Abstract
Background:
Patients who experienced acute kidney injury (AKI) may benefit from dedicated care following hospital discharge. Most of these patients will be followed by primary care providers. There is a lack of data on current practices and comfort for these care providers when offering post-AKI care.
Objective:
We surveyed nurse practitioners and family physicians to assess their awareness, perceptions, practice patterns and comfort regarding post-AKI care.
Design/Setting:
We distributed a web-based self-administered survey among clinicians from the Province of Quebec. We asked about their awareness and perceptions on how AKI should be disclosed and followed, the barriers encountered regarding the process of care following hospital discharge, and their level of comfort and expertise in offering dedicated post-AKI care. The survey integrated direct and scenario-based questions and was conducted from December 2022 to April 2023.
Participants:
We distributed the survey to practicing family physicians and nurse practitioners through the mailing list of the Fédération des Médecins Omnipraticiens du Québec, and the Association des infirmières praticiennes spécialisées du Québec, respectively. No incentives were provided.
Methods:
We conducted descriptive analyses and used chi-squared analysis to compare responses between family physicians and nurse practitioners and between hospital-based and cabinet-based practice.
Results:
The survey was opened by 779 potential participants. Of these, the response rate was 9% (70/779). Most participants were family physicians (79%) and dedicated 70% (±32) of their time in community outpatient clinics. Participants reported that 59% (±20) of all patients seen daily had at least 1 risk factor for AKI, whereas they estimated that 21% (±12) of recently discharged patients suffered from an AKI episode. The lack of awareness by the patient and lack of details on the discharge summary were the barriers most frequently reported impacting the overall process of care at follow-up. Most nurse practitioners (60%) and 33% of family physicians reported at least some levels of discomfort and lack of expertise when offering post-AKI.
Limitations:
The generalizability of our study is limited by its response rate. However, this is comparable with typical response rates seen in electronic surveys. The distribution was limited to a single province of Canada.
Conclusions:
We reported significant barriers regarding the hospital-to-community transition of care in patients who experienced AKI and the suboptimal comfort and expertise of primary care providers when offering dedicated post-AKI care. This reflects the need to improve communication, collaboration, and AKI training with primary care providers.
Introduction
Acute kidney injury (AKI) occurs in up to 20% of all hospitalized patients and more than 50% of critically ill patients. 1 This common clinical syndrome is associated with increased morbidity, mortality, and cost of care.2-6 The interaction between AKI and chronic kidney disease (CKD) progression is now better characterized,4-7 but the follow-up care suggested is still mostly based on expert recommendations.3,8 As an example, the Kidney Disease: Improving Global Outcomes AKI guidelines provide non-graded evidence advice for post-AKI management, simply focusing on the need that patients with AKI should be re-evaluated within 3 months. 9 Epidemiological data have shown that patients who experienced AKI are at higher risk for long-term albuminuria, CKD, hypertension, and cardiovascular events.4,5,10,11 Of note, a meta-analysis concluded potential long-term survival benefits when severe AKI patients were managed by nephrologists at discharge, 12 which at least partially validates the importance of offering dedicated care to these patients.
Survivors of critical illness complicated by AKI often have multiple hospital providers inside and outside of the hospital, which may be a barrier to effective transition of care from the hospital to the community once discharged. Recent epidemiological data from Alberta have shown that only 64% of discharged critically ill patients with AKI had an outpatient creatinine measurement within 3 months, and one quarter had urine protein measurement despite recommendations. 8 Notably, most follow-up visits (89%) were performed by family physicians (FPs), and only 5% of these AKI survivors had a follow-up performed by nephrologists, 8 confirming the need to involve primary care providers in such care.
Post-AKI care, including the recommended post-AKI workup for potential metabolic and nephroprotective interventions, remains unfamiliar to numerous medical providers due to its relative novelty. 3 Offering best practices for patients post-AKI should not be limited to nephrologists within dedicated clinics, 13 but should instead be integrated into the overall process of care which includes primary care providers. However, before making any advice on how such post-AKI care should be implemented by FPs and nurse practitioners (NPs), there is a need to explore current practice patterns, awareness, and day-to-day barriers of offering such dedicated care.
We, therefore, conducted a comprehensive survey targeting primary care providers to understand (1) their awareness and perception of how AKI should be followed and disclosed to patients, (2) the barriers encountered regarding hospital discharge follow-up, and (3) the current level of comfort and expertise to offer dedicated post-AKI care to such patients.
Methods
We conducted a web-based self-administered survey distributed across the Province of Quebec, the second largest province of Canada (~8 millions). The survey targeted primary care providers involved in the care of patients recently discharged from hospitalization. The survey was developed in accordance with current recommendations14,15 and was approved by the ethics committee of the Centre Hospitalier de l’Université de Montréal (#2023-11017).
The survey aimed to include FPs and NPs involved in the longitudinal care of patients discharged from hospitalization who might have been affected by AKI episodes. A specific focus has been made on identifying clinicians’ practice patterns regarding in-hospital vs cabinet and community-based clinical activities.
We followed current recommendations for survey research methodology and reporting from Canadian and international guidelines.14,15 To develop the survey, we assembled a panel of 4 investigators (3 nephrologists [J.-M.C, J.B., and W.B.-S.] and 1 FP [L.H.]) with experience in epidemiology, nephrology, post-AKI care, and longitudinal follow-up. Responses were in binary, multiple choice, or ordinal format (Likert scales). Respondents had the option of completing the survey in French or English. The survey was pretested among investigators and 4 additional respondents (FPs and fellows). After this pilot phase, the survey was optimized for presentation, readability, rapidity of completeness, and relevance. The final survey consisted of 23 questions and scenarios.
Our survey was distributed using a web-based survey tool (RedCAP) from December 2022 to April 2023 and was available for completion for an additional period of 2 months following a last reminder sent in March 2023. Our survey included a cover letter signed by the organizing team explaining the purpose of the survey and mentioning that participation was anonymous. The survey used non-probability sampling and was disseminated through the mailing lists of 2 contact networks: the Fédération des Médecins omnipraticiens du Québec (n~9500) and the Association des infirmières praticiennes spécialisées du Québec (n~1300), representing, respectively, all FPs and NPs of the Province of Quebec. We did not set a minimum sample size, or an upper limit of respondents. Questions were presented in the same sequence to all respondents, and participants were free not to provide an answer to any question. No incentives were provided for those who participated.
All questionnaires from consenting participants were included for analysis, including partially completed forms. Percentages presented throughout the manuscript represent the proportion relative to all complete answers to a given response. Categorical data were presented in a descriptive format. For some questions, multiple categories were combined to improve clarity in the main text. Continuous data were presented as means (± standard deviation [SD]) or medians (interquartile range [IQR]). Chi-squared test was used for proportions to compare responses between FPs and NPs and between hospital-based practice (emergency room, hospitalization service, or critical care) and cabinet-based practice (outpatient community clinic, academic-affiliated clinic, long-term facility care, palliative care or home care) unless one of the categories included fewer than 5 observations, in which case a Fisher’s exact test was used. All analyses were performed using SPSS 29.0.1 (IBM, Armonk, New York), considering P < .05 as significant.
Results
Participant Characteristics
The survey was distributed to approximately 10 800 professionals and opened by 779 potential participants (view rate of 7%). Of these 779, 87 consented to complete the survey. Among those, 70 participants completed at least 1 survey question and were included in the analysis (response rate of 9%). From them, 66 participants (94%) completed all sections of the survey. As shown in Table 1, 84% of respondents were female, 79% (n = 55) were FPs, and 21% (n = 15) were NPs. Medical practice experience was well distributed across respondents, whereas most individuals practiced in outpatient community clinics. The mean proportion of time dedicated to such primary care practice was 70% (±32). A minority (34%) reported having regular hospital-based activities, either as attending hospitalists, general intensivists, or emergency physicians. All administrative regions of the entire Province of Quebec were represented in this survey (see Supplementary Table S1).
Demographic Information and Practice Characteristics.

Acute Kidney Injury Risk Factors Prevalence
As shown in Figure 1, most patients seen on a daily basis were between 46 and 80 years old. When asked to estimate the proportion of all patients seen in the clinic presenting at least 1 major comorbidity, respondents reported that 59% (±20%) of them had at least 1 AKI risk factor. The most prevalent comorbidity was hypertension, followed by diabetes and CKD.

The proportion of patients encountered according to their age group and prevalent comorbidities seen in daily medical practice. Categorical semi-quantitative data reported by clinicians (<5%; 6%-25%; 26%-50% and >50% of patients seen).
When asked to estimate the number of patients who were recently discharged from hospitalization and to whom they have offered dedicated care, 57% of respondents reported having followed at least 6 patients in the last 3 months, and 4% of them reported having provided care to more than 25 discharged patients during the same period.
Acute Kidney Injury Awareness and Barriers to Identify Kidney Events
When asked to estimate the proportion of patients having suffered from an AKI event at any stage, as reported in the discharge summary, access to in-hospital lab results, or reported by the patient, the mean result was 21% (±12). As shown in Figure 2, when questioned on the recurrent limitations imposed on them to correctly identify AKI events in their patients, 76% of them reported not being adequately informed. Access to a discharge summary, the lack of details on that summary regarding kidney function, and the lack of awareness and/or medical literacy from patients regarding their recent hospitalization were categorized as having at least a moderate impact on the process of care as a primary care provider for 83%, 90%, and 89% of all responders, respectively.

Potential recurrent barriers for the identification of AKI events impacting the process of care of primary care providers during post-discharge follow-up. Graduated color legend reporting 0 to 10 Likert scale: Dark green refers to no impact (0/10), light green refers to minor impact (3/10), light blue refers to moderate impact (5/10), and royal blue to major impact (10/10).
Opinions on the Disclosure of Acute Kidney Events to Patients
Respondents were presented with 5 short clinical scenarios illustrating hospitalizations complicated by an AKI event from various KDIGO stages, 9 whether they would plan dedicated time to discuss with the patient (and/or relatives) the ongoing kidney event if they were the attending clinician (Table 2). Most participants (97%) agreed to disclose the ongoing AKI event to the patient in a severe stage 3 AKI. Although 82% of participants would have planned time to discuss kidney function with a patient with stage 2 AKI based on standard serum creatinine criteria, that proportion decreased to 61% for a stage 2 AKI solely based on urine output decline. In total, 45% of all respondents would have discussed kidney function with the patient in the clinical scenario illustrating a limited stage 1 AKI, whereas that proportion decreased to 39% for an early recovering stage 2 AKI. No significant differences were observed between respondents reporting in-hospital activities to those reporting only non–hospital-based practice (P = NS).
Proportion of Respondents Planning a Dedicated Time to Discuss Kidney Function in Various Clinical Scenarios Reporting AKI Events in Hospitalized Patients, According to Their Medical Practice.

Those scenarios were optional for survey participants who reported no in-hospital medical activities in their medical practice (n = 46). Pearson Chi-squared test (significance <.05). SCr = serum creatinine.
Opinions on the Follow-up Workup of Discharged Patients With Acute Kidney Injury
Respondents were then presented with 4 additional short clinical scenarios illustrating outpatient follow-up 6 weeks after a hospitalization complicated by an AKI episode. Participants were asked to determine their agreement to plan an additional workup for all scenarios. As shown in Table S2 (Supplementary Materials), agreement to order additional workup at the visit was 97% in the presence of a stage 3 AKI receiving kidney replacement therapy in the absence of a planned nephrology follow-up, whereas that agreement decreased to 35% when a parallel nephrology visit was already planned.
Comfort to Manage Acute Kidney Injury Patients Following Hospital Discharge
As shown in Figure 3, when asked to categorize their overall level of comfort when managing recently discharged patients from a hospitalization complicated by an AKI episode, 33% of FPs and 60% of NPs reported at least some levels of discomfort. Based on a clinical scenario, participants were therefore asked to classify their agreement (based on their current level of comfort and expertise) to plan various interventions as previously recommended 3 (Table 3 and Figure S2 in Supplementary Materials). Eighty-three percent of respondents with in-hospital medical activities, as opposed to 50% of them without hospital-based activities, were comfortable switching a calcium channel blocker agent to an angiotensin-2 receptor blocker agent (P = .007). No difference was reported regarding post-AKI cardiometabolic workup order (P = .65), or AKI risk factors counselling (P = .35). When asked if they would agree to prescribe non–steroidal anti-inflammatory drugs (NSAIDs) in this scenario, respondents with hospital-based activities had a higher level of agreement (21% vs 2%, P = .02).
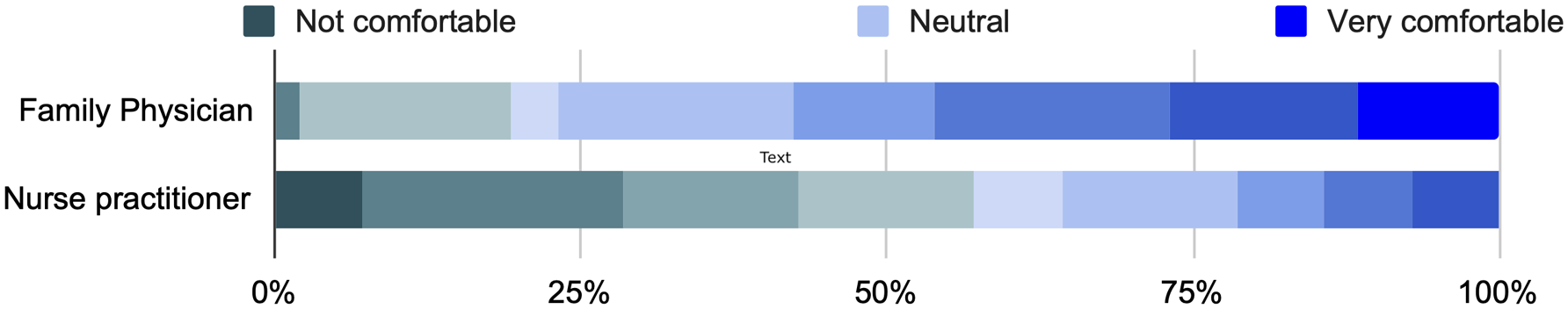
Level of comfort of family physicians and nurse practitioners to manage, as primary care providers, discharged patients following AKI episodes. Graduated color legend reporting 0 to 10 Likert scale: Dark green refers to being totally uncomfortable (0/10), light blue refers to a neutral level of comfort (5/10), and royal blue refers to being totally comfortable (10/10) to manage such discharged patients.
Agreement/Comfort to Order or Plan Various Interventions During the Follow-up Care of a Typical Severe AKI Survivor, According to Their Medical Practice.

This scenario was proposed to all survey participants (n = 70). Pearson chi-squared test. aStatistically significant (<0.05). Proposed scenario: A 71-year-old patient with hypertension and previous myocardial infarction without heart failure nor CKD (eGFR 71 mL/min) receiving acetylsalicylic acid, candesartan, and rosuvastatin. You see this patient at your clinic 8 weeks following a 10-day hospitalization for pneumonia, complicated by septic AKI. His max SCr was 321 µmol/L and decreased to 99 µmol/L (eGFR 53 mL/min) at discharge. His candesartan was replaced by amlodipine at discharge. CCB = calcium channel blocker; ACEi = angiotensin-converting enzyme inhibitor; ARB = angiotensin-2 receptor blocker; NSAID = non–steroidal anti-inflammatory drug.
Discussion
In this comprehensive survey, we identified significant variability in practices and comfort related to post-AKI care from primary care providers compared to recent expert-based recommendations. Our results also shed light on the limitations encountered by FPs and NPs when offering care to recently hospitalized patients.
First, we found that most primary care providers, either NPs or FPs, had trouble having access to adequate information regarding their patient’s recent hospitalization. Lack of access to a discharge summary and the lack of details and completeness when accessing that summary were reported as major limitations to allow primary caregivers to acknowledge AKI occurrence during hospitalization. This underlies a major barrier during the hospital-to-community care transition where the sharing of essential clinical information is the key to identifying those who may benefit from dedicated post-AKI care.
Second, the relative complexity of the renal system combined with the overall low level of patient medical literacy was reported as additional limitations in this survey. Effective education to patients on AKI/CKD risk factors and self-care management often relies on basic medical and more specific kidney-associated knowledge. However, recent data showed that 80% of severe AKI patients were unaware that they had experienced AKI while being hospitalized. 16 Notably, in that study, only 58% of patients reported discussing with their clinicians while hospitalized with a kidney problem, that proportion increased when receiving a nephrology consultation. 16 Interestingly, in this survey, although 97% of respondents would have planned to discuss kidney problems with the patient when facing a stage 3 AKI, only half of them would have done the same in the presence of a stage 1 AKI, and approximately one third for an early reversible stage 2 AKI, confirming the results from a previous study. 16 Patients unaware of their medical condition have limited empowerment in their self-care and might be less attentive to receiving counselling on post-AKI care and CKD prevention during follow-up. We suspect several reasons why clinicians might differ in disclosing an AKI event to their patients. First, knowledge of the long-term adverse outcomes of AKI episodes might be limited for some clinicians. Second, despite the adoption of standardized definitions of AKI, 9 this condition and its risk factors remain under-recognized in hospitalized patients, as it is possible that AKI, especially non-severe episodes, were not deemed clinically significant by clinicians. Even among nephrologists, post-AKI nihilism has been recognized and linked to a large discrepancy between expected follow-up and actual care offered to patients.11,17 Epidemiological evidence has reported potential benefits when offering dedicated post-discharge follow-up to patients having experienced AKI, as it is associated with a reduction in cardiovascular events and mortality. 18 However, as reported in the Nephrologist Follow-Up versus Usual Care after Acute Kidney Injury Hospitalization (FUSION) trial, the best post-AKI follow-up model adapted to patients’ need has yet to be determined. 19
Based on the results reported in this survey, we believe that some primary caregivers may not be aware that the long-term consequences of AKI could be significantly modified by counselling and proactive medical care, resulting in a low priority placed on allocating time to deliver AKI education and appropriate post-AKI follow-up. The fact that 9% of them would have been comfortable prescribing avoidable nephrotoxins such as NSAID shortly after a severe stage 3 AKI was remarkable and confirms the need for further medical education.
Then, we demonstrated that most primary care providers, especially NPs, were considerably uncomfortable with managing post-AKI patients in their current practice and, therefore, requested additional guidance on AKI. Regarding potential training that should be offered, we asked participants which topics should be prioritized. The AKI diagnosis, post-AKI prognosis, post-AKI patient counselling, post-AKI workup, and nephroprotective interventions were classified as priorities (Figure S3 in Supplementary Materials).
The strength of this study includes being among the first to examine the opinion of primary care providers on the process of care and current limitations for AKI patients’ management once discharged. Using a combination of direct and scenario-derived questions, we provide insights into variation in practice between FPs and NPs, as well as between primary caregivers with exclusive community/office practice and those with in-hospital activities. Urban and rural practices were included, and participants from all regions of the Province of Quebec were involved, allowing good representativity. Our study presents a few limitations. First, despite a large distribution through 2 major societies, only a limited proportion consented to participate, which may limit statistical power as well as generalizability. The initial distribution was performed during December, which, in retrospective, could have contributed to the initial low response rate. The survey was extensive, with multiple scenarios and required pre-consent before participation, which may have also contributed to the suboptimal response rate. The survey was limited to the Province of Quebec medical practice, which may impact the generalizability of findings. More female than male clinicians responded to the survey, which could be partially explained by the inclusion of NPs, potentially impacting the observed results. However, in a sensitivity analysis comparing both sex on their overall level of comfort when managing post-AKI patients, the proportion of them reporting at least some levels of discomfort were similar (female: 31% and male: 27%). Also, 43% of participants reported having offered medical care to only 5 or less recently discharged patients in the last 3 months, which could have impacted their overall comfort and experience regarding post-AKI care. Other known cardioprotective and nephroprotective interventions for CKD, such as statins or sodium-glucose transporter protein-2 inhibitors, were not addressed in the current survey. Finally, we cannot precisely estimate the total number of clinicians who received the invitation to participate.
In this comprehensive survey, we reported significant barriers regarding the hospital-to-community transition of care in patients having experienced AKI, concerning the access to discharge information, and the overall knowledge and comfort when offering dedicated post-AKI care. This reflects the need to improve communication, collaboration, and AKI training with primary care providers. Studies examining how AKI-related knowledge and specific interventions can improve outcomes are warranted.
Supplemental Material
sj-docx-1-cjk-10.1177_20543581241304517 – Supplemental material for Primary Care Providers Barriers, Comfort and Awareness in Follow-up Care of Acute Kidney Injury Patients: A Comprehensive Survey on Current Practices
Supplemental material, sj-docx-1-cjk-10.1177_20543581241304517 for Primary Care Providers Barriers, Comfort and Awareness in Follow-up Care of Acute Kidney Injury Patients: A Comprehensive Survey on Current Practices by Jean-Maxime Côté, William Beaubien-Souligny, Lauriane Hamel and Josée Bouchard in Canadian Journal of Kidney Health and Disease
Footnotes
Acknowledgements
The authors thank the Fédération des Médecins omnipraticiens du Québec (FMOQ), the Association des Infirmières praticiennes du Québec (AIPSQ) for endorsing and disseminating the survey to their members.
Author Contributions
J.-M.C., W.B-S., J.B., and L.H. contributed to conceptualization. J.-M.C., W.B.-S., and L.H. contributed to methodology. J.-M.C. contributed to formal analysis. J.-M.C. contributed to writing—original draft. W.B.S., J.B., and L.H. contributed to writing—review & editing.
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest: J.-M.C. reports Board Advisory for GlaxoSmithKline, received research funding from Bayer, and is supported by the Centre de recherche de l’Université de Montréal and the Université de Montréal Faculty of Medicine. J.B. declares no conflict of interest. L.H. declares no conflict of interest. W.B.-S. reports research funding from AstraZeneca and Bayer and is supported by Fonds de recherche en santé du Québec and KRESCENT program (Kidney Foundation of Canada). The authors declare no conflicts of interest with respect to this research.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics Approval
The current study was approved by local Research and Ethics Boards (#2023-11017).
Consent to Participate
An informed consent was obtained from all participants before survey completion.
Consent for Publication
Not applicable.
Data availability
The data that support the findings of this study are available on request from the corresponding author.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
