Abstract
Social media advertising has revolutionised the advertising world by providing data-driven targeting methods. One area where social media advertising is just gaining a foothold is in the recruitment of clinical study participants. Here, as everywhere, social media advertising promises more yield per money spent because the technology can better reach highly specialised groups. In this article, we point out severe societal risks posed by advertising for clinical studies on social media. We show that social media advertising for clinical studies in many cases violates the privacy of individual users (R1), creates collective privacy risks by helping platform companies train predictive models of medical information that can be applied to all their users (R2), exploits the weaknesses of existing guidelines in (biomedical) research ethics (R3) and is detrimental to the quality of (biomedical) research (R4). We argue that the well-intentioned promises, which are often associated with the use of social media advertising for clinical studies, are untenable from a balanced point of view. Consequently, we call for updates of research ethics guidelines and better regulation of Big Data and inferential analytics. We conclude that social media advertising – especially with vulnerable patient populations – is not suitable as a recruitment tool for clinical studies as long as the processing of (even anonymised) social media usage data and the training of predictive models by data analytics and artificial intelligence companies is not sufficiently regulated.
Keywords
Introduction
With the rise of social media, new communication possibilities have emerged, amongst them also targeted advertising. All kinds of offers are being communicated through
Recent clinical studies using social media advertising for their recruitment efforts have shown promising results for different parameters and study designs. 1 For an HIV vaccine clinical trial, Sitar et al. (2009) demonstrated that advertising on social media was successful in reaching a wider audience. Frandsen et al. (2014) were able to prove the viability of social media advertising as an addition to other, more traditional recruitment methods for smoking cessation clinical trials. Wisk et al. (2019) found that recruiting college students with type I diabetes to a longitudinal intervention trial via social media was feasible, efficient and acceptable, yielding a representative sample of the user-base from which they were drawn. Guthrie et al. (2019) revealed that social media advertising was feasible for clinical trial testing interventions to treat post-menopausal vaginal symptoms. Proponents of these studies stress that social media advertising for participant recruitment has various social benefits, such as increasing ‘fairness’ in access (Whitaker et al., 2017), promoting ‘trust’ and ‘transparency’ (Close et al., 2013; Denecke et al., 2015), or bringing hard-to-reach populations into research (Caplan, Friesen, 2017).
Balancing this often one-sided and positive perspective, we maintain in this article that social media advertising in clinical study recruitment carries a number of ethical and societal risks that have to be assessed and weighed up more thoroughly. The long-held view that social media advertising should be ethically evaluated in the same way as offline strategies (Gelinas et al., 2017) needs to be reconsidered. We highlight the fact that using data on the engagement of single users with clinical ads, social media platforms are able to train machine learning models to predict medical conditions of any third person based on their behavioural data. This poses a range of severe risks, including privacy risks and risks of unequal treatment. With both regulators and study operators as potential audiences in mind, we argue that an unregulated implementation of social media advertising for clinical studies poses significant risks to society and to the quality of research.
We start this article by differentiating four subcategories of ad targeting mechanisms (see ‘What is social media-based advertising and how does it differ from offline ads?’ section and Table 1): static, explicit, predictive and lookalike targeting. This list is ordered according to increasing sophistication in targeting techniques, which also come with growing ethical concerns. After establishing our typology, we will analyse four pressing ethical issues (R1–4, see ‘Risk analysis and ethical evaluation’ section) in relation to social media advertising for clinical trials. These issues are multidimensional, posing potential risks to individual patients, severe risks to society through the aggregation of medical data in the hands of commercial platform companies, and potential threats to the independence and effectiveness of clinical research.
Qualitative comparison of targeting types.

*This implies the certainty that a user does not get targeted by information they did not explicitly provide.
In principle, much of our analysis also holds for targeted advertising outside social media sites, that is, open-domain advertising services such as Google Ads that place targeted ads on any website. We still focus on social media advertising in this article to reduce the complexity of our investigation. Moreover, in our discussion, we use
What is social media-based advertising and how does it differ from offline ads?
We will first discuss in what ways social media advertising is different from existing forms of offline advertising for patient recruitment. Social media advertising has common roots with outdoor and print advertising on the streets, in the subway or in magazines. But with recent technological developments, qualitatively new features emerged in online advertising, which enable novel mechanisms of individualised targeting. To highlight these differences, we present a progressive list of four types of targeting mechanisms (Table 1), of which only the first and weakest is comparable to offline mass advertising.
Type A: Static audience targeting
A common form of offline advertising is street or magazine advertising. In patient recruitment, poster campaigns, for instance in subways, print magazines or medical waiting rooms are used to statically target potential participants. In the online realm, static targeting – similarly – uses digital advertising displays, such as banners or text snippets on websites: Advertisers choose a location, for example, a specific website, for a fixed advertisement that is displayed to all visitors of that location over a certain period of time. While the location is carefully chosen to match a specified audience, typically every person that passes by sees that advertisement, and the same version of it. We call this form of targeting ‘static targeting’ because there is no individualised (per visitor) and/or responsive decision mechanism that selects different versions of the advertising for different people walking by.
Static targeting is weak in comparison to more elaborate contemporary online targeting methods and does not play an important role in today’s online advertising, as it represents the technological state-of-the-art in the pre-social networking era of the internet (roughly until the turn of the millennium).
The paradigm shift: From offline to online
Indeed, static targeting misses all the specific advertising opportunities afforded by social media. In this case, with ‘social media’ we broadly refer to digital networked services that implement techniques to uniquely identify their users and their users’ real-world relationships (to other users, to brands, affiliations, topics, medical issues, etc.). ‘Identification’ means that subsequent interactions of the same real person with the service can be matched by the service to belong to one and the same user (represented by a digital ‘profile’, account or any other kind of persistent identifier), although this kind of identification does not necessarily rely on collecting information about the civic identity of a person. Thus, not only do platforms such as
The technological development of social media enabled a profound revolution in advertising due to its ability to aggregate extensive, high-resolution individual data profiles (see e.g. van Dijck, 2009). These data stocks can be leveraged to make automated, fine-grained targeting decisions on a per-user basis that exhibit two largely new features compared to the offline world:
Digital media can show different advertisements to different individuals. This could also include different versions of the same advertisement tailored to a user’s characteristics or interest profiles. Social media ad providers can collect real-time information about the
These two media-technological capacities of online as opposed to offline media enable various qualitative leaps in ad targeting methodology. This will be mapped out as we now continue the list of increasingly sophisticated targeting principles.
Type B: Explicit targeting
A first qualitative leap occurs when the targeting decision is based on a per-user matching of targeting criteria against explicitly recorded personal attributes. On social media platforms, users sign up with a personal profile and provide personal information through engaging with the platform. In the form of targeting we call ‘explicit targeting’, the matching operates against data fields that users explicitly enter in their profiles, such as age, gender, relationship status, personal interests, group memberships, friends, educational background, work affiliations, etc.
Providers of explicit targeting are mostly large platform companies because they need a large base of users who are incentivised (through mechanisms often unrelated to advertising) to provide as much personal information to the system as possible. On
Compared to static targeting, explicit targeting frequently renders the specification of a
In the case of patient recruitment for clinical studies, the explicit targeting method shifts attention from determining the best physical location of an advertisement to naming the key demographic and personal characteristics of the target audience. For example on
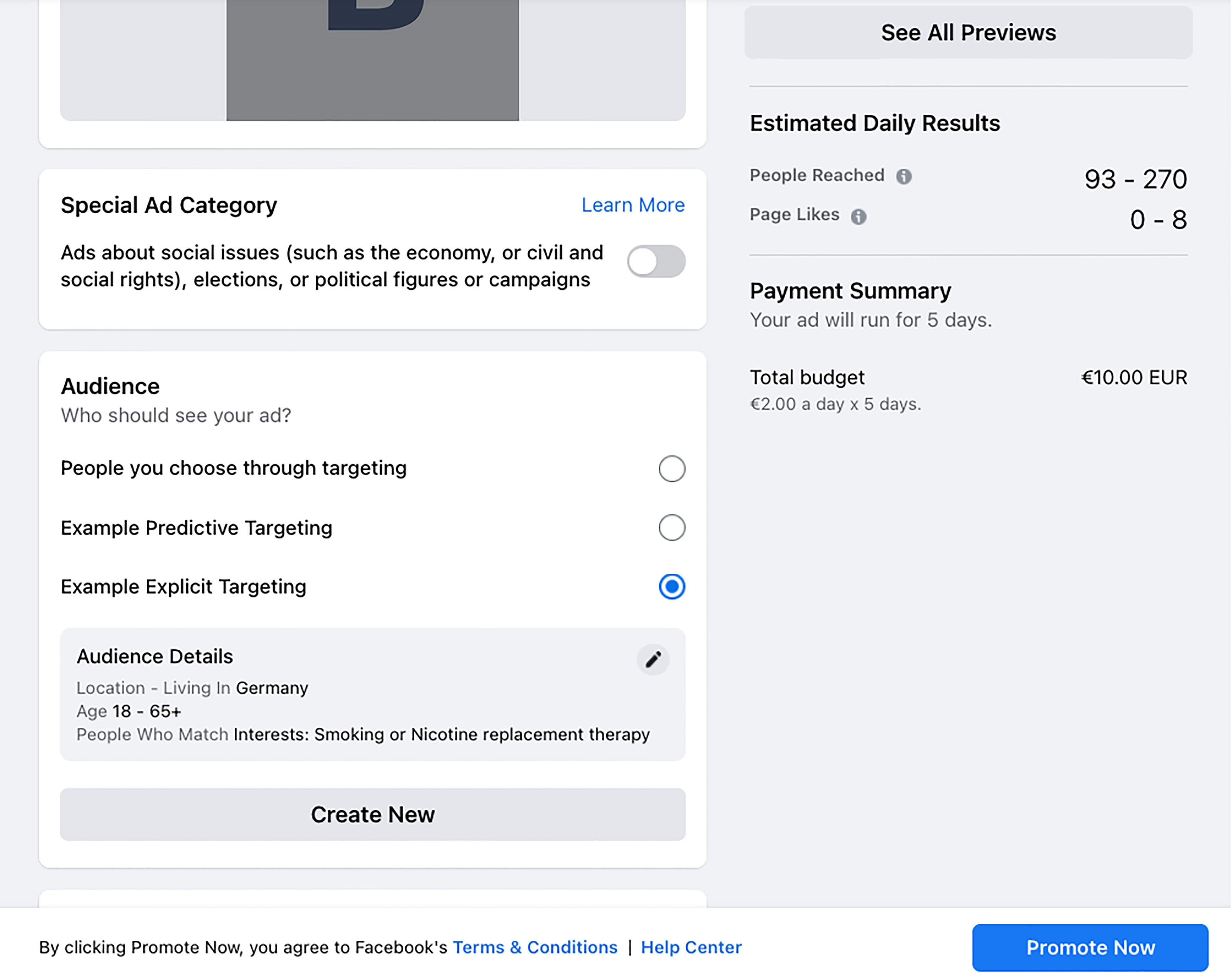
Screenshot Facebook.com: Configuration of an explicitly targeted online ad.
Type C: Predictive targeting
The next qualitative leap comes with individual targeting mechanisms that not only rely on personal attributes explicitly specified by the users, but also on predicted information. Imagine a user did not specify their age or gender in their profile information, while their extensive behavioural data (posts, likes, browsing history or social graphs) are available to the platform. Studies showed that the missing attributes can be estimated from the available data (Kosinski et al., 2013). Using advanced machine learning and data analytics techniques, what is referred to as ‘predictive targeting’ therefore leverages behavioural, usage and tracking data to estimate relevant targeting attributes about single users where such attributes are not explicitly given. 3
This method, however, is not limited to ‘filling the gaps’ in users’ profile information. Rather, this technique enables a covert expansion of the available targeting parameters to include information that hardly any user would voluntarily provide and whose explicit processing might even be prohibited by data protection regulations. This information includes, for example, purchasing power, wealth or credit risk scores, as well as estimated information on medical conditions, sexual orientation, ethnic or racial background (see e.g. Mühlhoff, 2021; O‘Neil, 2016). As Andreou et al. (2018) explain,
This step of ‘translation’ typically comes with an increase in the sensitivity of information, or infringement of privacy, as Mühlhoff (2021) argues. ‘Predictive analytics’ enables advertising providers to estimate highly sensitive and intimate information about users from less sensitive and often readily available data (cf. Mühlhoff, 2021; Figure 1). Among the information that is predictable from social media usage data are many medical data fields that might be of particular interest to advertisers in the field of patient recruitment for clinical studies. For instance, researchers at the University of Pennsylvania have shown that diseases such as depression, psychosis, diabetes or high blood pressure can be predicted from a user’s postings on
It is a reasonable assumption that most contemporary online advertising providers combine explicit and predictive targeting (types B and C) without allowing advertising customers to opt out of the predictive mechanism. 4 Advertising customers just specify certain targeting criteria that will be matched by the social media platform either with data explicitly provided by users (where available, e.g., for users who disclose their age in their profile) or with predictions of the same parameters when a user did not provide that information about themselves. In social media advertising for clinical studies, this would mean that medical – and thus potentially sensitive – attributes of users are being estimated based on data from other users that disclose such information. This could range from alcohol intake and smoking habits to diabetes or infectious diseases such as human immunodeficiency virus (HIV), hepatitis B or other highly stigmatised indications.
Type D: Lookalike targeting
Predictive targeting, as an ‘improved’ version of explicit targeting, makes ‘virtual’ (or estimated) audience attributes available as targeting criteria, in addition to the attributes users would specify about themselves. The next step in the increasing development of targeting methods presents a way to do without the specification of personal attributes as targeting criteria by the advertiser. In what we call ‘lookalike targeting’, advertisers provide a list of relevant

Screenshot Facebook.com: Creation of a lookalike target audience, showing the different attributes that can be specified, for example, email, phone number, names, gender, age, etc.
The power of this targeting principle becomes evident, for example, in combination with
The hidden epistemology of online targeting
The broader transformation from static to lookalike targeting marks a fundamental change in the implicit epistemology of advertising. The first transition, from static to explicit targeting, suggests a return to a positivistic reliance on explicit information about the single individual (cf. Kitchin, 2014). Whereas static targeting used locations (e.g. street corners, metro lines, magazines or event locations) as proxies to hit a certain market segment in a time when little direct individual data was available, explicit targeting makes use of the new wealth of information people have been disclosing about themselves on social media networks since the 2000s. This can be seen as the beginning of the era of ‘micro-targeting’ (Barbu, 2014).
This new positivism, however, outdoes itself when it transitions from explicit to predictive targeting. Here, a speculative element creeps into the underlying data epistemology because predicted attributes are often derived as the ‘best bet’ from statistical inferences (Joque, 2022; Mühlhoff, 2021). This represents a shift from relying on how people reflect on themselves to how they behave. The kind of reasoning that is implemented by these algorithms remains positivistic, but turns from subjectivism to the
Given this relational approach of predictive behavioural epistemologies, it seems logical that in the next step of the development of targeting methods, leading from predictive to lookalike targeting, we see the use of relational information coming fully to the fore. Lookalike targeting radicalises this approach by offering an alternative to specifying a list of personal attributes for ad targeting (which still makes the advertiser focus on the individual): advertisers simply specify a list of known users. This list fixates a relational constellation of existing persons instead of a grid of individual attributes, so that a matching algorithm can establish who else is in close proximity to those users.
In the context of patient recruitment in clinical studies, it is important to note that determining the similarity metric (i.e. the behavioural markers that determine the relevance of a person to the clinical study) is largely delegated to secret algorithms and their designers when proprietary targeting services are used. Specifying relevant personal attributes, seen in explicit and predictive targeting, is a way of establishing factual criteria for the potential relevance of a given person to the clinical study. This relation between criteria and advertising is, at least in principle, accessible to scientific explanation (e.g. based on knowledge about the prevalence of a certain disease in a demographic cohort or in relation to certain lifestyle aspects). Lookalike targeting breaks with this chain of reasoning. Ads will be shown to a person X not because they belong to a cohort that is statistically likely to suffer from a certain medical condition, but because an opaque, proprietary algorithmic procedure deems that it is profitable to show the ad to X (Joque, 2022).
In the next section we will discuss how the various stages of this epistemological transformation come with different ethical, data protection and epistemological risks.
Risk analysis and ethical evaluation
Multiple ethical and data protection concerns arise in relation to advertising clinical studies on social media. In this section, we put forward a selection of such concerns (risks R1–4, Table 2), differentiating according to the typology of targeting methods laid out in the previous section.
Risk comparison of targeting types.

For every targeting type (colums A–D) it is indicated in what way the different risks (rows R1–4) are prevalent.
R1: Violations of individual privacy
Social media targeting algorithms match audience information provided by the advertising customer with social media users. As we saw in the previous section, state-of-the-art predictive targeting mechanisms (type C) do not require that all users explicitly specify the attributes in question, as missing or undisclosed information is routinely estimated by predictive models. Moreover, predictive targeting technologies extend the range of available targeting attributes to personal information that users typically do not enter themselves.
The first ethical concern connected to this technology is that it violates users’ privacy in a new way. Under the title of ‘predictive privacy’, Mühlhoff (2021) pointed out that privacy can be violated by ‘if sensitive information about that person or group is predicted against their will or without their knowledge on the basis of data of many other individuals, provided that these predictions [could] lead to decisions that affect someone‘s social, economic, psychological, physical, … well-being or freedom’. (cf. Mühlhoff, 2021: 5)
To see in which way this definition applies to the present scenario, we have to examine three conditions. First, predictive targeting generates information about users without their knowledge and potentially against their will. As information that is predicted for targeting of clinical studies includes, or correlates with, sensitive information such as addictions, health, psychological conditions, sexual orientation, etc., we must assume that the application of predictive targeting in this context is very likely to involve information users would not willingly provide to the platform.
Secondly, predictive and lookalike targeting classify users through large-scale comparisons with the behavioural data of many other individuals and are thus enabled by the data that social media users
The technological possibility of predictive targeting is an effect of collective data aggregation, to which most of us regularly contribute through our use of networked platforms. The feasibility of this technology is unaffected by any single user’s decision to not disclose a certain piece of information, as long as there is still a large cohort sharing much of their data (and even if they do so anonymously). Predictive targeting therefore poses a challenge to all individualistic and control-oriented interpretations of privacy rights as implemented, for instance, in ‘informed consent’ policies (Blanke, 2020; Kröger et al., 2021; Wachter, 2019). As predictive algorithms can fill the data gaps that might result from single users’ deliberate non-disclosure of certain information, these users can still be targeted. By not joining the game, single users can neither prevent predictive analytics being applied to others nor to themselves. This is counter-intuitive and deceptive to many users who are not familiar with the predictive targeting methodology. A lack of public awareness thus contributes to the largely unregulated applicability of this kind of data processing.
Thirdly, to meet the requirements for ‘violation of predictive privacy’ according to the definition from above, we need to establish in what way the prediction of hidden targeting attributes could affect ‘someone‘s social, economic, psychological, physical, … well-being or freedom’. At this point, we need to consider the type of information that is implicitly or explicitly predicted in our concrete cases. In the context of clinical studies, reaching effective targeting decisions often correlates with an assessment of medical information about social media users since the advertising seeks to reach persons with specific diseases or medical (pre-)conditions. This makes training an effective predictive model for this ad targeting decision
In what way, though, could this information be used to anyone’s detriment? Tufekci pointed out that ‘when ‘big data’ reveals more than was disclosed’, these ‘computational violations of privacy’ have potentially severe ‘civil rights implications’ (Tufekci, 2015: 209). O‘Neil makes clear that predictive models are being used in a wide range of industrial applications with material consequences for individuals, ranging from (semi-)automated hiring processes on the job market to insurance and credit scoring to the criminal justice system (O‘Neil, 2016). As O‘Neil argues, the way predictive models are being used is ‘exacerbating inequality and punishing the poor’ (p. 17). Behind these analyses of the consequences of predicted information is the observation that predicted information is generally used for a differential treatment of users.
The urgency of an ethical and political debate of predictive violations of privacy is further underpinned by the observation that despite the extra sensitive status granted to medical information by many data protection regulations such as the EU’s GDPR, most of these regulations
R2: Collective privacy implications: Disclosure of medical information to the platform
An even stronger ethical concern regarding the violation of predictive privacy arises when we do not focus on the individuals that are part of a clinical study or that see the advertisement for a study on social media, but shift our attention to the effects on ‘digital bystanders’ as well as simply
To show why this is a concern, our main argument in this article is that social media advertising for clinical studies
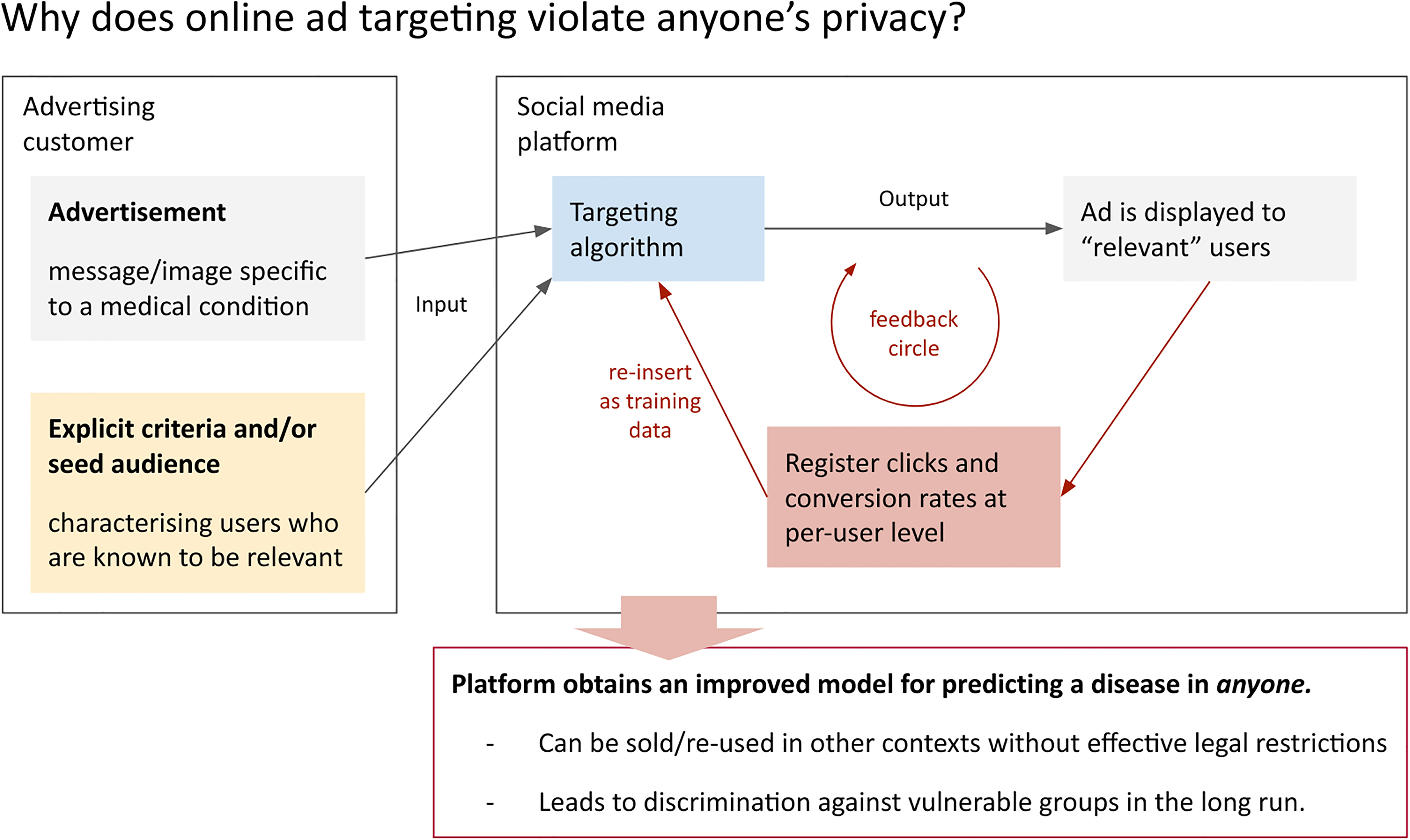
Advertisers help data companies to train predictive models.
While the exact workings of targeting algorithms are trade secrets, it is not only theoretically plausible but also empirically evident that social media platforms indeed leverage the ad engagement data to make their models ‘learn’. For instance, a 2018 study by Borodovsky et al. (2018) made use of ‘[T]he algorithms used to distribute advertisements appear to require a sufficient amount of time to complete a learning phase before they become effective. During this learning phase, enough data must be accumulated to determine which members of the target population have the highest probability of engaging with the advertisement. […] Currently, when we use Facebook advertisements to reach cannabis users, we begin advertising with a low spending limit of US $10 per day for 48 to 72 h, which we believe facilitates algorithm learning. After this 48- to 72-h time frame, we have consistently seen a notable increase in the rate of clicks’. (Borodovsky et al., 2018: 2)
Given the many opportunities of re-utilising these targeting models as predictive models of medical information and related risks, the social media platform benefits twice from the advertising deal. While study operators pay for access to the results of the predictive model, platform companies can re-use
In the hands of private actors in a largely unregulated market, such predictive models pose an immense threat to social justice and equality of treatment. They endow platform companies with technological capacities to treat individuals and groups differently at large scale, which marks a structural power asymmetry between society and business interests. As Barocas and Selbst (2016) argue, this power asymmetry exacerbates already existing structures of inequality and unfair discriminations when predictive algorithms ‘discover surprisingly useful regularities that are really just pre-existing patterns of exclusion and inequality’ in our societies. This is why an ‘unthinking reliance’ on, and unregulated spread of those technologies ‘can deny historically disadvantaged and vulnerable groups full participation in society’ (Barocas, Selbst, 2016: 671).
Consequently, the moral responsibility of study operators is not inconsiderable. Note that even a
It should also be mentioned that the data protection risk outlined in R1 and R2 is not restricted to the predictive forms of targeting (types C & D). It pertains to all digital advertising services that collect user-level engagement data (e.g. click rates).
R3: Exploiting the limits of (biomedical) research ethics
Protection of participants’ privacy and data protection rights have been well-established as a central pillar of biomedical research ethics through international frameworks and guidelines, such as those established by the World Health Organisation (WHO) and the Belmont report (CIOMS, 2016; The World Medical Association, 2013; cf. Beauchamp, Childress, 2012). According to the WHO, the collection, storage and use of data in health-related research must be governed by an informed consent process similar to those related to participation in the research procedure itself (CIOMS, 2016). Researchers, according to the WHO, are obliged to ‘anticipate, control, monitor and review interactions with their data across all stages of the research’ (CIOMS, 2016: 83). In this subsection, we argue that the WHO provision also applies to the participant recruitment stage.
In light of the previous discussion, we suggest that the frameworks be extended or sharpened corresponding to the specific challenges of social media recruitment strategies and technologies. There are at least Consent to be contacted: Online targeting involves implicit or explicit estimations of medical information about a large group of social media users before they even see an advertisement. If social media advertising is utilised for study recruitment for stigmatising or rare diseases, particularly sensitive medical information is estimated and processed by the platform Outsourcing ‘dirty business’: Existing biomedical research ethics guidelines are not devised for social media targeting and can easily be circumvented. For instance, guideline 22 in the WHO framework (CIOMS, 2016) demands that:‘Researchers collecting data on individuals and groups through publicly accessible websites without direct interaction with persons should, at a minimum, obtain permission from website owners, post a notice of research intent, and ensure compliance with published terms of website use’. (CIOMS, 2016: 83)
Due to the architectural differences of social media platforms compared to other publicly accessible websites to which the guideline refers, it is – in the case of social media advertising for clinical studies – almost impossible to comply with the requirements mentioned therein. Using a social media advertising service outsources a tremendous amount of data processing from the study operator to the social media platform. As a result, researchers (unwittingly) bypass severe ethical obligations that actually rest with the study operators. Moreover, while social media users give their
With this in mind, the use of social media platforms for advertising clinical studies presents an outsourcing of the ethically doubtful data processing work of targeting to the platform company. This opens up the possibility for study operators to make use of the advanced predictive technologies of social media platforms and have their data processed in ways they would ethically, legally and practically not be able to do themselves. To protect patients as well as clinical study operators, the social media-specific ethical considerations about data collection and processing should be covered in ethics guidelines (Hunter et al., 2018). Moreover, entirely new forms of informed consent procedures are required for specific cases that are unique to social media, for example, when researchers want to recruit in the networks of their study participants (Custers et al., 2014; Gelinas et al., 2017; O‘Neil, Schutt, 2013).
With predictive or lookalike targeting mechanisms, a user’s health is predicted on the basis of characteristics they did not explicitly disclose. This is likely to cause harm because individuals are confronted with a (potential) diagnosis without having chosen to be so (cf. Thornton et al., 2016). As discussed above (see R2), the feedback mechanisms of online ad targeting allow the platform to train a
Arigo et al. (2018) second this collectivist line of argumentation by pointing out that it needs to be considered how the infringement of privacy might affect not only potential patients, but also ‘bystanders’ such as relatives or other people with social (media) connections to potential participants. We go even further in pointing out that this issue shows a fundamental limitation of the informed consent principle which ignores that the decision made does not have consequences only for the person asked, but for society at large (cf. Kröger et al., 2021; Mühlhoff, 2021). Ethics guidelines, which reduce data protection to informed consent, therefore not only neglect one of the most serious challenges in data ethics and data protection in the context of social media, but also
R4: Impairment of the quality of (biomedical) research
Our analysis shows that delegating ad targeting decisions to Big Data-based advertising services buys into a comprehensive amount of ‘magic’ in deciding who is, and who is not, a potential candidate for a study. From the point of view of the researchers operating a clinical study, this means outsourcing targeting decisions to a ‘black box’ algorithm (cf. Pasquale, 2016). In this subsection, we argue that this has potential implications on the quality of the research in question.
The actual algorithmic functions of targeting mechanisms are typically not disclosed by social media platforms. Researchers working outside the respective platform, including recruiting researchers, usually have no control and often no knowledge of which data is collected, stored and used in the targeting process. Neither can external researchers control or ensure whether the algorithms have been updated during the recruitment phases by the respective platform and the targeting mechanisms have therefore undergone changes (Hitlin et al., 2019). These circumstances create a methodological pitfall according to existing ethics frameworks, which demand that study conductors publish not only the results of their research on human subjects, but also account for the completeness and accuracy of their reports, including disclosure of recruitment strategies and cohort emergence (The World Medical Association, 2013). As the CIOMS framework highlights: ‘groups, communities and individuals invited to participate in research must be selected for scientific reasons and not because they are easy to recruit because of their compromised social or economic position or their ease of manipulation’. (CIOMS, 2016: 7)
Social media-based recruitment violates these principles and thus sacrifices indispensable methodological rigour and control to commercial owners of data and algorithms. As recruiting decisions are central to a sound study design (see e.g. Patel et al., 2003; Puffer, Torgerson, 2003), adoption of social media-based recruitment strategies outsources to commercial actors what is actually
In fact, these circumstances described above lead to a seemingly paradoxical constellation: social media recruitment is often advertised in the name of justice for its acclaimed capacity to reach poorly accessible and vulnerable patient groups that are otherwise hard to reach (Bonevski et al., 2014; King et al., 2014; Wozney et al., 2019). However, studies for which this argument applies are usually characterised by inclusion or exclusion criteria based on particularly sensitive medical information. Hence, deploying social media advertising in this situation could supposedly target more individuals of a highly specific medical situation, but at the cost of an increased opacity and unaccountability in the targeting mechanisms, which compromises scientific rigour. In such cases, we also have to refer back to the increased severity of the predictive privacy implications (R2). Hence, the issues of justice and accessibility are easily turned around, with predictive targeting ultimately working against those groups who are supposedly better included by such measures.
Putting it all together: Austerity in the guise of benevolence
Social media-based advertising is often touted as
The proprietary data aggregated by platform companies as a corollary to the medical ad campaign allows those companies to build AI models that can predict the relevant medical condition in anybody. Those models, once they exist, are set to play a role in the mechanisms of structural power in our societies and will likely not play out to the benefit of the vulnerable groups (Mühlhoff, 2020; O‘Neil, 2016). Creation and circulation of those models is not effectively regulated by current data protection legislation such as the EU’s GDPR (Wachter, 2019). As both the training data (which is generated by the advertising feedback mechanisms) and the internal model parameters can be handled as anonymised data, data protection regulations do not apply (Mühlhoff, Ruschemeier, 2022). Thus, the collected data can be re-used in scenarios such as (semi-)automated job selection, insurance pricing, political persecution, access to financial, educational and other resources.
The supposed increase in efficiency of current ad campaigns will thus backfire many times in the form of technologically driven social selection and discrimination. From the perspective of platform companies, such advertising deals are just welcome opportunities to collect user-level data which will be used as AI training data in an epistemic field that is difficult to access. In a context where predictive analytics is as little regulated as it is today, study operators and funding bodies opting to enable or pursue this form of advertising for clinical studies are (unwittingly) complicit in enabling commercially driven forms of future injustice.
These considerations profoundly demystify the promise of benevolence that is often connected to the use of social media advertising for clinical studies. From a more structural and long-term perspective, the real incentive for using social media advertising seems first of all driven by austerity – with the same budget, advertisers seek to reach a more specific audience.
At this point, there is a high demand for better regulation. Big Data companies should be effectively regulated in their processing and re-purposing of aggregated and anonymised data in the form of predictive models that can be transferred to other contexts (Blanke, 2020; cf. Mühlhoff, 2021). Clinical research, on the other hand, must be prohibited from implicitly contributing to private companies collecting proprietary data that will harm our societies. At this point, a key to better and more effective regulation is that both researchers and regulators pay more attention to aspects of data protection that go beyond individual privacy. Protecting the
Conclusion
We have unpacked the apparently benevolent usage of social media advertising in the context of recruiting participants for clinical studies. After other studies had examined and highlighted the positive effects of social media recruitment (Frandsen et al., 2014; Guthrie et al., 2019; cf. Sitar et al., 2009; Wisk et al., 2019), we found severe potential for a range of negative effects regarding privacy, social inequality and scientific research quality.
Setting the stage for our investigation, we separated different types of ad targeting. We showed the general threats of online audience targeting (type A), supported by the explanation of the paradigm shift from offline to online. An increasing list of threats was introduced that originate from explicit targeting (type B), predictive targeting (type C) and lookalike targeting (type D).
In our risk analysis and ethical evaluation, we identified different risks originating from social media advertising. Risk R1 starts from the concern that the effect of the established principles of ‘informed consent’ and ‘privacy self-management’ are limited in online spaces (Kröger et al., 2021; Mühlhoff, Ruschemeier, 2022). Regarding individual privacy rights, predictive and lookalike targeting mechanisms are problematic as they derive potentially sensitive (medical) information from less sensitive information about arbitrary users – including those who are not targeted by the ad campaign. This constitutes a violation of users’
In risk R2, we transferred this argument to a structural level. We made the case that social media advertising for clinical studies enables social media platforms to build AI models that can predict medical conditions about
In risk R3 we then analysed the detrimental effects of biomedical research ethics guidelines that focus on privacy as merely an
In risk R4, finally, we pointed at the potential impairment of biomedical research quality that results from outsourcing recruitment decisions to ‘black box’ targeting algorithms of commercial actors. Patient selection is not scientifically accountable at the same level of rigour if delegated to closed-source social media platforms and their ad targeting algorithms.
We conclude that social media advertising should not be eligible as a recruitment tool for clinical studies so long as the processing of even anonymised social media usage data and the training of predictive models by data analytics and AI companies is not sufficiently regulated. The more specific and vulnerable the target group of a clinical study (e.g. rare or stigmatised diseases) is, the more severe are the structural ethical considerations proposed in our analysis. Moreover, it is likely (but will have to be detailed in future research) that many of the risks we pointed out also hold for targeted advertising services outside social media platforms, such as
Footnotes
Acknowledgments
We thank Anastasija Kocić, Mareike Lisker and Jan Siebold for critical discussions, background research and proof reading of this manuscript at its various stages.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Theresa Willem's contribution to this work was supported by the H2020 European Research Council (grant number 848223).
