Abstract
A 60-year-old female with a 5-year history of infiltrating basal cell carcinoma of the left ala underwent Mohs micrographic surgery requiring seven stages for complete clearance. The resulting 3.5 × 2.5 cm defect affected the entire left ala, nasal sidewall, medial cheek, lower lateral cartilage, and inferior nasal mucosa. Reconstruction involved using a bipedicle mucosal flap for internal lining, a scaphoid cartilage graft for structural support, and a paramedian forehead flap for the overlying cutaneous coverage, followed by a series of staged refinements for optimal cosmetic and functional outcomes. This case highlights principles for multilayered nasal reconstruction emphasizing subunit planning, mucosal lining restoration, and vascularized flap coverage to achieve both airway patency and esthetic integrity.
Introduction
Extensive nasal defects involving multiple subunits present a complex reconstructive challenge because restoration of both form and function must be achieved simultaneously. The esthetic subunit principle described by Burget and Menick recommends excision along the boundaries of esthetic subunits rather than simply filling partial defects. 1 This approach allowed the scars to be hidden within natural contours while restoring the integrity of each subunit. Subsequent studies have reinforced the value of this principle for extensive defects and explored its application in more complex clinical scenarios.2,3
Broader considerations such as skin color, texture, and minimizing donor site morbidity often influence individualized adaptations of the subunit principle. Singh and Bartlett described modifications to optimize esthetic outcomes while preserving structural stability. 4 Techniques that combine subunit-based excision with turn-over island flaps for internal lining and forehead flaps for external coverage have been reported to achieve excellent functional and cosmetic results. 5
The paramedian forehead flap has become the standard for cutaneous nasal reconstruction because of its robust vascularity, reliable arc of rotation, and close match in skin texture and color. 6 Large case series have demonstrated its safety and versatility in both single-stage and staged procedures with consistently favorable outcomes. 7
This case report describes a staged reconstruction of a large multisubunit nasal defect using subunit-based planning, mucosal lining reconstruction, cartilage grafting, and a paramedian forehead flap for cutaneous coverage.
Case report
A 60-year-old female presented with a 5-year history of primary infiltrating basal cell carcinoma of the left ala. Tumor clearance was achieved after seven stages of Mohs micrographic surgery. The resulting defect measured 3.5 × 2.5 cm and involved the entire left ala, the inferior nasal sidewall, the medial cheek, the lower lateral cartilage, and the inferior nasal mucosa (Figure 1).
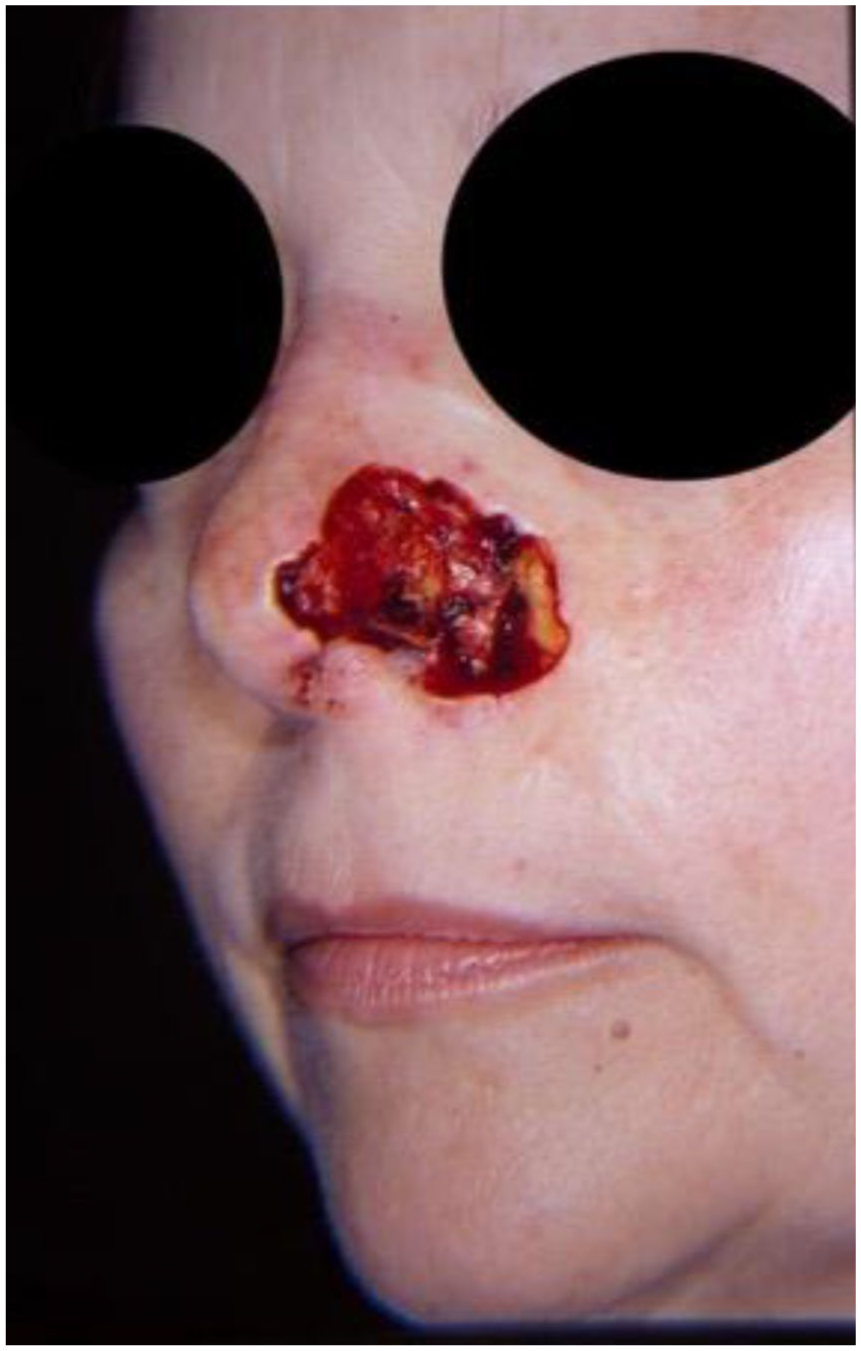
Preoperative defect involving left ala, sidewall, and medial cheek.
Reconstruction began with delineation of the subunit boundaries by excising residual skin of the left ala and nasal sidewall. The medial cheek defect was addressed first by undermining the tissue and advancing it medially toward the nasofacial sulcus. This advancement was secured using a periosteal suture anchored to the left nasal bone.
The internal nasal lining was reconstructed using a 10 mm-wide bipedicle mucosal flap incised medially from the nasal septum and extended laterally to the alar lining. The flap was undermined from the septum and advanced inferiorly in a bucket-handle fashion to recreate the nasal lining with thin, pliable mucosa. This minimized intranasal bulk and avoided the obstruction sometimes associated with turned-over pedicle flaps. The mucosal flap was positioned slightly below the anticipated cartilage graft to allow for secure inset and functional restoration.
A 10 mm-wide scaphoid cartilage graft was harvested to provide structural support. Pockets were created medially and laterally, and the graft was inset using 6–0 nylon sutures. Additional interrupted horizontal mattress sutures of chromic gut were used to secure the graft to the mucosal flap for stability.
An aluminum foil template was used to guide the design of a paramedian forehead flap centered on the supratrochlear artery (Figure 2). The 14 mm-wide pedicle was elevated with periosteum near the artery to preserve vascularity. The flap was undermined to the supraorbital ridge and thinned distally to the level of the hair bulbs, allowing single-stage contour refinement.

Intraoperative template for design of the alar and nasal sidewall defects, status post cheek advancement, bipedicle mucosal flap, and scaphoid cartilage graft.
The distal edge of the forehead flap was sutured to the free margin of the mucosal flap, and the remainder of the flap was inset to cover the defect (Figure 3). The donor forehead site was closed primarily, leaving a small residual area to granulate. Sutures were removed after 1 week. At 3 weeks, the pedicle was divided and inset to complete the reconstruction of the ala and nasal sidewall. At 3 months, further refinements deepened the alar–nasal crease to restore subunit definition. At 6 months, the patient demonstrated excellent functional nasal patency, symmetry, and minimal scarring (Figure 4).

Immediate postreconstruction result.

Final outcome at 6 months demonstrating nasal patency and cosmetic contour.
Discussion
This case illustrates the application of several fundamental principles in multisubunit nasal reconstruction. Restoring the internal lining with nasal mucosa was essential for preserving airway function and avoiding the bulk associated with turned-over skin flaps. The bipedicle mucosal flap provided thin, vascularized tissue that maintained intranasal patency without requiring secondary thinning procedures. 5
Structural support was restored using a scaphoid cartilage graft, which offered a balance between rigidity and minimal bulk. Compared with thicker conchal grafts, scaphoid cartilage provided stability while preserving a natural nasal contour and minimizing donor site morbidity. 4
The paramedian forehead flap served as the cornerstone for cutaneous coverage because of its robust axial blood supply and close color and texture match to nasal skin. Its vascularity allowed aggressive thinning during the initial surgery, which in many cases eliminates the need for additional stages while maintaining excellent flap viability.6,7
The staged approach consisted of an initial inset, pedicle division at 3 weeks, and contour refinements at 3 months, which allowed for precise reconstruction of both form and function. At 6 months, the patient achieved excellent cosmetic subunit definition and functional airway patency consistent with principles described in prior large reconstructive series (Figure 5).1,3,7

Inferior view showing nasal patency and maintained functionality 1 year postsurgery.
Overall, this case demonstrates that successful reconstruction of multisubunit nasal defects relies on meticulous subunit planning, restoration of thin vascularized mucosal lining, placement of stable cartilage support, and the use of a robust paramedian forehead flap for cutaneous coverage. A staged approach provides the best opportunity for both functional airway preservation and esthetic refinement.
Footnotes
Consent to participate
Written informed consent for patient information and images was provided by the patient.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
