Abstract
Case summary
A 12-year-old castrated male domestic shorthair cat was referred for investigation of lethargy, hindlimb weakness with plantigrade stance and ventroflexion of the neck. The cat was fed a balanced diet and had received methylprednisolone acetate at a dose of 20 mg intramuscularly every 6 months for 6 years. On blood work, severe hypokalaemia and marked elevation of muscle enzymes were noticeable. The findings were suggestive of hypokalaemic myopathy. Urine fractional excretion of potassium (FEk) was moderately high (9.04%), and serum aldosterone was below the reference interval. An adrenocorticotropic hormone (ACTH) stimulation test was compatible with adrenal suppression. Upon hospitalisation, the patient was given intravenous (IV) Ringer lactate solution supplemented with potassium chloride and oral potassium citrate. The serum potassium concentration normalised by the fifth day of hospitalisation; therefore, IV potassium supplementation was suspended. The cat was discharged with oral potassium and the dose was gradually reduced over time. After 4 months, the cat was clinically normal; the serum potassium concentration remained within the normal range and the adrenal glands showed some response to ACTH stimulation. Potassium supplementation was therefore discontinued. One month later, the serum potassium concentration was still within normal limits and at the time of writing (7 months after presentation), no clinical signs had reoccurred.
Relevance and novel information
This report describes a case of hypokalaemic myopathy associated with iatrogenic hypercorticism in a cat. This condition was successfully treated with supplementation of potassium and a complete clinical remission was achieved within 4 months.
Keywords
Case description
A 12-year-old castrated male domestic shorthair indoor cat was presented for lethargy, reluctance to jump, hindlimb weakness with plantigrade stance and ventroflexion of the neck (Figure 1) of 1 day’s duration. The cat had been treated with methylprednisolone acetate (Depo-medrol 40 mg/ml; Pfizer) at a dose of 20 mg intramuscularly (IM) twice a year for 6 years, for seasonal pruritus. The most recent dose was administered 25 days before presentation. The cat was fed a hydrolysed diet (Anallergenic; Royal Canin) for suspected skin allergy.

The patient at presentation: the cat showed hindlimb weakness, plantigrade stance and ventroflexion of the neck
On physical examination, the patient had a depressed mental state and was reluctant to move. The body condition score was 6/9. The coat was normal. The systolic blood pressure, measured by Doppler, was 220 mmHg; the fundic examination was normal.
Haematology, biochemistry, venous blood gas analysis and urinalysis were undertaken (Tables 1 and 2). Biochemistry (BT3500 Plus vet; Futurlab) showed a marked increase in creatine kinase (CK) activity (6911 U/l; reference interval [RI] 91–326), a moderate increase in aspartate aminotransferase activity (123 U/l; RI 15–35) and a mild increase in lactate dehydrogenase activity (316 U/l; RI 63–273) and alkaline phosphatase (ALP) activity (83 U/l; RI 19–70). A transient hyperglycaemia (100–245 mg/dl; RI 72–136) was also noticed. The serum total thyroxine (TT4) level was found to be within the normal RI.
Haematological and biochemical parameters in the cat at presentation and after 4 months

HPF = high-power field; RI = reference interval
Admission and follow-up venous blood gases in the cat
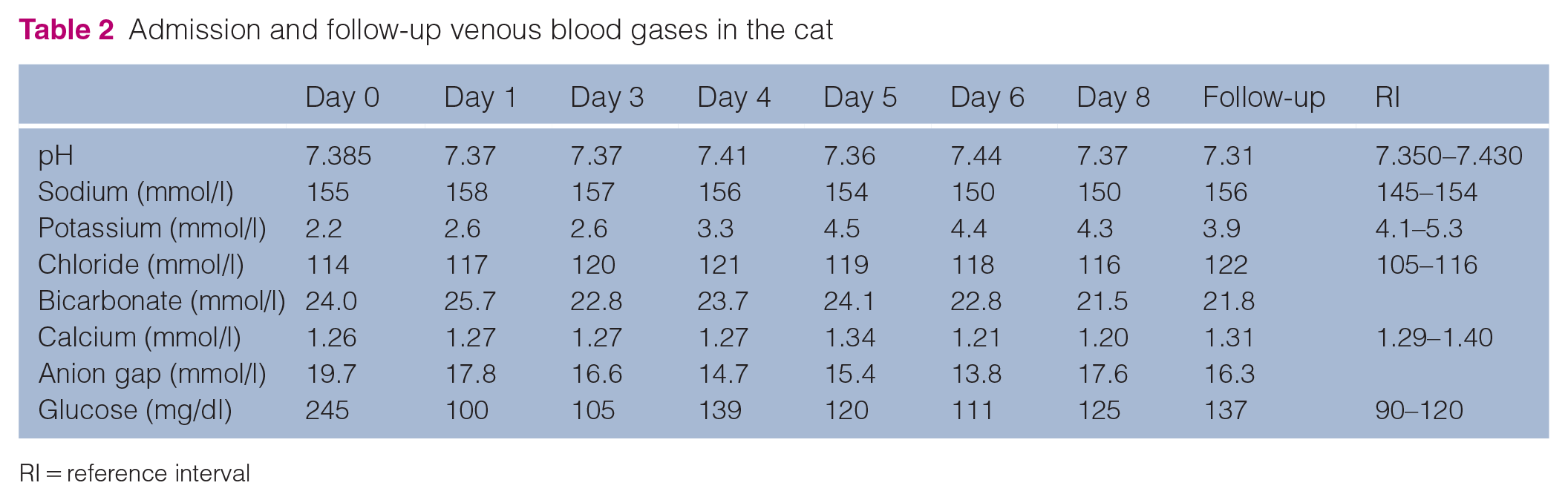
RI = reference interval
Venous blood gas analysis (ABL90 Radiometer) revealed severe hypokalaemia (2.2 mmol/l; RI 4.1–5.3) and mild hypocalcaemia (1.26 mmol/l; RI 1.29–1.4). Urinalysis showed a urine specific gravity (USG) of 1026, with neither glycosuria nor ketonuria. Urine protein:creatinine ratio (UPC) was borderline (0.4; RI <0.2). Urine fractional excretion of potassium (FEk) was 9.04%.
These findings were suggestive of hypokalaemic myopathy. The patient was hospitalised and given intravenous (IV) fluid therapy (Ringer Lactate 500 ml; SALF SpA) at a maintenance rate (2 mg/kg/h) supplemented with potassium (Potassium chloride 2 mEq/ml; Monico) and oral potassium citrate (1 g PO q12h; Karenal Pet NBF Lanes).
The next day, an abdominal ultrasound was performed (Affiniti 50G; Philips) (Figure 2a,b). The cat was sedated with butorphanol (0.3 mg/kg IM, Nargesic 10 mg/ml; ACME srl) and alphaxalone (0.4 mg/kg IM, Alfaxan 10 mg/ml; Jurox). The dorsoventral axis diameter of the caudal pole of the left and right adrenal gland measured 0.16 cm and 0.17 cm, respectively (Figure 2a,b). An adrenocorticotropic hormone (ACTH) stimulation test was performed after IM administration of 125 µg of synthetic ACTH (Cosacthen 0.25 mg/ml; Dechra). The results were compatible with adrenal suppression (Table 3); glucocorticoid supplementation was not started, because of the long-lasting effects of methylprednisolone acetate.

The dorsoventral axis of the caudal pole of the (a) left and (b) right adrenal glands at presentation and the dorsoventral axis of the caudal pole of the (c) left and (d) right adrenal glands after 4 months
Adrenocorticotrophic hormone stimulation test at presentation and after 4 months

RI = reference interval
Basal aldosterone value was below the RI (<20 pmol/l; RI 87–224). Folate (22.8 ng/ml; RI 11.1–21) and vitamin B12 (1117 pg/ml; RI 269–1333) were overall within normal limits.
On the fifth day of hospitalisation, the potassium concentration normalised (4.5 mmol/l) and blood pressure was within the RI. The cat showed a normal appetite and gait; therefore, IV potassium supplementation was suspended.
Just before discharge, the patient developed persistent hyperthermia (>40°C). On examination of the right front limb (where the IV catheter was), there was pain to touch and warmth of the skin; phlebitis was suspected, so the cannula was removed from the affected leg. As the cat showed ongoing depressed demeanour, blood tests were repeated (Table 4). Despite the neutrophil count being within the normal range, a blood smear evaluation revealed a marked increase of band neutrophils and toxic neutrophils. Biochemistry showed mild hypoalbuminaemia (2.2 mg/dl; RI 2.3–3.9) and a marked increase in serum amyloid A (SAA, 107 mg/l; RI 0–1.5). Venous blood gas analysis revealed mild hypocalcaemia (1.20 mmol/l). The cat was started on antibiotics (enrofloxacin 5 mg/kg IV q24h, Xeden 50/ml; Ceva, and metronidazole 10 mg/kg IV q12h, Deflamon 500 mg/100 ml; SPA), because of the suspicion of systemic infection.
Haematological parameters at the onset of hyperthermia (5 days after presentation) and at follow-up

1+ = mild; 2+ = moderate; 3+ = marked; RI = reference interval
The next day, leukocytosis, neutrophilia, left shift and toxic neutrophils were noticeable. A blood culture was performed and it was negative.
After 5 days of antibiotics, given complete clinical improvement, the cat was discharged on enrofloxacin 5 mg/kg PO q24h (Baytril 50 mg; Bayer) and oral potassium citrate 0.5 g PO q24h.
At 17 days after presentation, haematology and SAA showed a marked improvement (Table 4). Antibiotic therapy was suspended, and the oral supplementation of potassium was continued at 0.25 g PO q24h.
Four months later, the cat presented with a normal gait and good muscle tone (Figure 3). The pruritus was successfully controlled with off-label use of oclacitinib (5.4 mg PO q24h, Apoquel; Zoetis). Venous blood gas analysis revealed minimal changes. Urinalysis showed a USG of 1032 and UPC of 0.2. Another ACTH stimulation test was performed (Table 3): basal cortisol was higher than previously and the adrenal glands responded to the ACTH administration. An abdominal ultrasound showed that the dorsoventral axis of the caudal pole of the left and right adrenal gland measured 0.24 cm and 0.36 cm, respectively (Figure 2c,d).

The general appearance of the patient at re-examination (4 months later). The cat presented normal muscle tone and gait
Given the results, the oral potassium supplementation was suspended. One month later, the serum potassium concentration was still within the RI (4.2 mmol/l). At the time of writing (7 months after presentation), the cat was clinically normal, without oral potassium supplementation.
Discussion
The causes of hypokalaemia in cats are decreased intake, translocation into cells and increased gastrointestinal or renal losses (in the last instance, examples are hyperaldosteronism, chronic kidney disease and diabetes mellitus).1,2
Muscle weakness may develop when the serum potassium concentration drops to <3.0 mEq/l while increased CK concentration is usually evident when serum potassium concentration is <2.5 mEq/l and rhabdomyolysis with respiratory muscle paralysis may occur when serum potassium concentration is <2.0 mEq/l. 3 The cat in this study showed weakness, ventroflexion of the neck, plantigrade stance and markedly increased CK, due to severe hypokalaemia (2.2 mmol/l) as reported in the literature.4 –9
FEk can be used to help localise the source of potassium loss as, according to the literature, it should be <6% in the case of extrarenal loss.1,8 In our patient, FEk was 9.04%; therefore, an extrarenal loss was considered unlikely. 9
Potassium depletion has been reported in up to 17% of feline hyperthyroidism cases and is thought to be related to increased potassium uptake by the cells due to potentiated Na+-K+-ATPase pump activity. 2 This condition was considered unlikely in our case, owing to a normal TT4 concentration and no compatible clinical signs. Diabetes mellitus was also considered unlikely as there was no glycosuria, despite the detection of a transient, probably stress-related, hyperglycaemia. Considering severe but transient hypertension in the absence of target organ damage (probably due to the ‘white-coat effect’) and the small size of the adrenal glands, naturally occurring hyperaldosteronism was also ruled out, and this was further supported by the low serum aldosterone level, which is a physiological response to hypokalaemia. 6 Finally, chronic kidney disease and renal tubular acidosis 10 were not considered possible differential diagnoses because of the normal bicarbonate level and blood pH. Furthermore, USG normalised once normokalaemia was re-established, in favour of a transient polyuria and polydipsia since hypokalaemia decreases the renal response to antidiuretic hormone. 6
Based on the above results, the most likely differential diagnosis was iatrogenic hypercorticism (IHAC) causing hypokalaemic myopathy secondary to the mineralocorticoid effects of corticosteroids on the kidneys.11 –15 Cortisol has high affinity for the mineralocorticoid receptors; however, in vivo, cortisol is converted into cortisone, which has mild mineralocorticoid effects.2,16 In this case, it was suspected that the high-dose long-term steroid therapy might have bypassed this mechanism, leading to a pronounced mineralocorticoid effect.
The diagnosis of IHAC is uncommon because cats are thought to be resistant to prolonged administration of glucocorticoids. 14 Common clinical signs include abdominal enlargement, muscle wastage, poor hair coat and skin fragility with curled pinnae.14,17,18 Interestingly, in our study, the cat presented with clinical signs solely attributable to the severe hypokalaemia.
A previous study described cases of IHAC that developed a mean of 8.3 months after parenteral, oral or topical use of corticosteroids began. 13 Another report described the onset of feline hypercorticism after a considerably shorter period. 14 In contrast, a retrospective study found no signs of hypercortisolaemia in 25 cats that had received non-immunosuppressive doses of parenteral methylprednisolone acetate (10 mg/cat) for at least 3 years. 19 In our study, the cat had received steroids for 6 years before developing clinical signs.
In the literature,11,13,15 the most reported biochemical abnormalities are elevation of alanine transaminase and ALP, hyperglycaemia with concurrent diabetes mellitus, hypercholesterolaemia and hypertriglyceridaemia. In our study, as well as elevated CK, we found a mild increase in ALP, likely due to steroid-induced hepatopathy as has been described previously. 12 Furthermore, in spontaneous hyperadrenocorticism, up to 13% of cats showed mild hypocalcaemia, as detected here, while a separate case report showed marked hypercalcaemia.11,18
At the time of the episode of hyperthermia, the clinicopathological abnormalities were suggestive of an acute phase response to an inflammatory injury. This may have been secondary to immunodepression, caused by prolonged steroid administration, which could have increased the patient’s susceptibility to infections.20 –25 Despite the use of enrofloxacin in cats being rarely associated with acute retinal degeneration, 22 it was selected in this case because of the lack of a readily available, less retinotoxic, alternative. SAA is an extremely useful marker in monitoring treatment response23,26 as in the case here, where its normalisation was accompanied by the resolution of the neutrophil toxicity and clinical remission. In our case, it was not possible to identify a bacteraemia as the blood culture was negative; however, the blood sample was collected after starting the antimicrobial therapy and this could have jeopardised the results.
Lastly, there is little information about the efficacy and appropriate dose of oral potassium supplementation in cats; however, a previous study described the administration of oral potassium as an effective treatment for hypokalaemia. 27 The same study did not find a significant difference between the use of potassium gluconate and potassium citrate. 27 In the case presented here, oral supplementation of potassium citrate was commenced and the dose was gradually tapered down before being stopped once blood tests indicated a response by the adrenal glands to ACTH administration.
Conclusion
This study describes the first clinical report of feline IHAC after long-term administration of methylprednisolone acetate IM, which presented with generalised weakness due to severe hypokalaemia. It also demonstrates how the patient was successfully treated with the supplementation of oral potassium which led to complete clinical remission, still ongoing at the time of writing, with no oral potassium supplementation. Complications due to methylprednisolone acetate have been rarely reported in the literature, possibly due to the disbelief that cats are resistant to the side effects of glucocorticoids and this case report should serve as an eye-opener that, corticosteroids should be cautiously used in cats.
Footnotes
Conflict of interest
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
The work described in this manuscript involved the use of non-experimental (owned or unowned) animals. Established internationally recognised high standards (‘best practice’) of veterinary clinical care for the individual patient were always followed and/or this work involved the use of cadavers. Ethical approval from a committee was therefore not specifically required for publication in JFMS Open Reports. Although not required, where ethical approval was still obtained, it is stated in the manuscript.
Informed consent
Informed consent (verbal or written) was obtained from the owner or legal custodian of all animals described in this work (experimental or non-experimental animals, including cadavers, tissues and samples) for all procedures undertaken (prospective or retrospective studies). No animals or people are identifiable within this publication, and therefore additional informed consent for publication was not required.
