Abstract
The limb body wall complex is a rare congenital disorder that is marked by various anomalies such as thoracoschisis, gastroschisis, limb defects and exencephaly. These defects are not compatible with life and result in spontaneous abortion or stillbirth. It is important to diagnose the anomalies on time and counsel the patients extensively to make the right decision. In this case report, we present a woman in her early twenties pregnant with a fetus with multiple anomalies including ectopia cordis, gastroschisis, meningomyelocele, kyphoscoliosis and congenital talipes equinovarus diagnosed as limb body wall complex at 18 weeks of gestation. Despite extensive counselling by the consultant, the couple decided to continue the pregnancy due to cultural beliefs which ultimately affected the maternal health. The fetus was spontaneously delivered at 28 weeks when the mother came to the hospital with ruptured membranes and the fetus was pronounced dead at birth. The co-occurrence of all these anomalies poses a challenge in diagnosis and management. Extensive counselling is required for the patient to make the appropriate decision for better outcomes. Cultural beliefs can play a major role in the decision-making of the patients and their families which can have a significant effect on maternal outcomes.
Introduction
Limb body wall complex (LBWC) is a multisystem defect that presents with severe congenital malformations including thoracoschisis, gastroschisis and limb defects, and exencephaly which may be absent in some cases. Most fetuses do not reach term and are aborted spontaneously, very early in pregnancy. Despite being a collection of various fetal anomalies, whose origins have been attributed to different teratogens and genetic abnormalities, the exact aetiology of LBWC has not yet been described. The frequency of LBWC is reported to be 1 per 14,000 births to 1 per 31,000 births worldwide.1,2 This makes this fetal disorder a rare congenital anomaly that requires extensive research for further understanding of the condition and its diagnosis and prognosis.
The increased occurrence of congenital abnormalities in newborns is attributed to the influence of teratogens, maternal illnesses, chemical and radiation exposure, maternal nutritional excesses or deficiencies (e.g. folic acid) and indiscriminate use of some drugs by pregnant women. 3 Other possible causes include errors in embryogenesis or genetic defects and chromosomal abnormalities. Developing countries face a severe threat of fetal anomalies due to uncontrolled infections, co-morbidities and nutritional deficiency. Late diagnosis is another obstacle due to insufficient awareness and education. Multisystem anomalies pose a greater risk than isolated anomalies and are strongly linked to an increased likelihood of stillbirth.
In the current case from Pakistan, we present a rare occurrence of a male fetus diagnosed prenatally with multiple anomalies, including ectopia cordis, gastroschisis, kyphoscoliosis, and congenital talipes equinovarus (CTEV) diagnosed as LBWC with associated meningomyelocele (MMC). The case also portrays how cultural beliefs may play a role in decision-making by the expectant parents and hence affect maternal and fetal outcomes despite extensive counselling.
Case presentation
A primigravida aged 23 presented to a tertiary care hospital’s gynaecological unit at 18 weeks of gestation for an antenatal check-up. The patient was married to a 24-year-old man in a non-consanguineous marriage. The patient did not have a history of any significant diseases, smoking, alcohol or drug abuse, nor was she exposed to known teratogens. The patient was referred to an advanced radiology centre for an anomaly scan. The scan revealed a significant defect in the ventral wall of the upper abdomen and thorax, with the fetus’s liver and heart protruding into the amniotic cavity. These findings indicated the presence of gastroschisis associated with ectopia cordis. Additionally, the fetus exhibited MMC and bilateral CTEV. The fetal cardiac activity was normal, and other fetal ultrasound parameters, that is biparietal diameter and femoral length, corresponded to the gestational age. There was no reported family history of congenital anomalies. The patient had been taking folate since the first trimester based on self-education. Although the couple was well educated, they did not consult a gynaecologist prior to 18 weeks. Following comprehensive counselling, the couple first decided to abort the fetus due to little or no chances of survival but later decided to continue the pregnancy due to cultural and religious beliefs despite the challenging diagnosis.
After 20 weeks of gestation, the patient developed hypertension, evidenced by a blood pressure reading ranging from 140/90 to 160/100 mmHg. Labetalol was started at week 22 when the blood pressure remained high at around 160/100 mmHg constantly, and laboratory investigations revealed proteinuria. The patient, on the subsequent two visits, also complained of disturbed mental health, evidenced by anxiety and insomnia. At 28 weeks, she experienced labour pains and returned to the hospital with ruptured membranes. While an immediate caesarean section was planned if spontaneous delivery did not occur, the baby was ultimately delivered spontaneously after 8 h of labour at 28 weeks, with a birth weight of 900 g. The newborn was also examined by a neonatologist who concluded that the baby had multiple congenital anomalies, including ectopia cordis, gastroschisis, MMC, kyphoscoliosis and CTEV. The condition was diagnosed as LBWC (Figures 1 and 2). However, upon birth, the baby only gasped twice and did not exhibit a discernible heart rate, although it had been well detectable before birth. Furthermore, spontaneous breathing was absent. Regrettably, the newborn did not survive and was pronounced dead. The mother was discharged after 14 h. The X-ray, magnetic resonance imaging (MRI) or karyotyping of the delivered baby could not be done since the parents did not consent and were urged to perform the funeral at the earliest.
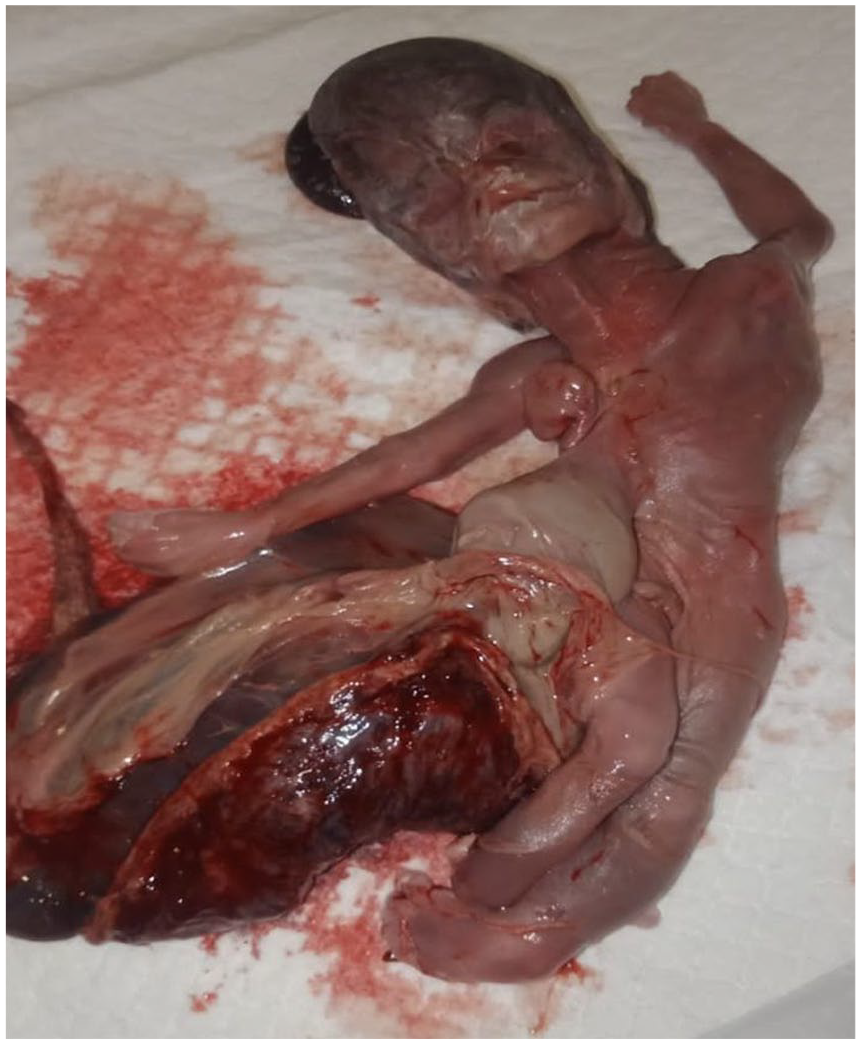
Ventral view of the delivered fetus.

Dorsal view of the delivered fetus.
The woman then conceived another baby 6 months later and presented to our gynaecological unit at the third week of gestation. All subsequent scans were normal, and the mother is expected to deliver the baby in July of this year.
Discussion
This case was about a male fetus diagnosed with multiple congenital anomalies, including ectopia cordis, gastroschisis, MMC and CTEV leading to the diagnosis of LBWC also called body stalk anomaly. This co-occurrence of ventral wall defects and musculoskeletal and neurological abnormalities is rare. Pepper et al. 4 documented a case of a phenotypic male fetus at 24 weeks of gestation with a ventral body wall defect, where the heart, liver, stomach, intestines and spleen were protruding, indicating a clinical presentation of ectopia cordis and gastroschisis. Kashyap et al. 5 documented a case report of an LBWC characterized by thoracoabdominal defects, ectopia cordis, left clubfoot and umbilical artery kyphoscoliosis. The patient in this case was a 30-year-old primigravida with a pre-existing condition of hypothyroidism and was diagnosed with gestational diabetes mellitus classified as A1. This case differs from our case in that the fetus in this case had no MMC. Also, the primigravida woman in our case had no underlying conditions that could increase the likelihood of congenital anomalies. The fetal anomaly, in our case, could be due to novel sporadic genetic mutations in the developing embryo or a disruption in development without any predisposing factors. In a case study by Devi et al., 6 a fetus at 24 weeks of gestation was diagnosed with LBWC. The findings included scoliosis, gastroschisis, lumbosacral meningocele, CTEV, and cleft palate. However, there was no information available on any potential risk factors associated with the mother. Risk factors such as pre-existing maternal diseases, use of teratogenic drugs by the expectant mother, consanguineous marriage or a family history of birth defects are frequently reported to be associated with babies born with birth anomalies.
The diagnostic criteria for LBWC are highly disputed and also vary depending on the phenotype; however, three main features have been described. These include exencephaly or encephalocele with facial clefts, thoraco and/or abdominoschisis, and limb defects. The different phenotypes also lead to differences in diagnostic criteria depending on placental-cranial attachment or placental-abdominal attachment.2,7 The fetus in this case exhibited ectopia cordis, gastroschisis and limb defects associated with MMC but not exencephaly or facial clefts. Nonetheless, the major features of ventral body wall and limb defects were enough to diagnose LBWC.
Karyotyping and DNA testing, like next-generation sequencing, can detect genetic mutations that lead to various fetal anomalies. However, these require modern techniques and skilled personnel. Although our hospital is a tertiary care centre, it lacks the technology and experienced personnel to carry out these tests. Moreover, the centres where these are available are quite expensive, and the parents did not consent to pathological autopsy or any sort of genetic testing. Therefore, we also could not carry out X-rays or MRIs of the delivered fetus to look for any other congenital anomalies.
Congenital anomalies can be detected very early in pregnancy, as demonstrated in previous cases reported in the literature. 8 Realistic Vue imaging and Crystal Vue imaging are new three-dimensional approaches based on image-contrast enhancement to view the embryo in utero with great detail and depth. Fetal development, chromosomal abnormalities and even the behaviour of the baby can be well assessed through the two software applications namely, Crystal Vue and Realistic Vue. This advanced technology and software applications were introduced by Samsung Medison Co. Ltd. via their Samsung WS80 Elite ultrasound device system.9,10 Early detection of anomalies can give the obstetrician and parents ample time for counselling and decision-making, depending upon the severity of the condition. Due to the unavailability of such techniques, we resorted to routine anomaly scans which are usually done around the 20th week of pregnancy. Nevertheless, in addition to the unavailability of such modern techniques, cultural beliefs also play a significant role in improving the quality of life of the mother through proper counselling and decision-making. In our case, we had done everything we could to diagnose the severe anomalies and counsel the patient extensively. Still, the patient did not consent to terminate the pregnancy despite first agreeing to do so.
Managing children with multiple congenital anomalies has been a challenge and uncertainties may arise. The decision-making process regarding investing in therapy and life support for children with multiple congenital anomalies is complex, as there are no simple rules or models to follow. Hence, distinguishing between therapeutic persistence and offering treatment with uncertain benefits remains unclear. 11 Proper counselling of the parents is essential after the diagnosis of the anomalies to prevent maternal mortality and morbidity and extensive healthcare burden. To carry out the required diagnostic tests during early pregnancy under the supervision of skilled personnel, an extensive spread of awareness is required among healthcare workers, especially in countries with a lack of resources. Awareness must be spread among the people regarding planned and supervised pregnancies and regular antenatal check-ups beginning early in pregnancy.
Conclusion
In this case report, we presented a fetus diagnosed with LBWC through an anomaly scan at 18 weeks of gestation. The presence of multiple anomalies in a fetus as presented in this case report usually has a poor prognosis. Handling such cases requires interdisciplinary cooperation, early prenatal screening and thorough counselling. Future developments in genetic and prenatal diagnostics can improve maternal outcomes and offer important new insights into the underlying mechanisms of various congenital defects.
Footnotes
Acknowledgements
None.
Author contributions
E.I. evaluated the case as the consultant of the patient, provided the required data and wrote the manuscript. M.A. and M.S.D. wrote the manuscript, and searched and revised the literature. A.W.M.J. wrote and revised the manuscript. All authors read and approved the final manuscript.
Availability of data and materials
Not applicable.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship and/or publication of this article.
Ethical approval
Our institution does not require ethical approval for reporting individual case report or case series.
Informed consent
A written informed consent was obtained from the patient for the use of the information and any accompanying images for writing this case report and its publication in a medical journal. A copy of consent is available for review by the editor.
