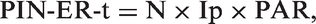Abstract
Vitamin D supplementation for all children <5 is recommended by the UK Department of Health for its skeletal effects. Vitamin D is also linked with a number of extra-skeletal effects; one of them being protection against type 1 diabetes. With a rapid increase in the incidence of type 1 diabetes and the associated costs, measures of curtailing the rapid increase of type 1 diabetes are needed. In this review, we look at type 1 diabetes using a statistical method (PIN-ER-t) and published data in an attempt to quantify the impact on the population of babies born in 2012 of increasing vitamin D supplementation rates. Calculations show that for the population of 729,674 babies born in England and Wales in 2012, 374 cases of type 1 diabetes (out of 1357 total predicted) could be prevented over 18 years if all were supplemented with vitamin D. This could lead to savings in excess of £62 million for the cohort. This piece of work adds to the argument for studying the potential link between vitamin D supplementation and type 1 diabetes further.
Introduction
Type 1 diabetes is an autoimmune condition leading to destruction of pancreatic insulin-producing β cells. It is well documented that the incidence of type 1 diabetes is increasing worldwide.1–3 Although the impact of such a diagnosis to individuals and their families is difficult to measure accurately, the estimated direct health costs for 2010/2011 in the UK are thought to be around £1bn, with the indirect societal and productivity costs given at £0.9bn for the same period. 4 Both figures are projected to increase, to £1.8bn and £2.4bn, respectively, for 2035/2036. 4
Higher chances of developing type 1 diabetes in those with affected first-degree relatives compared with the general population suggest that genetic influences are important. 5 However, it is clear that environmental factors are also important as evidenced by low-concordance levels in identical twins and observation that many children with genetic predisposition never develop the disease. 6
One of the environmental factors thought to be protective against development of type 1 diabetes is early supplementation with vitamin D.7–10 Vitamin D supplementation in infants is recommended in the UK for its skeletal effects for all infants and children under five years of age (if receiving less than 500 ml of formula milk a day). 11 Despite the advice, supplementation rates remain low. 12 There are indications that vitamin D supplementation of high-risk children is cost-effective compared with treating those displaying symptoms of hypovitaminosis D. 13
We set out to quantify potential improvements in the burden of type 1 diabetes on the population of babies born in 2012 by increasing vitamin D supplementation rates. Such quantification might prove useful to those considering cost-effectiveness of universal supplementation but also to front-line workers communicating risks and benefits to individuals and families. In order to facilitate this, we wanted to use an easily calculated measure and one that allows numbers to be communicated in a way that is easy to understand by both decision makers and the general public; such a statistical method, PIN-ER-t, has recently been described. 14 PIN-ER-t is a method of communicating effects of population interventions to decision makers and is defined as the potential number of disease events prevented in a specified population over the next t years by eliminating a risk factor. 14
Methods
Medline (Pubmed) was searched (1966 to June 2014) for systematic reviews and meta-analyses that had reported odds ratio or relative risk and 95% confidence intervals for the association between vitamin D supplementation and type 1 diabetes. The search terms used were ‘vitamin D’ AND ‘type 1 diabetes’. The main result of the meta-analysis (relative risk and 95% confidence intervals) was to be used in the calculation of PIN-ER-t. As the prevalence of type 1 diabetes is relatively small, it was felt appropriate to approximate odds ratio to relative risk if the latter was not available.
Population
PIN-ER-t was applied to the population of 729,674 live births known to have been born in England and Wales in 2012. 15 Prevalence of vitamin D supplementation in early life was taken from the recent ‘Diet and Nutrition Survey of Infants and Young Children’, 16 whose results (sample size 2683) were reported to be representative of the UK population. 16 The rate of supplementation observed in a four-day food diary varied with age (5% in the 4–6 months of age group; 5% in the 7–9 months group; 6% in the 10–11 months group and 7% in the 12–18 months group). 16 The highest percentage of supplementation with multivitamins (7%) was taken as the prevalence of supplementation with vitamin D.
Calculating PIN-ER-t
Definition of terms used in the PIN-ER-t calculations along with values and sources of these values in this case.

PIN-ER-t and 95% confidence interval were calculated using the relevant online calculator (http://www.phsim.man.ac.uk/pinert/Default.aspx). Although it would theoretically be possible to eliminate ‘no supplementation with vitamin D’, this is probably difficult to achieve in practice, therefore, the number of type 1 diabetes cases which could be prevented if current rates of supplementation are improved were calculated.
Costs
To calculate the cost of supplementation, we used the current recommendation of giving five drops of Healthy Start Vitamins per day to provide 300 IU (7.5 mg) of vitamin D3 for five years 11 (260 weeks). Each 10 mL bottle of Healthy Start Vitamins was taken to cost £1.38, 18 and there was an assumption that each supplemented infant would receive the correct daily amount with no wastage, so that each bottle would last the advertised eight weeks (33 bottles per supplemented child).
For the yearly cost of type 1 diabetes, we used the information provided by Hex et al. 4 to calculate the average cost per patient in 2010–2011 (£1.9 bn/400,000 patients = £4750). 1 For ease of calculation, we assumed that all patients developed type 1 diabetes at age 15. Finally, for the estimated average life-expectancy for those with type 1 diabetes, we used the information provided by Miller et al. 19 (69 y).
Results
The original systematic review and meta-analysis by Zipitis and Akobeng, 8 which evaluated the association between vitamin D supplementation and type 1 diabetes, was selected for use in the calculation of the PIN-ER-t. This is because a more recent review 10 came up with the same odds ratio as the original study. Further, there are methodological issues with the more recent review, such as pooling data from both case-control and cohort studies in the meta-analysis that we do not consider appropriate. The selected systematic review included a meta-analysis of four case-control trials from Europe (N = 6455; 1429 cases and 5026 controls). 8 The bottom line was that the risk of developing type 1 diabetes in those supplemented with vitamin D in infancy and early childhood was significantly reduced compared with those that were not supplemented (odds ratio 0.71, 95% confidence interval 0.60 to 0.84).
Assuming that odds ratio approximates to relative risk, the relative risk of type 1 diabetes due to non-supplementation in infancy and early childhood is 1/0.71 = 1.41. Based on the ‘Diet and Nutrition Survey of Infants and Young Children’, 16 we can see that only a maximum of 7% of babies are supplemented early on in life, giving us 93% which are not (Pe).
Number of cases of type 1 diabetes that could be prevented over 18 years at different prevalence levels of supplementation (total number of cases expected over 18 years for 729,674 babies in cohort is 1357).

Cost of supplementation, cost saving on prevented cases and final cost/benefit analysis for different levels of supplementation.

Discussion
Increasing vitamin D supplementation rates for its skeletal effects, as suggested by recent UK Department of Health advice, 11 could also lead to a much-desired decrease in rates of type 1 diabetes; an extra-skeletal effect of vitamin D. The model used here predicts 374 fewer cases over 18 years, if all 729,674 babies of the 2012 birth cohort in England and Wales 15 are supplemented early on in life. This is against a predicted total of 1357 cases predicted for the cohort over the 18 years. Figures for increasing rates of supplementation from current low baseline levels 16 are also provided as universal supplementation might be impractical. Cost calculation shows a financial benefit from supplementation, which appears to get progressively greater with increasing supplementation rates.
PIN-ER-t provides an easily understandable method of communicating the benefits that could be gained by the population if the exposure is modified or eliminated. 14 Using this measure, one can quantify the population burden of a risk factor and communicate it, so that both health professionals and members of the general public can understand and relate to it. 14
In calculating the PIN-ER-t, there has been an assumption that the reported odds ratio for the association between ‘no supplementation’ and type 1 diabetes approximated to relative risk. As mentioned previously, this is a valid assumption when the prevalence is small. However, it is generally accepted that odds ratios tend to overestimate the effect size compared with relative risks.20,21
We acknowledge certain limitations to the prediction model. Clearly, applying such measures implies causality, which some will dispute in view of the fact that the systematic reviews investigating the relationship between vitamin D supplementation and type 1 diabetes are not based on randomised controlled trials but rather on well-characterised cohorts and case-control trials.8–10 However, such randomised controlled trials would have to be massive, run over a few decades and be prohibitively expensive. Further, there are ethical dilemmas, as all infants and young children should be supplemented with vitamin D. 11 In addition, there are ways of establishing causality in the absence of evidence from randomised controlled trials 22 and publications demonstrating how the relevant criteria are met in the case of vitamin D supplementation in the first years of life and type 1 diabetes have been around for some time. 9 Another important issue to consider is the dosage of daily supplementation with vitamin D. In the examples above, we have assumed that the current recommended doses of supplementation (300 IU) would be enough to bring about the desired outcome. The available evidence to date recognises that there is a dose-response effect with higher daily doses of supplementation linked to lower risk of type 1 diabetes but an optimum dose remains elusive.7–9
The association of vitamin D with a range of extra-skeletal effects continues to cause controversy in the medical literature. This is also the case for the specific association between vitamin D and type 1 diabetes. This piece of work adds to the argument for studying this potential association further.
Conclusion
Improving vitamin D supplementation in infancy and early childhood remains an important public health goal. Such improvements might bring about extra-skeletal benefits such as a reduction in type 1 diabetes cases, with concomitant cost reductions. The model used in this study predicts 374 fewer cases over 18 years (out of a predicted 1357) if all 729,674 babies of the 2012 birth cohort in England and Wales are supplemented early on in life. The cost-saving for such a reduction over the expected average life expectancy of this cohort would be in excess of £62 m. The use of PIN-ER-t allows for an easily demonstrable and understandable way of communicating the population burden of a risk factor.
What is known about the topic?
The incidence of type 1 diabetes is increasing as are the already massive costs
associated with the condition. Early supplementation with vitamin D has been linked with lower risk of developing
type 1 diabetes.
What this study adds?
PIN-ER-t calculation suggests that the population burden of type 1 diabetes could be
decreased by increasing rates of supplementation with vitamin D; an estimated 374
fewer cases could be seen in the 2012 birth cohort over 18 years (out of a predicted
total of 1357 cases) if all children in the cohort were supplemented. Achieving 100% vitamin D supplementation rates could lead to savings in excess of
£62million for the cohort.
Footnotes
Declarations
Funding
None declared.
Ethical Approval
▪▪
Guarantor
CSZ
Contributorship
We confirm that all listed authors fulfill the ICMJE criteria for authorship. Further, that there is no other person that fulfills these criteria and is not listed here.
Acknowledgements
None
Provenance
Not commissioned; peer-reviewed by Lawrence Cheskin