Abstract
Background
Gestational diabetes mellitus (GDM) can increase the risk of adverse outcomes for both mothers and infants. Preventive interventions can effectively assist pregnant women suffering from GDM. At present, pregnant women are unaware of the importance of preventing GDM, and they possess a low level of self-management ability. Recently, mHealth technology has been used worldwide. Therefore, developing a mobile health app for GDM prevention could potentially help pregnant women reduce the risk of GDM.
Objective
To design and develop a mobile application, evaluate its acceptance, and understand the users’using experience and suggestions, thus providing a valid tool to assist pregnant women at risk of GDM in enhancing their self-management ability and preventing GDM.
Methods
An evidence-based GDM prevent app (Better pregnancy) was developed using user-centered design methods, following the health belief model, and incorporating GDM risk prediction. A convenient sampling method was employed from June to August 2022 to select 102 pregnant women at risk of GDM for the pilot study. After a week, the app's acceptability was evaluated using an application acceptance questionnaire, and we updated the app based on the feedback from the women. We used SPSS 26.0 for data analysis.
Results
The application offers various functionalities, including GDM risk prediction, health management plan, behavior management, health information, personalized guidance and consultation, peer support, family support, and other functions. In total, 102 pregnant women consented to participate in the study, achieving a retention rate of 98%; however, 2% (n = 2) withdrew. The Better pregnancy app's average acceptability score is 4.07 out of 5. Additionally, participants offered several suggestions aimed at enhancing the application.
Conclusions
The Better pregnancy app developed in this study can serve as an auxiliary management tool for the prevention of GDM, providing a foundation for subsequent randomized controlled trials.
Keywords
Background
Gestational diabetes mellitus (GDM) refers to the initial occurrence or detection of abnormal glucose tolerance during pregnancy, resulting from hormonal influences. It is recognized as one of the most common complications of pregnancy. 1 Currently, the global average incidence for GDM stands at 14.2%, with Southeast Asia experiencing a higher incidence rate of 20.8%. 2 In China, the prevalence of GDM has reached an alarming rate of 21%. 3 With the adjusted fertility policies and the changes in lifestyle, more pregnant women experience advanced maternal age or are overweight, and this has led to a consistent increase in the incidence of GDM. 4 GDM has various short-term and long-term risks to pregnant women and their offspring. Hyperglycemia during pregnancy can result in complications such as miscarriage, pregnancy-induced hypertension, polyhydramnios, preterm delivery, and cesarean section.4,5 Furthermore, the offspring of mothers with GDM are more likely to be a macrosomia, experience neonatal hypoglycemia, and pathological jaundice.6,7 Additionally, studies have also demonstrated significantly increased risks of developing type 2 diabetes and cardiovascular disease in women with GDM within 5–10 years postpartum, while their children are more prone to developing overweight or obesity.8–11 Therefore, prioritizing prevention strategies for GDM is crucial.
GDM-related guidelines in many countries and regions recommend early screening and lifestyle intervention for pregnant women at risk of GDM. This can effectively prevent the occurrence of GDM, and reduce complications for both mothers and infants.12–14 In China, a fasting blood glucose test is typically conducted during the initial prenatal check-up for pregnant women, and regular monthly follow-ups are conducted before 24 weeks of pregnancy. An oral glucose tolerance test is performed at 24–28 weeks to screen for GDM. At present, healthcare providers (HCPs) primarily rely on experience to identify the risks for pregnant women and provide health guidance during the first trimester. 15 The main intervention methods include face-to-face guidance and group education. 15 Despite the proven benefits of traditional interventions in encouraging self-care among pregnant women and reducing the risk of perinatal complications, significant hurdles remain in effectively preventing GDM. 16 For example, the HCPs are unable to accurately identify women at risk of GDM accurately, and it is difficult to provide real-time monitoring and guidance for the pregnant women's diet and activity levels, thus affecting the effectiveness of these interventions. Therefore, it is necessary to develop a scientific and effective intelligent tool to assist HCPs in identifying pregnant women at risk of GDM, and to assist pregnant women in developing a healthful lifestyle to prevent GDM.
Mobile Health (mHealth) refers to the medical and public health services provided through smartphones, wearable monitors, personal digital assistants, and other wireless devices. 17 mHealth facilitates a connection between HCPs and users, enabling them to monitor patients’ health or illness status. Additionally, it meets patients’ needs for self-management support, enhancing medication adherence and reducing self-management behavioral barriers. 18 Moreover, mHealth services save users time and transportation costs, alleviate the burden on hospitals and community health service institutions, and maximize the effectiveness of limited medical resources. 19 mHealth applications (mHealth apps) are the primary form of mobile health management, utilize smartphones, tablets, and other mobile devices as terminals, supported by mobile internet technology. These applications serve as a health service platform for patients and HCPs. 20 With their unique biofeedback function, mHealth apps enable real-time health assessment and provide feedback on patients’ health status. This promotes personalized and accurate health management by HCPs and holds a promising application prospect. 20
Studies have shown that mobile phone apps are extensively used for managing GDM; they effectively reduce glycated hemoglobin, fasting blood glucose, and postprandial blood glucose levels, while also improving patients’ self-management abilities.21–23 Therefore, we hypothesized that mobile phone apps may offer potential benefits for GDM prevention. However, there is a lack of apps specifically developed for GDM prevention. The aim of our research was to design and develop an app for GDM prevention, evaluate users’ acceptance, learn users’ using experience and suggestions to further improve the app, and provide a valid tool to assist pregnant women at risk of GDM in improving self-management abilities.
Materials and methods
Theoretical framework
In this study, we used the health belief model (HBM) to guide the app's development. 24 This theory emphasizes the dominant role of perception in the formation and maintenance of health behaviors, including (1) perceived susceptibility: an individual's perception of the likelihood of developing a health problem; (2) perceived severity: an individual's perception of the degree of harm caused by an unhealthy behavior or disease; (3) perceived behavioral benefits: the benefits of an individual's subjective judgment after adopting healthy behaviors; (4) perceived behavioral barriers: the obstacles that individuals face in subjectively judging the adoption of healthy behaviors; (5) self-efficacy: the ability of an individual to act effectively to produce a desired result. This study incorporates the HBM as a framework, integrating different components to construct the initial module. The strategies for implementing the HBM in Better pregnancy are detailed in Table 1.
The implementation strategy of the health belief model for Better pregnancy.

Study design and setting
This is a clinical feasibility study, aiming to investigate the acceptability of Better pregnancy among women at risk of GDM after using the app for one week. We collected pregnant women at risk of GDM from the Obstetrics and Gynecology Clinic of Beijing Friendship Hospital,Capital Medical University from June to August 2022. All pregnant women received standard antenatal care, including routine antenatal visits, handout brochures, and routine blood tests.
Sample
As this is a clinical feasibility study, we used a convenient sampling method to select pregnant women at risk of GDM. From June to August 2022, there were 673 pregnant women registered in the Obstetrics and Gynecology Outpatient Department of Beijing Friendship Hospital, 195 pregnant women were at risk of GDM, 88 pregnant women who used Apple mobile phones, 2 pregnant women's gestation weeks were more than 12 weeks, and 3 pregnant women did not want to participate in the study. A total of 102 pregnant women were selected for this study, and 100 women completed the survey in the end. The flowchart diagram is shown in Figure 1.

Flow chart of participants’ inclusion.
The inclusion criteria are as follows:
Chinese-speaking women who are ≥18 years old; Gestational age ≤12 weeks; Pregnant women with any of the risk factors for GDM, including age ≥35 years old; overweight or obese (body mass index (BMI) ≥ 24 kg/m2); history of diabetes; history of GDM; history of macrosomia; polycystic ovarian syndrome; adverse pregnancy history or impaired glucose tolerance. Because we have just developed the iOS version, we enrolled women whose mobile phones are iOS versions. We excluded multiple gestations. This is because there are differences in nutrition, exercise, and weight gain requirements between pregnant women with single and multiple gestations. Also, the lifestyle intervention strategy in the app we developed is only for single pregnant women; Women who have had severe cardiopulmonary dysfunction pre-pregnancy; Women with cognitive and mental disorders.
The exclusion criteria are as follows:
Procedures
Phase 1: development of the Better pregnancy
The aim of the app developed in our study was to accurately identify the women at risk of GDM, and carry out lifestyle interventions such as diet, exercise, and weight control, to improve the self-management ability, self-efficacy, and the level of social support of pregnant women, thereby effectively preventing GDM. The app development followed the four stages: analysis, design, development, and evaluation. 25 The development processes of Better pregnancy are illustrated in Figure 2.
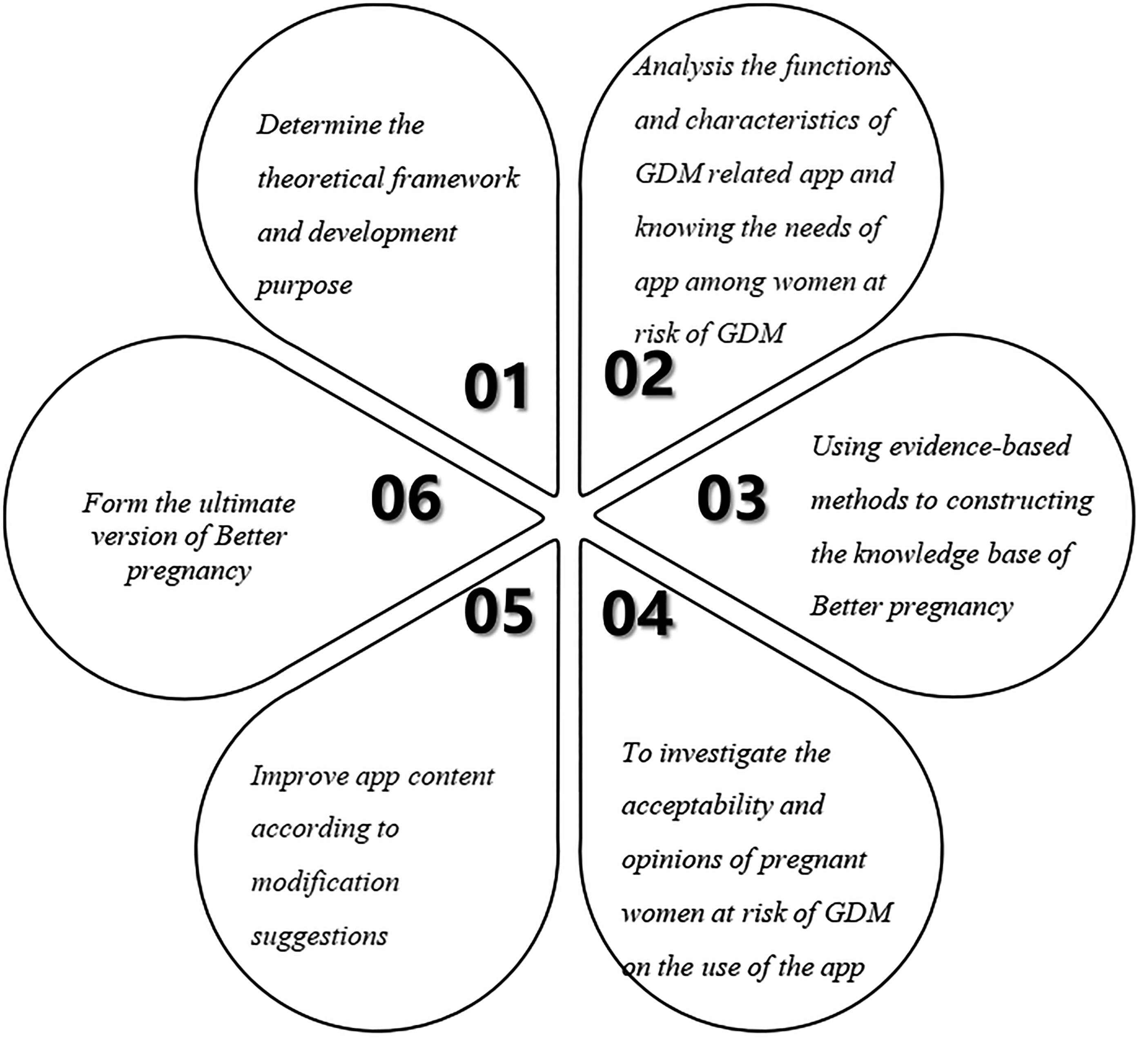
Development process of the Better pregnancy.
Analysis of the functions and characteristics of GDM-related apps
We searched the mobile application market and literature database using the keywords of “gestational diabetes mellitus,” “diabetes in pregnancy,” “GDM,” and “app” to identify GDM-related apps. By analyzing the functions and features of these apps, we gained insight into the current development status and functionality of these apps. This helps us understand the importance of developing apps specifically for preventing gestational diabetes. A total of 13 apps related to gestational diabetes health management were finally included, 3 in the application market and 10 in academic articles. Four were Chinese apps and nine were English apps.21,22,26–33 However, there was no app specifically for gestational diabetes prevention. The extracted functional analysis results are shown in Supplementary File 1. After analyzing the functions of the GDM-related apps, we conducted a group discussion to preliminarily determine the functional framework of the app.
Needs and functions analysis of mobile health app for women at risk of GDM
To further comprehend the demand for the developing Better pregnancy app among pregnant women at risk of GDM in early pregnancy, from August to September 2021, we conducted semi-structured in-depth interviews with women in their first trimester of pregnancy who had scheduled appointments at Beijing Friendship Hospital, Capital Medical University in China to understand their needs for using a mobile health management app and to further refine the app's functions. For the detailed interview outline, refer to Supplementary File 2.
The part of demand analysis of mobile health intervention for pregnant women at risk of GDM was finally included 15 women with GDM risk factors in early pregnancy for interview, with an average age of (32.33 ± 3.56) years old. There were three themes and 14 sub-themes, including main functional requirements (personalized recipe customization and diet replacement, suitable exercise and auxiliary monitoring, weight control and monitoring record, biofeedback), secondary functional requirements (accurate recommendation information, short video and recording, convenient professional support, reasonable reminder, peer support, mother and child auxiliary function, convenient recording, and individual points reward system), and clear interface logic. Based on the interview results, we made further improvements to the initially determined app functions, including adding a BMI calculation tool, displaying gestational age, and changing the live broadcast to short videos.
Constructing GDM prevention knowledge database using evidence-based methods
To ensure the contents pushed by the app are scientific and accurate, we constructed the evidence items using evidence-based methods, and stored it in the back end of the nurse terminal as the knowledge base for GDM prevention. Based on the methodological evaluation results (Supplementary Files 3–6), the content is modified to align with users’ lifestyle preferences, to provide personalized health information. We systematically searched the databases in both Chinese and English for the health management information for women at risk of GDM from June 2015 to June 2022. Evidence-based information was synthesized from high-quality articles. The Australian JBI evidence pre-classification and recommendation level system was used to assess the extracted evidence and provide recommendations. 34 We included 22 guidelines and reviewed the literature,12–14,35–53 and extracted 17 evidence items, involing four aspects, early screening, diet guidance, exercise guidance, and weight management guidance. The evaluation results and evidence are detailed in Supplementary File 7.
APP development
Then we set up a software development team, including two researchers, two senior software engineers (responsible for software functional architecture design and development, operation, and maintenance testing), and a professional User Interface (UI) designer (responsible for app UI design and Admin system UI design). Researchers made application development plans according to the subject and communicated with team members about existing problems promptly. The UI designer of the software development team used Photoshop to design the user interface, and the software engineers were responsible for the software development. PlantUml software was used to draw the use case diagram and data flow diagram, v9p diagram, and MySQL 8.1 was used as the database to deploy the test and production environment on Huawei Cloud. Java was used as the programming language to develop the application with Android development tools. Two researchers conducted preliminary trials on different types of mobile phones with the iOS system. The final version was determined through repeated iterations and tests of the application.
Mobile health system introduction
The app includes the user's terminal, family terminal, medical and nursing terminal, and website back-end management terminal, including GDM risk prediction and assessment, health management plan, behavior management, health information, interactive platform, personalized guidance and consultation, peer support, family support, platform management, account management, and other functions. Figure 3 shows the screenshots of the functions, including (1) sign-in interface; (2) homepage interface; (3) risk prediction interface (partial data). The core aspects of the app features are shown in Table 2.

The screenshot of the Better pregnancy app.
Introduction of Better pregnancy functions.

Phase 2: evaluation phase
We contacted the head nurse at the Department of Obstetrics and Gynecology of Beijing Friendship Hospital and obtained her permission. Then, the researcher (Beibei D) reviewed the pregnant women's appointment information from the hospital's outpatient electronic medical record system, identified potential participants who met the criteria, and conducted a face-to-face assessment of the eligible subjects on the day of the pregnant women's appointment.
At the time of enrollment, the HCPs informed the participants of the purpose and method of the study, obtained their written informed consent, recorded the names, risk factors, telephone numbers, etc., and personally added the pregnant women as WeChat friends to ensure the distribution of follow-up electronic questionnaires. Pregnant women downloaded the GDM prevention management app by scanning the QR codes and registered a personal account, and the nurses taught them how to use the app's features.
Data collection
A total of 102 questionnaires were distributed, and 100 were collected. Two of the participants did not respond to our research, one of them was immobile with threatened preterm labor and did not use the app, and the other one was transferred to another hospital and did not finish the questionnaire, with an effective response rate of 98%. At the time of enrollment, participants’ names, risk factors, and phone numbers were recorded. After pregnant women had been using the Better pregnancy app for a week, the link to the acceptance evaluation questionnaire was sent using the “Wenjuanxing” online survey platform to collect general information and acceptance of pregnant women at risk of GDM. We have set required fields and time limits, and one ID number can only be submitted once. After the study, we gave the pregnant women a small token of appreciation to thank the participants.
Data analysis
SPSS version 26.0 was used for statistical analysis. The continuous measurement data were tested for normal distribution. The normally distributed data were expressed as mean (M) ± standard deviation (SD), the data with non-normal distribution were expressed as median (MD) and inter-quartile range (IQR), and the count data were described by frequency and percentage.
Outcome measurement
We assessed the acceptance of the Better pregnancy among women at risk of GDM by using the Mobile Health Application Acceptance Questionnaire. Firstly, a socio-demographic data questionnaire for participants was designed, including women's identification numbers, age, weight, nationality, education level, religious affiliation, insurance coverage, employment status, number of pregnancies, number of children, history of adverse pregnancy, thyroid disease, polycystic ovarian syndrome, family history of diabetes, history of gestational diabetes, and history of macrosomia.
Secondly, a Mobile Health Application Acceptance Questionnaire was used to survey participants’ acceptance of the Better pregnancy. This questionnaire was developed by Chen and Han, 54 including 6 dimensions and 32 items: accessibility, usability, interface design, reliability, user attitude, and user tendency. Items were scored using a 5-point Likert scale, ranging from 1 (strongly disagree) to 5 (strongly agree). The maximum total score was 160. A higher score indicates greater acceptance of the application. We used the questionnaire results from the first 20 pregnant women to assess the reliability and validity of the questionnaire. The content validity index of the questionnaire was 0.97, with a Cronbach's α coefficient of 0.964. The app demonstrated good reliability and validity. Finally, we utilized open-ended survey questions to identify the issues that participants encountered while using the app.
Ethical consideration
This study was approved by the Ethics Committee of Capital Medical University (Z2019SY037) and Beijing Friendship Hospital affiliated to Capital Medical University (2019-P2-204-02). Before enrollment, the researcher explained the purpose and methods of the study to the pregnant women and their families, obtained their consent and signed the written informed consent. We assured that all data would be used solely for clinical research and that the information would be kept confidential.
Results
Socio-demographic information of women at risk of GDM
A total of 100 pregnant women participated in the app trial and completed the questionnaires. The retention rate after the trial was 98%. Out of 100 pregnant women, 41% were aged 35 or older, 32% of the participants showed overweight or obesity in BMI before pregnancy, 89% held a college degree or higher, and the proportion of a family history of diabetes, a history of GDM, and macrosomia were 24%, 12%, and 8% respectively. The socio-demographic information is presented in Table 3.
Socio-demographic characteristics of women at risk of GDM (n = 100).

Acceptability of Better pregnancy among women at risk of GDM
Pregnant women at risk of GDM had scores of about 4.0 points in each dimension of acceptance of the app, and the total score of acceptance was mean (SD) 128.87 (16.70) points, indicating that the app had a good acceptance (see Table 4).
Acceptance scores of the app among pregnant women at risk of GDM (n = 100).

Recommendations of Better pregnancy for women at risk of GDM
A total of 8 suggestions put forward by pregnant women were compiled, and 6 suggestions on diet, weight, blood sugar, as well as two other aspects were summarized. The specific contents are presented in Table 5.
Recommendations for pregnant women following the trial of Better pregnancy.

Discussion
Principal findings
Currently, there are relatively few gestational diabetes health management apps, and there is currently no app specifically for GDM prevention. Thus, our aim was to develop an app by integrating risk prediction and risk management of GDM to help pregnant women at risk of GDM in preventing GDM. We also assessed the app's acceptability among 100 pregnant women identified as being at risk of GDM. The app developed in this study serves as a tool for GDM prevention, can improve their awareness of GDM prevention, and assist them in setting personalized management goals. The app can also offer multi-dimensional social support, including peer, family, and professional support, for monitoring the implementation of maternal health management. This approach can inform the development of other health-related apps. Following a trial with pregnant women, the study demonstrated that the app was well-received, and we received positive feedback from participants, offering valuable insights for app optimization.
Compared to other studies
Previous studies have shown that mobile health interventions supported by theory can assist medical professionals in developing targeted measures to address patient behavior change mechanisms. 55 Chen et al. 56 and Kaveh et al. 57 indicated that many mobile medical apps in the health field currently lack theoretical guidance, resulting in varying quality. Cho et al. 58 revealed that only five of 14 mhealth studies incorporated behavior change theory. To address this gap, we adopted the HBM as a theoretical framework. HBM is a classical model for individual health behavior change. Based on the HBM, our study designed the risk prediction module and guided pregnant women to make behavior changes, to improve risk awareness and risk management capabilities, and better help them preventing GDM. In our study, users of our app are primarily pregnant women at risk of GDM, because our main aim is to prevent GDM rather than treat it. Al Hashmi et al. 32 also developed an app for GDM health management based on the HBM, utilized by women diagnosed with GDM. It focused on strategies to enhance self-efficacy, conducted a 4-week trial with 15 women with GDM and demonstrated good acceptance.
Evidence-based intervention strategies are more scientifically grounded. Health information in many applications is sourced from expert groups, and the majority of information draws on specialists’ experience, which may introduce some subjectivity.59,60 In our study, we thoroughly examined existing guidelines, systematic reviews, as well as relevant literature on GDM prevention. We extracted the most reliable evidence to create a knowledge base for GDM prevention management, providing evidence-based health management plans for pregnant women. Additionally, HCPs can tailor the intervention plan considering the risk factors, weight, lifestyle, and preferences of pregnant women. This facilitates the development of personalized prevention goals and strategies, tailoring intervention plans to individual needs. The app delivers health information through graphics and videos, covering topics including the disease's dangers, behavioral benefits, barriers to behavioral change, and self-efficacy. This information helps pregnant women understand the risks associated with gestational diabetes and the advantages of making behavioral changes. Furthermore, the app in our study provides support and guidance from medical professionals and peer pregnant women, enabling users to overcome challenges and boost their self-confidence, thereby helping to prevent gestational diabetes.
Acceptance, alternatively termed as subjective satisfaction, primarily reflects the user's satisfaction and acceptance of the product. It can also indicate the user's inclination to use the product. 61 This study revealed that women at risk of GDM had a higher acceptance of the app, as indicated by a total score of (128.87 ± 16.70), which exceeds the acceptance score of (72.47 ± 7.77) reported by Chen and Han 54 for elderly individuals using apps. The disparity may be due to the relatively young demographic in this study, the majority (89%) possessing a college degree or higher, and their readiness to embrace new technologies, particularly electronic products. Varnfield et al. 29 conducted the questionnaire survey to assess the acceptance of the M♡THer app among 23 GDM pregnant women, indicating that the app could monitor blood glucose levels, demonstrating easy of use and convenience. Al Hashmi et al. 32 also reported that all nine participants in the trial evaluation found the app useful and expressed they were satisfied. The interface dimension and usage tendency of the system received higher scores, suggesting a clear functional layout and the pregnant women's readiness to engage with the app. Nonetheless, the usability score was comparatively low, potentially due to the constrained research budget for app development, requiring manual recording of weight, blood sugar, and exercise data. In the future, pairing smartphones with fitness trackers and smart scales via Bluetooth could automatically log daily activity and weight data of pregnant women, minimizing the hassle of manual entry.
Strengths and limitations
The development of Better pregnancy adhered strictly to the steps of app development and incorporated all constructive and adverse feedback from users on the final version of the prototype. It is grounded on the HBM as the framework and relies on evidence-based evidence for preventive intervention in GDM among pregnant women. In line with the user-centered design concept, 62 the GDM risk prediction model from our previous research was utilized. Consequently, the research exhibits a high degree of rigor and scientific validity.
However, this study has some limitations. Firstly, we only interviewed pregnant women from a tertiary hospital in Beijing, which limited the sample sources. Secondly, we conducted only a preliminary assessment of the app's acceptance, and the app's usability and effectiveness should be further evaluated by a broader population. Lastly, we solicited only suggestions and opinions from participants regarding app improvements via open-ended questions, thus not fully exploring the user experience of the participants. In the future, we can conduct additional semi-structured interviews to gain a comprehensive understanding of users’ experiences with the app.
Conclusion
This study designed and developed an evidence-based app for GDM prevention, following a user-centered design approach and the standard app development steps. The app exhibits high acceptability. In the future, further evaluations will establish the app's effectiveness in preventing gestational diabetes, examine user experience, and assess the health economic implications of its use.
Supplemental Material
sj-docx-1-dhj-10.1177_20552076241266056 - Supplemental material for Development and acceptability of a gestational diabetes mellitus prevention system (Better pregnancy) based on a user-centered approach: A clinical feasibility study
Supplemental material, sj-docx-1-dhj-10.1177_20552076241266056 for Development and acceptability of a gestational diabetes mellitus prevention system (Better pregnancy) based on a user-centered approach: A clinical feasibility study by Beibei Duan, Zheyi Zhou, Mengdi Liu, Zhe Liu, Qianghuizi Zhang, Leyang Liu, Cunhao Ma, Baohua Gou and Weiwei Liu in DIGITAL HEALTH
Footnotes
Acknowledgments
We would like to thank the pregnant women who participated and supported our study.
Contributorship
Weiwei Liu designed the study, revised the manuscript, and guided the whole research; Beibei Duan and Weiwei Liu drafted the thesis; Beibei Duan, Cunhao Ma, Mengdi Liu, and Zhe Liu conducted the recruitment and data analysis of pregnant women. Zheyi Zhou translated and polished the article. All authors reviewed the draft and agreed to the final version of the paper.
Data availability statement
All data generated or analyzed during this study are included in this published article and its supplementary information files.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
This study was approved by the Hospital Ethics Committee of Capital Medical University (REC number: Z2019SY037) and Beijing Friendship Hospital, Capital Medical University (REC number: 2019-P2-204-02).
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the National Natural Science Foundation of China (grant number 71904133).
Guarantor
WL.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
