Abstract
Background
The impact of employee health on productivity in the workplace is generally evidenced through absenteeism and presenteeism. Multicomponent worksite health programmes, with significant online elements, have gained in popularity over the last two decades, due in part to their scalability and low cost of implementation. However, little is known about the impact of digital-only interventions on health-related outcomes in employee groups. The aim of this systematic review was to assess the impact of pure digital health interventions in the workplace on health-related outcomes.
Methods
Multiple databases, including MEDLINE, EMBASE, PubMed and PsycINFO, were used to review the literature using PRISMA guidelines.
Results
Of 1345 records screened, 22 randomized controlled trial studies were found to be eligible. Although there was a high level of heterogeneity across these studies, significant improvements were found for a broad range of outcomes such as sleep, mental health, sedentary behaviours and physical activity levels. Standardized measures were not always used to quantify intervention impact. All but one study resulted in at least one significantly improved health-related outcome, but attrition rates ranged widely, suggesting sustaining engagement was an issue. Risk of bias assessment was low for one-third of the studies and unclear for the remaining ones.
Conclusions
This review found modest evidence that digital-only interventions have a positive impact on health-related outcomes in the workplace. High heterogeneity impacted the ability to confirm what interventions might work best for which health outcomes, although less complex health outcomes appeared to be more likely to be impacted. A focus on engagement along with the use of standardized measures and reporting of active intervention components would be helpful in future evaluations.
Keywords
Introduction
Over the past two decades, the understanding of how employee health impacts productivity has advanced substantially.1–4 There is now a large body of evidence linking financial costs to employee health risks. This relationship is mainly defined by a loss of productivity driven by absenteeism and presenteeism. Absenteeism, defined as time away from work due to illness or disability, is a simple debt to calculate and has long been associated with lowered productivity.5–7 Presenteeism is slightly more complex in that it refers to time spent at work with decreased levels of productivity, which is often harder to measure. This lack of workplace performance can be due to mental or physical health issues, and it is often underestimated by organizations. 8 Both absenteeism and presenteeism are strongly correlated with unhealthy employee behaviours and status. Examples of these can include poor management of health conditions, obesity, insomnia, lack of physical activity or depression, all of which have been shown to have a detrimental economic impact on organizations.3,9–12
In addition, research has shown that many of the unhealthy lifestyle behaviours linked to reduced productivity are highly modifiable. Studies implementing interventions in the workplace designed specifically to address these behaviours have frequently shown health status improvements and consequent reductions in absenteeism and presenteeism in participants.13–17 The greater understanding of the causal link between employee health status and work performance metrics has resulted in a steady and sustained growth in employee focused health and well-being programmes. Once considered a ‘nice to have’ benefit, these programmes are now key to many organizations’ global investment and people management strategies. It has become commonplace for large organizations to conduct regular employee health risk assessments (HRAs) and to offer health promotion programmes to employees to address identified health issues. These programmes vary in length, composition and intensity, but are all designed to assess and promote an increase in healthy lifestyle behaviours, such as proactive stress management, better nutrition and greater physical activity.
The research literature suggests that the most successful approach to addressing employee health issues is through a multicomponent design.13–15,17–19 Multicomponent health interventions combine support from various sources such as health professionals, employee support groups, telephonic coaching programmes and most recently, web and mobile device-delivered applications. The advancement of digital technology over the last 20 years has penetrated almost every aspect of modern life, and health management is no exception. Digital health interventions have become increasingly popular within the health industry due to the ease with which they can be implemented and scaled to large and often dispersed populations. In addition, such an approach may be more cost effective compared with more traditional personnel-dependent programmes. Accessible through any internet-connected device, many organizations are using digital interventions to leverage support for the health and well-being of their employees. 20
Despite their popularity, one aspect that is not well understood about workplace health promotion programmes in the digital age is how much the digital element can itself, or as part of a multicomponent intervention, contribute to the overall programme efficacy and improved health outcomes. To address this question and the gap in the literature we conducted a systematic review of current peer-reviewed research of workplace-based ‘digital only’ interventions, which we hope will be a valuable resource for researchers and programme developers alike.
The main objective of this review was to assess the impact of digital health interventions in the workplace on health-related outcomes. This review implemented a conservative definition of digital interventions to exclude studies that included any form of employee support that was non-digital.
Methods
This review followed the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) statement 21 and is registered with PROSPERO (registration: CRD42017059621). 22
Eligibility criteria
Studies that were randomized controlled trials (RCTs), including pilots, reported in English, assessing the impact of digital health interventions in the workplace, with at least one primary outcome being health related were included. Participants recruited were eligible if they were aged 18 years or above and were employees. Digital interventions were considered eligible if they delivered through the use of a computer, tablet, smartphone or email, either as a website, app or downloadable software.
Digital interventions, which included further support such as meetings, health counselling or direct feedback from a health professional or coach (even those delivered digitally), were considered not purely digital and therefore were not included, as it was not possible to discern the impact of the digital component. The exception to this was the introduction of the intervention to participants or follow-up reminder for data collection, which were often conducted with human support for research purposes. Finally, interventions incorporating the use of wearable technology were not considered eligible as self-monitoring wearable devices can be considered a separate intervention on their own.
There was no limit to length or duration of interventions included within this review and outcomes were any health-related measure, including those quantifying physical or mental health, illness symptoms and health-related lifestyle behaviours.
Search strategy
Electronic databases including MEDLINE, EMBASE, PubMed, PsycINFO and CINAHL were searched for studies published up to and including December 2017. The search strategy was based on the PICO (population, intervention, comparison and outcome) strategy, 23 with the language restriction of English. Reference lists of eligible studies were screened for further papers meeting the inclusion criteria. Databases were searched using a combination of the key words such as: ‘work*’, ‘occupational’, ‘digital’, ‘web’, ‘internet’, ‘apps’, ‘well-being’, ‘health’, ‘intervention’ and ‘treatment’. Terms were based on MeSH indexing as well as free text terms (see supplementary File 1 for a full list of search terms and combinations).
Data collection and extraction
Using the predefined criteria, all searches were conducted by the first author (AH) based on abstract and title. Results were then screened independently by two authors (AH and PM) who rated the eligibility of the records to confirm relevant papers. Full texts for papers rated as relevant or potentially relevant were then retrieved and reviewed by two authors (AH and PM) to determine final eligibility. Any studies that were disagreed upon were discussed, and a consensus was reached for all articles included.
A data extraction of the following fields was then used to summarize the key points of the eligible studies: first author name, publication date, country, design and aim, participant characteristics (including age, gender and employment detail), type of intervention, type of comparison, main outcome measures and results (i.e. effects of interventions on outcomes). The extraction was conducted by AH and verified by SJ, JC and PM.
Assessment of quality
Methodological quality of the included studies was assessed for those with an RCT design using the Cochrane Handbook for Systematic Reviews of Interventions. 24 The handbook recommends using the Cochrane risk of bias tool 25 to allocate a risk of bias classification for each study. Grading with this approach was dependent on certain issues affecting bias such as reporting of randomization, blinding and allocation concealment and whether outcome measures were fully reported. Each study was reviewed by two authors (AH and PM), given an overall risk of bias grade of low, unclear or high and then discussed for consensus if there was disagreement in grading.
Analysis
Meta-analysis was not considered a feasible option based on the included studies, as there was a lack of the required homogeneity across outcome measures. 24 A narrative approach was therefore used to summarize findings.
Results
Selection of studies
The search identified 1354 papers and these articles were then screened using the inclusion criteria as illustrated by the PRISMA flow diagram
21
below (see Figure 1) by two authors (AH and PM). Duplicates were removed, and initial screening based on title and abstract resulted in 101 articles deemed eligible. Full-text articles for these records were then obtained and reviewed by two authors (AH and PM). From this process, a further 79 articles were excluded. The majority ( PRISMA flow diagram illustrating screening of studies.
Study characteristics
Overview of included studies.
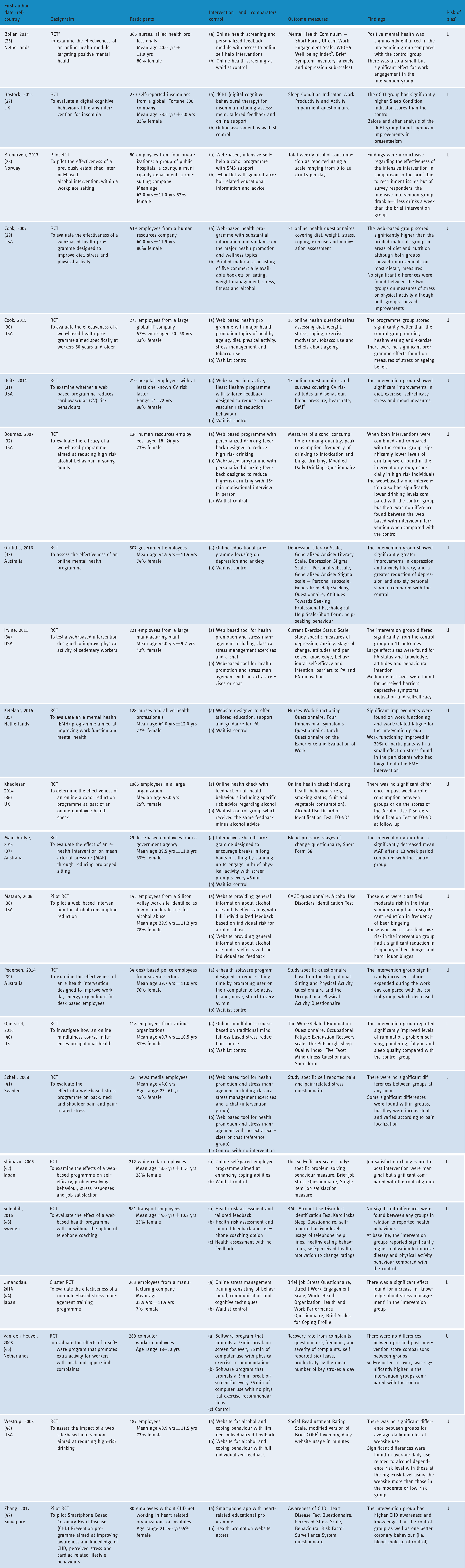
Randomized controlled trial (RCT).
WHO-5 Well-being Index (World Health Organization 5-item well-being index).
L: low risk of bias; U: unclear risk of bias.
BMI (body mass index).
EQ-5D (European Quality of Life-5 Dimensions).
COPE (Coping Inventory).
Summary of intervention characteristics of included studies.

Short messaging service (SM).
Body mass index (BMI).
Participant characteristics
The mean age of participants was 42 years (SD = 6.5 years) with over 90% being less than 50 years old and more than two-thirds being between 40 and 50 years of age. As the review inclusion criteria was a workplace setting, all participants were employees. Ethnicity was generally not specified with instead the location of the study being the only indication of participant nationality. Of the 22 studies, the gender ratios were tipped towards female participants with the average proportion of females in studies being 69%.
Participants were recruited from a variety of workplaces including public and private offices, academic or hospital settings and manufacturing plants. The majority of studies (
Over a quarter of the studies (
Attrition rates
Using available data reported within each study, attrition rates were calculated based on numbers at baseline compared with those included in the final analysis. Attrition rates ranged from 0 to 60%, with a median rate of 21%, but two studies stood out with no participants withdrawing,37,39 both of which included interventions aimed at reducing sitting time for desk-based employees. In contrast, the two studies35,44 with the highest attrition rate (i.e. 56% and 60%) were aimed at improving mental health and stress management.
Intervention characteristics
The contents of the interventions varied considerably (see Table 2) but most (n = 17) were formatted much the same way in that they included an assessment (e.g. screening) and individualized feedback based on the results of the assessment.26,28–33,35,36,38,41–47 The feedback component within these interventions usually consisted of a website with health and education information and/or interactive sessions to improve the targeted behaviour or outcome. The remaining interventions were specific software programs aimed at reducing sedentary behaviour in the work place (
While some interventions were introduced with human (e.g. researcher) contact, all participation with the actual intervention was digital, usually accessed with a private code or password once the employee consented to participate. Tailored feedback generated ranged from generic information related to response options chosen by participants during health or well-being screenings to fully individualized recommendations, homework, personal challenges or online diaries. Push notifications and encouraging emails automatically sent at certain stages throughout interventions were included within 50% of studies.
Just over half of the reviewed studies (
Duration of interventions
The average length of the interventions in the studies included was 3 months (median = 12 weeks) with nine being exactly 12 weeks in length26,29,30,36–39,42,46 and 10 studies running from 2 to 8 weeks.27,31–35,40,44,45,47 Of the three studies that had interventions that ran for longer, two ran for 6 months28,41 and one study had a general health behaviour intervention that was available to participants for 9 months. 43
Control and comparisons
There were a variety of control and comparison types used for the studies reviewed, all of which were time matched in length. More than half of the reviewed studies (
Outcome measures
Most studies used a mix of different outcome measures including physical, psychological, biological, behavioural or work measures. There were 30 instances where standardized measures were used, which are detailed in Table 1, but many measures were study specific to adapt to the digital nature of the intervention.
Physical measures
Physical health measures were both self-reported and biometric with 19 instances in total (see Table 1). The outcomes included self-reported measures of sleep, physical activity levels and healthy lifestyle rating as well as biological measures of heart rate, blood pressure and body mass index (BMI).
Psychological measures
The total number of instances of mental or well-being related measures was 25. These measures (see Table 1) ranged from perceived motivation ratings to self-efficacy scales with the most common being measures of anxiety and depression (
Other health-related measures
As per Table 1, most studies used a combination of health measures, which largely reflected the variety of study aims undertaken. This included health-related measures focused on alcohol and eating behaviours, website usage, logged activity counts and even productivity by daily mean number of keystrokes on a work computer keyboard. The total instances of occupational measures related to health was 17 with standardized measures such as the Brief Job Stress Questionnaire, 50 the Utrecht Work Engagement Scale 51 and the Work Productivity and Activity Impairment 52 questionnaire being common examples.
Design and aims of studies
All studies included in the review were RCTs, three of which were pilot RCTs28,38,47 and three clustered RCTs.26,44,45 Across the studies, the combined number of participants randomized was 6168. Sample sizes ranged from 29 to 1066 participants, with a median of 216. Less than one-fifth of studies randomized under 100 participants28,37,39,47 and two of these were pilots, which therefore aimed to recruit a smaller sample.46,47 Almost half (
Most of the studies (
Intervention effects
Out of the 22 studies reviewed, almost half (
Mixed and negative findings
The studies reviewed (
The remaining studies with mixed results (
Risk of bias
Of the 22 studies, seven were classified as having a low risk of bias26–28,37,40,41,44 based on qualities such as clearly defined randomization process reporting, appropriate blinding of group allocation where possible and complete reporting of all outcomes stated in the methods. The remaining studies (
Excluded studies
Throughout the study selection process, a total of 11 studies were found to be highly relevant but not eligible due to the inclusion criteria. Six of these studies included human input supplied in the form of health care professionals, such as physicians or counsellors, who were accessible in person or by phone, text or email.16,19,54–57 Another four studies did not report health-related outcomes and instead reported engagement and acceptability outcomes.53,58–60 One study was a cost analysis study that reported health care cost results with no data on specific health-related outcomes. 61
Discussion
The purpose of this systematic review was to assess the impact of digital health interventions in the workplace on health-related outcomes of employee participants. A key eligibility factor for study inclusion was the use of digital-only interventions so as to better discern the effect of the digital component. The final selection of articles was 22 RCTs covering a broad range of interventions and measured outcomes. Significant improvements were found in all studies but one, for at least one health-related outcome, although more than half of the studies had a mix of both positive and negative findings. The interventions varied in content, but most were formatted as a combination of an initial assessment followed by access to a website. Three of the studies differed slightly in approach; two used specific software programs downloaded on to work computers and one used a smart phone app. Although the study designs were all RCTs, three were pilot RCTs and three were cluster RCTs. These were considered eligible as they were randomized and included at least one primary health-related outcome. The quality of the studies included was adequate based on risk of bias assessment using the Cochrane risk of bias tool.
A high level of heterogeneity across the studies in terms of intervention aims, content, measures and overall outcomes made it difficult to compare or discern patterns of impact among the 22 included studies. However, from the group of nine studies that reported positive significant improvements for a primary health-related outcome, it would appear interventions that targeted specific health behaviours, such as being sedentary in the workplace, were especially engaging and effective. The two studies that exemplify this both used an intervention labelled ‘Exertime’.37,39 Both articles reported a 0% attrition rate, unmatched in this respect by any other intervention reviewed. It is worth noting that the ‘Exertime’ studies had substantially smaller samples sizes (ranging from 29 to 34 participants) compared with most of the other studies and it is therefore not clear whether this observed impact would be replicated in larger, more dispersed populations. It is clear, however, that the combination of intervention design and implementation garnered impressive engagement over the 12- to 13-week study period. This was potentially due to the ease with which the intervention, consisting of short and simple tasks, was integrated into participants’ daily workflow creating a high opportunity, low demand situation for the behaviour change to occur. Further supporting this type of approach was another study using a programme called ‘Get Moving’. 34 This intervention also aimed to improve sedentary work behaviour and reported significant findings and a low attrition rate of only 5%.
The concept of targeting a specific area of health to drive efficacy and outcomes was evidenced by two other studies with positive significant findings. These studies were aimed at improving insomnia in one instance 27 and heart healthy behaviour in the other. 31 Both were successful with sample sizes of over 200 participants and attrition rates lower than 25%, closer to the average rate for digital health interventions in general. 62
In contrast, studies targeting complex, and sometimes multifactorial, health-related behaviours did not appear to be as efficacious. An example of this was a collection of five studies that included interventions aimed at improving alcohol-related behaviours. Of these studies, four had significant findings but only within certain contexts. The first two studies38,46 found improvements for specific groups (e.g. moderate or high-risk alcohol groups) and for specific types of drinking behaviours (e.g. bingeing). As one of these studies 46 used website usage as an outcome measure, it is difficult to tell if this translated into actual behaviour change. The third study 32 had a significant result but only when two intervention arms were combined and compared with the waitlist control group, and the fourth study 28 found a significant difference between groups, but this effect disappeared when a sensitivity analysis was conducted to account for missing data. This highlights a major issue with evaluating any intervention that has a high attrition rate. The final study 36 had non-significant findings even though it utilized an intervention much the same as the previous four studies (i.e. online screening and tailored feedback specific to drinking) and resulted in the intervention group having an increased weekly average alcohol consumption of 5.6%.
Based on the studies within this review, it would appear that purely digital interventions are most beneficial when firmly embedded into the work environment (e.g. downloaded as software directly onto a work computer) and are restricted to targeting specific health behaviours that are routinely conducted during working hours (e.g. physical activity, eating). In the case of more complex health issues, especially ones where the health behaviours extend outside the workplace environment, a purely digital intervention may not be adequate and a multicomponent intervention, including human support, may be a better approach. 63
Limitations and future directions
Although the included studies were of robust design (i.e. RCTs), the frequent use of non-standardized outcome measures made attempts to draw comparisons between outwardly similar studies difficult, which is a limitation of the review overall. The results from the alcohol studies demonstrate the difficulties of assessing the impact of digital interventions in the workplace, especially when targeting complex health behaviours. Perhaps mirroring some of the same issues, many of the studies within this review reported both positive and negative results, making it difficult in particular to formulate conclusions in relation to which type of intervention is effective for which outcome. In addition, attrition rates (ranging from 0 to 60%) raise questions as to whether engagement or the measures used for quantifying outcomes were influencing results. An in-depth focus on engagement together with the use of standardized measures and better reporting of ‘active’ intervention components would strongly enhance future evaluations and perhaps allow for meta-analysis.
Conclusions
Existing evidence suggests that workplace digital health interventions show promise as a method for improving various aspects of employee health. This review systematically assessed current available research investigating purely digital interventions in the workplace. It is clear that more research is needed as a strong foundation of evidence is currently lacking. Many recently developed health interventions have begun to use the behaviour change taxonomy developed by Michie et al. (2013) 64 and future research should include the reporting of the ‘active’ components of interventions to help clarify how programmes are working. This together with the use of standardized measures will make it easier to demonstrate the type of interventions that are most efficacious for different health-related behaviours.
In addition, further investigation of intervention engagement is necessary. Investigators should address engagement early on in programme design as well as throughout implementation and evaluation. This approach, alongside the inclusion of measures that more clearly translate into return on investment (ROI) metrics, may be beneficial to many employers looking to quantify the value of workplace digital health interventions.
Finally, this review highlights the scalability of digital workplace interventions for improving health-related outcomes. Although there is evidence suggesting multicomponent interventions are superior in supporting employee health and well-being enhancement, further investigation of the digital components of these programmes is necessary. With smartphone internet access now surpassing traditional computer-based access, it would be advantageous for new studies to explore the efficacy of this particular medium. As mentioned earlier, only one study 47 in this review included a smartphone app as part of the intervention. Considering that the number of health apps available worldwide exceeded 318,000 last year, 65 it may be that evaluating existing smartphone apps in an employee population could be the next step in establishing the impact of digital health interventions within the workplace.
Supplemental Material
Supplemental material for The impact of digital health interventions on health-related outcomes in the workplace: A systematic review
Supplemental material for The impact of digital health interventions on health-related outcomes in the workplace: A systematic review by Ana Howarth, Jose Quesada, Jessica Silva, Stephanie Judycki and Peter R Mills in Digital Health
Footnotes
Contributorship
JQ, PM and AH conceived and designed the study. AH with the assistance of PM, SJ, JS and JQ, contributed to data extraction, conducted the analyses, and drafted and revised the manuscript. All authors read and approved the final manuscript.
Conflict of interest
All authors are either directly employed or contracted by Cigna Corporation, or one of its subsidiaries, which develops and markets a variety of health interventions. The authors declare that they have no conflicting interests.
Ethical approval
Not applicable.
Funding
This work was supported by Cigna Global Wellbeing Solutions Ltd, UK.
Guarantor
AH was the guarantor.
Peer review
This manuscript was reviewed by two reviewers who have both chosen to remain anonymous.
Supplementary Material
Supplementary material is available for this article online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
