Abstract
Objective
Training in video consultations is seldom included in the curriculum for future physicians. Exploration of preferred teaching methods and learning objectives in this context among medical students remains limited. This study addresses this research gap by conducting a survey among medical students in Germany to assess their educational requirements concerning video consultations and patient-centred distance learning.
Methods
This quantitative study employed an online questionnaire designed for German medical students, following the guidelines of the International Association for Health Professions Education. The study primarily focused on discerning the didactic preferences related to patient-centred digital teaching regarding family medical video consultations. We provided a detailed explanation of a concrete learning concept, a family medical synchronous distance learning seminar. Subsequently, we surveyed students to gauge their needs, expectations, and evaluations of this concept. The collected data were subjected to descriptive analysis.
Results
The analysis revealed that students aspire to offer video consulting services to their patients in the future (sample size (n) = 369, median (med) = 68 of 101 Likert scale points, interquartile range (IQR) = 53.75), despite having limited knowledge in this area (n = 353, med = 21, IQR = 33.25). To acquire expertise in telehealth, students favor blended learning models (n = 331, med = 76, IQR = 50). They also recognize the benefits of distance learning, particularly for students with family responsibilities or those who must travel long distances to their learning institutions,. The presented distance seminar concept resonated with them (n = 278, med = 72.5, IQR = 50.5), surpassing five other digital learning models in preference. Furthermore, they expressed a desire for its continued implementation beyond the Coronavirus SARS-CoV-2 pandemic (n = 188, med = 77.5, IQR = 44.75).
Conclusions
The deficiency in medical school education regarding video consultations requires attention. This issue could be resolved by integrating one of the five distance learning concepts outlined in this article.
Introduction
Video consultations are a vital component of telemedical patient care, and their international use has significantly increased, especially since the onset of the Coronavirus SARS-CoV-2 (COVID-19) pandemic.1–5 They offer various benefits to patients,6,7 and are anticipated to enhance patient care.5,8–10 Additionally, video consultations are actively promoted by various institutions.11–13
The COVID-19 pandemic not only accelerated the adoption of video consultations in healthcare but also prompted a digital transformation in medical education. The sudden need for social distancing led to emergency remote teaching, although its quality was often suboptimal.14–16 However, many aspects of digital education persisted and proved effective even after the pandemic-related restrictions were eased,17–19 presenting an opportunity for a more scientifically grounded educational system.20,21 This extends to the integration of telemedicine learning objectives into medical school curricula.22–24 Until now, medical students have acquired digital competencies for video consultations inconsistently, often in a fragmented manner or not at all,25–31 despite the acknowledgment of the utility of teaching about video consultations by both students and political committees.27,29,32–35
One avenue to develop these competencies is through digital learning, which encompasses various modes of teaching using information and communication technologies to connect students and educators who are physically separated. 20 Digital learning offers students flexibility in terms of location and time, fostering deeper information processing. On the other hand, blended learning, combining traditional in-person interaction with digital elements, caters to students with diverse learning styles. 20 The flexibility of digital education arises from various modalities, including synchronous/asynchronous, offline/online, group/individual, and the use of different devices, gamification, virtual reality, and interactive computer simulations. 20 Moreover, studies indicate that satisfaction and examination results in digital education are comparable to traditional face-to-face education. 36
To implement purely digital or blended learning modalities effectively, students and educators require digital skills and appropriate infrastructure.20,26,37 According to Aparicio's framework, which considers three main components—‘people,’ ‘technologies,’ and ‘services’—to enable digital learning, technology serves as a tool for human interaction, and ‘services’ include pedagogical models and instructional strategies that facilitate learning. 38 While other theoretical frameworks exist for digital learning,39–41 there is a dearth of such frameworks specific to learning video consultations. Given the focus of this article on digital learning of video consultations, we discuss the relevant issues and considerations within the context of Aparicio's framework.
Numerous digital learning methods for medical students in telemedicine, particularly in video consultations, have been presented in the literature. For instance, American medical schools have introduced a telemedicine distance learning curriculum based on telehealth competencies published by the Association of American Medical Colleges, albeit without direct patient contact. 23 Another example includes robotic hospital rounds, offering a real patient-centred approach to video consultations for medical students.42,43 Additionally, students can practice anamnesis and digital examinations on simulated patients.44–46 Various specialties incorporate video consultations between students and real patients in their home settings.47–50 Moreover, medical students can gain experience in conducting interviews and examinations with patients at family practices through distance seminars. 50
However, it remains unclear which of these learning methods is preferred by participants. In the Netherlands, medical students favored learning methods that involved direct patient contact from a distance under medical supervision. 35
This study explores the opinions of German medical students regarding the necessity and preferred methods for training in video consultations, particularly within the context of family practice, through digital, patient-centred teaching methods. It addresses a significant research gap by conducting a descriptive cross-sectional study using an online questionnaire. To our knowledge, this study represents the largest survey to date on this topic, with the participation of medical students from all semesters. Our research focuses on the following questions and hypotheses:
What is the current level of knowledge about video consultations among human medicine students in Germany?
This question pertains to the ‘people’ component of Aparicio et al.'s framework. To what extent is there a need among human medicine students in Germany to get taught by having contact with patients from home (patient-related distance learning)?
This question pertains to the “services” component of Aparicio et al.'s framework. Which digital learning methods do medicine students in Germany prefer to learn video consultations in a patient-oriented way?
This question pertains to customers’ opinion regarding a combination of all the component of Aparicio et al.'s framework. How do medical students in Germany evaluate the synchronous distance learning seminar at the University of Witten/Herdecke, where students engage in video consultations with family medicine patients?
What are their expectations from this learning model?
Methods
Survey
This study is a quantitative cross-sectional observational investigation conducted in adherence to the Declaration of Helsinki 51 and approved by the Ethics Committee of Witten/Herdecke University (protocol code S-54/2021, 30 March 2021). To the best of our knowledge, no existing questionnaire adequately assessed medical students’ opinions regarding patient-centered distance learning on family medicine video consultations. Therefore, we developed an online questionnaire, administered from September 10, 2021, to December 20, 2021, with the target population being all students pursuing human medicine in Germany. According to data from the Federal Statistical Office, there were 105,275 human medicine students at the time of the survey, 52 from which we obtained a convenience sample. Inclusion criteria encompassed participants who were German human medicine students with access to the online questionnaire and who actively consented to participate in the study. Exclusion criteria encompassed students from other academic departments or countries, those who contributed to the questionnaire design, and individuals who had completed their studies. Additionally, participants who did not provide or declined active consent for the online questionnaire were excluded. Consent to participate was sought on the questionnaire's homepage, which outlined the data collection, investigator identity, and study's purpose. The survey was designed to be anonymous, as the authors did not have access to connection data, and no personally identifiable information was collected to encourage the participation of as many German medical students as possible.
Due to lack of preparatory work, we developed our own questionnaire based on the AMEE guideline (Association for Health Professions Education). 53 Therefore, the questionnaire is not validated, but a pilot test was conducted (n = 15). The questionnaire was structured into three subareas: patient-centered distance learning, family medicine, and family medicine video consultations. We focused on eliciting preferences for didactic methodologies in these areas. A particular didactic model was explored in greater depth and presented to participants in a visual format (see Chapter “Learning model of a pilot project at the University of Witten/Herdecke”). In this section of the survey, the largest set of items was placed to elicit the learning objectives. The separation of the focal points into didactic formats and learning objectives corresponds to the structure of the survey by Vossen et al., 35 who examined medical teaching with regard to eHealth.
Following step 2 of the AMEE guideline, a focus group of 12 human medicine students provided their perspectives and insights on our research topic. This involved discussions on professional and didactic aspects and the completion of two qualitative questionnaires with predominantly open-ended questions as part of a pilot project.
We created a German-language online survey using the SoSci Survey web application. The survey comprised a total of 15 item complexes, each containing 1 to 21 items (see Table 1). These items were distributed across seven pages, with 2–4 item complexes per page (see Appendix 1 and 2). Eight of these item complexes employed sliders, representing an endpoint-scaled Likert scale with categories ranging from “does not apply at all” (1) to “fully applies” (101). We adopted this 101-point Likert scale to establish an interval scale and to provide participants with a more flexible response format.54–56
Visualization of all item complexes of the questionnaire with items, scales, and results in English. Sorted by category video consultations (No. 1,2), general medicine (No. 3–5), education (No. 6–8), pilot project (No. 9–14), demographic issues (No. 15–16) and feedback (No. 17).
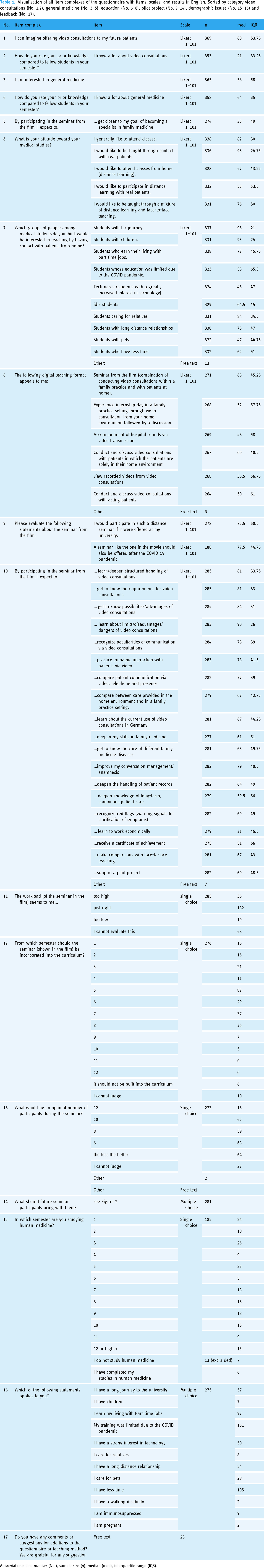
Abbreviations: Line number (No.), sample size (n), median (med), interquartile range (IQR).
In addition to the Likert scale, item complexes featured multiple-choice, single-choice, and free-text fields (see Table 1). Multiple-choice and single-choice items were based on information gathered from the pilot project in Witten–Herdecke. Free-text fields allowed participants to express opinions differing from those collected in the pilot project. Response options were not enforced, except for consent to the questionnaire. Participants could review and amend their answers using a Back button. The questionnaire did not contain adaptive questioning or alternated Items.
According to steps 5 and 6 of the AMEE guidelines, the items created were reviewed for relevance and clarity by a professor of medical didactics, and interpretations were sought from five medical students. Fifteen pretests, primarily involving medical students, assessed the usability and technical functionality of the questionnaire. Feedback and comments were recorded in empty text fields. The final original questionnaire in German is shown in Appendix 1. Appendix 2 contains the questionnaire translated into English. Table 1 contains all item complexes and corresponding question types.
The voluntary survey was conducted from September 10, 2021, to December 20, 2021, with initial contact made through online platforms and email. No incentives were offered for participation. The survey was announced and promoted through various channels, including emails sent via the German Association of Female Doctors and the Internal Working Group for Medical Education of the Federal Representation of Medical Students in Germany. Furthermore, students at Witten/Herdecke University were encouraged to participate during a digital semester kick-off event. Email outreach was also extended to 31 student councils and nine dean's offices of medical schools in Germany. The survey was advertised on five digital bulletin boards at universities. Thus, direct contact was made with a total of 38 of the 41 German medical universities. Additional recruitment occurred through personal contacts of the authors and social media. Further two advertising runs took place in October 2021.
The following formulations were used for e-mails and digital bulletin board postings, among others: “Dear medical students, what is your opinion about a form of teaching in which you care for patients as family physicians via video consultations? I ask you to support my doctoral thesis by filling out the following survey and passing it on to as many medical students in Germany as possible: https://www.soscisurvey.de/telelehre/. The time required is about 8 min. I would be very happy about your support.”, “Dear students, enclosed is a survey on telemedicine teaching in medical school. It provides a basis for moving the issue forward for you. It would be great if you would participate. To do so, simply click on the link below or copy it into your browser. https://www.soscisurvey.de/telelehre/. This is about practical teaching of telemedicine during studies. Mrs. Franziska Särchen, also a member of the DÄB, is doing a PhD on this. I co-initiated and designed the pilot seminar for this teaching format. We would also be pleased if you would forward this message to other medical students.”
This recruitment method introduced a self-selection bias, and other potential confounders include participants’ pre-existing interest in the topic, potential changes in opinion over time, and the possibility of multiple entries. No identification of multiple entries was performed, as neither cookies nor IP checks were employed to safeguard individual-related data and avoid exclusion of multiple users sharing the same computer.
Descriptive statistical analysis was conducted using Microsoft Excel, including the calculation of median (med) and interquartile ranges (IQRs) for scale responses. To streamline the assessment of participants’ responses on a Likert scale, the original 100 levels were transformed into a simplified 5-point scale encompassing ‘strongly agree,’ ‘agree,’ ‘neutral,’ ‘disagree,’ and ‘strongly disagree’. 57 The highest two categories (‘strongly agree’ and ‘agree’) and the lower two categories (‘disagree’ and ‘strongly disagree’) were merged into broader agreement (top) and disagreement (bottom) categories. Consequently, scores from 61 to 101 were regarded as agreement, scores ranging from 1 to 40 were categorized as disagreement, and responses falling in between were considered indecisive.
Participation rate and Completion rate have been calculated. Incomplete questionnaires were also included, as each item could be evaluated independently. A view rate was not determined, as the number of unique site visitors on digital bulletin boards was unknown.
Box plots and bar charts were generated to provide graphical summaries of the results and individual items were correlated using Bravis–Pearson measure coefficients. The medians and interquartile ranges (IQRs) of fully completed questionnaires were compared to those of all questionnaires.
Learning model of a pilot project at the University of Witten/Herdecke
Within the survey, we presented a learning concept for a digitally synchronous distance seminar on family medical video consultations in the form of a comic-style short film (see Figure 1). Subsequently, we assessed the need for this learning model, gathered students’ expectations, and evaluated the workload. We also gathered participants’ assessments regarding the optimal number and requirements for future participants in the seminar (see Table 1, lines No. 8–14).

Course of the distance seminar in pictures from the film in the questionnaire.
Prior to the survey, this learning concept had undergone testing and evaluation as a digitally synchronous distance seminar involving 12 human medicine students at the University of Witten/Herdecke in Germany. 50
The items used in this survey were largely derived from the qualitative descriptive evaluation of this learning concept. Below, we provide a brief explanation of the learning concept, which is also visually illustrated in Figure 1.
As part of the learning model, medical students connected to a video platform from their homes. In preparation for real patient consultations, they were provided with digital patient records (see Figure 1(b)). The seminar comprised both individual and group appointments. In individual appointments, each student conducted a video consultation with a patient in their home environment, with remote observation by a family physician and a fellow student (see Figure 1(c)). These consultations were later debriefed with the family physician and fellow student, as well as within the seminar group (see Figure 1(d)). Additionally, each student participated in five group appointments (see Figure 1(e)), where they were observed by 11 fellow students, a lecturer, and the family practitioner while conducting a consultation with a patient at the family doctor's office. Examination findings can be gathered with the support of the family doctor in the general practice. Subsequently, the seminar group engaged in discussions to deepen their theoretical knowledge about video consultations and family medicine (see Figure 1(f)).
Results
In 2021, there were 105,275 students studying human medicine in Germany, 52 all of whom were potentially eligible for inclusion in our study. A total of 439 participants consented to participate. The participation rate was 0.99 (calculated as the ratio of participants who agreed to participate, 439, to the visitors on the first survey page, 442). The completion rate was 0.67 (calculated as the ratio of users who completed the survey, 292, to those who agreed to participate, 439). We excluded 64 questionnaires due to inclusion and exclusion criteria, such as those providing fewer than one answer, refusing participation, being from a different field of study, or not being a student. Therefore, we evaluated 378 questionnaires, with 275 of them completed in full. Median (med) and interquartile ranges (IQRs) of the fully completed questionnaires differed from the total result of all questionnaires by a maximum of 3.5 Likert scale points.
Students from all 12 semesters participated (n = 185). Of these, 38% were in the preclinical study section (semesters 1–4), and 62% were in the clinical study section (semesters 5–12) at the time of the survey.
For detailed results of all items and their corresponding scales, please refer to Table 1.
Patient-centered distance learning about family medical video consultations
Fifty-eight percent of participants envisioned offering video consultations to their future patients (n = 369, med = 68, IQR = 53.75). However, the median for the statement “I know a lot about video consultations” on the 101-point scale was 21 (n = 353, IQR = 33.25).
This difference between interest and prior knowledge did not exist for the topic of general practice. With a median of 58, 58% of the participants reported being interested in general medicine (n = 365, IQR = 58), and the median for the statement “I know a lot about general medicine” was 44 (n = 358, IQR = 35).
These two topics could be educated through different didactic methods in medical school. Participants showed a preference for blended learning as a teaching method (n = 331, med = 76, IQR = 50), while patient-centred distance learning was less favoured (n = 332, med = 53, IQR = 53.5).
The heterogeneous attitudes towards patient-centred distance learning cannot be attributed to a lack of motivation regarding teaching in general (“I generally like to participate in teaching": n = 338, med = 82, IQR = 30). Participants also did not express disinterest in patient-centred teaching (n = 336, med = 93, IQR = 24.75). However, a weak positive correlation was observed between a negative attitude towards patient-centred distance learning and a willingness to attend classes from home (n = 328, r = 0.63).
Participants considered patient-centered distance learning particularly suitable for students with long travel distances and those with family responsibilities (e.g., childcare, caring for relatives, or long-distance relationships) (see Table 1, line No. 7). However, these results did not align with the frequency of participants disclosing personal circumstances in the multiple-choice item (see Table 1, line No. 16). In this context, 21% of 275 participants stated that they had to travel a long way to the university, and 25% stated that they were exposed to family stress in the context of caring for children/relatives or long-distance relationships. Most commonly, students reported experiencing limited education due to the COVID-19 pandemic (54% of 275), having limited time (38%) and earning their own living from part-time jobs (35%). Some participants noted in the open-text field that students with illnesses and those working on a second degree or dissertation could also benefit from patient-centered distance learning, although these groups were not included as specific items.
The participants considered the seminar of the pilot project of the University of Witten/Herdecke to be the most appealing learning concept compared to five other digital learning formats that included video consultations (see Table 1, line No. 8). In response to the final open-text question, seven participants expressed the view that these learning methods should be used as supplements rather than substitutes for face-to-face teaching.
Pilot project of the University of Witten/Herdecke
Sixty-three percent of participants would join the learning concept of the pilot project if it were offered at their university (n = 278, med = 72.5, IQR = 50.5). A smaller portion, 21%, declined to participate, while 16% were undecided. Additionally, 72% of participants agreed that the seminar should continue to be offered after the COVID-19 pandemic (n = 188, med = 77.5, IQR = 44.75). There was a weak positive correlation between agreement with this statement and willingness to participate in the seminar (r = 0.697).
Table 1, lines No. 10 and 5, provide insight into what students expected from their participation in the seminar in terms of telemedicine, family medicine, and didactics. Students primarily hoped to gain knowledge and experience about video consultations. Statements related to an increase in knowledge and experience about family medicine and didactics were only secondary concerns. Those who could envision offering video consultations to future patients were more likely to express interest in participating in the distance seminar (r = 0.466).
The workload within the presented distance learning seminar was rated by 64% of the participants as just right compared to other courses (n = 285). The workload was described to the participants as follows: “The seminar lasts 4 weeks. Students have an average of 2.5 h of compulsory attendance per week. Participants need an average of 22 min per week for preparation and follow-up work”. Of the 36 students who stated that the workload was too high, half would still consider joining.
When asked about the optimal group size, 23% of participants preferred a group as small as possible (n = 275). Twenty-five percent believed that six students were optimal, 21% preferred eight students, and 5% favoured 12 students (see Table 1, line No. 13).
Participants’ opinions on the optimal timing for integrating such a distance seminar into the curriculum were gathered. The most popular choice, selected by 40% of participants (n = 276), was to introduce the seminar at the beginning of the clinical study section (semesters 5 and 6) (see Table 1, line No. 12). In addition to the completed semesters, further requirements with regard to personal attitude, technical equipment and professional experience, which participants should bring to the remote seminar, were asked (Figure 2).

Evaluation of the information on the following question with multiple selection: “What should future seminar participants bring with them?” Number of participants: 281.
Discussion
Principal results
The first question aimed to assess the current level of interest in video consultations among medical students in Germany. Participants expressed a desire to offer video consultations to their future patients, even though they acknowledged having limited knowledge in this area. This finding supports prior research indicating that both German and European medical students tend to rate their eHealth competencies as low.35,58,59 However, they recognize the relevance of these competencies and express a need for more information on telemedicine.33,35,58,59 Therefore, there is a call to expand teaching on these digital competencies within medical schools. Additionally, it is crucial to nurture and cultivate basic digital health skills to enable thoughtful application of telemedicine in patient care. 60
The hypothesis that the first question belongs to the “people” component of the e-learning framework of Aparicio et al. can be confirmed by several points of view. On the one hand, the question considers the characteristics of the customers (students). On the other hand, the conclusion of the question contains a call to stakeholders suppliers (teachers, professional associations, student commissions and the Ministry of Education). Therefore, interaction between stakeholders is necessary to build digital education, although, as described in the framework, the interaction of stakeholders with digital education varies. 38
The second question was to what extent there is a need for patient-centred distance learning among medical students in Germany. The participants indicated a high interest in learning with real patients. Both German regulatory requirements and students from various health professions emphasize the importance of medical education being practical and patient-centred, often involving the direct involvement of real patients.61–63
The moderate interest in distance learning, in contrast to the high interest in blended learning, can be understood in the context of the COVID-19 pandemic. Students have experienced several semesters with a heavy focus on distance learning, which has its limitations, particularly related to reduced social interaction.64–66 Nevertheless, they recognize the advantages of remote learning, particularly in terms of inclusivity. It could be beneficial for students with long commutes and family responsibilities to engage with patients remotely. Additionally, students with chronic illnesses could benefit from accessing digital teaching from the comfort of their homes. 67
The survey was designed to assess interest in distance learning versus blended learning before participants watched the video. Therefore, their responses were unbiased. After viewing the video, most participants indicated a willingness to participate in the distance learning seminar, even if they initially favoured blended learning. In summary, participants expressed interest in both patient-centered distance learning and blended learning. Regarding patient-centred education, it is questionable whether face-to-face teaching can be completely replaced by digital means, especially about the acquisition of competencies for physical examination. 68 In the future, patient-centred teaching on video consultations, delivered through distance learning and blended learning, should complement traditional in-person medical education.
The theoretical framework is also applied in this research question. Within the e-learning framework, the “services” category is defined by pedagogical models and instructional strategies. 38 One of the main principles of pedagogical models is that „learning is a social process, learning in group is fundamental to achieve knowledge; distance is unimportant”. 38 This principle clarifies the second question with regard to distance learning. The question of patient classification is only touched upon in the framework within the “instructional strategies” through role playing. In conclusion, the second question aligns with the “services” category of the framework.
The third question aimed to identify the preferred patient-centred digital learning methods for German medical students to acquire skills in video consultations. The survey results revealed that students favoured the seminar presented in the video clip. In contrast, watching recorded videos of video consultations was not well-received by students. Conducting and discussing video consultations with patients, where patients are solely in their home environment, was considered moderately engaging by participants on average. Various models from different specialties have been reported in the literature for institutions seeking to incorporate this learning method into their teaching.47–49 Additionally, the concept of experiencing an internship day in a family practitioner's office through video consultations, followed by discussions, was rated similarly. This learning method has been integrated into pilot projects in both England and Germany, among other places.45,69,70 Some model projects represent digital learning methods that incorporate hospital rounds using video consultations.42,43 This type of digital teaching was also rated as moderately appealing by participants on average. Ideally, multiple learning methods are combined to acquire lifelong skills,71,72 with each combination including feedback. 73 Therefore, the results suggest that students appreciate multiple learning methods and can benefit from a combination of these methods to develop proficiency in performing video consultations.
The choice of learning methods, whether individually or in combination, and their implementation by universities depend on available resources. In the authors’ opinion, this decision should be left to individual institutes. General recommendations on how to integrate telemedicine content into medical education, based on the telehealth competencies outlined by the Association of American Medical Colleges (AAMC), have been reported by Noronha et al. 74
The learning methods included in the survey do not correspond to all the “services” and “technologies” mentioned in the framework. Instead, they were selected based on proven digital learning methods using video consultations described in the literature. There are numerous approaches to combining the components of the framework for teaching video consultations. Another approach to ensure widespread access to learning about video consultations could involve the use of massive open online courses (MOOCs). “MOOCs are capable of targeting different audiences with different needs and backgrounds, as well as with different learning expectations by also ensuring transferable credits both for university and continuing education “. 75
The framework makes a clear distinction between technologies and services. However, participants in the survey were provided with examples of e-learning methods. Their ratings of these examples were based on the overall concept and cannot be easily categorized into the individual components of the framework. The two best-rated examples, “Seminar from the film” and “Conduct and discuss video consultations with patients in which the patients are solely in their home environment,” fall under the “people” category, involving students, teachers, and real ambulant patients.
In the “pedagogical models” category, the seminar from the film offers distributed learning within a community, while the second example does not align with the pedagogical models mentioned in the framework. The technologies used in these examples, including digital audio and video, synchronous discussion areas, video conferencing, and assessment, can be employed to achieve various instructional strategies such as authentic activities, problem-solving, articulation and reflection, collaboration and negotiation, and scaffolding. Additionally, role-playing can be facilitated when considering patient conversations as such. The example “view recorded videos from video consultations” lacks both the “people” component of the patient and teacher, as well as several technologies and instructional strategies. However, the example “Experience an internship day in a family practice setting through video consultation from your home environment followed by a discussion,” which received moderate ratings, encompasses similar features in terms of the framework as the two highly rated examples. Hence, it is not possible to establish a correlation between the number of fulfilled components of the framework and the rating of the learning models of the questionnaire.
Questions related to point four focused on the evaluation and expectations regarding the synchronous distance learning seminar at the University of Witten/Herdecke. The learning concept of this pilot project could serve as an effective way to introduce video consultations to medical students. Since a large part of the participants would join if it were offered at their university, they preferred it in comparison to five other digital teaching formats including video consultations, and they stated that the seminar should be offered after the COVID-19 pandemic, this learning method is recommended.
The participants expected to gain knowledge about video consultations, especially about their limitations and possibilities. In addition, they would like to learn how to use it in a structured way and to know the prerequisites. This learning content is in line with the requirements of the AAMC, the German Society for Medical Informatics, Biometry and Epidemiology as well as the National Competence Based Learning Objectives Catalogue for Medicine (NKLM).76–78
Although the participants considered it useful to start the learning concept at the beginning of the clinical study section, a longitudinal installation of the model over several semesters could also be considered in order to deepen their competencies and to observe the progress with growing professional knowledge. The personal requirements for future participants in terms of empathy, motivation and appreciative interaction will be fundamentally beneficial for any kind of teaching. The technical requirements for future participants could be a financial challenge for universities that want to establish the learning model in the future.
Limitations
No sample size analysis was done in advance to calculate the sample size. During the statistical consultation, the objective was emphasized to reach the highest possible number of participants. Only 0.3% of the opinions of the target population were captured, which restricts the ability to make generalized statements about all medical students. Because it is an online questionnaire, it is unknown why people did not participate. However, with over 300 respondents, the minimum size for quantitative sampling is exceeded. 79 To our knowledge, it is the largest survey on this topic to date, and students from all semesters are represented.
Due to voluntary participation without a systematic sampling procedure, there is a self-selection bias. The extent of this bias cannot be estimated. It is also impossible to determine why some students chose not to participate.
Another issue is the lack of validation for the questionnaire. However, the questionnaire was developed according to AMEE criteria and a pilot test was conducted (n = 15).
It cannot be verified whether individuals participated more than once or if students from fields other than human medicine joined the survey. However, the survey link was not personalized or password-protected, allowing it to be easily completed by as many human medicine students as possible. The survey explicitly stated on its homepage that it was intended for students of medicine in Germany. Any questionnaires where the participant indicated they were not / no longer studying human medicine were excluded.
Interest in various patient-centred teaching methods related to video consultations was assessed in the survey only after participants viewed the video clip. This might have influenced their evaluation, particularly regarding the seminar from the film compared to the other learning methods. However, the learning methods being compared closely resemble students’ everyday experiences, which suggests a reasonable level of understanding among participants.
Implications for practice
Based on the results, it can be inferred that, from the perspective of medical students, the incorporation of video consultation education into the curriculum of German medical universities is warranted. This need is consistent with existing literature.26,33,35,58,59 These findings should serve as a catalyst for professional associations and decision-makers to actively promote this integration. Educators, healthcare practitioners, and universities can adopt the teaching and learning formats presented in this study for implementation. Alternatively, they can develop new learning formats tailored to the specific needs identified among medical students in this study. In selecting the content, we recommend aligning with the learning objectives outlined in this study and those established in the literature concerning telemedicine,76–78 fundamental digital health competencies 60 and the criteria for conducting good video consultations. 80
Implications for research
This study has demonstrated the alignment of practical questions with the theoretical e-learning framework, shedding light on the opportunities and requirements of medical students for digital learning, particularly in the context of video consultations. However, further research is warranted to gain a deeper understanding of the digital learning needs and preferences of medical students, with a specific focus on video consultations. There is a notable gap in the literature regarding the pedagogy of teaching video consultations, and this area merits comprehensive reviews.
Future research endeavors should also explore and compare alternative learning models with the ones presented in this study to identify best practices and innovative approaches. Additionally, it is imperative to gather the perspectives of various stakeholders, including educators, healthcare professionals, patients, professional associations, educational ministries, and policymakers. By integrating these diverse viewpoints with the insights gleaned from this study, a more holistic and effective medical education strategy can be developed to meet the multifaceted needs of all involved parties.
Conclusions
This study's findings highlight a significant gap in knowledge transfer concerning video consultations within medical faculties in Germany. Moreover, it underscores that medical students in Germany demand to learn more about this subject, for example through blended learning models and distance learning. Five digital patient-centred learning methods preferred by the participants were presented here. In terms of content, the students’ learning objectives regarding video consultations matched the learning objectives of the NKLM on this topic.
To further advance the field, additional research is imperative to understand international perspectives on preferred learning methods and to engage all stakeholders in the discourse. Moreover, these identified teaching methods warrant further in-depth investigation, comparative analyses, and implementation within medical universities.
Supplemental Material
sj-pptx-1-dhj-10.1177_20552076241230070 - Supplemental material for Digital learning about patients: An online survey of German medical students investigating learning strategies for family medical video consultations
Supplemental material, sj-pptx-1-dhj-10.1177_20552076241230070 for Digital learning about patients: An online survey of German medical students investigating learning strategies for family medical video consultations by Franziska Särchen, Susanne Springborn, Achim Mortsiefer and Jan Ehlers in DIGITAL HEALTH
Supplemental Material
sj-pptx-2-dhj-10.1177_20552076241230070 - Supplemental material for Digital learning about patients: An online survey of German medical students investigating learning strategies for family medical video consultations
Supplemental material, sj-pptx-2-dhj-10.1177_20552076241230070 for Digital learning about patients: An online survey of German medical students investigating learning strategies for family medical video consultations by Franziska Särchen, Susanne Springborn, Achim Mortsiefer and Jan Ehlers in DIGITAL HEALTH
Footnotes
Acknowledgements
We extend our heartfelt gratitude to all those who took the time to complete and share our survey. We are particularly appreciative of the support provided by the German Association of Female Doctors, the Federal Representation of Medical Students in Germany's Internal Working Group for Medical Education, and the student bodies of medical schools in Freiburg, Hanover, Mannheim, Mainz, Münster, Würzburg, and Witten/Herdecke for their invaluable assistance in distributing and promoting the questionnaire. Furthermore, we would like to express our appreciation to the medical schools in Bochum, Duisburg-Essen, Heidelberg, Cologne, and Regensburg for granting us the opportunity to advertise the survey on their digital bulletin boards. Finally, our sincere thanks go to all those who contributed to enhancing the questionnaire through their participation in the pretest.
Contributorship
All authors created the rough concept of the questionnaire. FS and JE researched literature, conceived the questionnaire and applied for ethical approval. SS reviewed the final version of the questionnaire. FS did the data analysis and wrote the first draft of the manuscript. AM revised the manuscript critically for important intellectual content. All authors reviewed and edited the manuscript and approved the final version of the manuscript.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
The study was conducted in accordance with the Declaration of Helsinki 51 and approved by the Ethics Committee of Witten/Herdecke University (protocol code S-54/2021, 30 March 2021). All participants actively provided informed consent for participation in the study.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Guarantor
JE
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
