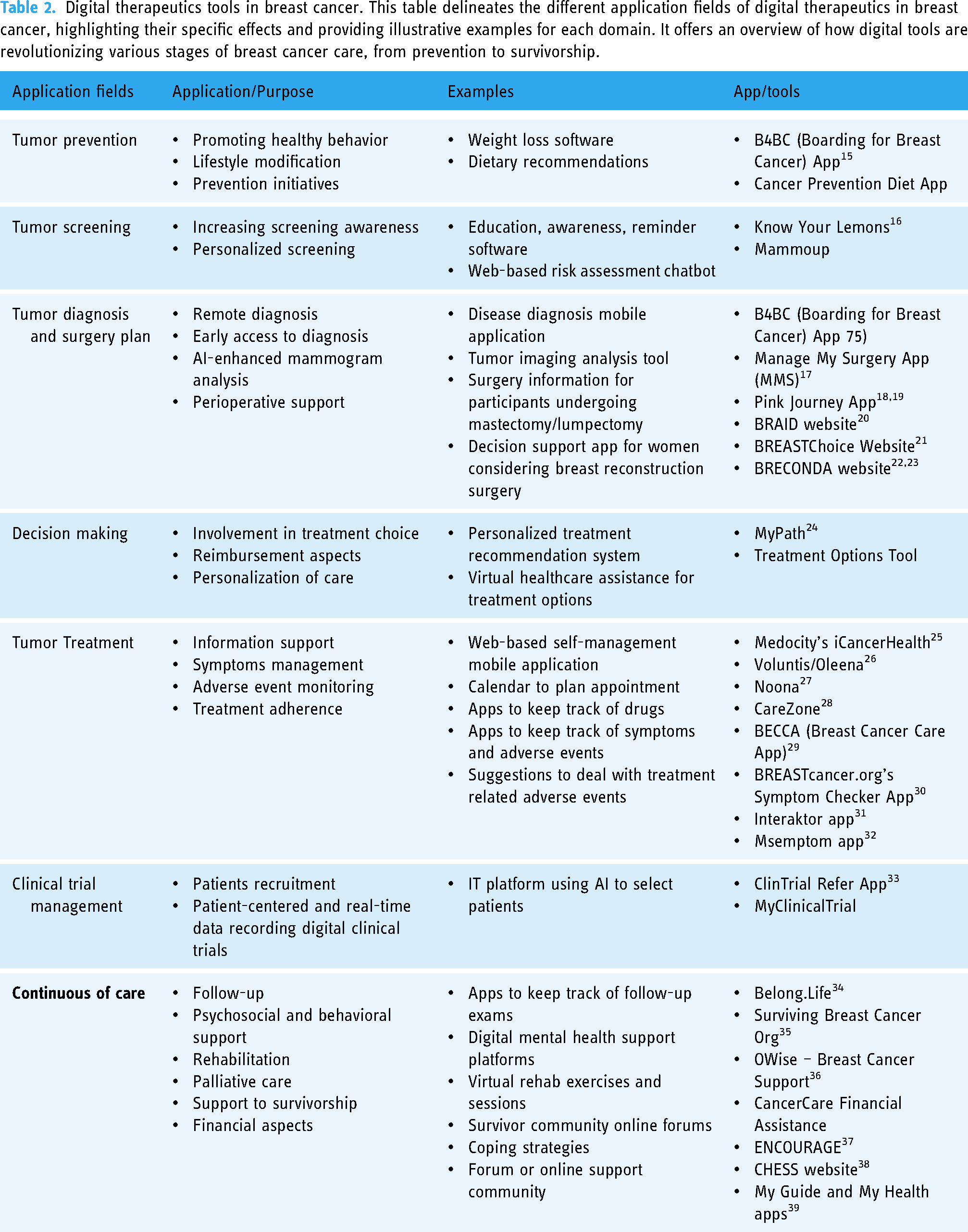
For tumor prevention, DTxs promote healthy behaviors and lifestyle modifications, such as apps focused on cancer-prevention diets. 15
In tumor screening, DTxs increase awareness among young women and provide personalized programs like the “Know Your Lemons” app, 16 promoting early intervention and comprehensive screenings. 40
Presurgery support is enhanced by mobile applications like “Manage My Surgery (MMS)”, 17 which aims to improve perioperative care for breast cancer surgery patients by providing educational content, facilitating communication, and collecting patient-reported outcomes. Evidence shows high patient satisfaction and preliminary improvements in anxiety, depression, and other health metrics.17,41 MMS is a user-friendly, free app accessible on multiple platforms, with plans for further studies to validate long-term outcomes and cost-effectiveness.
In treatment decision-making, apps such as “MyPath” 24 and “BECCA” 29 app from Breast Cancer Care provide valuable information, real-life stories, and practical advice for managing side effects and adjusting to life after treatment. These free apps feature an easy-to-use mobile interface designed to support patients throughout their treatment journey. Digital platforms may also ensure easy access to treatment, handle reimbursements, and offer personalized recommendations based on a patient's medical history, genetics, and preferences. 9
For clinical trial management, apps like "MyClinicalTrial” 33 developed in 2013 assist patients in finding suitable trials based on their disease characteristics. ClinTrial Refer is free to download and use, the app interface allows users to search for clinical trials, view key trial details, and contact trial locations directly. It has been recognized for increasing trial referrals and recruitment.
Throughout treatment, DTxs support patients by assessing the impact on daily life, managing symptoms and adverse events, and ensuring medication adherence. Beyond treatment, DTx fully supports follow-up care by providing psycho-social and behavioral assistance, facilitating rehabilitation, suggesting coping techniques, and extending support through chronic and palliative care stages to survivorship.42,43 For instance, Franzoi et al. implemented in 2023 a proactive survivorship care pathway that includes personalized care plans, education seminars, and a fee mobile app for personalized and self-management advice. 44 Evidence supporting its use includes high patient satisfaction rates and positive feedback on its usefulness. The app interface features functionalities for symptom measurement, educational content, supportive care information, and peer testimonials. Sella et al. developed the “Young, Empowered and Strong” (YES) web-based intervention to support young women with personalized education and symptom self-management resources. 45 The app was piloted in 2019 and is free to use. Evidence supporting its use includes high feasibility and acceptability, with participants reporting that it helped them learn, monitor, and manage their symptoms. The app interface includes features such as personalized symptom management content, educational resources, a journaling component, progress tracking, and secure messaging. 45
Patients undergoing breast cancer treatment often experience high levels of emotional distress, with studies showing that at least 38% suffer from depression and 32% report anxiety. 46 While psychosocial interventions have helped reduce these rates, it remains critical to find additional methods to manage the psychological burden of breast cancer.31,47 Educational resources through specialized apps and platforms may offer a promising solution, providing personalized support to help patients cope with their condition. 10
Apps like “Mika” have been shown to reduce distress, depression, anxiety, and fatigue through tailored psychosocial and self-management support. 48
Lifestyle interventions through DTx can improve symptoms, quality of life, and overall survival. A study in Iceland tested a DTx program that delivered education on mindfulness, sleep, stress, and nutrition, along with lifestyle coaching and daily missions for tracking physical activity and logging healthy food intake. The study found high engagement and acceptability, demonstrating the feasibility of multidisciplinary DTx for cancer patients. 49
Recent studies presented at ESMO 2023 highlighted the positive impact of digital interventions in breast cancer, emphasizing the potential for personalized, multifactorial digital solutions to enhance patient care. The DISCO trial explores the use of physical activity interventions administered via a web-based connected device for breast cancer patients. This multicenter, randomized, controlled study aims to dissect the individual contributions of different interventions on physical fitness, activity level, body composition, and quality of life, providing valuable insights for personalized patient interventions. 50 The IMPACT study, a prospective, randomized, controlled trial, evaluated the impact of a teaching tool (MOATT) on patients receiving oral treatments for advanced breast cancer. The study demonstrated a 40% reduction in the probability of treatment discontinuation when using MOATT compared to routine patient coaching. This emphasizes the effectiveness of multifactorial interventions in improving treatment adherence. 51 Additionally, the study on the Untire app, designed to help cancer patients manage fatigue, showed clinically significant reductions in fatigue levels and improvements in disease-related quality of life over a 12-week period. These results reinforce the potential of decentralized digital technologies to deliver meaningful improvements to patients. 52 While these findings are promising, integrating these diverse apps into a comprehensive care pathway remains a challenge. Issues of reimbursement, integration of electronic medical records, and patient care pathways must also be addressed. Personalized digital health technologies tailored to individual patient needs offer the potential for proactive patient care, reaching patients worldwide and potentially alleviating the burden on healthcare systems.
Summary of DTx application in breast cancer
To summarize, as digital health advances, DTx stands out as a decisive innovation in oncology. These tools represent more than just technological progress; they mark a transition to holistic, patient-focused cancer care, with various applications detailed below (Figure 1).
Awareness and prevention: DTx platforms offer invaluable education on cancer risks such as in breast cancer where apps guide users through correct self-examination methods and underscore the necessity of consistent screenings. By amplifying awareness and demystifying preventive methods, DTx serves as an essential link, fostering a proactive approach to health and underscoring the crucial role of early detection in fighting cancer.
53
Symptoms management: Cancer patients often face a multitude of symptoms, ranging from intense pain to constant fatigue. DTx tools offer solutions that enable real-time monitoring of these symptoms, providing immediate feedback and actionable insights. Through integrated platforms, patients can record their daily symptoms, which can be evaluated in relation to their treatment plan to provide proactive interventions. For instance, an app might guide a patient through pain management techniques or notify a medical team when side effects become dangerous. This approach not only improves the patient's overall well-being but also ensures the timely interception and management of any complications.
54
Adherence to treatment: The effectiveness of oncology treatments is largely dependent on strict adherence to prescribed regimens.
55
DTx tools measure compliance through timely reminders, interactive platforms, and personalized feedback that keep patients informed and committed to their treatment path.56,57 Psychological support: it is widely acknowledged that coping with cancer is an emotional and psychological challenge.
58
Anxiety, depression, or isolation are common among cancer patients, and traditional healthcare approaches often lack the resources to address them adequately.59,60 However, DTx may fill this gap with platforms offering cognitive-behavioral therapy sessions, meditation guides, and online support communities in order to teach how to manage their emotional needs, equipping them with resources to build resilience and find comfort even in difficult journeys. Lifestyle modifications: A holistic approach to cancer care often involves changes in lifestyle, from dietary modifications to incorporating physical activity.
58
DTx platforms are tailored to guide patients through these changes. Customized nutritional plans, fitness tracking tools, and resources that help address treatment-induced physical challenges can be integrated into daily life. DTx tools may assist patients with post-operative exercises and provide individualized dietary advice based on their treatment.61,62 Survivorship and rehabilitation: The completion of the treatment is a significant milestone, but the journey continues.
58
Survivors often face unique challenges, from addressing the long-term effects of treatment to managing the emotional landscape of survivorship. DTx tools designed for this phase are crucial.
44
They offer survivors tailored care plans, rehabilitation exercises, and resources that focus on both physical and emotional recovery. Additionally, these platforms can facilitate connection with other long survivor patients for mutual support and understanding.
63
Clinical cancer research trials: digital technology is going to reshape traditional clinical trials, making them more efficient, accessible, and inclusive.
64
Historically, these trials have been characterized by high costs, lengthy processes, and limited patient representation. Recent advancements, taking inspiration from other areas such as cardiology, have demonstrated the potential of DTx tools to streamline procedures and enhance data collection. These technologies can extend the reach of trials, overcoming geographical and demographic barriers and empowering patients with an active role in their care journey.
65
This shift promises to make clinical trials more patient-centered and widely representative, ultimately improving research outcomes and patient care.
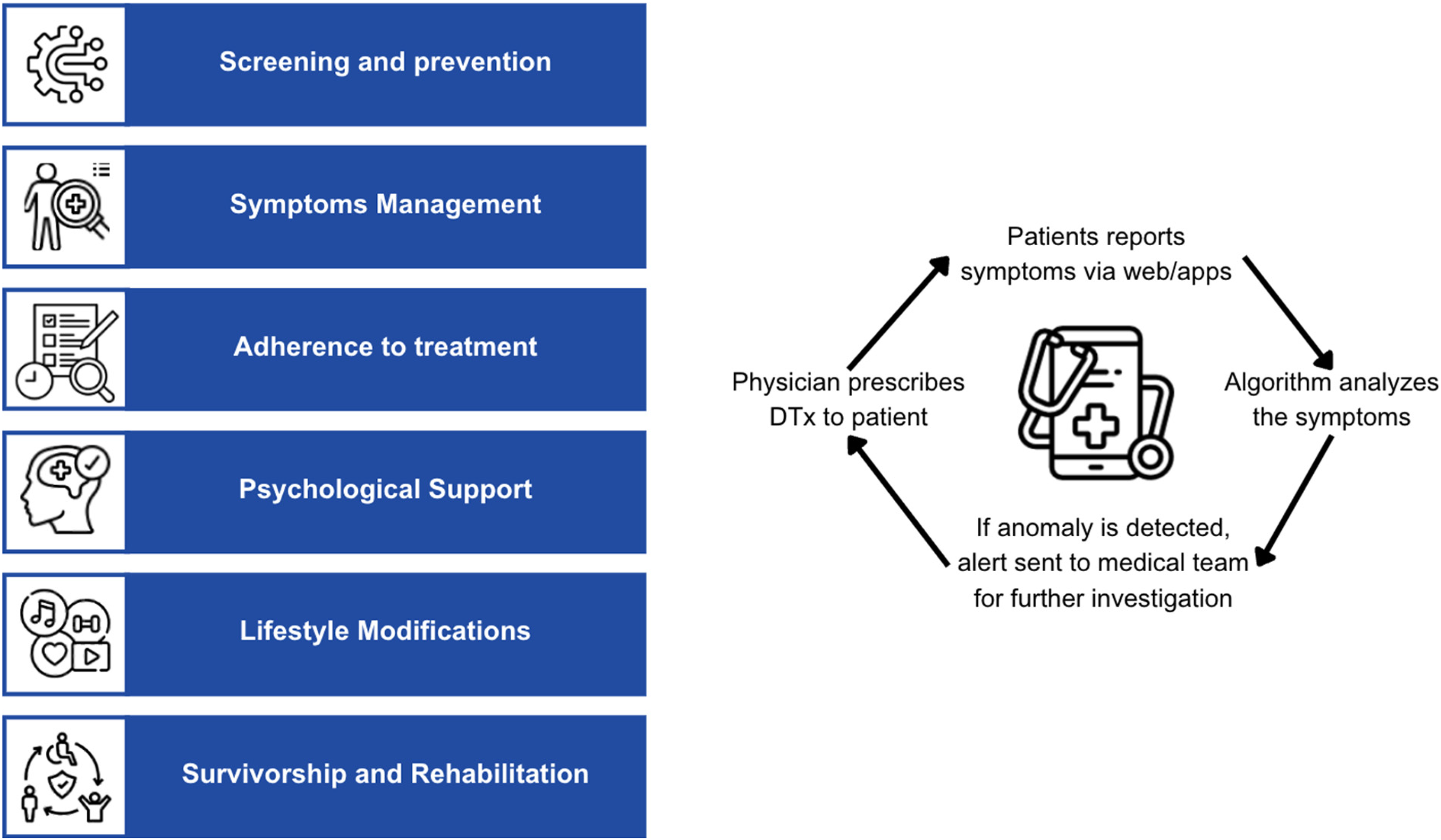
Digital therapeutics functioning and applications in oncology.
CDSS
Role of CDSS in breast cancer
CDSSs represent a transformative leap in medical practice, integrating cutting-edge technology with human expertise to enhance clinical decision-making and optimize patient care. 11 Their integration into clinical practice has been increasing over the past years, leading to improved healthcare services, quicker decision-making, and heightened patient well-being, while reducing healthcare costs and the likelihood of medical errors.66–68 Within oncology, CDSSs offer a multitude of benefits, such as safer drug prescriptions, streamlined testing processes, reduced clinician workloads, and easier access to evolving clinical evidence, contributing to better care and cost savings.66–71
Recent advances in precision oncology have expanded the repertoire of treatment options and driven the decision-making process. However, the diverse nature and application of CDSSs in breast cancer remain relatively underexplored with some critics arguing they often serve generic treatments rather than providing truly individualized approaches. 72
Examples of CDSS in breast cancer
A systematic review by Mazo et al. sheds light on the essential role of CDSS tools in breast cancer treatment decisions by analyzing 17 relevant research papers. 73 It underscores the CDSS’ diverse methodologies, from artificial intelligence to text mining techniques. Yet, the diverse methodologies, evolving validation datasets, and the constant need for updates pose challenges in standardizing and comparing CDSS. By enhancing patient safety, streamlining drug prescriptions and tests, and offering personalized therapeutic pathways, CDSSs enrich the decision-making process.73–76 They also reduce clinicians’ workload allowing more time for direct patient interaction, and ensure prompt application of the latest clinical findings, which is crucial for minimizing errors and enhancing patient experience. 70 Furthermore, by preventing redundant tests, diminishing adverse events, and promoting cost-effective generic alternatives, CDSSs contribute to healthcare cost savings. 71 Table 3 contains a comprehensive list of breast cancer-related CDSSs.
Clinical decision support systems in breast cancer. This table provides an overview of each CDSS's primary purpose and the clinical or pathological data they utilize, offering a comprehensive insight into the tools available.

Abbreviations: ALND: axillary lymph node dissection; BC: breast cancer; BCI: breast cancer index; BCRAT: Breast Cancer Risk Assessment Tool; BEFORE: Begin Exploring Fertility Options, Risks & Expectations; BMI: body mass index; BOADICEA: Breast and Ovarian Analysis of Disease Incidence and Carrier Estimation Algorithm; BRECONDA: Breast RECONstruction Decision Aid; CARG: Cancer and Aging Research Group; CDSS: Clinical Decision Support Systems; CGA: Comprehensive Geriatric Assessment; DCIS: ductal carcinoma in situ; DRFS: distant relapse-free survival; eBC: early breast cancer; EFS: event-free survival; ER: estrogen receptor; ET: endocrine therapy; HER2: human epidermal growth factor receptor 2; HR+: hormone receptor positive; HT: hormone therapy; LN: lymph node; MGI: molecular grade index; N+: node positive; NACT: neoadjuvant chemotherapy; OC: ovarian cancer; PgR: progesterone receptor; ROR: risk of recurrence; RS: Recurrence Score; SIOG: International Society of Geriatric Oncology; SLN: sentinel lymph node; SLNB: sentinel lymph node biopsy; START: Screening Tool to Alert to Right Treatment;
One major area of interest is breast cancer risk assessment. Tools such as BOADICEA 77 and BRACAPRO 78 are designed to calculate the risk of breast and ovarian cancer in women, taking into account factors like family and personal history, pathogenic variants, age of menarche, and other relevant health metrics. BOADICEA evaluates the probability of associated mutations in the BRCA1 or BRCA2 genes, incorporating comprehensive data on family history and other risk factors. 77 Similarly, BRACAPRO assesses the likelihood of these genetic mutations by considering familial patterns, including male breast cancer and dual diagnoses. 78
Another critical area is the prediction of breast cancer recurrence with tools such as Adjuvant! Online, 80 the Residual Cancer Burden Calculator, 81 and the CTS5 Calculator. 82 The Residual Cancer Burden Calculator, 81 developed by MD Anderson Cancer Center, assesses the extent of residual invasive carcinoma following neoadjuvant chemotherapy. Available since the early 2010s, this free tool features a user-friendly web interface where pathological data are input to calculate RCB scores, aiding in post-treatment evaluations. Its efficacy is supported by numerous studies validating its accuracy in predicting long-term outcomes. 81 The CTS5 Calculator focuses on estimating the risk of late distant recurrence after five years of endocrine treatment, considering factors such as age, nodal status, and tumor characteristics. 82 Developed in recent years, the CTS5 Calculator is accessible online for free. It features a straightforward interface where users input relevant clinical data to receive a risk assessment. Its reliability is backed by clinical evidence and research validating its prognostic capabilities. 82 Molecular data analysis and genomic tests form another essential category. Genomic tests like OncotypeDX, 89 Mammaprint, 90 and PREDICT 91 are instrumental in predicting recurrence and guiding treatment decisions. A notable example is a web application recently developed by Exact Sciences, designed to assist clinicians in navigating the reimbursement landscape for the OncotypeDX test in Italy. This tool exemplifies the practical application of CDSS in real-world settings, where factors such as tumor grading, size, nodal status, estrogen receptor levels, and Ki-67 proliferation index are used to determine eligibility for test reimbursement according to local regulations. By streamlining the decision process for prescribing the Oncotype test, this tool not only aids in personalizing patient care but also ensures adherence to regional healthcare policies, demonstrating the significant role CDSS plays in the intersection of clinical decision-making and health economics. 97
In the domain of treatment therapy and optimization, tools such as Breast Cancer Index (BCI)84,85 aid in identifying patients at risk for late distant recurrence after five years of endocrine therapy, using molecular gene expression and the HOXB13/IL17BR (H/I) index ratio to guide decisions about extending adjuvant therapy.
Finally, geriatric oncology tools are tailored to the unique needs of older adults with breast cancer, focusing on optimizing treatment and quality of life. The CARG (Cancer and Aging Research Group) 96 tool predicts the risk of chemotherapy toxicity in older adults, incorporating variables such as planned chemotherapy regimen, laboratory tests, and comorbidity presence. The Tyrer-Cuzick Model/IBIS assesses breast cancer risk considering personal and family history, including factors like age, age at menarche, and hormone therapy use.
Every year, several CDSS are introduced to personalize breast cancer treatment care. At ESMO Breast 2024, Jacobs et al. presented “RSC4All,” a Machine Learning (ML)-based tool designed to predict RSClin™ results. Developed by Exact Sciences, RSClin™ is a decision-support tool that combines genomic data from OncotypeDX with clinical-pathological information (such as age, tumor grade, and tumor size) to refine prognosis and guide treatment decisions for patients with hormone receptor-positive early breast cancer. Since RSClin is currently available only in the United States, RSC4All has been developed to estimate RSClin™ outcomes, showing promising validation results. 98 Similarly, Miglietta et al. introduced an Artificial Intelligence (AI) model predicting the switch from HER2-0 to HER2-low phenotype at relapse, with an accuracy of 74%. 99 These advancements reflect the continuous innovation in leveraging digital tools to improve breast cancer care, making treatments more personalized and accessible.
Summary of CDSS application in breast cancer
Some of the benefits and applications of CDSS in Oncology are listed below (Figure 2).
Personalized treatment recommendations: With the advent of genomics, oncologists can access granular insights into the unique genetic profiles of tumors. Using this genomic data and past patient records, CDSS can aid decision-making by suggesting individualized, genomic-driven treatment plans and expanding the range of treatment options.
100
Early detection and diagnosis: Advanced CDSS can alert doctors about minor changes in patient data, which might signal early stages of malignancies or recurrences. These quick, proactive insights can be crucial for timely interventions and better patient outcomes.
101
Data synthesis and analysis: Given the vast amounts of patient data, ranging from imaging results to laboratory reports, CDSS can aggregate and analyze this information, offering predictions on disease progression, treatment responses and potential complications.74,102 Moreover, a significant challenge in implementing CDSS in oncology is managing the huge amount of data, which risks cognitive overload for clinicians. Studies have shown that human decision-making accuracy drops substantially when faced with more than three variables, making it challenging to interpret complex data sets.
103
Although humans possess a unique ability for intuitive decision-making based on experience, the increasing complexity of precision medicine, characterized by its reliance on specific biomarkers for customized treatments, pushes these cognitive boundaries.
104
As oncology increasingly incorporates these biomarkers to forecast patient outcomes, the challenges of intricate treatment modalities and human cognitive constraints become more pronounced. With the advent of ML, the development of CDSS tools is expected to accelerate as it becomes easier to analyze big data and provide predictive tools for clinical practice. Integration with electronic health records (EHRs): Continuous integration of CDSS with EHRs ensures real-time data access and updating, which is crucial for accurate and up-to-date clinical recommendations.105,106 Enhancing multidisciplinary collaborations: Cancer care often involves multiple specialists. CDSS can merge diverse inputs from these experts, enabling collaboration and comprehensive treatment strategies. Drug interaction and toxicity alerts: Cancer treatment often involves a myriad of medications, each with its interactions and potential side effects. CDSS are vital in this landscape, offering instantaneous alerts regarding any harmful drug interactions.
107
Beyond just interactions, these systems can monitor and predict potential toxicities based on the chosen treatment regimens, helping to prevent severe side effects. Clinical trial matching: With thousands of clinical trials ongoing at any given time, CDSS can help match patients with suitable trials based on their cancer type, stage, genetic mutations, and other factors.65,108 This ensures that patients have access to novel treatments that are most aligned with their needs.

Clinical decision support system functioning and applications in oncology.
Challenges and considerations in implementing digital tools in oncology
The rise of digital solutions in oncology is undoubtedly promising. These technological advancements aim to streamline patient care, enhance treatment adherence, and facilitate more effective communication among care teams. However, as with any pioneering initiative, the integration of these digital tools in oncology comes with some challenges and considerations.12,109
Categorization and recognition
The world of digital health is vast, and a comprehensive categorization is essential. Each tool and application needs accurate classification to ensure it is correctly recognized and utilized for its therapeutic potential. 110 This recognition is pivotal, as it sets the stage for effective utilization, ensuring that each tool is leveraged to its utmost potential in patient care. Moreover, with a well-defined categorization, stakeholders can better differentiate between the various digital tools, appreciate their nuances, and make informed decisions in clinical.
Data privacy and security
With the proliferation of digital tools that handle sensitive patient information, the risk of data breaches increases. 111 Ensuring robust security protocols and transparency with patients regarding their data protection is crucial. Institutions and developers must work together to fortify digital infrastructures, ensuring that encryption methods are safe and access controls are stringent. Additionally, with the increasing sophistication of cyber threats, continuous vigilance, regular security audits, and prompt updates are essential to stay a step ahead and safeguard patient data comprehensively. Beyond the technical facets, educating patients about their data rights, the measures in place to protect them, and how their data aids in improving care can further solidify trust and foster a collaborative digital healthcare environment.
Generalization
Although many CDSS tools predominantly focus on survival predictions, their underlying datasets can sometimes be limiting. For instance, Adjuvant! Online tool predominantly relies on the Canadian population, potentially leading to biases. 80 Additionally, many tools are usually developed based on European or American populations, which may not be generalizable to all populations due to differences in genetic, environmental and lifestyle factors, such as those seen in Asiatic populations. Looking forward, it is essential for CDSS to evolve, incorporating factors like environmental metrics, lifestyle determinants and novel genomic evaluations. As oncology progresses, CDSS must keep pace with the ever-evolving complexities of breast cancer treatment.
Interoperability
As healthcare embraces a myriad of digital tools, from EHRs to specific diagnostic platforms, the exchange of information becomes crucial.112,113 Interoperability ensures that patient data flows smoothly across different platforms, giving care providers a comprehensive view of a patient's history and current status. 114 As healthcare becomes increasingly reliant on a multitude of digital tools, the potential pitfalls of systems that do not “speak” to each other become evident. Lack of standardization or incompatible designs can lead to isolated pockets of patient data, making it challenging to provide holistic and integrated care. Fragmented systems can result in redundant tests, missed diagnoses, or uncoordinated treatment plans, alongside increased administrative hassles for providers. To address this challenge, a solution might be the implementation of universal standards for data exchange. Ensuring that all stakeholders, from developers to healthcare institutions, adopt these standards can help overcome the barriers posed by fragmented systems. This will enhance the quality of patient care, facilitate smooth data flow, and promote a holistic, patient-centered approach in the digital healthcare landscape. 115
Equity and accessibility
There is a risk that digital solutions might accidentally create or widen disparities in care. 116 Indeed, not all patients have access to advanced digital tools or the necessary knowledge to use them, potentially leading to unequal care quality. The utilization of these tools is significantly influenced by factors such as socioeconomic status, geographical location, age, and education levels. 117 Moreover, language barriers or cultural differences might make certain tools less intuitive for some user groups, thus diminishing their efficacy. Additionally, there is a chance that as wealthier or tech-savvy patients share their feedback, developers may unconsciously tailor future versions towards these users, potentially excluding the needs of less represented groups. As digital healthcare evolves, it is imperative for all stakeholders to ensure widespread accessibility and offer the necessary training. An inclusive approach ensures that every patient, irrespective of their background, benefits equally from healthcare innovations.118,119
Commitment from physicians and care teams
For the effective integration of new digital tools in healthcare, physicians must be adequately trained and familiar with these new technologies. 110 For many healthcare professionals, the introduction of new digital instruments represents a significant shift from traditional practices. This change, though beneficial, can be met with hesitations. There is often a natural resistance to change, especially in a field as crucial and sensitive as healthcare. Clinicians might have reservations, wondering if these tools are as reliable as traditional methods. Ensuring that medical professionals are confident in using these innovations is vital to fully harness their potential in enhancing patient care.
“Digital fatigue” and user experience
In today's digital age, both clinicians and patients are overwhelmed with a myriad of apps, trackers, and platforms. Clinicians, often faced with a barrage of alerts, can experience “alert fatigue,” diminishing the effectiveness of these tools. Similarly, patients, when presented with an array of digital solutions, can feel overwhelmed and disengaged. Such digital overload can be counterproductive, leading to sporadic or incorrect usage. 114 Additionally, patient trust and acceptance of these digital tools can also be a significant challenge. Without trust and confidence in the efficacy and security of digital health solutions, patients may be hesitant to adopt them consistently. It is essential, then, to prioritize the development and selection of user-friendly, intuitive tools. 9 By simplifying interfaces and streamlining user interactions, consistent use and adherence can be more readily achieved, ensuring that the full benefits of these digital solutions are realized.
Regulatory hurdles
Digital solutions in the medical arena are not just about innovative technology; they also need to align with the stringent standards set by regulatory bodies to ensure safety, effectiveness, and reliability.9,12,114 Regulatory requirements are complex, covering aspects such as data privacy, clinical validity, interoperability standards, and user safety. 111 Furthermore, global compliance adds another layer of complexity as regulations might vary across regions and countries.
For instance, in the United States, the FDA regulates digital health tools under its Digital Health Innovation Action Plan, which includes guidelines for software as a medical device (SaMD). By contrast, the European Union follows the Medical Device Regulation (MDR) which sets stringent requirements for clinical evaluation and data security.
Although digital solutions hold transformative potential, there is a global call for clearer and more suitable regulatory systems for DTx. 120 A significant limitation in investigating the efficacy of digital health platforms is the absence of a formal regulatory process overseeing their development. Most studies rely on institutional protocols for content validity, making it challenging to generalize results across diverse patient demographics and cancer stages. 14
Economic considerations
Financing digital healthcare solutions is multi-faceted. The development, maintenance, and continuous updating of digital solutions require substantial funding. Balancing the economic aspects with the objective of broad accessibility and equity can be challenging. Moreover, due to the diverse economic dynamics and healthcare systems around the world, what is affordable in one region may not be in another. Hence, developers, policymakers, and stakeholders must deliberate thoroughly in order to balance cost considerations and the goal of equitable healthcare access.
Conclusion
The intersection of digital solutions and breast cancer represents a transformative era in oncology. This convergence is paving the progress for advancements, with the aim of improving patient outcomes and reshaping the framework of breast cancer care. The introduction of DTx tools and CDSS within the vast landscape of oncology offers innovative solutions ready to address critical issues in breast cancer management, spanning from prompt diagnosis to tailored treatment regimens. DTx holds the potential to provide real-time symptom management, improve adherence to treatment regimens, offer critical psychological support, and promote crucial lifestyle modifications. This marks a shift from traditional, compartmentalized treatment approaches to more comprehensive, integrated breast cancer care. Similarly, the strength of CDSS lies in their ability to leverage vast data sets, providing clinicians with actionable insights and personalized treatment recommendations and facilitating early detection—critical in situations where early interventions can significantly impact outcomes.
However, similar to any revolutionary transformation, some hurdles must be overcome. From ensuring data privacy and integrating diverse systems to achieving clinical validation and providing equity in access, the journey of incorporating digital solutions into breast cancer oncology is intricate. Moreover, since the digital landscape is continuously evolving, ensuring that digital solutions remain up-to-date, relevant, and in line with the latest research is an ongoing challenge. Through collaborative efforts among technologists, clinicians, and patients, strategies can be developed that not only tackle these challenges but also set the stage for a future where technology and healthcare merge harmoniously. Furthermore, while the potential of these digital tools is immense, conclusive evidence demonstrating their impact on patient outcomes and mortality is still lacking. Therefore, future research should focus on evaluating these tools comprehensively to determine their effectiveness and potential benefits in improving survival rates and overall patient outcomes.
In conclusion, as the healthcare landscape becomes increasingly digitized, digital tools are consolidating their role in breast cancer management. Their potential to personalize care, provide instant support, and empower patients is invaluable. Looking forward, we forsee a world where every breast cancer patient, regardless of their geographical location or socioeconomic background, has access to cutting-edge digital tools in order to facilitate timely and effective treatment and to empower patients and caregivers from mere passive recipients to engaged active participants in their healthcare journey.
Footnotes
Acknowledgments
Supported by Pfizer grant for Innovative Digital Health Projects in Oncology as a part of the ongoing project Generative Adversarial Networks (GANs) for Synthetic Data in Breast Cancer (protocol identifying number ONC/OSS-08/2022, version 1.0, 27 October 2022). European Union—Horizon 2020/2023 program (GenoMed4All project #101017549 to M.G.D.P.; S.D.; Synthema Project, #1101095530 to M.G.D.P.; S.D.); AIRC Foundation (Associazione Italiana per la Ricerca contro il Cancro, Milan, Italy—Project #22053 to M.G.D.P.).
Contributorship
Conception and design: all authors
Research and review of the literature: FJ, SD, EZ, MG, CB, GS, RG, DG, AL.
Data analysis and interpretation: FJ, SD, EZ, MG, CB, GS, RG, DG, AL.
Manuscript writing: all authors
Final approval of manuscript: all authors
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
The study is a review of the literature and did not require research ethics approval or patient consent.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Guarantor
Rita De Sanctis
