Abstract
Congenital syphilis remains a preventable cause of neonatal morbidity, often resulting from undiagnosed or untreated maternal infection. We report a case of a late-preterm infant born to a mother with late latent syphilis underdiagnosed during pregnancy. Vertical transmission occurred transplacentally, given that the neonate presented with respiratory distress and pathognomonic signs such as pemphigus on both feet at birth. Laboratory evaluation confirmed syphilis infection, with high titer of RPR (Rapid Plasma Reagin) and TPHA (Treponema Pallidum Hemagglutination Assay) and markedly elevated inflammatory markers. The infant received a 10-day course of intravenous penicillin, leading to rapid clinical improvement and resolution of skin lesions. Serial serological monitoring showed a steady decline in RPR titers, achieving seronegativity by 6 months, accompanied by catch-up growth by 1 year. This case underscores the importance of thorough antenatal screening, early diagnosis, and treatment of maternal syphilis, and comprehensive management and follow-up of infected infants, particularly in resource-limited settings as Cambodia.
Introduction
Mother-to-child transmission of syphilis remains a significant global health issue despite prevention efforts. 1 Caused by Treponema pallidum subspecies pallidum, syphilis can be transmitted vertically, mainly through the placenta during pregnancy or less commonly during delivery. 2 In 2016, the congenital syphilis rate was estimated to be 473 cases per 100,000 live births worldwide (661,000 cases), over half of which resulted in Adverse Birth Outcomes (ABOs). Only 6% of these occurred in mothers who were adequately screened and treated, highlighting gaps in prevention. 3 Although maternal treatment reduces transmission risk, vertical transmission can still occur, especially with late or inadequate therapy.4,5 Neonates with congenital syphilis may present with a range of symptoms, including hepatosplenomegaly, skeletal abnormalities, jaundice, and skin rashes. 6 Pemphigus syphiliticus, or congenital bullous syphilis, is a rare, yet important, presentation prompting diagnosis and treatment.6,7 In what follows, we report a case of pemphigus syphiliticus in a preterm infant born to a mother with undiagnosed latent syphilis, who was successfully treated and followed up for 12 months.
Case presentation
A female neonate was delivered via vaginal delivery at 34 6/7 weeks of gestational age (WGA), with normal anthropometric measurements: birth weight of 2,300 g (70th percentile), head circumference 30 cm (20th), and length 47 cm (87th). In spite of meconium-stained amniotic fluid (MSAF), the birth was uneventful with Apgar scores of 8, 9, and 10 at 1, 5, and 10 min, respectively.
Her 18-year-old mother, primigravida, had no pregnancy-related complications. Antenatal care (ANC) visits were done regularly at a private clinic. However, her syphilis rapid test was reactive during the last visit, yet she was neither tested nor treated for syphilis serologies because she was asymptomatic. About 2 years prior to the pregnancy, she and her partner, with skin lesions, were diagnosed with primary syphilis, were treated with unknown oral antibiotics for 2 weeks. She was admitted to our Maternity Ward for preterm labor at 34 4/7 WGA. Post-partum maternal serology after retrospective diagnosis of congenital syphilis revealed high titer of RPR (1:32) and TPHA (1:1280). She had a late latent syphilis, underdiagnosed and untreated.
The neonate was admitted to the Neonatal Intensive Care Unit (NICU) for respiratory distress in a late-preterm infant. At the initial physical examination, she was pink and active, with a good muscle tone. However, she had mild respiratory distress (respiratory rate of 70/min and SpO2 90% on room air) and pemphigus on both feet (Figure 1(a)). Fontanella was soft; there was no hepatosplenomegaly. She was put under a nasal cannula with oxygen 1 L/min. Chest x-ray was in favor of Transient Tachypnea of Newborn (TTN). Babygram showed no bone abnormalities. Benzyl-penicillin was given due to suspected Congenital Syphilis. Sepsis workup, prior to antibiotic administration, was done and revealed: a normal leucocyte count (17 × 109/L), with an absolute neutrophil count of 6.62 × 109/L, and Immature to Total neutrophil ratio (I/T ratio) of 0.13; hemoglobin and platelets were within normal range. However, C-reactive protein (CRP) was high (106 mg/L), and procalcitonin (PCT) was also elevated (Table 1). The newborn’s syphilis tests were positive (RPR 1:32, TPHA 1:640). Lumbar puncture was done and was within normal range; culture of blood and gastric aspirate were sterile. According to CDC guidelines for a ‘highly probable’ case, a 10-day regimen of Benzyl-Penicillin was prescribed at a dosage of 50,000 IU/kg, administered intravenously every 12 h for 7 days, followed by every 8 h for an additional 3 days.
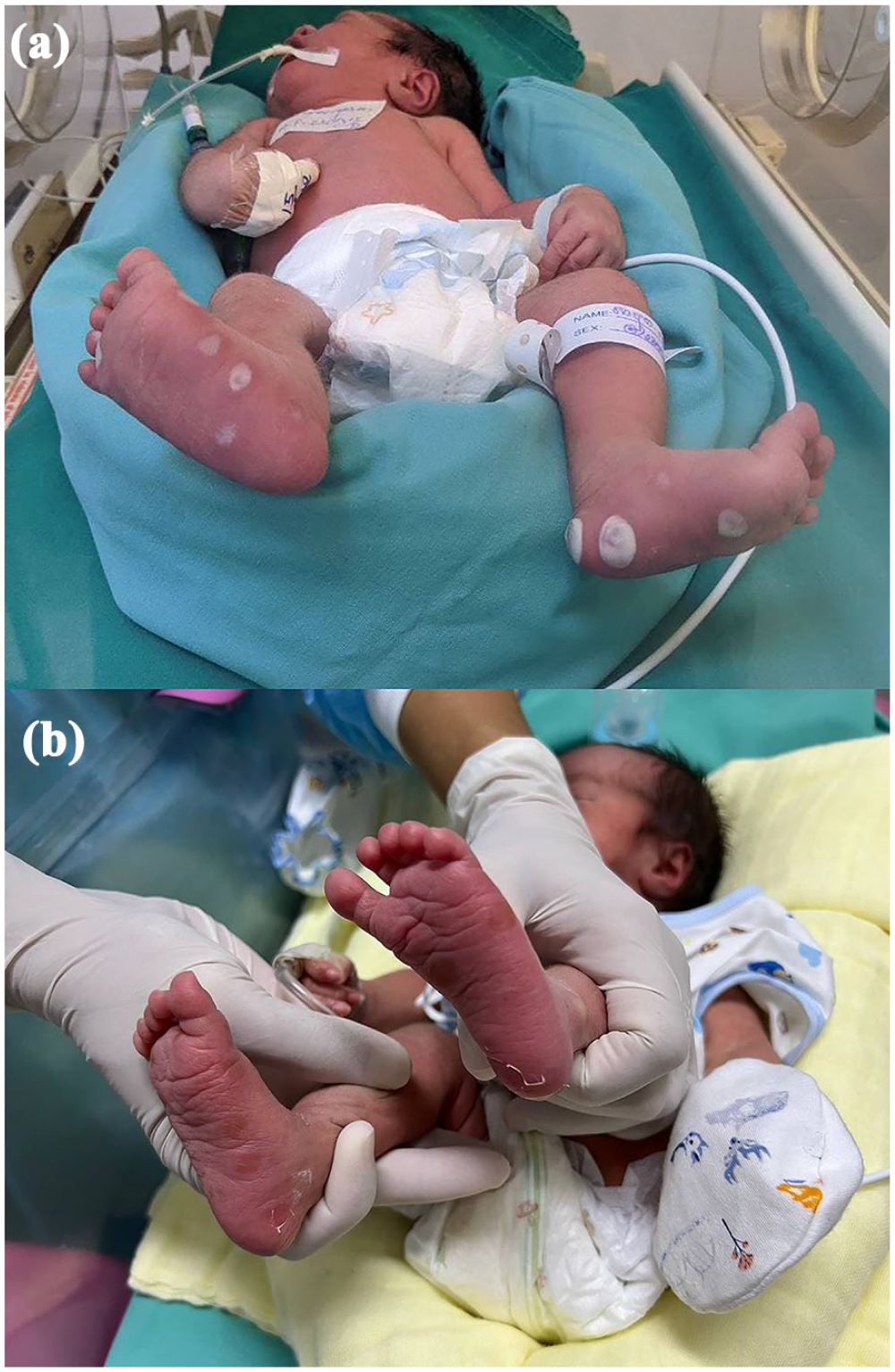
(a) Pemphigus syphiliticus on both feet at birth (b) Pemphigus at Day 2 after initiation of penicillin treatment.
Laboratory investigations of the neonate.

The infant’s clinical condition stabilized within 48 h of treatment, with gradual weaning of oxygen support and good tolerance to enteral feeding. Inflammatory markers significantly decreased, with CRP reducing from 106 to 33 mg/L and PCT from 1.8 to 0.7 mcg/L. The pemphigus lesions peeled rapidly and healed with residual induration (Figure 1b). Cranial and cardiac ultrasounds showed no abnormality. She was discharged on Day 10 of life, at a corrected gestational age of 36 weeks and 2 days, and was followed up at our department until the age of 1 year.
At our outpatient clinic, she was followed up every 3 months to monitor the progression of skin lesions, growth milestones, and syphilis serology (RPR and TPHA). Post-infection skin induration resolved spontaneously by the age of 6 months (Figures 2 and 3). Despite preterm birth and congenital infection, catch-up growth was successfully achieved by 12 months of age. Serial serological follow-up showed that the RPR titer decreased twofold by 1 month of age, indicating the effectiveness of the 10-day penicillin therapy, and became negative by 6 months of age (Table 2).

Pemphigus scarring at 1 month of life.

Healing of pemphigus at 3 months of life.
Syphilis serological follow-up.

Discussion
Congenital syphilis (CS) continues to be a major, yet preventable, cause of neonatal morbidity and mortality globally, with a marked resurgence in incidence despite the availability of effective screening and treatment.8,9 Through our aforementioned case, this challenge is clearly illustrated by a late-preterm neonate who developed CS following missed opportunities for maternal diagnosis and treatment, despite regular ANC. The mother’s reactive syphilis rapid test late in pregnancy, combined with the lack of confirmatory serology and absence of treatment, underscores ongoing gaps in ANC screening practices. This issue is reflected in recent case reports and surveillance data worldwide. For instance, in the United States, between 2020 and 2021, the incidence of CS increased by 30.5% (approximately 77.9 cases per 100,000 live births), representing a significant increase of 219.3% compared to 2017.9,10
Maternal-to-fetal transmission of Treponema pallidum can occur at any stage of pregnancy via transplacental spread, or less commonly, during delivery through contact with infectious lesions. 11 This case underscores that even asymptomatic mothers or those with a remote history of treated syphilis can transmit infection to the fetus in case of inadequate screening and treatment during the current pregnancy. Current guidelines recommend repeating syphilis testing in pregnancy for individuals at increased risk, such as those with late or no prenatal care, unstable housing, or a history of incarceration. 12
The newborn’s presentation with pemphigus and respiratory distress, without hepatosplenomegaly, exemplifies the broad and sometimes atypical clinical spectrum of CS. This presents a diagnostic challenge for both pediatricians and dermatologists due to the extensive differential diagnoses, particularly bullous dermatoses (e.g. bullous impetigo/staphylococcal scalded skin syndrome, bullous congenital ichthyosiform erythroderma, and neonatal pem-phigus). 13 Differentially, congenital pemphigus syphiliticus is characterized by fluid-filled vesicles and bullae predominantly on the extremities, which rapidly desquamate and heal with scarring. 14 Similar to other reported cases, such as those with unusual skin eruptions or isolated hematological findings, this variability can complicate early recognition and diagnosis 15 .
The diagnosis of CS presents challenges due to the transplacental passage of maternal IgG antibodies, which can complicate the interpretation of neonatal serologic tests. 12 As such, treatment decisions are often guided by a synthesis of factors, including maternal syphilis identification and treatment history, clinical and laboratory findings in the neonate, and comparison of maternal and neonatal nontreponemal titers (e.g. RPR or VDRL), ideally performed by the same laboratory.7,12 In our case, the diagnosis was confirmed by elevated RPR titers in both mother and infant, while neurosyphilis was initially excluded based on normal cerebrospinal fluid (CSF) analysis. However, it is important to note that although CSF abnormalities occur in 40% to 60% of infants with CS, a negative CSF VDRL or normal cell counts do not definitively rule out the infection or the potential for later development of neurosyphilis. 16 Therefore, accurate diagnosis requires a comprehensive approach that considers maternal history, infant physical examination, serologic testing, and other investigations, such as long-bone radiographs.12,16,17 Regarding the pemphigus syphiliticus, PCR or dark-field microscopy from skin lesions was not available due to resource limitations in our setting. The differential diagnosis was considered based on clinical presentation, absence of bacterial culture growth, and rapid response to penicillin therapy, which is not typical for bullous impetigo or genetic bullous disorders like epidermolysis bullosa. As shown in the presented case, the diagnostic strategy aligns with established guidelines recommending thorough evaluation-including CSF analysis, complete blood counts, and long-bone radiographs, in at-risk infants with inadequate or unknown maternal treatment.9,10
Prompt initiation of intravenous penicillin G resulted in rapid clinical improvement and reduction of inflammatory markers, consistent with international guidelines.12,16 Serial serological monitoring demonstrated an appropriate decline in RPR titers, with seronegativity achieved by 6 months, in favor of clinical outcomes and catch-up growth. These findings are consistent with the study of Sergio Fanella et al., emphasizing that infants treated appropriately for CS generally demonstrate a consistent decline in RPR titers, with seronegativity often achieved by 6 months of age. 18 In addition, the CDC recommends that all neonates with reactive nontreponemal tests undergo thorough follow-up examinations and serologic testing (RPR or VDRL) every 2 to 3 months until seronegativity is confirmed. 12 Arnold et al. further advise repeating nontreponemal tests at 1, 2, 4, 6, and 12 months post-treatment, noting that titers are expected to become nonreactive by 12 months if treatment is adequate, with many infants demonstrating seroreversion by 6 months. Persistently reactive titers beyond this timeframe may indicate treatment failure and warrant further evaluation. 16 However, adherence to the recommended follow-up remains a significant challenge. For example, Rocha et al. reported that 78.5% of infants with CS did not attend any of the recommended follow-up visits, indicating a low compliance rate of about 20%. 19 Similarly, another Brazilian cohort found that although most children attended at least one follow-up visit, 81.9% did not adhere to the full recommended schedule. 20 In contrast, our case demonstrates successful adherence to follow-up protocols, which was facilitated by dedicated outpatient clinic staff who maintained close contact with the family, involvement of community health workers, and comprehensive counseling on the importance of ongoing monitoring. These coordinated efforts contributed to the patient’s consistent attendance at serological and clinical follow-up visits for up to 1 year of age.
Conclusion
Our case further emphasizes the critical importance of comprehensive antenatal screening, timely maternal treatment, and newborn long-term follow-up. Despite the preventable nature of CS, missed opportunities for maternal diagnosis and treatment still lead to adverse outcomes, including prematurity, low birth weight, and, in some cases, irreversible sequelae in neonates. Hence, it is essential to strengthen antenatal syphilis screening, repeat testing in late pregnancy for high-risk women, ensure timely and adequate maternal treatment with penicillin, and implement partner notification and treatment to reduce reinfection. Neonates born to untreated or inadequately treated mothers require thorough evaluation and prompt antibiotic therapy, followed by structured serological and clinical follow-up to confirm cure and support healthy development.
Footnotes
Acknowledgements
The authors would like to thank the NICU staff of Calmette Hospital for their daily hard work, and especially the OPD staff for their close follow-up with the patient’s family.
Ethical considerations
Our institution does not require ethical approval for reporting individual cases or case series.
Consent to Participate
Written informed consent was obtained from the patient’s parents and is available for review upon request.
Consent for Publication
Written informed consent was obtained from a legally authorized representative(s) for anonymized patient information to be published in this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
