Abstract
Background
The use of internet videoconferencing in healthcare settings is widespread, reflecting the normalisation of this mode of communication in society and current healthcare policy. As the use of internet videoconferencing is growing, increasing numbers of reviews of literature are published.
Methods
The authors conducted a review of the existing reviews of literature relating to the use of internet videoconferencing for consultations between healthcare professionals and patients with long-term conditions in their own home. The review was followed with an assessment of United Kingdom National Institute for Health and Clinical Excellence guidelines for patient care in the context of common long-term illnesses to examine where videoconferencing could be implemented in line with these recommendations.
Results
The review of reviews found no formal evidence in favour of or against the use of internet videoconferencing. Patients were satisfied with the use of videoconferencing but there was limited evidence that it led to a change in health outcomes. Evidence of healthcare professional satisfaction when using this mode of communication with patients was limited. The review of guidelines suggested a number of opportunities for adoption and expansion of internet videoconferencing. Implementing videoconferencing in line with current evidence for patient care could offer support and provide information on using a communication channel that suits individual patient needs and circumstances. The evidence base for videoconferencing is growing, but there is still a lack of data relating to cost, ethics and safety.
Conclusions
While the current evidence base for internet videoconferencing is equivocal, it is likely to change as more research is undertaken and evidence published. With more videoconferencing services added in more contexts, research needs to explore how internet videoconferencing can be implemented in ways that it is valued by patients and clinicians, and how it can fit within organisational and technical infrastructure of the healthcare services.
Introduction
The use of internet videoconferencing in healthcare settings is widespread, particularly to support contact with patients in remote and rural areas across the world.1,2 Previous studies on the use of videoconferencing have reported increased benefits in patient care in terms of reduced travel to hospital sites and convenience in consulting with clinicians from the patients’ own homes,3,4 particularly for those with long-term conditions.5–7 Increasingly, policymakers in the United Kingdom (UK) and elsewhere, are encouraging the use of internet videoconferencing with patients in routine healthcare settings,
8
reflecting the normalisation of videoconferencing in society and current policy.9,10 In the UK, the government has been investing in the infrastructure for digital communication. The software has been rolled out to allow Skype to be used safely and securely in the specialist clinical settings.
11
However, there has been some concern that Skype may pose regulatory and logistical challenges and may not be acceptable to patients and healthcare professionals. In our recent LYNC study (
Clinical pathways are tools used by health professionals to determine the best way to manage specific medical conditions according to the best available evidence. 14 The pathways map out, in chronological order, the key activities in a healthcare process for specific patient populations. 15 In the UK, the National Institute for Health and Clinical Excellence (NICE) produces guidelines for health, public health and social care practitioners. Guidelines are published on the NICE website with the summarised evidence and resources to help practitioners implement them. These guidelines are also included in the NICE pathways, online tools that include up-to-date advice, quality standards and related information, from preventing and managing specific conditions to improving health and managing medicines in different healthcare settings. In recent years, NICE has developed many new care pathways, including those for long-term conditions. For example, the pathway for type 2 diabetes includes specific guidelines on monitoring patient’s blood pressure and glucose, as well as on identifying and managing complications and individualised care. As such, these tools can be implemented to improve care delivery for patients. However, videoconferencing pathways are not currently represented in these policy documents.
In this paper, we summarise the existing reviews of literature relating to the use of internet videoconferencing. We follow this review with an assessment of NICE pathways for common long-term conditions and identify where, from our interpretation of these guidelines, internet videoconferencing could be an appropriate option for healthcare delivery. Arguably, it may provide advantages to patients, their clinicians and/or healthcare systems. Finally, we interpret the results from the literature and NICE guidelines review in light of findings from the LYNC study, examining how videoconferencing fits with the use of other digital communication media.
Aims
The aims of this paper are:
To summarise the existing reviews of literature relating to the use of internet videoconferencing between patients with long-term conditions and their treating clinicians from the patient’s own home (or mobile device). To review the NICE guidelines for long-term conditions (LYNC study conditions: psychosis and schizophrenia, HIV, diabetes, liver fibrosis, eczema, psoriasis, cancer, asthma, cystic fibrosis, arthritis, kidney and sickle cell disease). To identify where, in the patient pathway, the use of videoconferencing might be possible and of advantage to the patient, their clinician and/or the healthcare system.
The review of reviews
Methods
In collaboration with a trained information specialist (RC), a set of searches was developed that aimed to capture reviews on the use of videoconferencing for clinical communication. Firstly, using search terms ‘skype’ ‘videoconferenc*’ ‘video-conferenc*’ ‘Google AND (talk or hangouts)’ in any field, we searched the
Results from the searches in 2014 were screened independently by one reviewer (HA) who rated the eligibility of the records to confirm relevant papers. Abstracts and full-text papers were then reviewed by two authors (HA and CJB) to determine studies to be included for full review. From each included paper, using a standardised form, two reviewers extracted information about (1) the purpose of the study; (2) patients and participants; (3) the clinical application area; (4) the study design; (5) the country, or countries, where the study was conducted; and (6) whether the study findings supported the clinical use of videoconferencing and Skype. The process was then repeated for papers from the updated searches in 2017 by AI and CB.
This review included literature reviews, systematic reviews and meta-analyses. Studies were included if they: (1) included reviews conducted in healthcare settings where internet video use was with a patient in their own home or on a mobile device; and (2) focused on patients with long-term illnesses. We included English language articles only, and only those published since 2009. We excluded reviews of reviews and those review articles that focused on patients with multiple long-term illnesses.
The quality of each study was appraised by reviewers using the Assessment of Multiple Systematic Reviews (AMSTAR) checklists. 16 Each checklist criterion was scored as 1 (checklist criterion satisfied); or 0 (checklist criterion not satisfied, or unclear) yielding a quality score across all criteria for each study in the range of 0 (worst) to 11 (best). Reporting was guided, where applicable, by PRISMA guidelines. 17 The data are presented as a narrative synthesis of the findings from the identified reviews.
Results
A total of 489 relevant studies were identified in the searches, which included several systematic reviews. After screening, a total of 149 abstracts were selected for full-text review and 35 review articles were included in the review (Figure 1).

Study PRISMA flow diagram.
Review characteristics
The characteristics of the included reviews are summarised in Table 1. These covered a wide range of long-term conditions, including: heart failure, depression, schizophrenia, stroke, asthma, spinal cord injury, and chronic pain. Of 35 articles included in this review, 25 were reviews or systematic reviews. Overall, eight looked at internet videoconferencing exclusively,7,18–24 with the remainder examining a range of telehealth interventions including videoconferencing. Only one review of the clinical use of Skype was identified. 7 Among the videoconferencing exclusive reviews, there were five that included more than 25 studies in their review.7,18,21,25,26 In 24 of the included reviews, forms of internet videoconferencing were compared with a face-to-face consultation or usual care.
Characteristics of included reviews.

Overall, the methodological quality of included reviews was poor (Table 2). Only six reviews were methodologically strong,7,22,26–29 with the remaining 31 obtaining a score of 6 or below, thus being of poor quality. The most common methodological weaknesses were limited details of the included study characteristics, such as clinical outcomes, participants’ demographics and potential biases in the selection of articles. Within the included reviews, low and variable uptake and the cost of establishing videoconferencing services across primary studies were often identified as a limitation.
Quality assessment of included reviews.
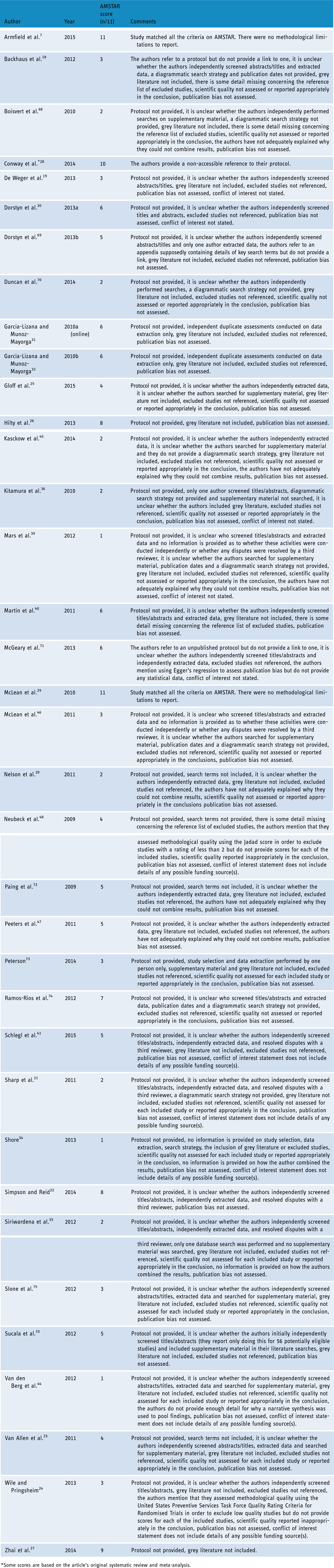
*Some scores are based on the article’s original systematic review and meta-analysis.
Patient, professional and health service delivery outcomes
The results from the included studies are presented in Table 3. The reviews commonly focused on effectiveness and outcomes for specific patient groups and conditions, and on patient satisfaction with this mode of communication. A total of six reviews found evidence of patient satisfaction and equivalence with face-to-face encounters and eight found improvement in at least one health outcome.
Results of included reviews.

Patient outcomes
A review of telecounselling for depression pooled results from 498 adults of African-American, Spanish, and Asian origin and found some evidence of increased satisfaction among individuals from ethnic minority communities. Limited data also pointed towards longer-term health benefits for these patients. 30 The review of telepsychiatry analysed results from a total of 1054 patients from psychiatric services and concluded that telepsychiatry is safe to use. However, there was insufficient evidence regarding its effectiveness in the routine management of mental health patients. 31 Furthermore, a review of videoconsulting for depression found it to be as beneficial as in-person care. 32
Overall, two reviews indicated that a good therapeutic alliance between clinician and patient is possible via video,33,34 but no improvement in health outcome was found in one of these reviews. 33 There were two reviews that indicated that this modality may be better than in-person care for some conditions, such as autism 26 and anxiety-related disorders. 19 This was often attributed to the difficulties and low motivation that can sometimes accompany these conditions, and may hinder engagement with alternative forms of intervention. The feasibility, acceptability, and sustainability of telemental health for children and adolescents have also been reported. Overall, two reviews found that telemental health assessment with this group of patients was, in general, reliable and feasible.20,23
In the review of the use of telemedicine in diabetes, 23 of the 27 randomised controlled trials reported improved metabolic outcomes. In total, 12 of the 23 studies produced significant results, while only two observed negative health outcomes. 35 Another review of 19 studies using videoconferencing in oncology found no conclusive evidence of a difference between video consultation and face-to-face consultation. 36 However, a review of telemedicine for asthma concluded that there was there was a reduction in hospital admissions.37 Some reviews found differences in outcome depending on the communication medium. For example, a review of telemedicine for heart failure concluded that videophone did not improve outcomes but structured telephone follow up and telemonitoring did, including all-cause mortality. 28 In another review of the use of digital communication between clinicians and young people requiring mental healthcare, 5 of the 12 studies concerned videoconferencing, but significant improvement in health outcome was only seen with email contact. However, the authors concluded that the evidence dealing with email and web-based discussion was more reliable and rigorous than for videoconferencing. 38
Only one review of the clinical use of Skype was identified. 7 Arnfield and colleagues summarised evidence from the 27 published studies and concluded that 26 of the 27 articles presented results that were supportive of Skype. In particular, Skype was adequate for patients across the age spectrum, although the majority of studies described applications involving adult patients. Overall, five studies concluded that Skype offered good communication between patients and clinicians. However, concerns about the security and privacy were raised in the majority of the included papers.
Healthcare professional outcomes
Overall, four reviews considered the health professional perspective in more depth. A review of forensic telepsychiatry in mental health reported that healthcare professionals were less satisfied with using videoconferencing for the purpose of assessment compared with the prisoners they were treating. 39 This is acknowledged in another review that found professionals preferred using email and other web-based approaches to videoconferencing when communicating with young people with mental health disorders. Emails were viewed as beneficial to therapy because written communication allowed clinicians to recount the young person’s personal and health experiences. 40 Schlegi and colleagues found that videoconferencing provides little benefit for clinical staff in terms of cost or time savings, but may assist patients who live in remote places to access specialist psychological service. 41 Weger and colleagues concluded that the studies tend to highlight that health professionals are more reluctant than the service users to use the technology. 19
Health service outcomes
Health service delivery outcomes represented an outcome of interest in 30 reviews. In the review on the use of telemental health, Hilty et al. reported reduced length of hospitalisation and better medication adherence. 26 Although the sub-analysis of a larger systematic review 28 and meta-analysis into heart disease42,43 found that structured telephone follow up and telemonitoring reduced heart failure-related hospitalisation admittances, the authors found no conclusive evidence that this occurred with videoconferencing. In another review on the use of telemedicine for older patients, 36 of the 50 studies (that included a medical endpoint) comprised various health service outcomes (i.e. cost, hospitalisation, healthcare utilisation). 44 The conclusion of the review was that video consultation may be an effective method for decreasing healthcare expenditure. A review focused on telepsychiatry reported that there were limited data in support of the cost-effectiveness of video technologies. 45 Another review of internet videoconferencing for long-term conditions reported similar findings about the evidence for cost-effectiveness. 46 Armfield and colleagues reported that Skype was more economical than face-to-face appointments with savings accruing from avoided travel, 7 while the review of Peeter et al. of the financial benefits of videoconferencing in comparison with usual care at home reported no advantages compared with usual care. 47 Taking into consideration the limited data surrounding the financial implications of telemedicine, some reviews were unable to form any meaningful conclusions about its cost-effectiveness.27,40,48
Summary of the findings
In the home setting, for patients with long-term conditions, the review of reviews indicates that there is no formal evidence in favour of or against the use of internet videoconferencing. Evidence for its impact on health outcomes suggests it mostly has equivalence with face-to-face communication. The evidence for equivalence seems to be the strongest in mental health conditions. Furthermore, internet videoconferencing seems to be an acceptable mode of care delivery for patients with long-term conditions. Research indicates that patients who have experienced videoconferencing with clinicians, like it. However, there is limited evidence about healthcare professionals’ satisfaction with this mode of communication. Little is also known about the impact of videoconferencing on health service costs. The discussion sections of most reviews often suggest that further research is needed around cost, ethics and safety, and the practical challenges when implementing internet videoconferencing. Finally, this review of reviews identified only one review of the clinical use of Skype. Many of the reviews identified included internet videoconferencing as one of a number of communication channels with the patient, making it difficult to disentangle the actual impact of videoconferencing.
In the remainder of this paper we explore where, in the patient pathway, videoconferencing could be used to deliver healthcare and offer advantages to patients, their clinicians and the healthcare system.
NICE pathways review
Methods
We undertook a review of NICE pathways for the diagnosis, treatment and management of long-term conditions for children, young people and adults. We chose to look at psychosis and schizophrenia, HIV, diabetes, liver fibrosis, eczema, psoriasis, cystic fibrosis, cancer, asthma, arthritis, kidney and sickle cell disease specifically as these were the conditions we researched in the LYNC study project.
Using the online NICE guideline pathway tool (available at www.nice.org.uk/guidance/published?type=apg,csg,cg,mpg,ph,sg,sc), we searched the guidance and advice list for the chosen conditions. For each condition, two reviewers (clinician and researcher) read all the statements and related quality standards, and noted whether videoconferencing could be used as a mode of healthcare delivery during the implementation of the guidelines. This involved going through the NICE interactive flowchart and examining all the recommendations. Depending on the condition, the flowchart covered information on preventing, detecting, diagnosing, monitoring and managing the long-term conditions in primary, secondary and community care. It also included principles of care and general statements about the quality of support provided to patients. We then compared our findings to those of the review of reviews and the LYNC study to further illustrate the practical applications of videoconferencing in clinical practice.
Results
Our assessment of NICE pathways suggests that Skype and other forms of internet videoconferencing could be used to review, monitor and plan care for patients with long-term conditions (Table 4). In line with the current evidence and guidelines, internet videoconferencing could be implemented to help clinicians support patients through:
Findings from the review of NICE guidance for chosen long-term conditions.

NICE: National Institute for Health and Clinical Excellence.
Advice and education: supporting patients in developing strategies to promote and maintain independence and self-efficacy.
Information: signposting and providing patients with information about their condition.
Relationships: enabling and helping to maintain better communication, and supporting patient and their family’s psychological and social needs.
There is a range of clinical, supportive, educational and administrative functions for which internet videoconferencing may be useful, from supporting care planning and monitoring, organising follow-up consultations, reviewing or adjusting medication to providing group or individual educational programmes for patients with diabetes. The findings from our assessment suggest that videoconferencing would be a particularly useful mode of communication when considering the NICE general principles of care and quality statements underpinning clinical practice, most notably, those around offering support and information on individual patient needs and circumstances.
Videoconferencing could be implemented to meet patient need and preference at the appropriate time and for specific reasons. Given that the main advantage of videoconferencing is its convenience, the wider literature indicates that the implementation of this method could potentially reduce barriers to treatment. For example, patients may be able to save time travelling to the clinic and, in doing so, avoid disruption to their daily activities. Patient education, either group or individual, could be undertaken using internet videoconferencing. Studies that have used videoconferencing for patient education report a number of advantages, including patient satisfaction, improved health outcomes and overcoming mobility and illness issues.49–51 Care planning, reviews and monitoring, especially for those patients that have considerable distances to travel for their appointments or are not well enough, could be assisted using videoconferencing. Examples from our own LYNC research suggest that one of the key benefits of digital clinical communication in comparison with face-to-face care was that it improved access to health services and increased patient engagement. Young people highlighted the role that digital clinical communication played in saving them time, they did not have to fit around the operating times of the clinic and were able to have a more frequent contact with their healthcare professionals. Digital clinical communication was thought to help reduce the power imbalance in the patient–clinician relationship, with clinicians fitting into the young person’s world rather than the young person being expected to fit into the clinical world. As a result, young people believed they had received a more personalised care tailored to their own preferences and healthcare needs. Both patients and clinical team members noted that this improved the relationship between patient and clinician, and prompted better control of young peoples’ condition levels of self-care. A number of issues contributed to this perceived improved personal relationship and self-management: the ability to have more frequent contact with a specific clinician who is known to the patient and likely to know that particular young patient’s personal circumstances and what is important to them; the ability to have questions or queries answered quickly and therefore take better control of the condition; and the ability to communicate with clinical teams between appointments.
Overall, the review of NICE pathways points to a number of opportunities for adoption or expansion of internet videoconferencing for patients with long-term conditions. However, the opportunities to use this mode of communication and the actual benefits derived from it are likely to depend on many factors. The focus on the patient experience is important but this experience may vary substantially according to the treatment pathway. Choosing to utilise internet videoconferencing may be influenced by patients’ preference, their digital resources and skills, clinician’s motivation to use it, the organisational and resource considerations, the healthcare setting and the actual long-term condition. The LYNC study found that these factors were likely to impact on the implementation of digital clinical communication, but could be minimised if the clinician is clear on what they hope to achieve in terms of the ability of the patient to manage their condition and health outcome. Furthermore, adoption of internet videoconferencing is likely to vary based on factors such as patient group or clinical setting. For example, communication problems in the elderly patients, such as visual or hearing impairment, are likely to impact the use of videoconferencing. In our study, the use of different modes of communication varied across clinical teams and according to the reason for making contact. Digital modes of communication also appeared to work best for patients and clinicians who had pre-existing and established relationships.
Despite these insights, the use of videoconferencing in line with the current guidelines for patient care may entail a number of challenges. Issues such as reliability of the internet connection, privacy in terms of surrounding environment, confidentiality of the information shared and informed consent, support for patients and clinicians using the technology, cost to the patient, and challenges surrounding information governance, compliance with legal and regulatory standards around privacy and data protection are often mentioned in the literature, but rarely explored in detail. The lack of data and the need to consider not only costs to health services, but also costs to patients and their social networks, are often highlighted as an important issue to explore. 52 Furthermore, the use of videoconferencing raises a number of ethical questions. In the LYNC study, young people had different understandings of confidentiality and privacy than clinicians, and expressed different levels of concern about possible breaches. 53 Clinicians emphasised the importance of informing patients clearly about the implications of using digital communication and seeking their consent prior to commencing this service. However, they also expected that patients will take responsibility for knowing the risks. There are inherent challenges around the roles and responsibilities of clinicians when using videoconferencing for consultation purposes. With a growing number of opportunities for adoption and expansion of videoconferencing, further research exploring the actual implementation challenges to inform and support the development of services is also needed. If internet videoconferencing is to be used in line with the current guidelines for patient care, the risks and benefits for different patient groups and healthcare settings ought to be explored.54,55
Discussion
This review of reviews identified and synthesised a body of literature relating to the use of internet videoconferencing between patients with long-term conditions and their treating clinicians from the patient’s own home. The review indicated that there was no formal evidence in favour of or against the use internet videoconferencing. A total of 6 out of 35 review articles included in this review concluded that patients were satisfied with the use of videoconferencing. However, there was limited evidence that its use led to a change in health outcomes. In some cases, it compared unfavourably with other methods of communication, such as web or telephone-based communication. Evidence of healthcare professional satisfaction when using this mode of communication with patients was limited. Little was also known about the impact of videoconferencing on health service cost, ethics and patient safety.
To our knowledge, this is the first review of reviews conducted in this topic area. However, in comparing our findings with the systematic reviews of internet videoconferencing in areas other than chronic conditions, it appears that some findings are comparable. For instance, research has shown that such modes of communication are acceptable to patients and effective for support after premature birth, 56 follow up after total joint arthroplasty57,58 and care for paediatric patients with various healthcare conditions. 59 Good evidence from reviews also exists for other settings, some forms of videoconferencing have been found to be feasible and acceptable for patients based in hospitals, clinics or nursing homes. 60 However, the reviews also highlight that despite a number of studies on videoconferencing, high-quality evidence is only beginning to emerge. In this review, we identified a considerable number of reviews that were of lower quality. Limited details of included studies’ characteristics, potential biases in the selection of articles and the methodological limitations of primary studies included in the reviews are often cited as difficulties in bringing the conclusions together. Many of the reviews in our review focused on various internet videoconferencing modes and included them as one of a number of communication channels studied, providing little evidence on the actual impact of videoconferencing. Publication bias might also be a potential issue. Videoconferencing technology can often be implemented and used in routine healthcare practice, but the evidence of its acceptability and efficacy may not be published in academic literature. As such, and despite a substantial increase in the number of published papers on videoconferencing in the last few decades, further research on its deployment is needed. Our review of reviews adds to the knowledge by summarising the extent, range, and nature of findings of many separate reviews.
In the UK, there is a strong policy and political push towards the use of digital technologies for clinician–patient communication to improve and transform care models and patient pathways. Software has been rolled out to allow Skype to be used safely and securely in the specialist clinical settings. The evidence base for the clinical use of Skype is growing, our review of reviews concluded that Skype offered good communication between patients and clinicians and was more economical than face-to-face appointments with savings accruing from avoided travel. The review of NICE pathways points to a number of opportunities for adoption and expansion of Skype and other forms of videoconferencing for patients with long-term conditions. However, as the review and the lessons from the LYNC project highlight, implementing internet videoconferencing services poses a number of challenges. Past research suggests, for example, that video consultations can be less reliable61,62 and less safe 63 in comparison with face-to-face meetings. Issues of privacy, confidentiality and informed consent, support for patients and their clinicians, and challenges around information governance and compliance are often explored superficially. Very few studies have looked at how they are interconnected and impact on implementing the videoconferencing services.54,55 Internet videoconferencing for patient–clinician consultations also requires some basic necessary technical conditions to be in place, including basic technological infrastructure and available technical support. Recent research shows that the quality of videoconferencing can be affected due to failed calls and audio/video jitter. 64 The evidence of the practical issues when introducing video consultations from the UK is only beginning to emerge, suggesting that establishing such services is complex because of disruption of routines in traditional clinic, and real and perceived information governance issues (see, for example VOCAL study findings 54 ). The introduction and implementation of videoconferencing services inevitably changes the clinical and administrative ways of working. The lack of training and support for clinicians and patients are often cited as barriers to the use of videoconferencing.65,66
Furthermore, with non-secure modes of communication such as Skype, the challenges surrounding information governance and compliance with legal and regulatory standards around privacy and data protection have further implications for how the communication is undertaken. There are inherent risks and ethical issues for clinicians and patients, not least around finding appropriate physical space for the video interaction and ensuring that that the technology works. The clinicians need to be aware of the risks associated with use of non-secure modes and make best efforts to minimise these risks, while also ensuring that the patient also understands the risks of sharing information in this way.
Finally, the research on internet videoconferencing is rapidly changing, terminology and modes of communication are becoming established and increasingly used in routine practice. Studies that have examined longitudinal changes in content within the internet videoconferencing literature show that publications on such modes of communication have moved from technical aspects to focusing more on patients and clinical applications. 67 While current evidence base for the use of videoconferencing is equivocal, it is likely to change as more research is undertaken and evidence published. With more videoconferencing services added in more contexts, research needs to explore how internet videoconferencing can be implemented in ways that it is valued by patients and clinicians, and how it can fit within organisational and technical infrastructure of the healthcare service.
Limitations of the study
Our review of reviews had some limitations. In order to retrieve a manageable number of records with a high chance of relevance, search terms focused on the specific technology of videoconferencing. More general terms, such as telehealth and remote consultation, that may be used to describe the use of a wide range of remote communication tools in this context, including videoconferencing, telephone, email, etc. (and are therefore also likely to retrieve a large number of irrelevant records), were not included. There is no guarantee that all relevant systematic reviews were retrieved. However, the use of the MeSH term ‘videoconferencing’ in the search, which was first introduced to
In addition to our review of literature, this study examined the NICE guidelines and identified where, in the patient pathway, the use of videoconferencing might be possible and of advantage. However, the pathway review presented challenges too. While the NICE pathways are generally considered a way of implementing evidence-based guidelines into practice, they are recommendations and should be used in conjunction with practitioner’s judgement and discussion with people using services. Therefore, we recognise that we may not have been able to summarise all the clinical functions for which internet videoconferencing may be useful, at best, the review reflects the possible opportunities for adoption or expansion of this mode of communication for patients with long-term conditions.
Conclusions
The evidence base for the use of internet videoconferencing for consultation between a healthcare professional and patient is growing, but there is still a lack of clear evidence relating to the impact on outcomes and cost. While internet videoconferencing appears to be feasible and acceptable to patients, there are unanswered questions about the ethics of these consultations and the actual implementation challenges.
Supplemental Material
Supplemental material for Internet videoconferencing for patient–clinician consultations in long-term conditions: A review of reviews and applications in line with guidelines and recommendations
Supplemental Material for Internet videoconferencing for patient–clinician consultations in long-term conditions: A review of reviews and applications in line with guidelines and recommendations by Agnieszka Ignatowicz, Helen Atherton, Celia Janine Bernstein, Carol Bryce, Rachel Court, Jackie Sturt and Frances Griffiths in Digital Health
Footnotes
Acknowledgements
The authors would like to acknowledge and extend their gratitude to Dr Frances Taggart for her contribution to the original LYNC study Skype review.
Contributorship
FG and JS led the LYNC study from design through to writing up study reports. HA led the systematic reviews component of the LYNC study. AI, HA, CJB, RC and CB undertook the review of reviews. AI and FG undertook the review of the NICE guidelines. AI, FG and JS drafted this paper. All authors reviewed, edited the manuscript and approved the final version.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was supported by the UK National Institute for Health Research, Health Services and Delivery Research Programme and forms part of the LYNC study project (project number 12/209/51).
Department of Health disclaimer: the views and opinions expressed herein are those of the authors and do not necessarily reflect those of the UK Health Services and Delivery Research Programme, NIHR, NHS, or the UK Department of Health.
Guarantor
AI
Peer review
This manuscript was reviewed by two individuals who have chosen to remain anonymous.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
